Table of Contents
Definition / general | Essential features | Terminology | ICD coding | Epidemiology | Sites | Pathophysiology | Etiology | Clinical features | Diagnosis | Radiology description | Radiology images | Prognostic factors | Case reports | Treatment | Gross description | Gross images | Microscopic (histologic) description | Microscopic (histologic) images | Positive stains | Electron microscopy description | Molecular / cytogenetics description | Molecular / cytogenetics images | Videos | Sample pathology report | Differential diagnosis | Additional references | Practice question #1 | Practice answer #1 | Practice question #2 | Practice answer #2Cite this page: Tariq MU, Ud Din N. Parosteal osteosarcoma. PathologyOutlines.com website. https://www.pathologyoutlines.com/topic/boneparostealosteo.html. Accessed August 26th, 2025.
Definition / general
- Parosteal osteosarcoma (PO) is a rare malignant bone surface tumor
- Most common surface osteosarcoma
Essential features
- Most commonly occurs in third decade of life with slight female predominance; commonly involves metaphysis of long bones
- Radiologically, tumor is a lobulated, ossified mass attached to bone surface with radiologic intact periosteum
- Microscopically, tumor shows lamellar and woven bony trabeculae with intervening low grade spindle cell component; cartilage component is common and dedifferentiation is seen in some cases
- MDM2 and CDK4 gene amplification and immunohistochemical expression are hallmark and useful for diagnostic purpose
- Overall survival is excellent, with substantial risk of local recurrence and late distant metastasis
Terminology
- Juxtacortical osteosarcoma (not recommended)
ICD coding
- ICD-O: 9192/3 - parosteal osteosarcoma
- ICD-10: C41.9 - malignant neoplasm of bone and articular cartilage, unspecified
- ICD-11: 2B51.Z & XH8HG5 - osteosarcoma of bone and articular cartilage of unspecified sites & parosteal osteosarcoma
Epidemiology
- Age range: 9 - 75 years with peak incidence in third decade of life; slight female predominance
- Most common surface osteosarcoma; constitutes 4.5% of all osteosarcomas (Bone Joint J 2015;97:1698)
- No causal connection or association
Sites
- Commonly involves metaphysis of long bones
- Posterior aspect of distal femur is the most common site (~70% of cases), followed by proximal tibia and proximal humerus
- Less frequently involved sites include fibula, radius, ulna, scapula, ilium, ribs, metatarsals, metacarpals, maxilla, mandible, etc. (Hum Pathol 2019;91:11)
Pathophysiology
- Characteristic molecular aberration in parosteal osteosarcoma is the presence of supernumerary ring chromosome(s) containing amplified material encoding MDM2 and CDK4 genes (Genes Chromosomes Cancer 2010;49:518)
Etiology
- Unknown
Clinical features
- Slow growing tumor; symptom duration is typically > 1 year and may remain undetected for 15 years
- Usually painless swelling; can be painful in some cases
- May be associated with restricted movements at associated joints
- Dedifferentiated tumors present with shorter symptom duration
- Tumor size range: 1.2 - 29 cm; mean: 7.6 cm (Hum Pathol 2019;91:11)
Diagnosis
- Plain radiographs, CT scan and MRI scan confirm tumor location at bone surface
- Incisional / open biopsy is done to histologically confirm the diagnosis before undergoing tumor excision
- Reference: Int J Surg Oncol (N Y) 2017;2:e50
Radiology description
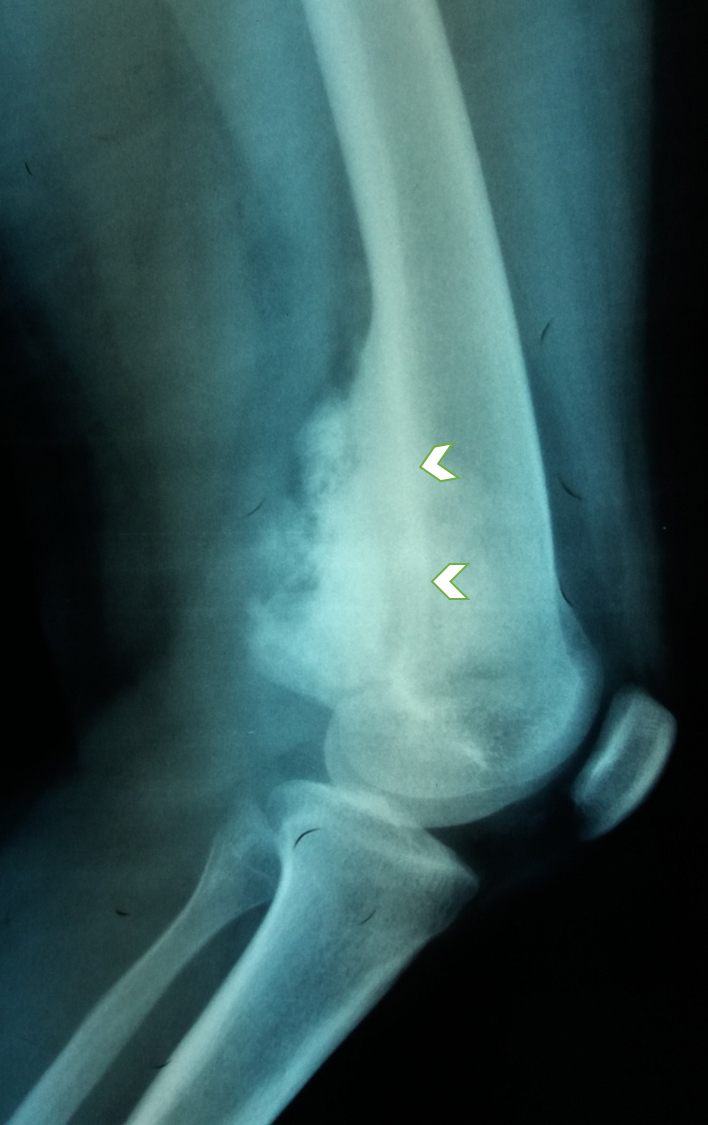
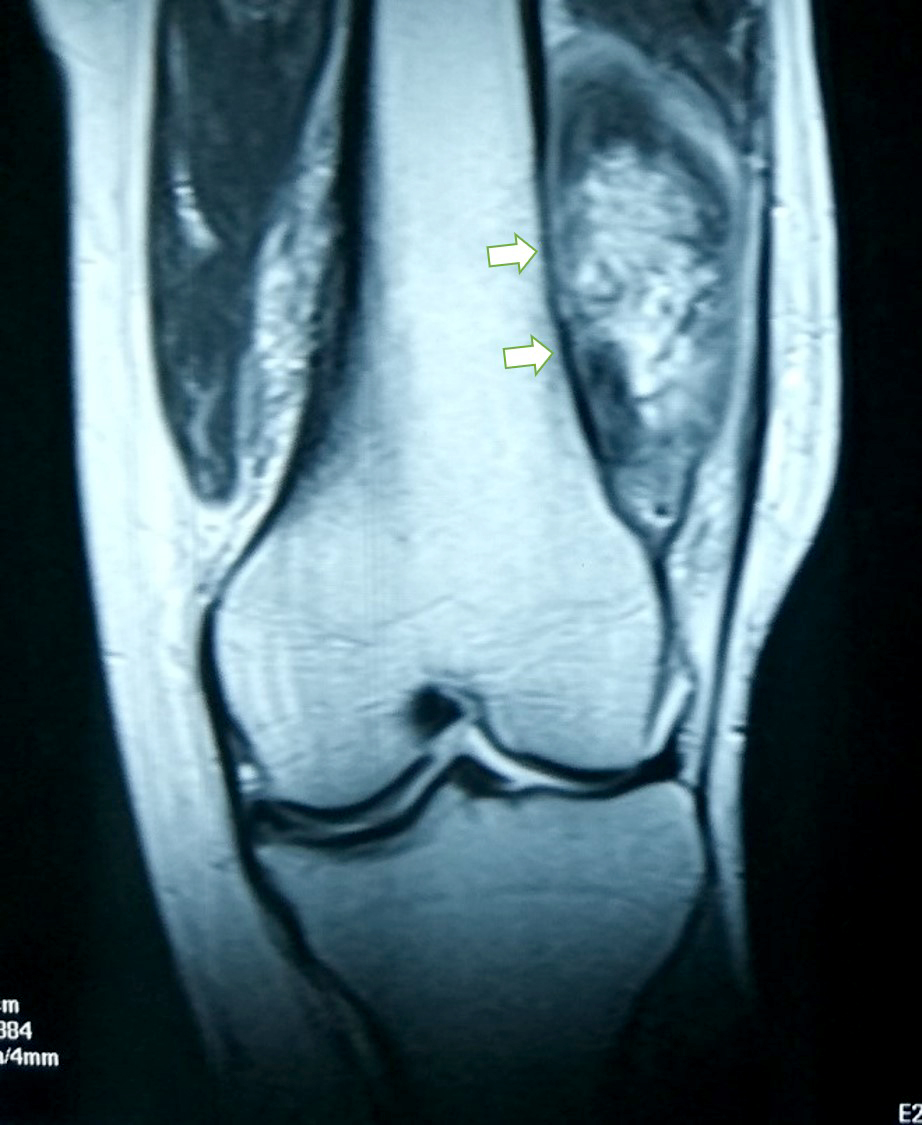
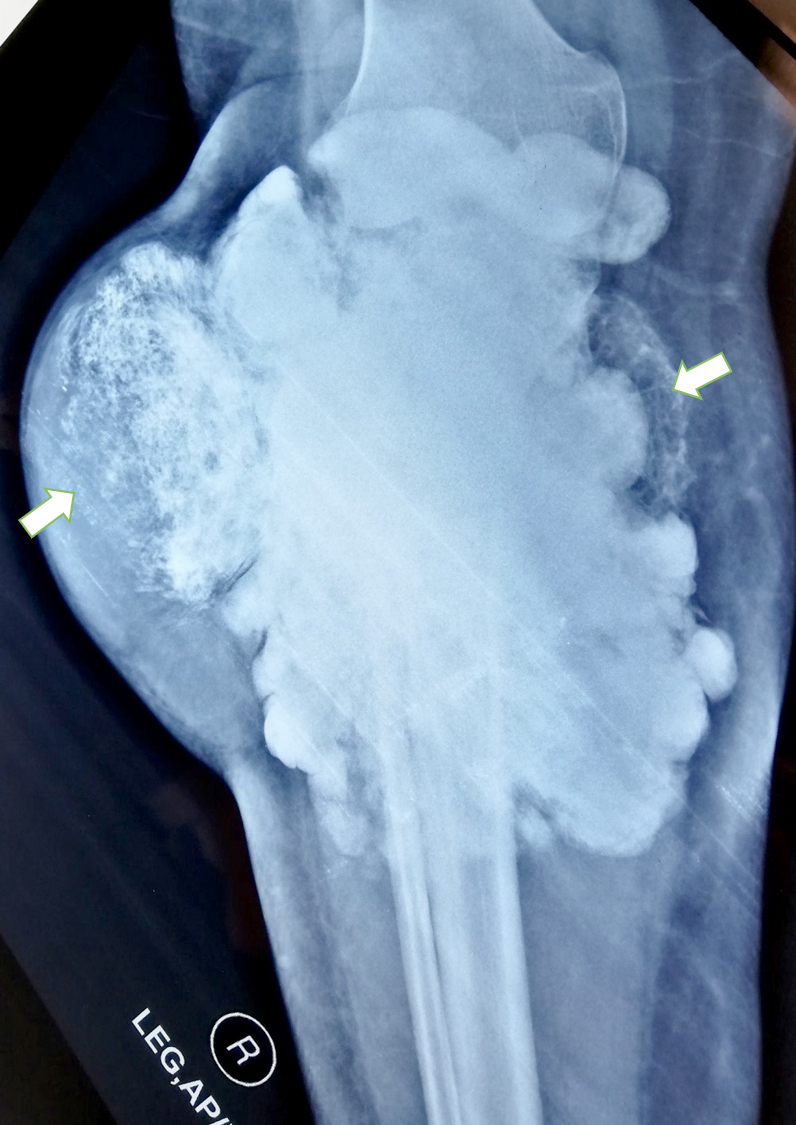
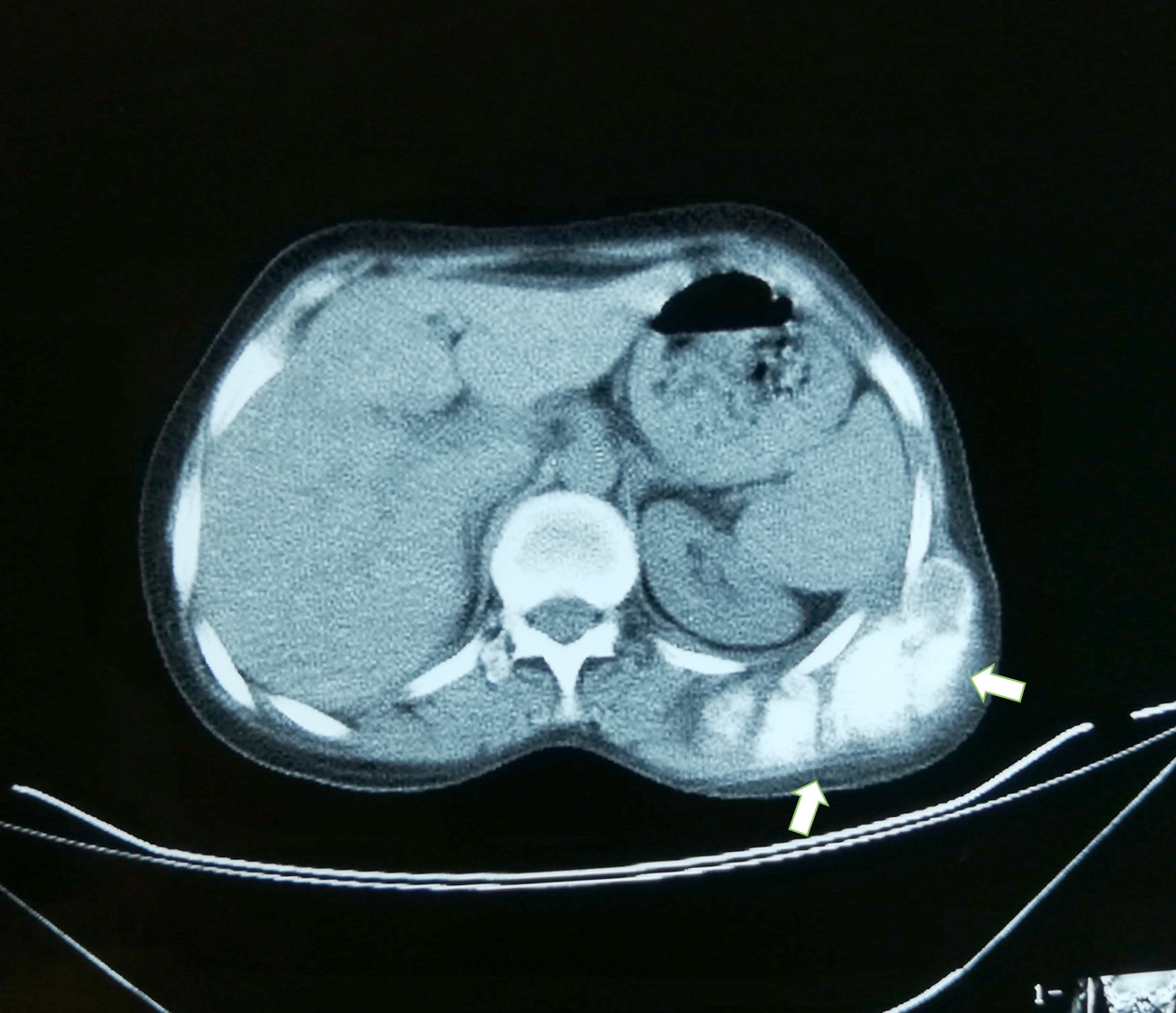
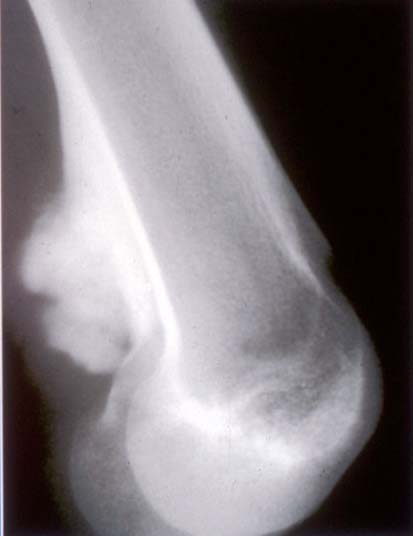
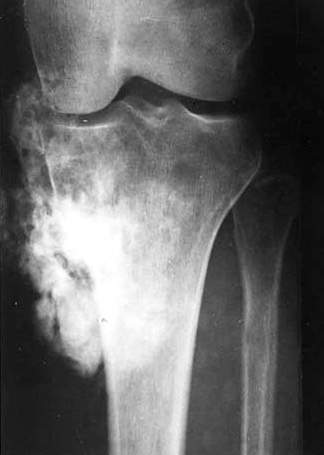
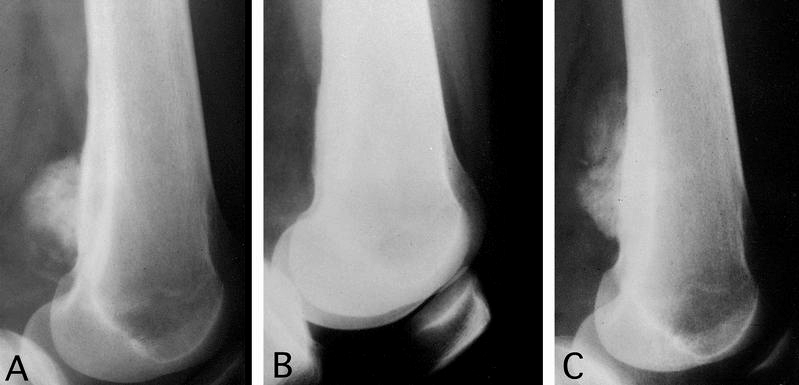
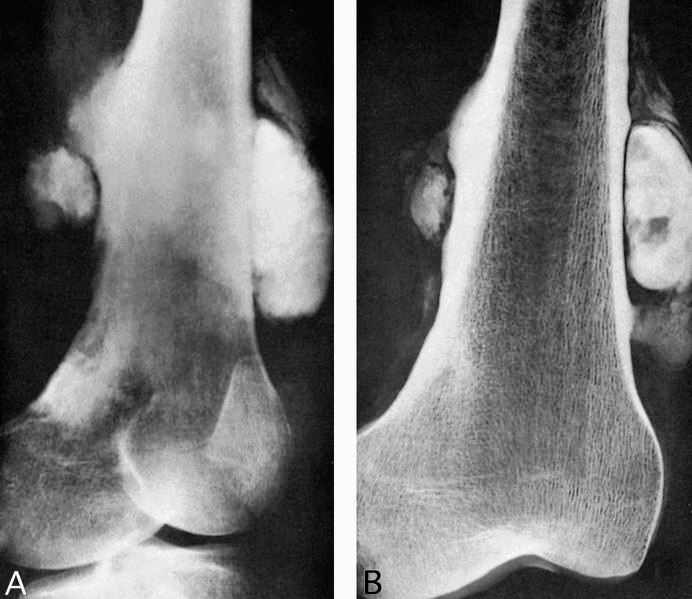
- Plain radiograph: lobulated, sessile, mineralized mass attached to the bone surface through a pedicle with thin radiolucent cleavage plane of intact periosteum; no periosteal reaction is seen
- CT scan findings: cortical changes and intramedullary extension
- MRI scan findings: intramedullary extension, dedifferentiated component, cartilage component at tumor surface
- MRI scan is more sensitive for detection of medullary involvement, while CT scan is more specific (Int J Biol Markers 2020;35:31)
Radiology images
Prognostic factors
- Overall 5 year survival rate is 91.8% and 10 year survival rate is 87.8% (Bone Joint J 2015;97:1698)
- Prognosis of conventional parosteal osteosarcoma is better than conventional osteosarcoma, while the prognosis of dedifferentiated parosteal osteosarcoma is similar to conventional osteosarcoma
- Recurrence rate up to 23% has been observed
- Higher in incompletely or marginally resected tumors
- Develops after a long term interval
- Distant metastatic rate up to 19% has been observed
- Higher in dedifferentiated tumors
- Develops after a long term interval (Skeletal Radiol 2021;50:301)
- Female gender and young age are good prognostic factors (Bone Joint J 2015;97:1698)
- Poor prognostic features include dedifferentiation, medullary involvement, distant metastasis and local recurrence
Case reports
- 9 year old boy with conventional parosteal osteosarcoma of femur treated with chemotherapy (Pediatr Blood Cancer 2016;63:1471)
- 23 year old woman with tumor of tibia having well differentiated liposarcoma-like component (Skeletal Radiol 2021;50:243)
- 28 year old woman with tumor of femur showing telangiectatic dedifferentiation (Skeletal Radiol 2000;29:597)
- 35 year old woman with pancreatic metastasis (Case Rep Oncol 2021;2021:983)
- 45 year old woman with dedifferentiated tumor of the maxilla (J Med Case Rep 2018;12:235)
Treatment
- En bloc resection with clear margins is recommended for low grade, localized tumors
- Amputation is performed in occasional cases
- Adjuvant chemotherapy is usually administered in tumors with higher grade, dedifferentiation and local recurrence; no obvious benefit on survival (Bone Joint J 2015;97:1698)
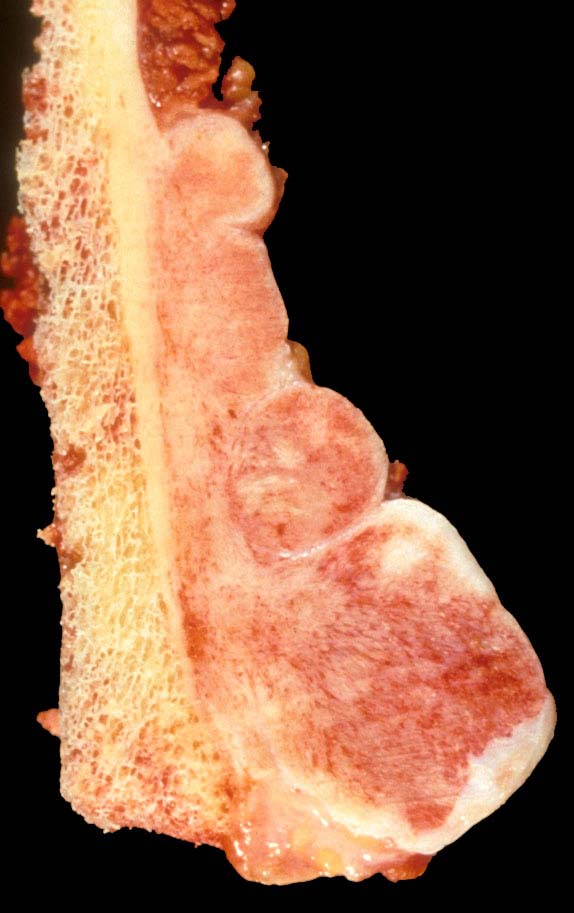
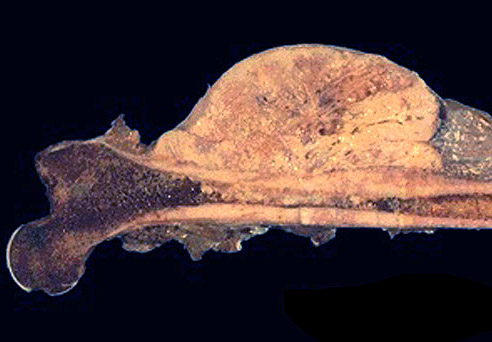
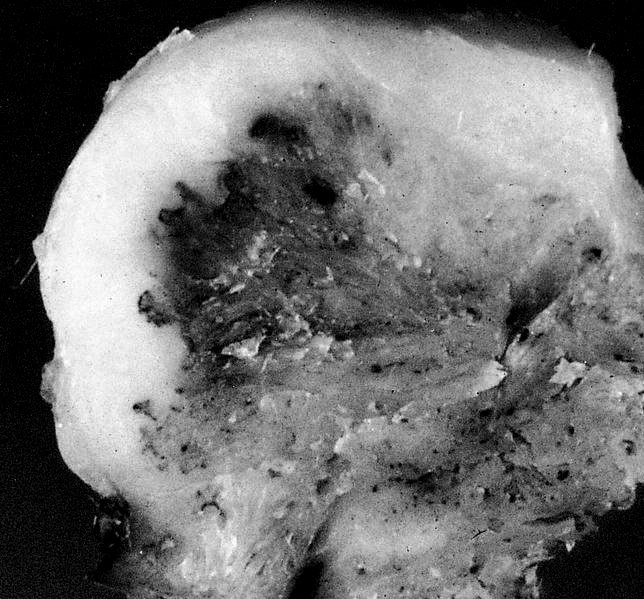
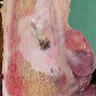
Gross description
- Lobulated mass attached to the outer surface of the bone by a broad pedicle; may invade into bone, involve medullary cavity or encircle the bone
- Satellite nodules can be seen, especially in recurrent tumors
- Cut surface may appear grey, white fibrous, cartilaginous or bony hard, depending on the different tumor components (Am J Clin Pathol 2000;114:S90)
- Dedifferentiated areas may appear soft and fleshy
- Cartilage cap may be grossly appreciable
Gross images
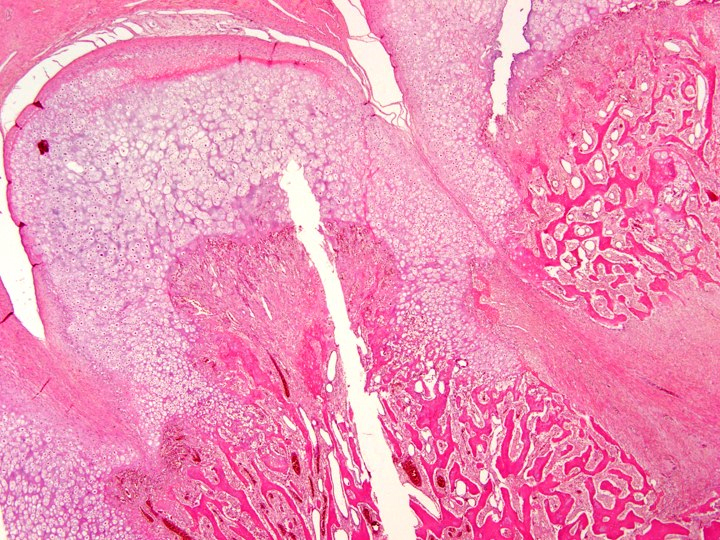
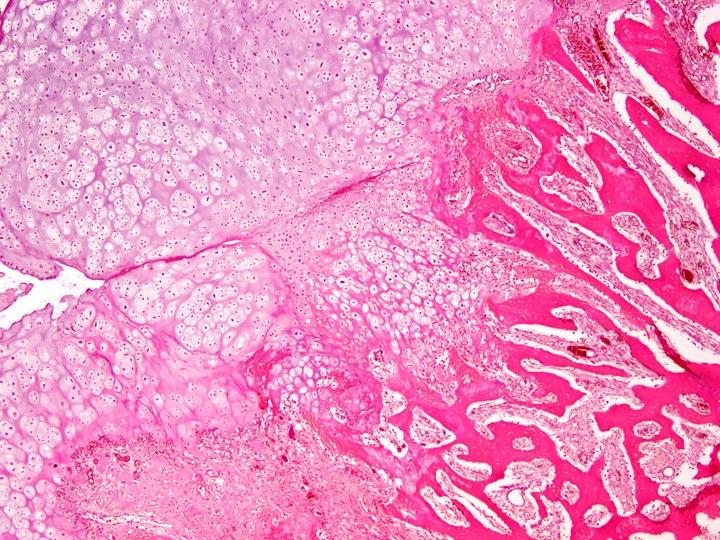
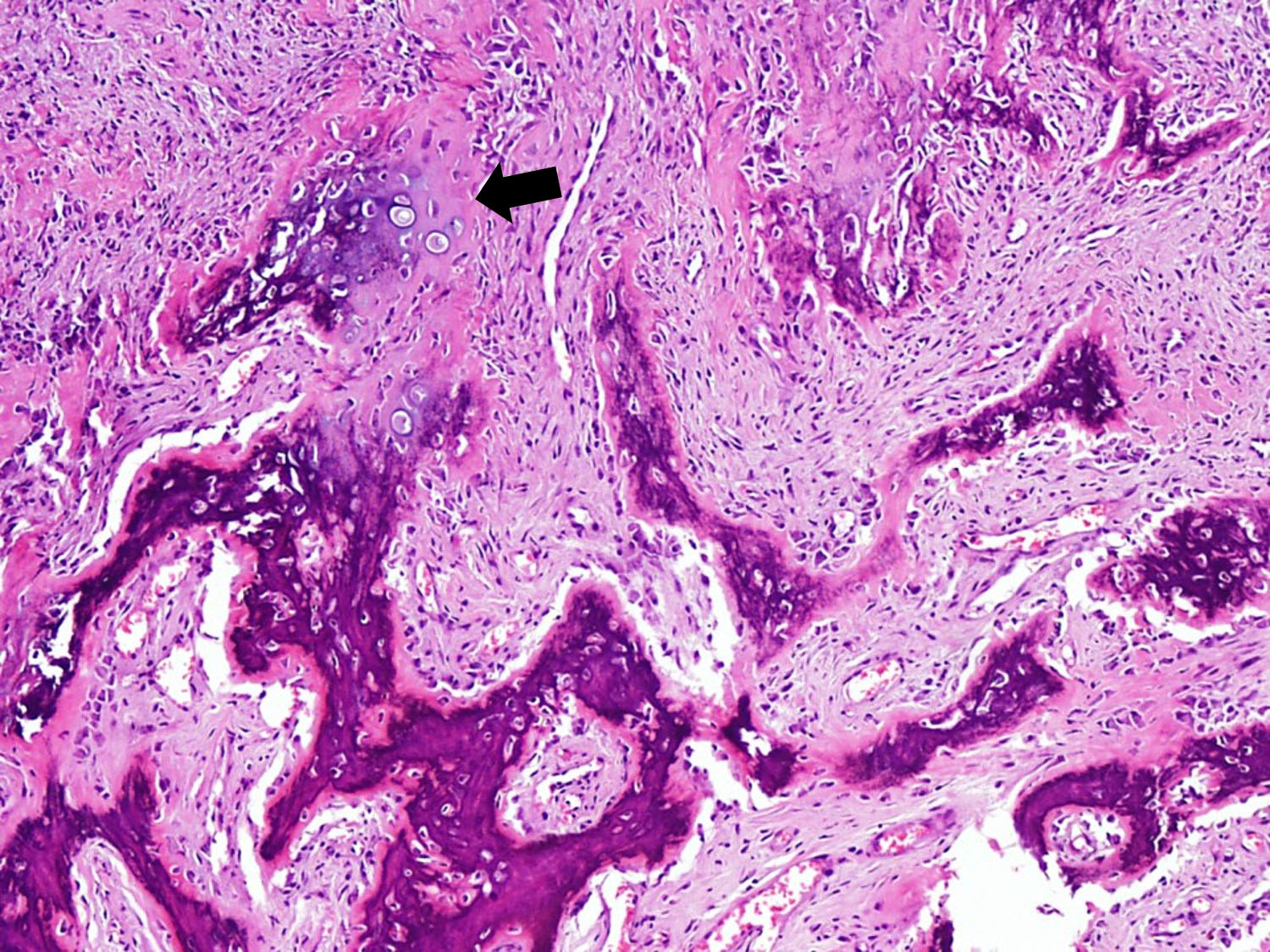
Microscopic (histologic) description
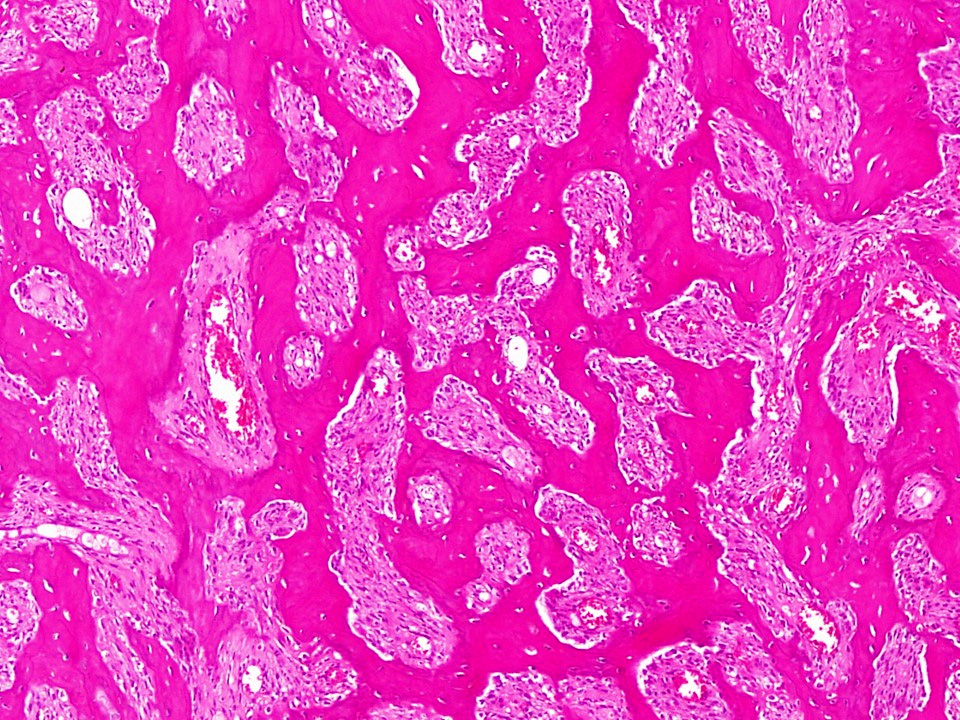
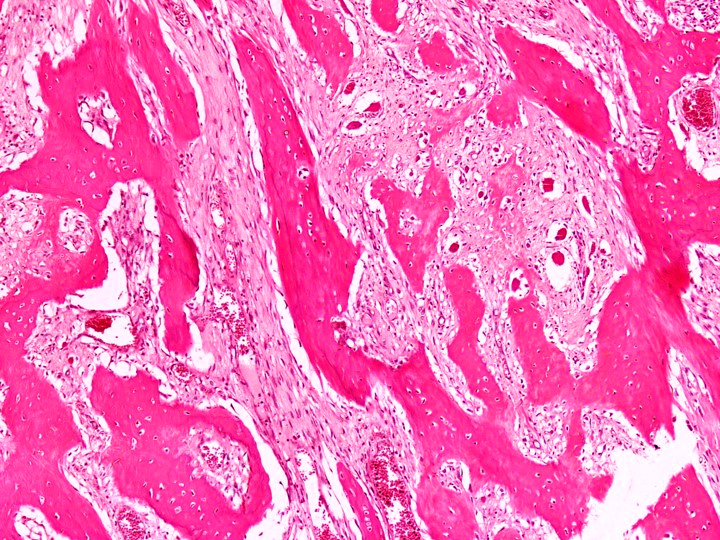
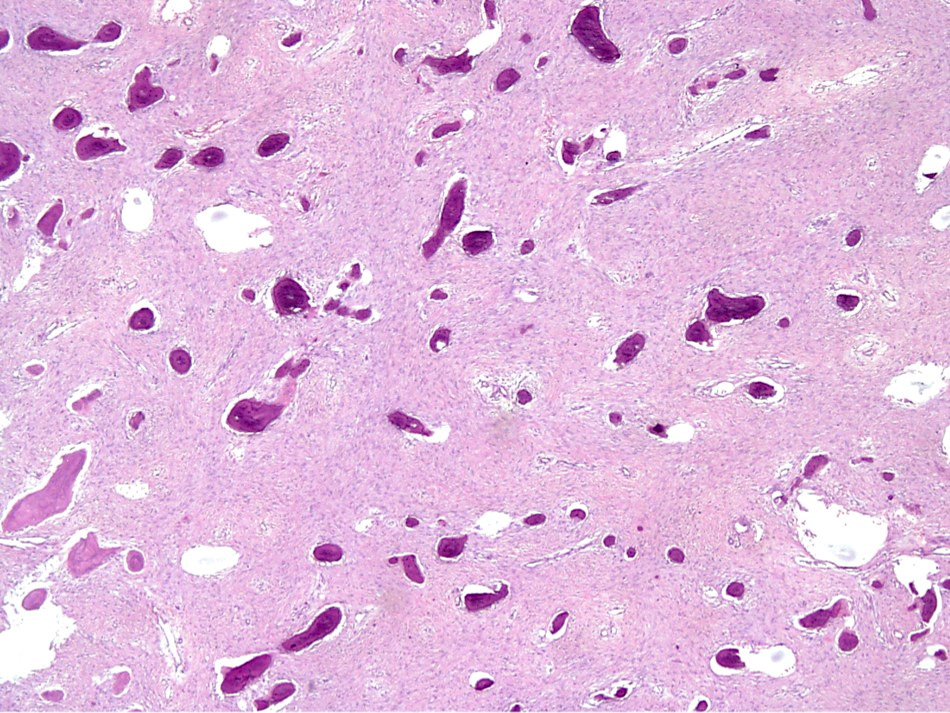
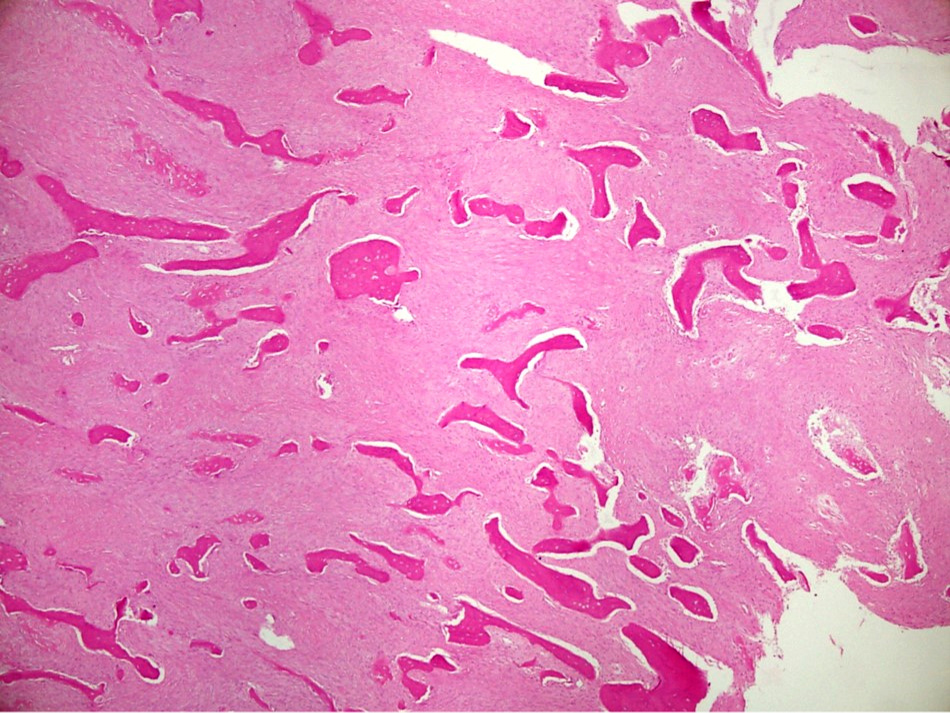
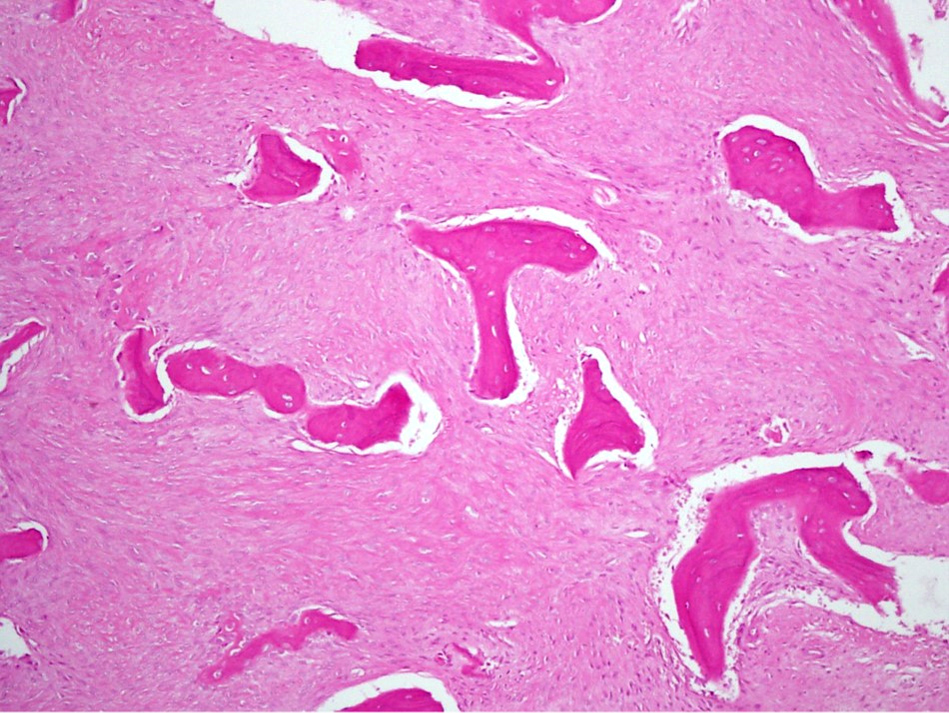
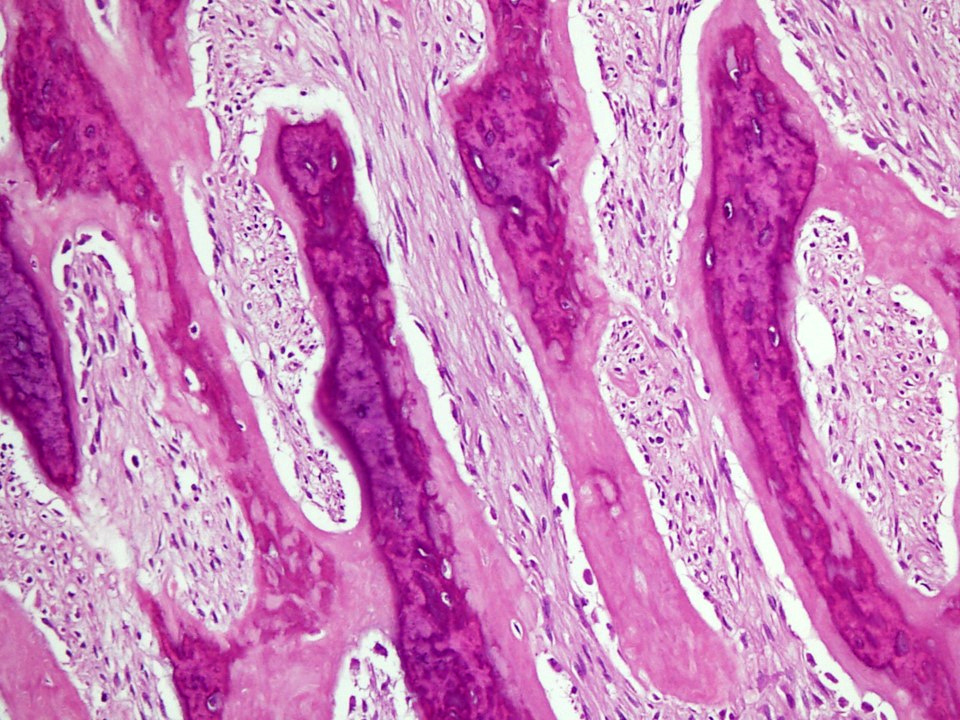
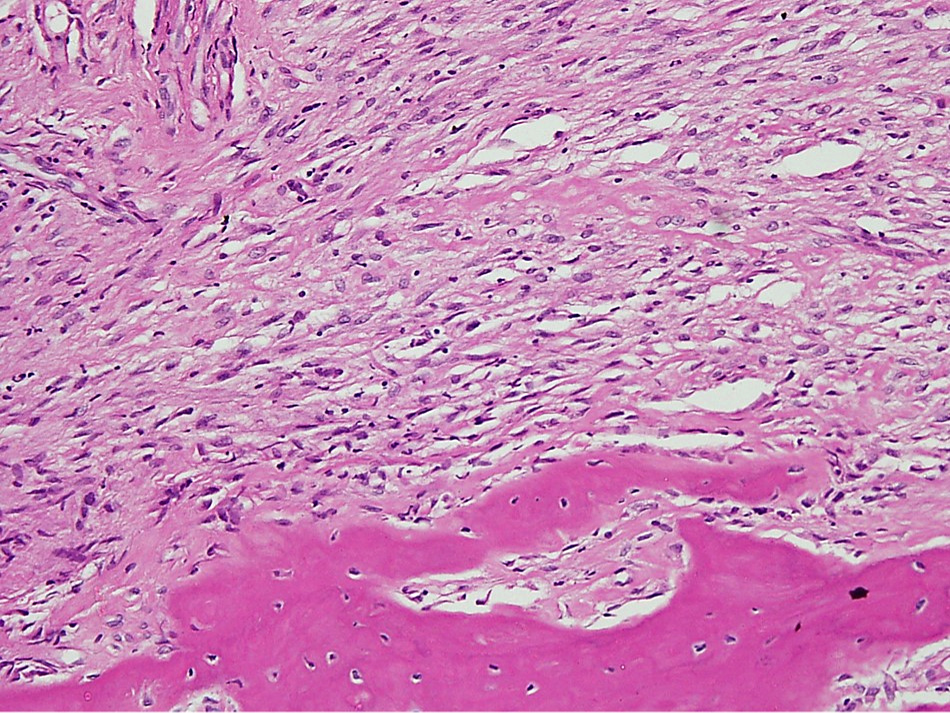
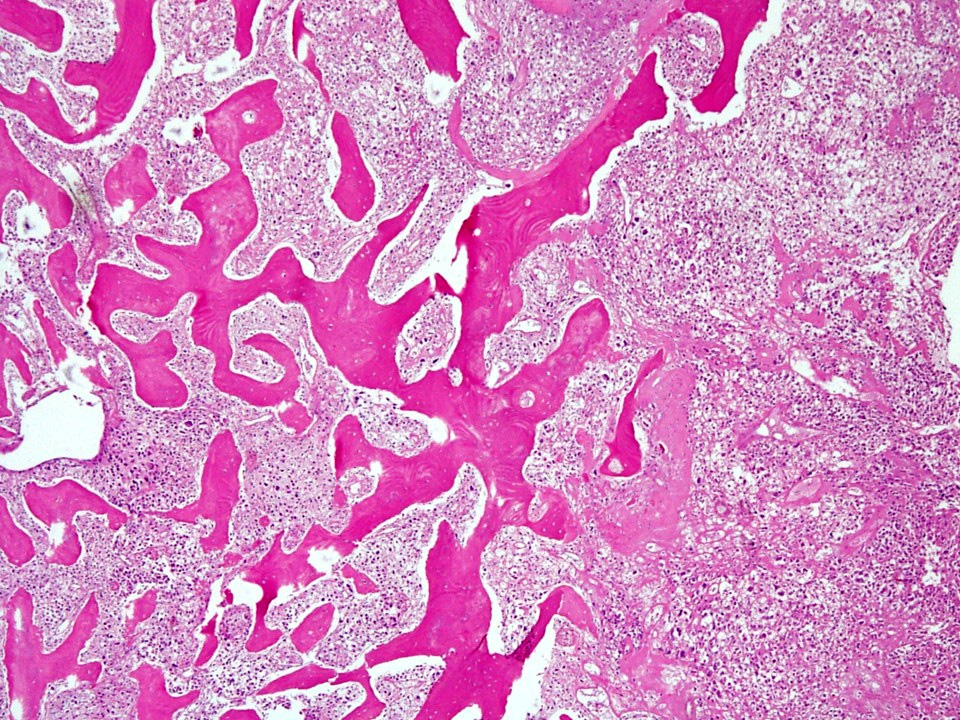
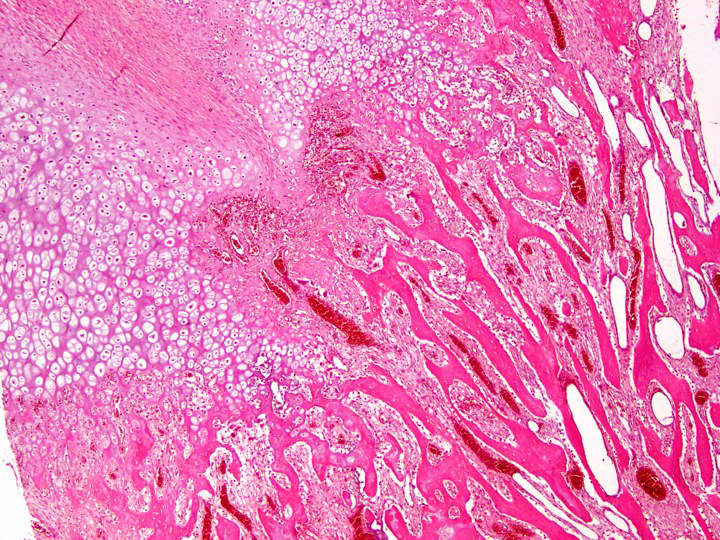
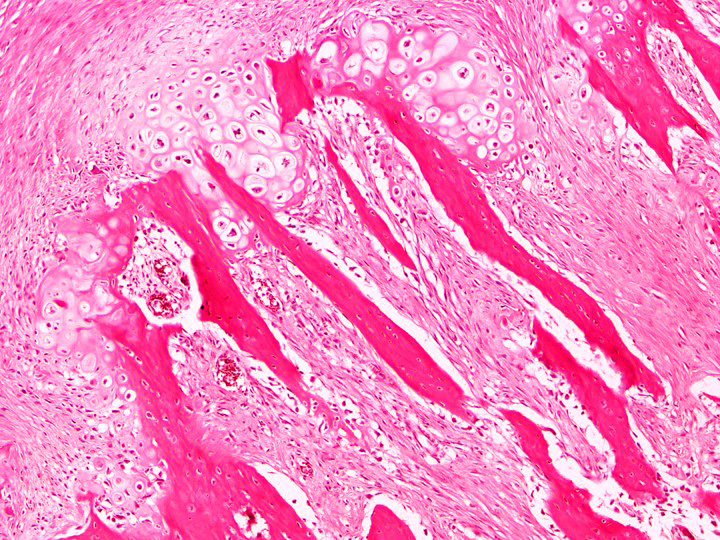
- Tumor has 2 basic components: bone trabeculae and spindle cells
- Spindle cells are typically arranged as fascicles in intertrabecular spaces and show low cellularity, minimal atypia, low mitotic count and hyalinized background
- Some tumors may show increased cellularity, higher nuclear grade and frequent mitotic activity
- Spindle cell component is graded I - III (according to Broder's grading system) on the basis of cellularity, nuclear pleomorphism and mitoses; this grading system is not routinely practiced since its prognostic value is still not well established (J Bone Joint Surg Br 1984;66:313, Journal of Solid Tumors 2016;6:17, J Bone Joint Surg Am 1977;59:632)
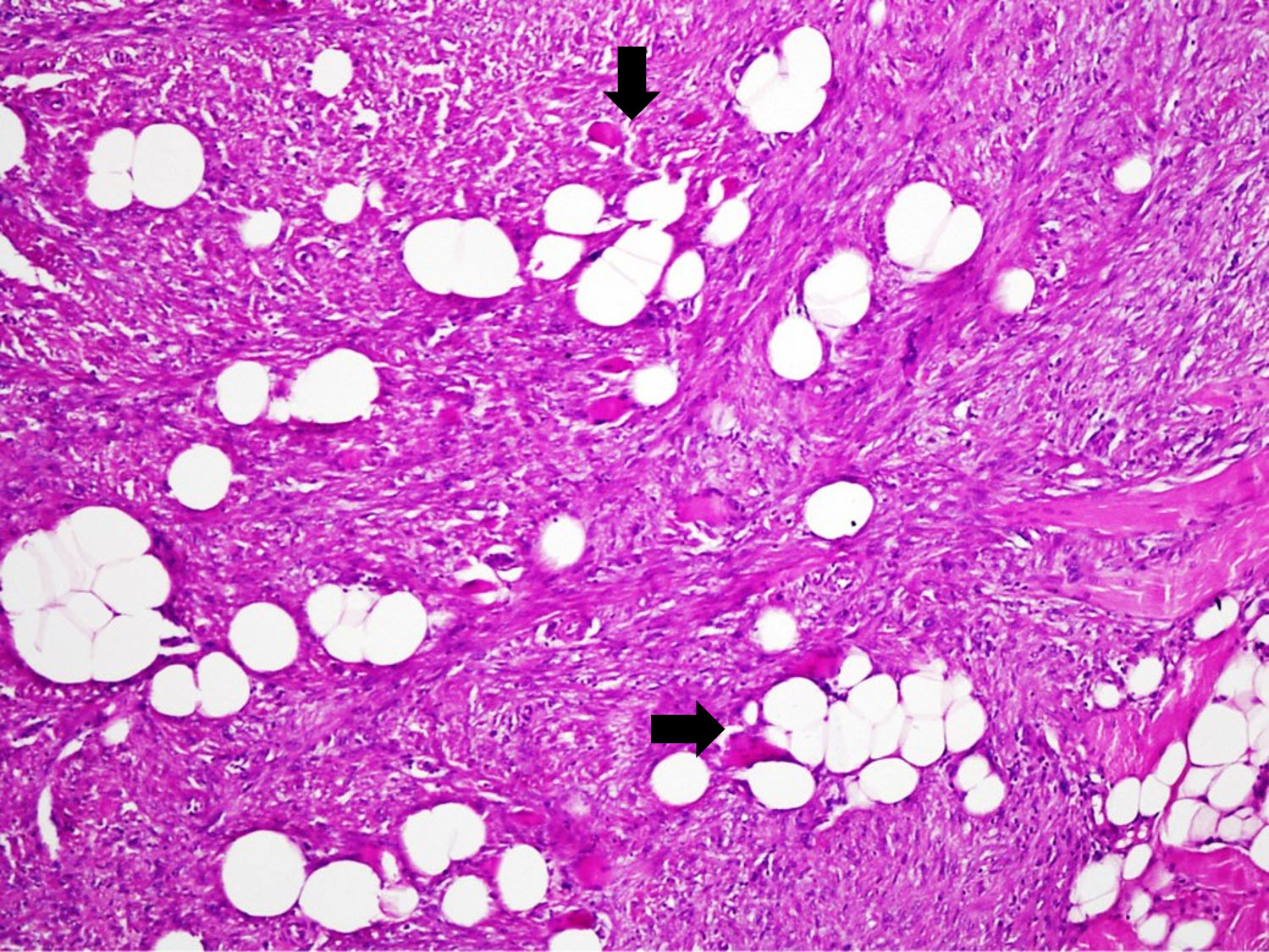
- At the periphery, spindle cells increase in cellularity and infiltrate into fat and muscle fibers; may take the form of spindle cell nodules
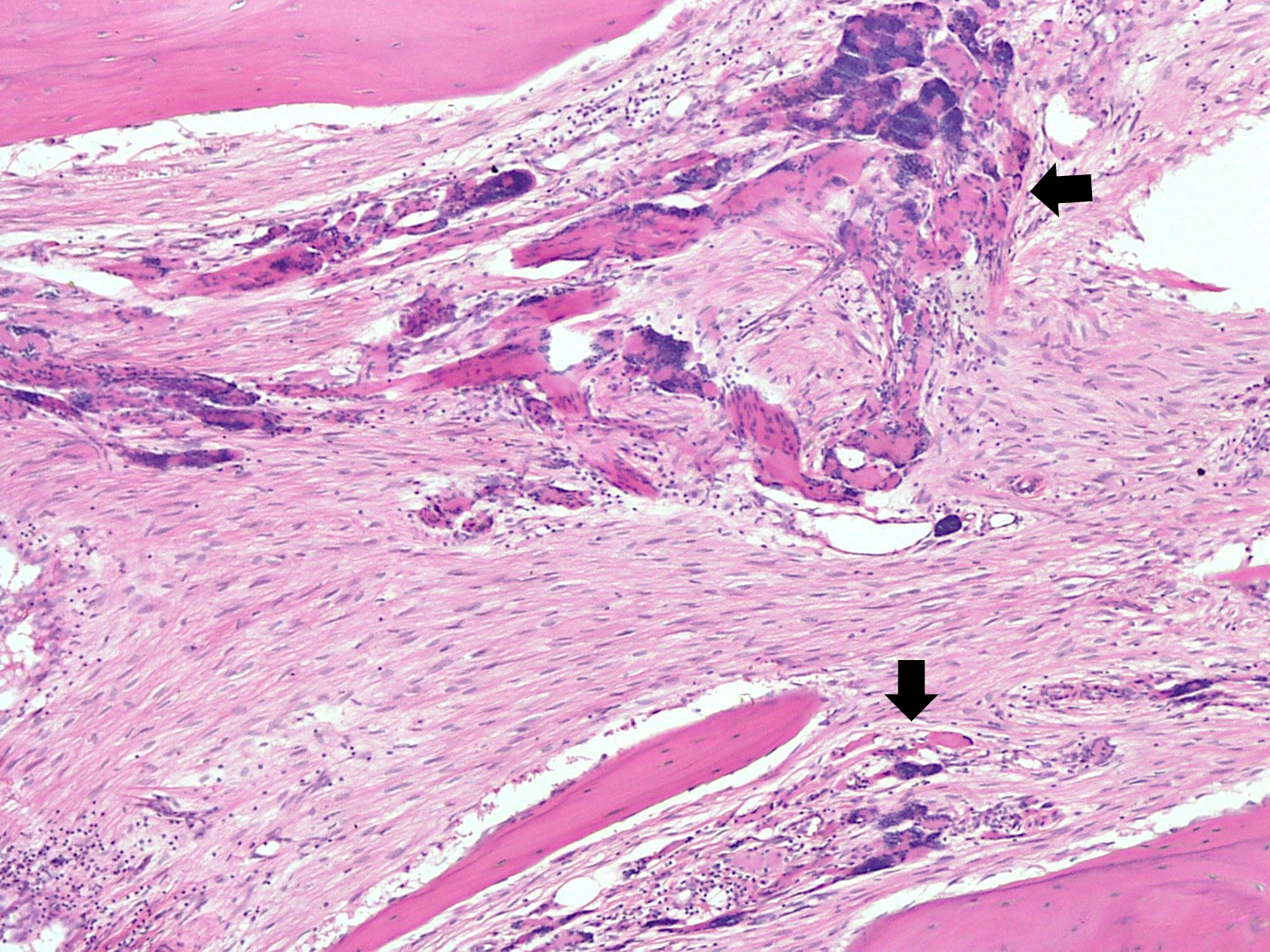
- Bone trabeculae are commonly parallel streams of lamellar bone; interconnected trabeculae and woven bone may also be present and osteoblastic rimming may or may not be seen
- Parallel streams of bone are seen in ~61% of cases
- Medullary involvement in present in 35% of cases
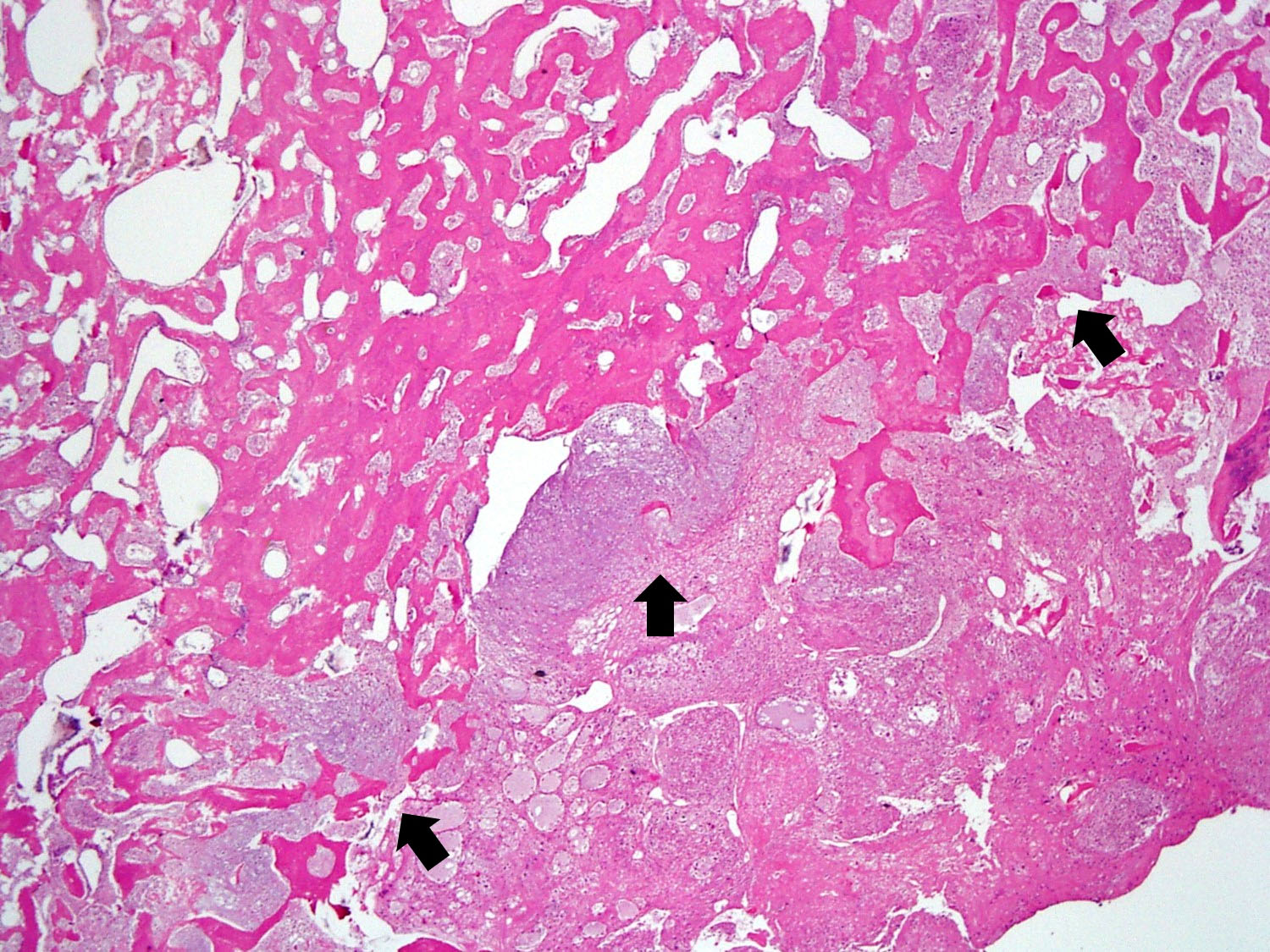
- Dedifferentiation is observed in 15 - 43% of cases; primary or recurrent tumors may show features of osteosarcoma, undifferentiated spindle cell sarcoma, chondroblastoma or rhabdomyosarcoma
- Cartilaginous component is present in 25 - 50% of cases in the form of peripheral cartilage cap or cartilage nodules within tumor (Journal of Solid Tumors 2016;6:17)
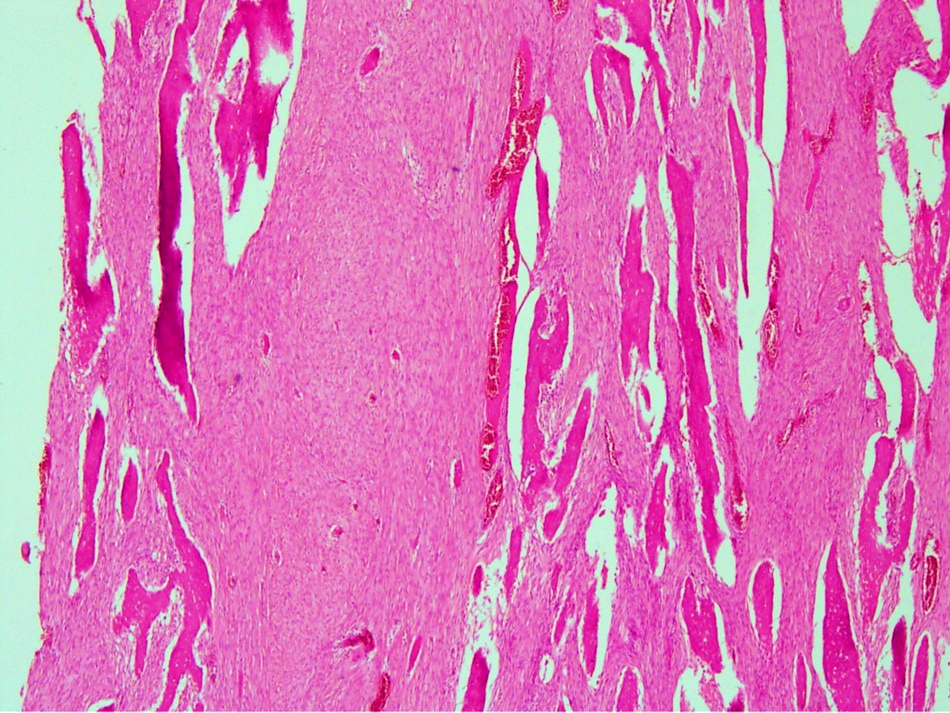
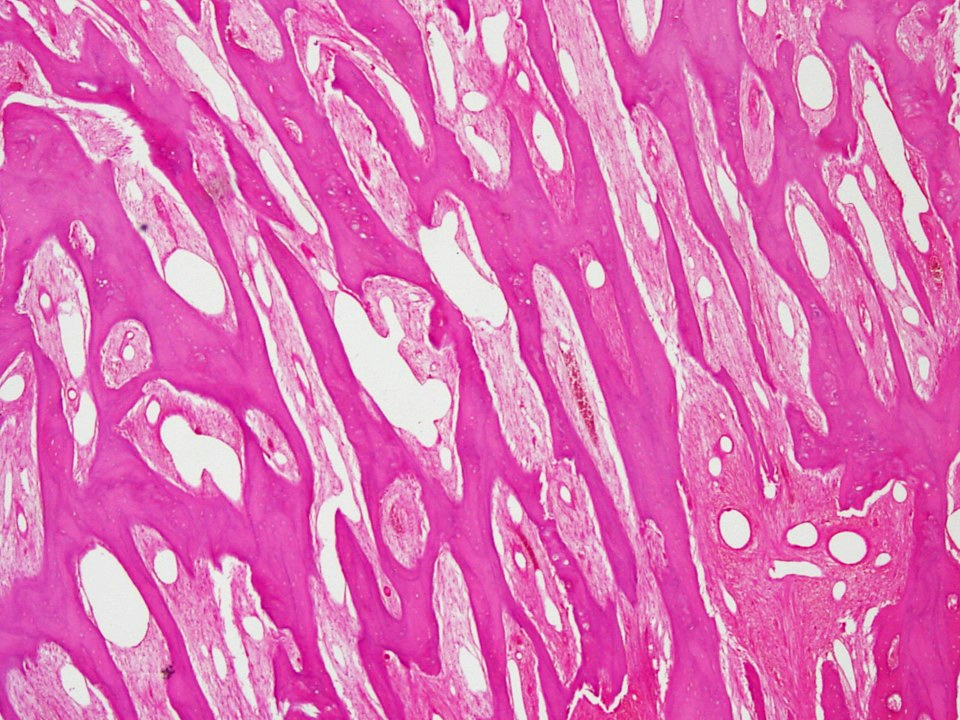
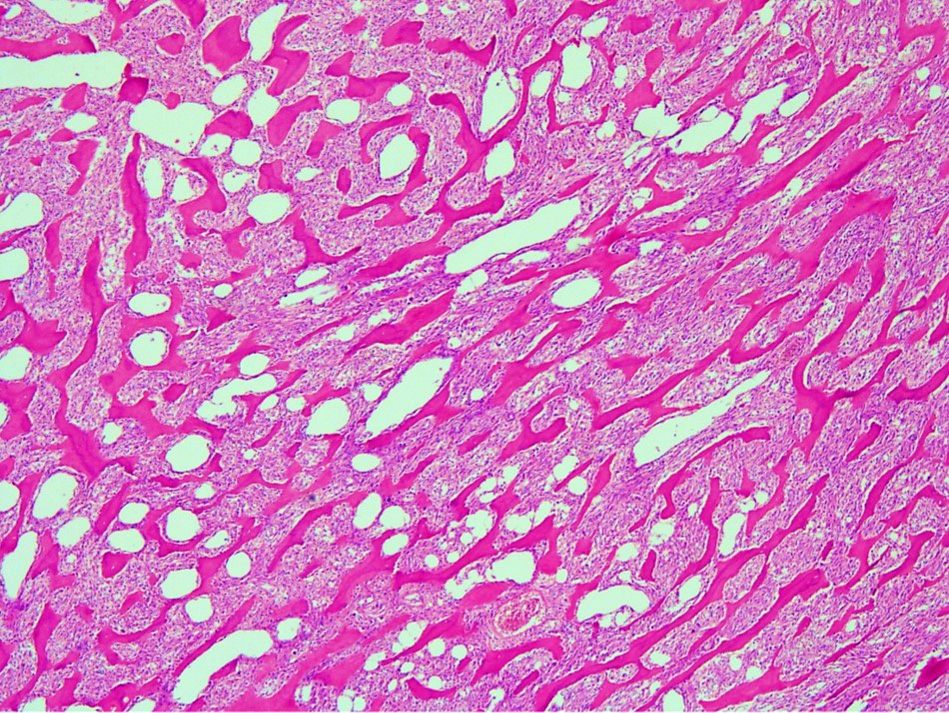
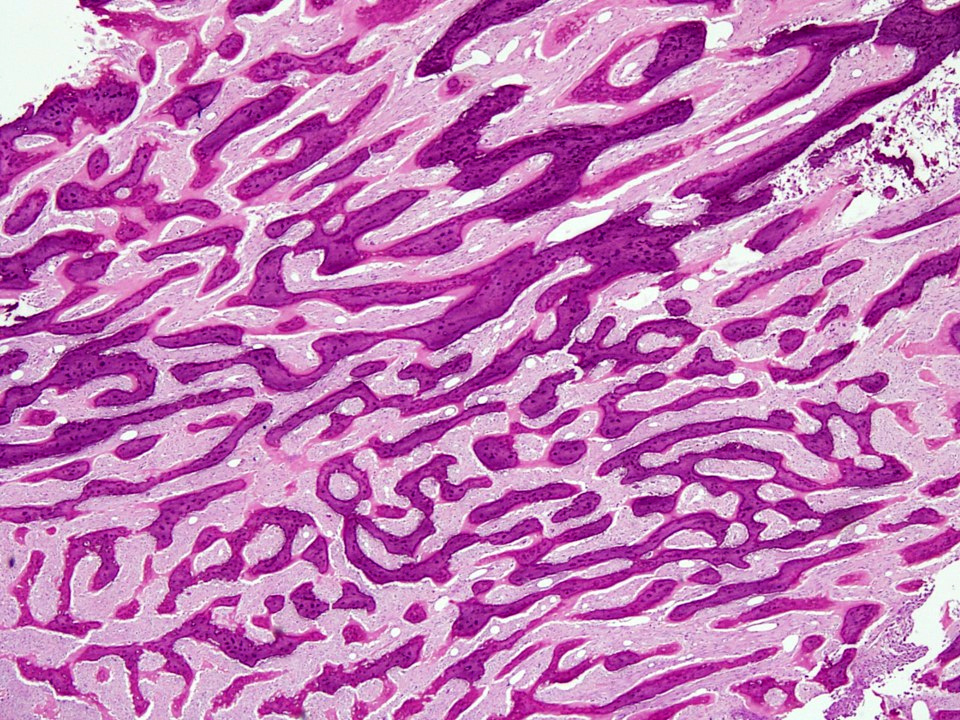
Microscopic (histologic) images
Contributed by Nasir Ud Din, M.B.B.S.
Positive stains
- MDM2 and CDK4 immunohistochemistry stains are positive in > 80% of cases (Mod Pathol 2011;24:624, Hum Pathol 2019;91:11)
Electron microscopy description
- Predominantly composed of myofibroblasts along with fibroblasts and some osteoblasts
- Tumor cells are separated by abundant intercellular matrix and collagen fibers (Cancer 1982;50:949)
- Cartilage component is normal
- Desmosomes may be seen between undifferentiated cells (Hum Pathol 1980;11:373)
Molecular / cytogenetics description
- Parosteal osteosarcoma is near diploid, cytogenetically characterized by one or more supernumerary ring chromosome(s), which contain(s) amplified material encoding MDM2 and CDK4 genes
- MDM2 and CDK4 gene amplifications are detected by FISH in > 85% of cases (Genes Chromosomes Cancer 2010;49:518)
- Activating GNAS mutations are also observed in 55% of cases (Am J Surg Pathol 2014;38:402)
Videos
Parosteal osteosarcoma
by Lewis Hassell
Parosteal osteosarcoma made easy by Vikram Deshpande
Sample pathology report
- Distal femur, wide local resection:
- Parosteal osteosarcoma, grade 1 (see comment)
- Tumor size: 7 x 5 x 3 cm
- Dedifferentiated component: absent
- Necrosis: absent
- Involvement of medullary cavity: absent
- Soft tissue and skeletal muscle invasion: present
- Margins of resection are negative, with sarcoma closest at … cm from … bone margin and at … cm from … soft tissue margin
- Pathologic TNM stage: pT1
- Comment: Radiographs show a heterogeneous ossified mass attached to the posterior aspect of the distal femur at the metaphyseal region. The tumor is hypocellular and composed of well formed bone trabeculae with intervening fascicles of spindle cells with minimal atypia and low mitotic activity. At the periphery of the tumor, the spindle cell component invades into the adjacent skeletal muscle. Progression to high grade sarcoma is not identified. The findings support the above diagnosis.
- The prognosis of parosteal osteosarcoma is excellent, with a 90% overall survival rate at 5 years. Wide local resection is curative for pure (low grade) parosteal osteosarcoma.
- pN: Not assigned (no nodes submitted or found); pM: Not applicable - pM cannot be determined from the submitted specimen
Differential diagnosis
- Fibrous dysplasia with exophytic growth (fibrous dysplasia protuberans):
- Ground glass appearance on radiology
- Lacks parallel streams of bone
- Lack of MDM2 gene amplification and immunohistochemistry is negative (Mod Pathol 2011;24:624)
- Low grade central osteosarcoma
- Low grade spindle cell component with neoplastic lamellar or woven bone in parallel or interanastomosing arrangement pattern
- Difficult to differentiate from conventional parosteal osteosarcoma histologically; positive expression for MDM2 and CDK4 IHC markers and gene amplifications
- Radiology is helpful; tumor location is central (intramedullary) and tumor is osteolytic or sclerotic rather than lobulated, radio opaque parosteal osteosarcoma at bone surface (World J Orthop 2013;4:327, Sarcoma 2012;2012:764796)
- Conventional osteosarcoma with periosteal spread:
- Difficult to differentiate from dedifferentiated parosteal osteosarcoma
- Absence of conventional parosteal osteosarcoma areas
- Aneuploidy, lack of ring chromosome and less frequent MDM2 and CDK4 amplification (Am J Surg Pathol 2012;36:423, Genes Chromosomes Cancer 2010;49:518)
- High grade surface osteosarcoma:
- Difficult to differentiate from dedifferentiated parosteal osteosarcoma
- Absence of conventional parosteal osteosarcoma areas
- Aneuploidy, lack of ring chromosome and lack of MDM2 and CDK4 amplification (Arch Pathol Lab Med 2014;138:694, Am J Surg Pathol 2012;36:423, Genes Chromosomes Cancer 2010;49:518)
- Osteochondroma:
- Continuity of tumor with underlying bone
- Perpendicular arrangement of chondrocytes
- Low cellularity, lack of atypia, presence of adipose tissue or marrow elements in intertrabecular spaces (Clin Sarcoma Res 2011;1:2)
- Myositis ossificans, florid reactive periostitis ossificans and bizarre parosteal ossifying periostitis (BPOP):
- Orderly maturation (zonation)
- Soft tissue component may show tissue culture-like areas (Journal of Solid Tumors 2016;6:17)
- Exuberant fracture callus:
- History and radiological evidence of fracture
- Lack of lamellar bone (Arch Pathol Lab Med 2014;138:694, Journal of Solid Tumors 2016;6:17)
- Desmoplastic fibroma:
- Lacks bony component (Arch Pathol Lab Med 2014;138:694)
Additional references
Practice question #1
A 29 year old woman had a painless swelling at the posterior aspect to knee. Xray of the knee joint showed a sessile tumor at the posterior surface of femur with underlying intact cortex. Microscopically, tumor showed a cartilage cap and interconnected bone trabeculae with intervening low grade spindle cell population. What is the most likely diagnosis?
- Conventional osteosarcoma
- Myositis ossificans
- Osteochondroma
- Parosteal osteosarcoma
- Periosteal chondroma
Practice answer #1
D. Parosteal osteosarcoma. The closest differential diagnosis is parosteal osteosarcoma and osteochondroma. In parosteal osteosarcoma, the intertrabecular spaces contain spindle cell component, while the intertrabecular spaces in osteochondroma contain hematopoietic precursors or adipocytes.
Comment Here
Reference: Parosteal osteosarcoma
Comment Here
Reference: Parosteal osteosarcoma
Practice question #2
Which of the following is the most important prognostic feature in parosteal osteosarcoma?
- Dedifferentiation
- Histologic grade
- Infiltration into adjacent soft tissue
- Necrosis
- Tumor size
Practice answer #2
A. Dedifferentiation is the most important prognostic feature. The prognosis of conventional parosteal osteosarcoma is better than conventional osteosarcoma, while the prognosis of dedifferentiated parosteal osteosarcoma is similar to conventional osteosarcoma.
Comment Here
Reference: Parosteal osteosarcoma
Comment Here
Reference: Parosteal osteosarcoma