Table of Contents
Definition / general | Terminology | Epidemiology | Sites | Pathophysiology | Etiology | Clinical features | Laboratory | Prognostic factors | Case reports | Treatment | Differential diagnosis | Additional referencesCite this page: Crookston K, Rosenbaum LS, Gober-Wilcox J. Factor X deficiency. PathologyOutlines.com website. https://www.pathologyoutlines.com/topic/coagulationfactorXdef.html. Accessed April 19th, 2024.
Definition / general
- Factor X deficiency is a rare congenital bleeding disorder that is inherited as an autosomal recessive trait, and is characterized by a variable bleeding tendency
Terminology
- Also known as Stuart-Prower Factor Deficiency
- Deficiency classified as either:
- Type I: decreased functional activity and antigen level (quantitative defect)
- Type II: decreased functional activity and near normal antigen level (qualitative defect)
Epidemiology
- Estimated incidence of 1 in 500,000 to 1,000,000; however, in countries where consanguinity is more common (e.g. Iran), incidence is reported to be 1 in 200,000
- Estimated carrier incidence of 1 in 500
Sites
- Bleeding into skin and mucosa, joint and muscle, genitourinary tract, gastrointestinal tract, CNS (see clinical features below)
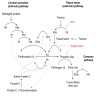
Pathophysiology
- Factor X is a vitamin K-dependent serine protease produced in the liver
- It is the first enzyme in the common pathway to form a fibrin clot
- Its activated form (in complex with factor Va, Ca++ and phospholipid) cleaves prothrombin to thrombin
- It has a long half-life of 20 - 40 hours
Images hosted on other servers:
Etiology
- Inherited as an autosomal recessive trait
- More than 80 mutations have been identified, which include small deletions, missense and frameshift mutations
Clinical features
- May be associated with bruising, epistaxis, menorrhagia, GI / GU bleeding, umbilical stump bleeding or bleeding after surgery, trauma, dental procedures, pregnancy or circumcision, recurrent fetal loss
- Bleeding symptoms in severe deficiency are similar to that seen in patients with factor VIII (hemophilia A) and factor IX (hemophilia B) deficiency
- Heterozygotes are usually asymptomatic but may have mild mucocutaneous bleeds
- Patients with severe deficiency are either homozygous or compound heterozygous
- Bleeding symptoms tend to correlate with factor X activity levels: mild (> 6% - 10%), moderate (1% - 5%) or severe (< 1%)
- A small percentage of patients develop factor X inhibitors with factor replacement therapy
Laboratory
- Prolonged PT and PTT that correct with mixing study
- Prolonged Russells viper venom time (measures the direct activation of factor X)
- Normal thrombin and bleeding time
- Factor X specific functional and immunologic assays for confirmation
Prognostic factors
- Particular genotypes [Gly(- 20)Arg, Gly94Arg and Gly380Arg mutations] are associated with higher rates of hemarthrosis and intracranial bleeding
Case reports
- Factor X deficiency presenting as chronic bilateral subdural hematomas in a 7 month old infant (Pediatr Neurosurg 2010;46:54)
Treatment
- For minor bleeding episodes, maintain factor X levels at 10% - 15% of normal using FFP (15 - 20 mL/kg followed by 3 - 6 mL/kg every 24 hours)
- For major bleeding episodes, trauma or surgical procedures, factor X rich prothrombin complex concentrates can be used to maintain factor X levels at 50% of normal
Differential diagnosis
- Acquired factor X deficiency (liver disease, vitamin K deficiency): also exhibits reduced levels of other coagulation factors; isolated factor X deficiency is associated with respiratory infection, AML and other malignancies, amyloidosis
- Acquired factor X inhibitors in patients without congenital factor X deficiency are rare but have been reported in leprosy and chemical exposure
- Other factor deficiencies: e.g. factor V, prothrombin
Additional references