Table of Contents
Definition / general | Essential features | ICD coding | Epidemiology | Sites | Pathophysiology | Etiology | Clinical features | Diagnosis | Laboratory | Radiology description | Prognostic factors | Case reports | Treatment | Gross description | Gross images | Frozen section description | Frozen section images | Microscopic (histologic) description | Microscopic (histologic) images | Positive stains | Negative stains | Sample pathology report | Differential diagnosis | Additional references | Practice question #1 | Practice answer #1 | Practice question #2 | Practice answer #2Cite this page: Hayes R, Asa SL. Parathyroid gland hyperplasia. PathologyOutlines.com website. https://www.pathologyoutlines.com/topic/parathyroidpthhyper.html. Accessed September 22nd, 2025.
Definition / general
- Absolute increase in nonneoplastic parathyroid parenchymal cells in multiple parathyroid glands
- Secondary hyperparathyroidism: compensatory proliferation of parathyroid parenchyma
Essential features
- Primary hyperparathyroidism, required to be in the absence of a physiological stimulus, is very rarely if ever associated with an increase in nonneoplastic parathyroid cells; it has now been classified as neoplastic and the previous use of hyperplasia in patients with germline predisposition (e.g., multiple endocrine neoplasia [MEN] syndromes) is now recognized as multiglandular adenomas
- Secondary hyperparathyroidism is a compensatory diffuse hyperplastic response to persistent low calcium levels, high serum phosphate or vitamin D deficiency
- Tertiary hyperparathyroidism is neoplastic proliferation arising in hyperplasia and giving rise to autonomous secretion of parathyroid hormone (PTH) in the setting of prolonged secondary hyperparathyroidism; necrosis, fibrosis or hemorrhage in a dominant nodule should prompt evaluation for malignancy
ICD coding
Epidemiology
- Primary hyperparathyroidism: see multiglandular adenomas
- Water clear cell hyperplasia: no known cause or specific genetic predisposition
- Secondary hyperparathyroidism: chronic kidney disease, vitamin D deficiency
- ~50% of the world population has vitamin D deficiency (Front Nutr 2023;10:1070808)
- Chronic kidney disease affects ~15% of the U.S. population (Kidney Int Suppl (2011) 2022;12:7)
- Tertiary hyperparathyroidism: neoplasm arising in a background of secondary hyperplasia
Sites
- Parathyroid glands, usually perithyroidal but also in the mediastinum
Pathophysiology
- Secondary: renal insufficiency leading to hypocalcemia, hyperphosphatemia and low 1,25 dihydroxyvitamin D3 with compensatory increase in parathyroid hormone and chief cell proliferation
- Tertiary: loss of parathyroid hormone receptors and mutation accumulation in parathyroids with secondary hyperplasia
Etiology
- Secondary: renal failure, hypocalcemia, low 1,25 dihydroxyvitamin D3 (Clin J Am Soc Nephrol 2011;6:913)
- Tertiary: prolonged untreated secondary hyperparathyroidism (Clin Ter 2021;172:241)
Clinical features
- Bone remodeling, deformities, fractures (J Am Soc Nephrol 2004;15:2208)
- Extraosseous calcification, kidney stones (Urol Clin North Am 2000;27:275)
- Psychologic and neurologic manifestations (Front Surg 2022;9:885188)
Diagnosis
- PTH, calcium, phosphorus, vitamin D levels, renal function (Clin J Am Soc Nephrol 2011;6:913)
Laboratory
- Increased PTH (Clin J Am Soc Nephrol 2011;6:913)
- Decreased vitamin D
- Decreased calcium
- Biochemical features of renal failure
Radiology description
- Parathyroid enlargement (not usually visible on imaging)
- Sestamibi scan unusually nonlocalizing (Sci Rep 2019;9:14634)
- Brown tumors of bone (rare) (Am J Otolaryngol 1996;17:407)
Prognostic factors
- Increased chance of recurrence if multiple foci are present, increased mitotic index, nodularity or persistent renal disease (Cancer 2007;110:255)
Case reports
- 49 year old man with surgically managed secondary parathyroid hyperplasia (Medicine (Baltimore) 2022;101:e31362)
- 50 year old woman with chronic malabsorption, renal disease and tertiary hyperparathyroidism (Cureus 2024;16:e70179)
- 58 year old woman with tertiary hyperparathyroidism after longstanding end stage renal disease with renal transplantation (CEN Case Rep 2021;10:208)
- 61 year old man with secondary hyperparathyroidism due to stage 4 chronic kidney disease in a background of autosomal dominant polycystic kidney disease and hypertension (Clin J Am Soc Nephrol 2020;15:1041)
Treatment
- Surgical excision
- Renal transplant (secondary hyperparathyroidism due to chronic kidney disease) (Ann Surg 2008;248:18)
- Recurrence - parathyromatosis; can make treatment more difficult, especially with the following features (Cancer 2007;110:255)
- Markedly nodular
- Highly proliferative
- Persistence of chronic renal failure
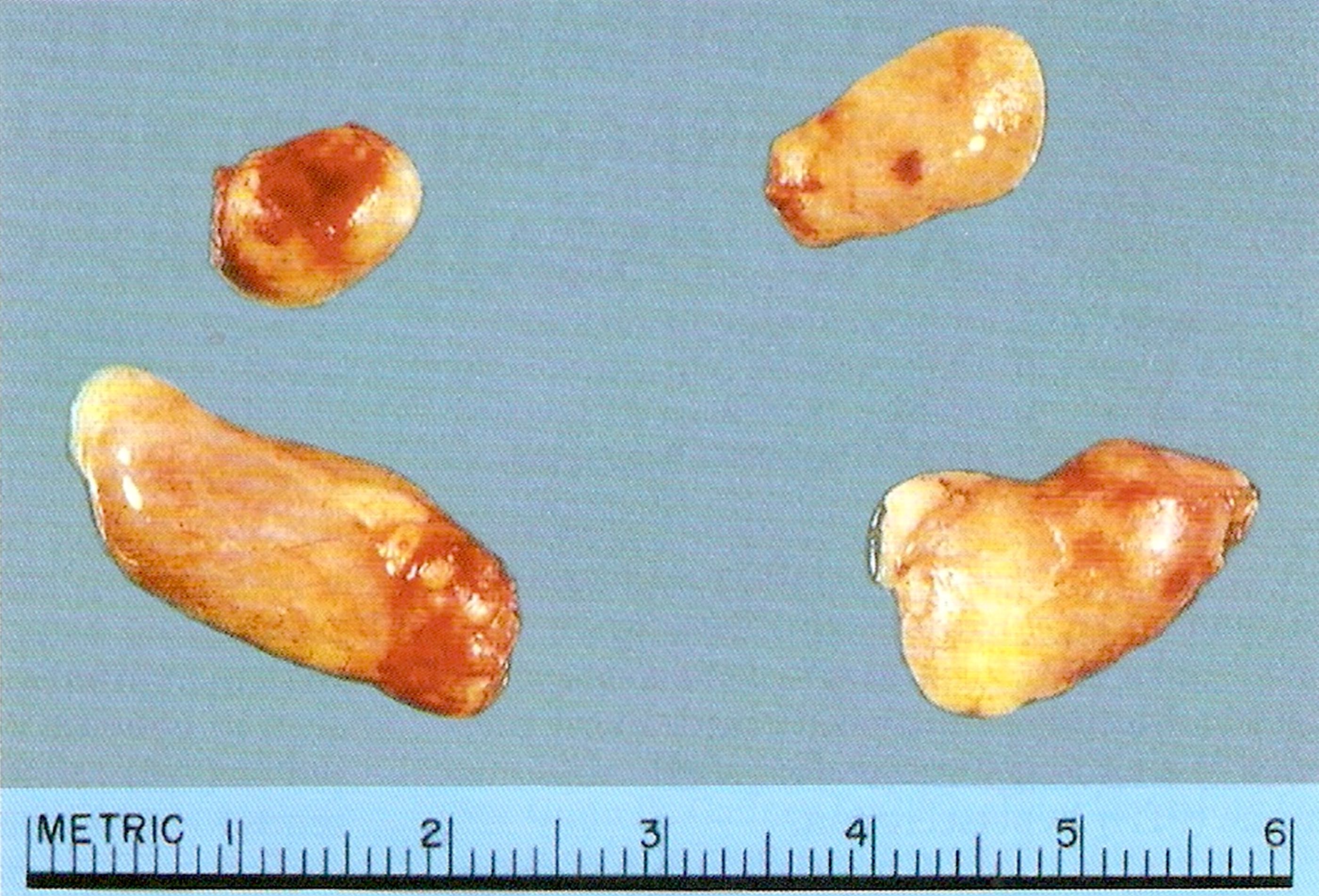
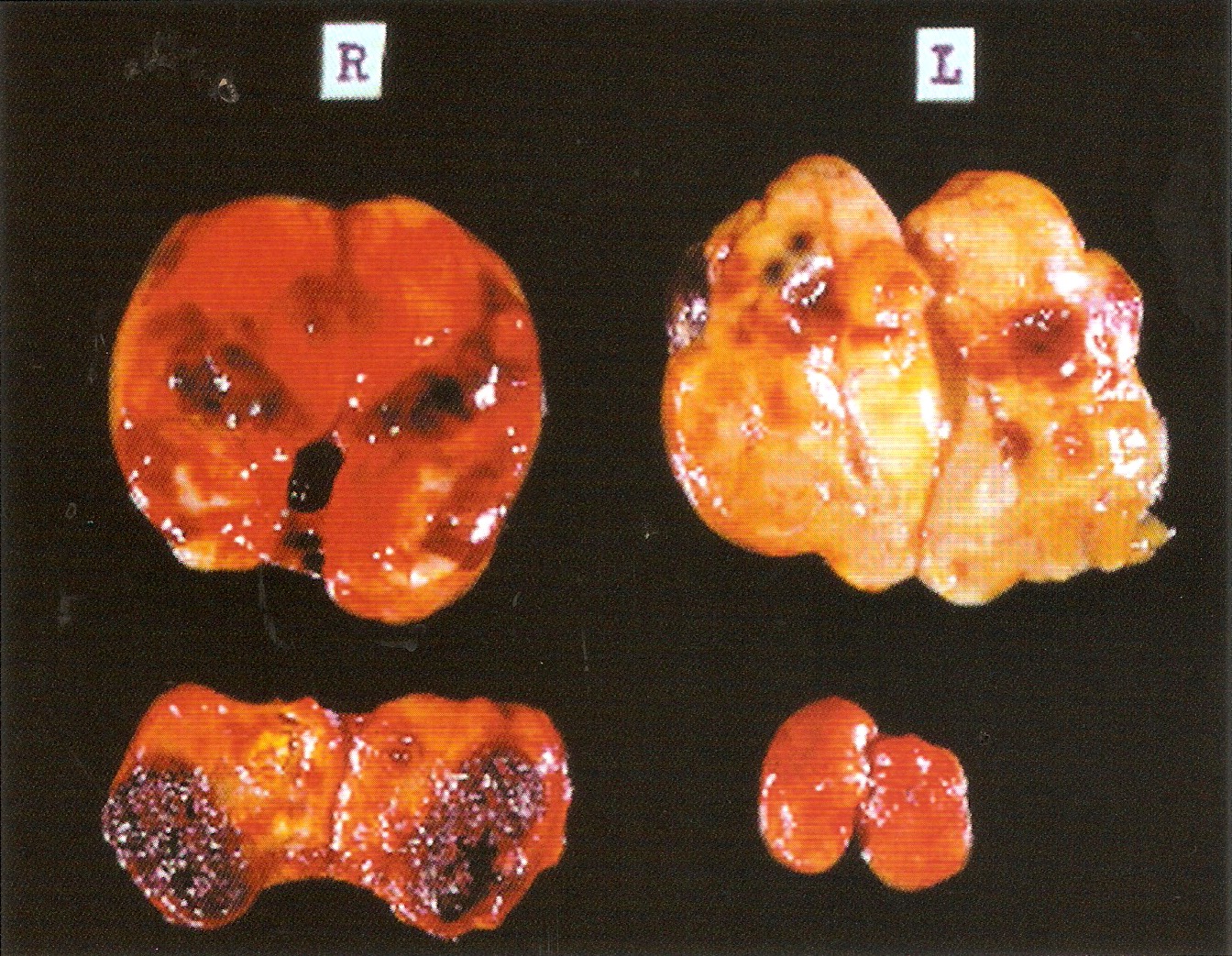
Gross description
- Secondary: diffuse enlargement > 1.2 g (Mod Pathol 2011;24:S78)
- Tertiary: dominant nodule present in an enlarged parathyroid
- Primary water clear cell hyperplasia > 1 g
- Upper glands heavier than lower glands
Gross images
Frozen section description
- Frozen section is not usually performed on the enlarged hyperplastic parathyroids
- If used, it is typically performed on a biopsy that is used only to confirm that the tissue is parathyroid, rather than lymph node or other mimics
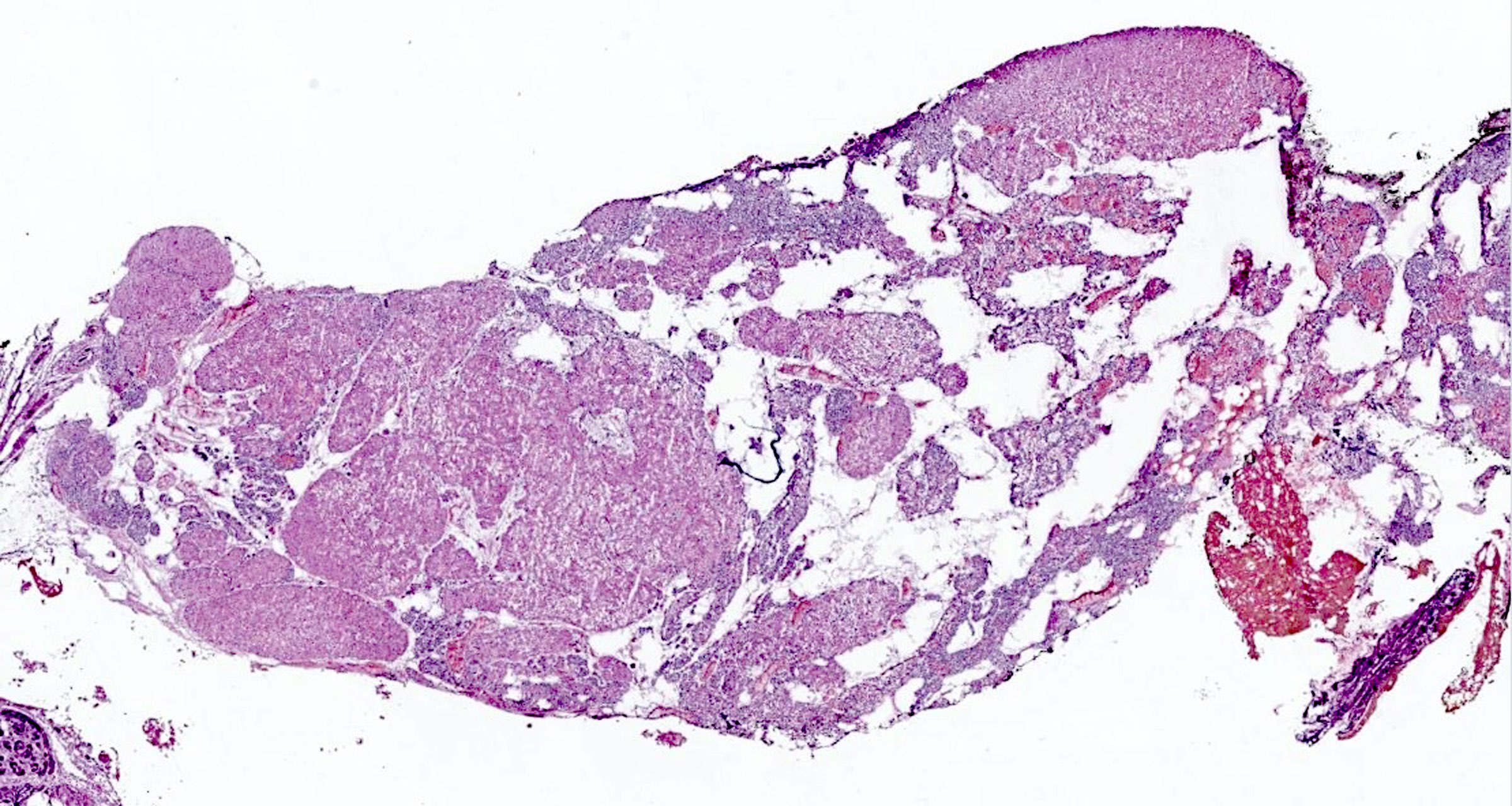
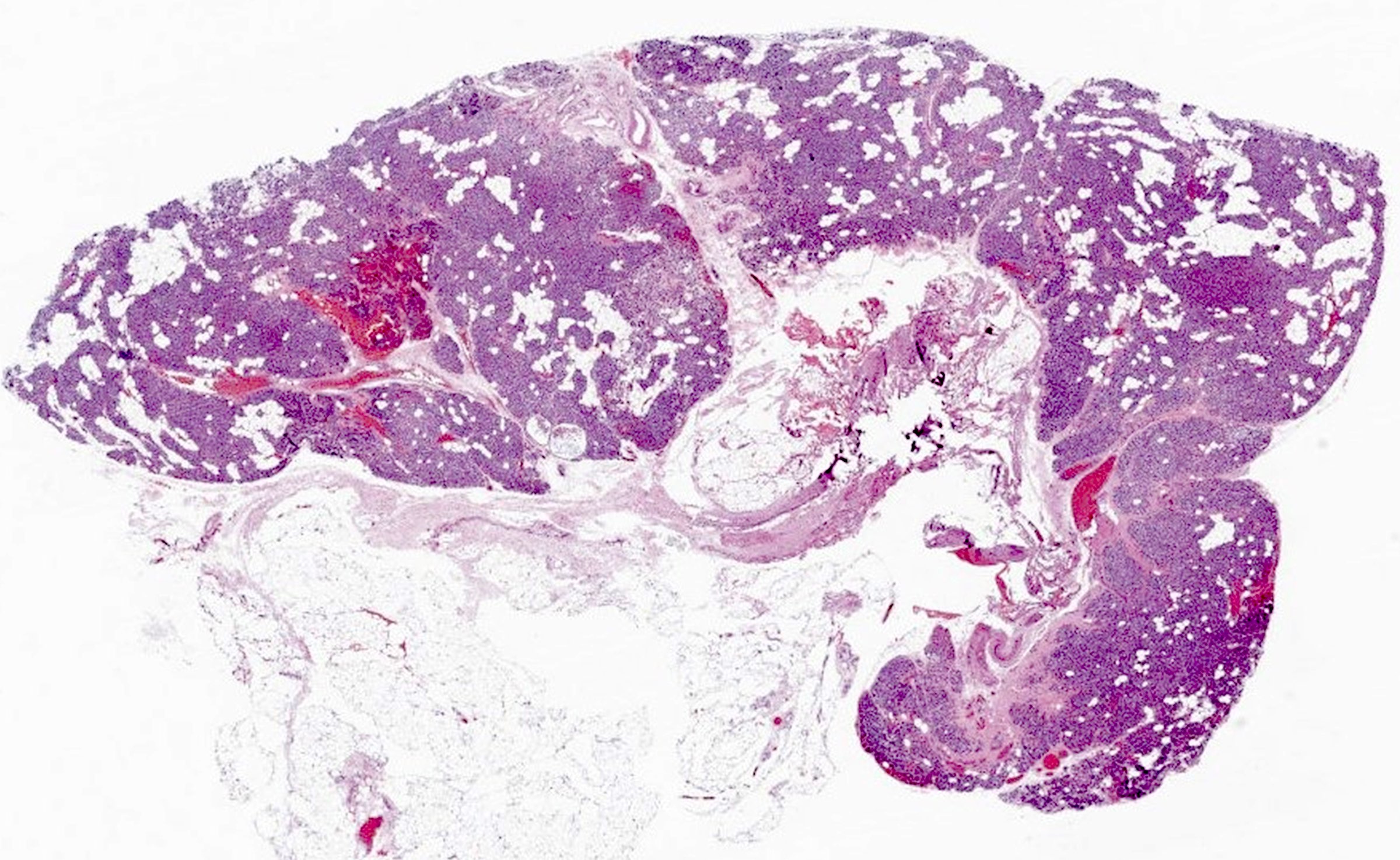
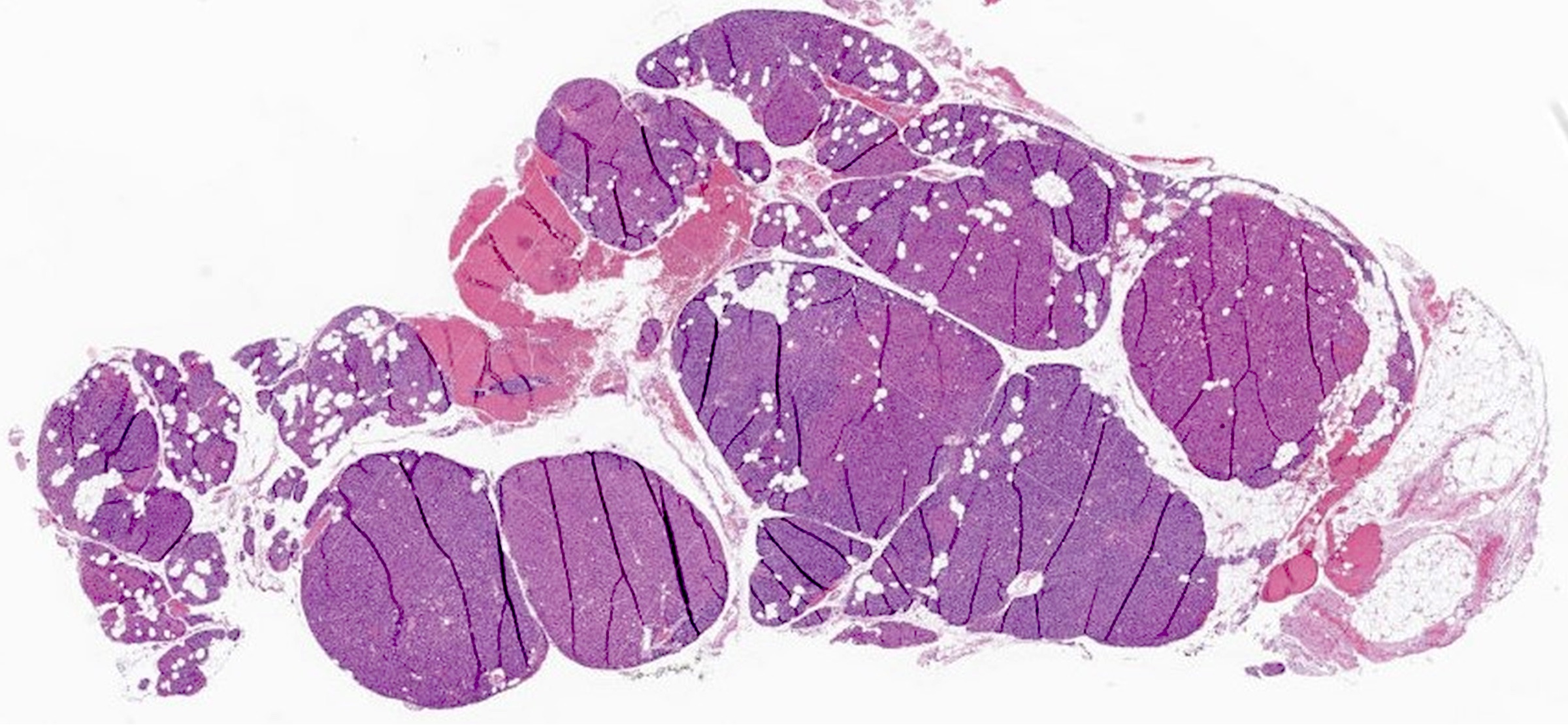
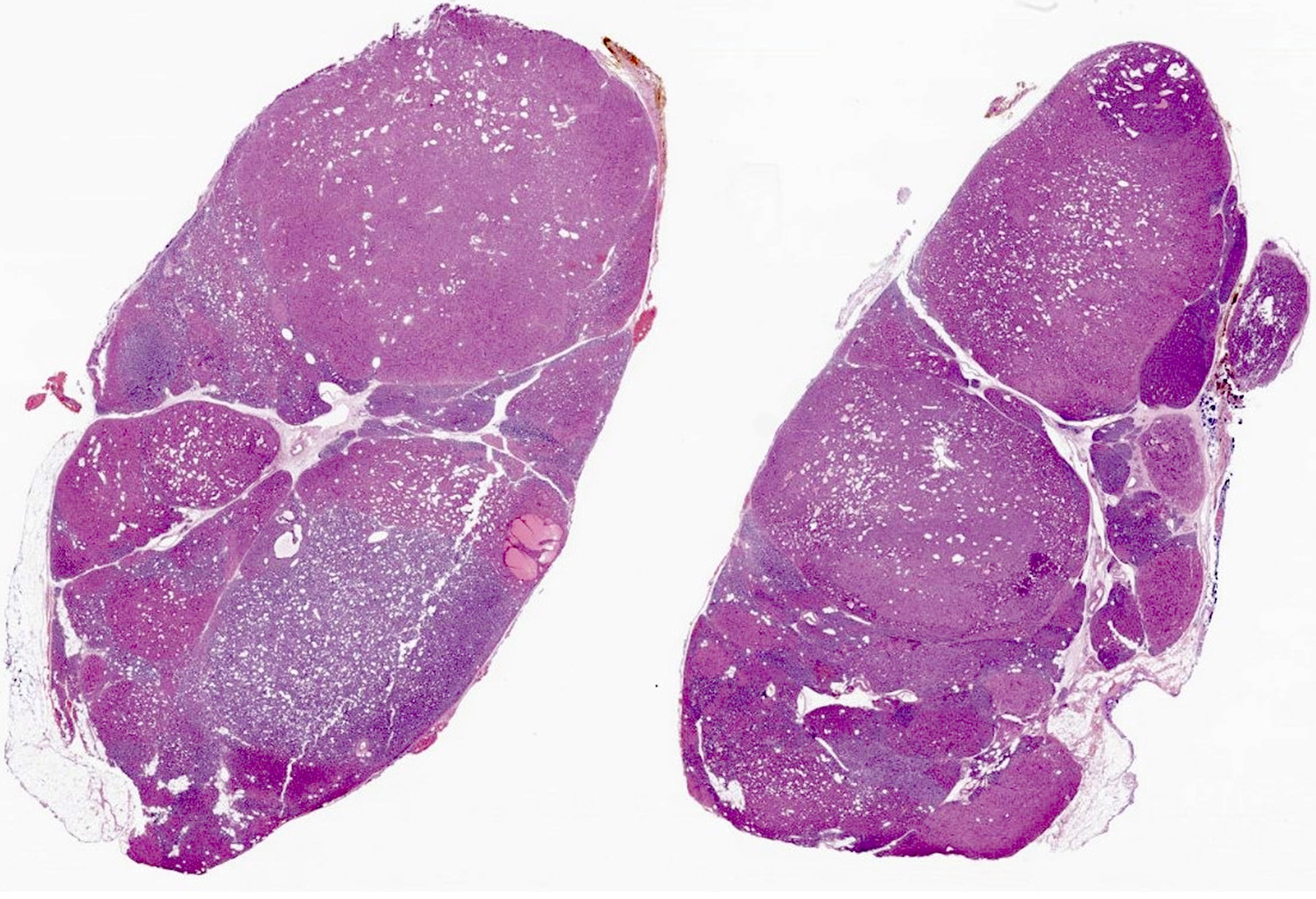
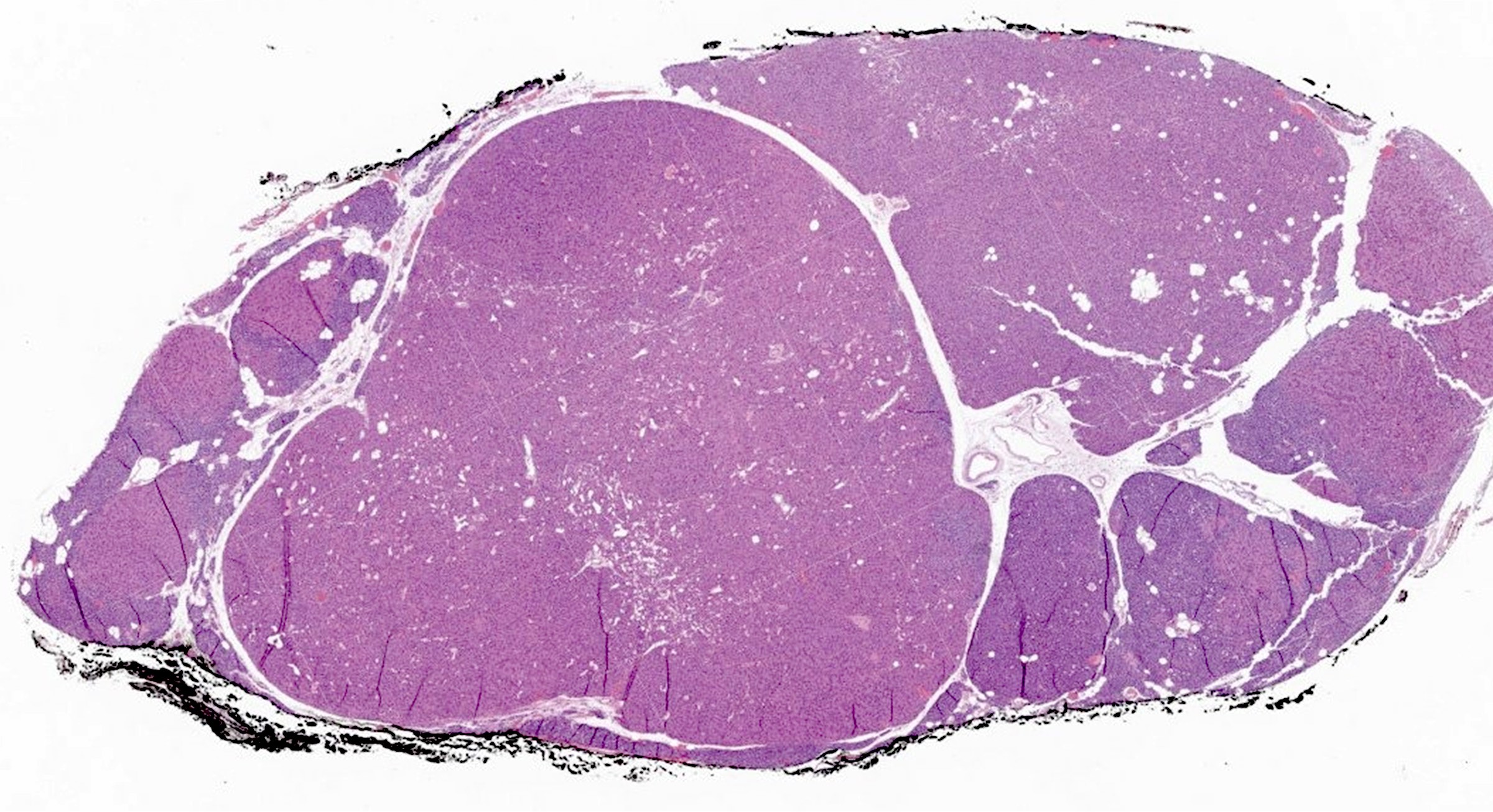
Microscopic (histologic) description
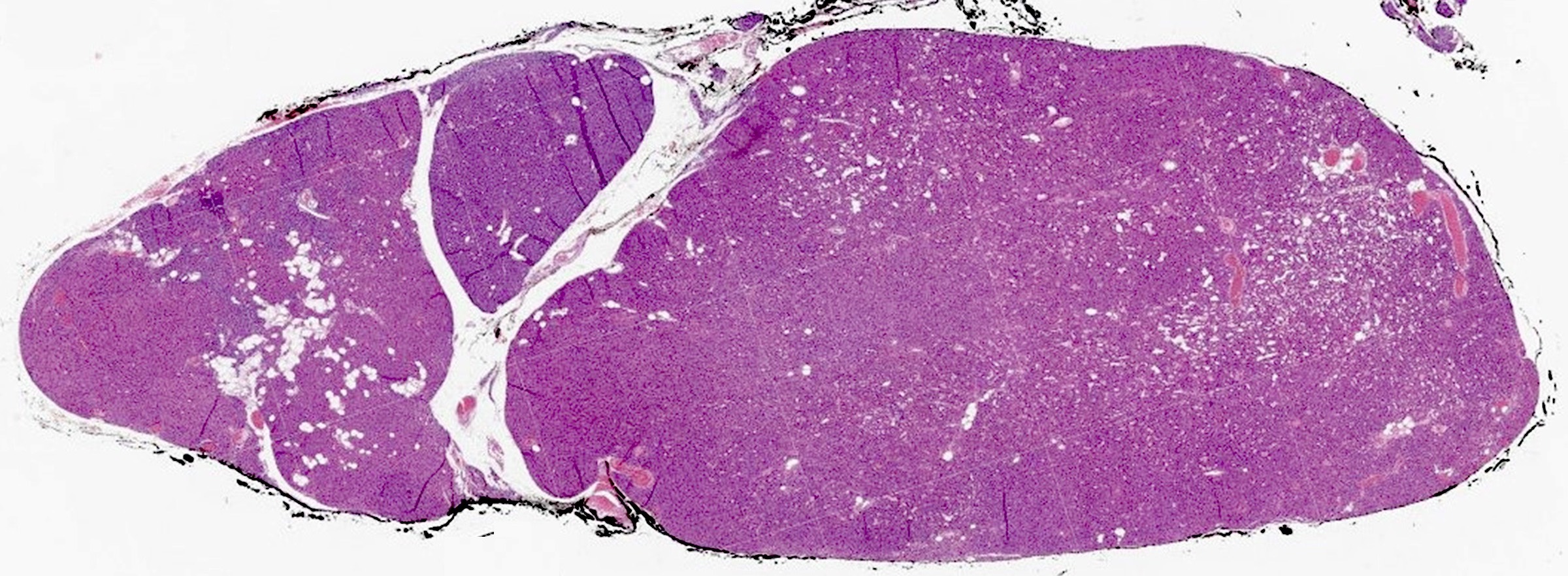
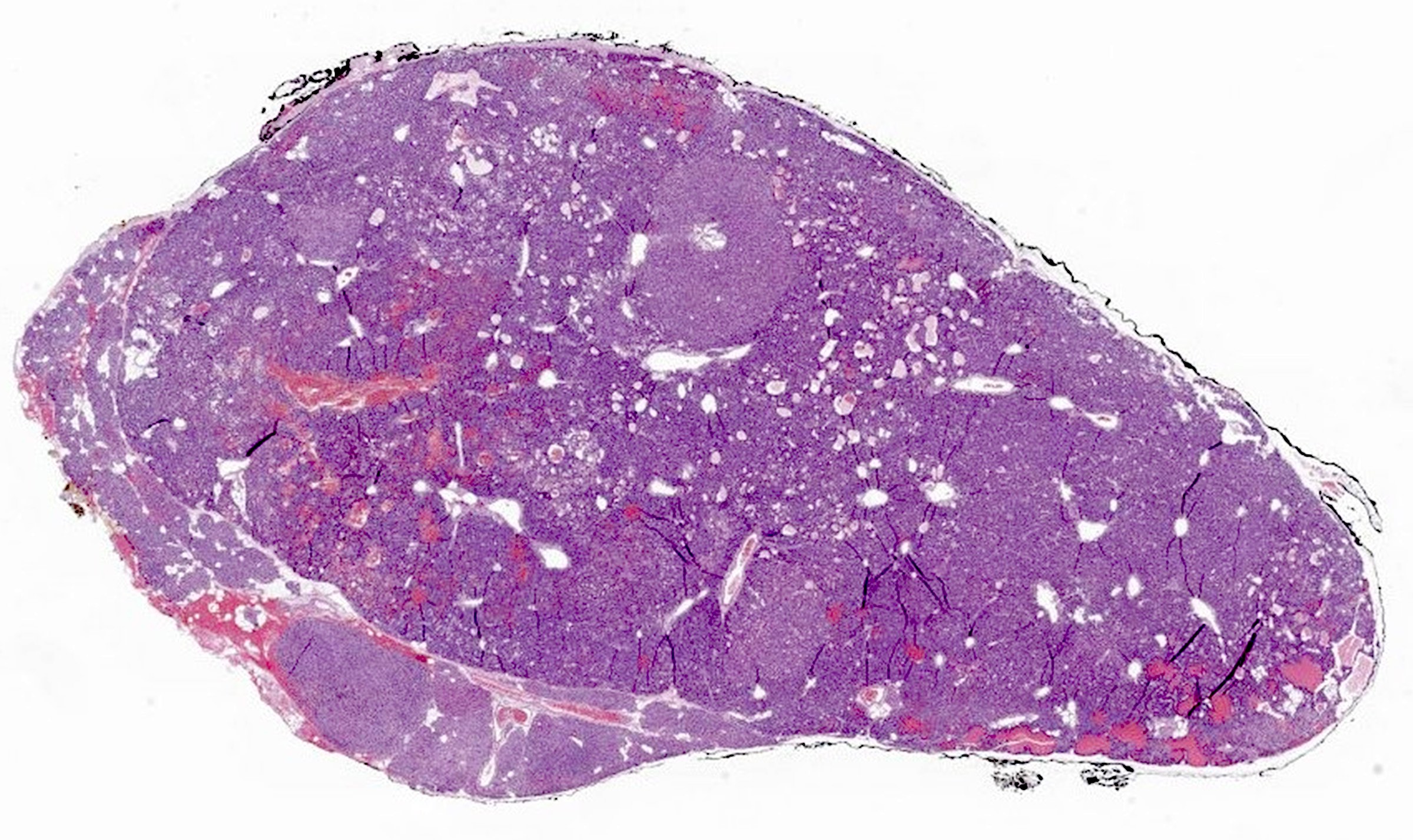
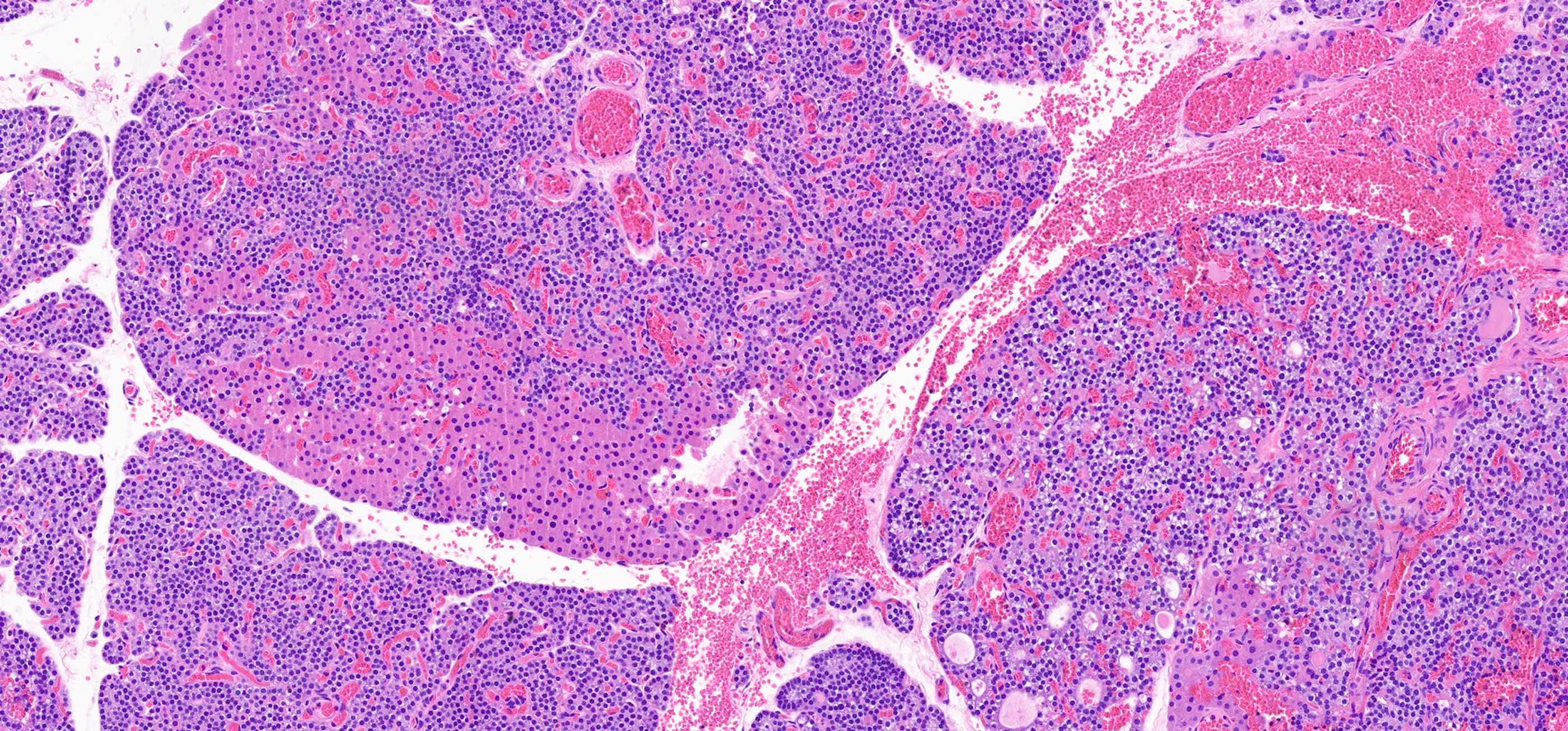
- Secondary: increased parenchymal cells with decreased stroma (Chirurgia (Bucur) 2019;114:594)
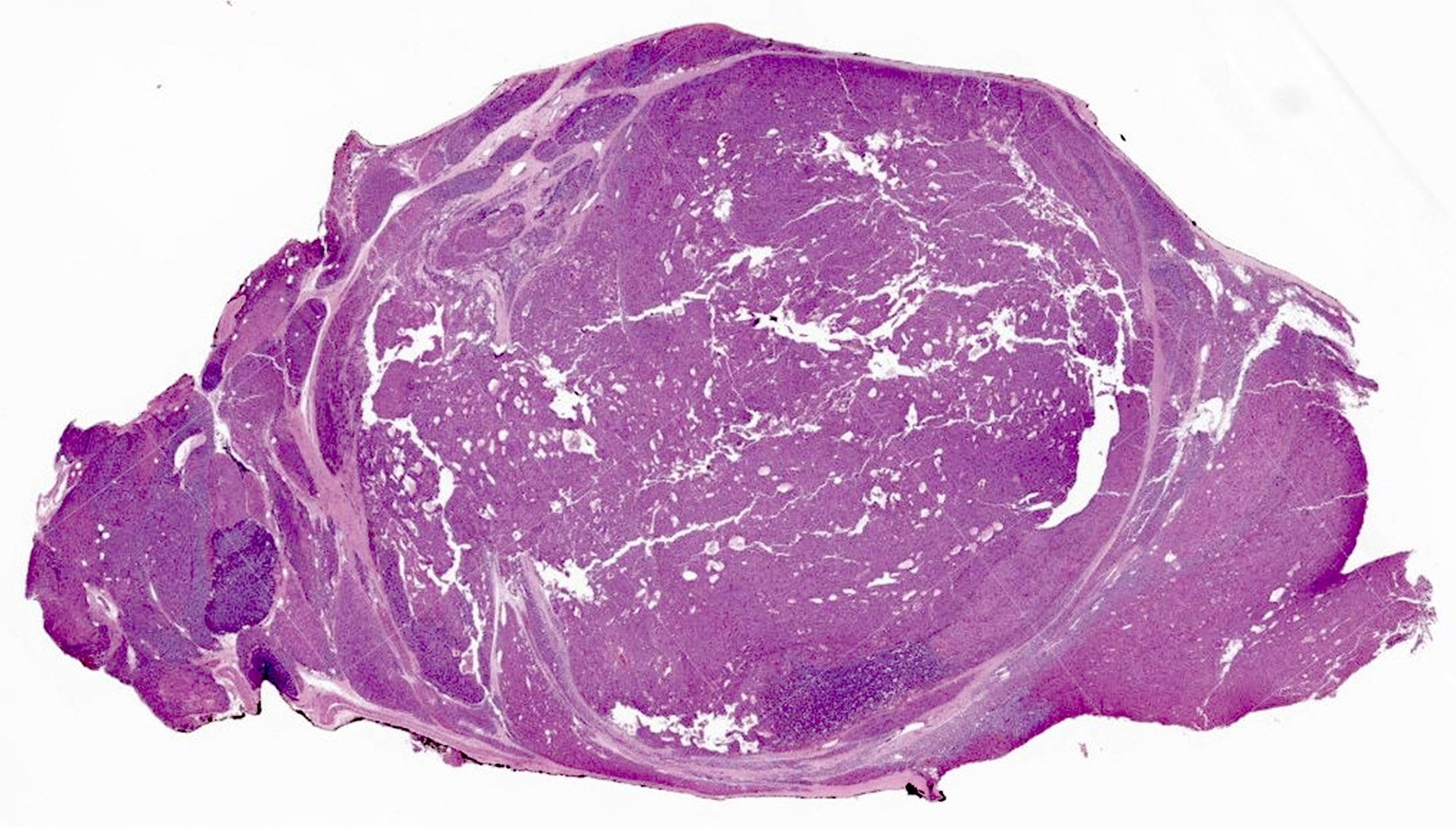
- Increased fibrosis and nodularity with later development
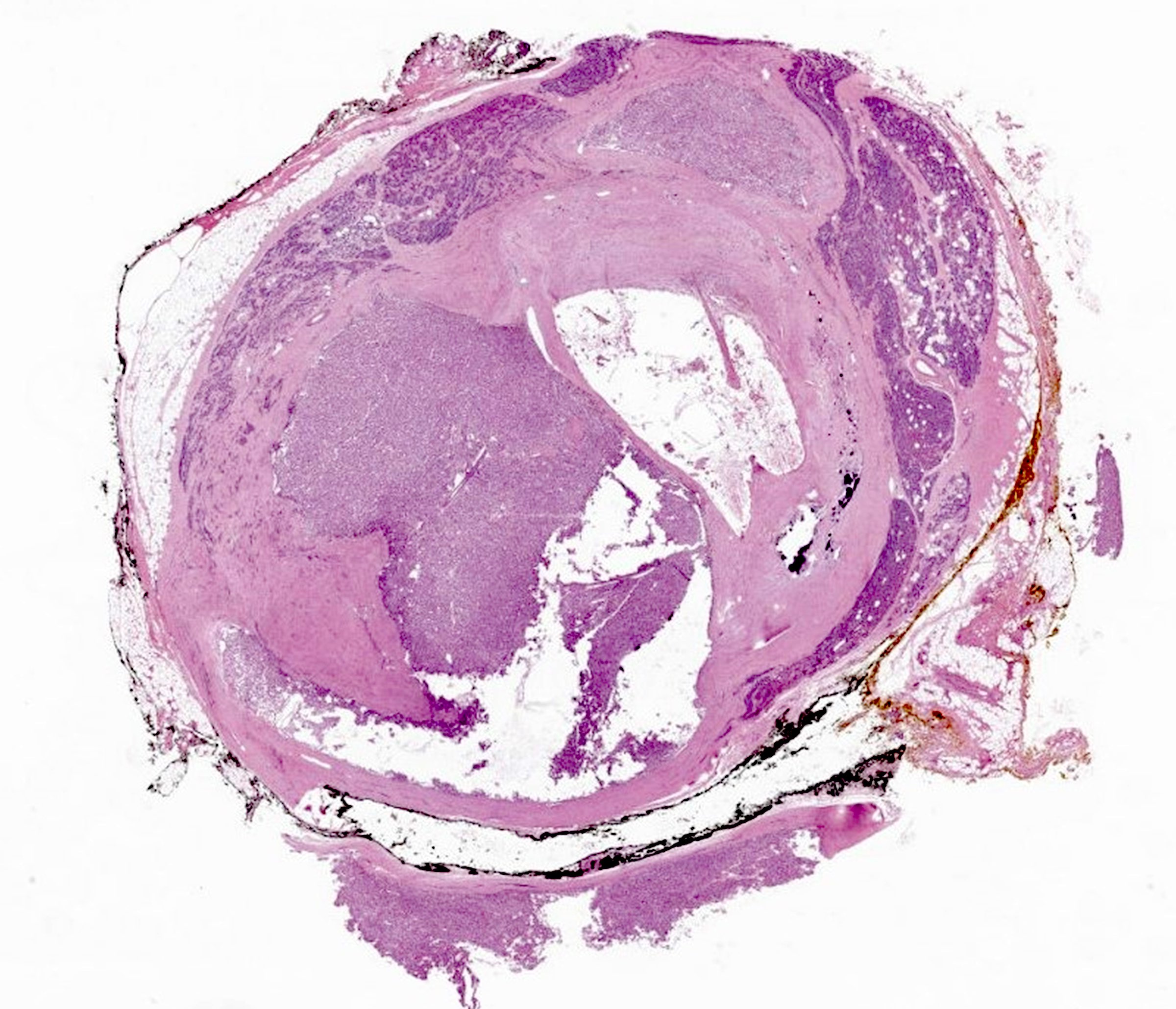
- May have mitotic figures, necrosis and hemorrhage with later development
- May indicate carcinoma if nodular
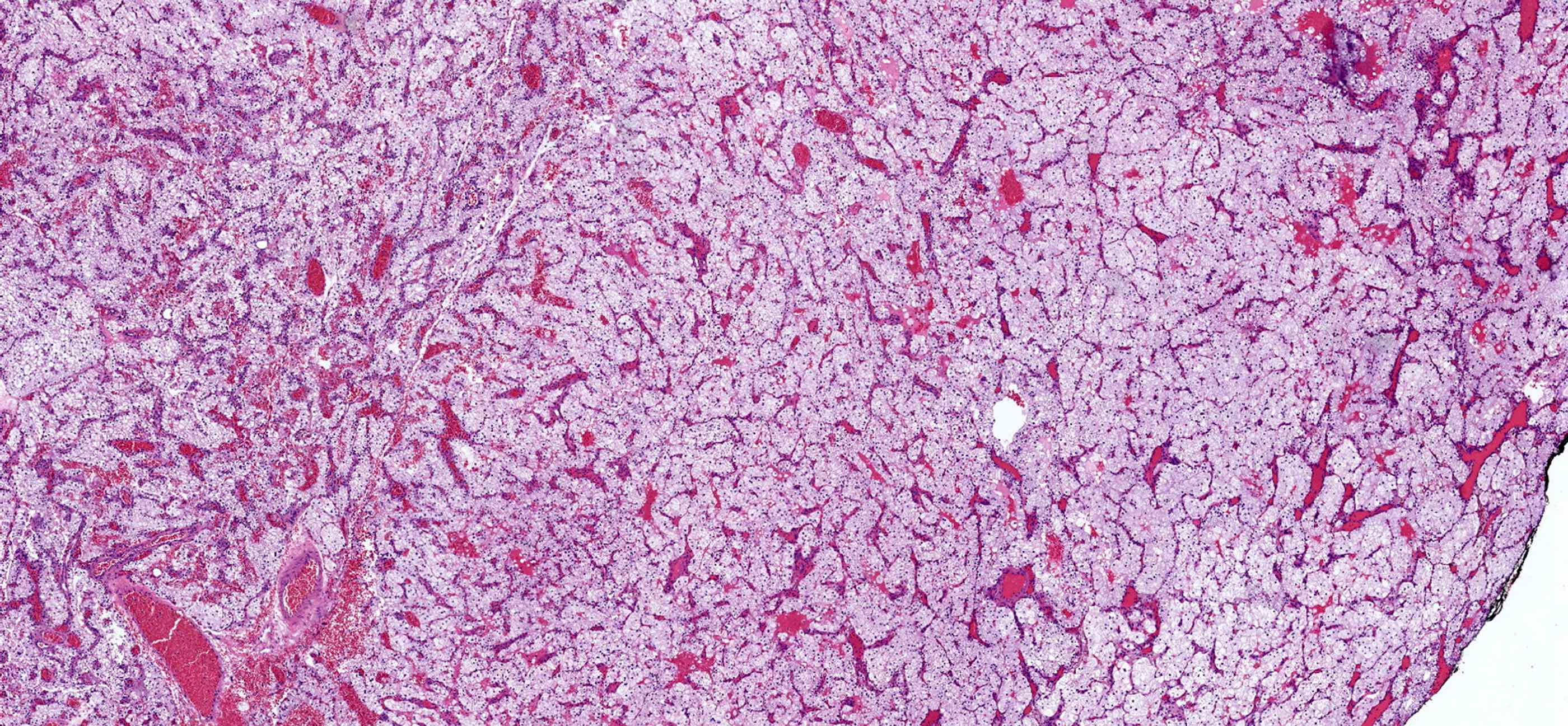
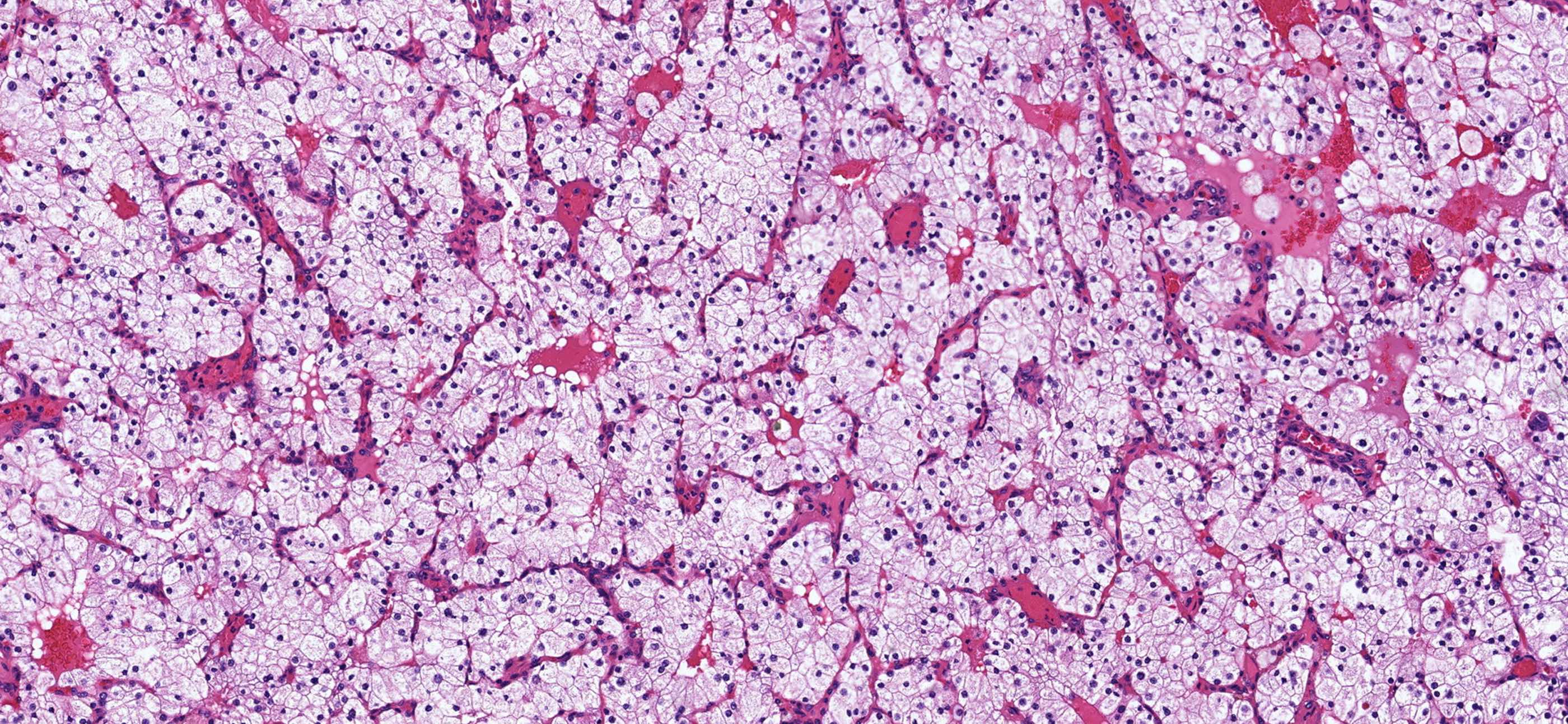
- Water clear cell hyperplasia: clear cytoplasm, distinct cell borders, diffuse (Pathology 2021;53:852)
Microscopic (histologic) images
Contributed by Sylvia L. Asa, M.D., Ph.D.
Positive stains
- Parathyroid hormone, synaptophysin, chromogranin A, GATA3, CAM 5.2, CK7, CK8, CK18 and CK19 (Endocr Pathol 2018;29:113)
- GATA3 (Diagn Cytopathol 2021;49:70)
- Polyclonal PAX8 is nonspecific because monoclonal PAX8 is negative in parathyroid (Endocr Pathol 2018;29:91)
- CDC73 (parafibromin)
Negative stains
Sample pathology report
- Parathyroid, left superior, parathyroidectomy:
- Diffuse and nodular hyperplasia
Differential diagnosis
- Parathyroid adenoma:
- Nodules with surrounding unremarkable parathyroid tissue
- Individual glands involved
- PTH and calcium both elevated
- Parathyroid lipoadenoma:
- Enlarged parathyroid, > 1 g
- Grossly, yellow surface
- > 50% adipose component of the nodule
- Parathyroid carcinoma:
- Significantly elevated PTH and calcium
- Poorly circumscribed or invasive nodule
- Vascular or perineural invasion
- Metastasis
- Follicular thyroid adenoma:
- Well encapsulated nodule
- Abundant to scant colloid present
- Micro or macrofollicular architecture
- Cuboidal to columnar epithelium
- Clear to eosinophilic cytoplasm
- Uniform round nuclei with coarse chromatin
- No capsular or vascular invasion
- Often solitary but may arise in the setting of follicular nodular disease
- Atypical parathyroid tumor:
- Cytological atypia, calcifications, fibrosis or increased mitotic rate
- Negative for full thickness capsular invasion, angioinvasion or perineural invasion
- Positive for PTH, GATA3 and chromogranin A
- Elevated PTH and calcium levels between those of a parathyroid adenoma and carcinoma
- Often associated with prior neck manipulation
Additional references
Practice question #1
A 70 year old man with end stage renal disease undergoes surgical resection of an enlarged parathyroid gland. On examination, which of the following features is most concerning?
- Fibrosis within multiple small nodules
- Hemorrhage within a dominant nodule
- Markedly decreased stroma
- Weight over 1.2 g
Practice answer #1
B. Hemorrhage within a dominant nodule. The presence of hemorrhage within a dominant nodule warrants further evaluation for possible neoplastic changes. Answer D is incorrect because 1.2 g is the lower limit of weight for secondary parathyroid hyperplasia. Answer A is incorrect because fibrosis and multinodular development are routine findings in longstanding secondary parathyroid hyperplasia. Answer C is incorrect because decreased stroma is a feature of secondary parathyroid hyperplasia.
Comment Here
Reference: Parathyroid gland hyperplasia
Comment Here
Reference: Parathyroid gland hyperplasia
Practice question #2
A 63 year old woman has surgical resection of an enlarged parathyroid gland. The specimen has the above histology. What lab values would be expected in this patient prior to excision?
- Decreased Ca2+, decreased PTH, decreased vitamin D
- Decreased Ca2+, increased PTH, decreased vitamin D
- Decreased Ca2+, increased PTH, increased vitamin D
- Increased Ca2+, decreased PTH, decreased vitamin D
- Increased Ca2+, increased PTH, increased vitamin D
Practice answer #2
B. Decreased Ca2+, increased PTH, decreased vitamin D. The finding of secondary parathyroid hyperplasia is a physiologic response to chronically decreased calcium levels, most often due to inadequate vitamin D production causing increased PTH levels. Answers D and E are incorrect because decreased calcium levels are a primary driver of increased PTH production. Answer A is incorrect because PTH levels should be elevated in the setting of parathyroid hyperplasia. Answer C is incorrect because increased vitamin D is a suppressor of parathyroid hyperplasia.
Comment Here
Reference: Parathyroid gland hyperplasia
Comment Here
Reference: Parathyroid gland hyperplasia