13 August 2020 - Case of the Month #494
All cases are archived on our website. To view them sorted by case number, diagnosis or category, visit our main Case of the Month page. To subscribe or unsubscribe to Case of the Month or our other email lists, click here.
Thanks to Dr. Farres Obeidin, UCLA Medical Center, California (USA) and Dr. Borislav Alexiev, Northwestern University Feinberg School of Medicine, Illinois (USA), for contributing this case and to Dr. Farres Obeidin for writing the discussion.

Advertisement Register for the webcast here
Case of the Month #494
Clinical history:
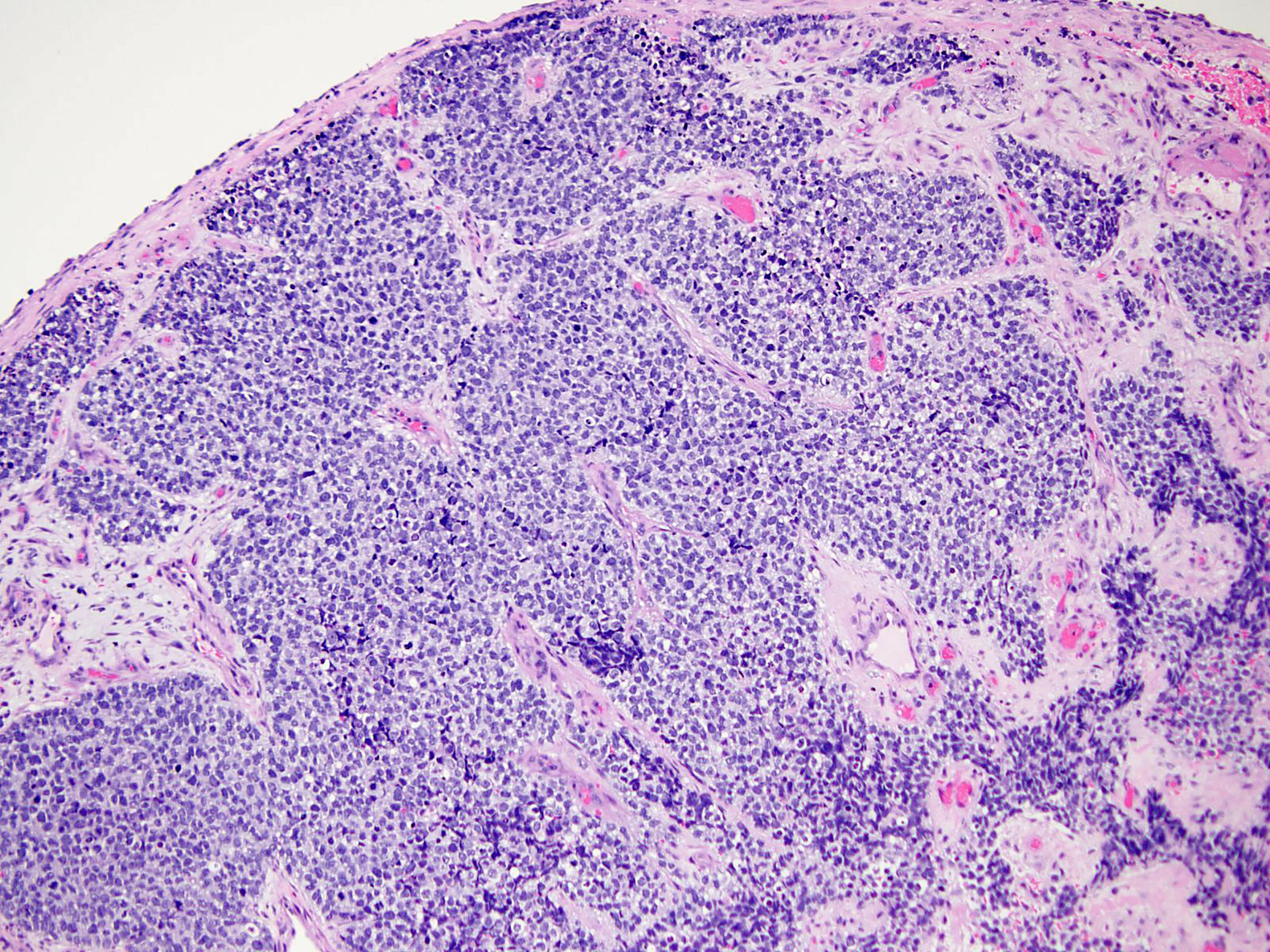
A 49 year old man with no significant medical history presented with symptoms of nasal obstruction. CT imaging revealed a large right nasal mass with involvement of the ethmoid sinus. An excisional biopsy was performed and reveals the morphology below.
Histopathology images:
What is your diagnosis?
Diagnosis: Alveolar rhabdomyosarcoma
Test question (answer at the end):
Which of the following molecular aberrations may be seen in alveolar rhabdomyosarcoma?
A. COL1A1-PDGFB
B. SS18-SSX1
C. EWSR1-FLI1
D. FOXO1-PAX7
E. PAX3-MAML3
Stains:
Discussion:
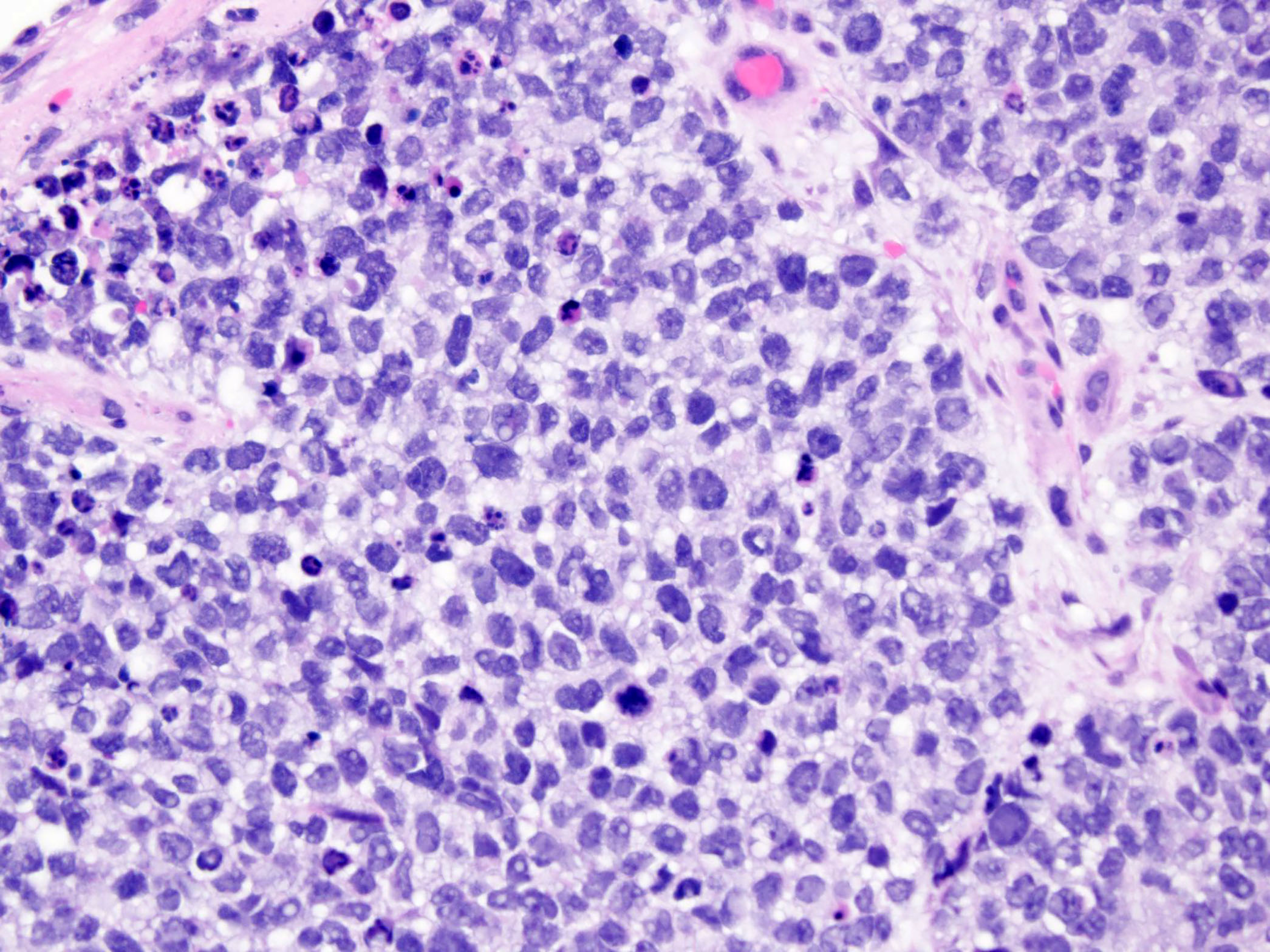
Alveolar rhabdomyosarcoma (ARMS) is a malignant neoplasm comprised of a monomorphous population of round blue cells that exhibit myogenic features. ARMS may occur at any age but is most common in young adults and adolescents (median age 6.8 - 9.0 years). Most commonly, ARMS presents in the extremities but additional sites of involvement include paraspinal and perineal regions, paranasal sinuses and the breast. ARMS is the most common sarcoma found within the sinonasal tract (Laryngoscope 2012;122:2137).
Classically, ARMS has been defined histologically by monotonous round cells with variable morphology depending on the presence of or absence of fibrous stroma that separates the tumor into nests and produces the picket fence alveolar pattern. However, the solid variant of ARMS lacks the fibrovascular septa and forms sheets of round blue cells, sometimes with little to no distinct rhabdomyoblastic differentiation. Rare cases showing mixed features of both ARMS and embryonal rhabdomyosarcoma (ERMS) have been described (Am J Clin Pathol 2013;140:82).
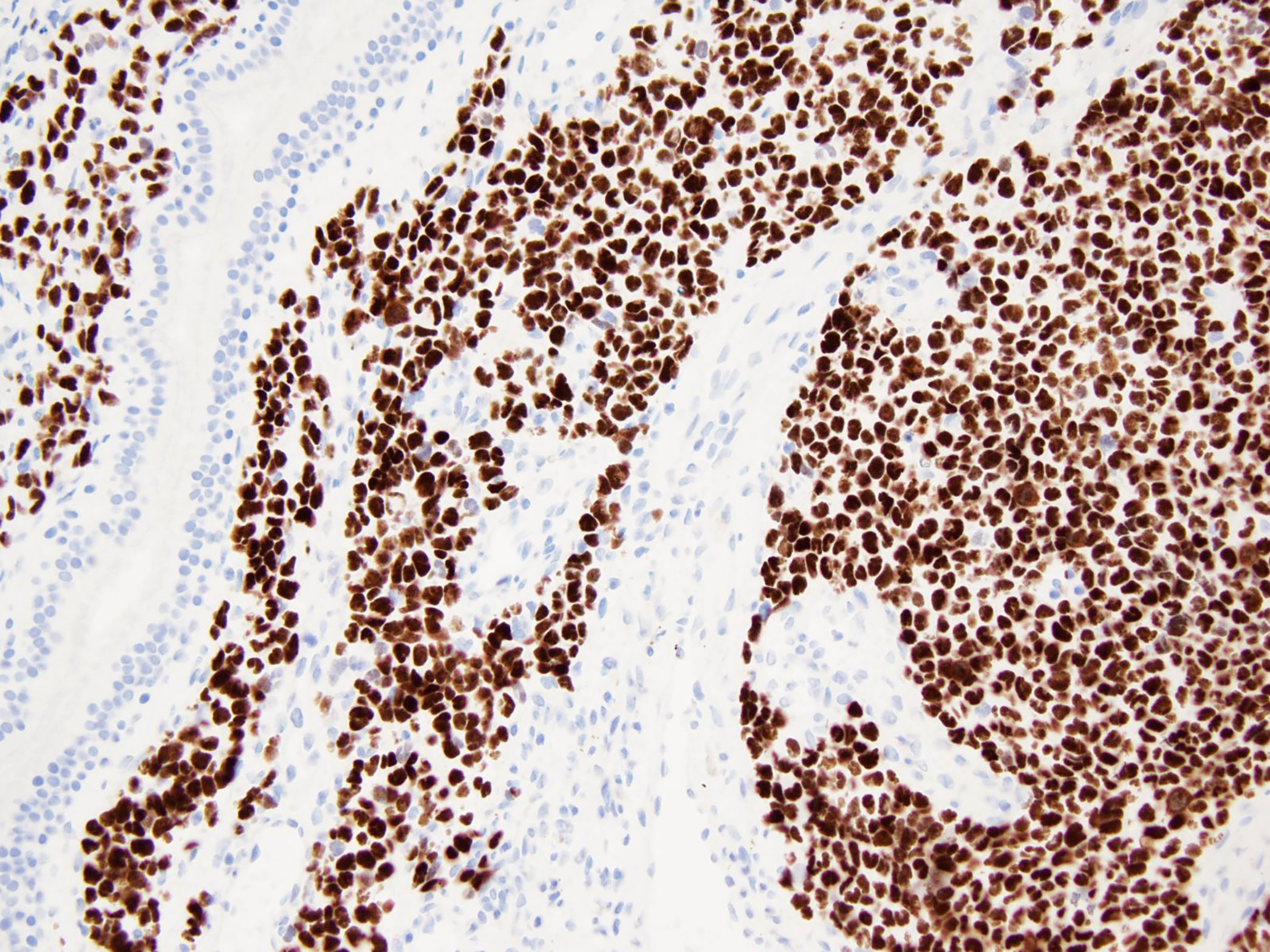
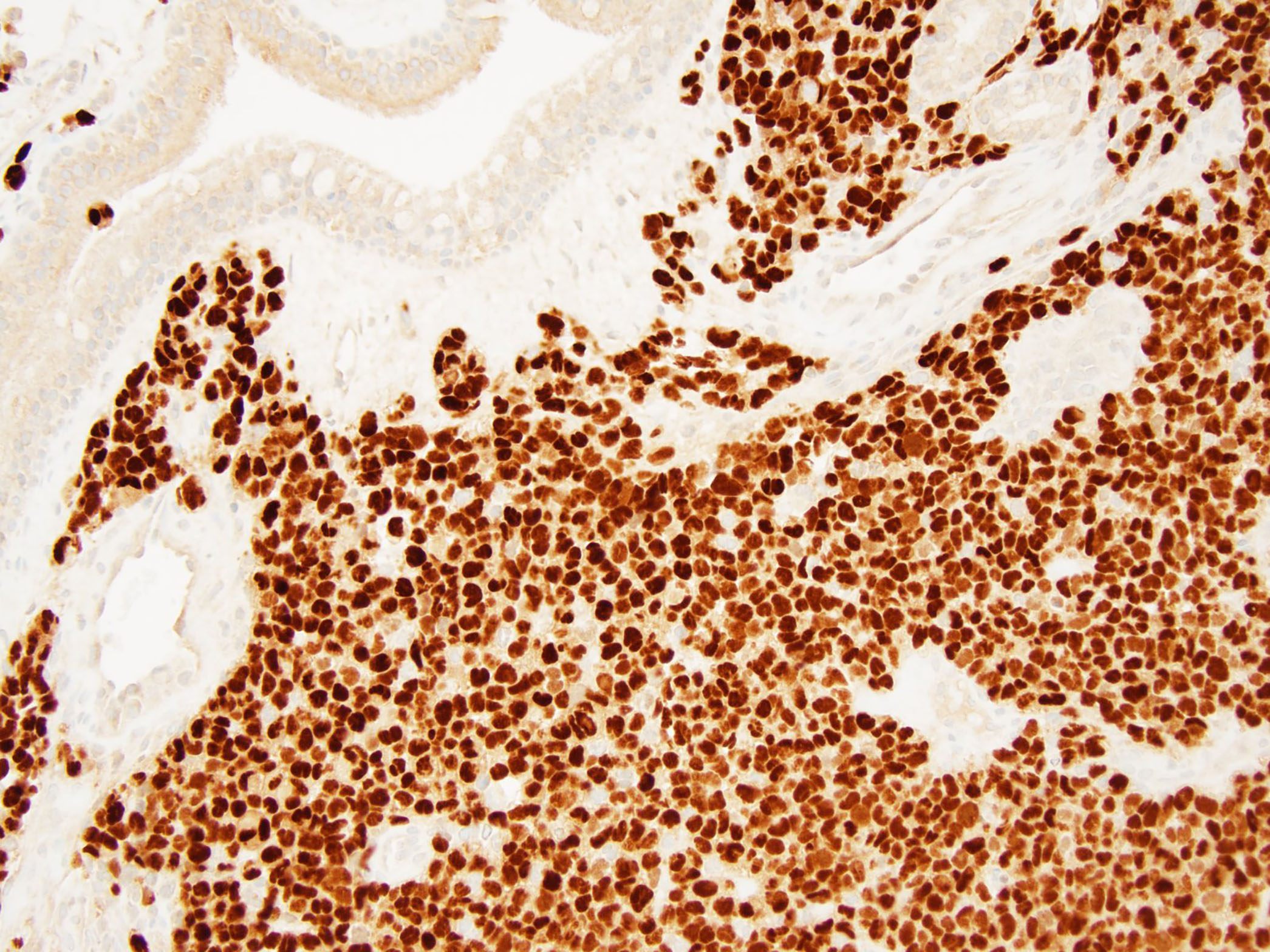
Ancillary studies are recommended to both confirm ARMS, distinguish it from other small round cell tumors as well as ERMS and to aid in prognostication. ARMS shows positivity for MyoD1 and myogenin by IHC. The majority of ARMS harbor translocations involving the FOXO1 gene (77%). Among fusion positive ARMS, 55% have FOXO1-PAX3 and 22% have FOXO1-PAX7 (J Clin Oncol 2002;20:2672). It has also been observed that fusion positive ARMS cases characteristically show diffuse, strong expression of myogenin while fusion negative ARMS and ERMS show relatively weak myogenin expression in 70 - 80% of cases (Am J Clin Pathol 2013;140:82).
The International Classification of Pediatric Sarcomas has stratified pediatric rhabdomyosarcoma into several prognostic groups: superior prognosis (botryoid and spindle cell / sclerosing rhabdomyosarcoma), intermediate prognosis (conventional ERMS) and poor prognosis (ARMS, undifferentiated sarcoma). In adults, spindle cell / sclerosing rhabdomyosarcoma and pleomorphic rhabdomyosarcoma have poor prognosis. Within the ARMS classification, the overall survival is higher in FOXO1-PAX7 translocated tumors than in FOXO1-PAX3 translocated tumors. Fusion negative ARMS cases have similar outcomes to ERMS. Solid or alveolar morphology does not affect prognosis (Adv Anat Pathol 2013;20:387, Pediatr Blood Cancer 2016;63:634).
On small biopsies, there is much difficulty in distinguishing small round blue cell tumors so the differential is broad. Sarcomas comprise less than 1% of head and neck malignancies and only 10 - 15% of all sinonasal malignancies. Care must be taken to rule out nonsarcomatous tumors in this setting (BMC Ear Nose Throat Disord 2018;18:4). The epithelial tumor differential includes basaloid squamous cell carcinoma, nasopharyngeal carcinoma, sinonasal undifferentiated carcinoma (SNUC), NUT carcinoma, solid adenoid cystic carcinoma, SMARCB1 deficient sinonasal carcinoma and neuroendocrine carcinoma (Head Neck Pathol 2016;10:75). Other nonepithelial tumors that arise in this differential include olfactory neuroblastoma (Arch Pathol Lab Med 2015;139:1498), melanoma and lymphoma. Sarcomas that arise in the small round blue cell tumor differential include the following: rhabdomyosarcoma, Ewing sarcoma, undifferentiated round cell sarcoma (Ewing-like tumors), desmoplastic small round cell tumor, poorly differentiated synovial sarcoma, mesenchymal chondrosarcoma and small cell osteosarcoma (Head Neck Pathol 2016;10:75). While there is often overlap between these diagnoses in terms of nonspecific IHC markers like keratins and CD99, the diagnosis is aided by the presence of MyoD1 / myogenin immunoreactivity (rhabdomyosarcoma), tumor specific translocations (alveolar rhabdomyosarcoma, Ewing sarcoma, synovial sarcoma, DSRCT, mesenchymal chondrosarcoma) or extracellular elements like cartilaginous / osteoid differentiation.
The tumor in this case shows a small round blue cell tumor morphology with no distinct differentiation on H&E. No rosette structures, malignant osteoid / cartilage, striated rhabdomyoblasts or prominent desmoplasia are seen. Immunostains show diffuse positivity for desmin, MyoD1 and myogenin. Confirmatory FISH testing with a break apart probe revealed the presence of a FOXO1 rearrangement, confirming the diagnosis of alveolar rhabdomyosarcoma.
Test question answer:
D. FOXO1-PAX7
Alveolar rhabdomyosarcoma is characterized by the presence of translocations involving FOXO1 (typically with PAX3 or PAX7) in the majority of cases. Translocation negative cases have been described and is a poor prognostic indicator. COL1A1-PDGFB may be seen in dermatofibrosarcoma protuberans. SS18 fusions are characteristic of synovial sarcoma. EWSR1-FLI1 is the most common fusion in Ewing sarcoma. PAX3-MAML3 is a fusion product found in biphenotypic sinonasal sarcoma, characterized by coexpression of myogenic and neural features.
Additional Sources:
Fletcher: WHO Classification of Tumours of Soft Tissue and Bone (Medicine), 4th Edition, 2013
All cases are archived on our website. To view them sorted by case number, diagnosis or category, visit our main Case of the Month page. To subscribe or unsubscribe to Case of the Month or our other email lists, click here.
Thanks to Dr. Farres Obeidin, UCLA Medical Center, California (USA) and Dr. Borislav Alexiev, Northwestern University Feinberg School of Medicine, Illinois (USA), for contributing this case and to Dr. Farres Obeidin for writing the discussion.

Advertisement Register for the webcast here
Case of the Month #494
Clinical history:
A 49 year old man with no significant medical history presented with symptoms of nasal obstruction. CT imaging revealed a large right nasal mass with involvement of the ethmoid sinus. An excisional biopsy was performed and reveals the morphology below.
Histopathology images:
What is your diagnosis?
Click here for diagnosis, test question and discussion:
Diagnosis: Alveolar rhabdomyosarcoma
Test question (answer at the end):
Which of the following molecular aberrations may be seen in alveolar rhabdomyosarcoma?
A. COL1A1-PDGFB
B. SS18-SSX1
C. EWSR1-FLI1
D. FOXO1-PAX7
E. PAX3-MAML3
Stains:
Discussion:
Alveolar rhabdomyosarcoma (ARMS) is a malignant neoplasm comprised of a monomorphous population of round blue cells that exhibit myogenic features. ARMS may occur at any age but is most common in young adults and adolescents (median age 6.8 - 9.0 years). Most commonly, ARMS presents in the extremities but additional sites of involvement include paraspinal and perineal regions, paranasal sinuses and the breast. ARMS is the most common sarcoma found within the sinonasal tract (Laryngoscope 2012;122:2137).
Classically, ARMS has been defined histologically by monotonous round cells with variable morphology depending on the presence of or absence of fibrous stroma that separates the tumor into nests and produces the picket fence alveolar pattern. However, the solid variant of ARMS lacks the fibrovascular septa and forms sheets of round blue cells, sometimes with little to no distinct rhabdomyoblastic differentiation. Rare cases showing mixed features of both ARMS and embryonal rhabdomyosarcoma (ERMS) have been described (Am J Clin Pathol 2013;140:82).
Ancillary studies are recommended to both confirm ARMS, distinguish it from other small round cell tumors as well as ERMS and to aid in prognostication. ARMS shows positivity for MyoD1 and myogenin by IHC. The majority of ARMS harbor translocations involving the FOXO1 gene (77%). Among fusion positive ARMS, 55% have FOXO1-PAX3 and 22% have FOXO1-PAX7 (J Clin Oncol 2002;20:2672). It has also been observed that fusion positive ARMS cases characteristically show diffuse, strong expression of myogenin while fusion negative ARMS and ERMS show relatively weak myogenin expression in 70 - 80% of cases (Am J Clin Pathol 2013;140:82).
The International Classification of Pediatric Sarcomas has stratified pediatric rhabdomyosarcoma into several prognostic groups: superior prognosis (botryoid and spindle cell / sclerosing rhabdomyosarcoma), intermediate prognosis (conventional ERMS) and poor prognosis (ARMS, undifferentiated sarcoma). In adults, spindle cell / sclerosing rhabdomyosarcoma and pleomorphic rhabdomyosarcoma have poor prognosis. Within the ARMS classification, the overall survival is higher in FOXO1-PAX7 translocated tumors than in FOXO1-PAX3 translocated tumors. Fusion negative ARMS cases have similar outcomes to ERMS. Solid or alveolar morphology does not affect prognosis (Adv Anat Pathol 2013;20:387, Pediatr Blood Cancer 2016;63:634).
On small biopsies, there is much difficulty in distinguishing small round blue cell tumors so the differential is broad. Sarcomas comprise less than 1% of head and neck malignancies and only 10 - 15% of all sinonasal malignancies. Care must be taken to rule out nonsarcomatous tumors in this setting (BMC Ear Nose Throat Disord 2018;18:4). The epithelial tumor differential includes basaloid squamous cell carcinoma, nasopharyngeal carcinoma, sinonasal undifferentiated carcinoma (SNUC), NUT carcinoma, solid adenoid cystic carcinoma, SMARCB1 deficient sinonasal carcinoma and neuroendocrine carcinoma (Head Neck Pathol 2016;10:75). Other nonepithelial tumors that arise in this differential include olfactory neuroblastoma (Arch Pathol Lab Med 2015;139:1498), melanoma and lymphoma. Sarcomas that arise in the small round blue cell tumor differential include the following: rhabdomyosarcoma, Ewing sarcoma, undifferentiated round cell sarcoma (Ewing-like tumors), desmoplastic small round cell tumor, poorly differentiated synovial sarcoma, mesenchymal chondrosarcoma and small cell osteosarcoma (Head Neck Pathol 2016;10:75). While there is often overlap between these diagnoses in terms of nonspecific IHC markers like keratins and CD99, the diagnosis is aided by the presence of MyoD1 / myogenin immunoreactivity (rhabdomyosarcoma), tumor specific translocations (alveolar rhabdomyosarcoma, Ewing sarcoma, synovial sarcoma, DSRCT, mesenchymal chondrosarcoma) or extracellular elements like cartilaginous / osteoid differentiation.
The tumor in this case shows a small round blue cell tumor morphology with no distinct differentiation on H&E. No rosette structures, malignant osteoid / cartilage, striated rhabdomyoblasts or prominent desmoplasia are seen. Immunostains show diffuse positivity for desmin, MyoD1 and myogenin. Confirmatory FISH testing with a break apart probe revealed the presence of a FOXO1 rearrangement, confirming the diagnosis of alveolar rhabdomyosarcoma.
Test question answer:
D. FOXO1-PAX7
Alveolar rhabdomyosarcoma is characterized by the presence of translocations involving FOXO1 (typically with PAX3 or PAX7) in the majority of cases. Translocation negative cases have been described and is a poor prognostic indicator. COL1A1-PDGFB may be seen in dermatofibrosarcoma protuberans. SS18 fusions are characteristic of synovial sarcoma. EWSR1-FLI1 is the most common fusion in Ewing sarcoma. PAX3-MAML3 is a fusion product found in biphenotypic sinonasal sarcoma, characterized by coexpression of myogenic and neural features.
Additional Sources:
Fletcher: WHO Classification of Tumours of Soft Tissue and Bone (Medicine), 4th Edition, 2013