Table of Contents
Definition / general | Clinical features | Clinical images | Microscopic (histologic) description | Microscopic (histologic) images | Negative stains | Differential diagnosis | Additional referencesCite this page: Hamodat M. Necrobiosis lipoidica. PathologyOutlines.com website. https://www.pathologyoutlines.com/topic/skinnontumornecrobiosislipoidica.html. Accessed April 23rd, 2024.
Definition / general
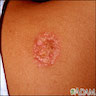
- Atrophic, yellow depressed plaques, usually on legs of diabetic patients
Clinical features
- Also associated with hypo and hyperthyroidism, inflammatory bowel disease and vasculitis
- Atrophic, yellow depressed plaques, telangiectasia and active inflammatory edge
- Chronic lesions may show ulceration and crusting
- Solitary or multiple, often symmetrical in lower extremities in pretibial area
- Involvement of penis with a lesion resembling chronic balanitis has been described
- Rarely, squamous cell carcinoma may arise in chronic lesions
Microscopic (histologic) description
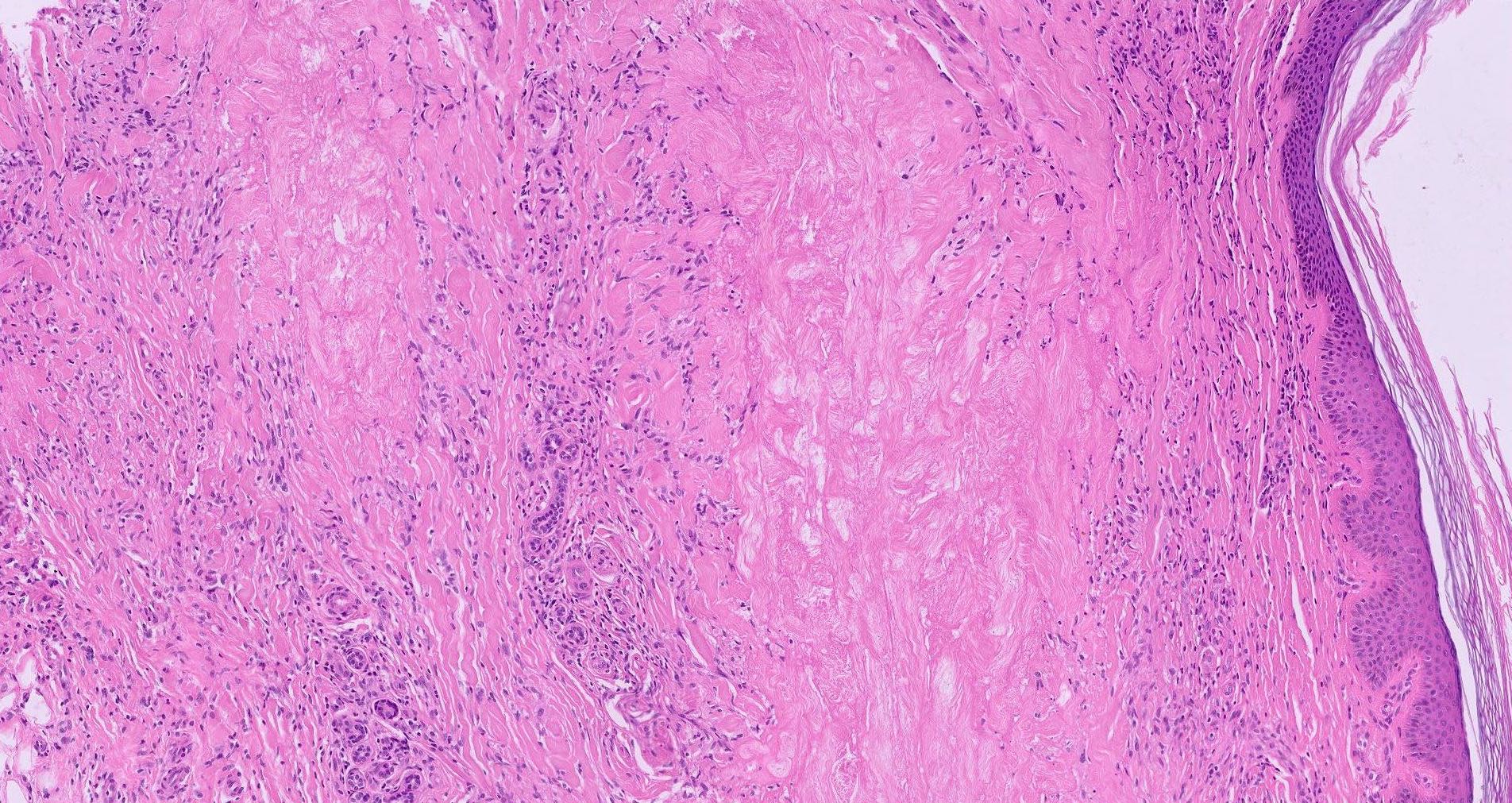
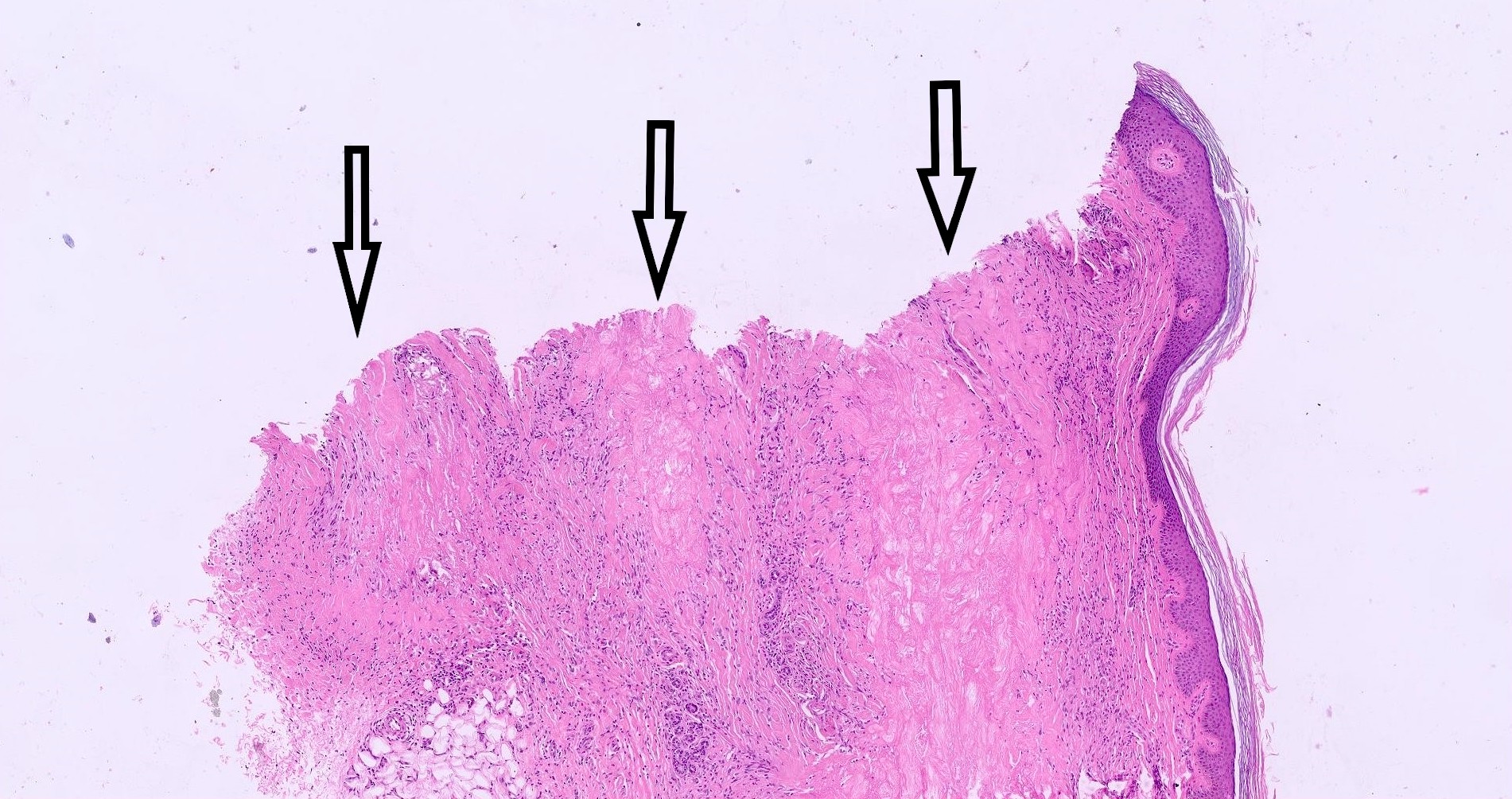
- Epidermal changes may be inconspicuous or absent; variable acanthosis, atrophy or hyperkeratosis
- Palisading, necrobiotic granuloma consist of a large confluent area of necrobiosis centered in the superficial dermis and subcutaneous fat
- Usually epithelioid histiocytes, giant cells and sometimes a well formed granuloma
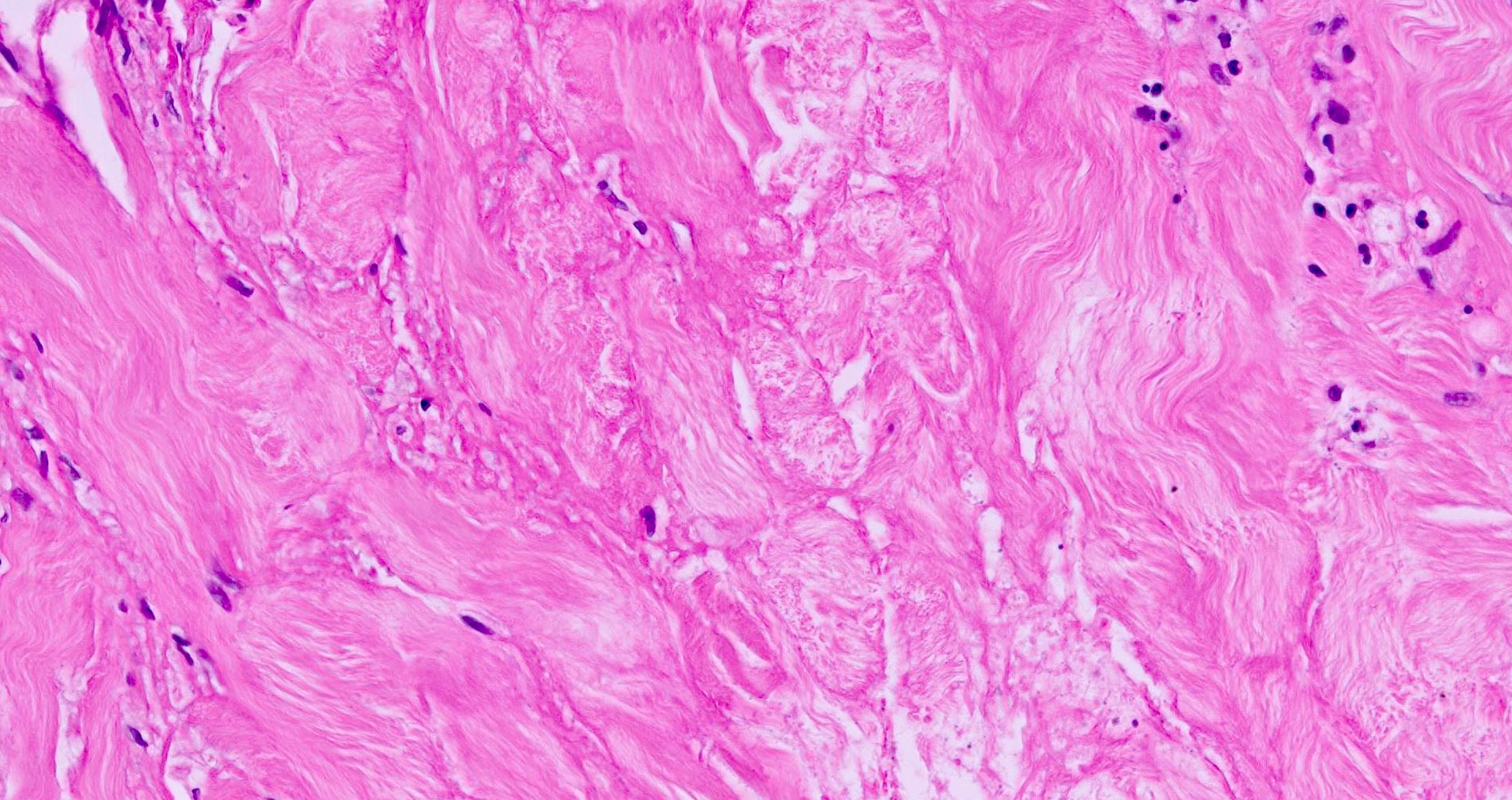
- Eosinophilic, swollen or degenerate collagen appears hyalinised with surrounding infiltrate of lymphocytes and histiocytes
- Linear infiltrate of histiocytes between collagen bundles; occasionally lipomemebranous fat necrosis
- Blood vessel wall thickening with intimal proliferation and narrowing of the lumen; also mild to moderate perivascular lymphocytic infiltrate
- Plasma cells are almost always present
- Cholesterol clefts are rare
- Loss of elastic tissue
Microscopic (histologic) images
Differential diagnosis
- Granuloma annulare: mucin+, lysozyme+
- Necrobiotic xanthogranuloma: head and neck of patients with paraproteinemia, not associated with diabetes
Additional references