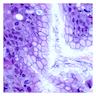
Helicobacter pylori, a carcinogen of gastric cancer
Some information below is from the Nobel Prize lecture given by J. Robin Warren in 2005. (The Nobel Prize: J. Robin Warren - Nobel Lecture [Accessed 25 January 2022])
First discovery of Helicobacter pylori (H. pylori) in gastric and pyloric ulcers, precancer lesions in the stomach
- Before the era of flexible endoscope (i.e., pre-1970s), there was no good quality stomach biopsy; thus, description of gastric pathological features was limited.
- Robin Warren, an Australian pathologist, was interested in gastric pathology and began his study of Whitehead's description and classification of active gastritis. (J Clin Pathol 1972;25:1)
- In 1979 flexible endoscope was available at his institution, thus Warren was able to examine good quality gastric biopsies from patients with gastritis.
- Warren observed histological changes described by Whitehead and found an unusual blue line on the surface of the inflamed gastric tissue.
- On high magnification of this surface, he observed numerous small, curved bacilli. (Lancet 1983;1:1273)
- At that time, the Warthin-Starry silver stain was successfully utilized to detect spirochetes but there were not many other stains available for detecting bacteria in tissue; Warren experimented with the gastritis tissue and this silver stain and found small, curved, spiral bacilli attached to the mucosal surface.
- To learn more about these bacteria he then examined the biopsies under electron microscopy and found that the bacteria resembled Campylobacter.
- Although he was unsure about the significance, from then on he always documented this finding in his pathology reports.
- In approximately half of the gastric biopsies, he found an association between the presence of this bacterium and histological gastritis in a severe and active form.
Points of disbelief from specialists
- It was argued that these bacteria were caused by gastritis and not vice versa.
- "If it is true, why were they not recognized before?"
- Scientists of the time believed that the stomach was sterile because its acid would likely kill all the gastric bacteria.
- These disbeliefs came from the lack of a clinicohistopathological correlation study.
A clinical trial study establishing the causal relationship between H. pylori and duodenal ulcer
- The clinical importance of this association was revealed when a gastroenterologist named Barry Marshall joined Warren to conduct a blinded clinical trial; in order to test their hypothesis they obtained gastric biopsies (including normal gastric antrum tissue) from a hundred outpatients to determine if there was a presence of the bacteria in the normal tissue.
- In addition to histologic examination, the tissues were cultured using Campylobacter techniques.
- The trial resulted in unexpected findings (Lancet 1984;1:1311):
- Bad breath and burping were related only to gastritis or bacteria.
- The bacterium was found to present in 100% of duodenal ulcer and 77% in gastric ulcer. This means that duodenal ulcer was strongly related to this infection.
- A new species was identified - Helicobacter pylori.
- After the trial, these findings were published. (Lancet 1984;1:1311)
Inventing assays for detecting H. pylori and the first introduction of triple therapy
- Marshall did additional work such as inventing CLOtest, serology and breath test, and triple therapy for duodenal ulcers in 1984.
- Marshall and Arthur Morris used Koch's postulates to prove the strong causal relationship between H. pylori and duodenal ulcer. (Med J Aust 1985;142:436)
More studies exploring and supporting the causal relationship between H. pylori and gastric cancer
- In addition to causing chronic gastritis and gastric ulcer, H. pylori is identified as a carcinogenic agent of gastric cancer with sufficient evidence in humans. (IARC: Agents Classified by the IARC Monographs [Accessed 25 January 2022])
- H. pylori infection is strongly associated with localized stage gastric MALToma or MALT lymphoma. (Gut Liv 2016;10:706, United European Gastroenterol J 2016;4:395)
Effect of H. pylori eradication on gastric cancer treatment and prevention
- H. pylori eradication can cure 60 - 80% of low stage MALT lymphoma that does not contain a t(11,18) translocation. (Gut 2017;66:6, Gut 2012;61:507)
- Early gastric cancers that are limited to mucosa and submucosa can be prevented from metachronous gastric cancers by H. pylori eradication. (N Engl J Med 2018;378:1085)
- H. pylori eradication therapy reduced 9.2% of gastric cancers in Japan, as demonstrated over 4 years of national insurance coverage for this therapy. (Helicobacter 2017;22:e12415)
Microscopic (histologic) images
Videos
Helicobacter: the ease and difficulty of a new discovery