Table of Contents
Definition / general | Essential features | Epidemiology | Sites | Etiology | Clinical features | Diagnosis | Laboratory | Radiology images | Prognostic factors | Case reports | Treatment | Gross images | Microscopic (histologic) description | Microscopic (histologic) images | Positive stains | Sample pathology report | Differential diagnosis | Board review style question #1 | Board review style answer #1Cite this page: Gonzalez R. Herpes simplex virus hepatitis. PathologyOutlines.com website. https://www.pathologyoutlines.com/topic/liverherpeshep.html. Accessed April 25th, 2024.
Definition / general
- Rare complication of herpes infection resulting in geographic (nonzonal) hemorrhagic necrosis that is usually fatal
- 1% of acute liver failure (Clin Transplant 2009;23:37)
Essential features
- Geographic (nonzonal) hemorrhagic necrosis
- Usually pregnant women or immunocompromised patients
- Often clinically unsuspected (Liver Transpl 2007;13:1428)
- Often not diagnosed until autopsy due to nonspecific clinical features
Epidemiology
- Immunocompromised patients are most susceptible
- Immunocompetent patients can be affected (Am J Clin Pathol 1986;85:694)
- Risk factors include malignancy and pregnancy (mean 31 weeks) (Hum Pathol 1992;23:183)
- Neonates can also acquire herpes congenitally (as it is one of the TORCH infections), with roughly a quarter of them at risk for developing fulminant hepatitis
Sites
- Liver
Etiology
- HSV1 or HSV2
Clinical features
- Uncommon cause of liver failure in adults (Liver Transpl 2008;14:1498)
- Anicteric (not accompanied by jaundice)
- Fever (98%), coagulopathy (84%) and encephalopathy (80%) (Liver Transpl 2008;14:1498)
- Clinical presentation in adults is typically that of shock
Diagnosis
- HSV DNA can be detected in the blood
- 58% diagnosed at autopsy via histologic and immunohistochemical analysis of liver tissue (Liver Transpl 2007;13:1428)
Laboratory
- Marked elevation of liver serum markers (AST, ALT, bilirubin, alkaline phosphatase, GGT)
- Leukopenia
- HSV DNA identified via PCR
Prognostic factors
- Rapid downhill course with acute liver failure, usually fatal (up to 81% of adults) due to massive hepatic necrosis (Clin Transplant 2009;23:37), even with rapid antiviral therapy or liver transplantation (Liver Transpl 2008;14:1498)
- Better survival after transplantation in children (69%) than adults (38%) (J Hepatol 2011;55:1222)
- Worse prognosis (Liver Transpl 2008;14:1498): male gender
- Age > 40 years
- Immunocompromised
- ALT > 5,000 U/L
- Platelet count < 75 x 103/L
- Coagulopathy
- Encephalopathy
- Absence of antiviral therapy
Case reports
- 11 day old boy successfully treated without transplantation (ACG Case Rep J 2017;4:e23)
- 18 year old women with fever and pharyngodynia (Case Reports Hepatol 2017;2017:4630621)
- 41 year old women at 31 weeks of pregnancy with fatal course (Intractable Rare Dis Res 2017;6:124)
- 44 year old woman with nausea and vomiting (Case of the Month #481)
- 67 year old man with lesions mimicking abscess (Case Reports Hepatol 2016;2016:8348172)
- 89 year old man with sepsis secondary to urinary tract infection and fatal course (Eur J Case Rep Intern Med 2018;5:000982)
Treatment
- Empiric antiviral therapy (acyclovir)
- Liver transplantation with lifelong acyclovir prophylaxis
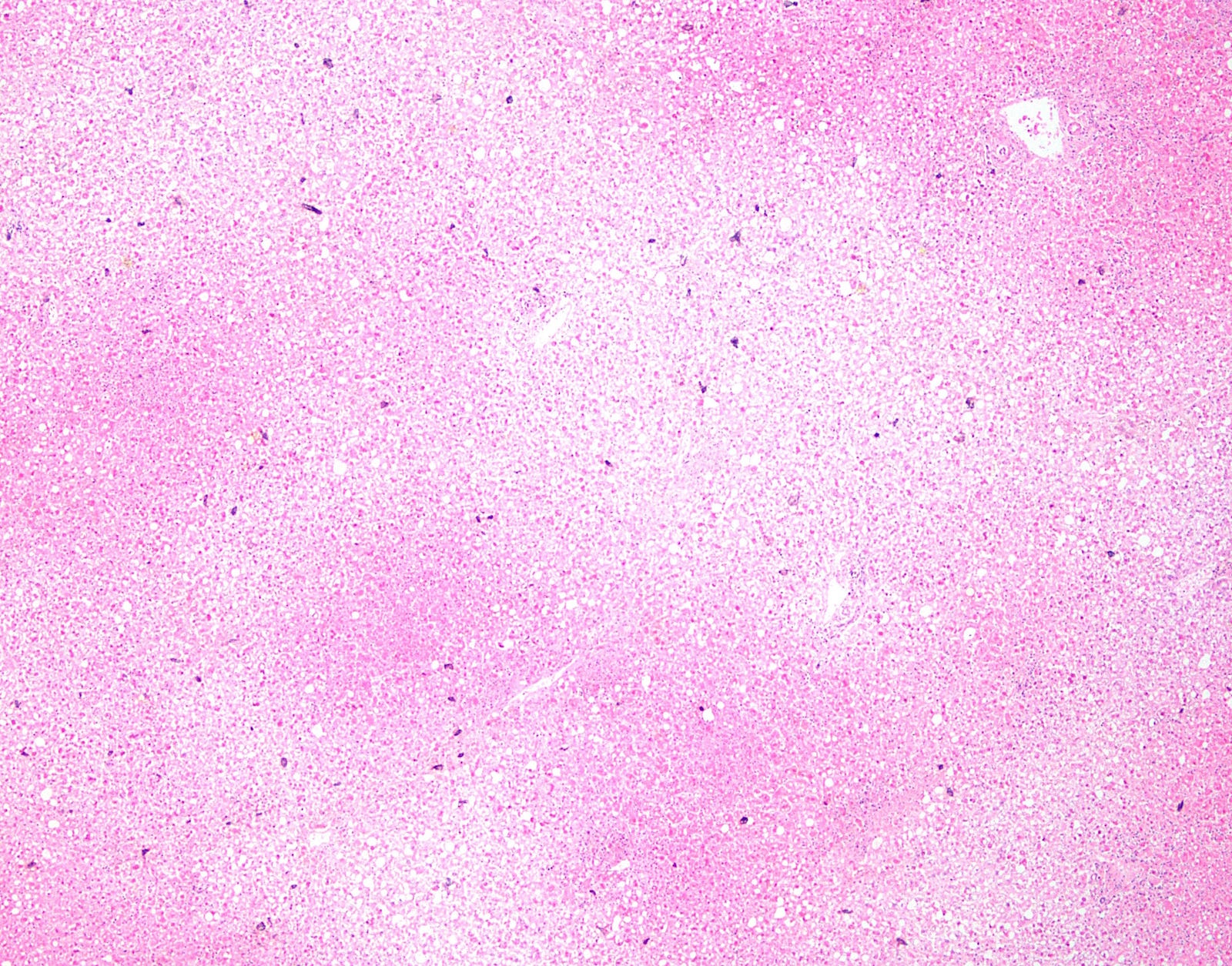
Microscopic (histologic) description
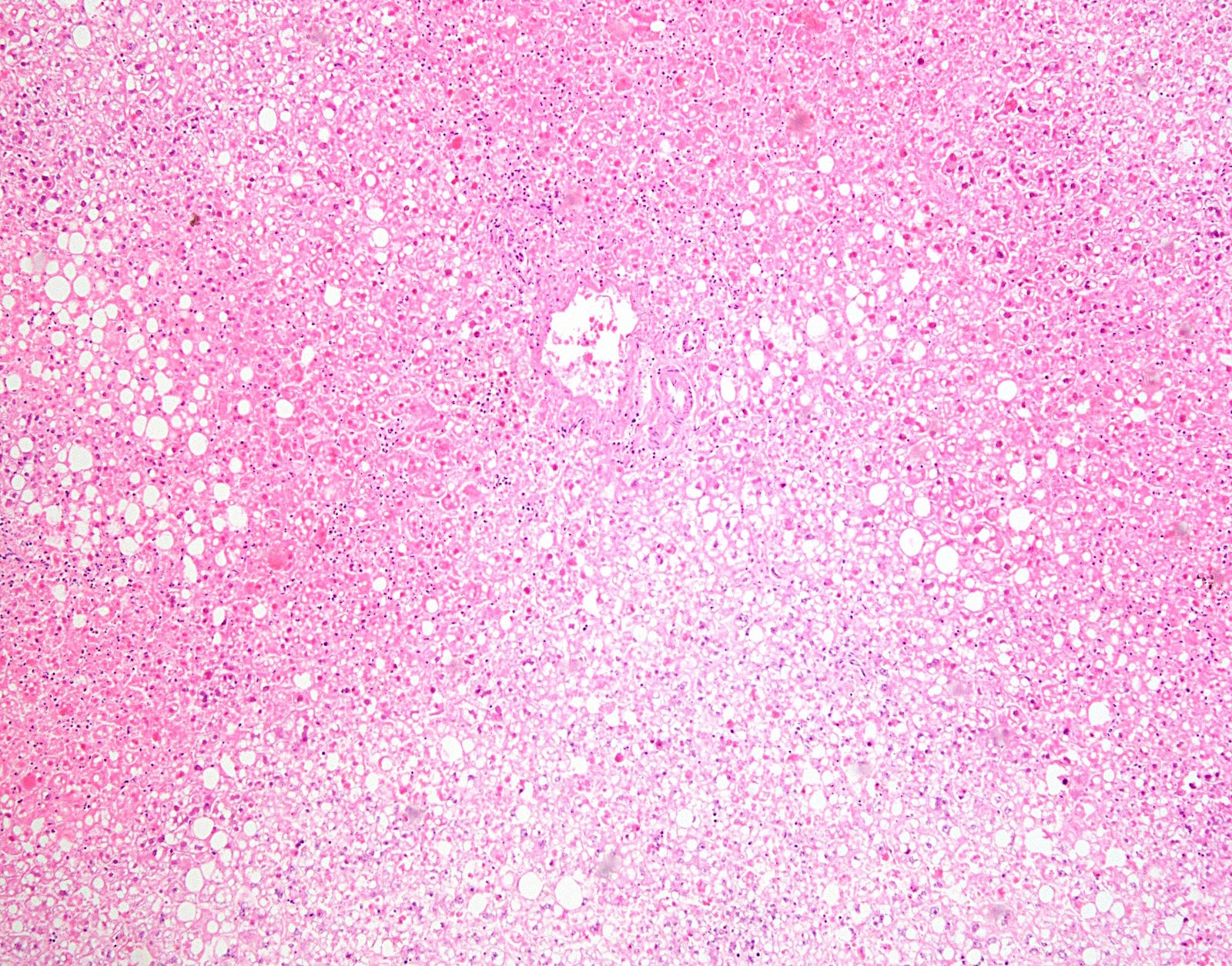
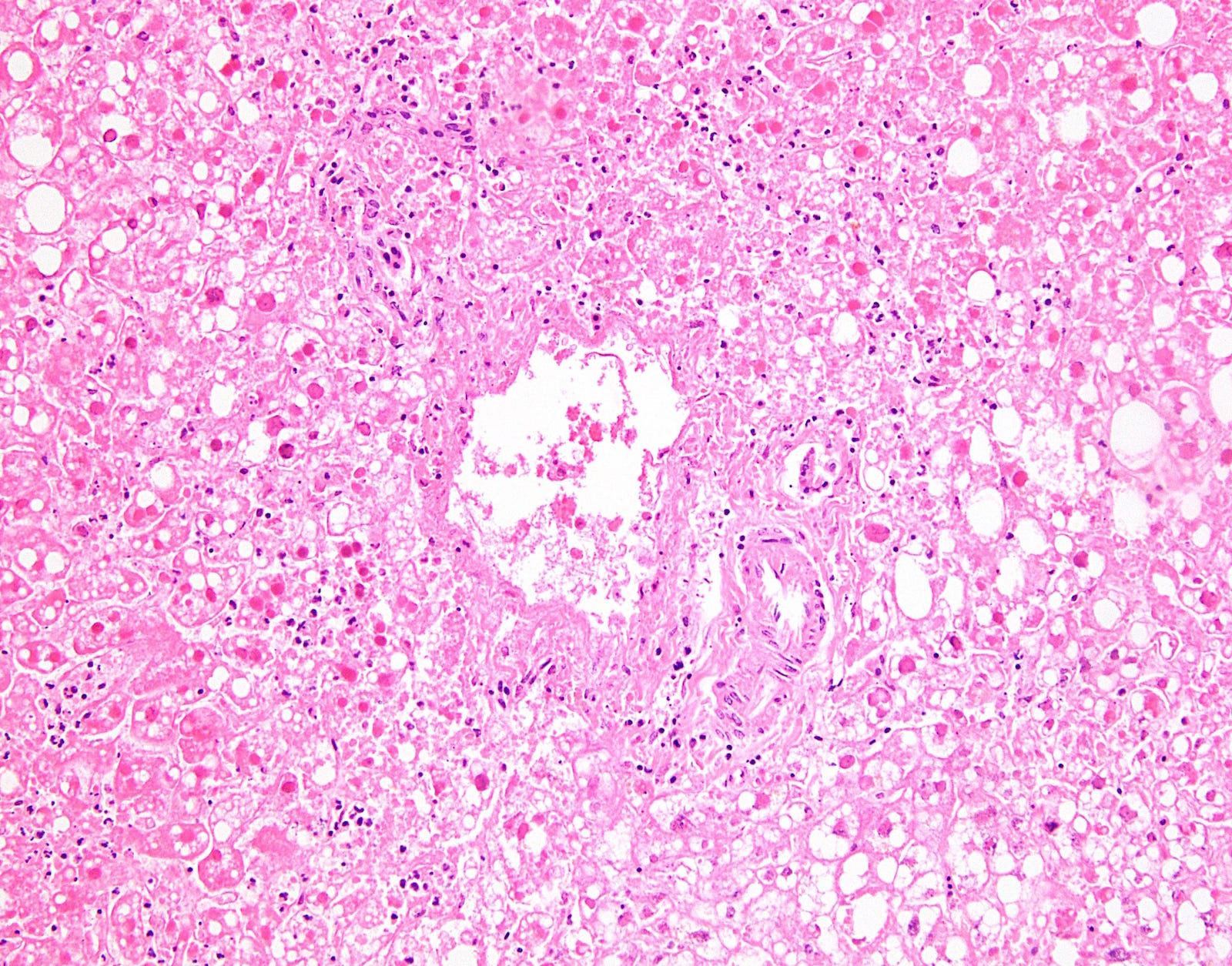
- Geographic (nonzonal) hemorrhagic necrosis
- Viable and nonviable areas distributed in a patchy, seemingly random fashion, sometimes with a clean separating border
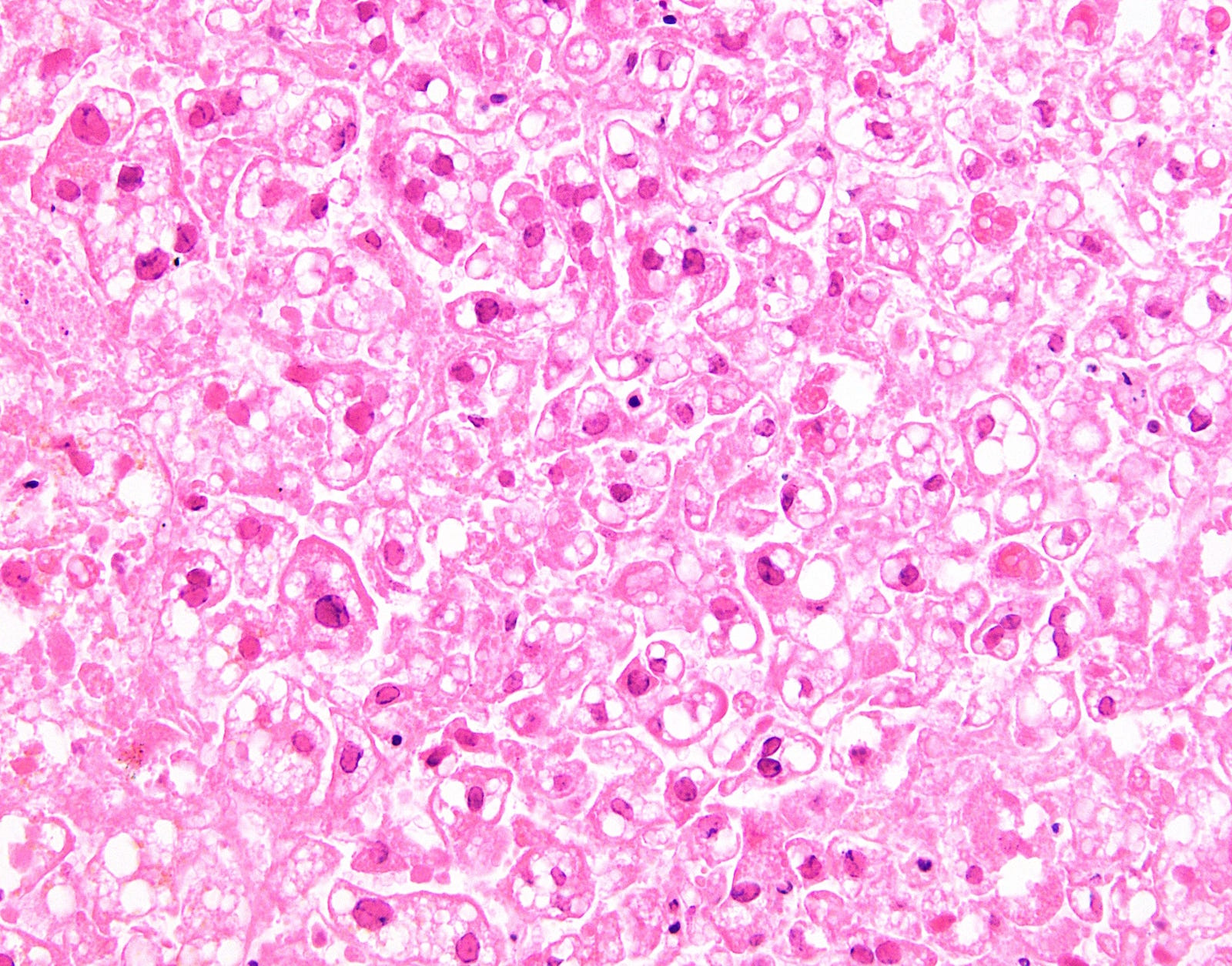
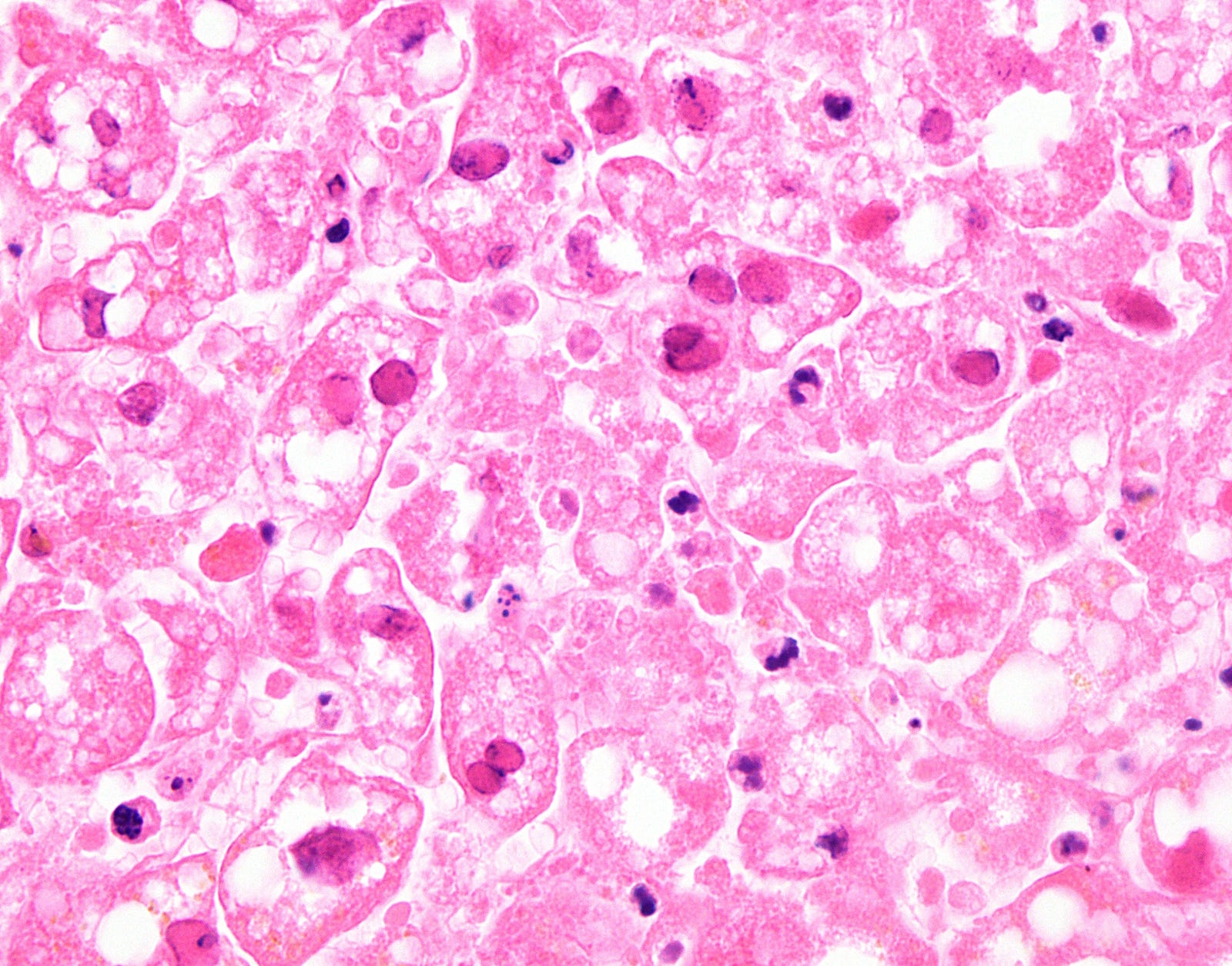
- Classic nuclear features of herpes infection (margination, multinucleation, molding) are seen in hepatocytes, though multinucleation is not always observed
Positive stains
- HSV
Sample pathology report
- Autopsy:
- Widespread liver necrosis consistent with herpetic hepatitis (see comment)
- Comment: Geographic (nonzonal) hemorrhagic necrosis of the liver is present, along with viral cytopathic effect in surviving hepatocytes. Immunohistochemistry for HSV1 is positive, confirming the diagnosis.
Differential diagnosis
- The differential diagnosis includes other causes of hepatic necrosis and other causes of viral cytopathic effect:
- Hypoperfusion (e.g., due to hypovolemic shock)
- Can cause zone 3 necrosis
- Medications that cause hepatic necrosis
- Acetaminophen causes zone 3 necrosis
- Unusual substances may primarily induce necrosis in other zones
- Viral hemorrhagic fever (e.g., yellow fever)
- Can cause zone 2 necrosis, possibly also with zone 2 necrosis
- Disseminated intravascular coagulation and eclampsia
- May cause zone 1 necrosis
- Cytomegalovirus
- Can cause prominent "owl's-eye" inclusions in hepatocytes, endothelial cells and biliary epithelium
- Easier to detect in immunocompromised patients
- Fulminant hepatic failure is not the typical presentation but can occur
- Adenovirus
- Close histologic mimicker of hepatic hepatitis
- Causes random zones of necrosis and viral cytopathic effect
- Involved hepatocytes have a basophilic, smudgy nucleus without any multinucleation
- Immunohistochemistry for adenovirus can distinguish adenovirus from herpes
- Herpes zoster virus
- Can cause same histologic picture in liver
- Generally only occurs in immunocompromised patients
- HSV immunostain is negative, but VZV staining is positive
- Measles
- May cause multinucleation without margination or molding
- Eosinophilic cytoplasmic inclusions may be detected
- Necrosis would be spotty
- Hypoperfusion (e.g., due to hypovolemic shock)
Board review style question #1
- Herpes simplex hepatitis causes necrosis of hepatocytes in what pattern?
- Nonzonal necrosis
- Zone 1 necrosis
- Zone 2 necrosis
- Zone 3 necrosis
Board review style answer #1