Table of Contents
Definition / general | Essential features | Terminology | ICD coding | Epidemiology | Sites | Birt-Hogg-Dubé syndrome | Clinical features | Radiology description | Prognostic factors | Case reports | Treatment | Gross description | Gross images | Microscopic (histologic) description | Microscopic (histologic) images | Cytology description | Cytology images | Positive stains | Negative stains | IHC panels | Electron microscopy description | Electron microscopy images | Molecular / cytogenetics description | Differential diagnosis | Board review style question #1 | Board review style answer #1 | Board review style question #2 | Board review style answer #2Cite this page: Tretiakova M. Chromophobe. PathologyOutlines.com website. https://www.pathologyoutlines.com/topic/kidneytumormalignantrccchromo.html. Accessed April 26th, 2024.
Definition / general
- Solid tumor composed of granular pale cells with prominent cell borders, finely reticular cytoplasm, perinuclear halos and wrinkled hyperchromatic nuclei
- First described in 1985 (J Pathol 1988;155:277)
- Cell of origin: intercalated cells of distal convoluted tubules
Essential features
- Solid sheet-like architecture
- Sharply defined cell membranes (plant-like)
- Wrinkled irregular nuclei (raisinoid)
- Perinuclear halos (koilocytic)
Terminology
- Chromophobe renal cell carcinoma (ChRCC), classic variant
ICD coding
- ICD-10: C64 - malignant neoplasm of kidney, except renal pelvis
Epidemiology
- Third most common renal cell carcinoma (RCC) subtype; 7% of adult renal epithelial tumors (Arch Pathol Lab Med 2019;143:1455)
- Majority are sporadic and incidental, no gender preference
- Mean age 58 years (Cancer 2004;100:1406)
Sites
- Solitary kidney mass
- Most commonly in renal cortex
Birt-Hogg-Dubé syndrome
- Multiple tumors (mean 5.3); mean age 51 years at first renal tumor diagnosis
- Bilateral multifocal ChRCC, oncocytomas or hybrid oncocytic chromophobe tumor (HOCT), also may have oncocytosis (Am J Surg Pathol 2002;26:1542)
- Autosomal dominant syndrome: small dome shaped papular fibrofolliculomas of face, neck and upper trunk, renal tumors, lung cysts and spontaneous pneumothorax
- Mutations in the folliculin gene (FLCN) at 17p11.2, leading to premature truncation and loss of function of the folliculin protein (Cancer Cell 2002;2:157, Hum Mutat 2010;31:E1043)
Clinical features
- Most are organ confined T1 - T2, N0, M0 and have good prognosis (Cancer 2004;100:1406)
- Recurrence or metastatic disease developing in 4 - 10% cases (Eur J Cancer 2017;80:55)
- 5 and 10 year cancer specific survival are 93% and 88.9%, respectively (BJU Int 2012;110:76)
Radiology description
- Usually large, well circumscribed, hypovascular mass with relatively homogeneous contrast enhancement; may show central scar
Prognostic factors
- Poor prognostic factors
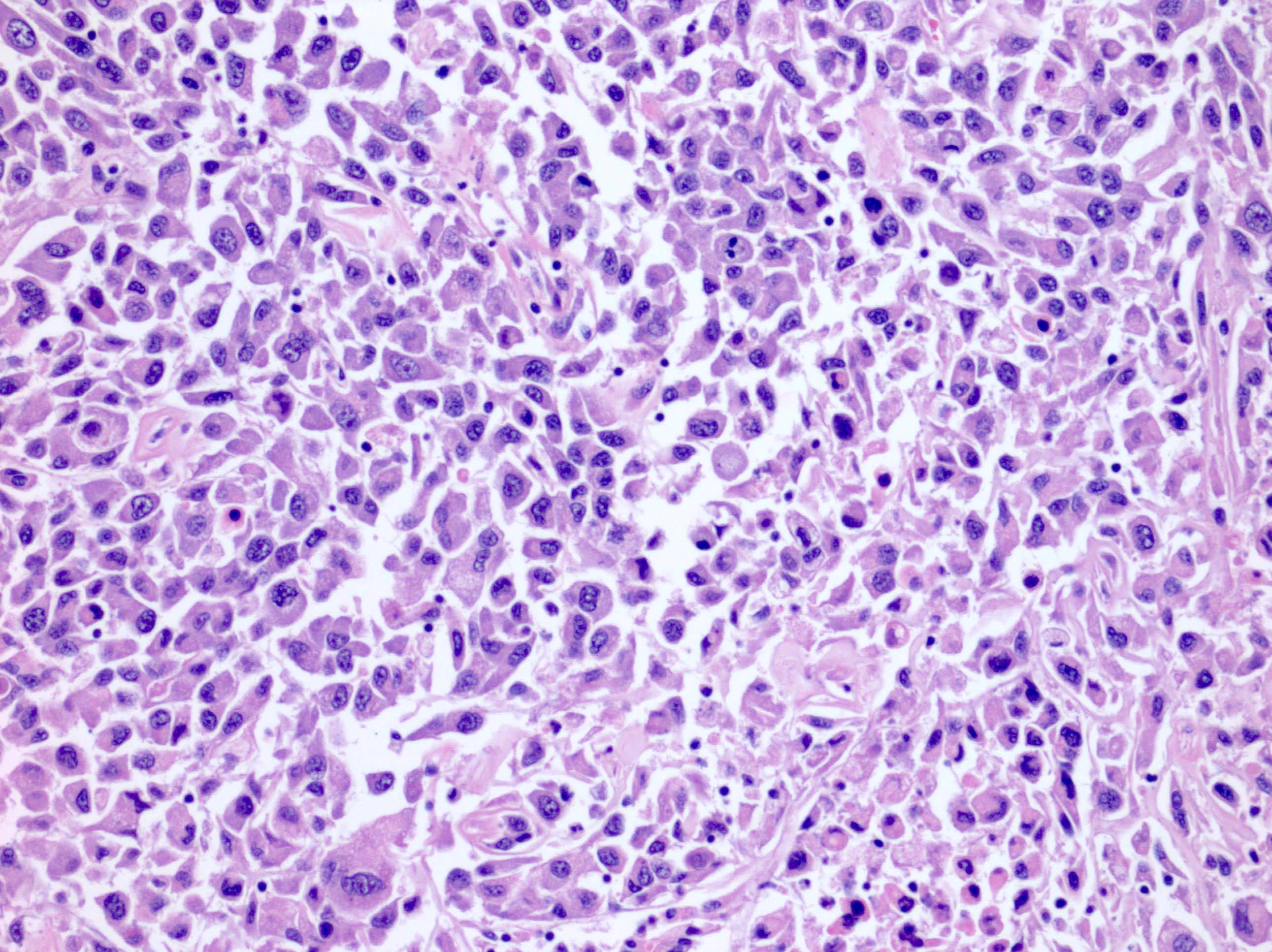
- Sarcomatoid change (~5%), microscopic necrosis, vascular invasion (Am J Surg Pathol 2008;32:1822, Am J Surg Pathol 2011;35:962)
- Tumor size (> 7 cm)
- Higher clinical T category and pathologic TNM stage
- Male gender (BJU Int 2012;110:76)
- Tumor grading is not prognostically relevant and not recommended (J Clin Pharm Ther 2019;44:268)
Case reports
- 41 year old woman with significant response to nivolumab for sarcomatoid metastatic ChRCC (BMC Urol 2018;18:26)
- 46 year old man with de novo ChRCC in the graft 3 decades after renal transplantation (Saudi J Kidney Dis Transpl 2020;31:271)
- 61 year old man with sarcomatoid heterologous component (Iran J Pathol 2020;15:57)
- 65 year old man with retrograde venous invasion and gain of chromosome 21 (Int J Surg Pathol 2018;26:536)
- 70 year old man with neuroendocrine differentiation (Urol Ann 2015;7:383)
Treatment
- Surgery, cryoablation and targeted systemic chemotherapy for metastatic disease with antiangiogenic, TK and mTOR inhibitors (Eur J Cancer 2017;80:55)
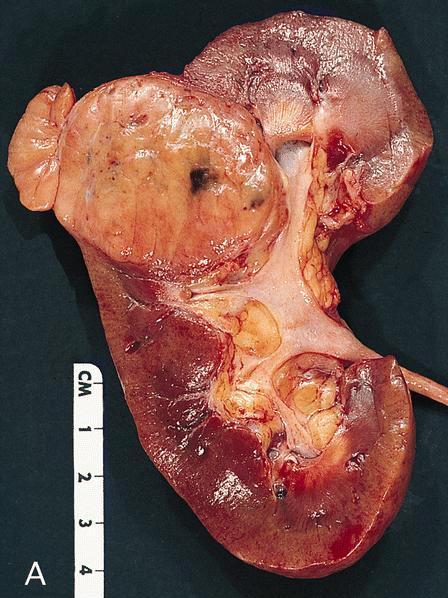
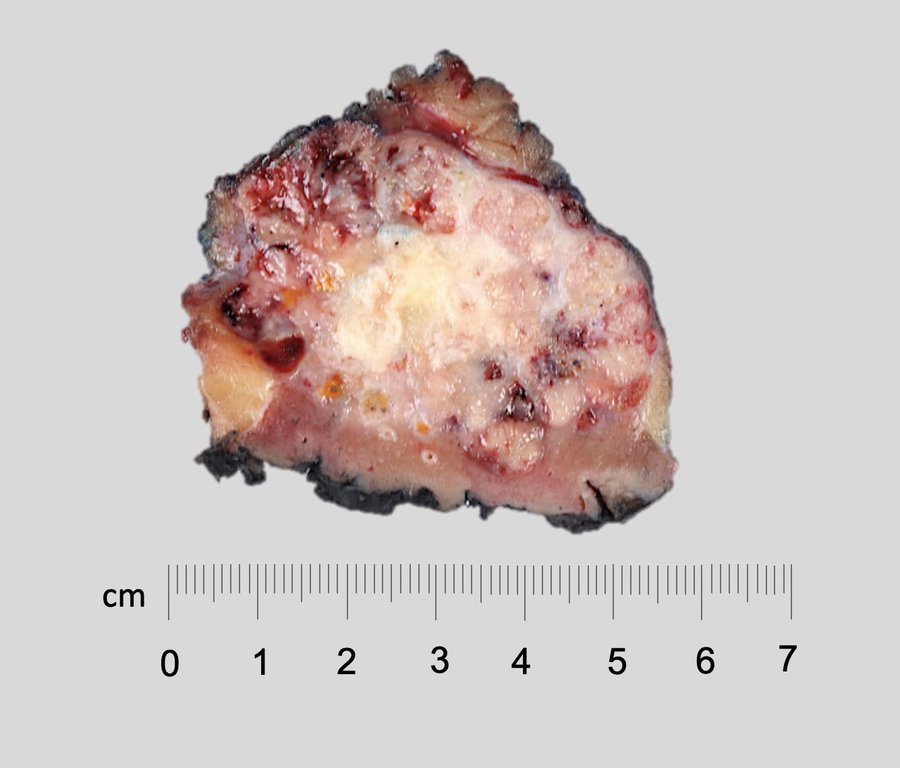
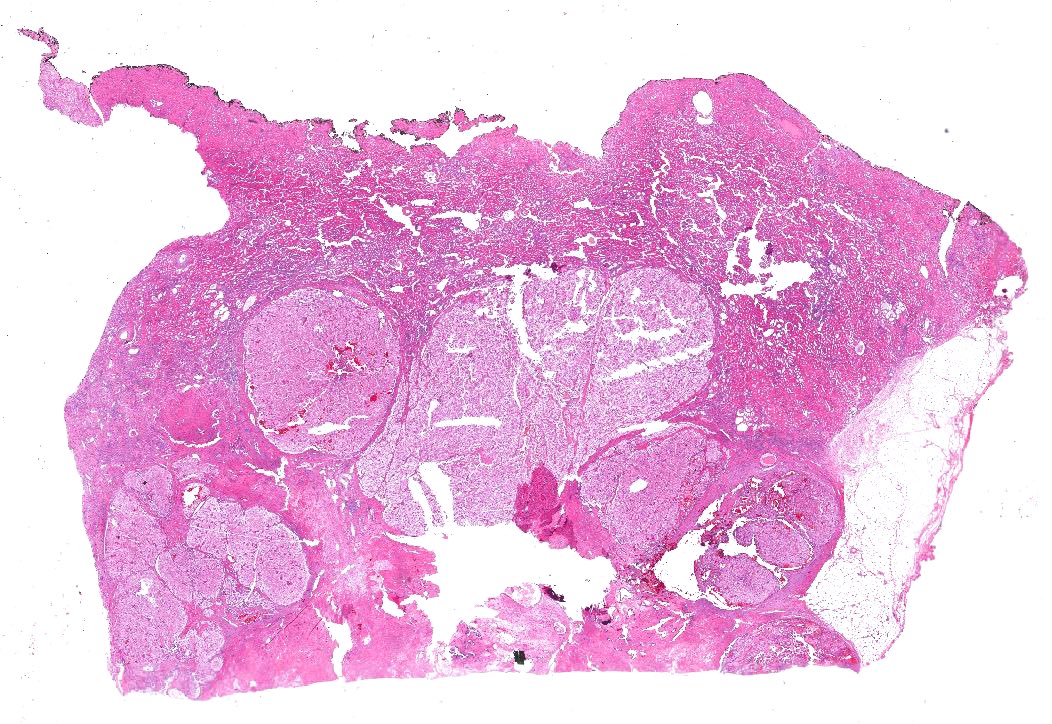
Gross description
- Well circumscribed, unencapsulated, tan to light brown
- Average size 8 cm (BJU Int 2012;110:76)
- Necrosis, hemorrhage and small cysts (25 - 30%)
- Occasionally central scar (~15%); multifocal (10%)
Gross images
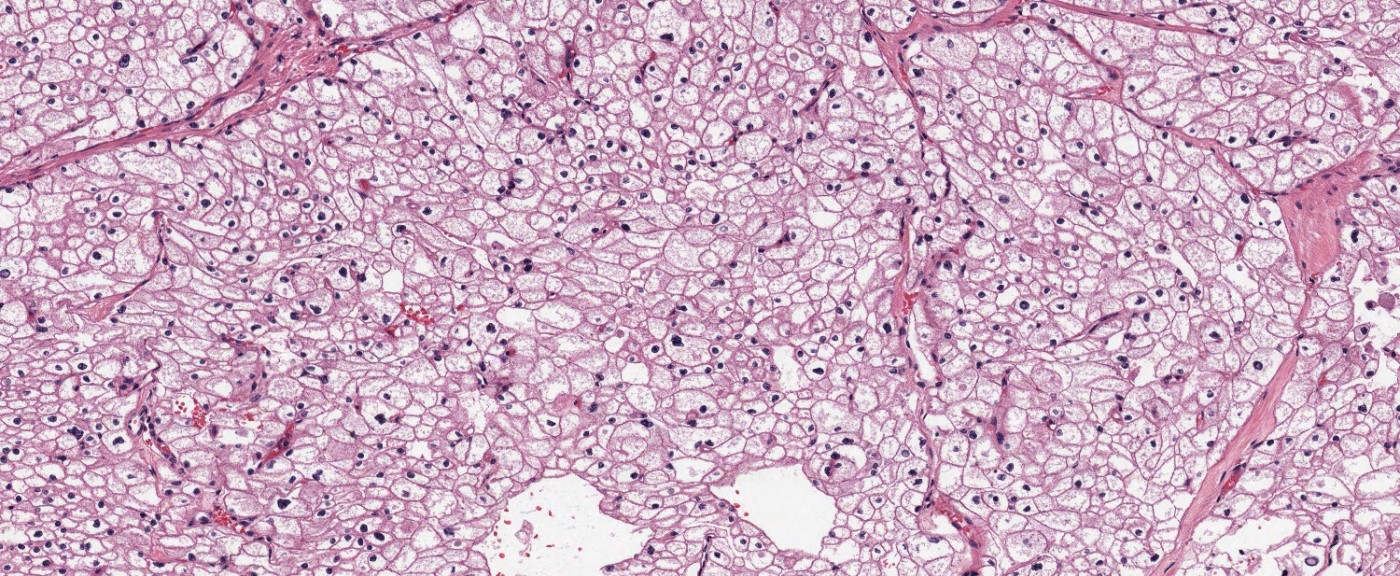
Microscopic (histologic) description
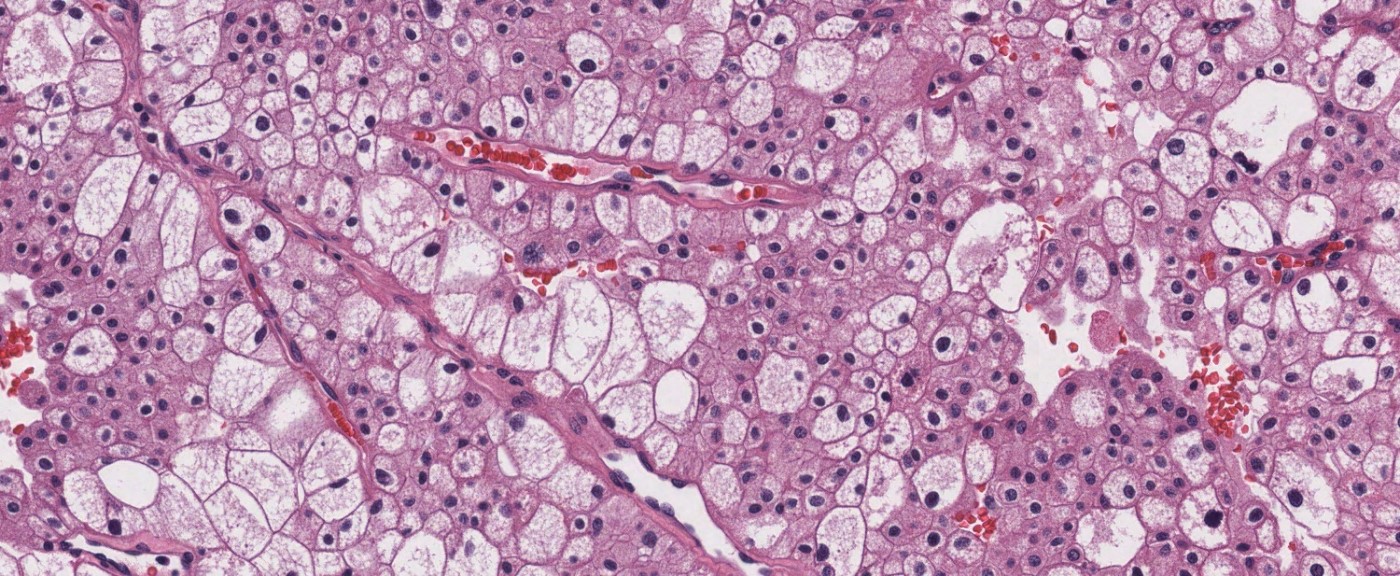
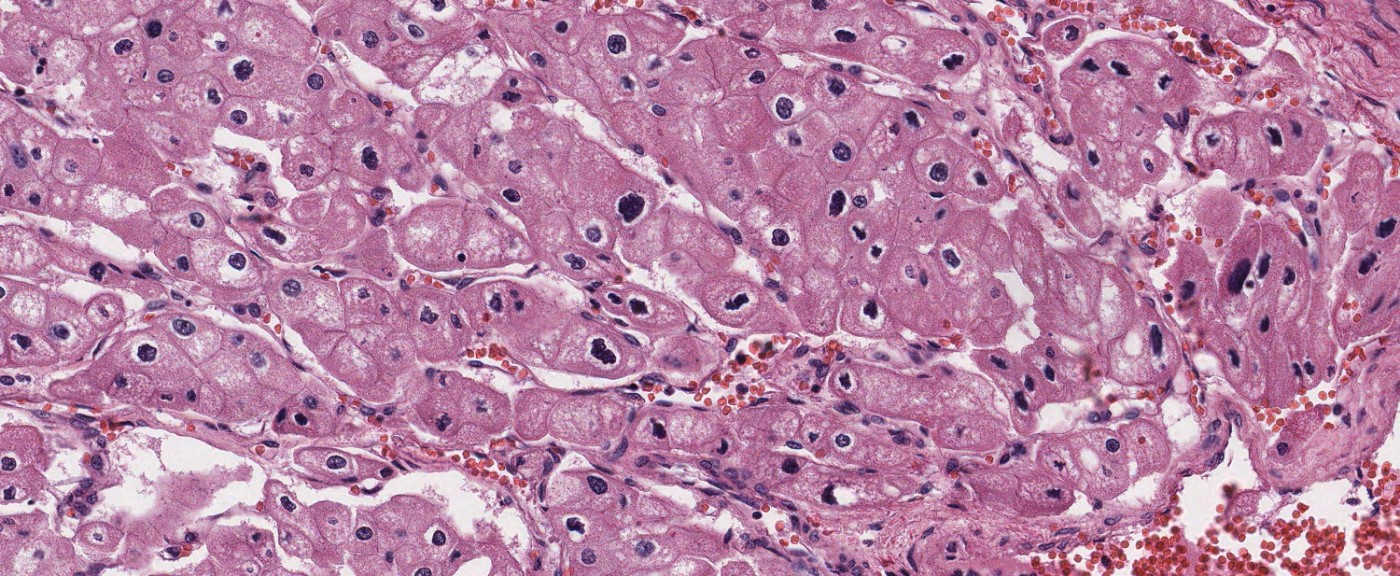
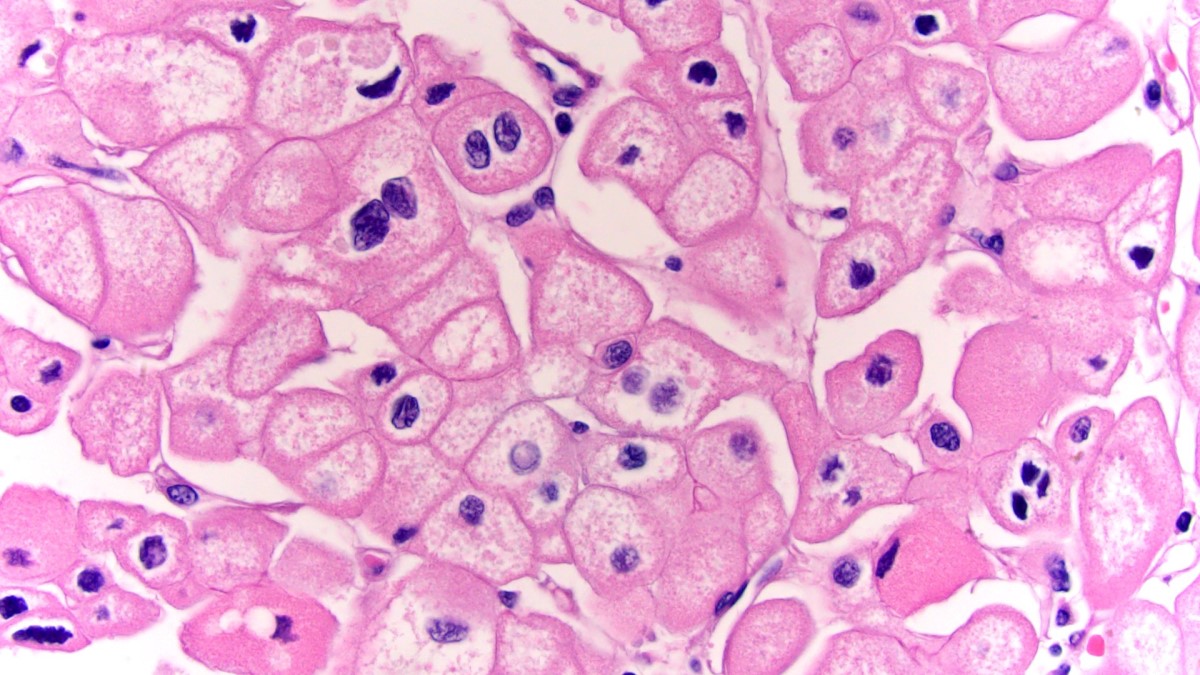
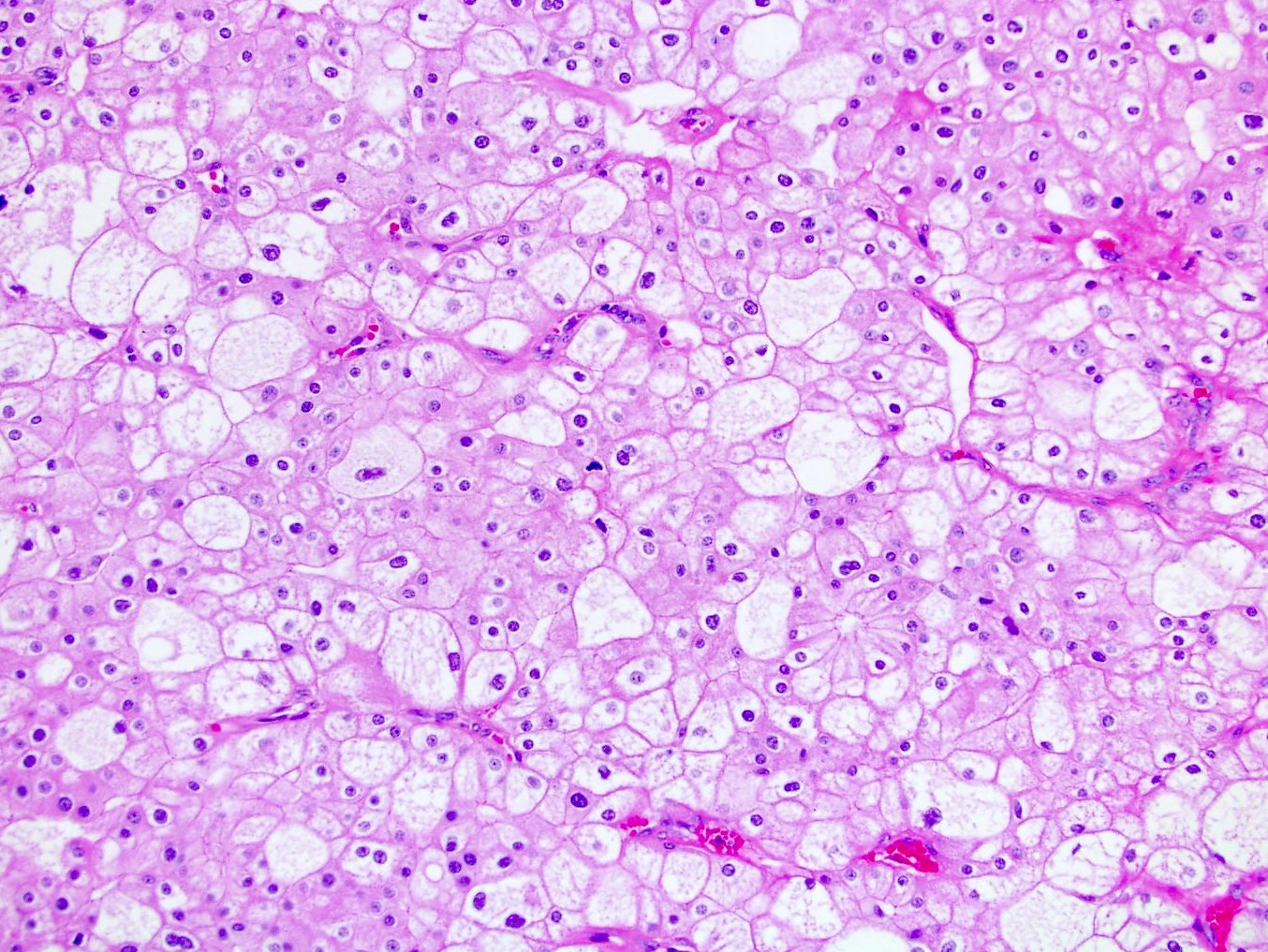
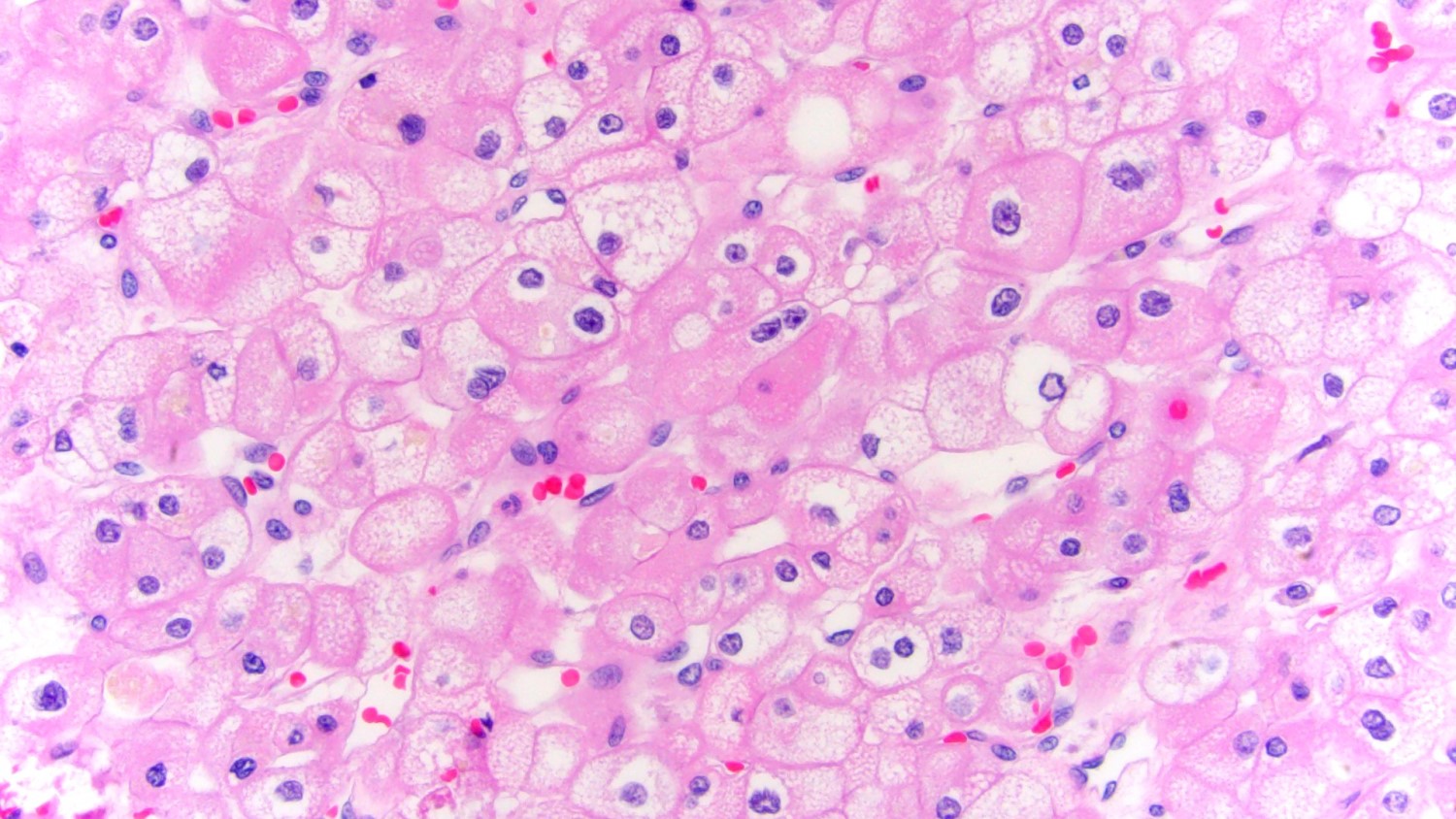
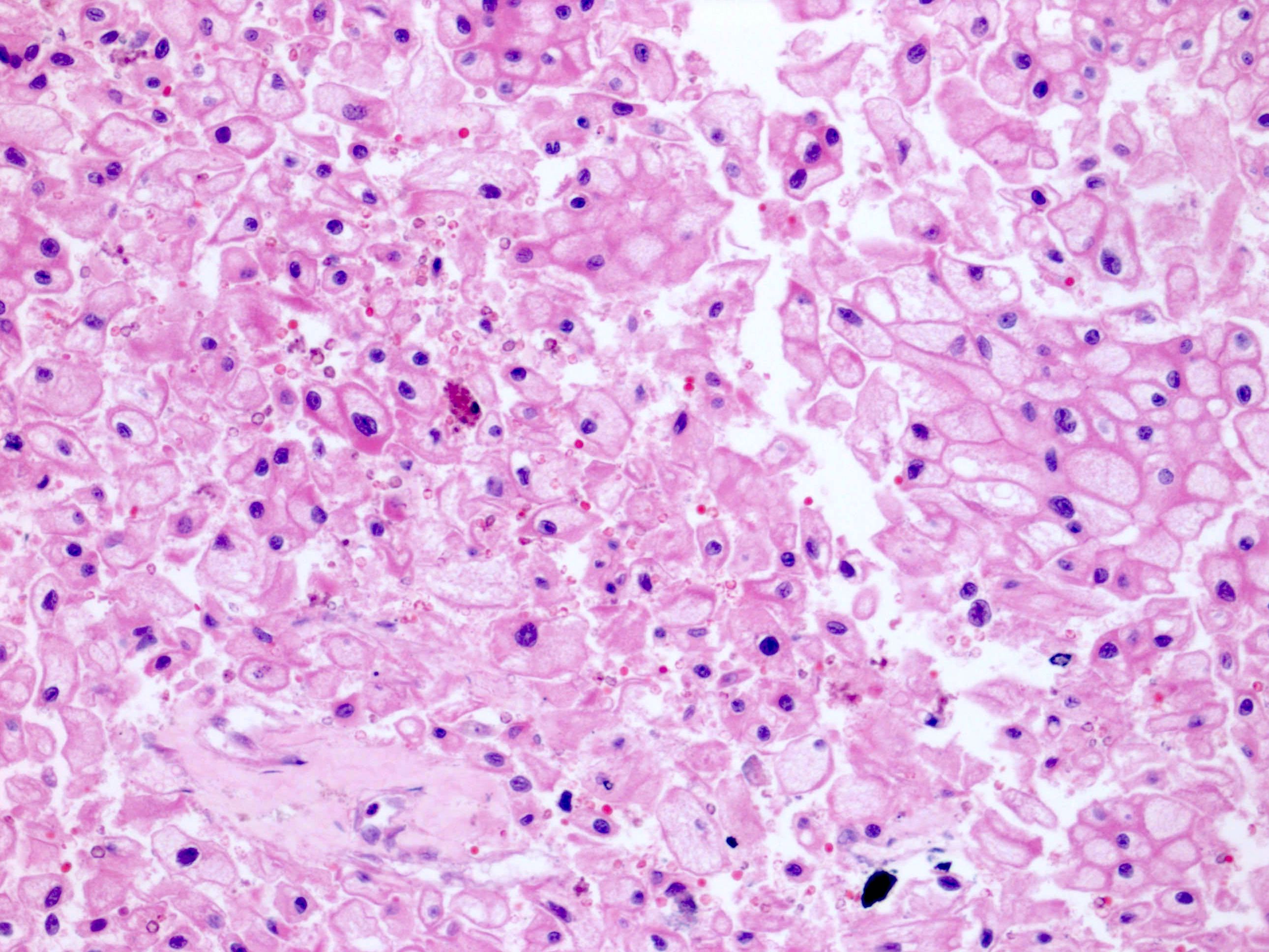
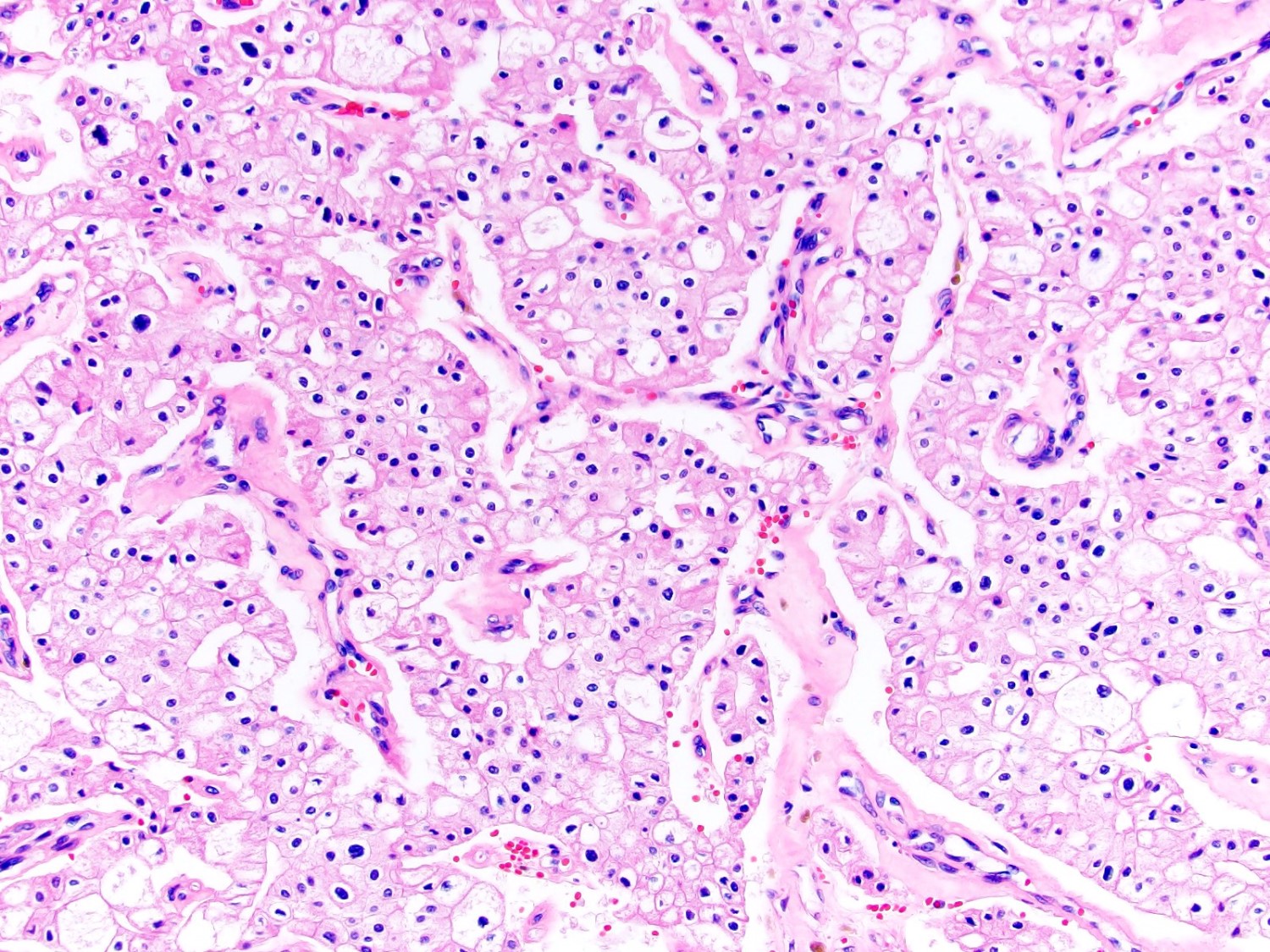
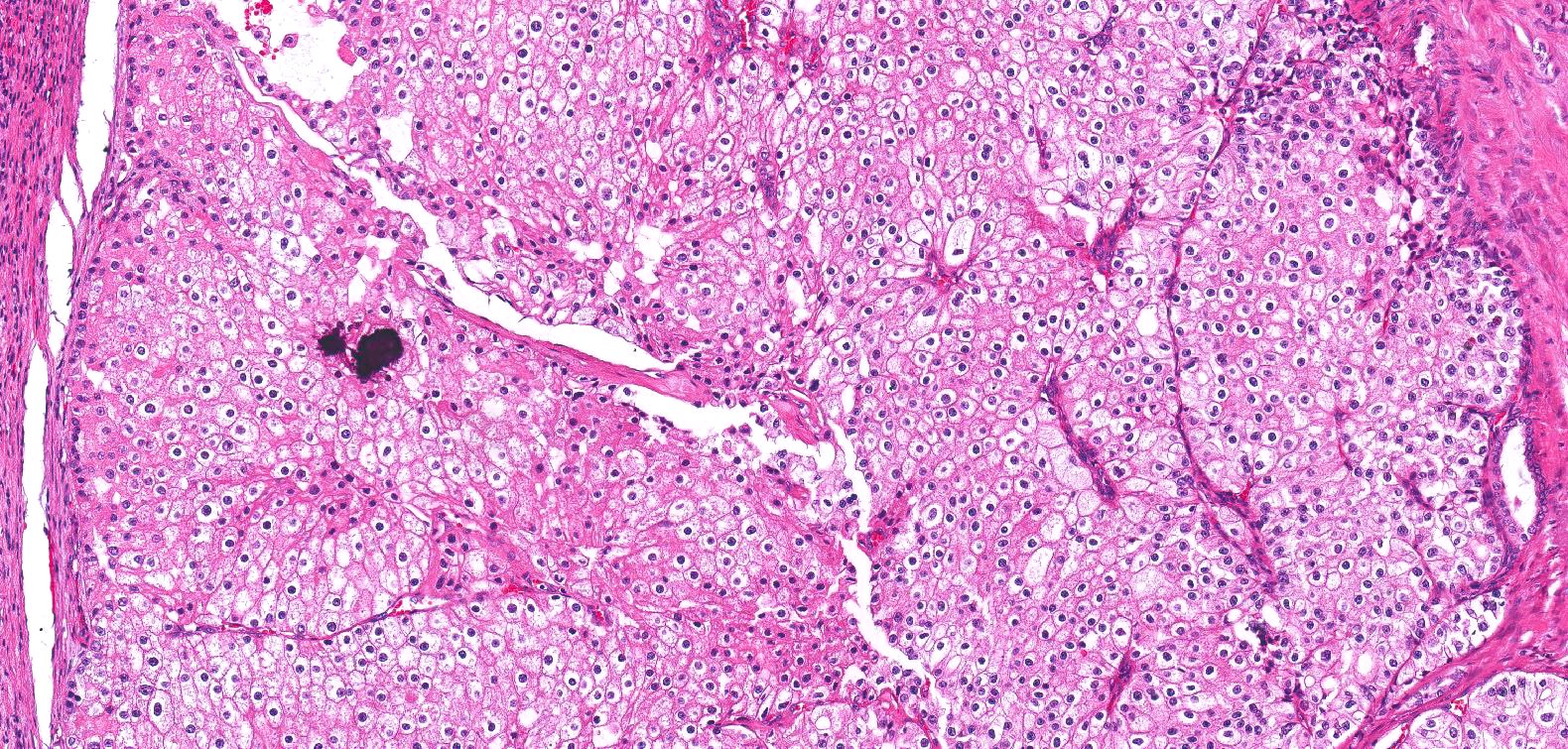
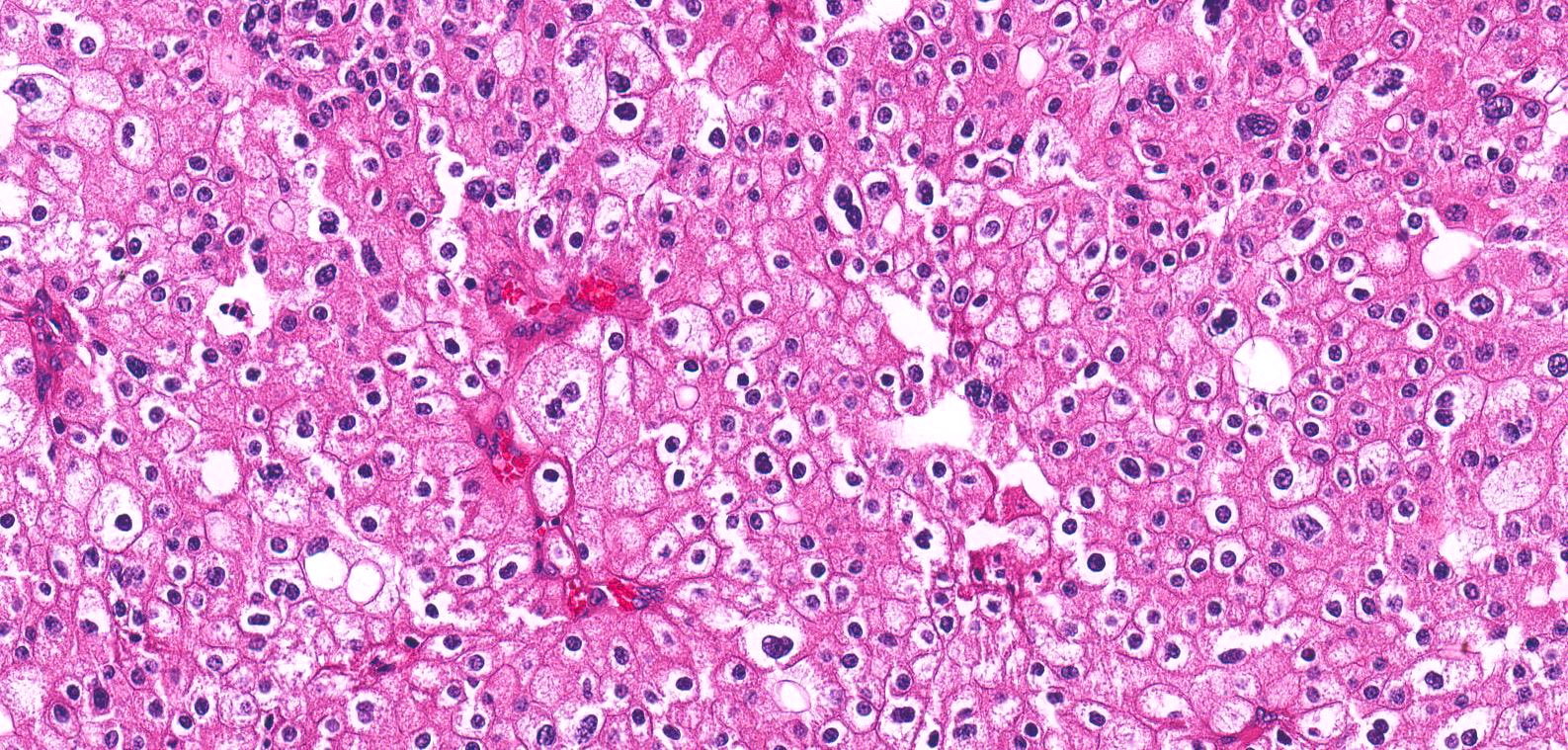
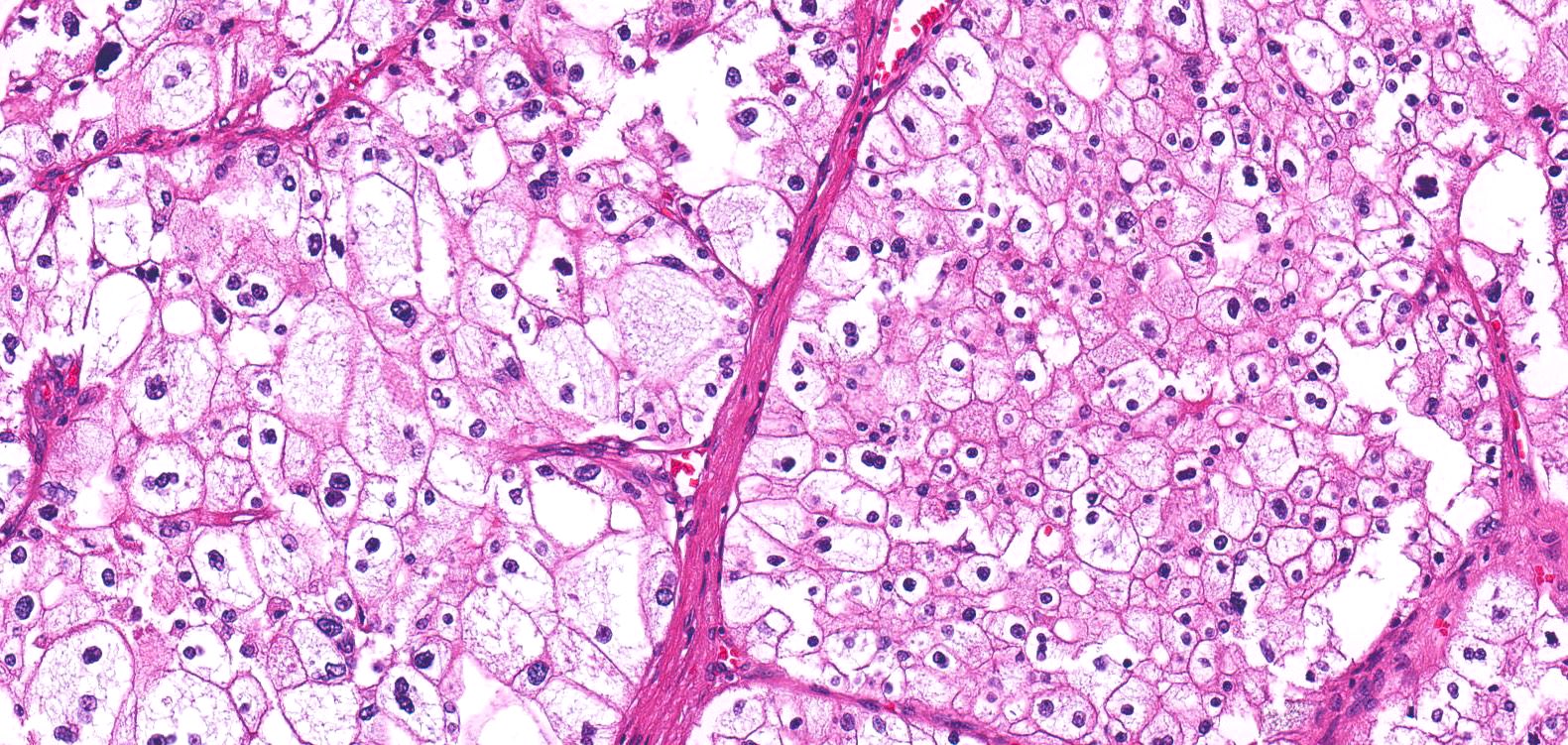
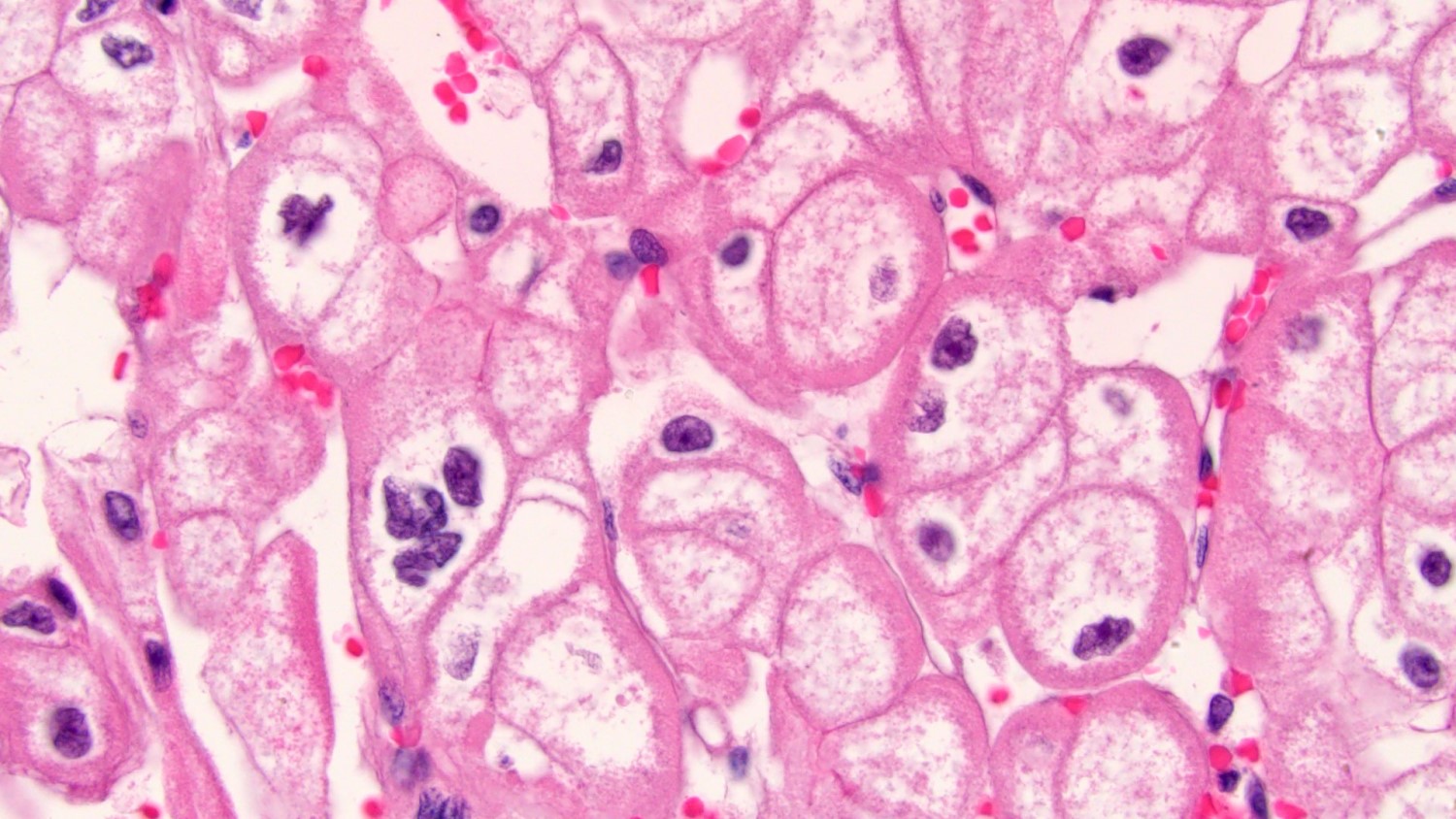
- Typically confluent solid growth with nests, sheets or alveoli / trabeculae composed of pale cells with sharply defined plant-like cell borders (vegetable cells)
- 2 types of tumor cells:
- Type 1: large, polygonal cells with hard cell border; abundant cytoplasm with reticular pattern
- Type 2: smaller cells with finely granular eosinophilic cytoplasm (predominant in eosinophilic variant)
- Nuclei are irregular, wrinkled and angulated with coarse chromatin (raisinoid)
- Common binucleation, multinucleation and perinuclear halos (koilocytic atypia)
- Mitotic figures present but usually scant
- Stroma minimal, composed of incomplete fibrovascular septae around solid sheets
- No chicken wire vasculature (more fibrovascular than vascular)
- Fuhrman / WHO grading has no prognostic value and is discouraged (Histopathology 2019;74:4)
- Paner grading system adds no prognostic value after considering TNM stage and sarcomatoid differentiation (Am J Surg Pathol 2010;34:1233, Am J Surg Pathol 2012;36:851)
- Eosinophilic variant of chromophobe renal cell carcinoma: when composed entirely of smaller eosinophilic cells
Microscopic (histologic) images
Contributed by Maria Tretiakova, M.D., Ph.D., Daniel Anderson, M.D., M.B.A. and @katcollmd on Twitter
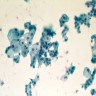
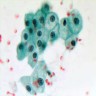
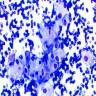
Cytology description
- Single cells and small, discohesive, monolayered groups; cells vary in size from small to large
- Large cells show clear, flocculent cytoplasm with small, eccentric nuclei and frequent binucleation, occasional nuclear pseudoinclusions
- Small cells usually have dense, homogeneous cytoplasm, clear cytoplasmic spaces resembling perinuclear halos, binucleation and marginal nuclear location
- No necrosis, no basement membrane or other stromal material (Cytopathology 2009;20:44, Cancer 1997;81:122)
Cytology images
Positive stains
- Most commonly used:
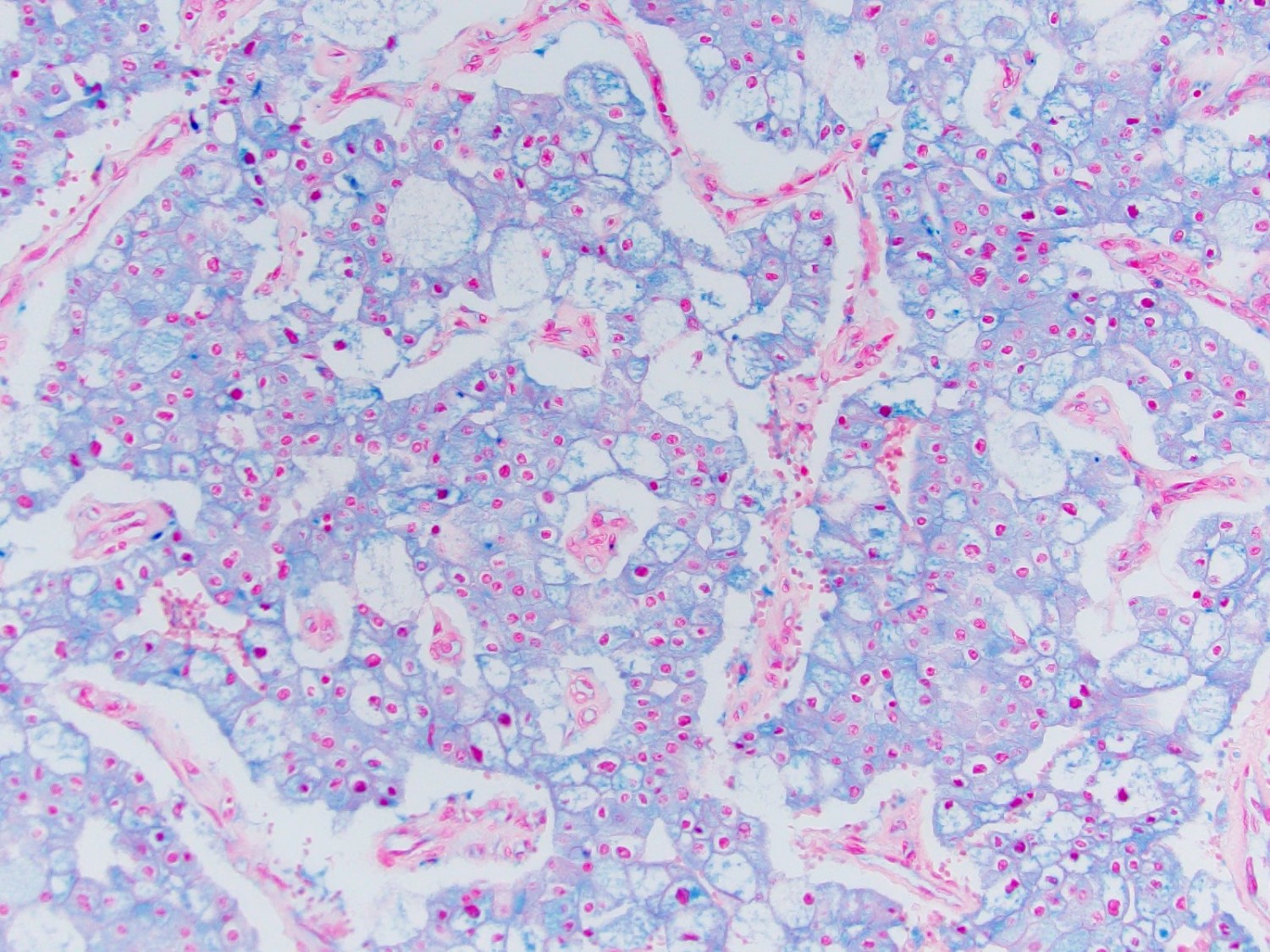
- Hale colloidal iron: stains acid mucopolysaccharides in microvesicles, diffuse and strong, reticular (J Pathol 1988;155:277, Am J Surg Pathol 1998;22:419)
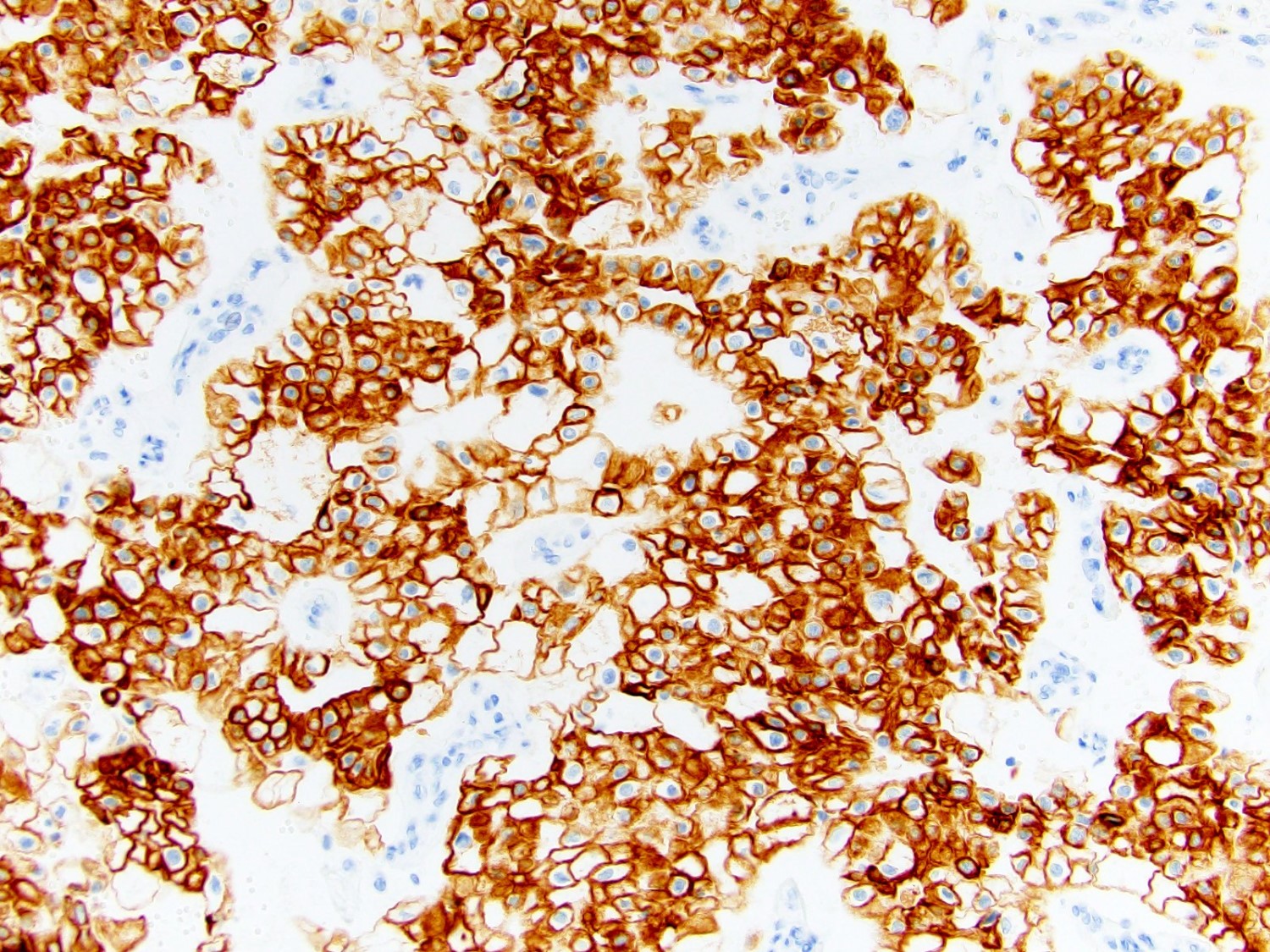
- CK7: diffuse and strong (compared with oncocytoma with scattered single cells) (Am J Clin Pathol 2007;127:225)
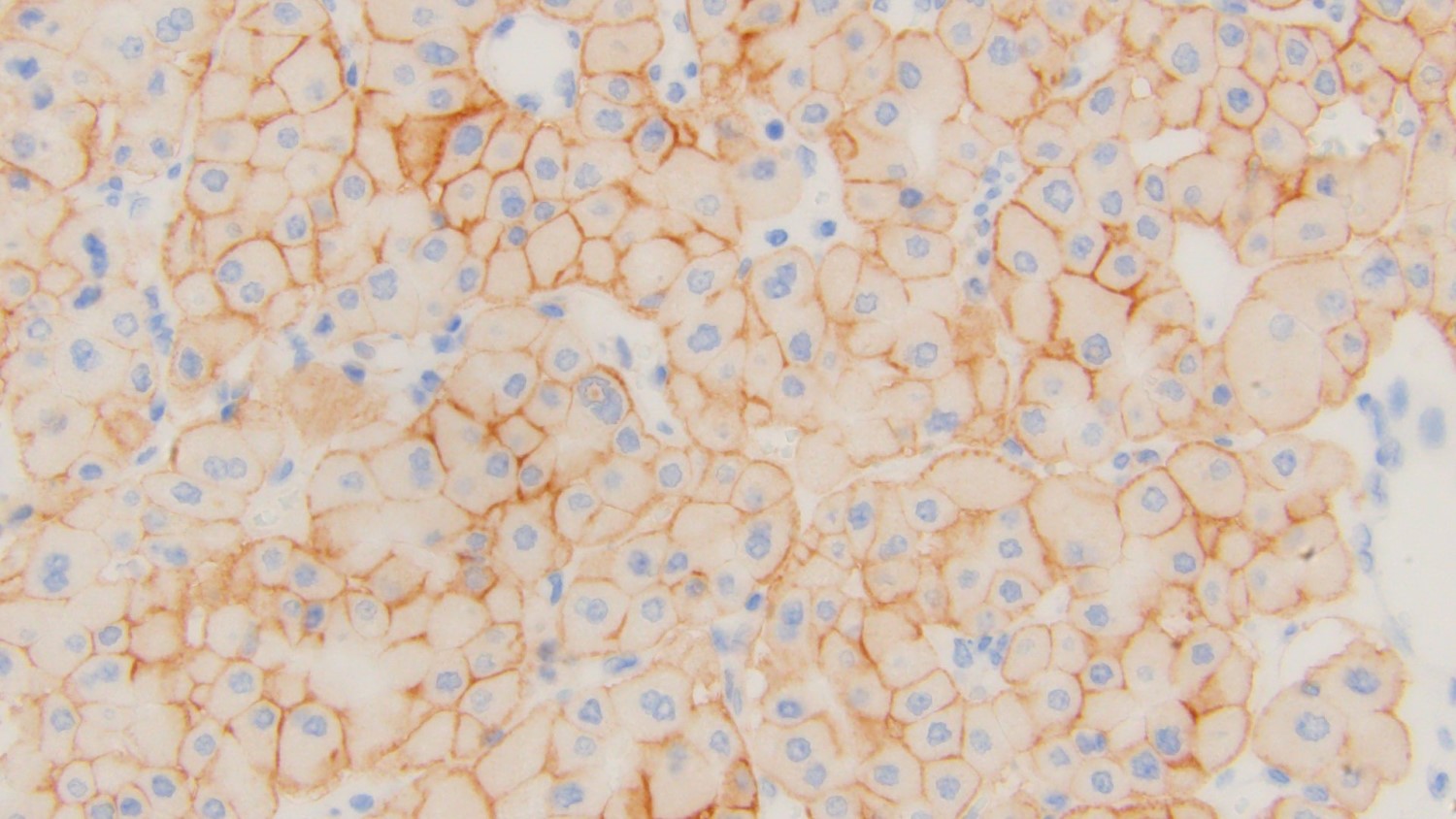
- CD117 / KIT: membranous (Hum Pathol 2005;36:262)
- Other positive stains:
- E-cadherin, claudin7 (distal nephron marker) (Arch Pathol Lab Med 2007;131:1541, Hum Pathol 2009;40:206)
- Kidney specific cadherin (Am J Clin Pathol 2006;126:79, Mod Pathol 2005;18:933)
- EMA / MUC1 (diffuse cytoplasmic) (Mod Pathol 2004;17:180)
- Low molecular weight keratin (CK8 / CK18), RCC, CD10 (Mod Pathol 2004;17:1455)
- Parvalbumin (calcium binding protein) (Mod Pathol 2001;14:760)
- Cytochrome c oxidase positive versus negative in oncocytoma (Appl Immunohistochem Mol Morphol 2015;23:54)
- DOG1 (Pathol Res Pract 2015;211:303)
- PR (90% cells) (Arch Pathol Lab Med 2019;143:1455)
- PDL1 22C3 expressed in a minority of cases (Med Oncol 2016;33:120)
Negative stains
- Vimentin (or weak), CAIX, AMACR, N-cadherin, low Ki67 labeling index (Mod Pathol 1999;12:310, Mod Pathol 1998;11:1115)
- Cyclin D1 (Pathol Res Pract 2015;211:303)
IHC panels
| Hale | KIT | CK7 | S100A1 | VIM | CAIX | AMACR | SDH | TFE3 | |
| Chromophobe RCC | +++ | +++ | +++ | - | - | - | - | +++ | - |
| Clear cell RCC | - | - | - | - | +++ | +++ | - | +++ | - |
| Oncocytoma | - | +++ | rare | +++ | - | - | - | +++ | - |
| Papillary RCC | - | - | +++ | - | +++ | - | +++ | +++ | - |
| Translocation RCC | - | - | - | - | - | - | ++ | +++ | +++ |
| SDH deficient RCC | - | - | - | - | - | - | - | - | - |
References: Pathol Res Pract 2015;211:303, Ann Diagn Pathol 2020;44:151448, Am J Surg Pathol 2014;38:e6, Arch Pathol Lab Med 2019;143:1455, Transl Androl Urol 2019;8:S123, Hum Pathol 2020 Jul 13 [Epub ahead of print]
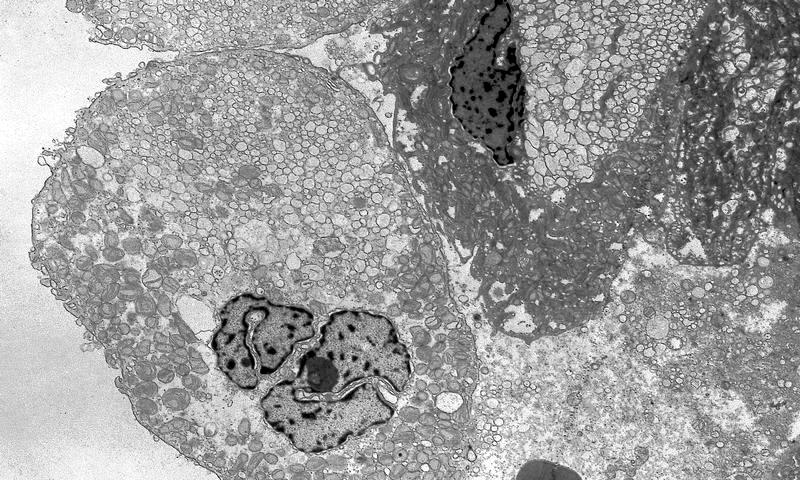
Electron microscopy description
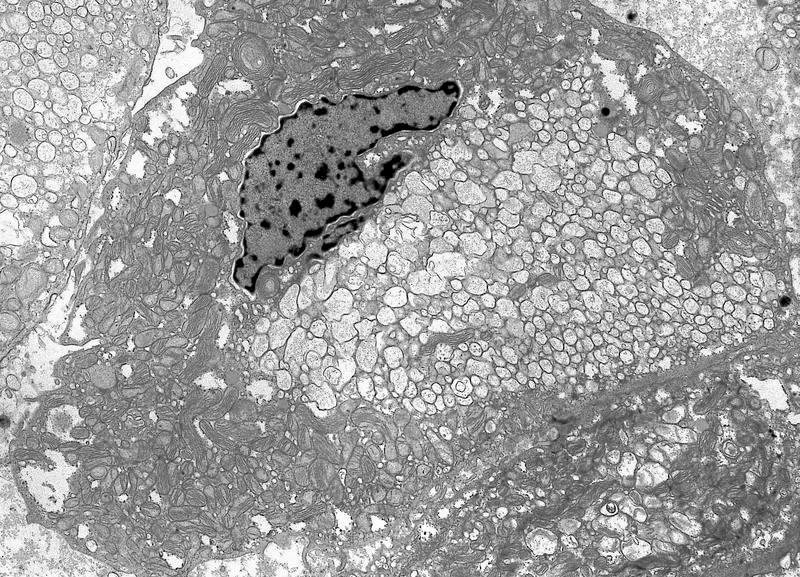
- All contain cytoplasmic microvesicles, which are considered a unique and consistent ultrastructural feature (Am J Surg Pathol 2000;24:1247)
- These 150 - 350 nm membrane bound microvesicles do not stain with H&E stain (chromophobe), often concentrated in perinuclear location corresponding to perinuclear halos on light microscopy and reticular pale cytoplasm
- Microvesicle origin is uncertain but possibly from mitochondrial outpouchings or defective mitochondriogenesis
- Eosinophilic cells are similar but with more mitochondria; mitochondria often show tubulocystic cristae, rare short and stubby microvilli (Am J Surg Pathol 2000;24:1247)
Electron microscopy images
Molecular / cytogenetics description
- Multiple losses of whole chromosomes, most often 1, 2, 6, 10, 13, 17, 21 or Y (versus no loss in oncocytoma) (Hum Pathol 1998;29:1181, Mod Pathol 2005;18:161)
- FISH and SNP arrays may be more helpful than karyotyping (Am J Clin Pathol 2010;133:116)
- DNA rearrangement breakpoints within the TERT promoter region
- TP53 and PTEN mutated in 10 - 30% cases (TCGA cohort) (Cancer Cell 2014;26:319)
- NRAS, mTOR and TSC1 / TSC2 in ~5% cases (JCI Insight 2017;2:e92688)
- Mitochondrial (mt) mutations DNA most commonly affect MT-ND5 (Cancer Cell 2014;26:319)
- Increased expression of genes encoding enzymes in the Krebs cycle (expression is suppressed in clear cell RCC) (Cancer Cell 2014;26:319)
- Sarcomatoid tumors have different genetic abnormalities (Mod Pathol 2007;20:303)
- MiRNA expression patterns may be associated with progression, recurrence free survival and overall survival (Sci Rep 2015;5:10328)
Differential diagnosis
Board review style question #1
Which of the following is true about chromophobe (ChRCC)?
- Binucleation is pathognomonic
- Cellulose deposition explains plant-like prominent membranes
- Cytoplasmic clearing is due to high concentration of lipids
- Multinucleation is an unfavorable prognostic feature
- Perinuclear halos are due to accumulation of cytoplasmic microvesicles
Board review style answer #1
E. Perinuclear halos are due to accumulation of cytoplasmic microvesicles. The presence of cytoplasmic microvesicles is a unique and consistent ultrastructural feature of ChRCC. Microvesicles are often concentrated in perinuclear location, corresponding to perinuclear halos on light microscopy. These vesicles lack affinity for H&E stain, resulting in cells with clear, reticular or flocculent cytoplasmic appearance on light microscopy (chromophobe). The origin is uncertain but likely related to defective mitochondria (Am J Surg Pathol 2000;24:1247).
Comment Here
Reference: Chromophobe
Comment Here
Reference: Chromophobe
Board review style question #2
What is the best statement describing chromophobe renal cell carcinoma (ChRCC)?
- Can be reliably distinguished from clear cell RCC by CK7, CKIT (CD117), CAIX and vimentin
- Classic autosomal dominant genetic correlation is Birt-Hogg-Dubé syndrome, which is associated with a mutation of the HOGG gene on chromosome 3p
- Fuhrman / WHO grading is useful prognostic indicator
- Sarcomatoid dedifferentiation is very common
- To establish the diagnosis, a documentation of monosomies involving chromosomes 1, 2, 6, 10, 13, 17, 21 or Y is needed
Board review style answer #2
A. Chromophobe shows multiple losses of whole chromosomes, most often 1, 2, 6, 10, 13, 17, 21 or Y but documentation of monosomies is not required for diagnosis. Sarcomatoid change is a significant poor prognostic indicator in chromophobe renal cell carcinoma but observed in ~5% of cases. Birt-Hogg-Dubé is caused by an autosomal dominant mutation of the Folliculin gene (FLCN) at 17p11.2 leading to premature truncation and loss of function of the folliculin protein. Von Hippel-Lindau syndrome, also autosomal dominant, is caused by a mutation of the VHL tumor suppressor gene (3p25-26). Depending on the subtype, VHL is associated with clear cell renal cell carcinoma, CNS and retinal hemangioblastomas, visceral cysts in the kidney, pancreas and epididymis, endolymphatic sac tumors, pancreatic neuroendocrine tumors, paragangliomas and pheochromocytomas (Front Horm Res 2013;41:30). Unlike clear cell renal cell carcinoma, Fuhrman / ISUP grade has no prognostic value. ChRCC by immunostaining CAIX and vimentin are negative and CK7 and CKIT (CD117) positive. Clear cell RCC shows opposite expression with CAIX and vimentin positive and CK7/CKIT negative.
Comment Here
Reference: Chromophobe
Comment Here
Reference: Chromophobe