Table of Contents
Definition / general | Essential features | Terminology | ICD coding | Epidemiology | Sites | Pathophysiology | Etiology | Diagrams / tables | Radiology description | Radiology images | Prognostic factors | Case reports | Treatment | Gross description | Gross images | Microscopic (histologic) description | Microscopic (histologic) images | Positive stains | Negative stains | Electron microscopy description | Molecular / cytogenetics description | Molecular / cytogenetics images | Differential diagnosis | Board review style question #1 | Board review style answer #1 | Board review style question #2 | Board review style answer #2Cite this page: Palsgrove D, Argani P. Eosinophilic, solid and cystic. PathologyOutlines.com website. https://www.pathologyoutlines.com/topic/kidneytumorescrcc.html. Accessed April 24th, 2024.
Definition / general
- Emerging subtype of renal cell carcinoma (RCC) with abundant eosinophilic cytoplasm and solid / cystic growth, not yet recognized in the 2013 International Society of Urological Pathology (ISUP) Vancouver Classification of Renal Neoplasia or the updated 2016 World Health Organization (WHO) renal tumor classification (Am J Surg Pathol 2013;37:1469, Eur Urol 2016;70:93)
Essential features
- Solid and cystic components
- Voluminous eosinophilic cytoplasm which frequently displays basophilic intracytoplasmic stippling / inclusions
- No clinical history or features of tuberous sclerosis complex
- CK20+ / CK7- / c-kit- / PAX8+ immunoprofile
- Frequently harbors somatic loss of function mutations in TSC1 or TSC2
Terminology
- ESC RCC
ICD coding
Epidemiology
- F > M
- Broad age range (14 - 75 years)
- No documented clinical features, family history or germline genetic testing suggestive of tuberous sclerosis complex; see differential diagnosis below for more information
Sites
- Left = right (no reported predilection)
Pathophysiology
- Sporadic tumors believed to fall within a spectrum of renal neoplasms that harbor TSC1 / 2 genetic alterations (including the granular eosinophilic macrocystic subtype of tuberous sclerosis associated RCC and possibly the oncocytoid subtype of RCC postneuroblastoma, Am J Surg Pathol 2018;42:1166)
- TSC1 (hamartin) and TSC2 (tuberin) form a functional heterodimer in the cytoplasm involved in cell signaling and proliferation through the kinase mTOR
- Negative regulators of the AKT / mTOR signaling pathway
- Loss of function mutations in TSC1 or TSC2 lead to constitutive mTORC1 activation that is uncoupled from upstream signaling inputs
Etiology
- Somatic loss of TSC1 or TSC2 tumor suppressor function (Eur Urol 2018;74:483, Am J Surg Pathol 2018;42:911, Am J Surg Pathol 2018;42:1166)
- No known predisposing factors
Radiology description
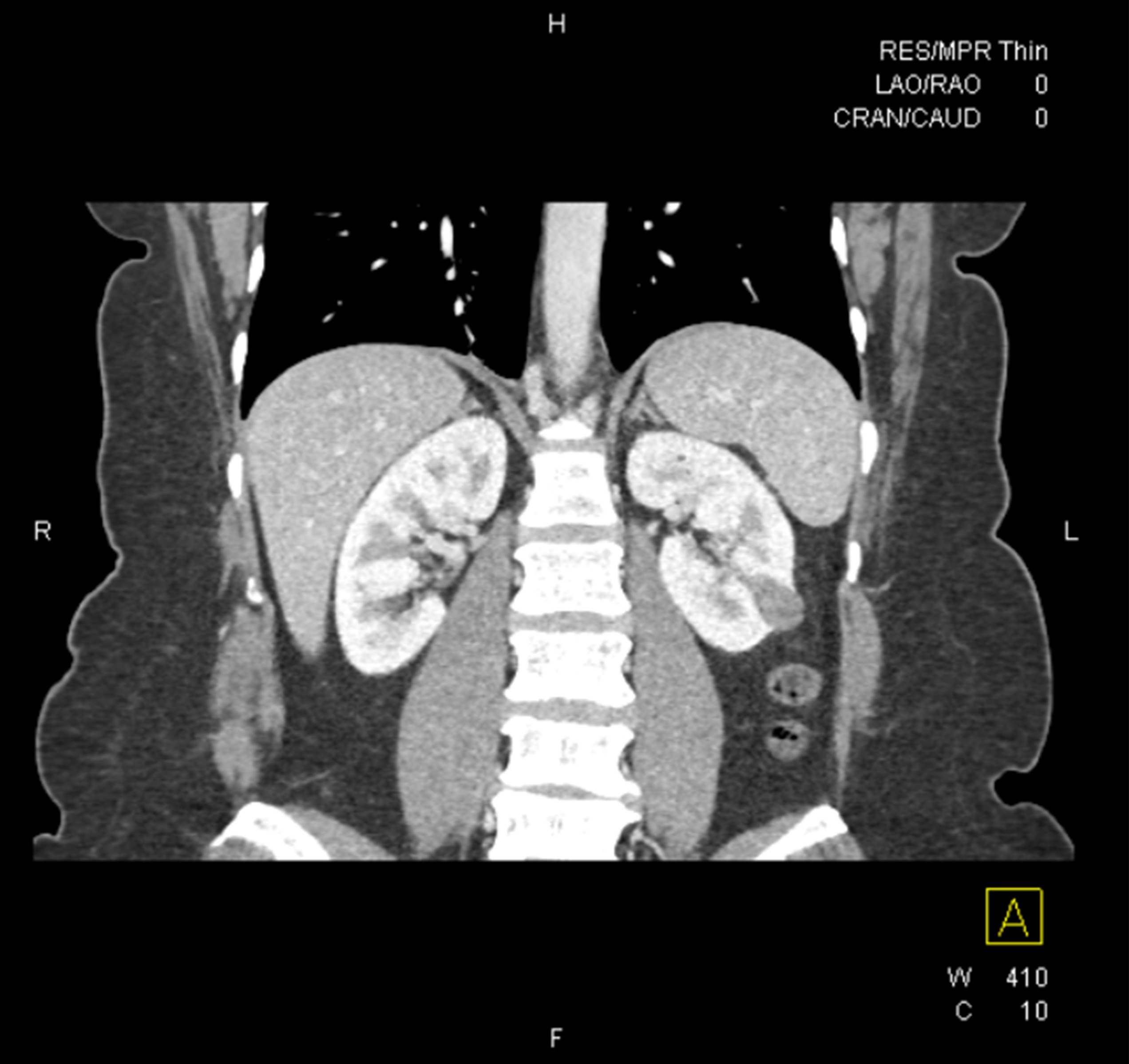
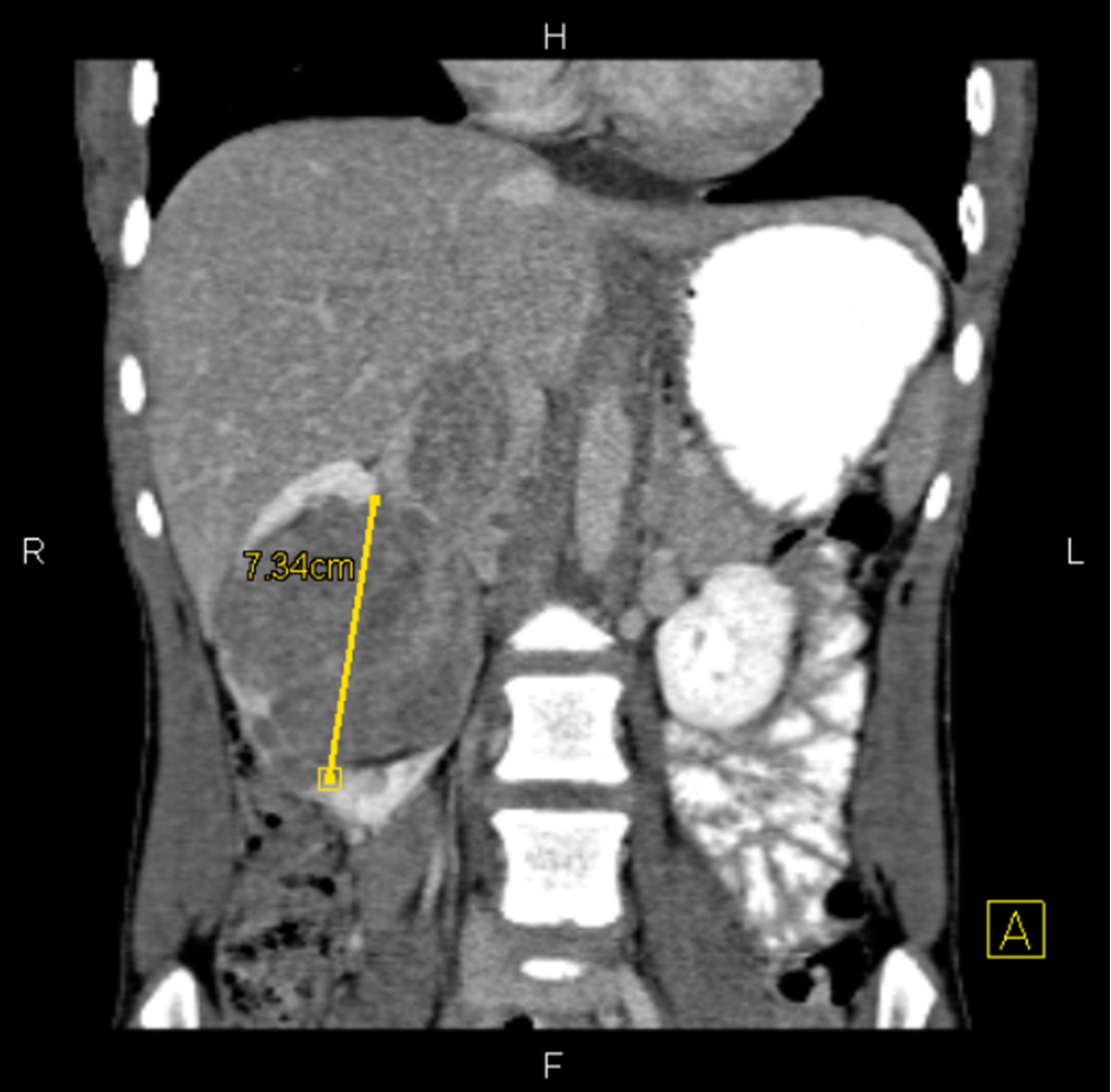
- Heterogeneous, well defined nodule(s) with small cystic areas (Urology 2018;114:e9)
- Cysts may display thickened irregular walls and septa
Radiology images
Prognostic factors
- Typically display indolent behavior
- May rarely be locally aggressive or metastasize
- Lymph node (Histopathology 2018;72:1066)
- Liver (Histopathology 2018;72:588)
- Lung (Histopathology 2018;72:588)
- Bone (Hum Pathol 2018;80:65)
Case reports
- 33 and 65 year old women with loss of function mutations in TSC2 (Am J Surg Pathol 2018;42:911)
- 69 year old woman with metastasis to renal hilar lymph node (Histopathology 2018;72:1066)
Case series:
- 4 cases (3 women, 1 man; ages 27 - 50) including 1 with bone metastases and 1 with locally aggressive disease (Hum Pathol 2018;80:65)
- 6 cases (all women; ages 42 - 66), all with deleterious mutations in either TSC1 or TSC2 (biallelic alterations in 2 cases) (Am J Surg Pathol 2018;42:1166)
- 10 cases (all women; ages 32 - 85) including 1 case with multifocal disease (Am J Surg Pathol 2017;41:1299)
- 10 cases (6 women, 4 men; ages 14 - 35) including 4 cases with multifocal lesions (1 bilateral), 1 case with metastatic disease to the liver and lung and 1 case with history of sickle cell trait (Histopathology 2018;72:588)
- 16 cases, all solitary sporadic neoplasms with indolent behavior occurring in women (ages 31 - 75) (Am J Surg Pathol 2016;40:60)
Treatment
- Surgery is typically curative without progression of disease (solitary, renal confined lesions)
- Possible role for mTOR inhibition in metastatic cases
- Complete clinical response in a case of metastatic TSC2 mutated tumor using first generation rapamycin analog everolimus (Am J Surg Pathol 2018;42:1166)
Gross description
- Frequently solitary lesions (occasionally multifocal, rarely bilateral) (Histopathology 2018;72:588)
- Well delineated with a circumscribed pushing border
- Yellow-tan solid nodules typically interspersed with macrocystic spaces
- Occasional cases may be exclusively solid (Am J Surg Pathol 2017;41:1299)
- < 1.0 - 20.5 cm in greatest diameter (Hum Pathol 2018;80:65)
- Variable hemorrhage with associated necrosis
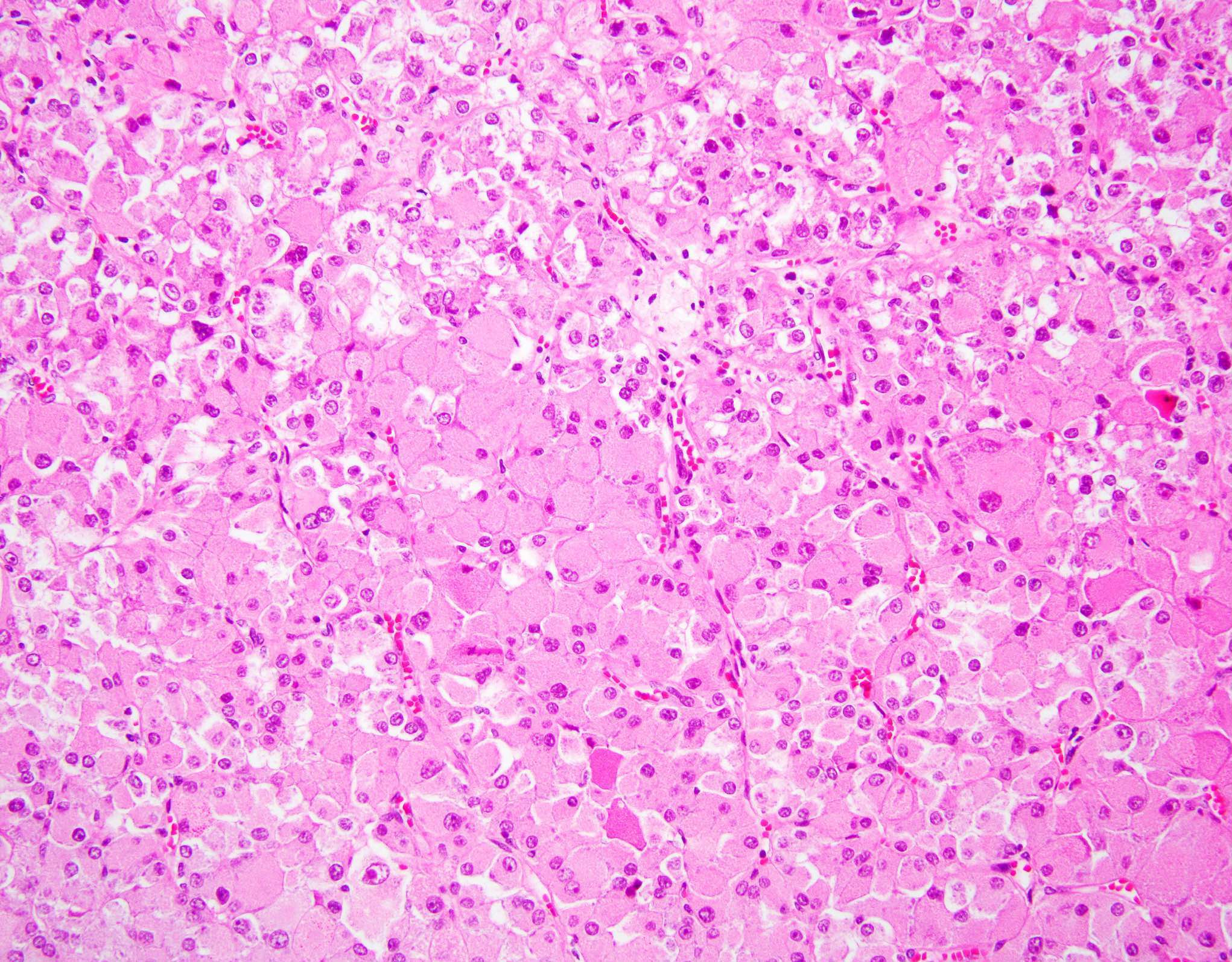
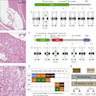
Microscopic (histologic) description
- Unencapsulated
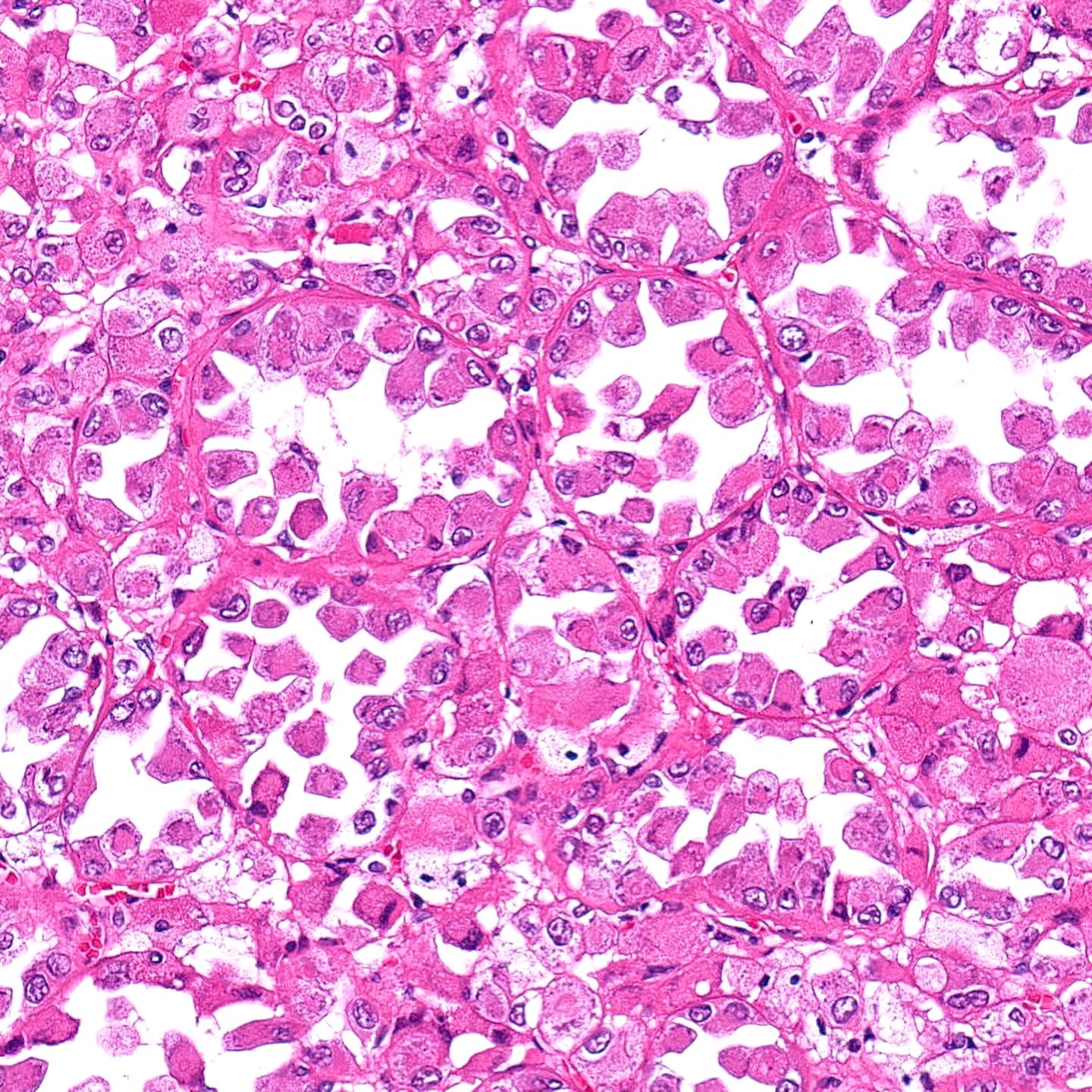
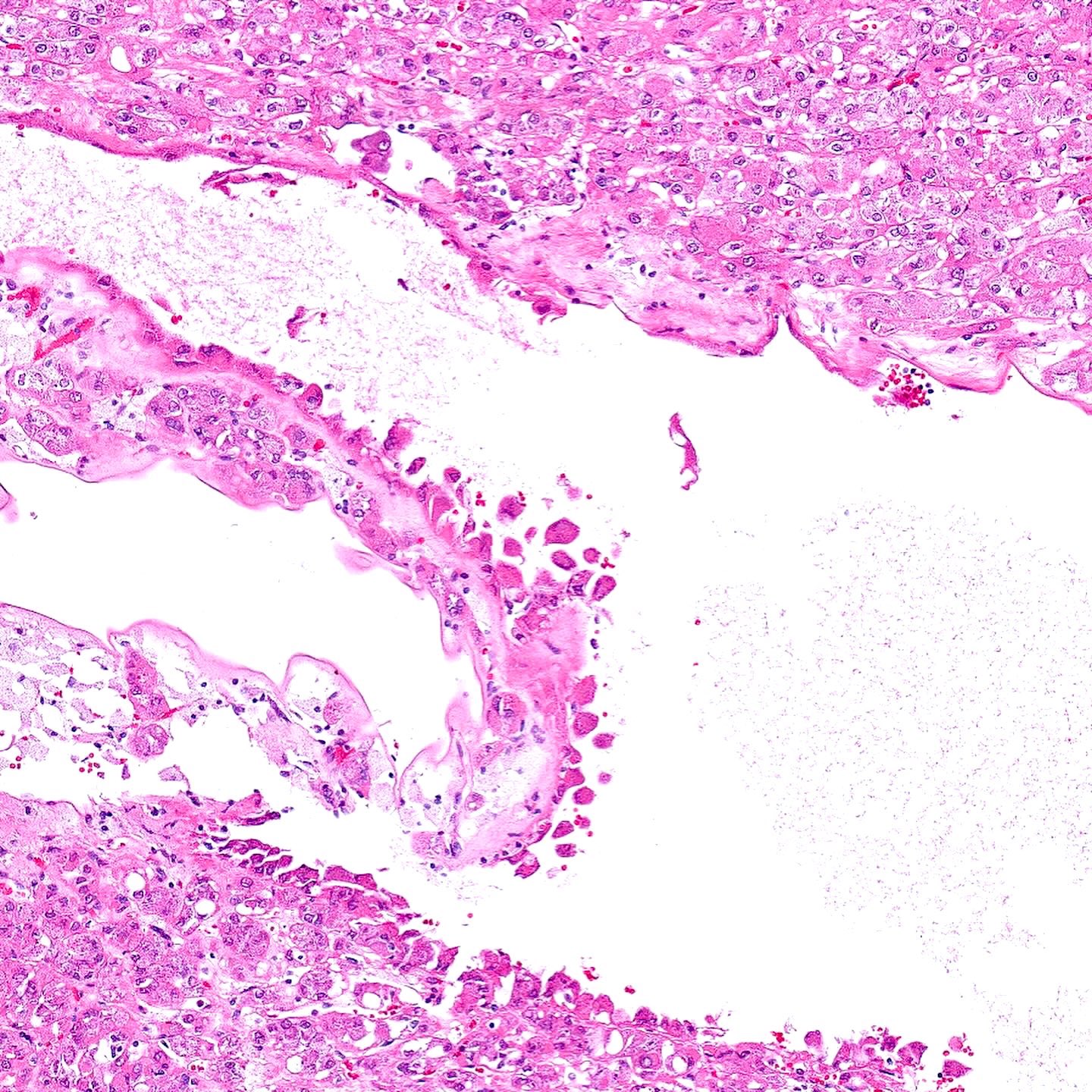
- Solid or compact nested growth of eosinophilic cells admixed with macroscopic cysts or microscopic tubules / cysts (cysts may be focal to absent) (Am J Surg Pathol 2016;40:60)
- Cysts typically lined by a single hobnail layer of neoplastic cells that are often multinucleated
- May display papillary architecture
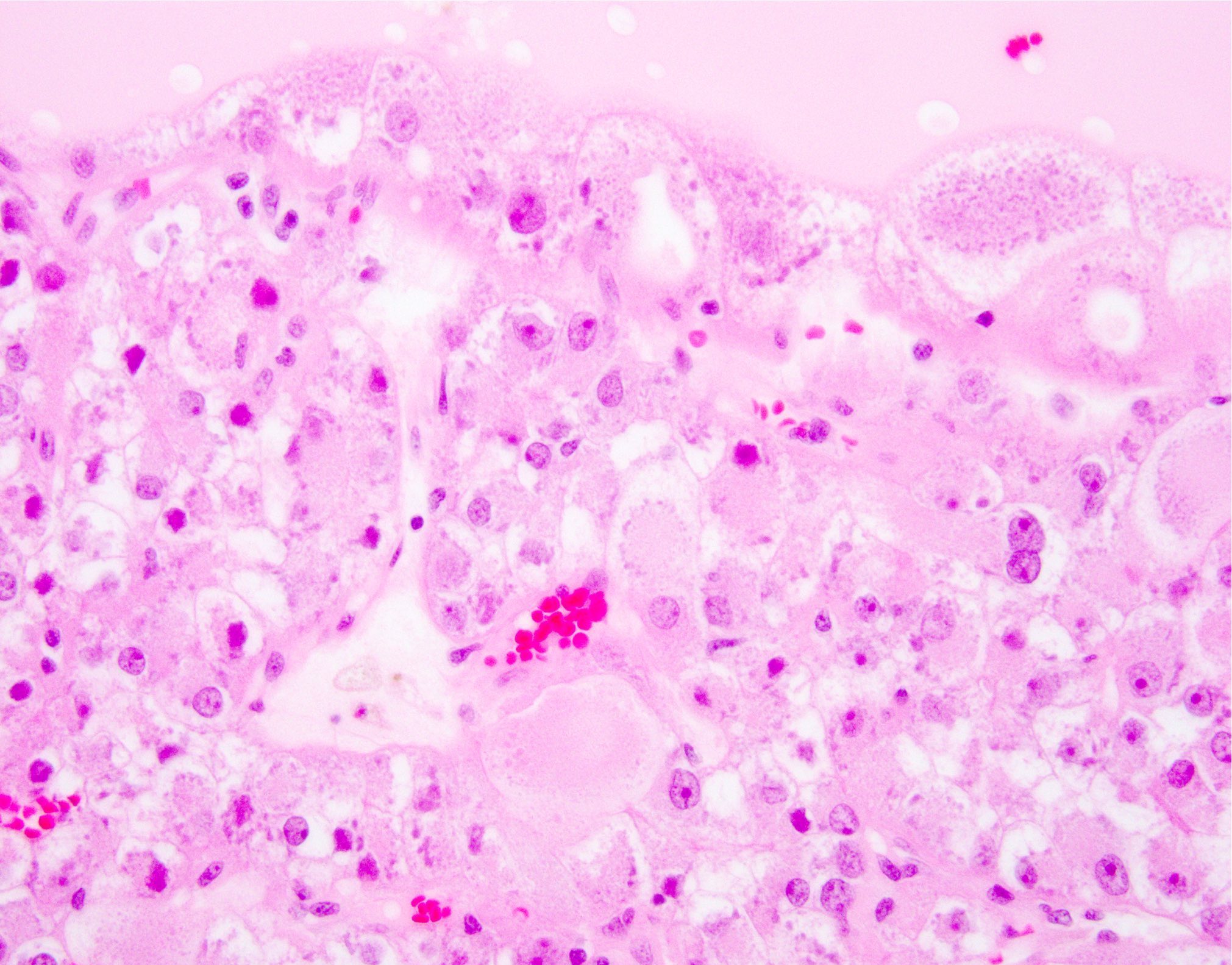
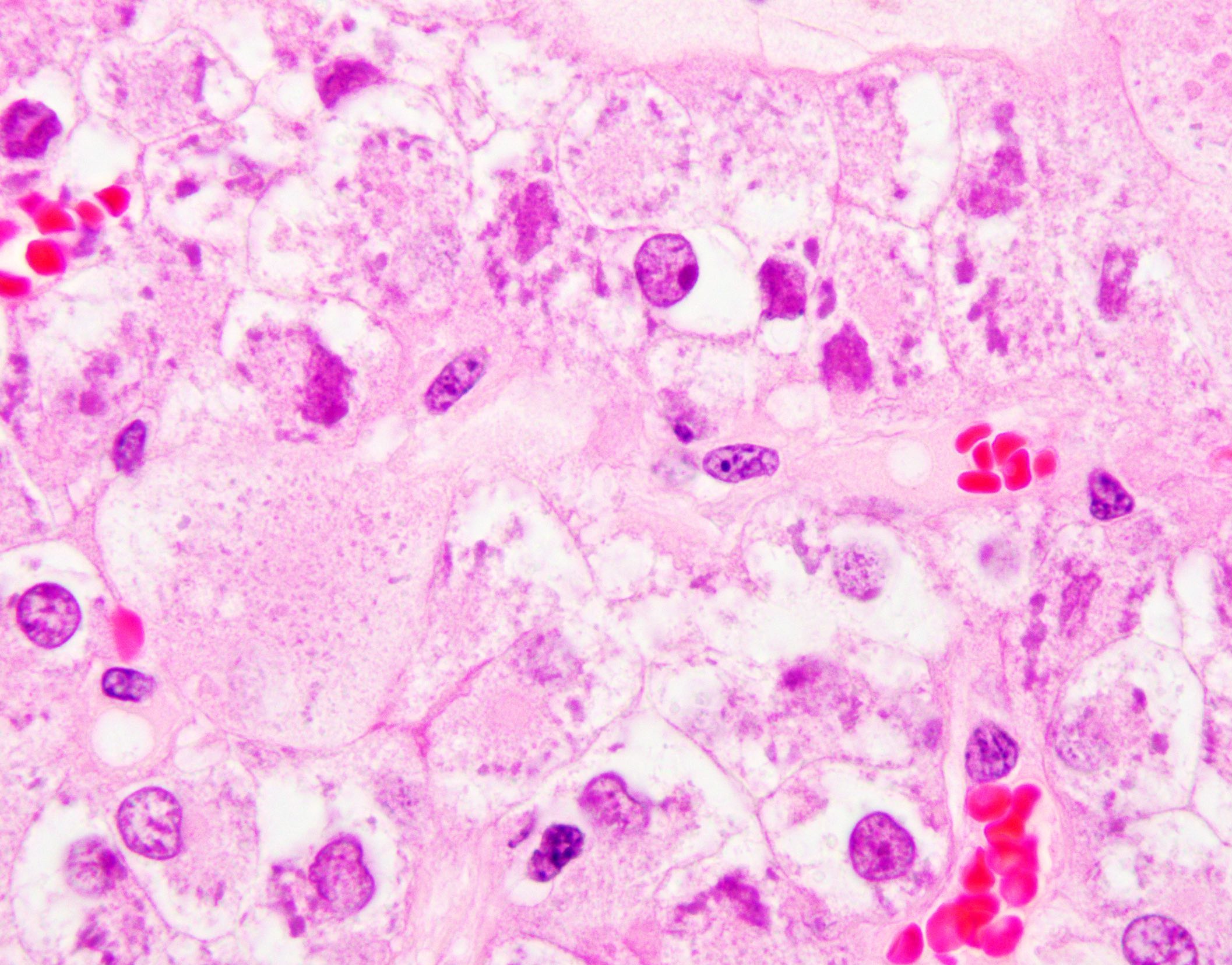
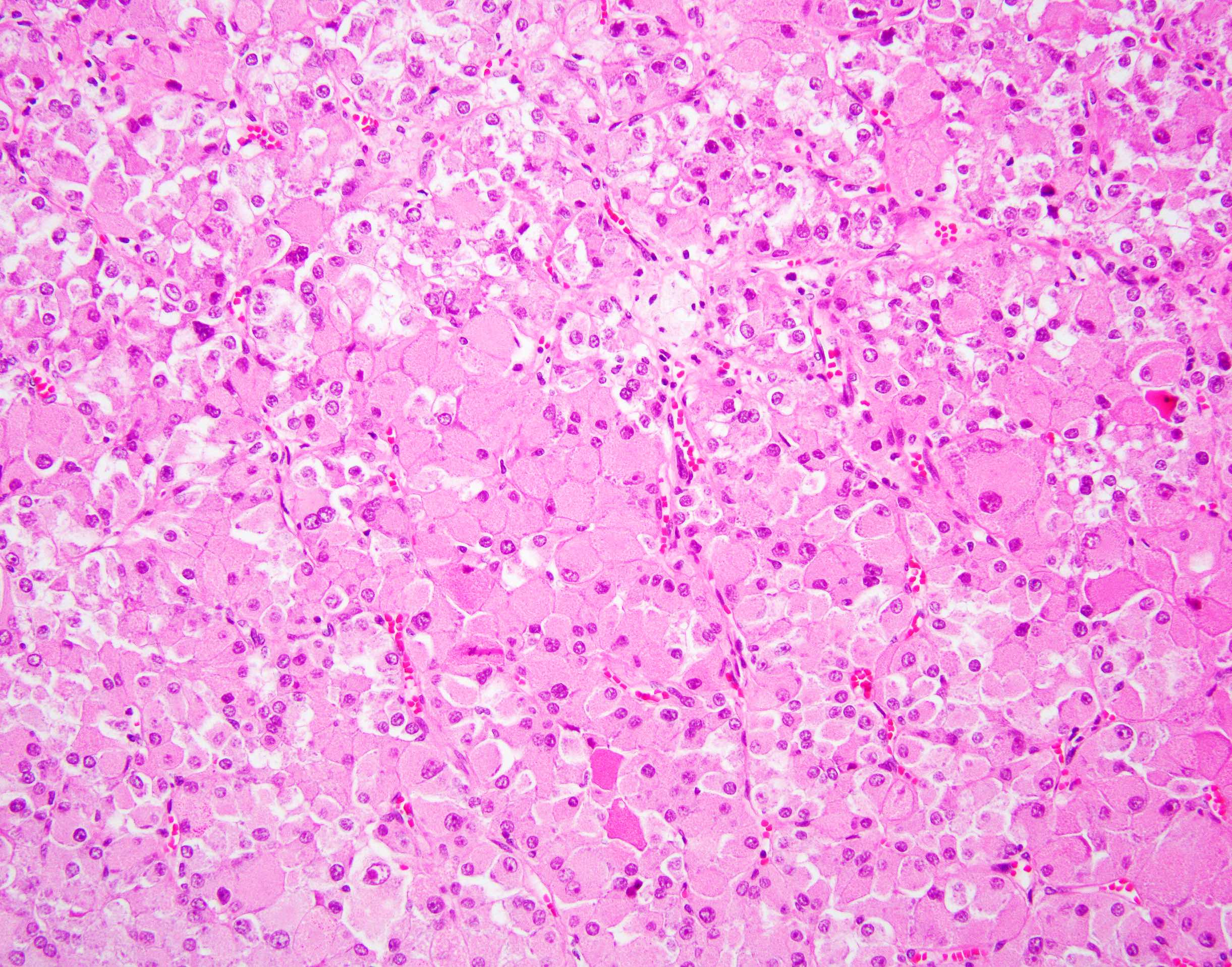
- Voluminous granular eosinophilic cytoplasm, sometimes condensed centrally with a surrounding rim or more clear or flocculent cytoplasm (solid foci may have less voluminous cytoplasm)
- Finely granular to coarse basophilic intracytoplasmic stippling / inclusions (most cases)
- Densely eosinophilic to purple cytoplasmic globules surrounded by a delicate clear rim, reminiscent of leishmaniasis
- Round to oval nuclei with mild pleomorphism and variably prominent nucleoli
- Scattered binucleation / multinucleation
- Cytoplasmic vacuolization (either macrovesicular or microvesicular) may give areas a clear cell appearance
- Foamy macrophages (common)
- Calcifications or osseous metaplasia (rare) (Hum Pathol 2018;80:65)
Microscopic (histologic) images
Positive stains
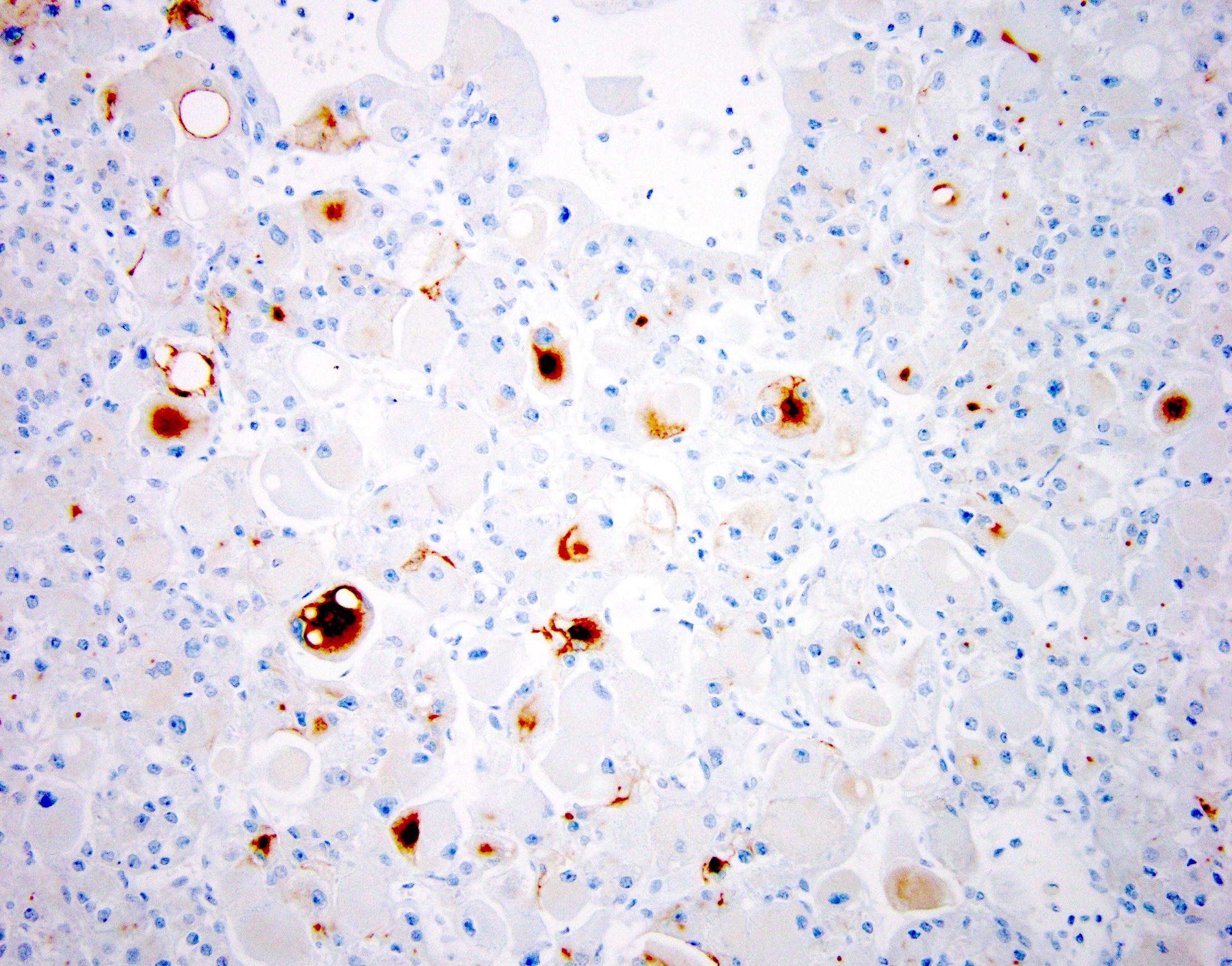
- PAX8 (strong, nuclear, diffuse)
- CK20 (74%, diffuse to patchy but may be focal) (Am J Surg Pathol 2017;41:1299)
- AMACR (84%, patchy to focal) (Am J Surg Pathol 2017;41:1299)
- CD10 (79%) (Am J Surg Pathol 2017;41:1299)
- SDHB (retained cytoplasmic expression)
- Fumarate hydratase (intact)
- Vimentin (90%) (Am J Surg Pathol 2017;41:1299)
- Cathepsin K (variable) (Am J Surg Pathol 2018;42:1166, Hum Pathol 2018;80:65)
- MelanA (variable) (Hum Pathol 2018;80:65)
Negative stains
- CK7 (may be focal in 31%) (Am J Surg Pathol 2017;41:1299)
- CD117 (may be focal in 5%) (Am J Surg Pathol 2017;41:1299)
- CAIX (no membranous staining)
- HMB45 (may show scattered positivity) (Hum Pathol 2018;80:65)
- TFE3
Electron microscopy description
- Abundant rough endoplasmic reticulum, accompanied by granular material (Am J Surg Pathol 2016;40:60)
Molecular / cytogenetics description
- Frequent somatic loss of function mutations in TSC1 (9q34.13) or TSC2 (16p13) (Eur Urol 2018;74:483, Am J Surg Pathol 2018;42:911, Am J Surg Pathol 2018;42:1166)
- "Second hit" genetic alterations (e.g. loss of heterozygosity or > 1 deleterious mutation) in the same gene (TSC1 or TSC2) are sometimes seen (Eur Urol 2018;74:483, Am J Surg Pathol 2018;42:911, Am J Surg Pathol 2018;42:1166)
- Copy number gain
- 16p13.3 - q23.1 (33 - 67%, including TSC2 locus in 42%) (Am J Surg Pathol 2017;41:1299)
- 7p21.2 - q36.2 (42 - 50%) (Am J Surg Pathol 2017;41:1299)
- Copy number loss
- TSC1 (33%) (Am J Surg Pathol 2017;41:1299)
- Loss of heterozygosity
- 16p11.2 - 1 (75%) (Am J Surg Pathol 2017;41:1299)
- Xq11.1 - 13.1 (75%) (Am J Surg Pathol 2017;41:1299)
Differential diagnosis
- Tuberous sclerosis complex (TSC) associated RCC:
- Clinical diagnosis of tuberous sclerosis complex
- Highly penetrant autosomal dominant genetic disorder with variable expressivity
- Infantile spasms or seizures (most frequent clinical manifestation, Arch Dis Child 2011;96:1020)
- Updated 2012 clinical diagnostic criteria for TSC (Pediatr Neurol 2013;49:243)
- Major features: 1) ≥ 3 angiofibromas or fibrous cephalic plaque; 2) ≥ 2 ungual fibromas; 3) ≥ 3 hypomelanotic macules; 4) shagreen patch; 5) multiple retinal hamartomas; 6) cortical dysplasias including tubers and cerebral white matter radial migration lines; 7) subependymal nodules; 8) subependymal giant cell tumor; 9) cardiac rhabdomyoma; 10) lymphangioleiomyomatosis; 11) ≥ 2 angiomyolipomas
- Minor features: 1) "confetti" skin lesions; 2) ≥ 3 dental enamel pits; 3) ≥ 2 intraoral fibromas; 4) retinal achromic patch; 5) multiple renal cysts; 6) nonrenal hamartomas
- Definite diagnosis: 2 major features or 1 major feature with ≥ 2 minor features
- Possible diagnosis: either 1 major feature or ≥ 2 minor features
- Updated 2012 genetic diagnostic criteria for TSC (Pediatr Neurol 2013;49:243)
- Either a TSC1 or TSC2 pathogenic mutation (i.e. deleterious or loss of function) in DNA from normal tissue (definite diagnosis)
- De novo mutations (69 - 83%, mostly TSC2) (Sci Rep 2017;7:16697, Eur J Pediatr 2002;161:393, Genet Med 2007;9:88)
- Renal cell carcinoma in tuberous sclerosis complex (2 - 4% of patients, Kidney Int 2006;70:1777)
- TSC2 mutations > TSC1 mutations
- May coexist with angiomyolipoma (most common tuberous sclerosis complex renal neoplasm)
- Bilateral or multifocal (± heterogeneous morphologies, synchronous or metachronous)
- Concurrent renal cysts (common, background kidney)
- Lined by cells with prominent eosinophilic cytoplasm and round nuclei with prominent nucleoli
- Prominent cyst formation
- May indicate autosomal dominant polycystic kidney disease
- Corresponds to large deletion extending from TSC2 into adjacent PKD1 gene on chromosome 16p (may require alternative molecular testing for detection)
- Various histologic types
- Granular eosinophilic macrocystic morphology (11%): morphologically similar to sporadic eosinophilic, solid and cystic RCC (Am J Surg Pathol 2014;38:1457, Int J Surg Pathol 2010;18:409)
- Hybrid oncocytic / chromophobe tumor (HOCT) (chromophobe-like or oncocytoma-like) (59%) (Am J Surg Pathol 2014;38:1457, Am J Surg Pathol 2014;38:895)
- Renal angiomyoadenomatous tumor (RAT-like), RCC with angioleiomyoma-like stroma or RCC with a tubulopapillary architecture and clear cytoplasm separated by smooth muscle stroma (30%, Am J Surg Pathol 2014;38:1457, J Pathol Clin Res 2018;4:167)
- Clear cell RCC
- Clinical diagnosis of tuberous sclerosis complex
- RCC postneuroblastoma:
- Prior history of neuroblastoma
- Various subtypes
- Oncocytoid: morphologically similar to sporadic eosinophilic, solid and cystic RCC (Am J Surg Pathol 2016;40:989, Am J Surg Pathol 2018;42:1166, Am J Surg Pathol 1999;23:772)
- Hybrid oncocytic chromophobe tumor (HOCT)
- Clear cell RCC
- Papillary RCC-like
- MiT family translocation RCC
- TSC2 or MTOR mutated sporadic RCC with eosinophilic and vacuolated cytoplasm (Am J Surg Pathol 2019;43:121):
- 7 reported cases (Am J Surg Pathol 2019;43:121)
- Well circumscribed, unencapsulated solitary renal mass
- M = F
- Mean age at presentation, 54 years
- Nested growth pattern with dispersed single cells, extreme vacuolization and thick walled vessels
- CK7- / CK20-
- Cathepsin K+ in most cases
- Inactivating mutations of TSC2 or activating mutations of MTOR
- May be related to eosinophilic, solid and cystic RCC
- 7 reported cases (Am J Surg Pathol 2019;43:121)
- High grade oncocytic tumor (HOT) (Virchows Arch 2018;473:725):
- 14 reported cases (Virchows Arch 2018;473:725)
- F > M
- Median age, 50 years (range, 25 - 73)
- Well circumscribed and unencapsulated
- Predominantly nested growth pattern in a background of loose fibromatous oncocytoma-like stroma
- Entrapped nonneoplastic renal tubules and prominent thick walled vessels at the periphery
- Voluminous, variably granular cytoplasm with large cytoplasmic vacuoles or inclusions of flocculent eosinophilic material
- Distinct cell membranes
- Rounded nuclear contours with conspicuous nucleoli
- CD117+ in most cases
- CK7 and CK20 negative to focally positive
- Cathepsin K+ / CD10+ in most cases
- Molecular characterization limited with no sequencing data available; possibly related to TSC2 or MTOR mutated sporadic RCC with eosinophilic and vacuolated cytoplasm (see above)
- 14 reported cases (Virchows Arch 2018;473:725)
- MiT family translocation RCC:
- Epithelioid angiomyolipoma:
- Papillary RCC, solid variant, oncocytic type:
- SDH deficient RCC:
- Chromophobe RCC, eosinophilic type:
- Clear cell RCC, eosinophilic morphology:
Board review style question #1
Board review style answer #1
B. PAX8+ / CK20+ / CD117-. This is an eosinophilic, solid and cystic (ESC) renal cell carcinoma. ESC RCCs are consistently immunoreactive for PAX8, frequently CK20+ (74% of cases, may be focal) and usually CK7- / CD117- (may be focal but never diffuse). Epithelioid angiomyolipomas, on the other hand, are typically negative for PAX8 and CK20 and positive for CD117. Both entities would be negative for strong nuclear TFE3 and show intact SDHB expression.
Comment Here
Reference: Eosinophilic, solid and cystic renal cell carcinoma
Comment Here
Reference: Eosinophilic, solid and cystic renal cell carcinoma
Board review style question #2
Eosinophilic, solid and cystic (ESC) renal cell carcinoma is most frequently associated with genetic alterations in which gene(s)?
- FLCN
- SDHB
- TSC1 / 2
- VHL
Board review style answer #2