Table of Contents
Definition / general | Essential features | Terminology | ICD coding | Epidemiology | Sites | Pathophysiology | Etiology | Diagrams / tables | Clinical features | Diagnostic criteria | Laboratory | Case reports | Treatment | Gross description | Microscopic (histologic) description | Microscopic (histologic) images | Positive stains | Negative stains | Flow cytometry description | Molecular / cytogenetics description | Differential diagnosis | Additional references | Board review style question #1 | Board review style answer #1 | Board review style question #2 | Board review style answer #2Cite this page: Ozkaya N, Jaffe ES. Follicular neoplasia in situ. PathologyOutlines.com website. https://www.pathologyoutlines.com/topic/lymphomafollicularneoplasiainsitu.html. Accessed April 17th, 2024.
Definition / general
- In situ follicular neoplasia is a monoclonal proliferation of BCL2 positive B cells confined to follicle centers
- B cells are positive for t(14;18)(q32;q21) (Blood 2002;99:3376)
Essential features
- Histopathologic and immunohistochemical evaluation are essential
- Clinical and pathological evidence of usual follicular lymphoma is lacking in other sites
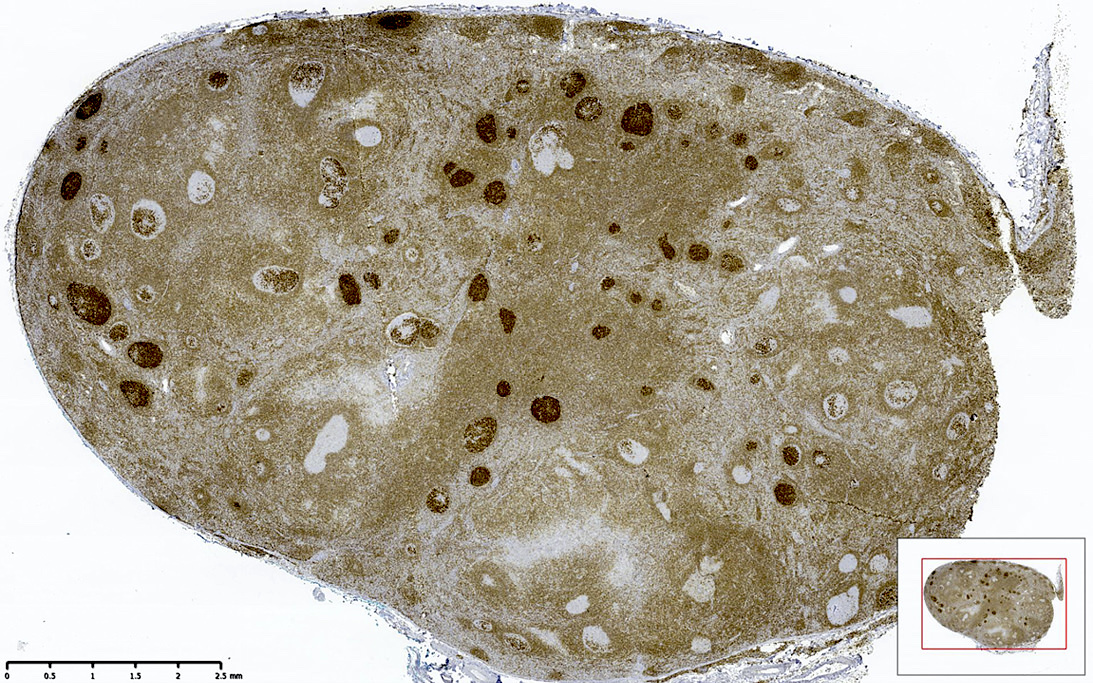
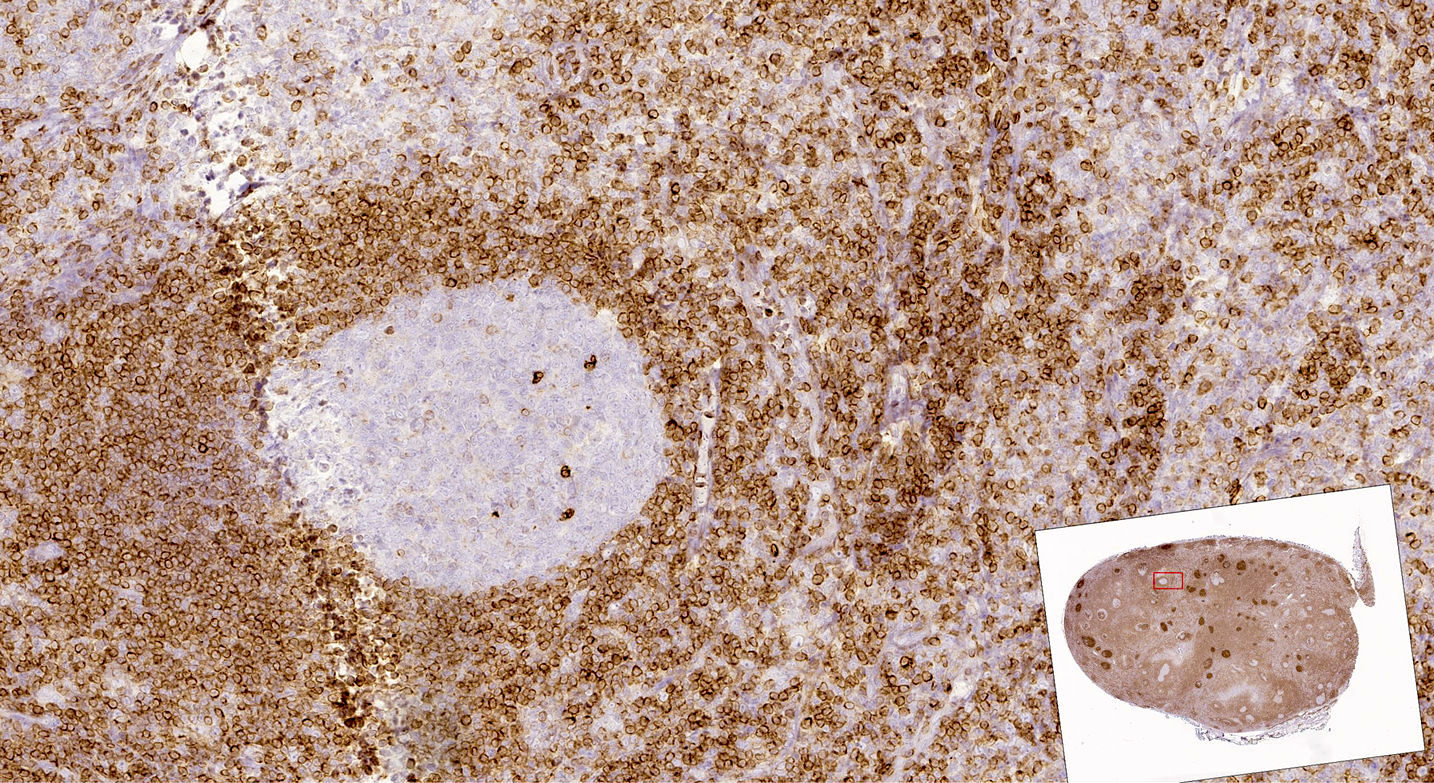
- BCL2 intensity in germinal centers is strong, stronger than adjacent mantle cuff
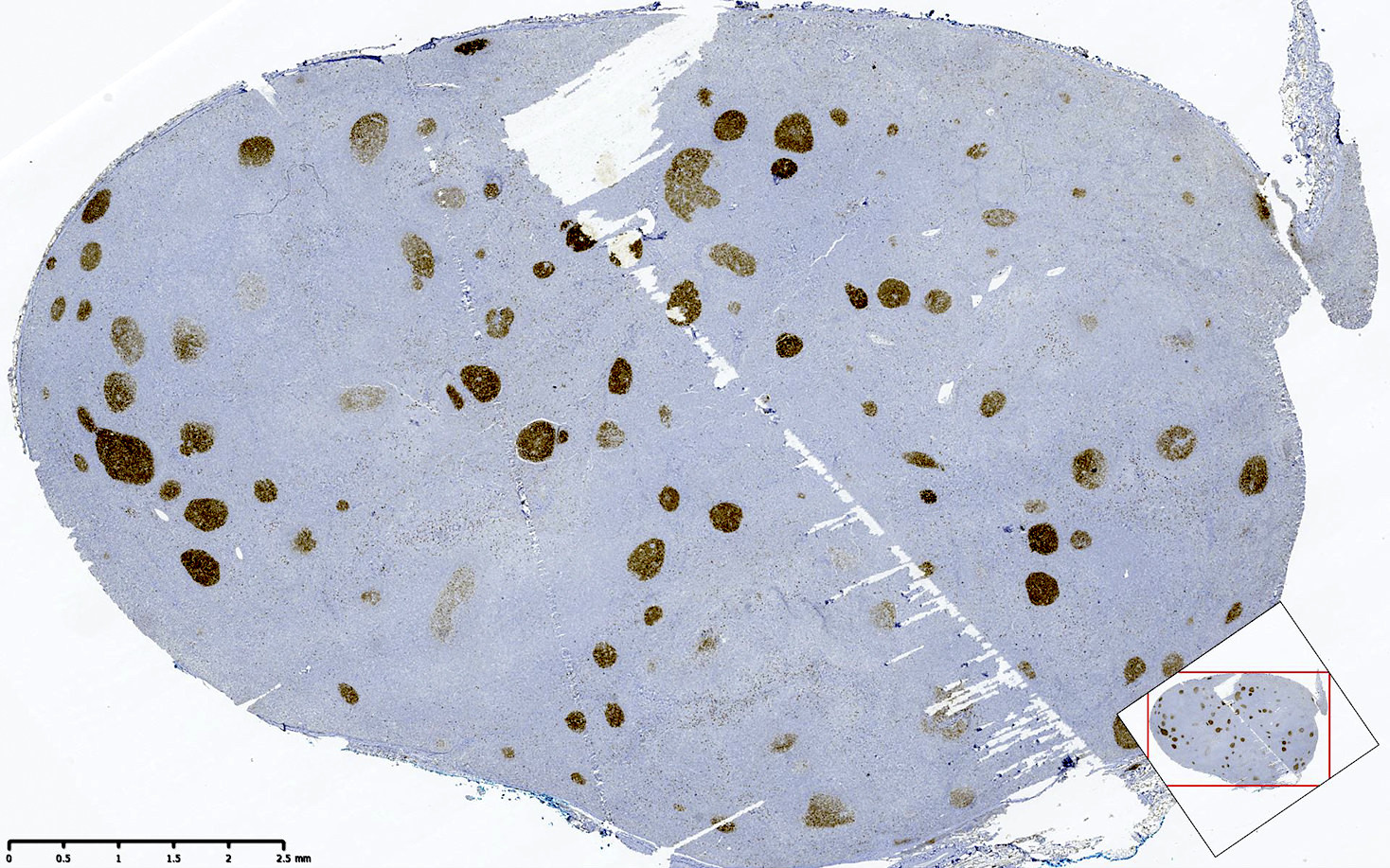
- CD10 is strongly positive
- Variable number of germinal centers may be involved
- Lymph node architecture is preserved
Terminology
- Formerly follicular lymphoma in situ
- "In situ follicular lymphoma" terminology is discouraged, because risk for clinically significant lymphoma is small
ICD coding
Epidemiology
- Detected in ~2 - 3% of randomly selected reactive lymph node biopsies by immunohistochemical screening for BCL2 (Histopathology 2011;59:139, Haematologica 2012;97:270, Am J Surg Pathol 2016;40:943)
- Exclusively found in adults
Sites
- Lymph node otherwise showing follicular hyperplasia
- May be seen in secondary lymphoid follicles of tonsil, spleen and lymphoid tissue in extranodal sites
Pathophysiology
- Precursor lesion of conventional follicular lymphoma but progresses to follicular lymphoma in fewer than 5% of cases
- B cells with BCL2 rearrangement within germinal centers
- Other than BCL2 rearrangement, low level of genetic aberrations is found
- Very early step in lymphomagenesis (Blood 2018 Nov 6 [Epub ahead of print])
Etiology
- High environmental exposure to pesticides and herbicides associated with increase in cells carrying t(14;18)(q32;q21) (IGH / BCL2) translocation in the peripheral blood
Clinical features
- Always an incidental finding
- Risk for clinically significant follicular lymphoma less than 5%
- Low incidence of other lymphoma subtypes in affected patients, mainly mantle cell lymphoma, chronic lymphocytic leukemia, marginal zone lymphoma and diffuse large B cell lymphoma
Diagnostic criteria
- BCL2 and CD10 strongly positive in lesional cells
- Neoplastic cells confined to follicle centers of secondary follicles
- Lymph node architecture is preserved
- Lymph nodes may show other pathology or involvement by unrelated lymphoma, usually of B cell lineage
Laboratory
- Low levels of B cells with the BCL2 rearrangement in the peripheral blood may be found by PCR
- In blood, referred to as follicular lymphoma-like B cells (Haematologica 2013;98:1571)
Case reports
- 60 year old woman and 69 year old man (Am J Hematol 2011;86:E66)
- 63 year old woman with two nonhematopoietic neoplasms (Leuk Lymphoma 2016;57:2917)
- 78 year old man with concomitant follicular lymphoma, grade 1 - 2 (CD10+, BCL2-) (Blood 2011;118:3442)
- 84 year old woman with composite follicular lymphoma and mantle cell lymphoma each with an in situ component (Am J Clin Pathol 2011;136:481)
Treatment
- Clinical evaluation for follicular lymphoma at other sites recommended at diagnosis
- No treatment indicated if only in situ follicular neoplasia is found
Gross description
- No gross finding is evident
- Involved lymph node may be enlarged secondary to lymphoid hyperplasia or other pathology
Microscopic (histologic) description
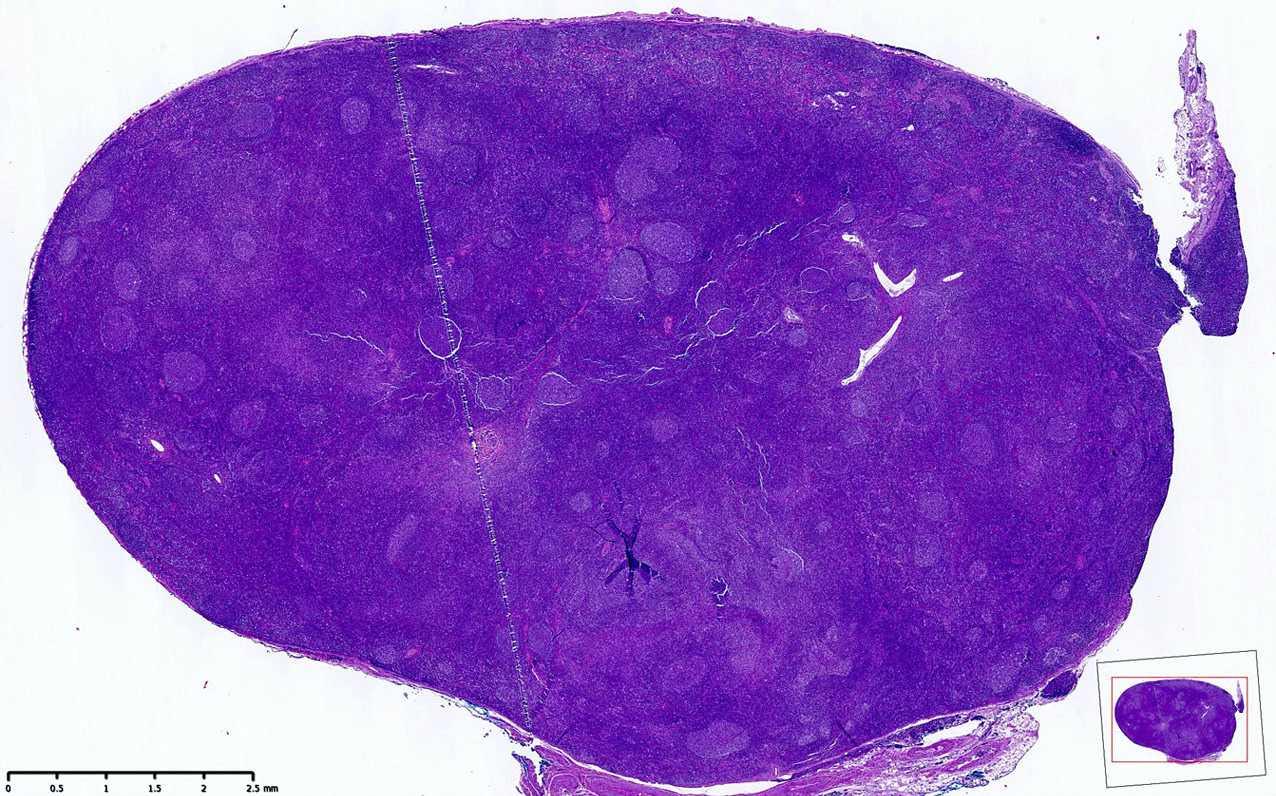
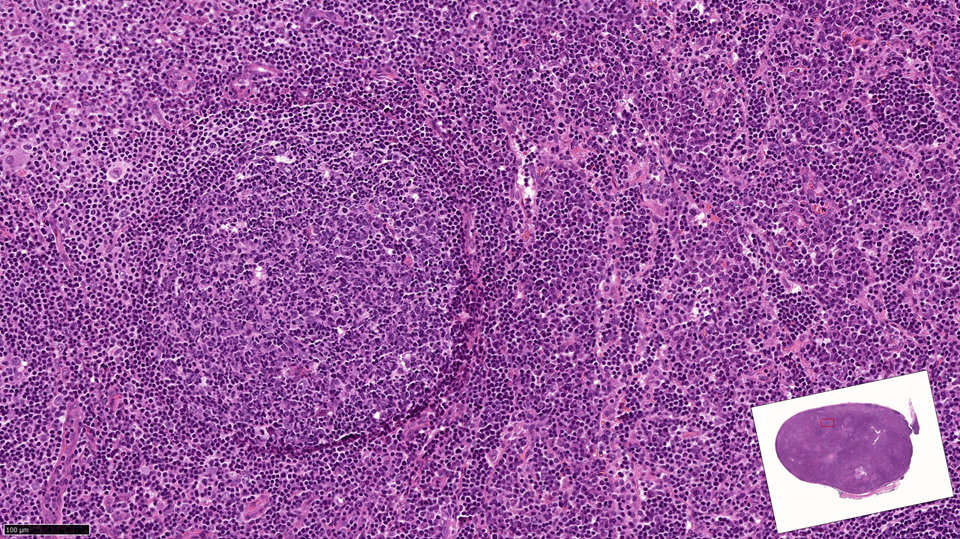
- Lesion generally not evident on routine H&E stained sections
- Lymph node architecture is intact
- Involved follicles are generally normal in size
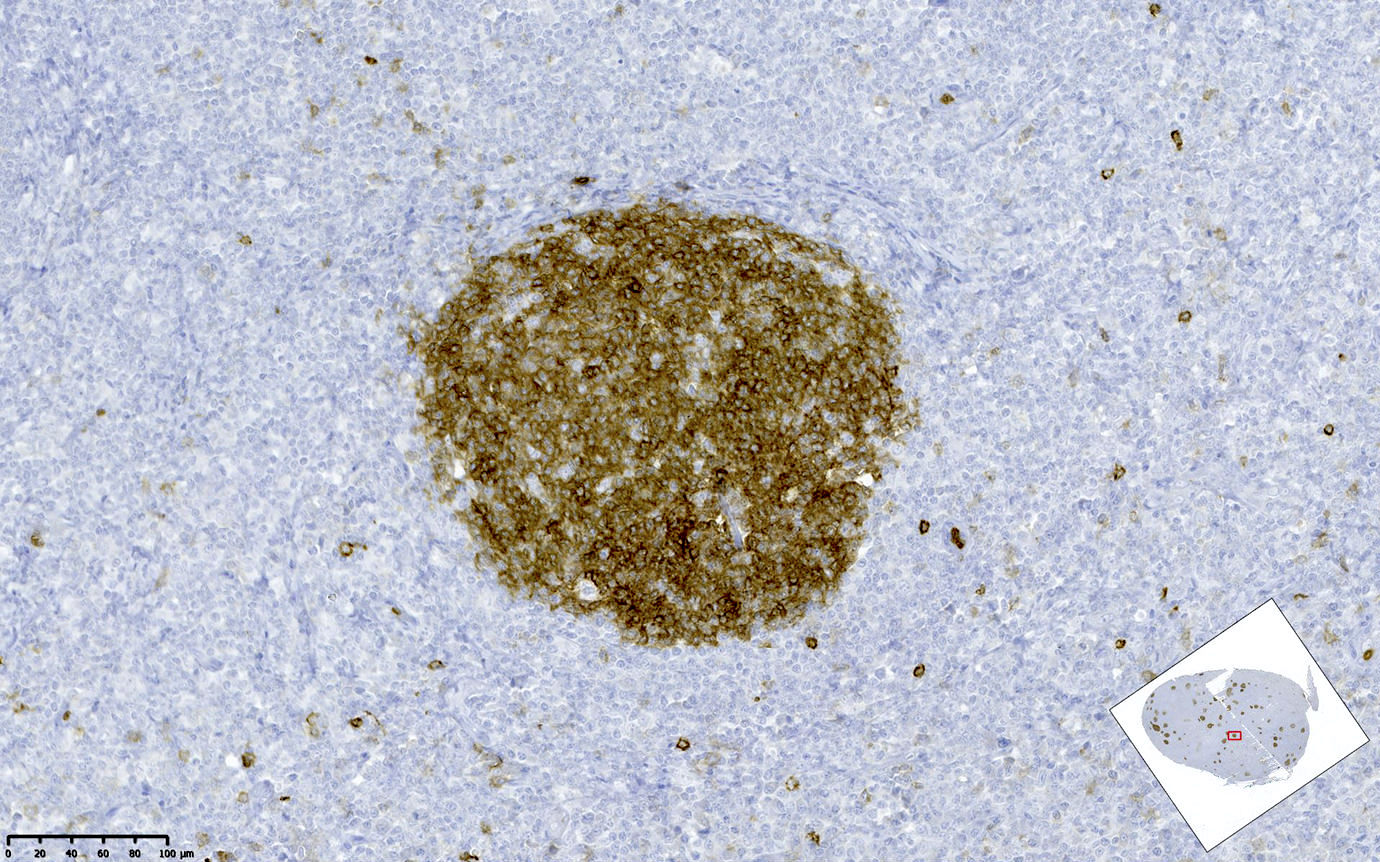
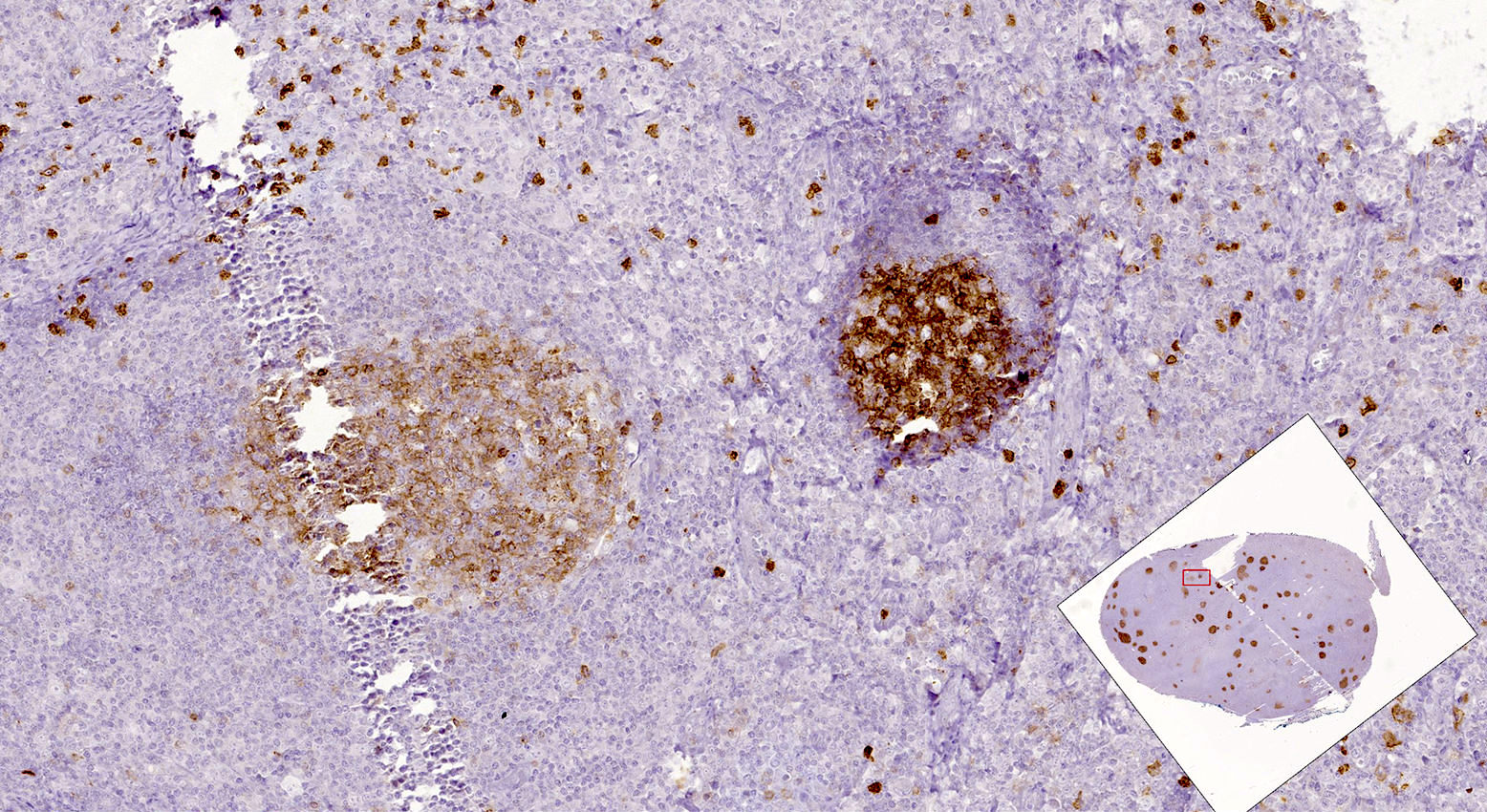
- The neoplastic cells (BCL2 strong+, CD10 strong+) are exclusively centrocytes, confined to the follicle centers
- Individual germinal centers show varying degrees of involvement
- By definition, no interfollicular infiltration is seen
- Involved follicles show low proliferation fraction with Ki67
Microscopic (histologic) images
Positive stains
Negative stains
Flow cytometry description
- Uncommon detection of minor population of light chain restricted B cells that coexpress CD10 (Haematologica 2013;98:1571)
Molecular / cytogenetics description
- t(14;18)(q32;q21) (IGH / BCL2) translocation
- Frequent mutations in CREBBP
- EZH2, KMT2D, TNFRSF14, EP300 mutations have been identified in a small subset of cases (Leukemia 2014;28:1103, Blood 2018 Nov 6 [Epub ahead of print])
Differential diagnosis
- Reactive follicular hyperplasia: reactive follicles are negative for BCL2, show polarization and have a high proliferation index
- Partial involvement by follicular lymphoma: BCL2 and CD10 immunostaining more variable in intensity; follicles expanded on H&E with some distortion of lymph node architecture
Additional references
Board review style question #1
Which of the following is characteristic of in situ follicular neoplasia?
- Bone marrow involvement is common at diagnosis
- Common in childhood
- Lymphocytosis is a common finding
- Tend to involve extranodal sites
- Typically an incidental finding
Board review style answer #1
Board review style question #2
Which of the following is true about in situ follicular neoplasia?
- Composed exclusively of centrocytes
- High mitotic rate
- Interfollicular infiltration of neoplastic B cells is common
- Positive for BCL6 rearrangement
- Positive for CCND1 rearrangement
Board review style answer #2
A. In situ follicular neoplasia has a monomorphic appearance and is composed exclusively of centrocytes.
Comment here
Reference: Follicular neoplasia in situ
Comment here
Reference: Follicular neoplasia in situ