Table of Contents
Definition / general | Essential features | Terminology | ICD coding | Epidemiology | Sites | Pathophysiology | Etiology | Clinical features | Diagnosis | Radiology description | Radiology images | Prognostic factors | Case reports | Treatment | Clinical images | Gross description | Gross images | Frozen section description | Frozen section images | Microscopic (histologic) description | Microscopic (histologic) images | Virtual slides | Cytology description | Cytology images | Positive stains | Negative stains | Electron microscopy description | Electron microscopy images | Molecular / cytogenetics description | Videos | Sample pathology report | Differential diagnosis | Additional references | Board review style question #1 | Board review style answer #1 | Board review style question #2 | Board review style answer #2 | Board review style question #3 | Board review style answer #3Cite this page: Stewart BD, Nascimento AF. Fibromatosis-palmar / plantar. PathologyOutlines.com website. https://www.pathologyoutlines.com/topic/softtissuefibromatosissuperficial.html. Accessed April 25th, 2024.
Definition / general
- Palmar and plantar fibromatosis are benign nodular fibroblastic / myofibroblastic proliferations typically arising in the volar aspect of the hands and fingers or involving plantar aponeuroses, respectively
- Both processes are histologically similar, composed of a bland cellular proliferation of spindle cells with a bluish appearance and with a variable amount of background collagen, depending on the age of the lesion (J Pathol Transl Med 2021;55:265)
Essential features
- Bland, variably cellular proliferation of spindled fibroblasts / myofibroblasts
- Collagenous stroma
- Involvement of aponeurosis and variably subcutis and dermis
- A subset shows nuclear beta catenin expression, despite the absence of CTNNB1 or APC gene mutations (Histopathology 2007;51:509, Mod Pathol 2001;14:695)
Terminology
- Palmar fibromatosis: Dupuytren disease or contracture
- Plantar fibromatosis: Ledderhose disease, morbus Ledderhose
ICD coding
Epidemiology
- Palmar fibromatosis
- Most common type of superficial fibromatosis (1 - 2% of population)
- Prevalence increases with age (~20% of population at age 65)
- M:F = 3 - 4:1
- 50% bilateral
- Most common in northern Europeans
- Rare in Black population
- Most common type of superficial fibromatosis (1 - 2% of population)
- Plantar fibromatosis
- Prevalence not currently understood (Foot Ankle Spec 2018;11:168)
- Middle aged patients
- Several reports of patients < 16 years old to as young as 9 months (J Pediatr Orthop 1997;17:16)
- NIH list of rare diseases (< 200,000 people)
- ~25% bilateral
- M > F (Orthop Res Rev 2018;11:1)
- 2 genetic variants found in genome wide association study suggest a possible genetic predisposition
- 1 indel (chr5:118704153:D) and 1 SNP (rs62051384) (Int J Sports Med 2018;39:314)
Sites
- Palmar fibromatosis
- Metacarpophalangeal joint, the proximal interphalangeal joint or both joints (Hand (N Y) 2011;6:149)
- Plantar fibromatosis
- Most often the medial and central bands of plantar aponeurosis
Pathophysiology
- Palmar fibromatosis
- Proliferation of fibroblasts, their differentiation into myofibroblasts and the production of extracellular matrix
- Proposed roles of fibroblast growth factor (FGF), wingless / integrated (WNT) and transforming growth factor beta (TGFβ) in disease progression (Exp Cell Res 2010;316:2390, Med Hypotheses 2012;78:385, Cell Physiol Biochem 2012;30:927, N Engl J Med 2011;365:307, Ann Plast Surg 2019;83:594)
- Plantar fibromatosis
- Proliferative phase: increased fibroblastic activity and cellular proliferation
- Active phase: nodule formation occurs
- Residual phase: collagen deposition, scar formation and tissue contracture
Etiology
- Palmar fibromatosis
- Unknown (WHO 5th edition)
- May be caused by fibrogenic cytokines (J Hand Surg Br 2005;30:557)
- Associations with diabetes, smoking and repetitive vibrational trauma reported but not validated (WHO 5th edition)
- Plantar fibromatosis
- Unknown (WHO 5th edition) (Foot Ankle Spec 2018;11:168)
- Associations with long term phenobarbital usage for epilepsy, frozen shoulder, smoking, alcohol addiction, diabetes and repeated trauma have not been validated (WHO 5th edition) (Epilepsia 2008;49:1965, Foot Ankle Spec 2018;11:168)
Clinical features
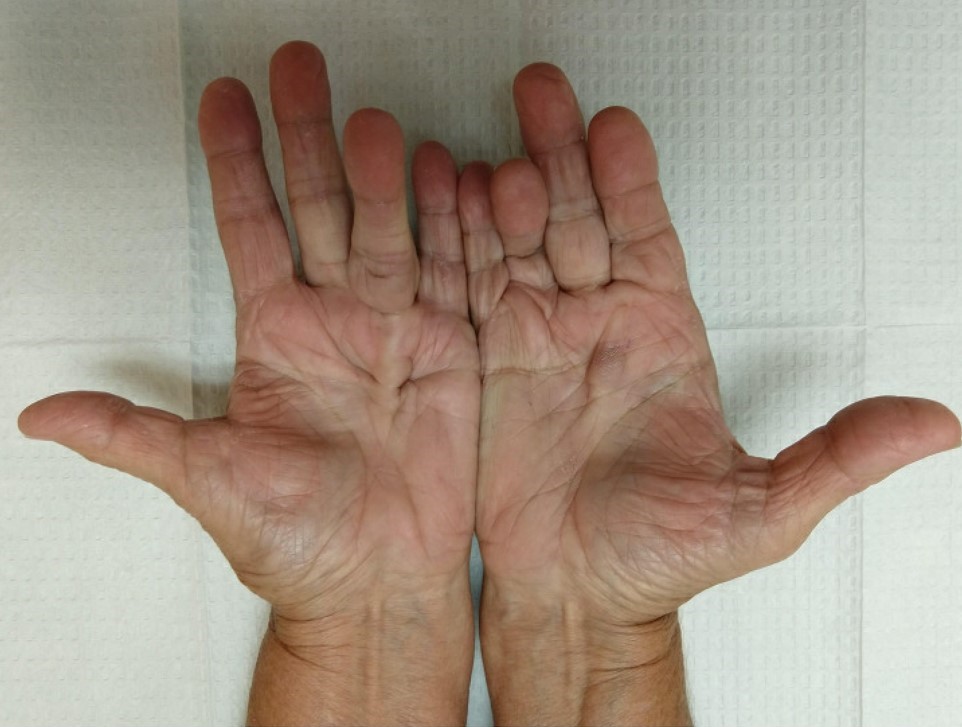
- Palmar fibromatosis
- Often presents with subcutaneous nodules on distal palmar crease
- Puckers overlying skin as it ages
- Causes flexion contracture, most commonly of digits 4 and 5, due to cord-like expansion of digital aponeurotic slips
- Does not involve deep structures (i.e., tendons or skeletal muscle)
- 10% also have plantar disease; 1 - 4% have penile fibromatosis
- Plantar fibromatosis
- 0.5 - 3.0 cm in diameter subcutaneous nodule(s), slow growing and located in the medial or central plantar aponeurosis
- Initially painless but later associated with pain after standing or walking, typically on the medial aspect of the sole (arch)
- Associated with concomitant palmar and penile fibromatoses and keloids
- Usually not associated with contractures (Foot Ankle Int 2018;39:751)
Diagnosis
- Usually clinical; however, occasionally may be a histologic confirmation
Radiology description
- Palmar fibromatosis
- Ultrasound
- Nodules superficial to flexor tendons in superficial fascia
- Early lesions: hypoechoic with hypervascularity
- Chronic lesions: hyperechoic without vascularity (J Ultrason 2012;12:381)
- Magnetic resonance imaging (MRI)
- Subcutaneous nodules
- Typically uniformly low signal intensity on both T1 and T2 (AJR Am J Roentgenol 1993;160:813)
- Ultrasound
- Plantar fibromatosis
- Radiographs usually normal
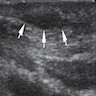
- Ultrasound
- Better than MRI (Semin Musculoskelet Radiol 2010;14:334)
- Lesion(s) embedded on the plantar fascia
- Less reflective to the much brighter plantar fascia surrounding it with sharp juxtaposition (Semin Musculoskelet Radiol 2010;14:334)
- Hypo to mixed echogenicity
- Discrete, fusiform, multinodular thickening of plantar fascia (AJR Am J Roentgenol 2002;179:1167)
- Comb sign in 51% of cases (J Ultrasound Med 2018;37:2725)
- Alternating linear bands of hypoechogenicity and isoechogenicity relative to the plantar fascia
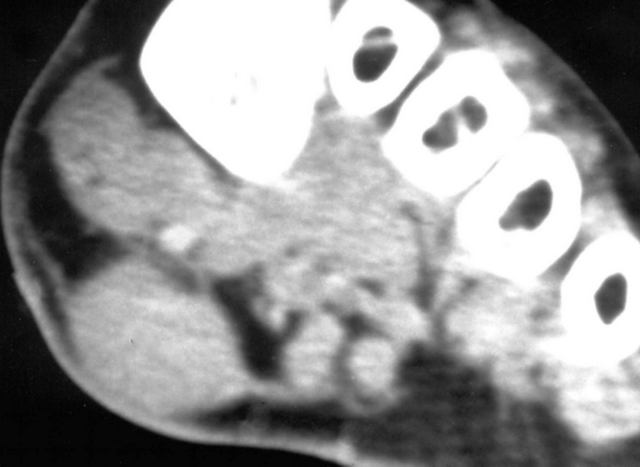
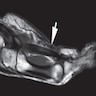
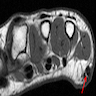
- MRI
- Nodules appear as focal, oval shaped areas of disorganization embedded in plantar fascia (Semin Musculoskelet Radiol 2010;14:334)
- T1: iso to low signal (compared to muscle)
- T2: low to intermediate signal (AJR Am J Roentgenol 2002;179:1167, Radiographics 2000;20:333)
Radiology images
Prognostic factors
- Palmar fibromatosis
- Worse in White men with a strong family history, bilateral involvement, severe disease and ectopic manifestations (BMJ 2006;332:397)
- Plantar fibromatosis
- Worse with bilateral involvement, multiple nodules and a positive family history (Foot (Edinb) 2017;31:31)
Case reports
- Palmar fibromatosis
- 59 year old woman with bilateral Dupuytren contractures of the thumb interphalangeal joints (J Plast Reconstr Aesthet Surg 2012;65:1738)
- 65 year old man with hand flexion contracture (BMJ 2014;349:g6137)
- 82 year old man with heterotopic ossification in Dupuytren disease (J Bone Joint Surg Br 2011;93:1676)
- Plantar fibromatosis
- 28 year old Brazilian woman with 6 year history of painless bilateral plantar nodules (J Clin Aesthet Dermatol 2010;3:45)
- 30 year old man presented with painful bilateral plantar nodules (Surg J (N Y) 2016;2:e102)
- 51 year old woman with giant bilateral plantar fibromatosis (Int J Dermatol 2018;57:365)
- 54 year old man with nodular swelling of the right plantar arch (Diagn Interv Imaging 2014;95:893)
- 64 year old woman with osseous metaplasia in a case of plantar fibromatosis (J Foot Ankle Surg 2004;43:430)
Treatment
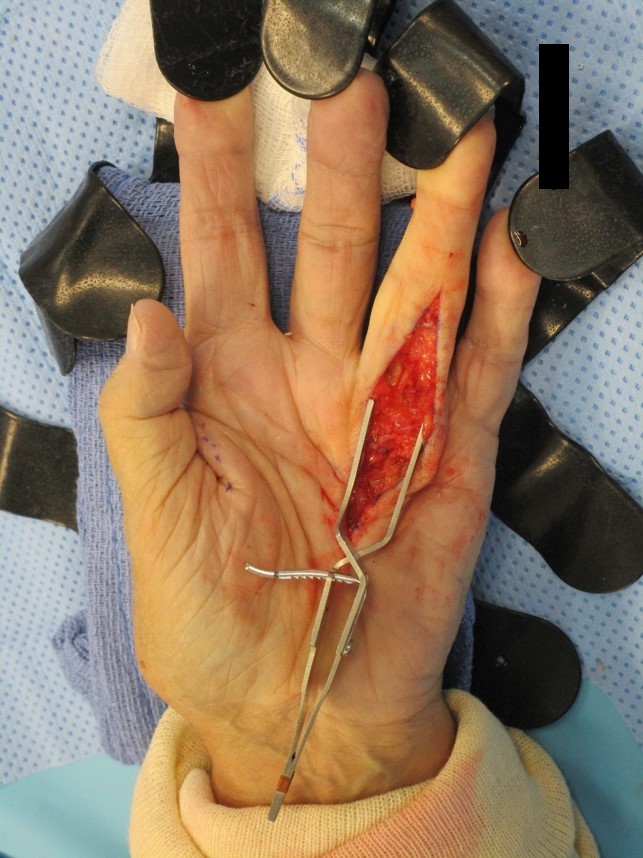
- Palmar fibromatosis
- Observation, excision or incision of contracture band
- Often recurs
- Surgical treatment is necessary if the contracture results in functional disability and the total flexion deformity is > 30° (Plast Reconstr Surg 2017;139:240e)
- Collagenase (clostridial collagenase histolyticum) (Plast Reconstr Surg 2017;139:240e, Ir J Med Sci 2020;189:529, Foot Ankle Spec 2018;11:168)
- Plantar fibromatosis
- Conservative measures should be used prior to recommending surgery (Orthop Res Rev 2018;11:1)
- Observation, surgery if symptomatic; complete fasciectomy has fewer recurrences (0 - 50%) than local excision (57 - 100%) and wide excision (8 - 80%) (Plast Reconstr Surg 2008;122:486, Foot Ankle Spec 2018;11:168, Orthop Res Rev 2018;11:1)
- Wide excision: 2 - 3 cm margin
- Several nonoperative treatments with variable scientific support (Orthop Res Rev 2018;11:1)
- Steroid injections
- Verapamil
- Radiation therapy
- Extracorporeal shock wave therapy
- Tamoxifen
- Collagenase
Gross description
- Palmar fibromatosis
- Small nodules or nodular masses associated with aponeurosis and subcutaneous fat with gray-yellow-white cut surface (color depends on collagen content)
- Plantar fibromatosis
- 2 - 3 cm nodules associated with aponeurosis and subcutis with gray-yellow-white cut surface (color depends on collagen content)
- Reference: Weiss: Enzinger and Weiss's Soft Tissue Tumors, 7th Edition, 2019
Frozen section description
- Same as Microscopic (histologic) description but immaturity of the fibroblasts is less evident (blue staining is less intense)
Frozen section images
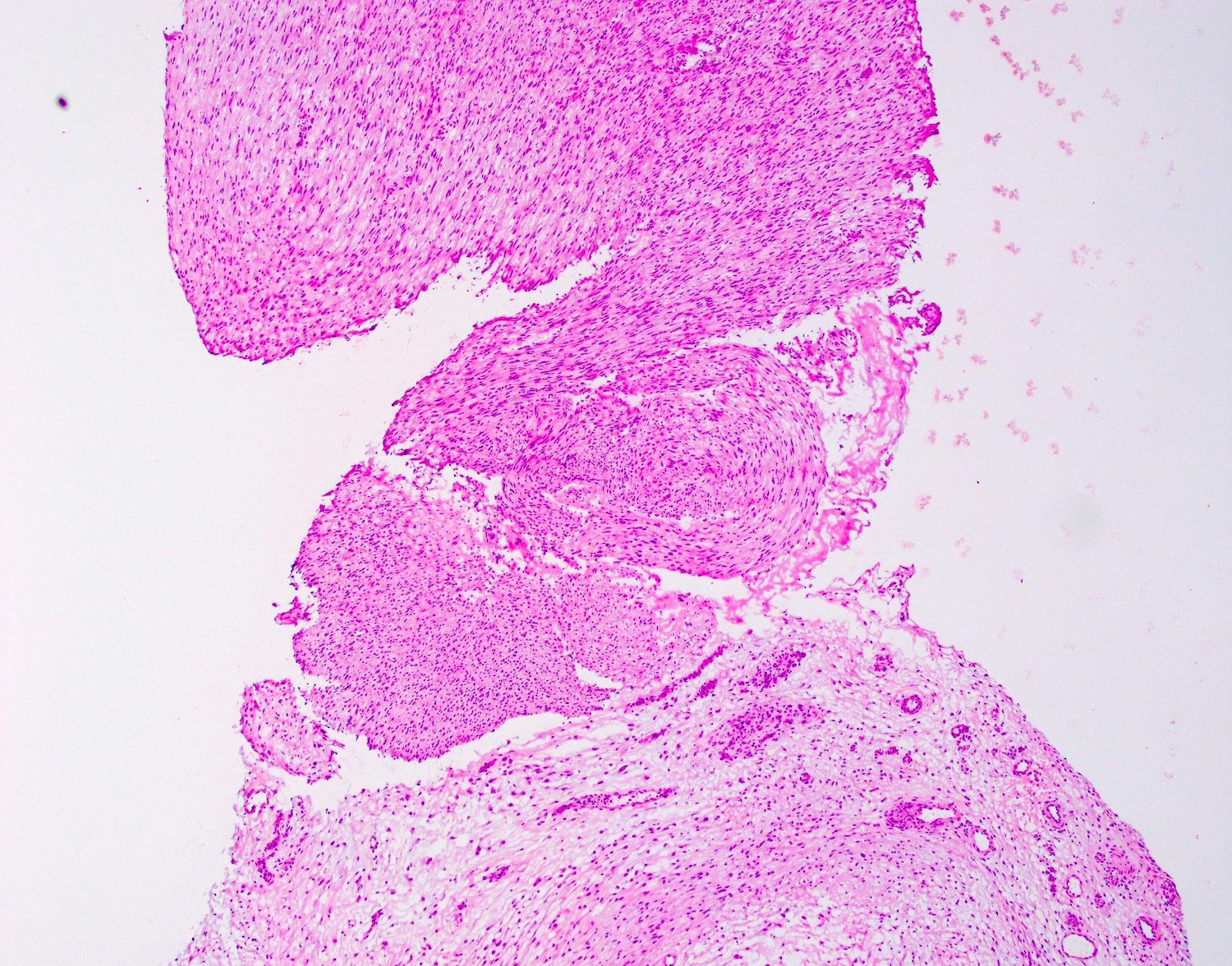
Microscopic (histologic) description
- Both processes are histologically similar
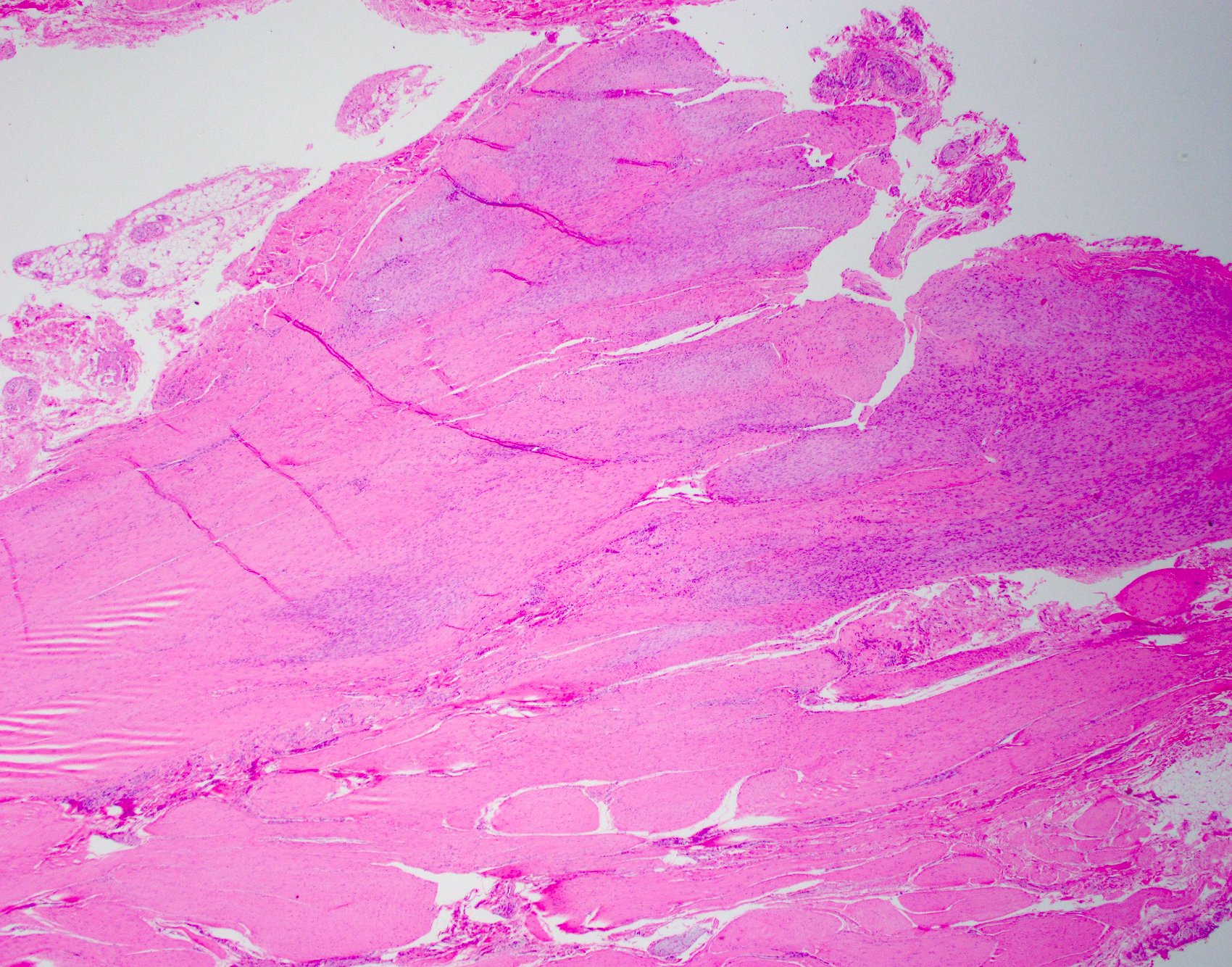
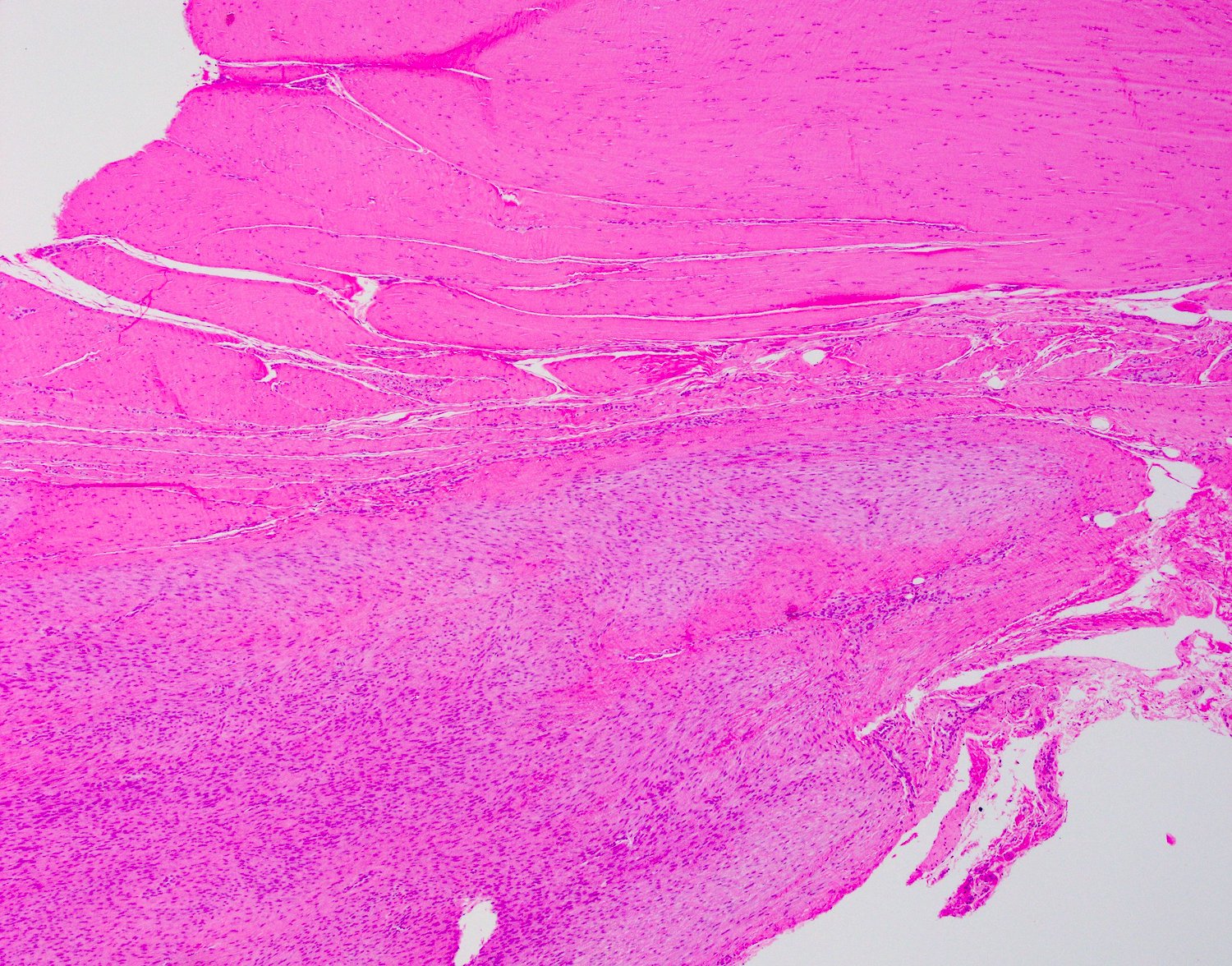
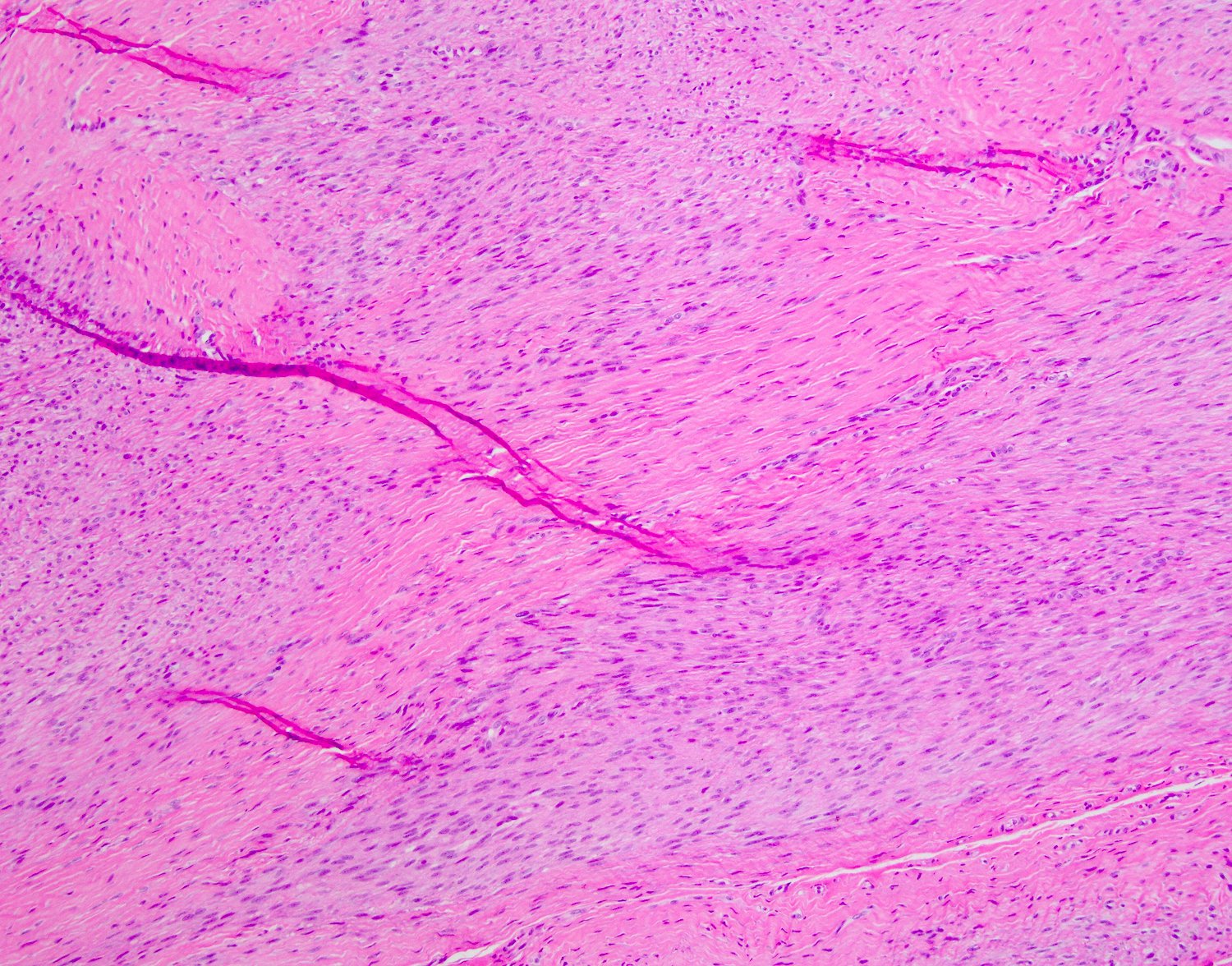
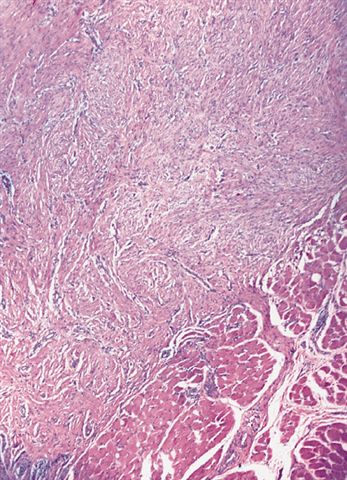
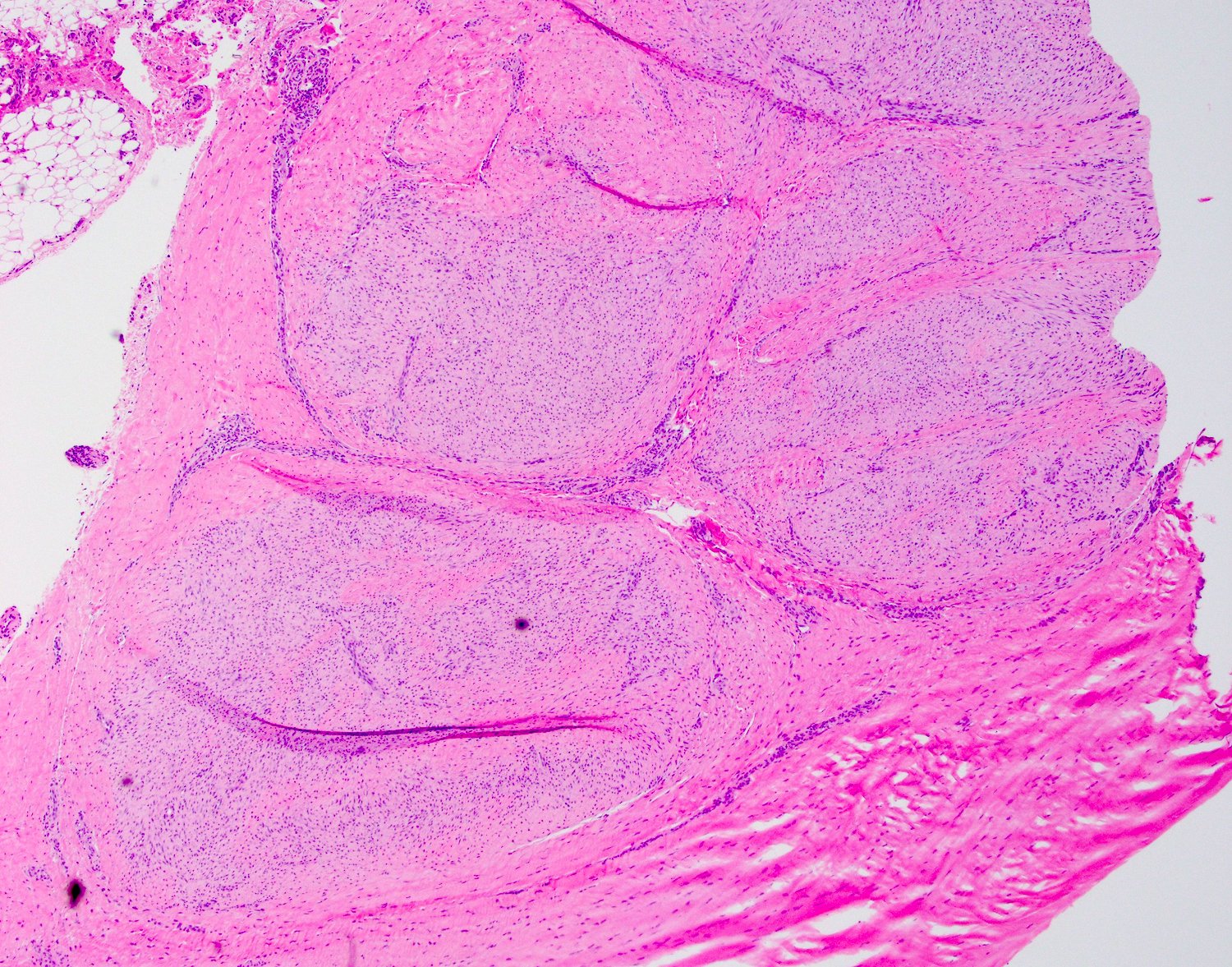
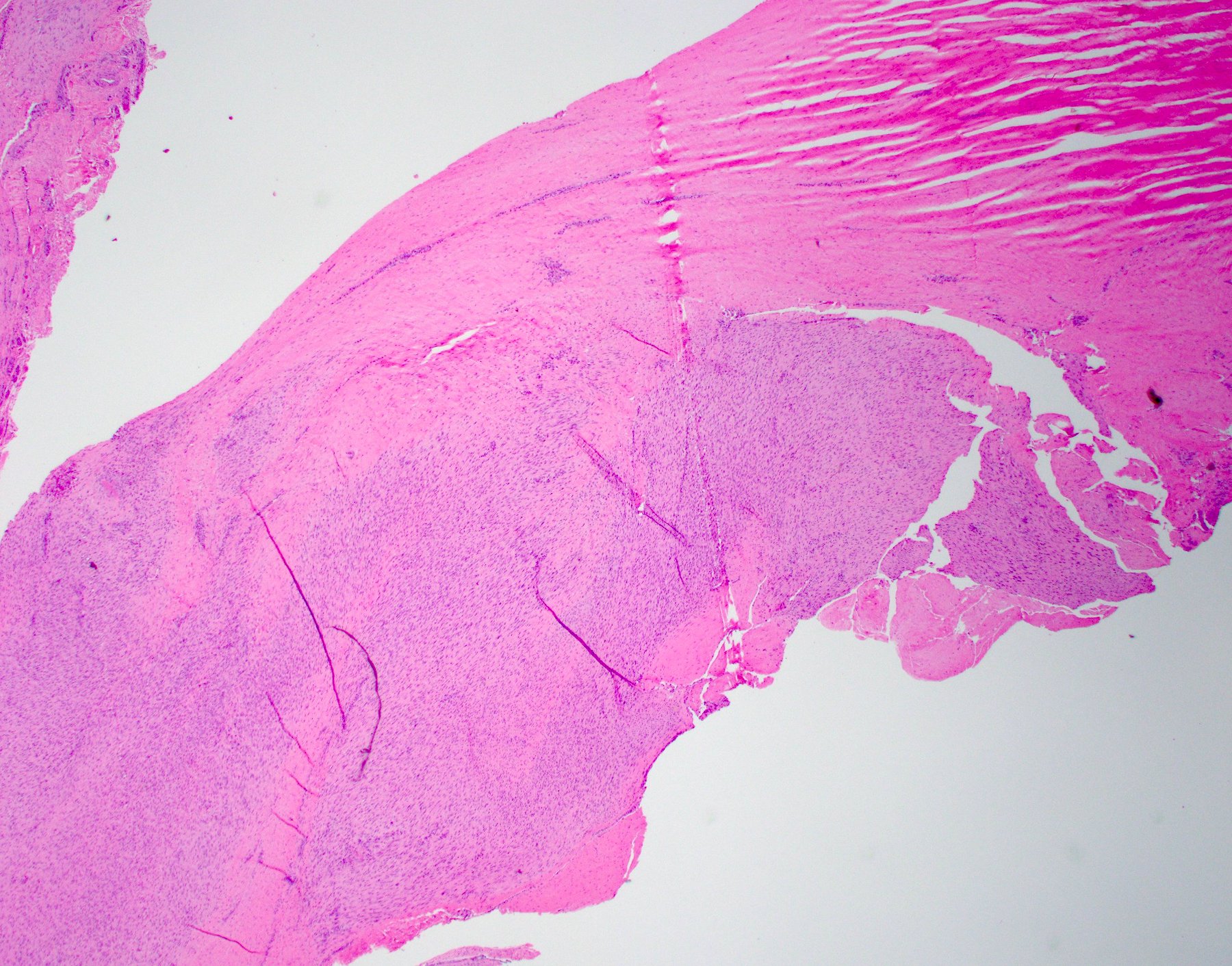
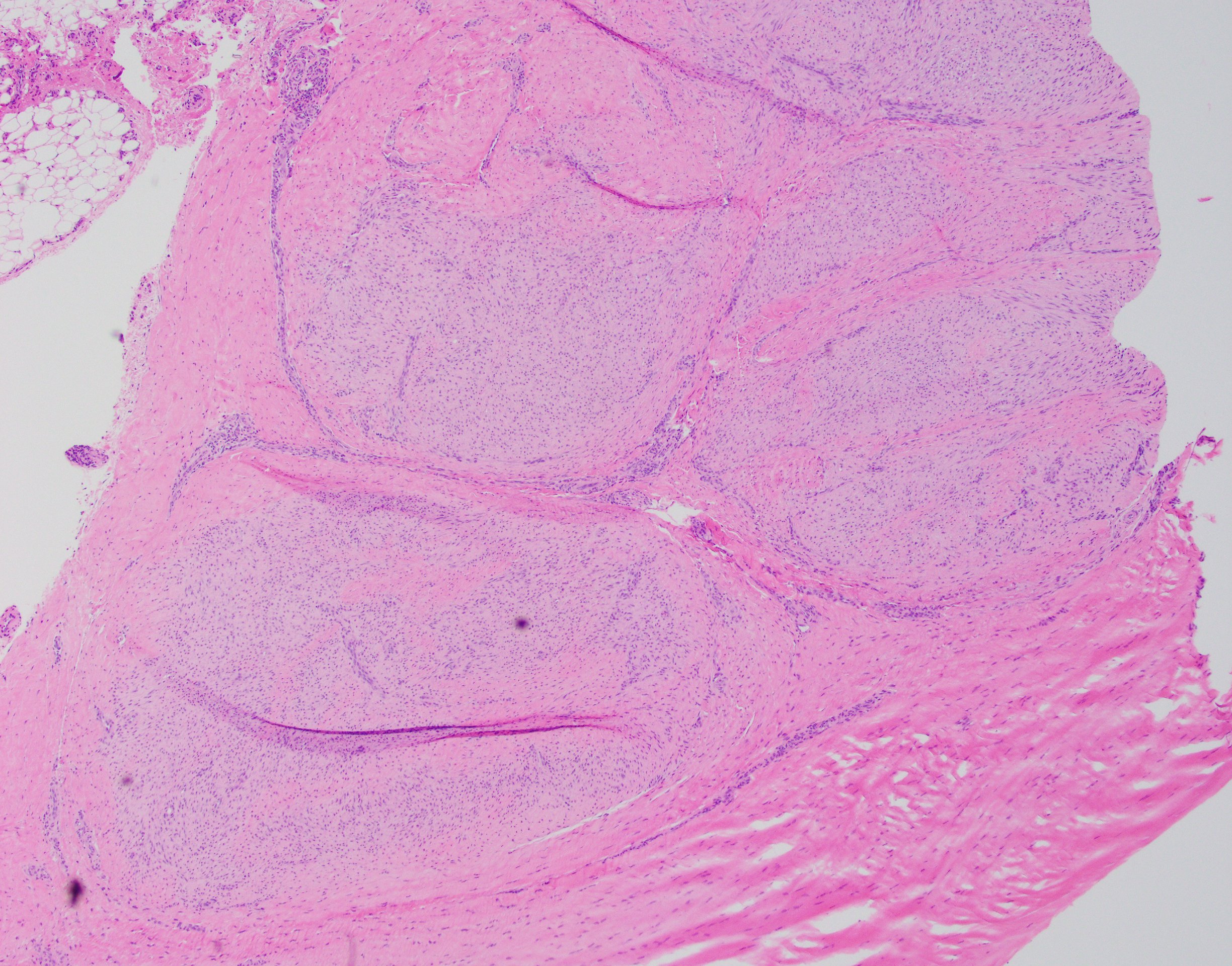
- Typically, tumors involve a thickened palmar / plantar aponeurosis and form single or multiple discontinuous, moderately cellular spindle cell nodules in a collagenous stroma (Am J Surg Pathol 2005;29:1095)
- Morphologically, there are 3 phases of growth (proliferative, involutional and late stage)
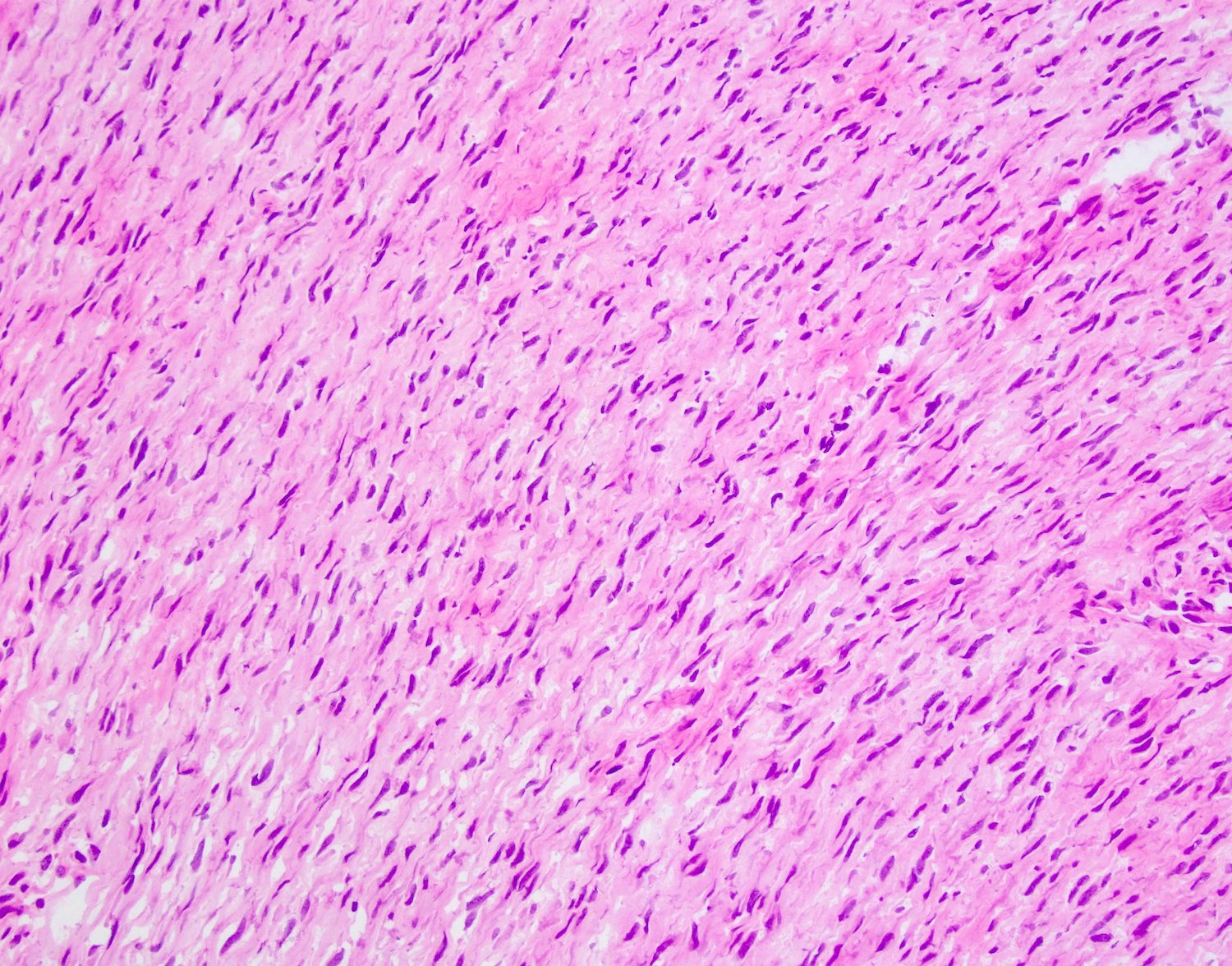
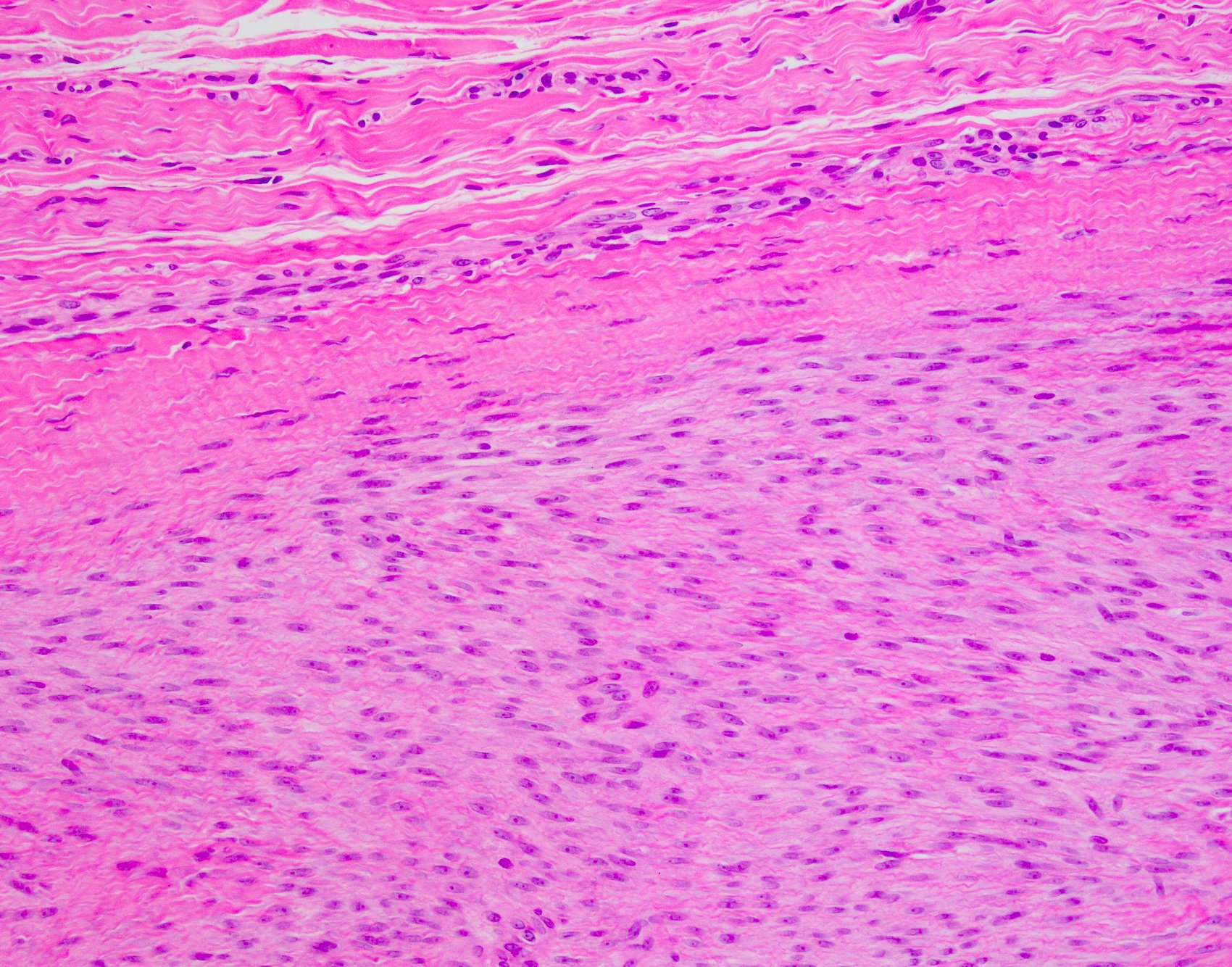
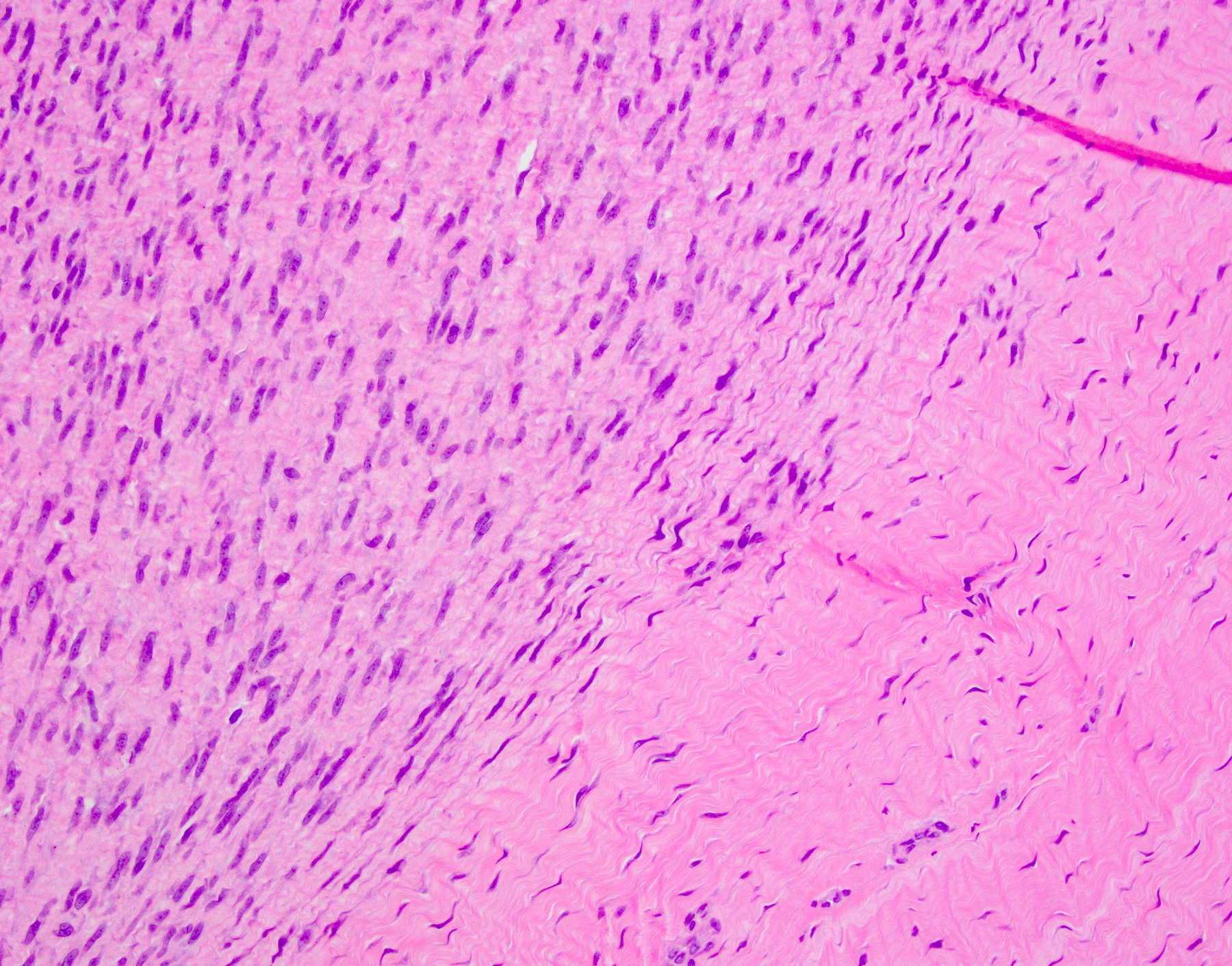
- Proliferative phase
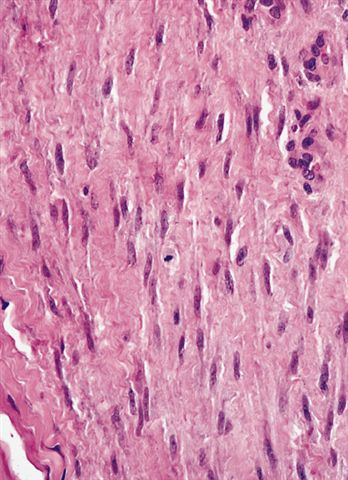
- Cellular, parallel fascicles of bland, plump, relatively uniform spindled fibroblasts with tapering nuclei, vesicular chromatic and small or inconspicuous nucleoli, with minimal stromal collagen
- Some plantar lesions are hypercellular and can mimic spindle cell sarcomas but they lack atypia
- Scattered chronic inflammation and occasional typical mitotic figures, especially in early lesions
- Mitotic activity may be prominent in pediatric patients
- Occasional, particular plantar lesions show interspersed multinucleated cells (Am J Surg Pathol 2002;26:244)
- Late stage
- Increase collagenous matrix and decreased cellularity
- Proliferative phase
- Reference: WHO 5th edition
Microscopic (histologic) images
Contributed by Brian D. Stewart, M.D. and AFIP
Palmar fibromatosis
Plantar fibromatosis
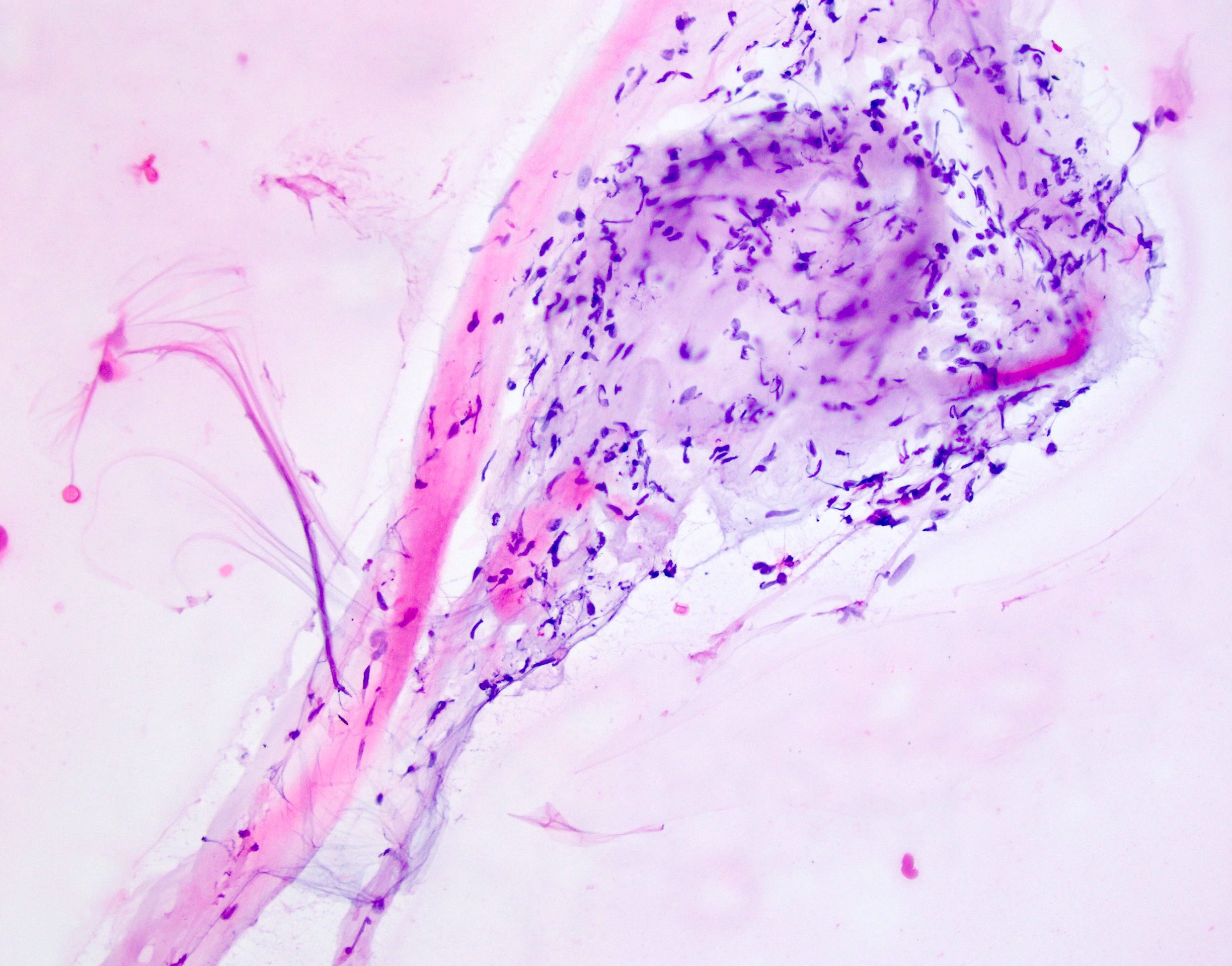
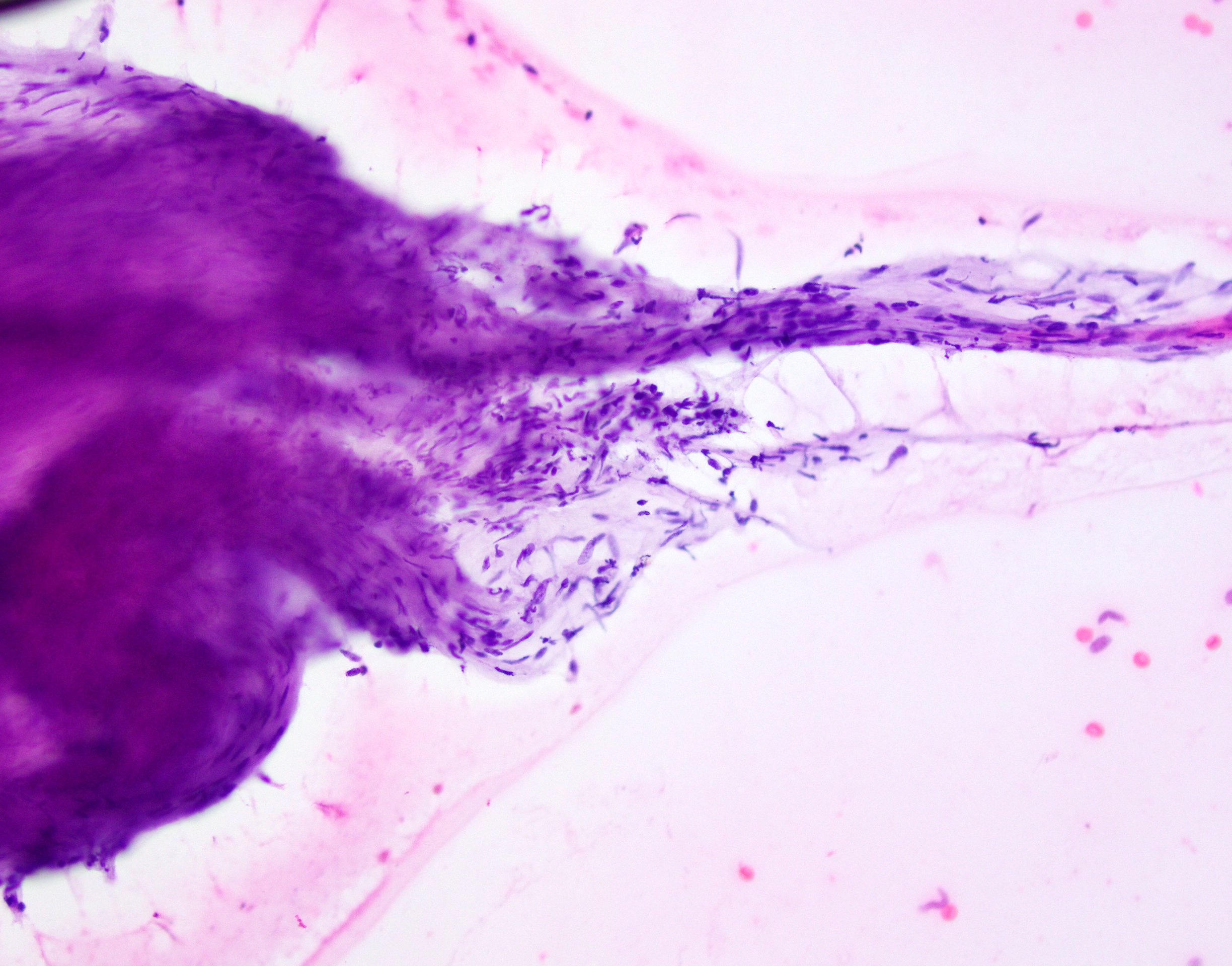
Cytology description
- Usually limited to touch preps during rare frozen sections (Acta Cytol 1993;37:323)
- Low cellularity, clusters of bland spindle cells with oval to elongated nuclei, no atypical features, rare or absent mitotic activity
Positive stains
- Palmar fibromatosis
- Usually not necessary to perform due to characteristic histology
- Vimentin, variable actin - muscle specific and smooth muscle actin, less frequently desmin
- Aberrant nuclear expression of beta catenin common (Mod Pathol 2001;14:695, Histopathology 2007;51:509)
- Plantar fibromatosis
- Vimentin, variable actin - muscle specific and smooth muscle actin, less frequently desmin
Negative stains
- Palmar fibromatosis
- Plantar fibromatosis
- Reference: Weiss: Enzinger and Weiss's Soft Tissue Tumors, 7th Edition, 2019
Electron microscopy description
- Fibroblasts and myofibroblasts
Molecular / cytogenetics description
- The tumor lacks the CTNNB1 and APC mutations characteristic of desmoid fibromatosis (Histopathology 2007;51:509, Mod Pathol 2001;14:695)
- Palmar fibromatosis
- Near diploid, often +7 or +8, no gene amplifications or deletions (Cancer Genet Cytogenet 2008;183:6)
- Loss of Y chromosome (Mod Pathol 2000;13:1080)
- Usually considered reactive, not neoplastic (J Transl Med 2006;4:21)
- Aberrations in Wnt signaling pathway but no somatic mutations of beta catenin genes, unlike desmoid fibromatosis (N Engl J Med 2011;365:307, Plast Reconstr Surg 2012;129:921, Joint Bone Spine 2012;79:7, Mod Pathol 2001;14:695)
- Plantar fibromatosis
- Near diploid, often +7 or +8; no somatic mutations of beta catenin genes, unlike desmoid fibromatosis (Mod Pathol 2001;14:695)
- Trisomy 8 and 14 (Cancer Genet Cytogenet 1999;108:176)
- Reciprocal t(2;7)(p13;p13) (Cancer Genet Cytogenet 2005;158:67)
Videos
Plantar fibromatosis
Sample pathology report
- Soft tissue, hand nodule, excision:
- Palmar fibromatosis (Dupuytren contracture) (see comment)
- Comment: Sections show a variably cellular proliferation of spindled fibroblasts and myofibroblasts without atypia set within a collagenous stroma, morphologically consistent with palmar fibromatosis (Dupuytren contracture).
- Soft tissue, foot nodule, excision:
- Plantar fibromatosis (see comment)
- Comment: Sections show a variably cellular proliferation of spindled fibroblasts and myofibroblasts without atypia set within a collagenous stroma, morphologically consistent with plantar fibromatosis.
Differential diagnosis
- Palmar fibromatosis
- Spindle cell sarcomas (i.e., synovial sarcoma, malignant peripheral nerve sheath tumor, etc.)
- Desmoid type fibromatosis:
- Rare in hand
- Dominant mass infiltrates skeletal muscle
- Epithelioid sarcoma:
- Epithelioid sarcoma commonly presents in the hand but cells will show a distinctive epithelioid appearance with abundant eosinophilic cytoplasm (J Pathol Transl Med 2021;55:265)
- Central necrosis or hyalinization is often seen
- Epithelioid sarcoma is characteristically reactive for cytokeratins and CD34 and shows a loss of nuclear staining for SMARCB1 (INI1)
- Plantar fibromatosis
- Clinical differential without nodules: calcaneal stress fracture, tarsal tunnel syndrome, plantar fasciitis (Orthop Res Rev 2018;11:1)
- Clinical differential with nodules: melanoma, synovial sarcoma, Kaposi sarcoma
- Calcifying aponeurotic fibroma:
- Plump or epithelioid fibroblasts palisading around cartilage and spotty calcification
- Desmoid type fibromatosis:
- Rare in feet
- Infiltrates skeletal muscle
- > 3 cm
- Often beta catenin+
- Spindle cell sarcomas (i.e., synovial sarcoma, malignant peripheral nerve sheath tumor, etc.):
- Monophasic synovial sarcoma:
- Uniformly hypercellular
- Often staghorn vascular pattern or ropy collagen
- Patchy keratin or EMA
- Rearrangement of SS18
- Malignant peripheral nerve sheath tumor:
- Monophasic synovial sarcoma:
Additional references
- WHO Classification of Tumours Editorial Board: Soft Tissue and Bone Tumours, 5th Edition, 2020, eMedicine: Dupuytren Contracture [Accessed 14 August 2023], Wikipedia: Dupuytren's Contracture [Accessed 14 August 2023], J Am Acad Orthop Surg 2011;19:746, Wikipedia: Plantar Fibromatosis [Accessed 14 August 2023], eMedicine: Plantar Fibromatosis [Accessed 14 August 2023]
Board review style question #1
Which of the following is true about the disease pictured in this photomicrograph of a painful nodule on the sole of the foot?
- Associated with similar processes in other body sites
- Beta catenin will show diffuse nuclear reactivity, confirming the diagnosis
- Most common in adolescents
- Most common in the central and lateral portions of the foot
- t(x;18) is pathognomonic
Board review style answer #1
A. Associated with similar processes in other body sites. Plantar fibromatosis is associated with similar processes in other body sites. Answer B is incorrect because beta catenin usually shows nuclear reactivity in palmar fibromatosis but not in plantar fibromatosis. Answers C and D are incorrect because plantar fibromatosis is most common in the medial and central bands of the plantar aponeurosis and in middle aged patients. Answer E is incorrect because synovial sarcoma has a pathognomonic t(x;18).
Comment Here
Reference: Palmar / plantar fibromatosis
Comment Here
Reference: Palmar / plantar fibromatosis
Board review style question #2
Which statement about plantar fibromatosis is correct?
- Associated with diabetes
- Bilateral in 5% of cases
- Often cured without recurrence after excision
- Synonymous with plantar fasciitis
- Usually rapidly growing
Board review style answer #2
A. Associated with diabetes. Plantar fibromatosis has been shown to have an association with diabetes. Answer B is incorrect because plantar fibromatosis is bilateral in about 25% of cases. Answer C is incorrect because recurrence is common after excision. Answer D is incorrect as plantar fasciitis is inflammation of the ligament itself and does not form nodules; it is part of the differential diagnosis of plantar fibromatosis. Answer E is incorrect because plantar fibromatosis is usually slow growing.
Comment Here
Reference: Palmar / plantar fibromatosis
Comment Here
Reference: Palmar / plantar fibromatosis
Board review style question #3
Which of the following stains may be positive in palmar or plantar fibromatosis although not specific?
- CD34
- CD56
- DOG1
- Keratin
- Smooth muscle actin
Board review style answer #3
E. Smooth muscle actin is the correct answer as it is reactive in many spindle cell proliferations and is not specific. Answers A - D are incorrect as all of these markers are negative in palmar and plantar fibromatosis.
Comment Here
Reference: Palmar / plantar fibromatosis
Comment Here
Reference: Palmar / plantar fibromatosis