
Management of Pathology Practices
November 2008
The Tangled Web of Claim Payments
How Managed Care Contracts Kill Your Revenue
By Mick Raich, Vachette Pathology
The goal of this article is to help billing companies understand how their physicians’ managed care contracts are interconnected and how these interconnected contracts are designed to keep payment for services intentionally confusing.
Over the past six years my pathology company has reviewed managed care contracts for over 100 pathology practices. Often we ask the pathology practice or their billing entity to provide a list of the insurance carriers and a list of all their managed care plans. Although this article is based upon my experience as an auditor of pathology practices, it applies to other physician practices as well.
During our research, we often find that practices have contracts and discounted relationships with insurance carriers that they never really thought they had.
When you dissect the details, you find that there are plans paying discounts, when in fact, the group may be adamant that it is not contracted with this plan.
How does this happen? First you have to understand that there has been massive consolidation of managed care plans. This consolidation can be easily compared to the consolidation of hospitals after the implementation of DRGs. When an industry matures, often it consolidates, and the managed care industry is no exception. Consolidation led to various insurance plans buying other insurance plans. When this happens, the plans basically buy the contracted covered lives.
Another issue is the development of affiliated relationships or contracts. If a managed care plan does not have market penetration, but still wants to provide service to its covered lives in a given area, it may develop an affiliate relationship in order to “access the network.” This access allows the plan basically to scrub its claim to the affiliated insurance plan; instead of paying the claim “out-of-network” at a higher price, the claim is re-priced under the affiliated contract at a discount.
How Providers Lose
Here is an example. Group A has a contract with Great West, which is a mid level Third Party Administrator (TPA). A physician sees a patient in the National Care Network (NCN). The physician does not have a contract with NCN, but NCN does have a deal that gives it access to the Great West contract. Instead of the claim being paid out of network at 80% of the physician’s charge by NCN, the claim is re-priced as in-network under Great West at the discounted rate of their contract, perhaps 40% of the charge. The provider loses.
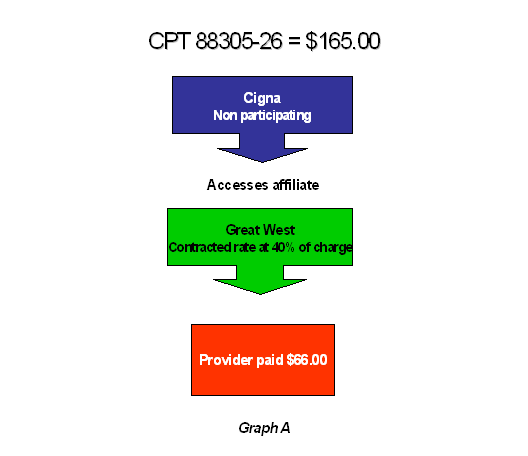
Think this comparison is done? Sorry. Another example could be that the provider is participating with Great West, but non-participating with Cigna. However, remember that Cigna owns Great West. So in fact, although the provider is non-participating with Cigna, the claim is moved to Great West and is paid at a participating rate. See Graph A.
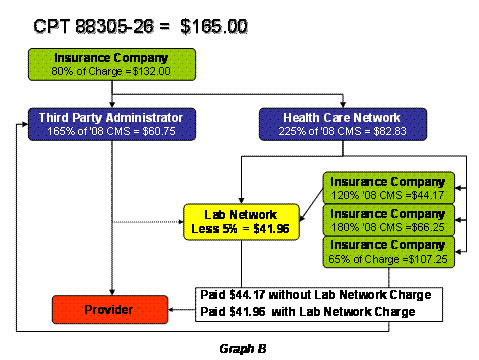
Next, some claims are subject to two re-pricers. For example, you may see the claim go to one TPA and then see it routed through a regional lab network that charges you a percentage to “process” the claim. In this case, your claim is discounted by the TPA and then the regional lab network also takes a percentage. See Graph B.
Here is yet another point to ponder. Many billing services have spent considerable time and effort developing managed tracking mechanisms. They are to be commended for their efforts trying to unravel this quagmire of claims. The real problem lies when the provider has TPAs and networks have a tiered payment system. In this case you could have three different rates being paid for the same CPT code. One payer, Multiplan, actually has over 600 insurance plans in its network.
It will not surprise you to know that the insurance industry has actually published articles on how to prevent your claim from going out of network and how to lower costs by routing claims into discounts. An Internet review of some of the networks shows that many plans have a 20-page list of insurance plans with which they have contractual relationships.
Solving the Problem
Many providers and biller companies audit their billing EOBs every quarter. These are the groups that find and decipher this payment octopus. Also, these are the practices that get checks back from insurance companies for erroneous underpayments. It is not unusual for billing companies to discover hundreds of thousands of dollars of underpayments.
In the pathology field, the truly best practices have eliminated the majority of these issues by being non-participating with as many managed care plans as possible. They have no contracts with TPAs, insurance networks, lab networks, or PHOs. Our best practices have only one or two managed care plans, plus the government payors. If you look outside pathology, you will see similar paths carved out by boutique practices that have developed in the family practice arena. In this case, these practices do not accept any insurance.
A final note here should really put things into perspective. After you review all these contracts and their various alliances, there is one fact that is truly clear: the providers are not getting richer out of this deal; the billing companies are not profiting from this; and in fact it can be noted that billing costs have gone up as the payment process has become more muddled. Only the middlemen, such as insurance plans, TPA, networks, and claims processors, are making money.
Interrelated Insurance Plans
Below is a partial list of various insurance plans and who they own or may have a relationship with. Please remember these are fluid relationships and they are changing even as we speak, therefore, the partial list below is just our opinion of how the relationships present at this moment in time.
Aetna
owns US Healthcare
owns Cofinity
owns Sloan
owns PPOM
utilizes Preferred Health Plan as TPA
Blue Cross Blue Shield Association
BlueCross and BlueShield companies are independent, community-based and locally operated. Collectively, they provide healthcare coverage to more than 102 million people - one in three – Americans.
Alabama, Blue Cross and Blue Shield
Alaska, Premera Blue Cross Blue Shield
Arizona, Blue Cross and Blue Shield
Arkansas Blue Cross and Blue Shield
California, Anthem Blue Cross
California, Blue Shield
Colorado, Anthem Blue Cross and Blue Shield
Connecticut, Anthem Blue Cross and Blue Shield
Delaware, Blue Cross and Blue Shield
District of Columbia, CareFirst Blue Cross Blue Shield
Florida, Blue Cross and Blue Shield
Georgia, Blue Cross and Blue Shield
Hawaii Medical Service Association
Idaho, Blue Cross
Idaho, Regence BlueShield of Idaho
Illinois, Blue Cross and Blue Shield
Indiana, Wellpoint, Inc.
Iowa, Wellmark Blue Cross and Blue Shield
Kansas, Blue Cross and Blue Shield
Kentucky, Anthem Blue Cross and Blue Shield
Louisiana, Blue Cross and Blue Shield
Maine, Anthem Blue Cross and Blue Shield
Maryland, CareFirst Blue Cross Blue Shield
Massachusetts, Blue Cross and Blue Shield
Michigan, Blue Cross and Blue Shield
Minnesota, Blue Cross and Blue Shield
Mississippi, Blue Cross and Blue Shield
Missouri, Anthem Blue Cross Blue Shield
Missouri, BlueCross and BlueShield of Kansas City
Montana, Blue Cross and Blue Shield
Nebraska, Blue Cross and Blue Shield
Nevada, Anthem Blue Cross and Blue Shield
New Hampshire, Anthem Blue Cross and Blue Shield
New Jersey, Horizon Blue Cross and Blue Shield
New Mexico, Blue Cross and Blue Shield
New York, BlueCross & BlueShield of Western
New York, BlueShield of Northeastern
New York, Empire Blue Cross and Blue Shield
New York, Excellus BlueCross BlueShield
North Carolina, Blue Cross and Blue Shield
North Dakota, Blue Cross and Blue Shield
Ohio, Anthem Blue Cross and Blue Shield
Oklahoma, Blue Cross and Blue Shield
Oregon, Regence BlueCross BlueShield of Oregon
Pennsylvania, Blue Cross of Northeastern -- Wilkes-Barre
Pennsylvania, Highmark Blue Shield
Pennsylvania, Capital Blue Cross -- Harrisburg
Pennsylvania, Highmark Blue Cross Blue Shield -- Pittsburgh
Pennsylvania, Independence Blue Cross -- Philadelphia
Puerto Rico, La Cruz Azul de
Puerto Rico, Triple-S
Rhode Island, Blue Cross and Blue Shield
South Carolina, Blue Cross and Blue Shield
South Dakota, Wellmark Blue Cross and Blue Shield
Tennessee, Blue Cross and Blue Shield
Texas, Blue Cross and Blue Shield
Utah, Regence BlueCross BlueShield of Utah
Vermont, Blue Cross and Blue Shield
Virginia, Anthem Blue Cross and Blue Shield
Washington, Premera Blue Cross
Washington, Regence BlueShield
West Virginia, Mountain State Blue Cross and Blue Shield
Wisconsin, Anthem Blue Cross and Blue Shield
Wyoming, Blue Cross and Blue Shield
International Plans
Jamaica, Blue Cross of Jamaica Ltd.
Panama, BlueCross BlueShield of Panama
Uruguay, Blue Cross & Blue Shield de Uruguay
Cigna
owns Great West
owns CCN
owns One Healthplan
Coalition American
owns National Preferred Provider Network (NPPN)
accesses Provider Select Network
Concentra
accessed Viant Holdings
owns ppo Next
owns BeechStreet Network merged with CappCare
owns Focus PPO Network
Coventry
owns Group Health Plan owns Care Management Resources
owns FirstHealth
owns CCN
owns HealthAmerica
owns Healthcare USA
owns Mail Handlers
accesses the Concenta network
Evolutions Healthcare Systems
Network partners with
AmeriSys, Inc.,
FOCUS Healthcare Management
Third Party Administrators and other Payor Relationships (not inclusive) with
Anchor Benefit Consulting
CoreSource
Corporate Benefit Services of America
Assurant
Hospital Benefits
Humana
owns Choicecare
owns OSF
accesses Concentra Network
accesses Viant Network
accesses Cofinity in Michigan
MMO
owns MedBen
owns CareWorks (Mco)
UHC
owns Americhoice
owns Evercare
owns Great Lakes
owns Golden Rule
owns Empire UHC
owns Ingenix
owns Optimum Health
owns Ovations
owns Oxford
owns PacifiCare
owns Multiplan
owns PHCS
owns Health EOS
owns BCE Emergis
formerly ProAmerica
Wellmark, Inc.
dba Wellmark Blue Cross Blue Shield of Iowa
dba Wellmark of South Dakota, Inc.
also provides third-party administration through subsidiaries in Iowa and South Dakota
Wellpoint
owns Anthem Blue Cross
independent licensee of the Blue Cross Blue Shield Association
operates through Unicare
TPAs / Networks
· 4Most
· Apex Benefit Services
· Beechstreet
· Care Management Resources
· Central Benefits Administrators
· Direct Care America
· First Health/CCN Network/Mail Handlers
· Fortified Provider Network
· Health Advantage, Inc.
· HealthSpan
· HFC, Inc.
· Multiplan (has over 600 insurance plans in its network)
· NPP
· National Preferred Provider Network (NPPN)
· Ohio Health Choice
· Private Healthcare Systems (PHCS)
· PPOM and Sloans Lake
· ppoNext (aka HealthStar)
· Preferred Health
· SelectNet
· Three Rivers Provider Network
· UP & UP (United Payers & United Providers)
EXAMPLES OF ROUTING
Health Alliance Plan uses Cigna as TPA
National Care Network processes discount through Great West
Cofinity states rates for Humana/Choicecare in Michigan would be the same as Aetna/PPOM.
Preferred Health Plan Group network doesn’t contract with Michigan, contract only extends from Louisville, KY, to Indiana. If a member has the plan they would go thru PPOM or Cofinity Network.
Mick Raich is the President and CEO of Vachette Pathology. Vachette Pathology provides practice management and consulting services to over 50 pathology groups nationwide. Contact: mraich@vachettepathology.com or call 866-407-0763.