Table of Contents
Definition / general | Epidemiology | Sites | Clinical features | Diagnosis | Case reports | Treatment | Clinical images | Gross description | Microscopic (histologic) description | Microscopic (histologic) images | Positive stains | Differential diagnosis | Additional referencesCite this page: Rishi A, Cornish TC. Granuloma inguinale. PathologyOutlines.com website. https://www.pathologyoutlines.com/topic/anusgranulomainguinale.html. Accessed April 19th, 2024.
Definition / general
- Synonym "donovanosis"
- Causative organism was previously classified as Calymmatobacterium granulomatosis; subsequent molecular characterization reclassified the causative organism as Klebsiella granulomatis
- Gram negative, nonmotile and encapsulated organism
- May extend to perianal region
Epidemiology
- Most common in tropical regions, no gender preference
- Bacterial infection associated with sexually transmitted disease or via childbirth with infected genital tract
- Development of lesion requires repeated exposure because of low pathogenicity of organism
- Fewer than 100 cases reported annually in United States
- Untreated lesions may have superadded infections, progression to extensive fibrosis, obstruction of lymphatic vessels and massive lymphedema
Sites
- Penile ulcers (sulcocoronal and balanopreputial)
- Labia minora
- Fourchette
- Cervix (uncommon)
Clinical features
- Median incubation period is ~50 days but exact incubation period is unknown
- There are four predominant types of clinical presentations:
- Nodular
- Ulcerovegetative
- Cicatricial
- Verrucous
- The lesion starts as an elevated nodular or papular area which then progresses to anulcerated lesion with communicating satellite nodules and ulcerations
- Anal involvement is more common in men
- Extragenital involvement occurs in minority of cases (6%) and results from direct or local spread
Diagnosis
- Made by swabbing the lesion and Giemsa staining of the air dried smear
- Other stains that may be used are Warthin-Starry, Gram stain, Toluidine blue and Leishman stain
- Recommended to acquire specimen at base or edge of ulceration or by aspirating enlarged regional lymph node
- Culture of the organism is difficult and needs specialized methods using human peripheral blood mononuclear cells or Hep - 2 cells
- Polymerase chain reaction and indirect immunofluorescence are available but not commonly used
Case reports
- 46 year old man with cutaneous metastases of rectal mucinous adenocarcinoma mimicking granuloma inguinale (Intern Med 2012;51:2479)
- HIV+ patient with malignant transformation (Dermatol Online J 2008;14:8)
Treatment
- Either trimethoprim / sulfamethoxazole or tetracyclines (doxycycline) for at least 3 weeks (choice is based on allergies, pregnancy or other clinical conditions)
- Resistant lesions are treated longer
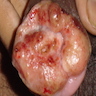
Gross description
- Varies based on age of lesion and immunosuppression
- Ulceration with ragged beefy red edges and indurated base
- Ulcer size ranges from 0.5 cm to 5 cm
- Usually multiple ulcers
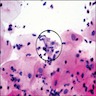
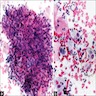
Microscopic (histologic) description
- Marked reactive changes in surface epithelium secondary to inflammation and ulceration; marked pseudoepitheliomatous hyperplasia adjacent to ulcer
- Numerous histiocytes and plasma cells, with fewer neutrophils and lymphocytes
- Granulomatous inflammation, neutrophilic microabscesses (particularly in ulcer bed)
- Large vacuolated / foamy macrophages / histiocytes with multiple intracytoplasmic organisms (bacteria are called Donovan bodies, not the histiocytes; have bacillary or coccobacillary appearance); Donovan bodies may be extracellular
- Acute and chronic granulation tissue, fibrosis (dermal and subcutaneous cicatricial) in late stages
- Prominent lymphatic channels
Microscopic (histologic) images
Positive stains
Differential diagnosis
- Infectious causes may have overlapping histology as well as clinical presentations:
- Chancroid
- Herpes simplex
- Lymphogranuloma venereum
- Syphilis
- Tuberculosis (can case massive lymphedema-like donovanosis) (J Med Case Rep 2010;4:369)
- Squamous cell carcinoma: may grossly as well as clinically resemble the ulcerative and verrucous type of granulomas inguinale lesions