Table of Contents
Definition / general | Essential features | Terminology | ICD coding | Epidemiology | Sites | Pathophysiology / etiology | Diagrams / tables | Clinical features | Diagnosis | Laboratory | Prognostic factors | Case reports | Treatment | Clinical images | Gross description | Microscopic (histologic) description | Microscopic (histologic) images | Immunofluorescence description | Immunofluorescence images | Videos | Sample pathology report | Differential diagnosis | Board review style question #1 | Board review style answer #1 | Board review style question #2 | Board review style answer #2 | Board review style question #3 | Board review style answer #3Cite this page: Smith MH. Pemphigoid. PathologyOutlines.com website. https://www.pathologyoutlines.com/topic/oralcavitypemphigoid.html. Accessed April 25th, 2024.
Definition / general
- Chronic, immune mediated, subepithelial blistering disease that predominantly affects mucous membranes
- Autoantibodies directed at components of the basement membrane zone
Essential features
- Second most common immune mediated, subepithelial blistering disease, after bullous pemphigoid (J Invest Dermatol 2016;136:2495)
- Most often presents in the oral cavity
- Autoimmune (IgG, IgA or C3) attack of hemidesmosomes / basement membrane zone
- May affect the oral cavity, conjunctiva, subglottis, larynx, nose, esophagus, penis, vulva, anal mucosa or skin
Terminology
- Mucous membrane pemphigoid
- Benign mucous membrane pemphigoid (BMMP)
- Cicatricial pemphigoid
- Mucosal pemphigoid
ICD coding
- ICD-10: L12.1 - benign mucous membrane pemphigoid
Epidemiology
- Wide age range; predilection for middle aged to older adults
- Slight female predominance
Sites
- Affects the oral cavity (96.7%), conjunctiva (42.2%), subglottis, larynx, nose, esophagus, skin or anogenital regions (27.9%) (J Eur Acad Dermatol Venereol 2016;30:72)
- Oral cavity is the most commonly affected site
- Gingiva > buccal mucosa > palate > alveolar ridge > tongue > lower lip
Pathophysiology / etiology
- Likely an autoantibody induced and complement mediated sequestration of leukocytes (predominantly neutrophils) with release of cytokines and leukocyte enzymes leading to detachment of epithelium at the basement membrane zone (Br J Oral Maxillofac Surg 2008;46:358)
- Combination of IgG (94.6%), C3 (85.8%) or IgA (16.5%) autoantibodies directed against epithelial basement membrane zone components BP180, BP230, alpha 6 integrin, beta 4 integrin or laminin 332 (laminin-5) (J Eur Acad Dermatol Venereol 2016;30:72, Acta Derm Venereol 2004;84:381)
- BP180 is the most frequently affected target, in ~75% (Br J Dermatol 2006;154:90)
- Oral only subset: α6 integrin target antigen (Oral Surg Oral Med Oral Pathol Oral Radiol Endod 1998;85:37)
- Ocular only subset: β4 integrin (J Invest Dermatol 2006;126:2631)
- Mechanism that links the binding of autoantibodies to the basement membrane zone and the subsequent scarring process is unknown (Clin Dermatol 2012;30:34)
- Association with HLA-DQB1*0301 (Br J Dermatol 2001;145:805, Br J Dermatol 2001;145:406, Br J Oral Maxillofac Surg 2008;46:358)
- Emerging association with anti-PDL1 medications (Front Med (Lausanne) 2018;5:268, J Immunother 2019;42:359, J Eur Acad Dermatol Venereol 2019 Oct 29 [Epub ahead of print], Br J Dermatol 2018;179:993)
Clinical features
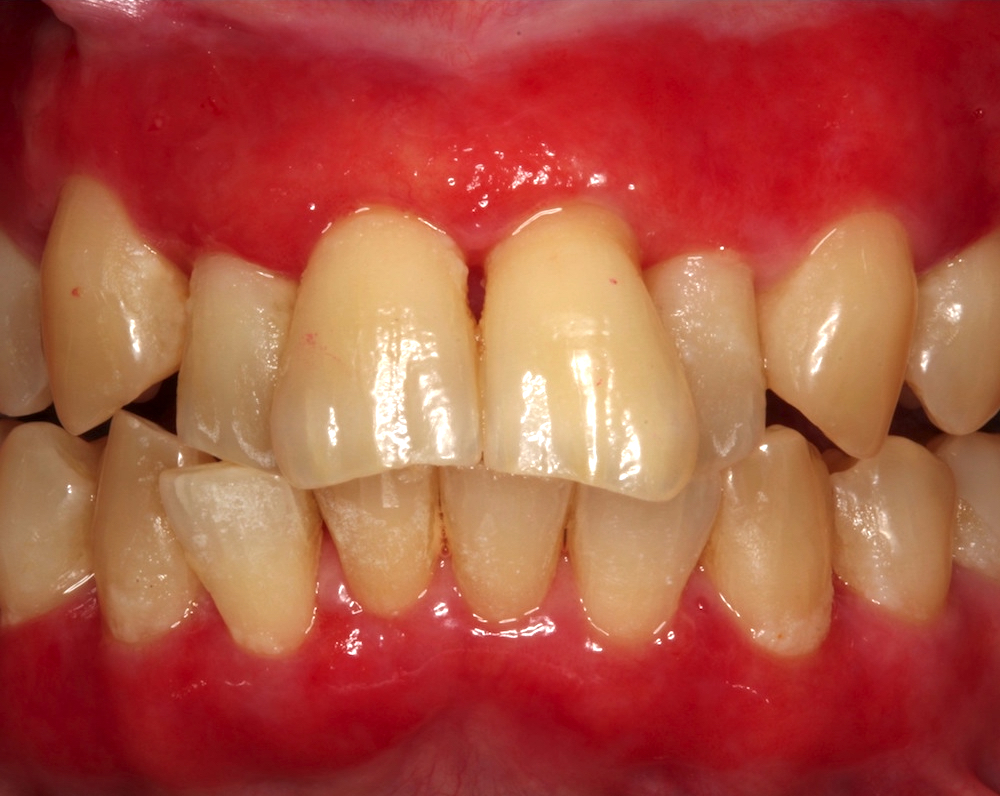
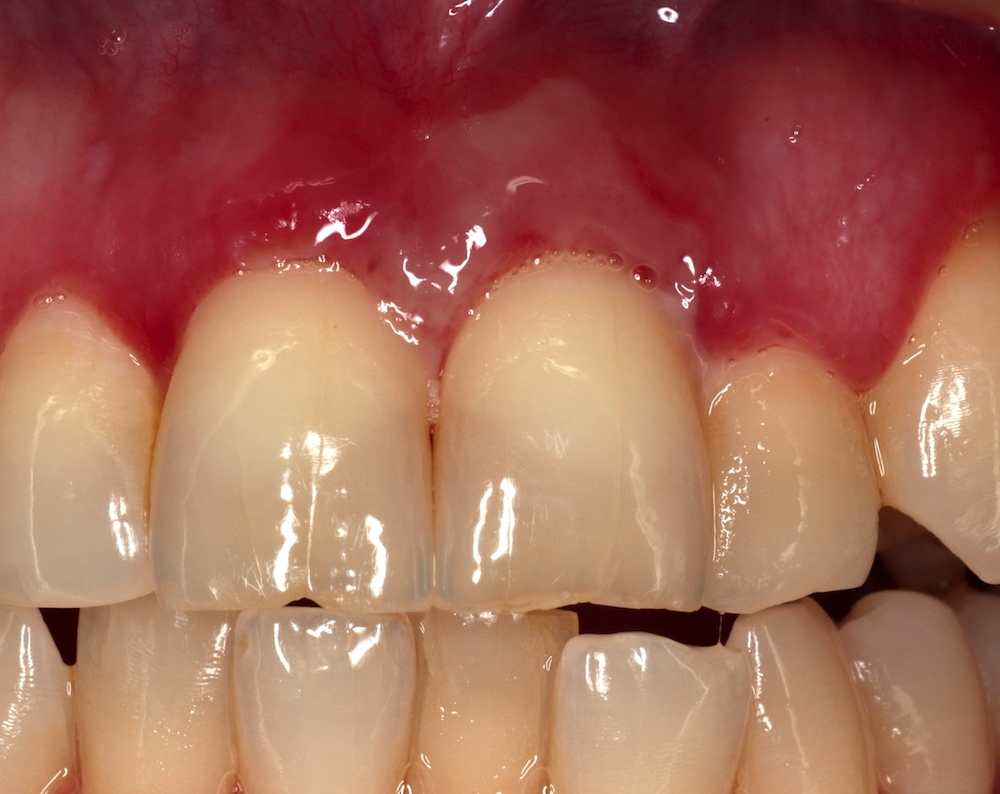
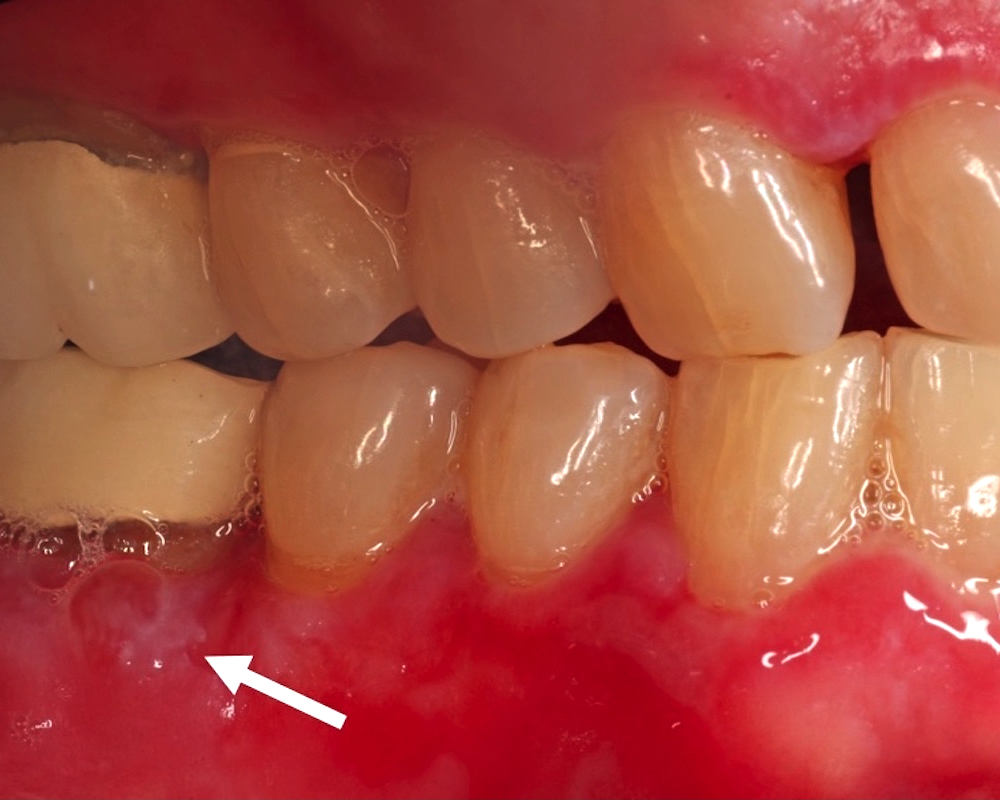
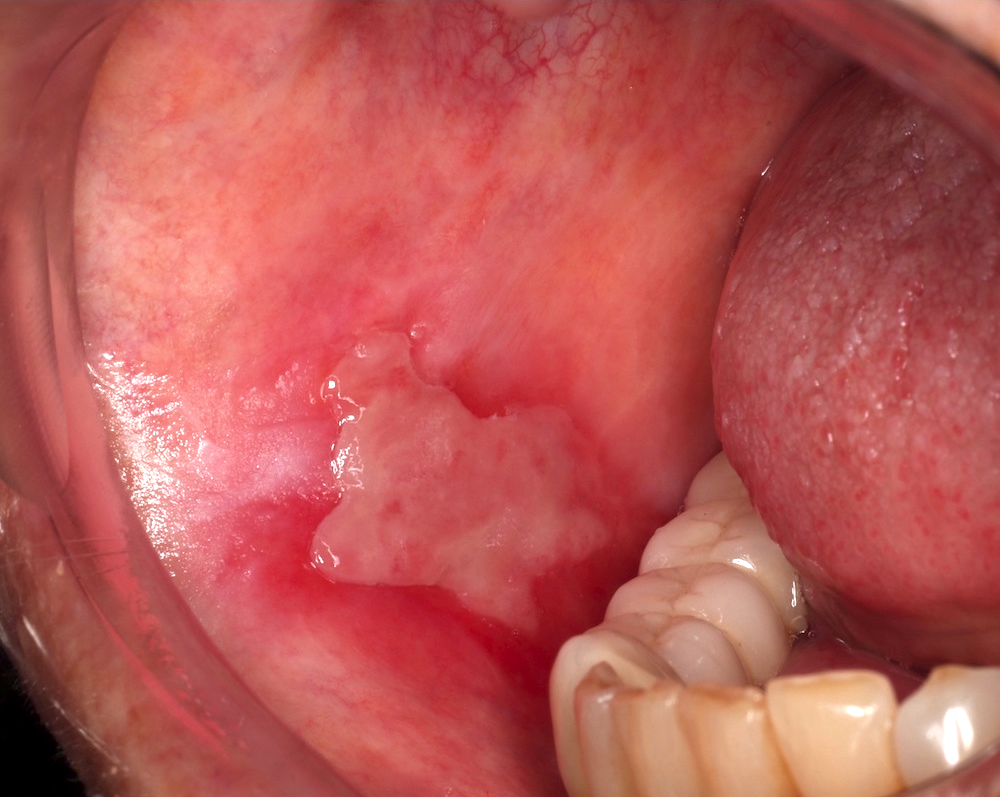
- General: erythematous or ulcerated mucous membranes +/- blood blister formation (+ Nikolsky sign); periodic episodes leading to potential scarring (Br J Oral Maxillofac Surg 2008;46:358)
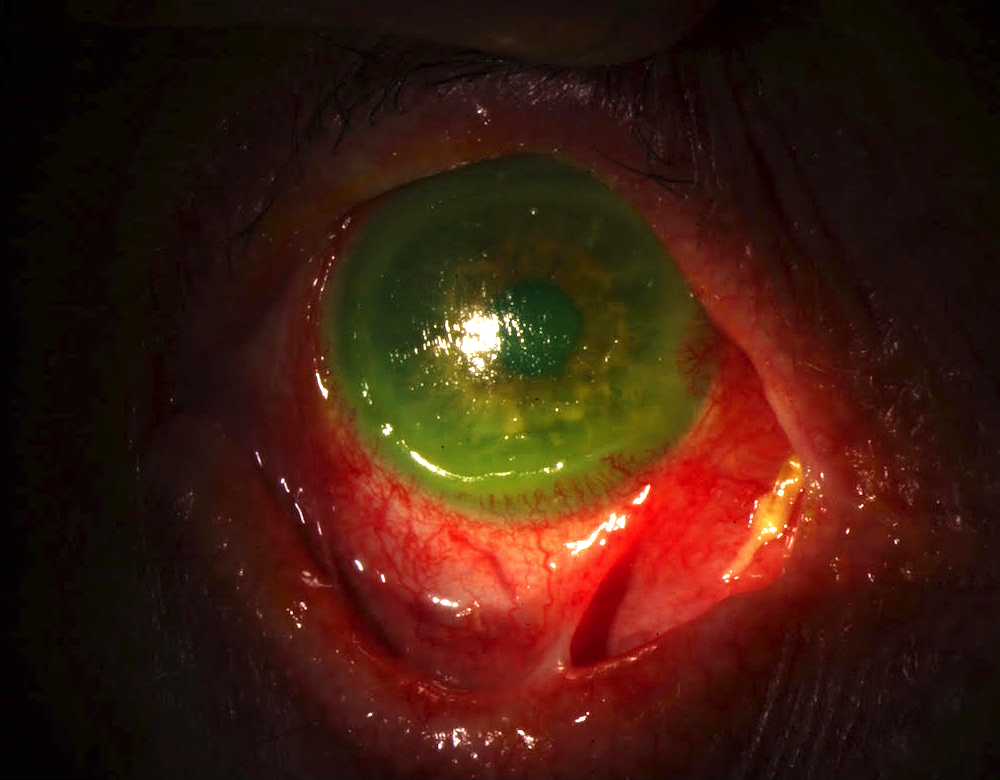
- Ocular: scarring on the conjunctiva may produce a symblepharon or blindness
- Oropharynx: dyspnea, hoarseness
- Esophagus: difficulty swallowing or bleeding; stenosis
- Nose: nosebleeds
- Skin: rare; vesicles / bullae
- Laryngeal involvement can lead to airway loss
Diagnosis
- Diagnosis made on routine H&E histological examination and biopsy for direct immunofluorescence
- Direct immunofluorescence is gold standard for diagnosis
- Cases may be followed with indirect immunofluorescence, immunoblotting or enzyme-linked immunosorbent assay (ELISA) testing
- 2015 consensus group created a disease area index table to standardize diagnosis (J Am Acad Dermatol 2015;72:168)
Laboratory
- IgG autoantibodies against basement membrane zone components (BP180, BP230, alpha 6 integrin, beta 4 integrin or laminin 332) detected
- IgG titers correlate with disease severity (Br J Dermatol 1999;140:645)
- Laminin-332 is detected in up to 20% of patients (J Invest Dermatol 2001;116:348, Br J Dermatol 2019;180:149)
Prognostic factors
- Detection of both IgG and IgA autoantibodies associated with more severe disease (Br J Dermatol 1998;138:602)
- Laminin-332 is associated with more severe disease and solid organ tumors in up to 30% (J Invest Dermatol 2001;116:348, Br J Dermatol 2019;180:149)
Case reports
- 58 year old man presents with painful mouth sores, cutaneous blisters, paronychia and onychomadesis (BMC Dermatol 2019;19:3)
- 83 year old patient presenting with oral blisters and erosions after taking pembrolizumab (Front Med (Lausanne) 2018;5:268)
Treatment
- Mild-to-moderate disease:
- Topical therapies, including betamethasone, fluticasone propionate or clobetasol propionate
- Dapsone (Br J Oral Maxillofac Surg 2008;46:358) or sulfapyridine
- Moderate-to-severe disease:
- Mycophenolate mofetil, azathioprine, sulfa drug or prednisolone
- Severe, recalcitrant disease:
- Pulsed IV cyclophosphamide, IV immunoglobulin and rituximab (Clin Exp Dermatol 2019;44:732)
- Rituximab (anti-CD20 therapy) in combination with conventional immunosuppressive therapy leads to more rapid and sustained disease control with fewer potential adverse events (J Am Acad Dermatol 2016;74:835)
- Encourage excellent oral hygiene habits and regular ophthalmologic examinations
Clinical images
Gross description
- Thin wedge of white-tan surface epithelium with underlying tan-brown connective tissue
- Epithelium occasionally separated from underlying connective tissue
Microscopic (histologic) description
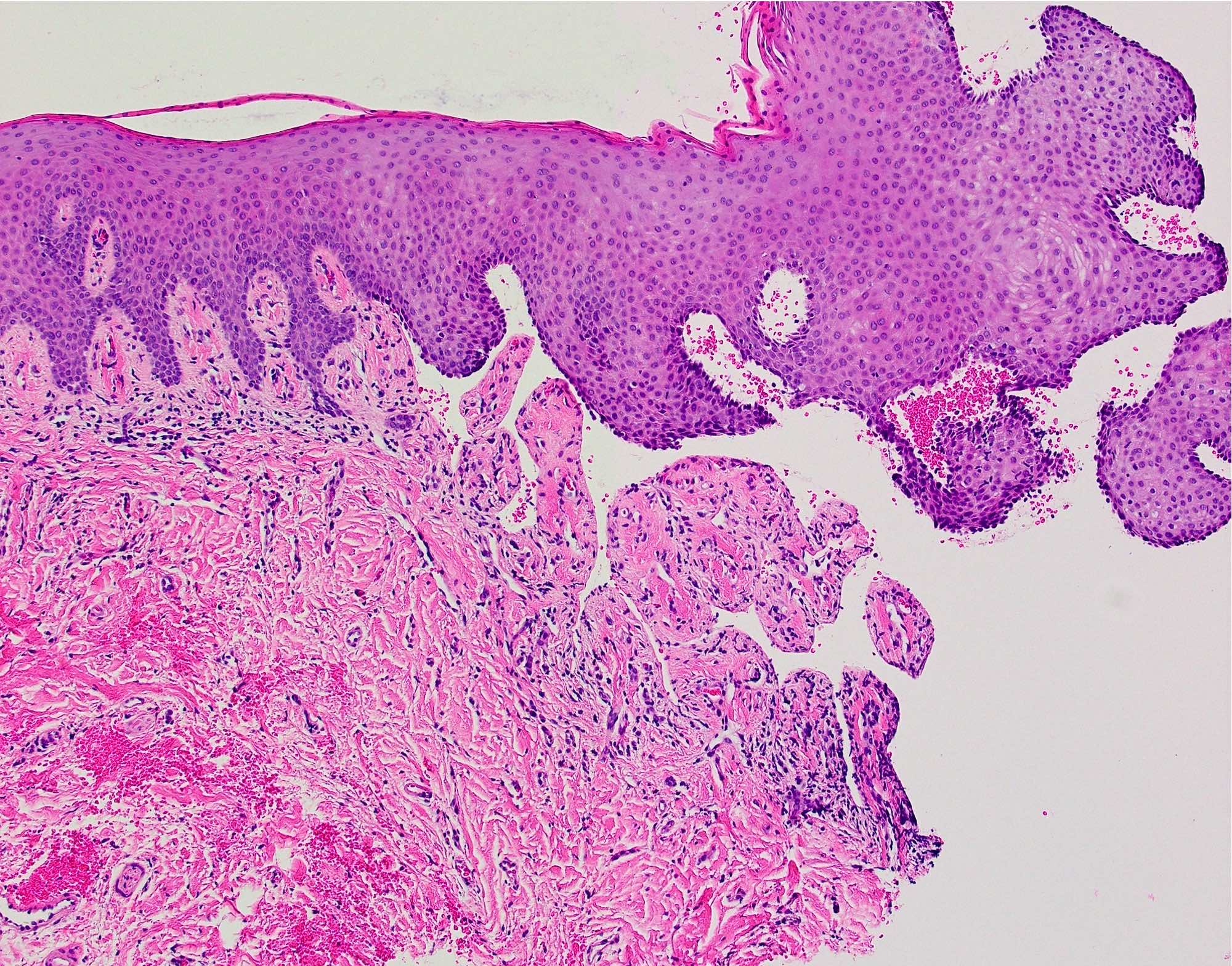
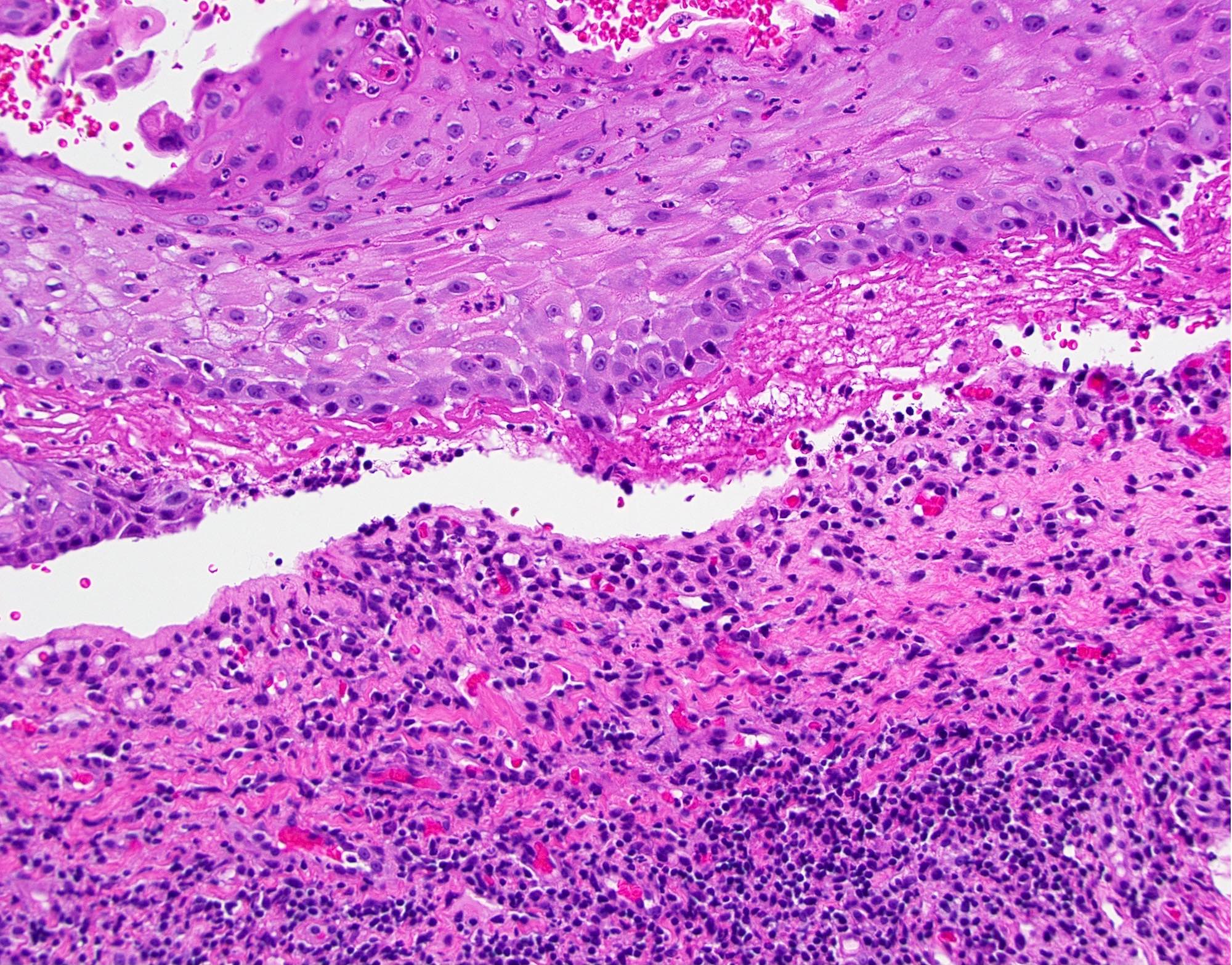
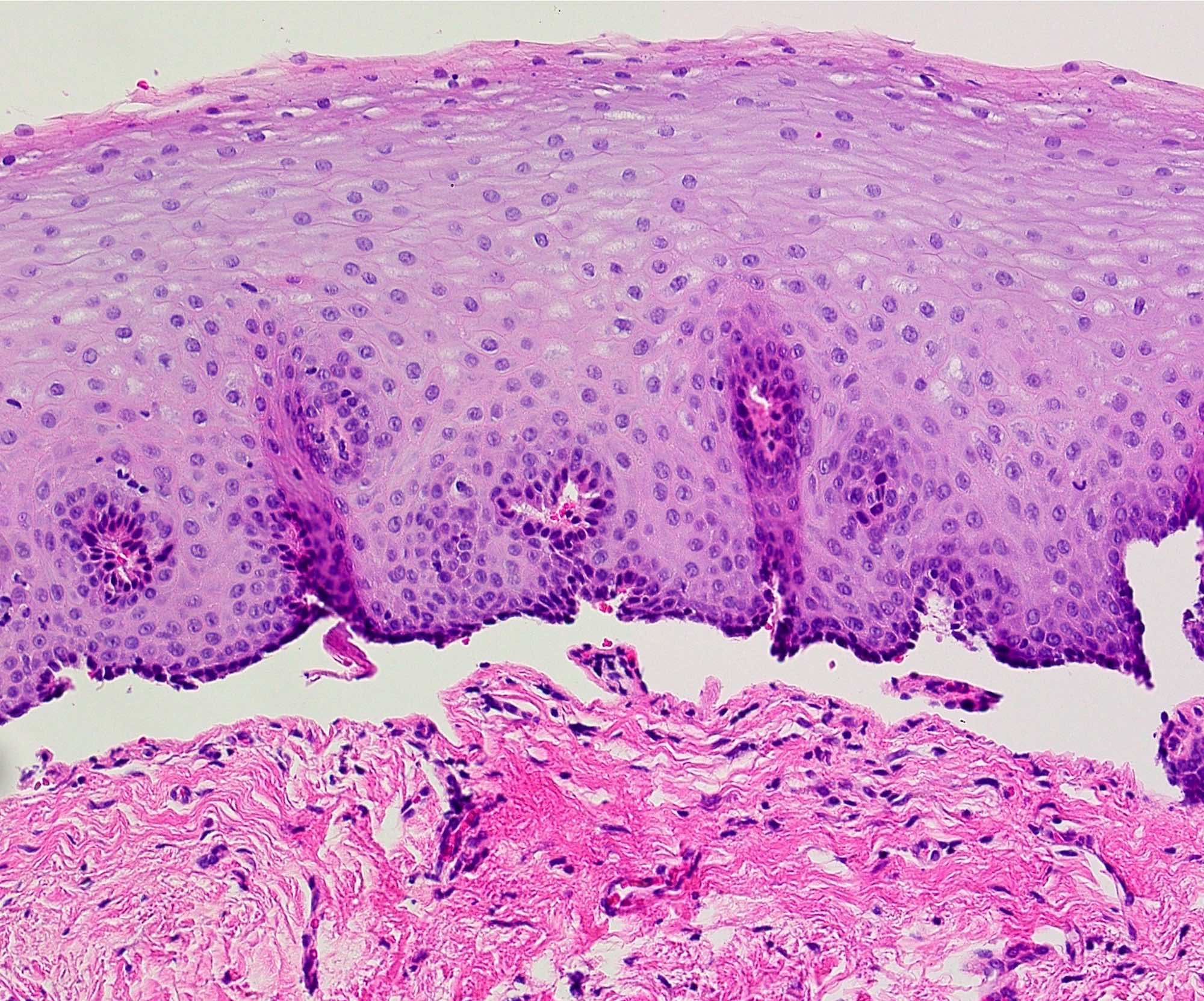
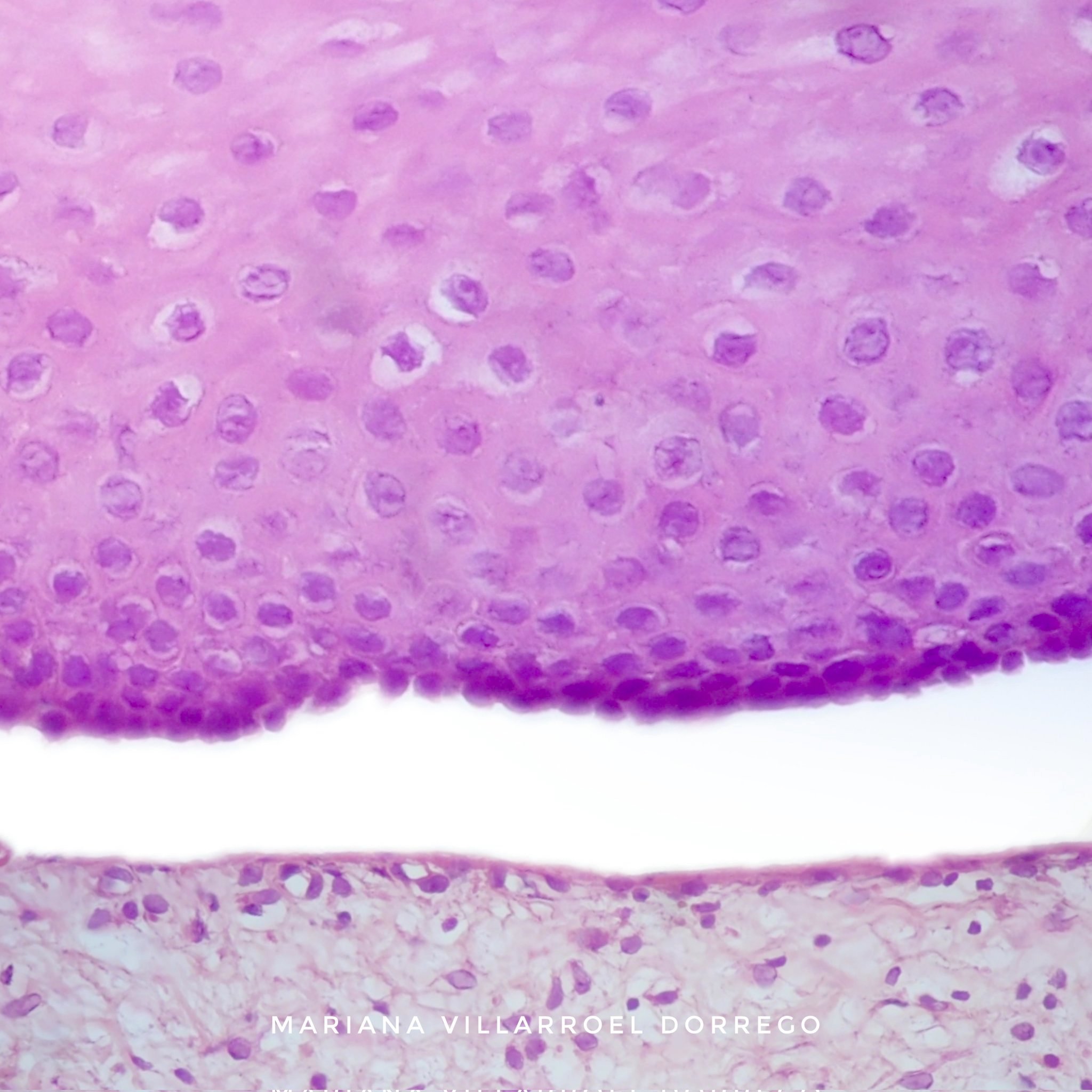
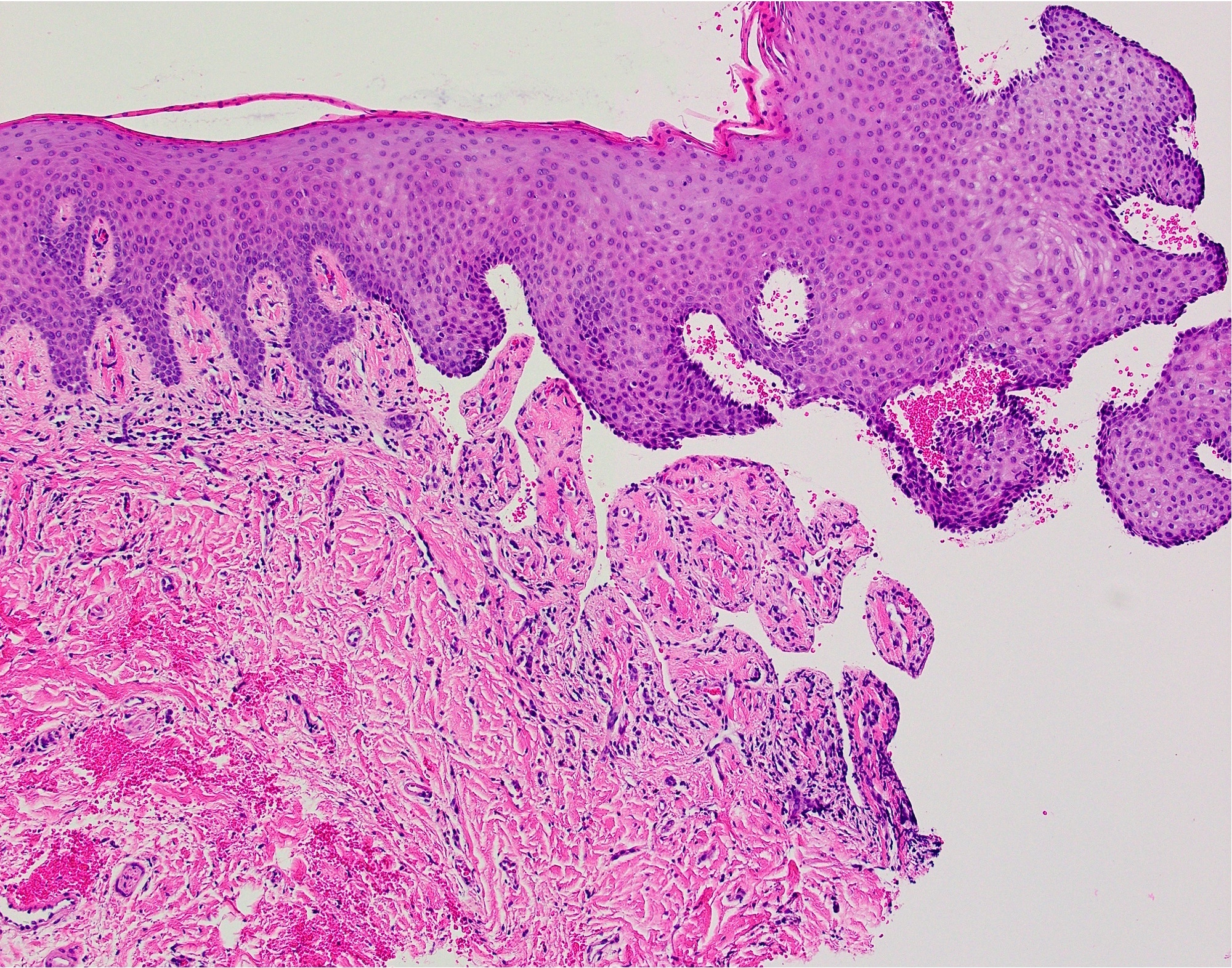
- Surface epithelium cleanly detached from the underlying connective tissue at the point of the basement membrane zone
- Superficial lamina propria contains a variable amount of inflammation that may contain lymphocytes, eosinophils and neutrophils (Br J Oral Maxillofac Surg 2008;46:358)
- Aggregates of erythrocytes may be present in area of bullae formation
Microscopic (histologic) images
Immunofluorescence description
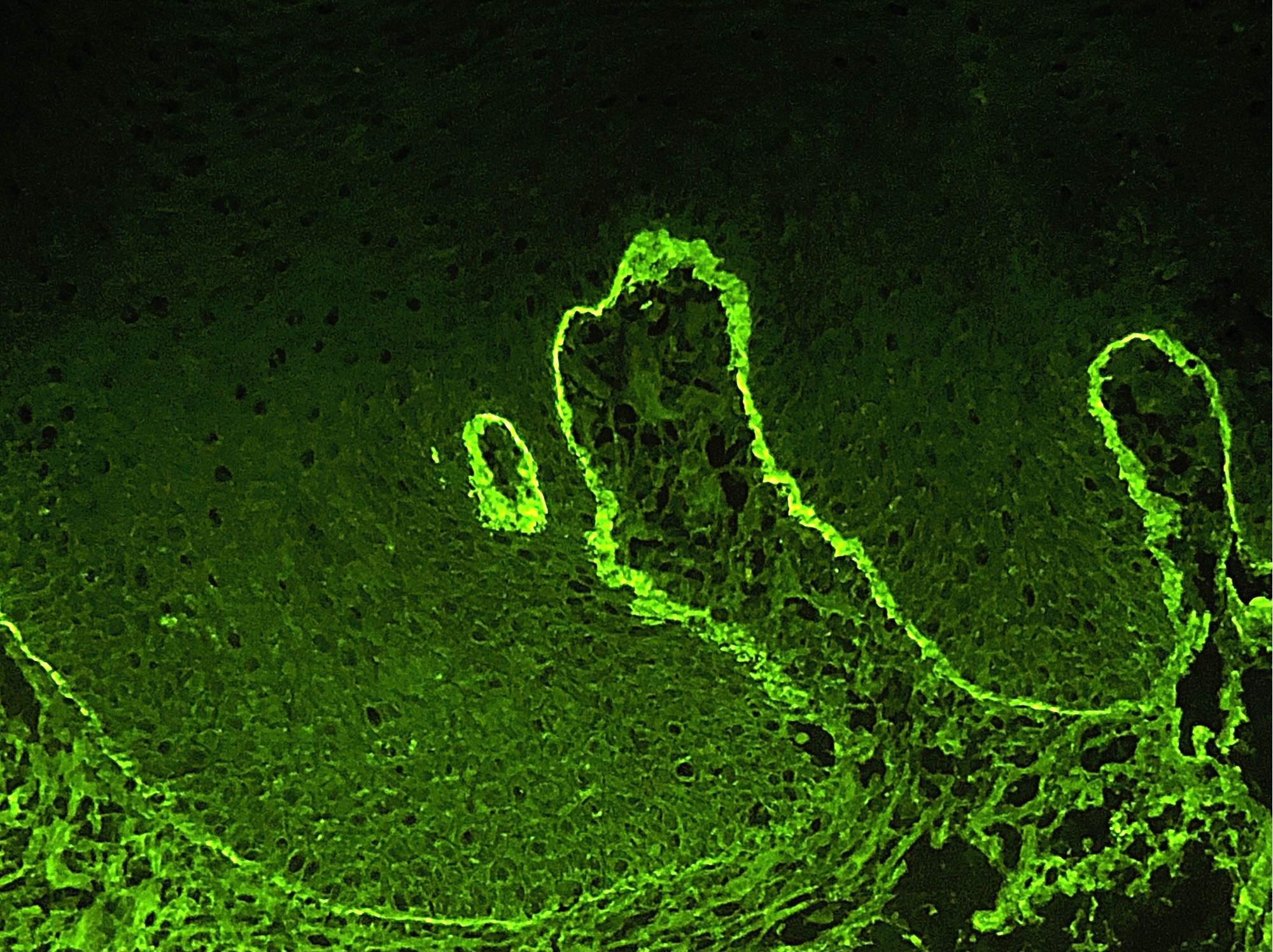
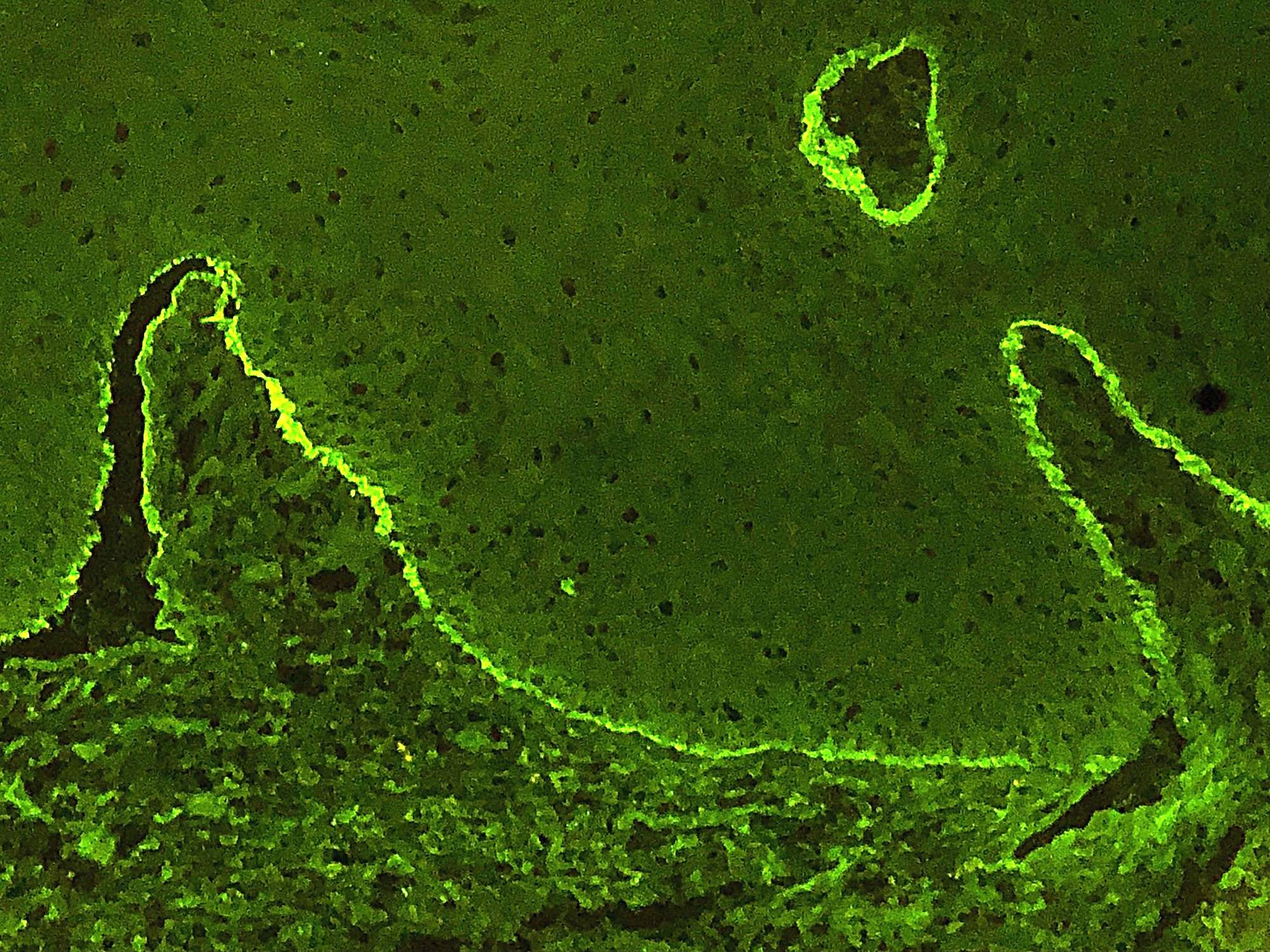
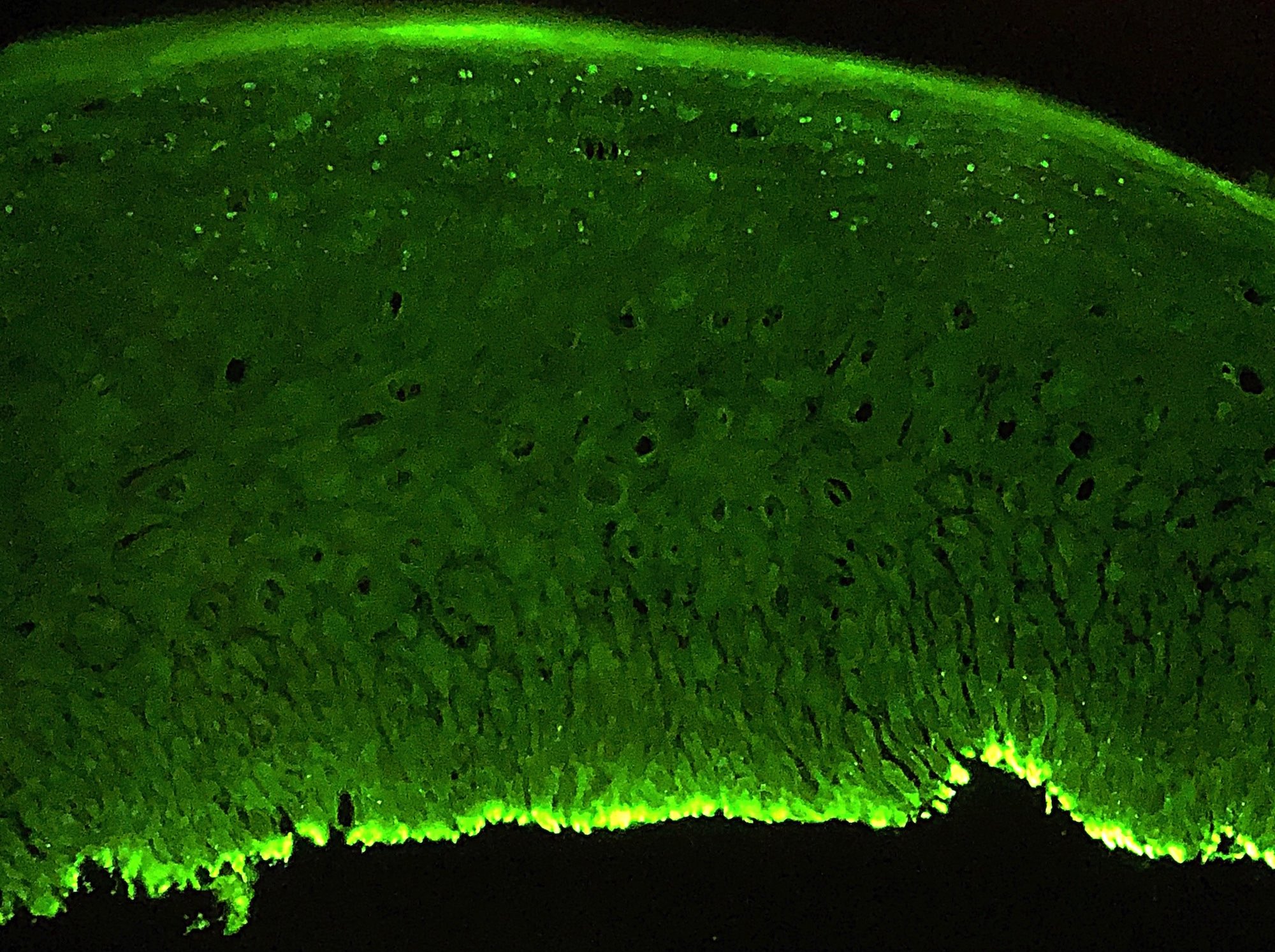
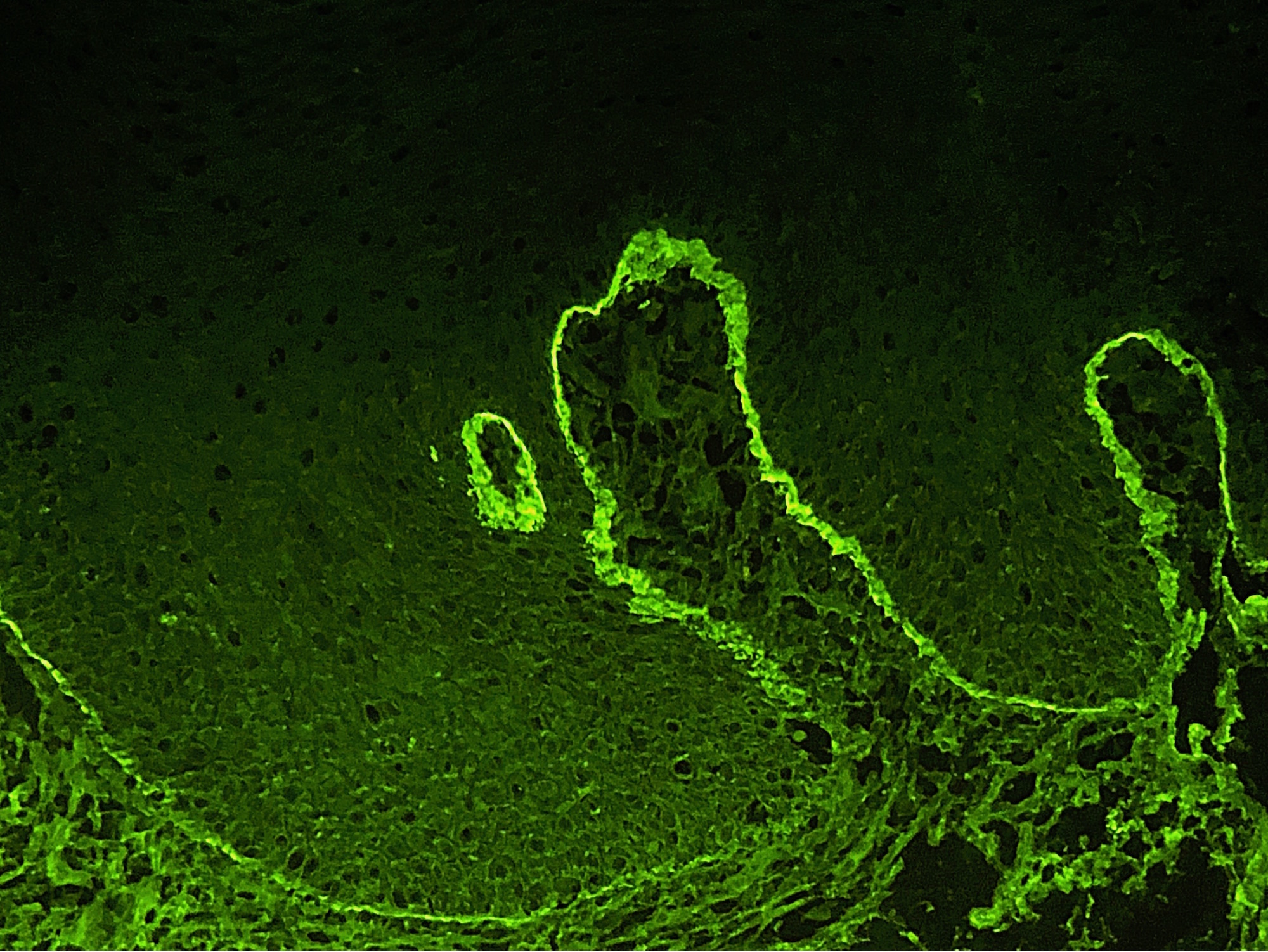
- Direct immunofluorescence (DIF): linear deposits of IgG, IgA or C3 along the basement membrane zone (Br J Oral Maxillofac Surg 2008;46:358)
- Indirect immunofluorescence (IIF): IgG autoantibodies against the basement membrane zone with known target antigens including BP180, BP230, alpha 6 integrin, beta 4 integrin or laminin 332 (laminin-5)
Videos
Clinical, histology, laboratory findings with discussion on pathophysiology
Sample pathology report
- Buccal gingiva, incisional biopsy:
- Subepithelial vesiculo-erosive condition consistent with benign mucous membrane pemphigoid (see comment)
- Comment: On H&E, there is a clean separation of the superficial stratified squamous epithelium from the underlying connective tissue at the layer of the basement membrane zone. On direct immunofluorescence, a shaggy and linear deposition of IgG, C3 and IgA is present in the basement membrane zone.
Differential diagnosis
- Bullous pemphigoid (BP)
- Most common immune mediated, subepithelial blistering disease
- Widespread skin lesions
- Persistent mucosal lesions are not seen
- Propensity to scar is less frequent
- Infrequent in the oral cavity
- Pemphigus vulgaris
- Autoimmune bullous disease directed against desmosomes
- Skin lesions heal without scarring
- Buccal mucosa > palate > tongue > labial mucosa > gingiva
- Suprabasilar clefting with acantholysis
- Direct immunofluorescence shows intracellular IgG and C3 staining
- Enzyme-linked immunosorbent assay demonstrates antibodies directed against desmoglein 1 and 3
- Paraneoplastic pemphigus
- Autoimmune blistering condition that indicates an underlying benign or malignant disease
- Patient may be unwell at time of diagnosis
- Intraepidermal-acantholytic bullae
- Direct immunofluorescence may demonstrate intracellular or basement membrane zone IgG and C3 staining
- Immunoblotting reveals antibodies to desmoglein 3 (Dsg3), BP230, envoplakin, plectin, periplakin or epiplakin
- Erosive lichen planus
- T-cell mediated autoimmune disease
- Interface mucositis with Civatte bodies
- Subepithelial band of lymphocytes
- Direct immunofluorescence shaggy fibrin deposition at basement membrane zone
- Epidermolysis bullosa acquisita
- Immune mediated, subepithelial blistering condition
- Differentiate using salt split testing or enzyme-linked immunosorbent assay
- Enzyme-linked immunosorbent assay detects antibodies against type VII collagen
- Antibodies bind to the connective tissue floor of the bullae in epidermolysis bullosa acquista rather than the roof of the bullae as seen in metalloproteinases
- Lichen planus pemphigoides
- Generally younger
- Lichenoid lesions along with bullae
- Also has lichenoid characteristics
- Similar direct immunofluorescence with IgG, C3 or IgA+ at basement membrane zone
- Bullous lichen planus
- Least common variant of oral lichen planus
- Extremely rare
- Demonstrates clinical features similar to lichen planus and lichen planus pemphigoides; vesicles or bullae on pre-existing lichen planus lesions
- Histopathologic and immunofluorescent antibody studies are similar to lichen planus
- Angina bullosa hemorrhagica
- Often traumatic in nature
- Blood filled blisters on the soft palate
- Can be a mimicker on H&E
- Direct immunofluorescence is usually negative (Dermatol Reports 2014;6:5282)
- Erythema multiforme
- Self limiting blistering condition
- Lesions typically last 2 - 4 weeks
- Triggers may include infections (HSV, mycoplasma) or medications
- May demonstrate target lesions on the skin
- Lichenoid infiltrate in basement membrane zone
- Epithelium is edematous and spongiotic with necrosis of basal and suprabasal epithelial cells (intraepithelial and subepithelial bullae formation)
- Direct immunofluorescence shows diffuse granular staining of C3 in basement membrane zone
Board review style question #1
- Which is true about this entity (biopsied from the oral cavity)?
- Affected patients are often young, in the second to third decades of life
- Gingiva is the most commonly affected location
- Patients demonstrate significant ulceration and blistering of mucous membranes without subsequent scarring
- This entity mimics erosive lichen planus on direct immunofluorescence
Board review style answer #1
B. Gingiva is the most commonly affected location. This is mucous membrane pemphigoid.
Comment Here
Reference: Mucous membrane pemphigoid
Comment Here
Reference: Mucous membrane pemphigoid
Board review style question #2
- Which of the follow target antigens is not associated with mucous membrane pemphigoid?
- BP180
- BP230
- Desmoglein 1
- Laminin-332
- α6 integrin
Board review style answer #2
Board review style question #3
- Which target antigen is associated with malignancy in up to 30% of mucous membrane pemphigoid cases?
- BP 180
- BP 230
- Desmoglein 3
- Laminin-332
- Type VII collagen
Board review style answer #3