12 December 2013 - Case #294
All cases are archived on our website. To view them sorted by case number, diagnosis or category, visit our main Case of the Month page. To subscribe or unsubscribe to Case of the Month or our other email lists, click here.
Thanks to Dr. Ankur Sangoi, El Camino Hospital (California), for contributing this case. This case was reviewed in May 2020 by Dr. Jennifer Bennett, University of Chicago and Dr. Carlos Parra-Herran, University of Toronto.
Case #294
Clinical history:
A 43 year old woman presented with uterine bleeding, leading to an endometrial biopsy. She subsequently underwent a total abdominal hysterectomy.
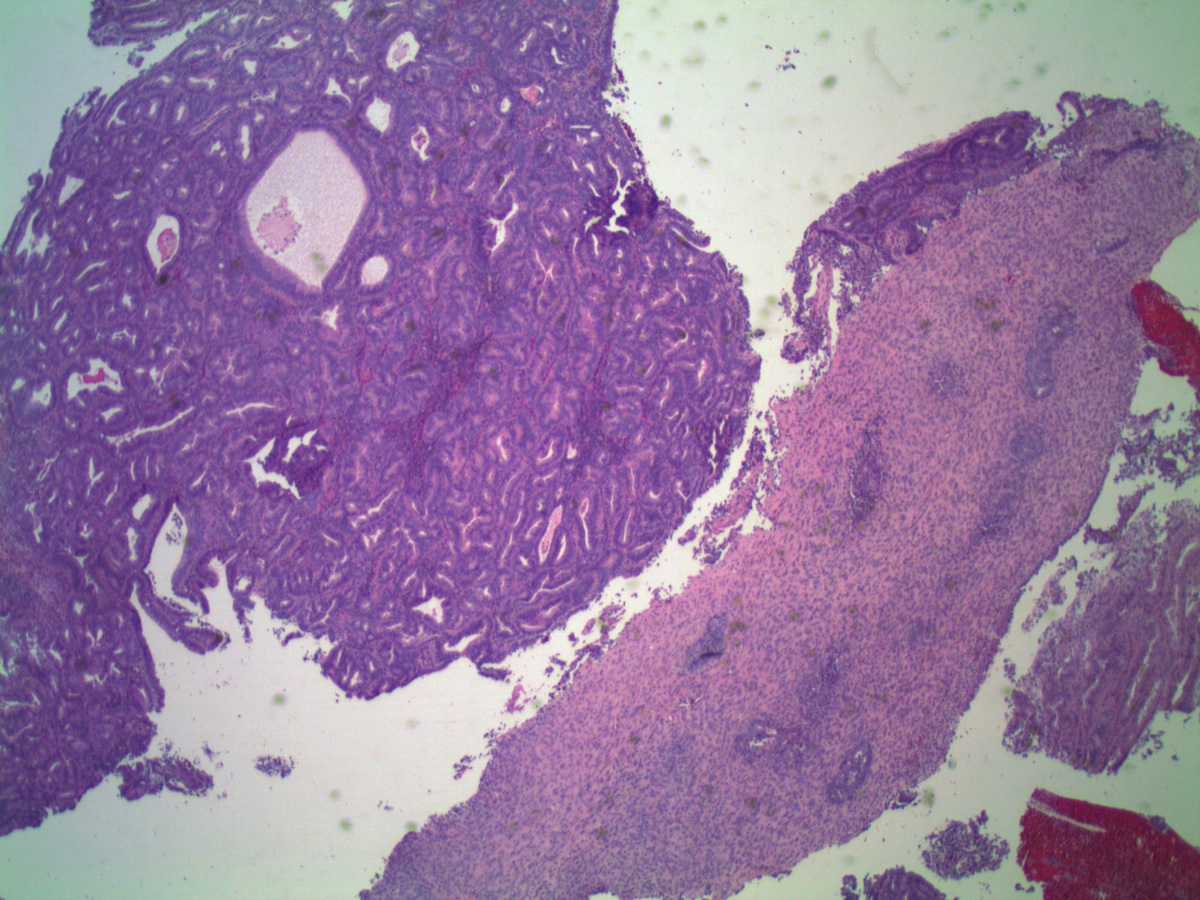
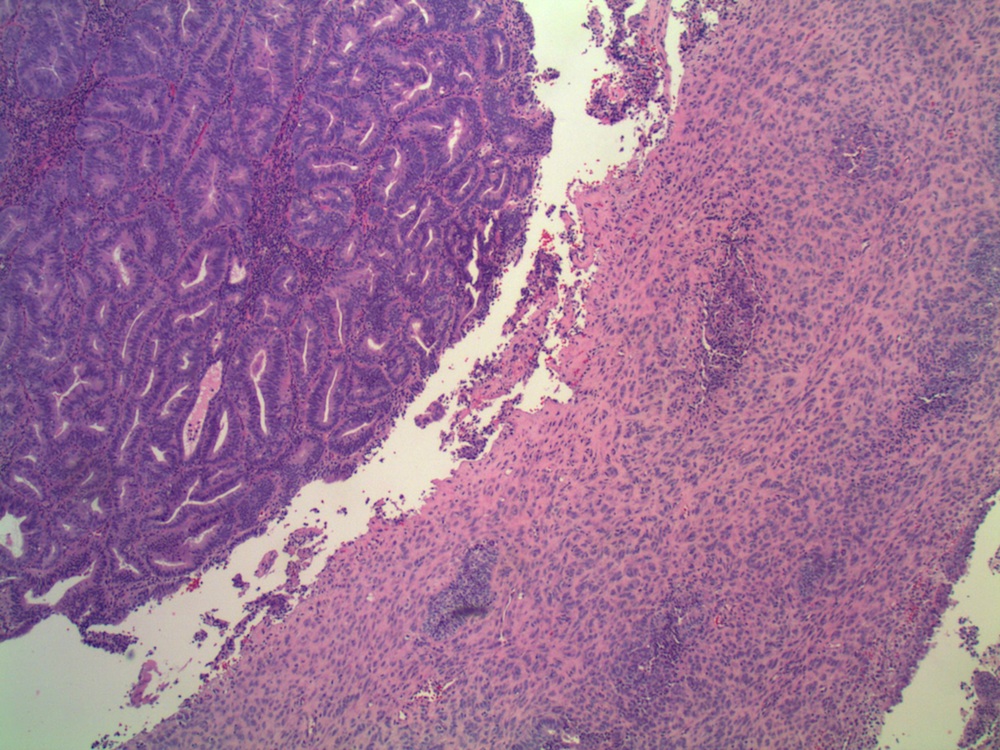
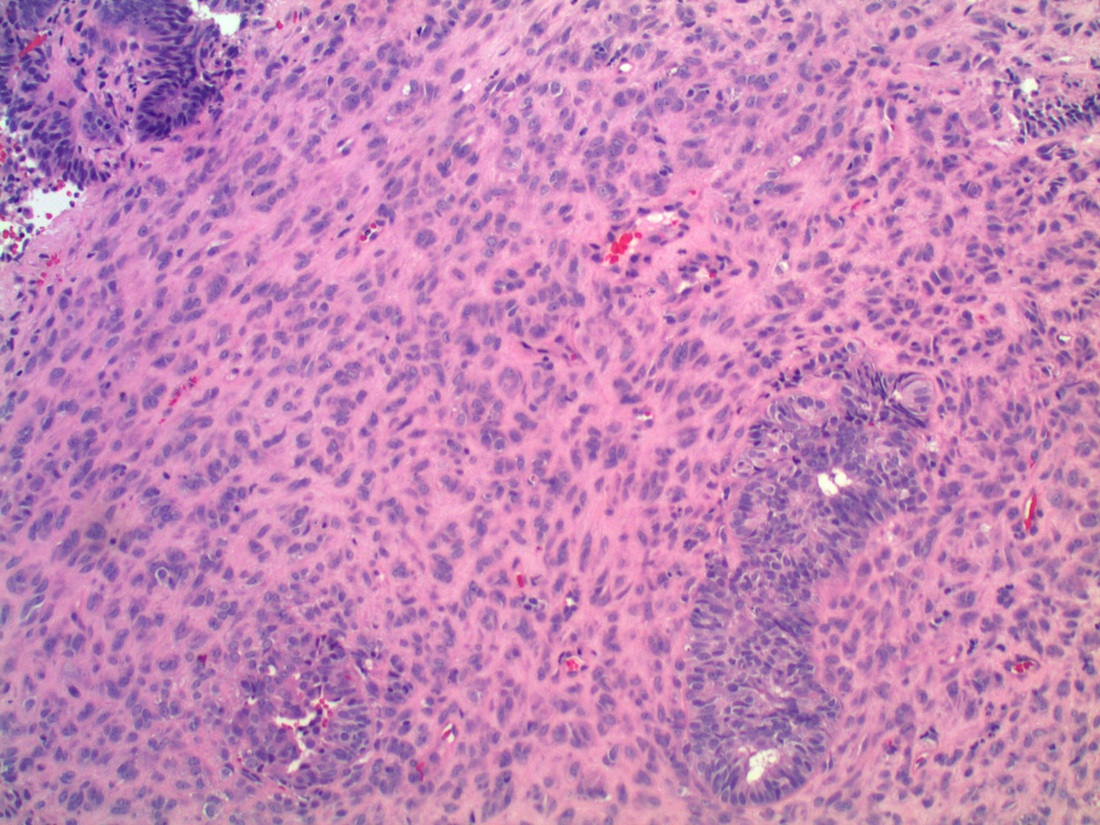
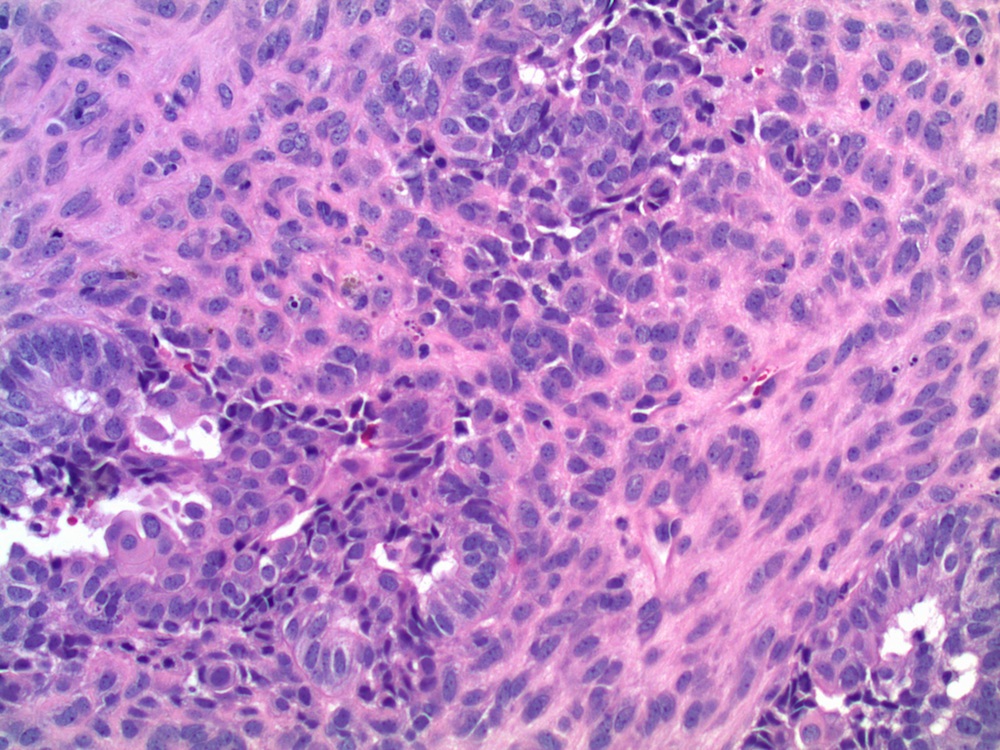
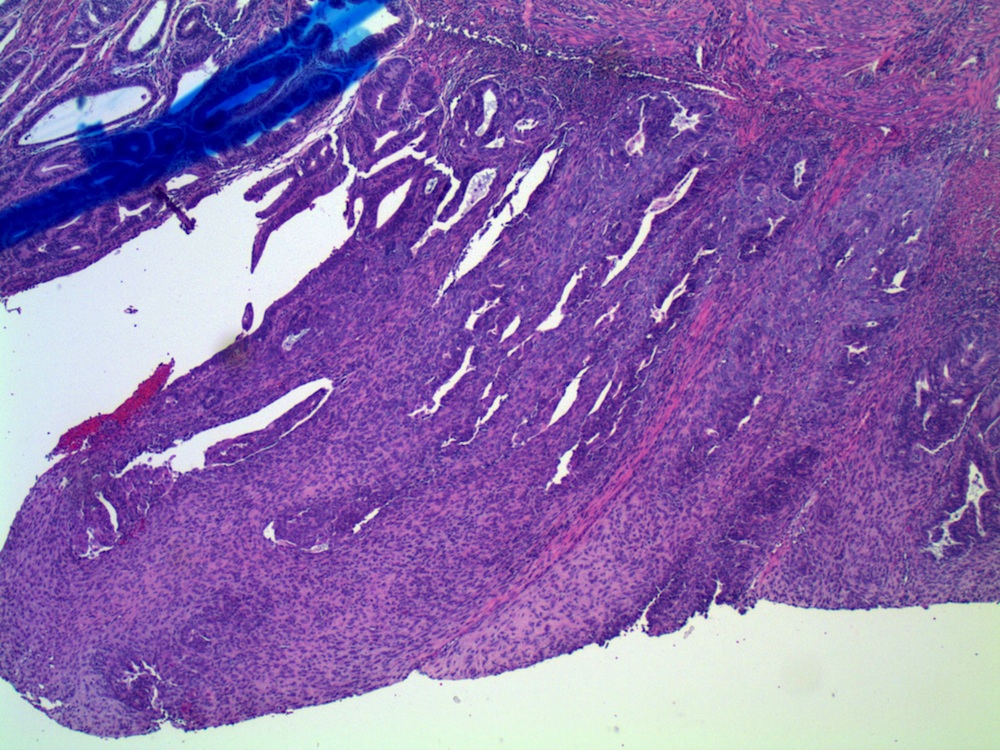
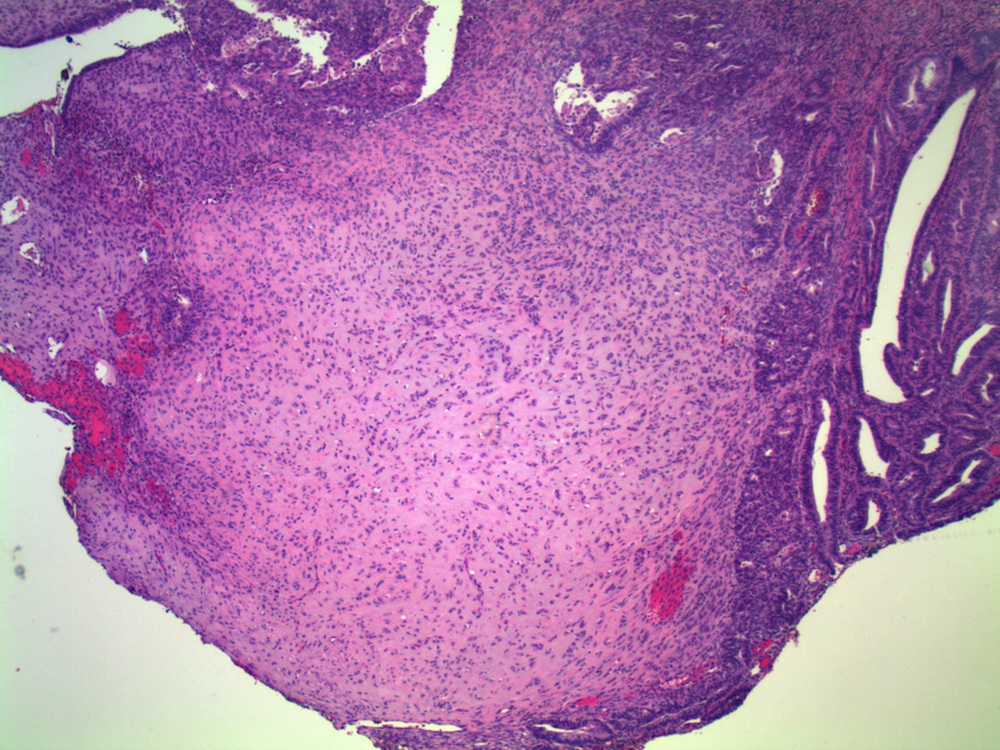
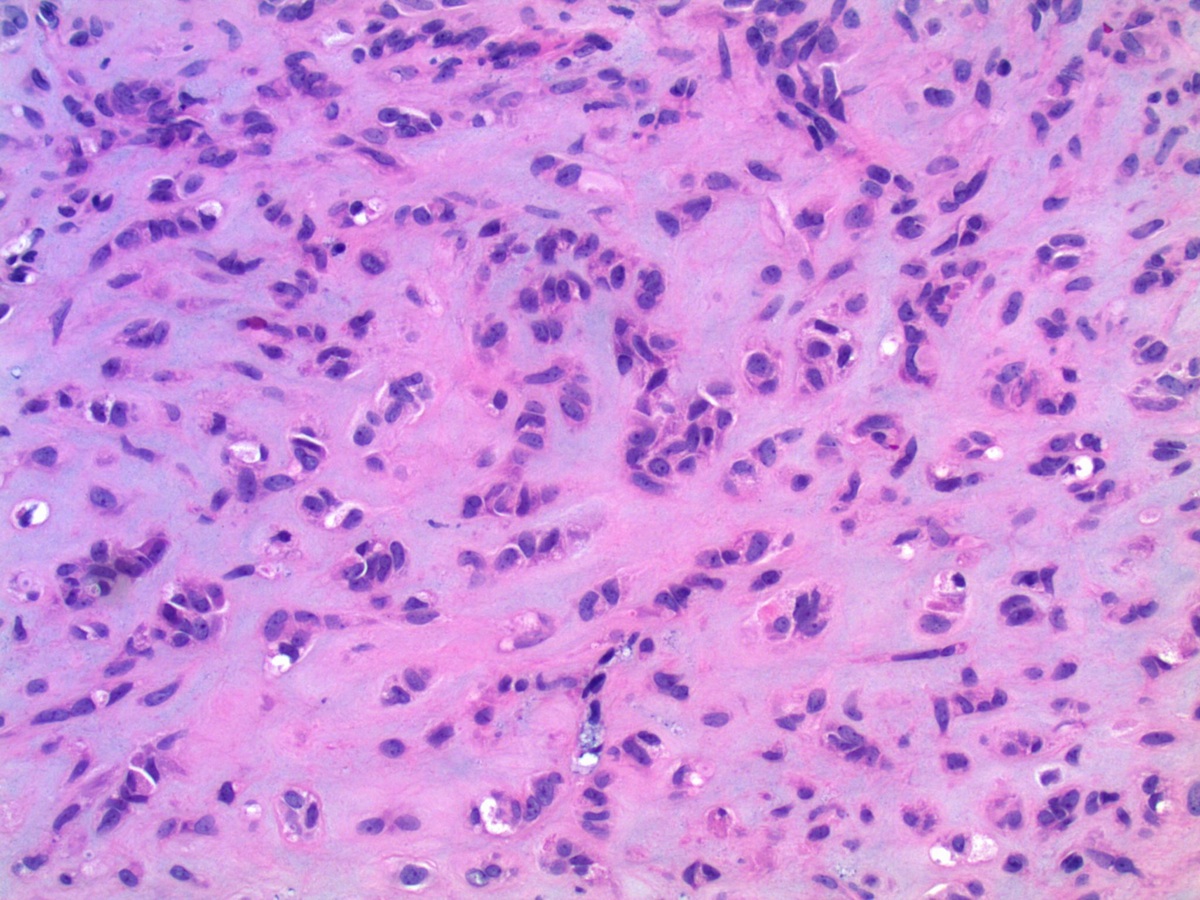
Microscopic images:
What is your diagnosis?
Diagnosis: Endometrioid adenocarcinoma, corded and hyalinizing pattern
Discussion:
In 2005, Young et. al. described uterine endometrioid carcinomas with epithelial cords, spindle cells and a hyalinized stroma that sometimes formed osteoid, mixed with classic endometrial carcinoma, which they termed corded and hyalinized endometrioid carcinoma (Am J Surg Pathol 2005;29:157). The mean patient age was 52 years and 65% were stage I, despite the appearance of a sarcoma. In addition, 70% exhibited squamous differentiation and 50% had background endometrial hyperplasia. Unusual features included cords of cells with a hyalinized of loose fibromyxoid stroma, and areas of diffuse spindle cells resembling endometrial stroma or even smooth muscle. Two - thirds of the tumors were grade 1 and the remainder were grade 2.
The classic endometrial carcinoma component was keratin positive, with weaker / variable staining in the epithelial cords. The cords were negative for muscle markers (desmin, actin), CD10, inhibin and p53. A subsequent study showed nuclear beta catenin expression and complete loss of membranous E-cadherin expression in all cases, due to mutation of exon 3 of the beta catenin gene in spindled or corded areas (Histol Histopathol 2009;24:149). These patients have a good prognosis after hysterectomy, with 83% alive with no evidence of disease at follow up in the original study.
The differential diagnosis includes carcinosarcoma / MMMT, which is a common pitfall. Unlike endometrioid carcinoma with corded, hyalinized and spindle cell elements, carcinosarcoma has high grade carcinomatous and sarcomatous components, and an aggressive clinical course. Of note, in this case the biopsy was signed out initially as carcinosarcoma. Other diagnoses to consider include uterine tumor resembling ovarian sex cord tumors and epithelioid smooth muscle tumors. Of note, an ovarian serous carcinoma with this corded and hyalinized pattern was recently described (Arch Pathol Lab Med 2013;137:275).
All cases are archived on our website. To view them sorted by case number, diagnosis or category, visit our main Case of the Month page. To subscribe or unsubscribe to Case of the Month or our other email lists, click here.
Thanks to Dr. Ankur Sangoi, El Camino Hospital (California), for contributing this case. This case was reviewed in May 2020 by Dr. Jennifer Bennett, University of Chicago and Dr. Carlos Parra-Herran, University of Toronto.
Website news:
(1) Each month, we add new Board Review questions, courtesy of BoardVitals, which are accessible via our CME page.
Visit and follow our Blog to see recent updates to the website.
(1) Each month, we add new Board Review questions, courtesy of BoardVitals, which are accessible via our CME page.
Visit and follow our Blog to see recent updates to the website.
Case #294
Clinical history:
A 43 year old woman presented with uterine bleeding, leading to an endometrial biopsy. She subsequently underwent a total abdominal hysterectomy.
Microscopic images:
What is your diagnosis?
Click here for diagnosis and discussion:
Diagnosis: Endometrioid adenocarcinoma, corded and hyalinizing pattern
Discussion:
In 2005, Young et. al. described uterine endometrioid carcinomas with epithelial cords, spindle cells and a hyalinized stroma that sometimes formed osteoid, mixed with classic endometrial carcinoma, which they termed corded and hyalinized endometrioid carcinoma (Am J Surg Pathol 2005;29:157). The mean patient age was 52 years and 65% were stage I, despite the appearance of a sarcoma. In addition, 70% exhibited squamous differentiation and 50% had background endometrial hyperplasia. Unusual features included cords of cells with a hyalinized of loose fibromyxoid stroma, and areas of diffuse spindle cells resembling endometrial stroma or even smooth muscle. Two - thirds of the tumors were grade 1 and the remainder were grade 2.
The classic endometrial carcinoma component was keratin positive, with weaker / variable staining in the epithelial cords. The cords were negative for muscle markers (desmin, actin), CD10, inhibin and p53. A subsequent study showed nuclear beta catenin expression and complete loss of membranous E-cadherin expression in all cases, due to mutation of exon 3 of the beta catenin gene in spindled or corded areas (Histol Histopathol 2009;24:149). These patients have a good prognosis after hysterectomy, with 83% alive with no evidence of disease at follow up in the original study.
The differential diagnosis includes carcinosarcoma / MMMT, which is a common pitfall. Unlike endometrioid carcinoma with corded, hyalinized and spindle cell elements, carcinosarcoma has high grade carcinomatous and sarcomatous components, and an aggressive clinical course. Of note, in this case the biopsy was signed out initially as carcinosarcoma. Other diagnoses to consider include uterine tumor resembling ovarian sex cord tumors and epithelioid smooth muscle tumors. Of note, an ovarian serous carcinoma with this corded and hyalinized pattern was recently described (Arch Pathol Lab Med 2013;137:275).