Table of Contents
Definition / general | Epidemiology | Pathophysiology | Etiology | Clinical features | Diagnosis | Laboratory / cardiac testing | Radiology description | Radiology images | Prognostic factors | Case reports | Treatment | Diagrams / tables | Gross description | Microscopic (histologic) description | Microscopic (histologic) images | Immunohistochemistry & special stains | Molecular / cytogenetics description | Additional referencesCite this page: Amita R. Infective myocarditis. PathologyOutlines.com website. https://www.pathologyoutlines.com/topic/heartinfectiousmyocarditis.html. Accessed April 19th, 2024.
Definition / general
- The term 'myocarditis' was first introduced by Corvisart
- It is defined by WHO / International Society and Federation of Cardiology (ISFC) as an inflammatory disease of the heart muscle, diagnosed by established histological, immunological and immunohistochemical criteria
Epidemiology
- Postmortem data identify myocarditis in 8.6% to 12% of cases of sudden death in young adults
- The Myocarditis Treatment Trial reported the incidence of biopsy proven myocarditis in patients with unexplained heart failure to be 9.6%
Pathophysiology
- Murine models of enteroviral myocarditis suggest viral myocarditis is characterized by 3 phases
- Acute: entry of virus into myocytes, mediated through specific receptors such as the transmembrane coxsackievirus and adenovirus receptors (CAR)
- Subacute: acute injury of the myocytes, induced by virus replication leading to myocyte necrosis
- This exposes the intracellular antigens (e.g. cardiac myosin) and activates the host immune system
- The first phase is virus induced myocyte injury; the second phase is autoimmune mediated injury due to activated virus specific T cells which may target host organs by molecular mimicry
- The immune response declines with virus elimination; ventricular function usually recovers without sequelae or it may persist leading to the
- Chronic phase, characterized by myocardial remodeling and development of dilated cardiomyopathy (DCM)
Etiology
- Parvovirus B19, Coxsackie B virus, human herpesvirus 6 (HHV6) type B, adenovirus (Arch Cardiovasc Dis 2009;102:559 - Table 1)
Clinical features
- Highly nonspecific
- Patient may be asymptomatic or present with signs / symptoms of myocardial infarction or cardiac failure, including chest pain and cardiac arrhythmias
Diagnosis
- Endomyocardial biopsy is the gold standard to diagnose myocarditis
- As myocarditis is a focal disease, four to five biopsy samples obtained in more than one area of the right ventricular (RV) septum should be analysed using light microscopic examination and immunohistochemical assays
Laboratory / cardiac testing
- Leukocytosis and increased CRP levels but normal values do not exclude myocarditis
- Cardiac biomarkers such as troponins and creatine kinase lack specificity but may help to confirm the diagnosis of myocarditis
- Higher levels of troponin T may have prognostic value
- Serology of infective organisms is helpful
- Interpretation of antibody assays is complicated by other confounders such as reactivation or reinfection (e.g. HSV) or by cross reactions (e.g. EBV or enterovirus)
- ECG: widely used as screening tool despite low sensitivity
- Findings vary from nonspecific T wave and ST segment changes to ST segment elevation mimicking an acute myocardial infarction
- Atrial or ventricular conduction delays, supraventricular and ventricular arrhythmias can occur in patients with myocarditis
- The presence of Q waves or a new left bundle branch block (LBBB) are associated with higher rates of cardiac death or heart transplantation
Radiology description
- Chest Xray: cardiomegaly due to chamber dilation or pericardial effusion; may show pulmonary venous congestion, interstitial infiltrates, pleural effusions
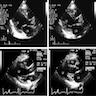
- Echocardiography:
- Evaluates cardiac chamber size and wall thickness
- Assess systolic and diastolic function
- Rule out other causes of cardiac failure such as valvular heart disease or other cardiomyopathies (hypertrophic or restrictive cardiomyopathy)
- Before an endomyocardial biopsy (EMB) procedure, echo is needed to exclude pericardial effusion and intracavitary thrombi
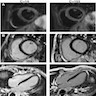
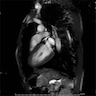
- Cardiovascular MRI: edema in T2 weighted imaging indicates acute myocardial inflammation
- Myocardial early gadolinium enhancement: T1 weighted segmented inversion recovery gradient echo sequence shows a difference in signal intensity between diseased and healthy myocardial regions with Gd-DTPA accumulation in late gadolinium enhancement (LGE) imaging
- Combination of these findings is currently regarded as the most sensitive and specific noninvasive approach to diagnose myocarditis
Radiology images
Prognostic factors
- Depends on clinical presentation, clinical parameters and EMB findings
- Patients with acute myocarditis and preserved left ventricular ejection fraction (LVEF) have a good prognosis with a high rate of spontaneous improvement without sequelae
- Patients with fulminant viral myocarditis and hemodynamic compromise at presentation have an excellent long term prognosis and are more likely to experience complete recovery if aggressive treatment or mechanical circulatory support is initiated early during the fulminant phase
Case reports
- 14 year old boy with family history of dilated cardiomyopathy induced by viral myocarditis (Case Reports in Cardiology 2012;2012)
- 15 year old boy with myocarditis mimicking acute coronary syndrome following influenza B virus infection (Cases J 2009;2:6809)
- 19 year old woman with viral myocarditis (Mayo Clin Proc 2009;84:1001)
- 23 year old man with idiopathic acute myocarditis during treatment for controlled malaria infection (Malar J 2014;13:38)
- 27 year old man with parvovirus B19 associated fulminant myocarditis successfully treated with immunosuppressive and antiviral therapy (Antivir Ther 2010;15:681)
- 34 year old man with acute myocarditis from coxsackie infection, mimicking subendocardial ischemia (Hellenic J Cardiol 2009;50:147)
- 46 year old woman with fulminant myocarditis (Rev Port Cardiol 2012;31:503)
- Two cases of dengue myocarditis (Infection 2013;41:709)
Treatment
- As no pathogen specific therapy of viral myocarditis has been shown to improve survival, treatment is symptomatic and based on clinical presentation
Diagrams / tables
Gross description
- Findings are nonspecific and include normal or dilated chambers
- May have softening and pallor of ventricles
- May have pericardial effusion and pericarditis with viral or bacterial myocarditis
- Late stages may show fibrosis that is focal or diffuse but the distribution is often random (see the image below), in contrast to the subendocardial fibrosis typically seen in ischemia
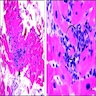
Microscopic (histologic) description
- Dallas criteria:
- Acute myocarditis: lymphocytic infiltrates in association with myocyte necrosis
- Borderline myocarditis: inflammatory infiltrates without evidence of myocyte necrosis
- Due to high interobserver variability, IHC is increasingly used for diagnosis
Microscopic (histologic) images
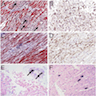
Immunohistochemistry & special stains
- CD3 for T cells
- CD68/PGM1 for activated macrophages
- HLA-DR to assess HLA class II
- EMB is considered to be inflamed by immunohistochemical detection of focal or diffuse mononuclear infiltrates (T lymphocytes and macrophages) with 14 cells / mm2, in addition to enhanced expression of HLA class II antigen
Molecular / cytogenetics description
- Nested PCR / real time PCR in EMB
- In situ hybridization techniques for identification of replicating viral genomes