Table of Contents
Definition / general | Essential features | Terminology | Epidemiology | Sites | Pathophysiology | Diagrams / tables | Clinical features | Diagnosis | Laboratory | Case reports | Treatment | Clinical images | Microscopic (histologic) description | Microscopic (histologic) images | Practice question #1 | Practice answer #1 | Practice question #2 | Practice answer #2Cite this page: Cotter T, Samra H. Fusobacterium necrophorum. PathologyOutlines.com website. https://www.pathologyoutlines.com/topic/microbiologyfnecrophorum.html. Accessed August 29th, 2025.
Definition / general
- Gram negative anaerobe; common oropharyngeal pathogen
- Taxonomy: genus Fusobacterium, species necrophorum, subspecies necrophorum / fundiliforme (GMS Infect Dis 2018;6:Doc03)
Essential features
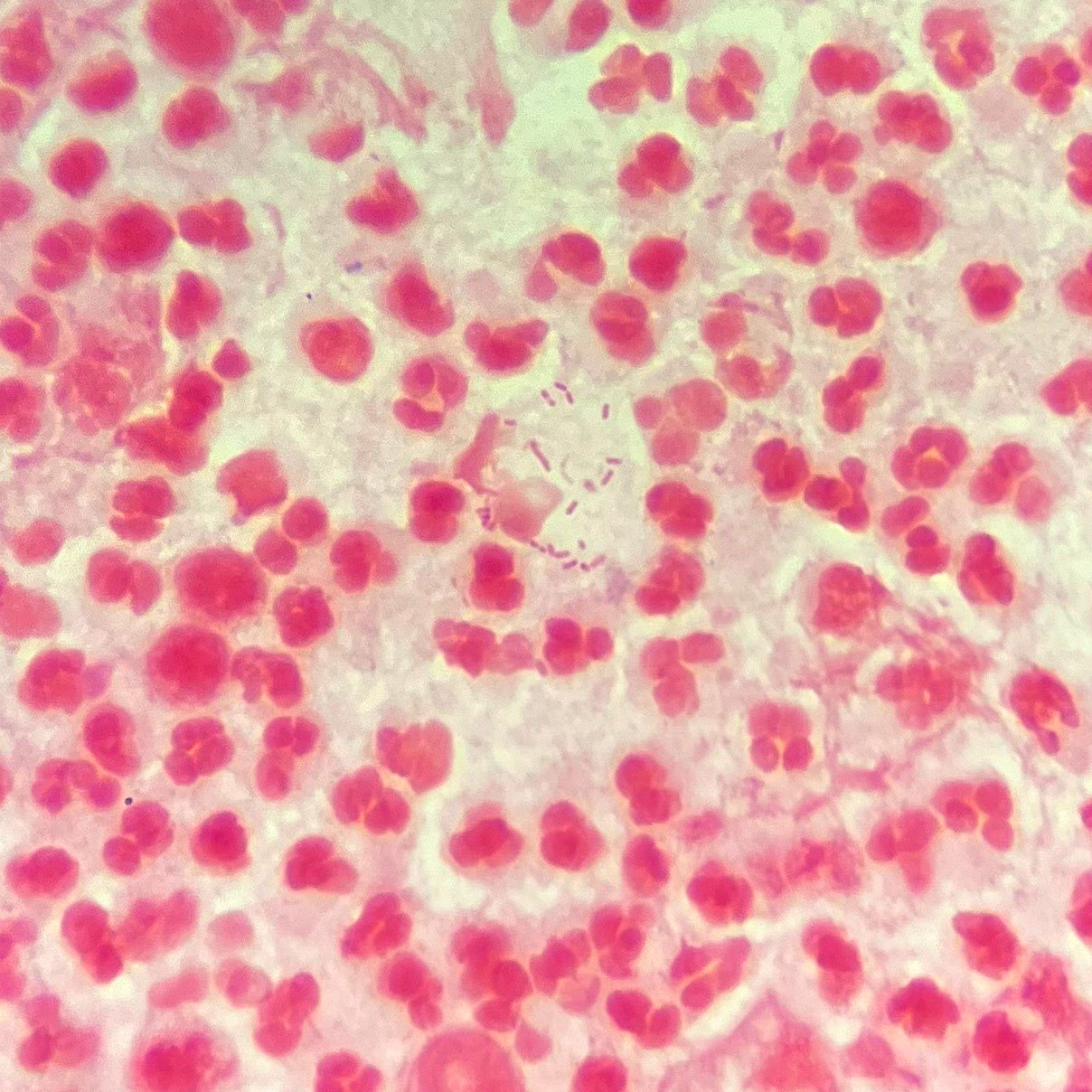
- Gram negative, rod shaped, obligate anaerobe; nonspore forming, nonmotile
- Most common causal agent of Lemierre syndrome; oropharyngeal infection leads to septic thrombophlebitis of the internal jugular vein
- Debated if commensal or exogenous invader of orophopharynx (Anaerobe 2006;12:165, Anaerobe 2015;34:120)
Terminology
- Lemierre syndrome: invasive F. necrophorum disease, postanginal sepsis, necrobacillosis
- Historical: nekrosebazillus (Anaerobe 2006;12:165)
- Postanginal: following a purulent pharyngitis or peritonsillar abscess
Epidemiology
- Lemierre syndrome is rare; F. necrophorum tonsillitis / pharyngitis rate of progression to Lemierre syndrome unknown
- Demographic: previously healthy adolescents and young adults, ages 14 - 24
- M:F = 2:1 (Anaerobe 2006;12:165)
- Trends: Lemierre syndrome dramatic increase in last several decades
- Decreased antibiotic use for sore throat
- Decreased indication for tonsillectomy (Clin Otolaryngol Allied Sci 2004;29:161)
- Mortality: 5 - 18% (Case Rep Crit Care 2016;2016:1264283)
Sites
- Oropharyngeal: acute tonsillitis, peritonsillar abscess
- Tonsillitis, historically called angina tonsillaris, hence postanginal sepsis
- Head and neck: acute otitis
- Spread to meninges / meningitis
- Female urogenital tract
- Metastasis from septic thrombophlebitis of the internal jugular vein
- Lungs: pneumonia from septic pulmonary emboli
- Joints: septic arthritis
- Heart: endocarditis (mortality: 75%) (Anaerobe 2015;34:120)
Pathophysiology
- Lemierre syndrome:
- F. necrophorum invades into adjacent internal jugular vein and causes nidus of septic thrombophlebitis (leukotoxin induces thrombosis by aggregating platelets) (Infect Immun 2002;70:4609)
- Thromboemboli travel hematogenously, causing pneumonia / pleural empyema / distant metastatic lesions (J Microbiol Immunol Infect 2020;53:513)
- Virulence factors:
- Endotoxins: lipopolysaccharide (LPS) in the cell wall, coagulase enzyme
- Exotoxins: leukotoxin, hemolysin, lipase (Anaerobe 2006;12:165)
Diagrams / tables
Clinical features
- Lemierre syndrome: multistep disease progression
- Pharyngitis / tonsillitis: sore throat, cervical lymphadenopathy
- F. necrophorum local invasion of tissue / internal jugular vein (IJV): tender neck, high fever, rigors
- IJV thromboemboli seed other organs: cavitating pulmonary infarcts, septic arthritis, soft tissue infection / abscesses, endocarditis, meningitis
- Thrombocytopenia, sepsis / septic shock (J Clin Microbiol 2017;55:1147, Clin Microbiol Infect 2020;26:1089.e7)
Diagnosis
- Invasive infections:
- Positive blood culture
- 16S rDNA sequencing
- Culture from sterile sites (Clin Microbiol Infect 2020;26:1089.e7)
- Criteria for Lemierre syndrome:
- Tonsillitis / pharyngitis in the preceding 4 weeks
- Metastatic lesions in lungs or another site
- Internal jugular vein thrombophlebitis or isolation of F. necrophorum or Fusobacterium sp. from a normally sterile site
- Imaging: CT / MRI / US internal jugular vein thrombophlebitis
Laboratory
- Anaerobic growth in routine culture conditions, 37 °C
- Fastidious anaerobe agar (FAA) or blood agar / vitamin K / hemin / menadione
- Pale yellow, round, smooth colonies, fluoresce green-yellow under long wave UV
- Produces butyric acid from glucose: smells like overcooked cabbage or rancid butter (Anaerobe 2006;12:165)
- Beta hemolytic
- Positive: indole, lipase
- Negative: catalase, hydrogen sulfide, esculin
- MALDI TOF mass spectrometry, 16S rDNA sequencing, PCR targeting rpoB gene (Anaerobe 2016;42:89)
Case reports
- 15 year old boy with prior tonsillitis presents with neck pain (Malays Fam Physician 2018;13:37)
- 19 year old man with life threatening Lemierre syndrome following sore throat (Case Rep Crit Care 2016;2016:1264283)
- 21 year old woman presents in septic shock after feeling burst in her neck (Cureus 2021;13:e14713)
- 22 year old woman, who presents with flu-like syndrome, has fatal gynecological Lemierre syndrome (Med Mal Infect 2019;49:72)
- 37 year old woman presents with suspected COVID-19 acute respiratory syndrome (Cureus 2021;13:e15984)
- 4 cases of Lemierre syndrome (Cureus 2021;13:e18436)
Treatment
- Antibiotics: beta lactam agents (penicillins), metronidazole
- Surgery: debridement and drainage of abscesses (Cureus 2021;13:e18436)
Microscopic (histologic) description
- Slender fusiform rods with tapered ends, with or without pleomorphic filaments / coccoid (Medicine (Baltimore) 2002;81:458)
Practice question #1
A 22 year old woman presented to the emergency department with a sore throat. She now has pain with swallowing and was found to have a left tonsillar abscess. PCR for group A strep (Streptococcus pyogenes) was negative. The abscess was drained and sent for aerobic and anaerobic bacterial cultures. Culture grew Fusobacterium necrophorum. What is true about this organism?
- Associated with Lemierre syndrome
- Gram positive cocci on Gram stain
- Indole negative
- The organism is obligate aerobe
Practice answer #1
A. Associated with Lemierre syndrome. Fusobacterium necrophorum is a strict anaerobic, pleomorphic, gram negative bacillus. The organism is catalase negative and indole positive.
Comment Here
Reference: Fusobacterium necrophorum
Comment Here
Reference: Fusobacterium necrophorum
Practice question #2
The clinical microbiology laboratory has isolated a gram negative rod from the blood culture of a young patient admitted with suspected septic thrombophlebitis. The isolate forms a pale yellow colony with slight level of hemolysis on complete blood count agar and produces a blue spot when placed on filter paper and treated with indole. Which of the following is the organism?
- Bacteroides fragilis
- Fusobacterium necrophorum
- Klebsiella pneumoniae
- Streptococcus pyogenes
Practice answer #2
B. Fusobacterium necrophorum. The patient presentation is consistent with that of Lemierre syndrome. Fusobacterium necrophorum is strict anaerobic and indole positive. While Bacteroides fragilis is an anaerobic gram negative bacillus, it is indole negative. Streptococcus pyogenes is a gram positive coccus and Klebsiella pneumoniae is a facultative anaerobe.
Comment Here
Reference: Fusobacterium necrophorum
Comment Here
Reference: Fusobacterium necrophorum