Table of Contents
Definition / general | Etiology | Clinical features | Case reports | Treatment | Clinical images | Gross description | Microscopic (histologic) description | Microscopic (histologic) images | Cytology description | Positive stains | Electron microscopy description | Molecular / cytogenetics description | Differential diagnosisCite this page: Roychowdhury M. Hyperparathyroidism. PathologyOutlines.com website. https://www.pathologyoutlines.com/topic/parathyroidprimarypth.html. Accessed April 24th, 2024.
Definition / general
- Autonomous, spontaneous overproduction of parathyroid hormone / parathormone / PTH by parathyroid tissue, with no evidence of prior parathyroid stimulation by renal or intestinal disease
- Important cause of hypercalcemia (0.3 - 5.0 cases/1000 adults)
- Higher incidence in women; usually age 50+
- Associated with irradiation in some; may be associated with sarcoidosis
- Rarely presents with bone disease (Am J Clin Pathol 1993;100:697)
- Normocalcemic primary hyperparathyroidism also occurs
Etiology
- Adenoma (85%), hyperplasia (15%), carcinoma (~1%)
Clinical features
- Often asymptomatic (no skeletal or renal lesions)
- Detected via screening studies for serum calcium
- To diagnose, PTH level must be elevated inappropriately to level of serum calcium
- Associated with low serum phosphorus, high urinary calcium and phosphorus, high serum alkaline phosphatase
Symptoms (due to increased serum PTH and calcium): bones, stones, groans, moans
Bone disease:
- Osteoporosis (from osteoclast prominence and remodeling), with later deformities and fractures
- Osteitis fibrosa cystica (also called brown tumors, von Recklinghausen disease [not neurofibromatosis]): thin cortex, marrow with increased fibrous tissue, hemorrhage and cysts; often in jaw
Stones:
- Renal calcium stones in 20%
- Also nephrocalcinosis (calcification of renal interstitium and tubules)
- Renal stones cause hypertension, are important cause of death
- Renal abnormalities may progress after treatment
Groans from GI distress:
- Nausea, peptic ulcers (associated with high serum gastrin that decreases after surgical excision), constipation, pancreatitis, gallstones
Moans from CNS disturbance:
- Depression, lethargy, seizures
- Also weakness, fatigue, calcifications of aortic and mitral valves; metastatic calcification in stomach, lungs, myocardium, blood vessels
Calciphylaxis
- Rare and life threatening condition of vascular calcification, first described in 1962, that causes ischemic damage to skin (usually lower extremity) and other organs (G Ital Nefrol 2012;29:674, Hum Pathol 1995;26:1055)
- Also known as calcific uremic arteriopathy (CUA), calcifying panniculitis, vascular calcification-cutaneous necrosis syndrome
- Affects 1 - 4% of dialysis patients; associated with primary, secondary or tertiary hyperparathyroidism
- 60 - 80% mortality
- Diagnosis: bilateral, symmetrical, superficial skin lesions with persistence of dorsal pulses; confirm with biopsy
- Treatment: parathyroidectomy
Secondary hyperparathyroidism
- Hyperparathyroidism due primarily to non-PTH disease
- Bone changes usually less severe than primary hyperparathyroidism
- Dialysis patients may have discrete, punched out bone lesions with minimal resorption or osteoblast activity (Am J Surg Pathol 1987;11:205)
- Due to hypocalcemia, which causes elevated PTH levels; causes of hypocalcemia are renal failure (phosphorus retention directly depresses serium calcium levels), inadequate calcium intake, steatorrhea (failure to absorb vitamin D), vitamin D deficiency or resistance; note:
- ~60% monoclonal
Tertiary hyperparathyroidism
- Autonomous parathyroid hyperplasia / adenoma arising from secondary hyperparathyroidism
- Often detected after hemodialysis or transplantation corrects the renal disease
- May have 10-40x increase in parathyroid mass
- Treatment: surgical excision
- Micro description: marked hyperplasia, with predominance of chief cells and abundance of oxyphil cells (Hum Pathol 1985;16:772)
Case reports
- 69 year old woman with primary hyperparathyroidism due to parathyroid adenoma (Arch Pathol Lab Med 2001;125:1351)
- 70 year old man with end stage renal failure secondary to IgA nephropathy (J Med Case Rep 2009;3:9297)
Treatment
- Surgical excision of enlarged gland plus one additional gland for diagnostic purposes
- Use selective venous catheterization to localize abnormal gland preoperatively
- Also total parathyroidectomy with autotransplantation of parathyroid tissue into forearm muscle but may get recurrence of hyperparathyroidism and hyperplastic gland may infiltrate the skeletal muscle and look malignant
Gross description
- Solid and cystic areas, brown due to hemosiderin
Microscopic (histologic) description
- Osteoblastic and osteoclastic activity, cysts, hemosiderin laden macrophages
- Pale, vacuolated cells arranged in a trabecular pattern are also seen in non-PTH mediated hypercalcemia (Am J Surg Pathol 1985;9:43)
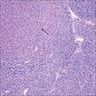
Microscopic (histologic) images
Cytology description
- FNA shows organoid or trabecular architecture of cellular tissue fragments with epithelial cells arranged around capillary cores and frequent microacini
- Cells have round, fairly uniform nuclei 6 to 8 microns
- Larger oxyphil cells may show considerable anisonucleosis
- No features of thyroid tissue such as hemosiderin laden macrophages, abundant colloid, paravacuolar granules (Hum Pathol 1995;26:338)
Positive stains
- Cyclin D1 (61%, Mod Pathol 1999;12:412)
Electron microscopy description
- Ribosomal lamellar complexes and groups of centrioles is suggestive of adenoma
- Examination of normal appearing glands can detect chief cell activity associated with hyperplasia (Hum Pathol 1986;17:1036)
Molecular / cytogenetics description
- ~40% monoclonal
- 95% sporadic; also associated with MEN 1 and MEN 2 / 2A syndromes (usually chief cell hyperplasia)
- PRAD1 / cyclin D1 (parathyroid adenoma 1) protein: inversion of gene on #11 puts PRAD1 next to 5'-PTH gene regulatory sequences which are constitutively active; seen in 10% of adenomas
- MEN1: loss of 11q13 tumor suppressor gene usually found; also noted in 20% of sporadic adenomas
- MEN 2 / 2A: may see chief cell hyperplasia and medullary carcinoma at the same time
Differential diagnosis
- Familial hypocalciuric hypercalcemia: young patients with family history, autosomal dominant, usually mild parathyroid hyperplasia (Hum Pathol 1981;12:229)
- Giant cell reparative granuloma: similar histology and both in jaw so use laboratory findings to differentiate
- Giant cell tumor: evenly spaced giant cells, plump stromal cells, less osteoblastic activity
- Also hyperthyroidism, myeloma, sarcoidosis, vitamin A or vitamin D intoxication
- Medullary carcinoma of thyroid if intrathyroidal tissue: PTH-, calcitonin+ (Am J Surg Pathol 1983;7:535)
- Tumor related hypercalcemia: has PTH related protein, more common in squamous cell carcinomas, renal cell carcinoma, ovarian clear cell carcinoma, rarely leukemia (Am J Clin Pathol 1981;75:149), Kaposi sarcoma (Am J Clin Pathol 1976;66:998)