Table of Contents
Definition / general | Essential features | Terminology | ICD coding | Epidemiology | Pathophysiology | Etiology | Diagrams / tables | Clinical features | Diagnosis | Radiology description | Radiology images | Prognostic factors | Case reports | Treatment | Gross description | Gross images | Frozen section description | Frozen section images | Microscopic (histologic) description | Microscopic (histologic) images | Positive stains | Negative stains | Sample pathology report | Differential diagnosis | Board review style question #1 | Board review style answer #1 | Board review style question #2 | Board review style answer #2Cite this page: Ikura Y. Nonalcoholic fatty liver disease / nonalcoholic steatohepatitis (NASH). PathologyOutlines.com website. https://www.pathologyoutlines.com/topic/liverNASH.html. Accessed April 17th, 2024.
Definition / general
- Nonalcoholic fatty liver disease (NAFLD) is hepatic steatosis generated in association with overweight / obesity, type 2 diabetes mellitus or other metabolic dysregulations
- Morphologically, NAFLD covers all forms of hepatic steatosis with or without inflammation / fibrosis
Essential features
- Macrovesicular hepatosteatosis accentuated on zone 3, potentially accompanying fibroinflammatory changes in metabolic patients
- Presence of concomitant liver disease does not become a reason for excluding metabolic (dysfunction) associated fatty liver disease (MAFLD) (NAFLD/NASH) (Gastroenterology 2020 May;158:1999)
- Steatohepatitis is not the sole progressive form of NAFLD (J Hepatol 2015;62:1148)
- Histologic grade is assessed using a scoring system including steatosis, lobular inflammation and ballooning degeneration (Hepatology 2005;41:1313)
- Patients are at risk for fibrosis, cirrhosis and hepatocellular carcinoma
Terminology
- Nonalcoholic fatty liver disease (NAFLD) refers to any fatty liver disease caused by metabolic dysregulation, as above
- Nonalcoholic steatohepatitis refers to an aggressive form of the disease characterized by inflammation and ballooning in addition to steatosis
- Metabolic (dysfunction) associated fatty liver disease (MAFLD) has been proposed as a new, more accurate term for NAFLD (J Hepatol 2020 Apr 8 [Epub ahead of print])
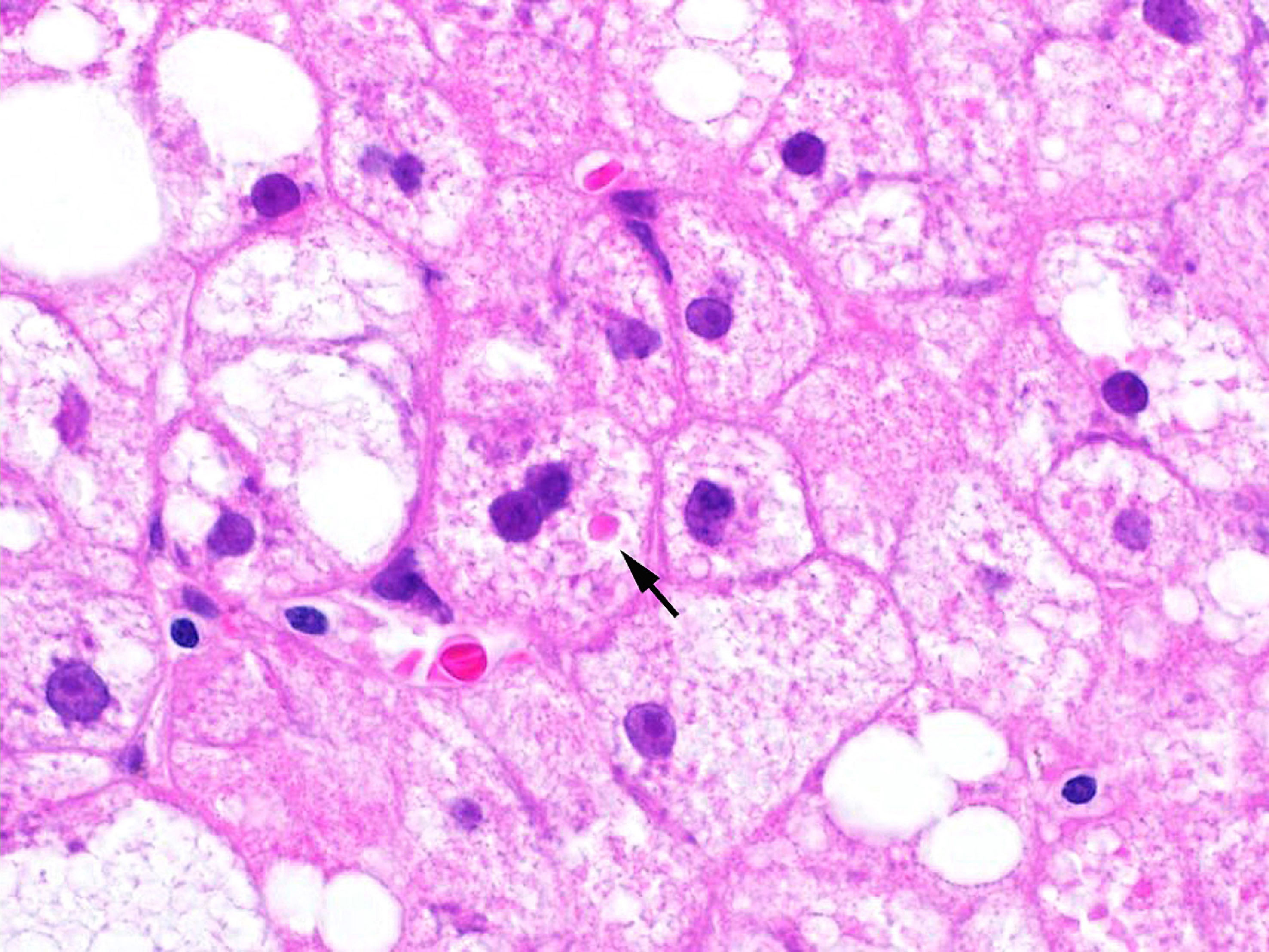
- Cytoplasmic inclusions known as Mallory-Denk bodies (see microscopic images) are also termed Mallory’s hyaline and intracytoplasmic hyaline
ICD coding
- ICD-10: K76.0 - fatty (change of) liver, not elsewhere classified
Epidemiology
- One of the most important causes of liver disease worldwide in adults and children (Nat Rev Gastroenterol Hepatol 2018;15:11)
- Global prevalence is ~24% (Nat Rev Gastroenterol Hepatol 2018;15:11)
- It largely affects patients with unhealthy metabolic conditions but can occur even in lean individuals (Medicine (Baltimore) 2012;91:319)
Pathophysiology
- Hepatic manifestation of metabolic disorders
- Oxidative stress and lipotoxicity are considered key factors in disease progression (Hepatology 2006;43:506, J Atheroscler Thromb 2009;16:893)
- Genetic variants in patatin-like phospholipase domain containing protein 3 (PNPLA3), transmembrane 6 superfamily 2 (TM6SF2), membrane bound O-acyltransferase domain containing 7 (MBOA7) and hydroxysteroid 17-beta dehydrogenase 13 (HSD17B13) are known modifiers of NAFLD (Clin Med (Lond) 2018;18:s54, J Hepatol 2018;68:268)
Etiology
- Overweight / obesity and type 2 diabetes mellitus (J Hepatol 2020 Apr 8 [Epub ahead of print])
- Other metabolic disorders (dyslipidemia, insulin resistance, hypertension, etc.) (J Hepatol 2020 Apr 8 [Epub ahead of print])
Clinical features
- Most patients with MAFLD (NAFLD) are asymptomatic and diagnosed incidentally (Clin Liver Dis 2016;20:277)
- The prevalence of MAFLD (NAFLD) is high in people of Asian and Hispanic origin (Clin Liver Dis 2018;22:39)
- Fatty livers induced by alternative causes (medications, starvation, inherited disorders of lipid metabolism, etc.) are not metabolic (dysfunction) associated fatty liver disease (J Hepatol 2020 Apr 8 [Epub ahead of print])
Diagnosis
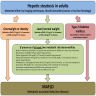
- Clinically or histologically detected hepatic steatosis in patients with metabolic disorders (see diagram)
- Presence of other concomitant liver diseases, including alcoholic liver disease, is not an exclusion criterion (J Hepatol 2020 Apr 8 [Epub ahead of print])
- Disease severity is evaluated semiquantitatively with the NASH Clinical Research Network criteria (Hepatology 2005;41:1313)
- Distinction between simple steatosis and steatohepatitis is unnecessary (J Hepatol 2020 Apr 8 [Epub ahead of print])
- Fatty livers induced by alternative causes (medications, starvation, inherited disorders of lipid metabolism, etc.) are not considered NAFLD (J Hepatol 2020 Apr 8 [Epub ahead of print])
Radiology description
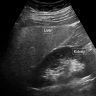
- Bright liver and increased hepatorenal contrast on ultrasound (US) (Tohoku J Exp Med 1983;139:43)
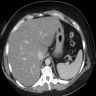
- Liver / spleen attenuation ratio < 1.1 on computed tomography (CT) (Hepatol Commun 2019;3:1347)
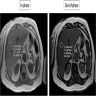
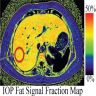
- High signal intensity on T1 weighted magnetic resonance images (MRI)
- Whole hepatic lipid volume is quantifiable by using a special MRI technique (Hepatol Res 2019;49:1374)
Radiology images
Prognostic factors
- Presence of fibrosis is a sole prognostic factor in NAFLD (Gastroenterology 2015;149:389, Hepatology 2015;61:1547)
Case reports
- 14.5 year old boy diagnosed histologically as having nonalcoholic fatty liver disease (Cold Spring Harb Mol Case Stud 2018;4: a003087)
- 52 year old man urgently hospitalized because of intraabdominal hemorrhage (J Diabetes 2017;9:311)
- 56 year old woman with nonalcoholic steatohepatitis and Graves disease (Intern Med 2016;55:2019)
- 67 year old obese woman who received methotrexate for rheumatoid arthritis (Int J Clin Exp Pathol 2015;8:1961)
Treatment
- Currently, there is no approved specific therapy
Gross description
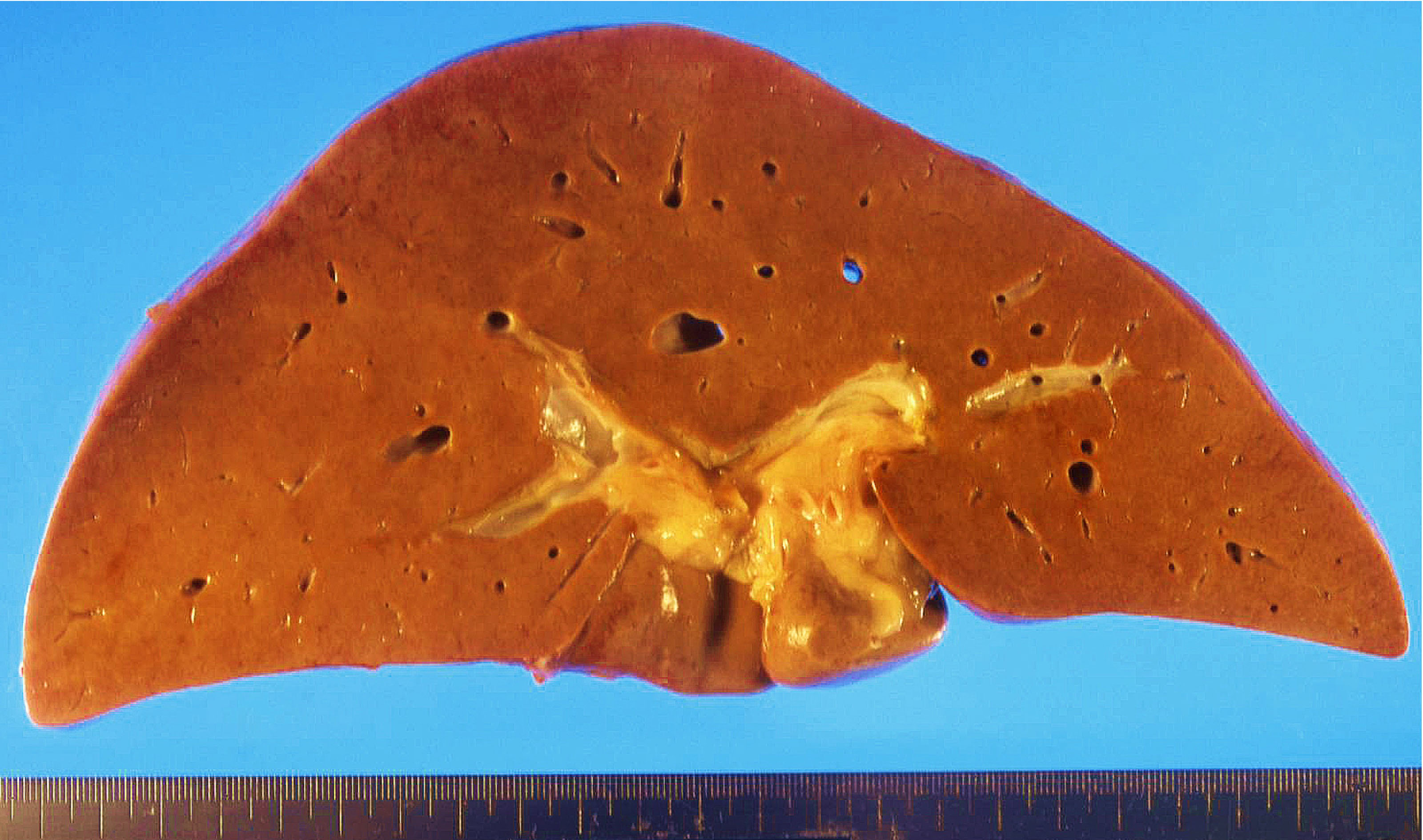
- Swollen soft liver with yellowish brown color
- Surface of affected liver becomes irregular with progression of fibrosis
- Some cases show cirrhosis or hepatocellular carcinoma
Frozen section description
- Lipid stain methods (Oil Red O, Sudan black B, filipin, etc.) to detect liver fat can be performed on frozen sections
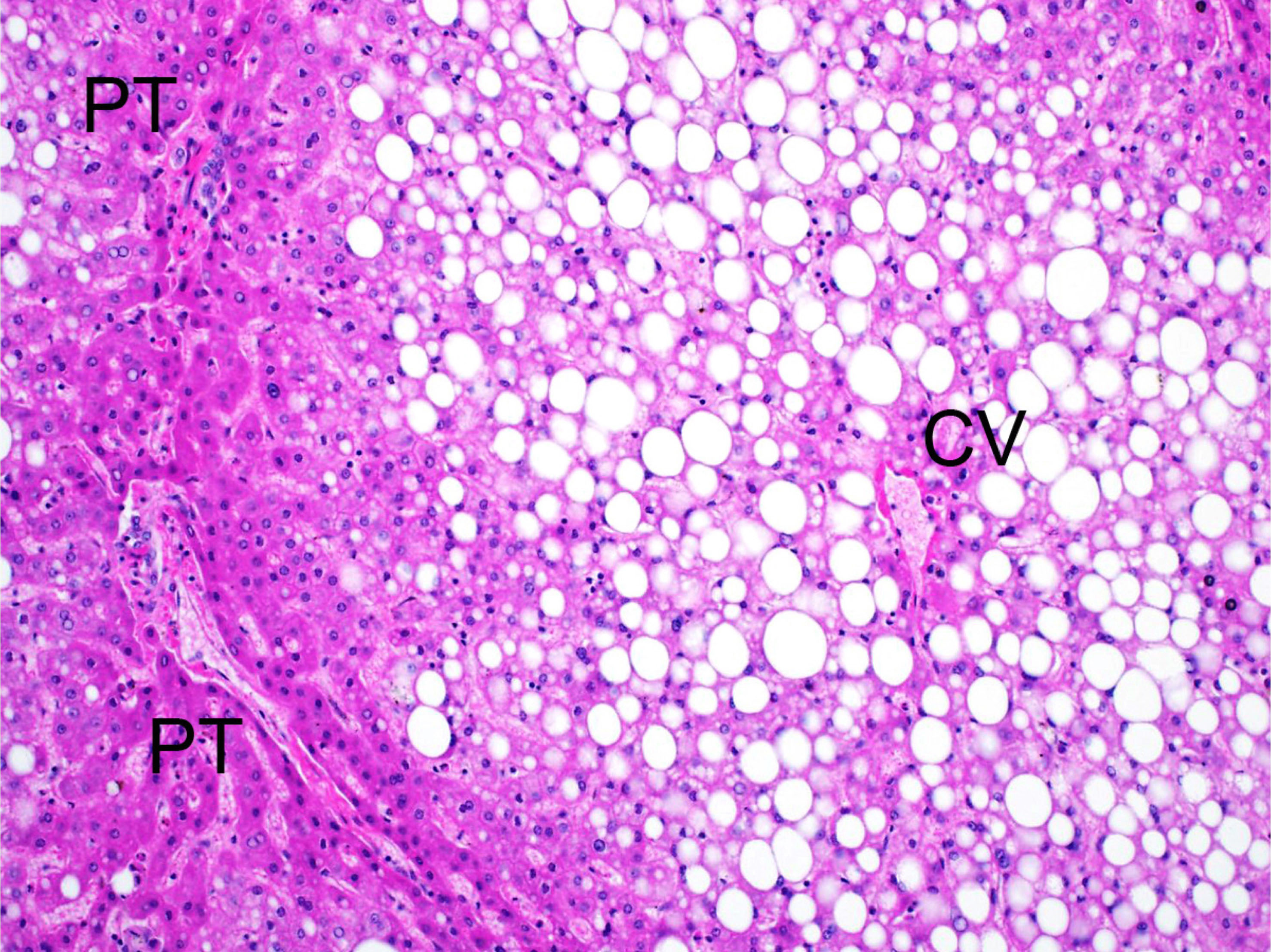
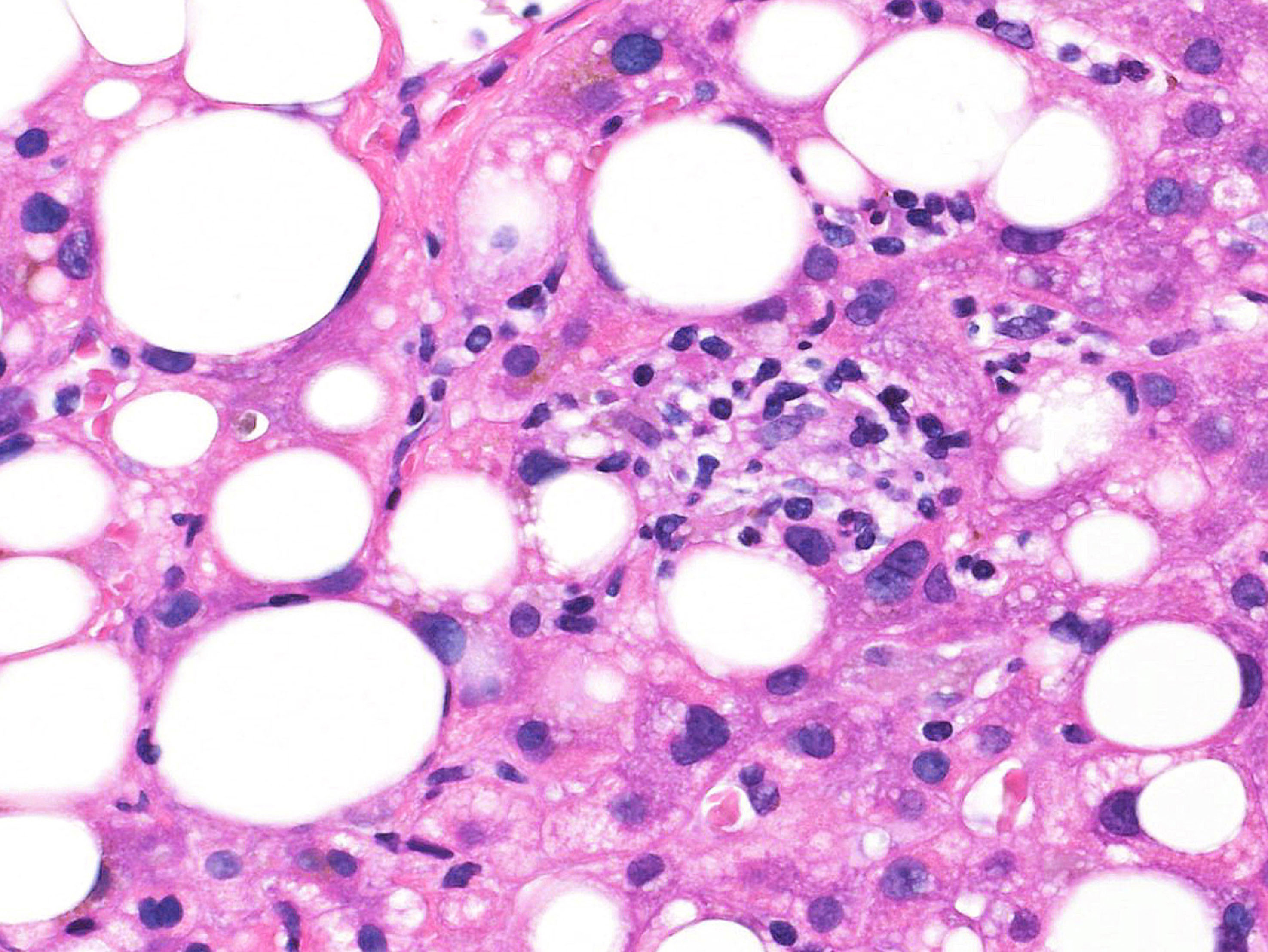
Microscopic (histologic) description
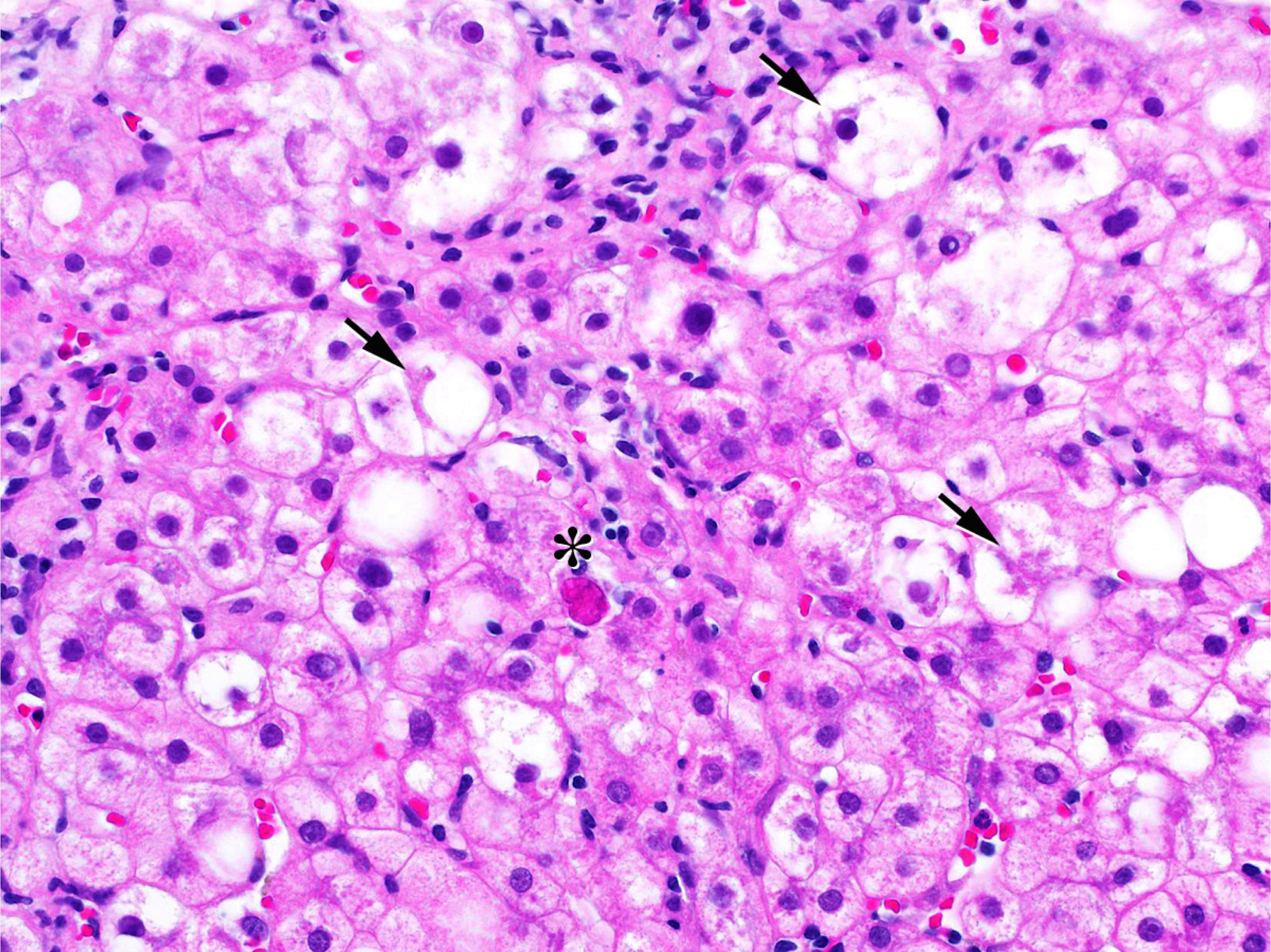
- Predominantly macrovesicular steatosis in ≥ 5% hepatocytes under low magnification (4x or lower) observation is a sole histologic requirement for diagnosis of NAFLD
- Disease severity is evaluated separately by grade of activity and stage of fibrosis
- Activity grade is assessed according to nonalcoholic fatty liver disease activity score (NAS) using the sum of 3 components (total 0 - 8 points) (Hepatology 2005;41:1313)
- Steatosis (0: < 5%; 1: 5 - 33%; 2: 34 - 66%; 3: > 66%)
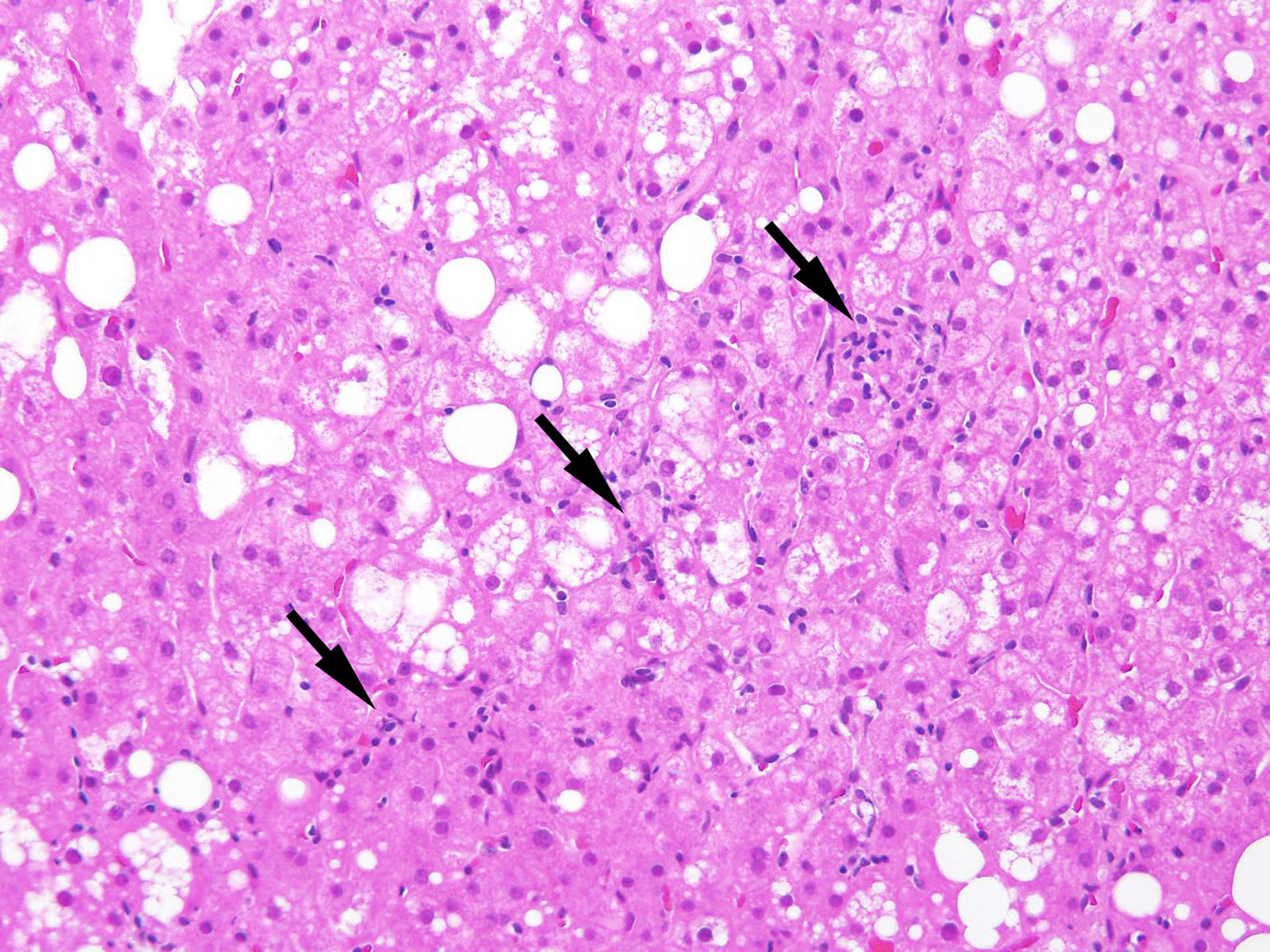
- Lobular inflammation (0: none; 1: < 2 foci/20x field; 2: 2 - 4 foci/20x field; 3: > 4 foci/20x field)
- Ballooning degeneration (0: none; 1: few; 2: many)
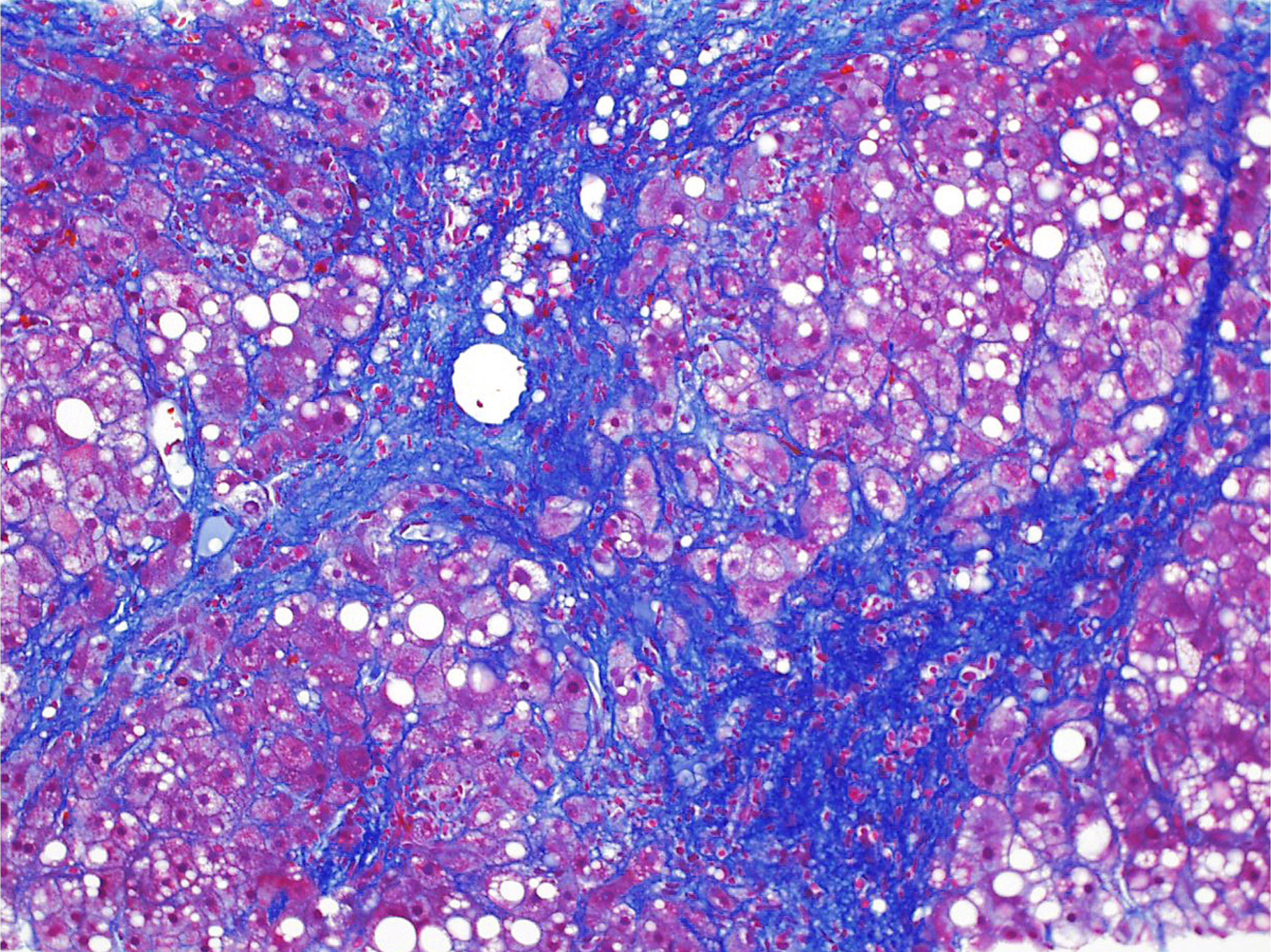
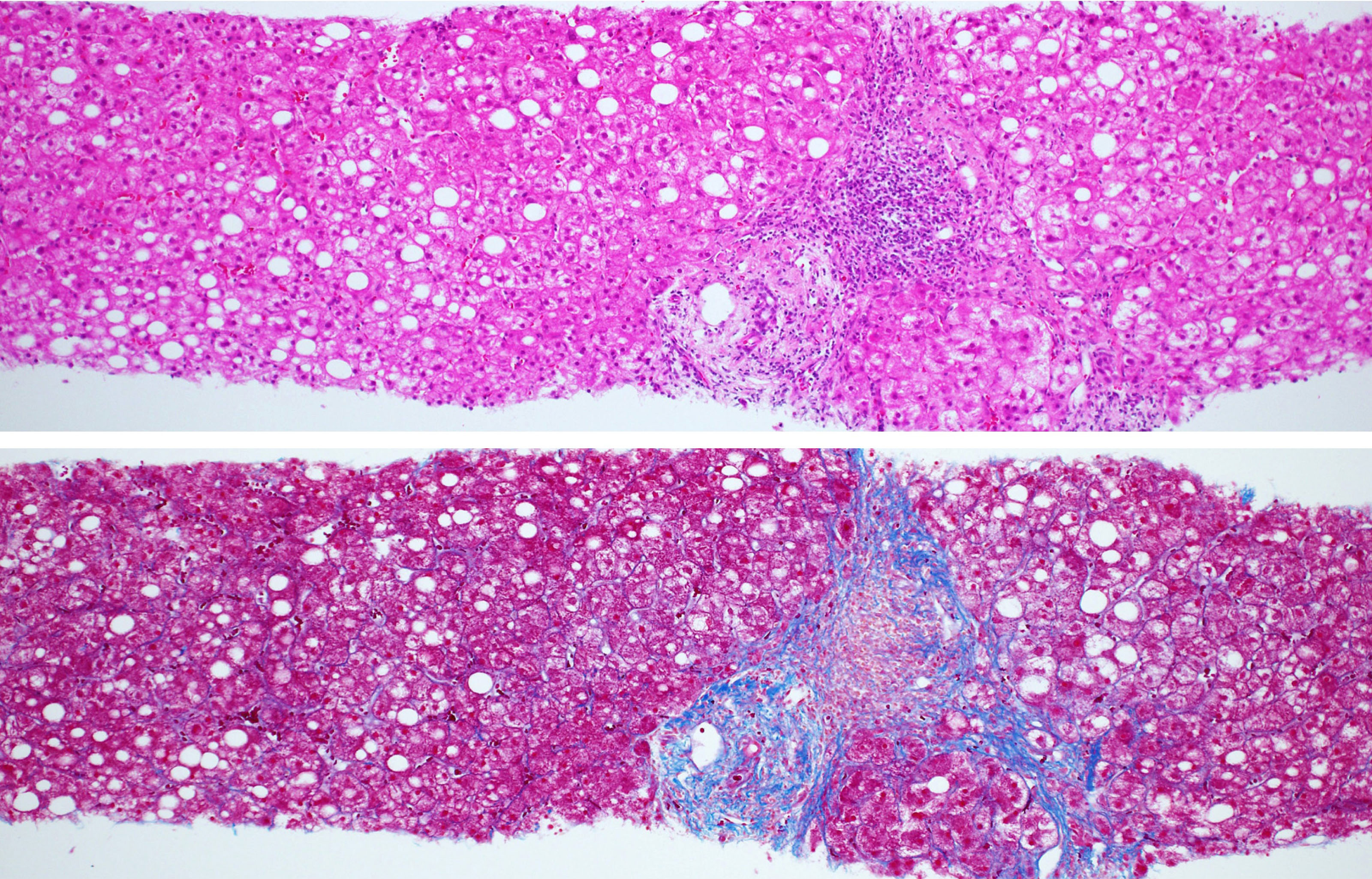
- Fibrosis stage is assessed into 5 levels; stage 0, none; stage 1, perivenular (zone 3) fibrosis; stage 2, perivenular + portal fibrosis; stage 3, bridging fibrosis; stage 4, cirrhosis (Hepatology 2005;41:1313)
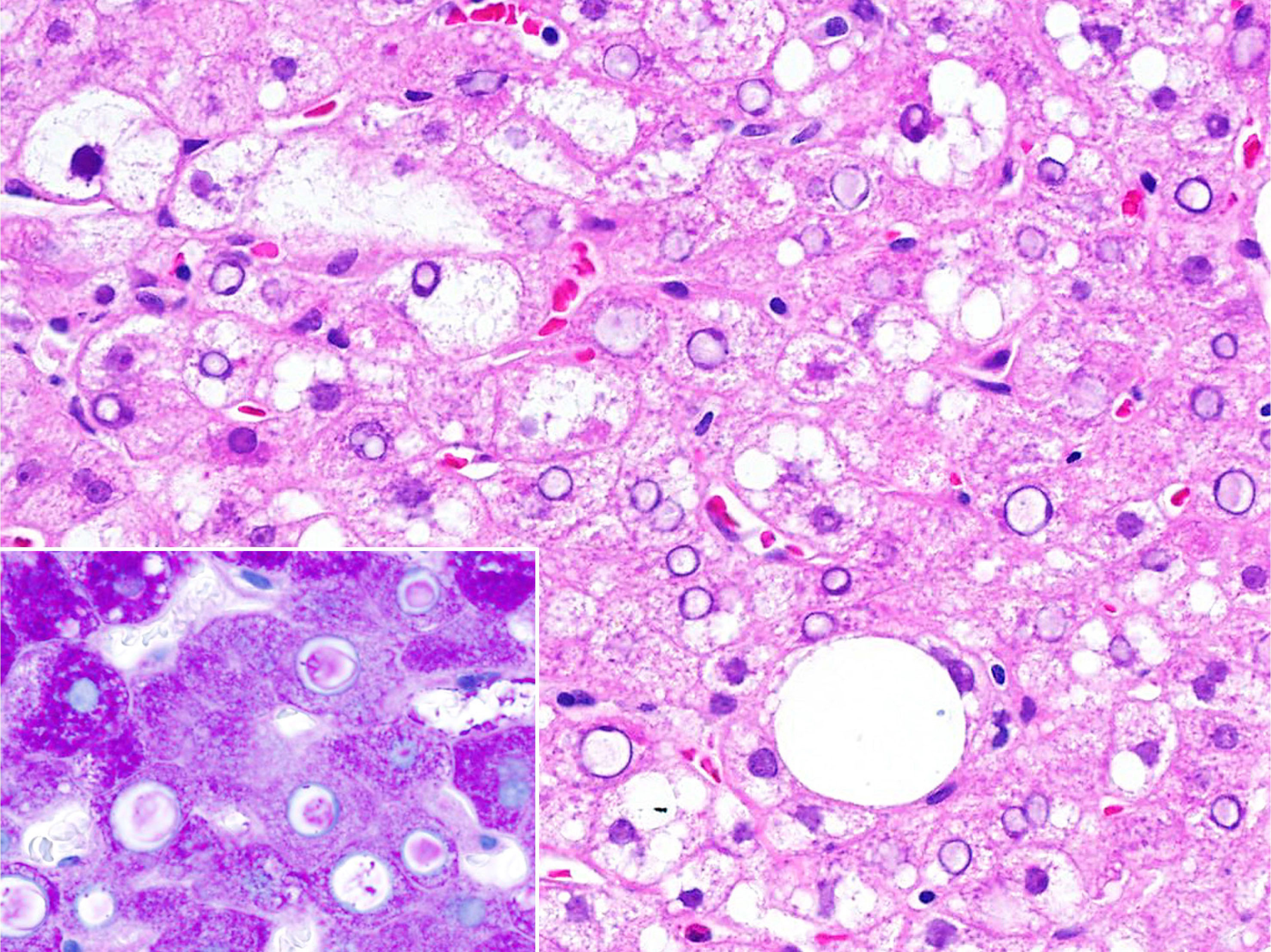
- Other characteristic findings are Mallory-Denk bodies, glycogenated nuclei, giant mitochondria (megamitochondria) and lipogranuloma
- Histologic changes of concomitant liver conditions may be seen
- In NAFLD associated cirrhosis, steatotic hepatocytes may be burnt out, resulting in a loss of visible steatosis, but the term "cryptogenic cirrhosis" should not be used for this condition (J Hepatol 2020 Apr 8 [Epub ahead of print])
Positive stains
- Special stains for collagen (Masson trichrome, Sirius red, Azan-Mallory, etc.) mandatory: faint fibrosis cannot be detected on hematoxylin eosin tissue slides
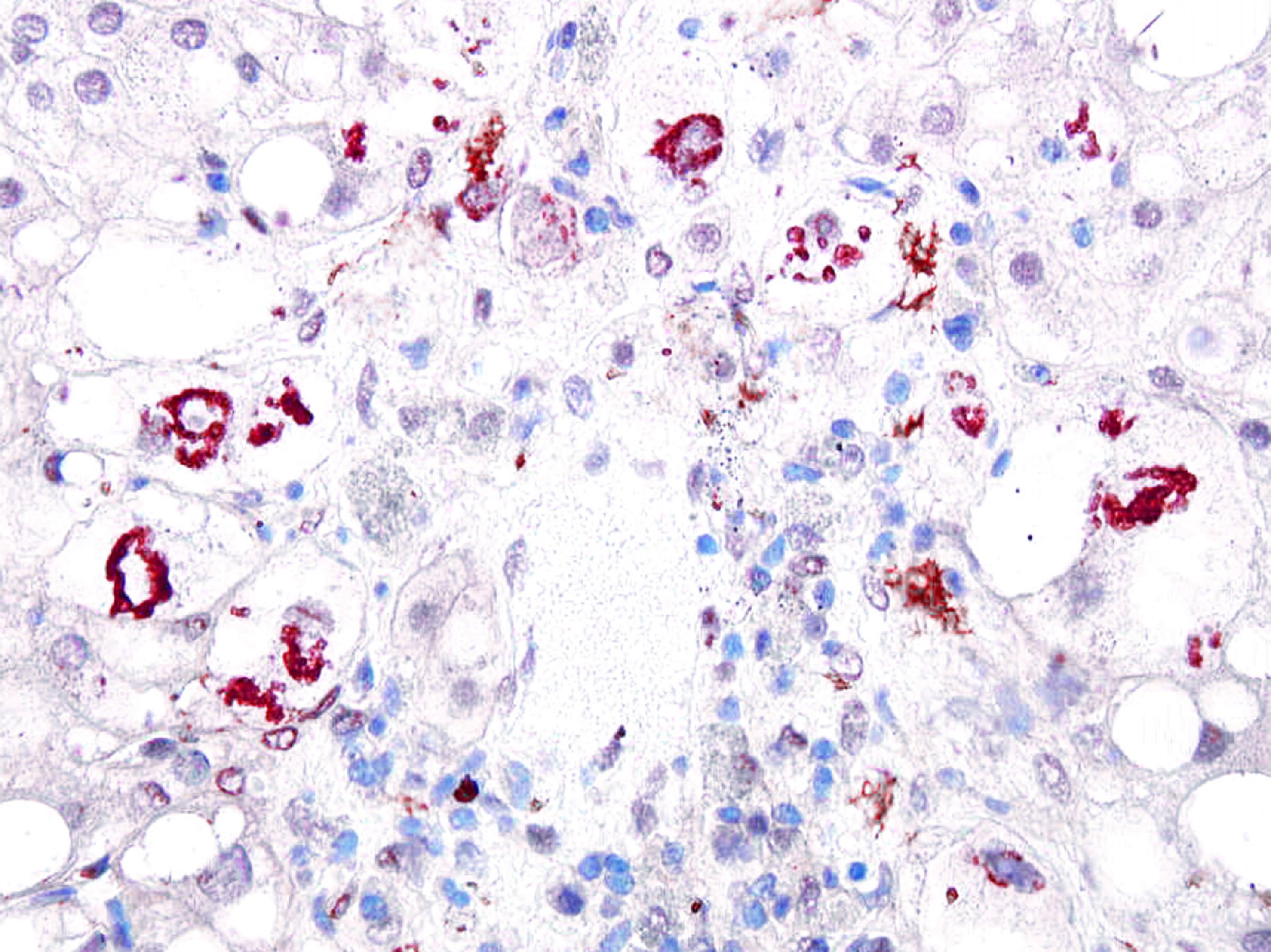
- Ubiquitin, p62, CK18: Mallory-Denk bodies are stained
- References: Histochem Cell Biol 2008;129:735, Exp Mol Pathol 2011;90:252
Negative stains
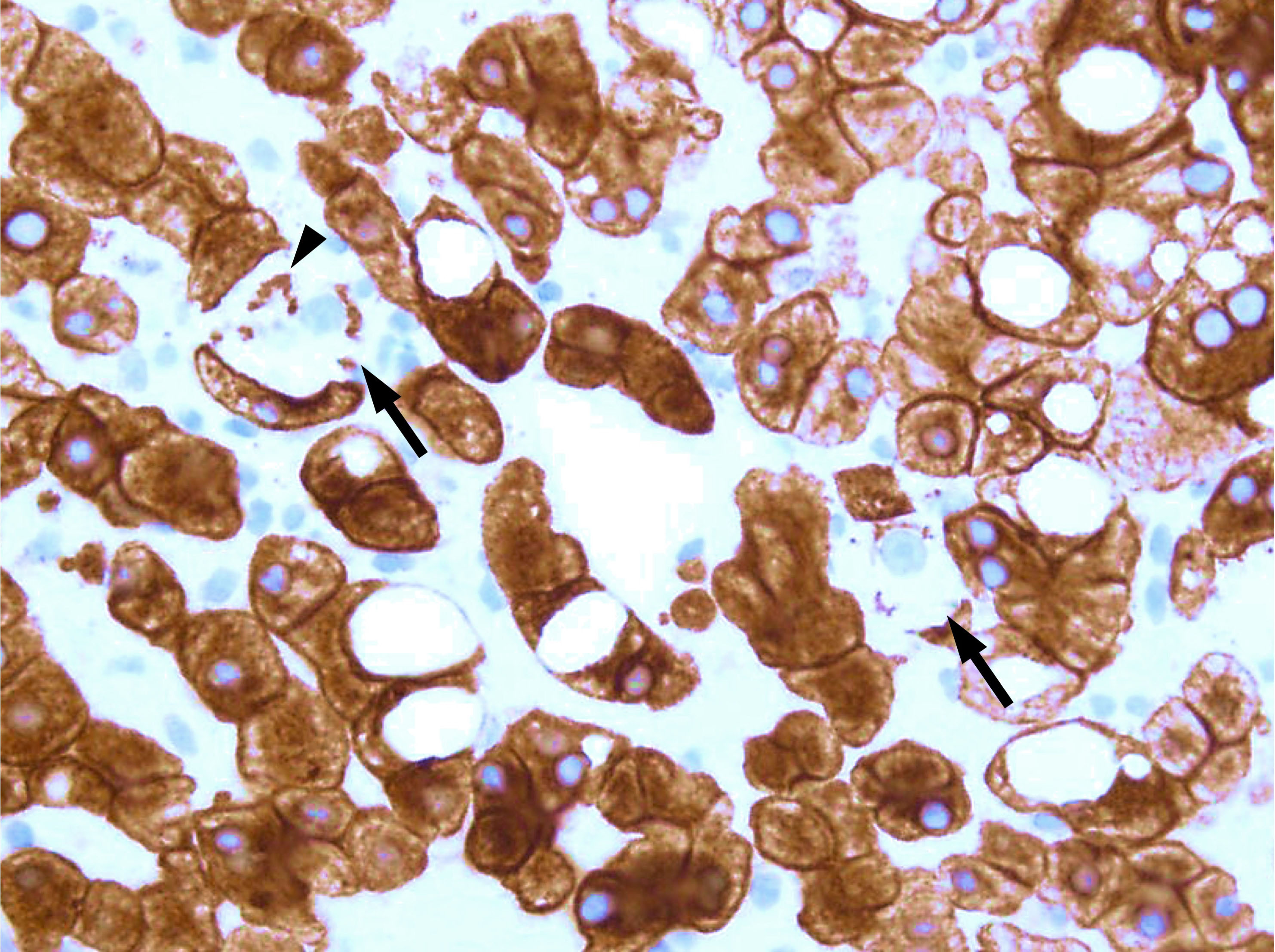
- CK18: ballooned hepatocytes are characteristically negative (J Hepatol 2010;53:719)
Sample pathology report
- Liver, needle biopsy:
- Fatty liver, consistent with nonalcoholic fatty liver disease
- NAS 6 points = steatosis 2 + inflammation 2 + ballooning 2
- Stage 2 (perivenular + portal fibrosis)
Differential diagnosis
- Can coexist with any type of liver diseases including alcoholic damage (J Hepatol 2020 Apr 8 [Epub ahead of print])
- Histologic mimics of NAFLD include some genetic conditions (Wilson disease, lysosomal acid lipase deficiency, etc.) and some forms of drug induced liver injury (methotrexate, etc.) (Cold Spring Harb Mol Case Stud 2018;4: a003087, Med Clin North Am 2019;103:991, Int J Clin Exp Pathol 2015;8:1961)
- Differential diagnosis of fatty liver diseases should be made clinically
Board review style question #1
A 78 year old woman with a > 10 year treatment history of rheumatoid arthritis shows elevated serum levels of liver enzymes (AST, 120 IU; ALT, 136 IU; GGT, 129 IU). She is an occasional drinker and does not have metabolic disorders. She is taking methotrexate (MTX). Hepatitis virus B and C are negative and antinuclear antibody is ×160. Liver biopsy, shown above, shows steatosis and inflammation. What should be done next in the diagnostic workup?
- Administration of steroids
- ATP7B gene testing
- Cessation of MTX
- Drug induced lymphocyte stimulation test
- Serum AMA
Board review style answer #1
C. Cessation of MTX. MTX is a first line therapy for rheumatoid arthritis and can cause steatohepatitis that mimics NAFLD.
Comment Here
Reference: Nonalcoholic fatty liver disease (NAFLD) / nonalcoholic steatohepatitis (NASH)
Comment Here
Reference: Nonalcoholic fatty liver disease (NAFLD) / nonalcoholic steatohepatitis (NASH)
Board review style question #2
Board review style answer #2
E. Ubiquitin positive. The inclusion shown is a Mallory-Denk body. It is a ubiquitinated aggregate of keratin filament that occurs in ballooned hepatocytes.
Comment Here
Reference: Nonalcoholic fatty liver disease (NAFLD) / nonalcoholic steatohepatitis (NASH)
Comment Here
Reference: Nonalcoholic fatty liver disease (NAFLD) / nonalcoholic steatohepatitis (NASH)