Table of Contents
Definition / general | Essential features | Terminology | ICD coding | Epidemiology | Sites | Pathophysiology | Etiology | Diagrams / tables | Clinical features | Diagnosis | Laboratory | Radiology description | Radiology images | Prognostic factors | Case reports | Treatment | Gross description | Gross images | Frozen section description | Microscopic (histologic) description | Microscopic (histologic) images | Videos | Sample pathology report | Differential diagnosis | Practice question #1 | Practice answer #1Cite this page: Pitale S, Esnakula AK. Choledochal cyst. PathologyOutlines.com website. https://www.pathologyoutlines.com/topic/gallbladdercholedochalcyst.html. Accessed August 29th, 2025.
Definition / general
- Choledochal cyst is an anomaly, either congenital or acquired, that affects segments of either the extrahepatic or intrahepatic bile ducts or both (StatPearls: Choledochal Cyst [Accessed 24 March 2025], HPB (Oxford) 2023;25:14)
- Classified based on the anatomic extent of involvement of the biliary tree and the classification by Todani et al. (1977) is commonly used to guide management
- Increased risk of malignant transformation, with the highest risk associated with type I and IV cysts
Essential features
- Anomaly of the biliary tree of unknown etiology and a risk of malignancy (type I and IV cysts) (J Am Coll Surg 2014;219:1167)
- Endoscopic retrograde cholangiopancreatography (ERCP) and magnetic resonance cholangiopancreatography (MRCP) have the highest diagnostic accuracy rate (Mymensingh Med J 2007;16:113)
- Early detection and timely surgical intervention have demonstrated outstanding outcomes with reduction of risk for malignancy; excision is associated with an 89% rate of being event free and a 5 year survival rate exceeding 90% (StatPearls: Choledochal Cyst [Accessed 24 March 2025])
Terminology
- Choledochal cysts were first described in 1723 by Vater and Ezler (J Am Coll Surg 2014;219:1167)
- Biliary cysts (as it includes intrahepatic cysts as well) (StatPearls: Choledochal Cyst [Accessed 24 March 2025])
- Certain subtypes of choledochal cysts are referred to by various terminologies: choledochocele, common bile duct diverticulum and Caroli disease
Epidemiology
- Predominantly occurs in female infants and young children
- More common in populations of East Asian descent (J Am Coll Surg 2014;219:1167)
- Disease is rare in Western populations but has an incidence of 1 in 13,500 live births in the U.S.
- Type I and IV are more prevalent in female patients; F:M = ~4:1 or 3:1
- Reasons behind the higher incidence in Asian populations and the female predominance are not yet understood (StatPearls: Choledochal Cyst [Accessed 24 March 2025])
- Most choledochal cysts are diagnosed in childhood and only ~25% are identified in adults but adults constitute the majority of patients in recent studies (Curr Opin Gastroenterol 2016;32:225)
Sites
- Extrahepatic and intrahepatic bile ducts of the biliary tree
Pathophysiology
- Exact causes and development is unknown, leading to several hypotheses (StatPearls: Choledochal Cyst [Accessed 24 March 2025], HPB (Oxford) 2023;25:14)
- Babbitt's theory
- Suggests that choledochal cysts arise from an anomalous pancreaticobiliary junction (APBJ)
- APBJ occurs when the biliary and pancreatic ducts join 1 - 2 cm proximal to the sphincter of Oddi, resulting in a long channel not covered by the sphincter
- This leads to backflow and mixing of pancreatic and biliary secretions, activating pancreatic enzymes, increasing pressure and causing dilation, inflammation, epithelial damage, dysplasia and malignancy in the biliary tree
- Supported by high amylase levels and studies showing elevated phospholipase A2 and trypsinogen in bile from choledochal cysts
- Animal studies also support this theory, showing ductal dilation and cyst formation after creating APBJ
- Challenged by findings that APBJ is present in only 50 - 80% of cases and that some antenatally diagnosed choledochal cysts do not show reflux; also questioned due to the limited capacity of neonatal pancreatic acini to produce sufficient enzymes
- Congenital theories
- Kusunoki et al. propose that choledochal cysts may result from a deficiency of ganglionic cells in the distal common bile duct (CBD), causing dilation of the proximal common bile duct, like achalasia and Hirschsprung disease (Arch Surg 1988;123:984)
- Type specific theories
- Type II (true common bile duct diverticulum): suggested to be due to biliary duplication cysts
- Type III (choledochocele): suggested to be related to biliary or duodenal duplication cysts, with possible blockage at the ampulla of Vater
- Caroli disease (type V)
- Believed to result from a disruption in the remodeling of ductal plates
- Associated with biliary atresia and may share similar ductal plate malformation pathogenesis
- Also linked to autosomal recessive polycystic kidney disease (PKD) and less frequently to autosomal dominant polycystic kidney disease
- Babbitt's theory
Etiology
- Congenital or acquired
- Exact cause is unknown; several hypotheses have been proposed, as discussed in Pathophysiology
Clinical features
- Classic triad of symptoms for choledochal cysts: abdominal pain, palpable abdominal mass and jaundice
- Abdominal pain is the most common presenting feature in adults
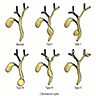
- Todani et al. (1977) classification: based on the anatomic extent of biliary tree involvement (StatPearls: Choledochal Cyst [Accessed 24 March 2025], HPB (Oxford) 2023;25:14)
- Type I cysts: fusiform (most common: 50 - 80%)
- Characterized by cystic dilation of the common bile ducts
- Rarely, dilatation could extend into the intrahepatic ducts (J Hepatobiliary Pancreat Surg 2003;10:340)
- Subdivided into 3 subgroups
- Type IA: cystic dilation of the entire extrahepatic biliary tree with APBJ
- Type IB: segmental dilation of the extrahepatic biliary tree without APBJ
- Type IC: diffuse fusiform dilation of the entire extrahepatic biliary tree with APBJ
- Type II cysts (rare: 2%)
- Characterized by a true diverticular dilation along the extrahepatic duct
- Type III cysts (choledochocele: 1.4 - 4.5%)
- Intraduodenal cystic dilation of the distal common bile duct
- Difficult to identify on ultrasound
- Type IV cysts (15 - 35%)
- Type IVA: multiple dilations affecting both intrahepatic and extrahepatic biliary trees
- Type IVB: multiple dilations confined to the extrahepatic biliary tree
- Type V (Caroli disease, 20%)
- Characterized by multifocal segmental dilations confined to the intrahepatic biliary tree
- Type VI
- Choledochal cyst arising from the cystic duct (Int J Surg Case Rep 2020;68:111)
- Type I cysts: fusiform (most common: 50 - 80%)
Diagnosis
- Imaging studies are crucial for diagnosis and subtyping
- Ultrasound is an initial choice of investigation
- Diagnosis can be confirmed by MRCP or ERCP
- Reference: StatPearls: Choledochal Cyst [Accessed 24 March 2025]
Laboratory
- No specific laboratory tests are required to diagnose choledochal cyst
- Elevated levels of liver enzymes and alkaline phosphatase may be seen in cholangitis
- Serum amylase and lipase levels are elevated in cases of pancreatitis
- Indirect and direct hyperbilirubinemia is present with obstructive jaundice
- Reference: StatPearls: Choledochal Cyst [Accessed 24 March 2025]
Radiology description
- Imaging studies are crucial for diagnosis and subtyping
- Ultrasonography (StatPearls: Choledochal Cyst [Accessed 24 March 2025], HPB (Oxford) 2023;25:14)
- Prenatal: detects cystic structures at the porta hepatis
- Postnatal: preferred initial imaging with 71 - 97% sensitivity; provides information on cyst location, hepatic echotexture and portal structures
- Computed tomography (CT) cholangiography
- Useful for assessing the extent of dilation and planning surgical approaches
- Technetium 99 hepatobiliary iminodiacetic acid (HIDA) scan
- Differentiates choledochal cysts from biliary atresia in neonates
- Useful for detecting spontaneous cyst rupture with dye leakage into the peritoneal cavity
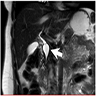
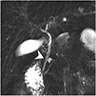
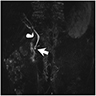
- Magnetic resonance cholangiopancreatography (MRCP)
- Considered a gold standard for diagnosis (90 - 100% sensitivity)
- Noninvasive, no ionizing radiation and does not cause complications like ERCP
- Endoscopic retrograde cholangiopancreatography (ERCP)
- Highest diagnostic accuracy for choledochal cysts
- Limited use due to invasiveness, risk of complications and ionizing radiation
- Offers both diagnostic and therapeutic benefits, especially for type III choledochoceles, where endoscopic sphincterotomy can be performed
Radiology images
Prognostic factors
- Malignancy (StatPearls: Choledochal Cyst [Accessed 24 March 2025], HPB (Oxford) 2023;25:14)
- ~11% of choledochal cyst cases develop cancer
- Malignancy is more common in type I and IV choledochal cysts
- 5 year survival rate for those with malignancy is ~5%
- Risk of malignancy is 4 times higher in cases treated with only surgical drainage compared to those with complete cyst excision
- Risk of biliary malignancy remains postresection; hence, long term follow up is recommended
- Bile stasis and stone formation can lead to
- Ascending cholangitis and liver abscess
- Acute pancreatitis (commonly presents in adults)
- Portal hypertension may arise in association with choledochal cysts due to
- Secondary biliary cirrhosis or fibrosis
- Portal vein thrombosis
- Caroli disease with congenital hepatic fibrosis (Indian J Surg 2012;74:29)
Case reports
- 4 month old girl with a giant choledochal cyst (Afr J Paediatr Surg 2023;20:243)
- 15 month old boy with type I choledochal cyst induced pancreatitis (Pediatr Emerg Care 2000;16:265)
- 3 year old girl with an abdominal mass (Narra J 2023;3:e201)
- 10 year old boy who presented with a choledochal cyst originating from primary sclerosing cholangitis (Int Surg 2011;96:316)
- 35 year old woman with an enlarged, palpable mass in the right upper abdomen (Int J Surg Case Rep 2020;68:111)
- 38 year old woman with severe abdominal pain for 1 month (Int J Surg Case Rep 2020;70:33)
Treatment
- General management (StatPearls: Choledochal Cyst [Accessed 24 March 2025], HPB (Oxford) 2023;25:14)
- Cysts should be resected and bile flow restored
- Early surgical excision is advised to reduce risks of malignancy, biliary stones and other associated complications
- Type I and type IV cysts
- Managed with complete excision of the choledochal cyst and bile flow restoration
- Preferred methods: Roux-en-Y hepaticojejunostomy or hepaticoduodenostomy
- Type II cysts
- Managed with simple excision or diverticulectomy and occlusion of the diverticular neck
- Type III cysts (choledochocele)
- Treated with sphincterotomy for symptomatic cases
- For asymptomatic cases, sphincterotomy or cyst marsupialization (via ERCP or transduodenal approach) with biopsy to check for dysplasia and epithelium type
- Caroli disease (type V cysts)
- Localized / unilobular disease: segmental hepatic resection
- Diffuse / bilobular and symptomatic disease: orthotopic liver transplant
- APBJ
- If no cyst is present but an APBJ is detected, cholecystectomy is recommended due to high risk of gallbladder cancer
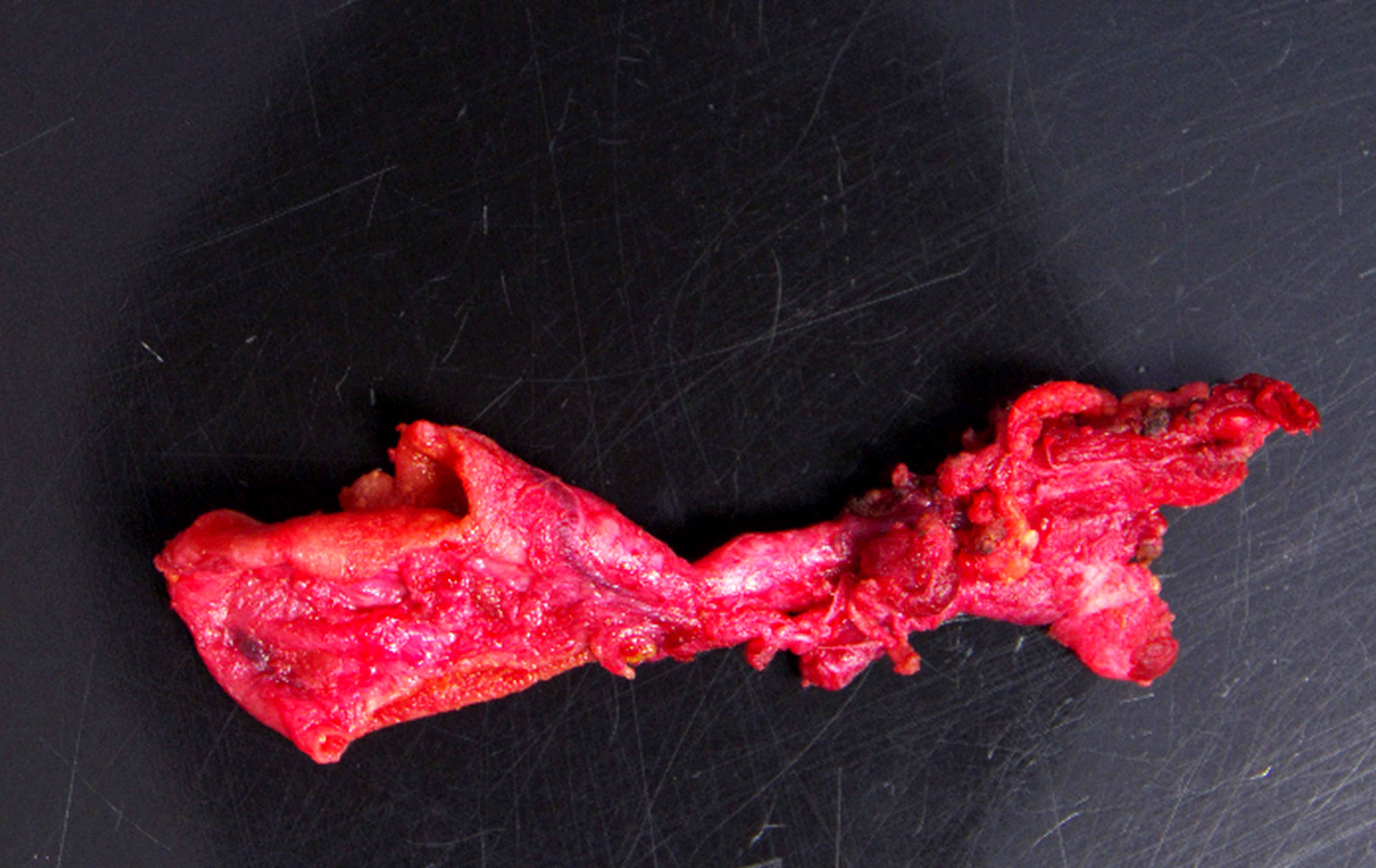
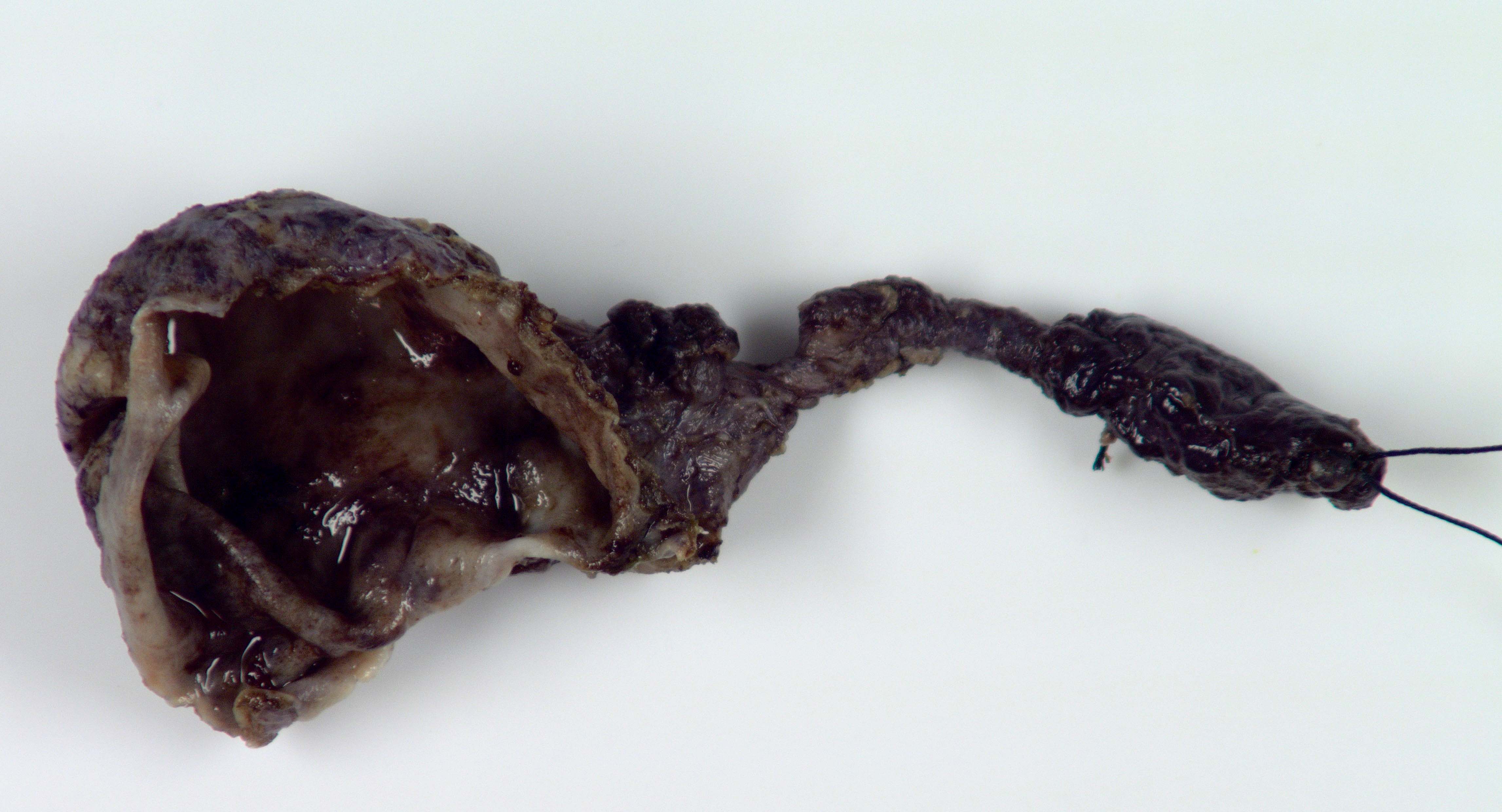
Gross description
- Segmental or complete dilatation of extrahepatic bile duct with mucosal hemorrhage and ulceration are common gross findings
- Some choledochal cysts can show double lumen (double bile duct)
- Can be associated with choledocholithiasis
- Mass lesion with firm, gritty cut surface when associated with malignancy
- References: Am J Surg Pathol 2021;45:627, Am J Surg Pathol 2017;41:354
Gross images
Frozen section description
- Intraoperative consultation may be requested to exclude the possibility of cholangiocarcinoma
Microscopic (histologic) description
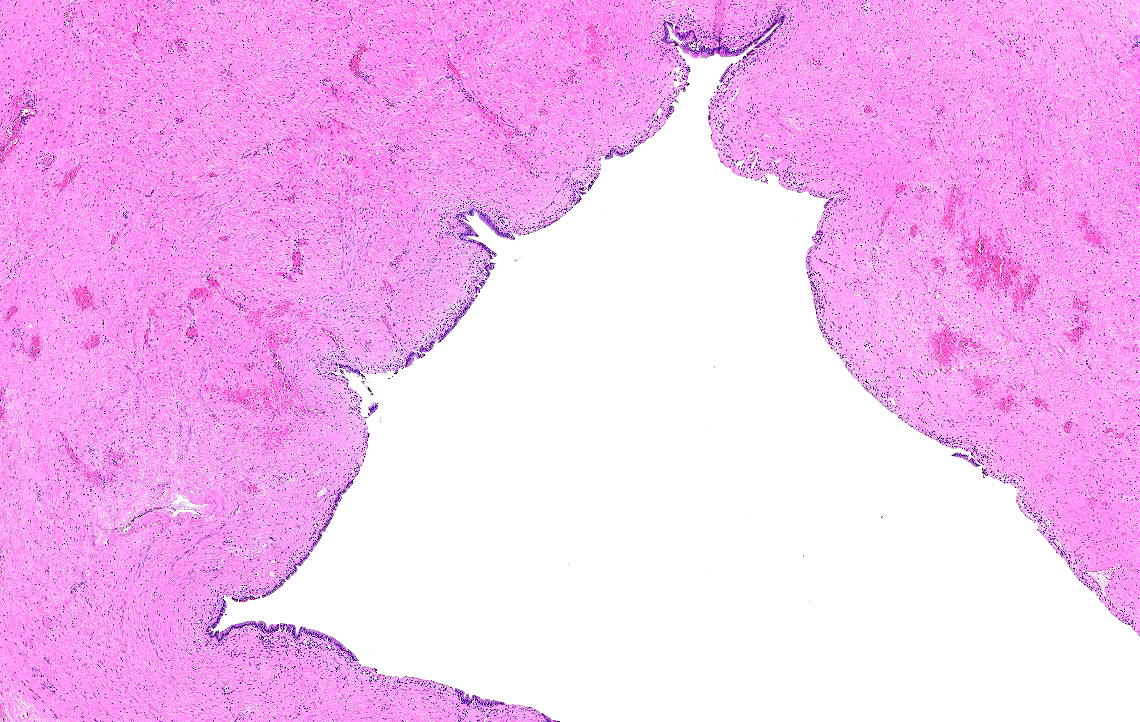
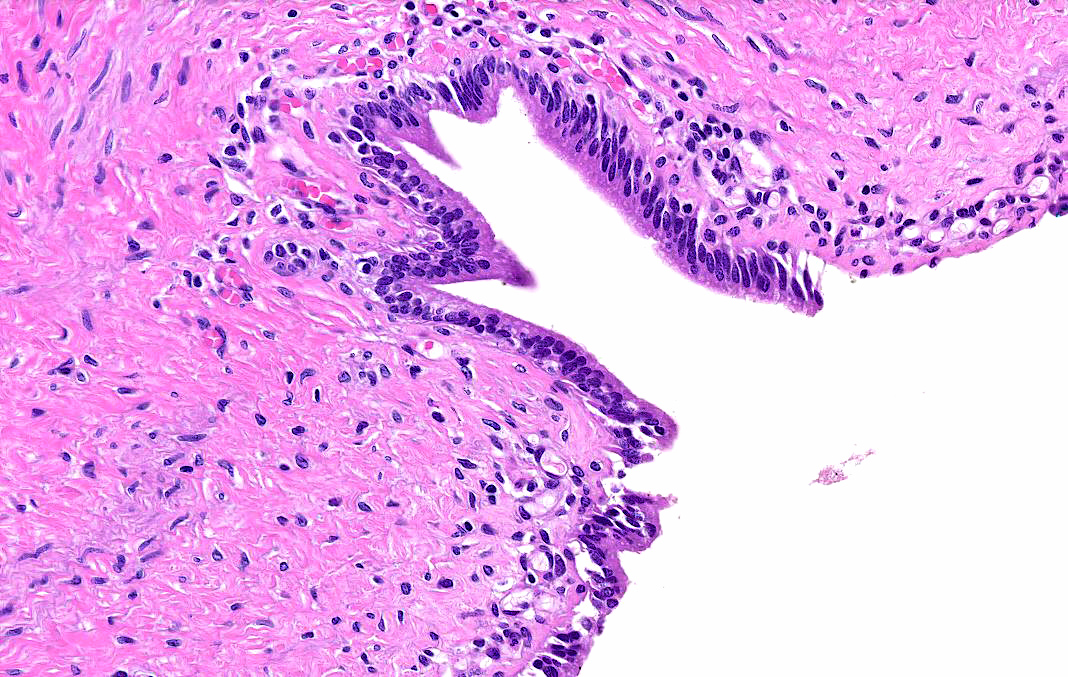
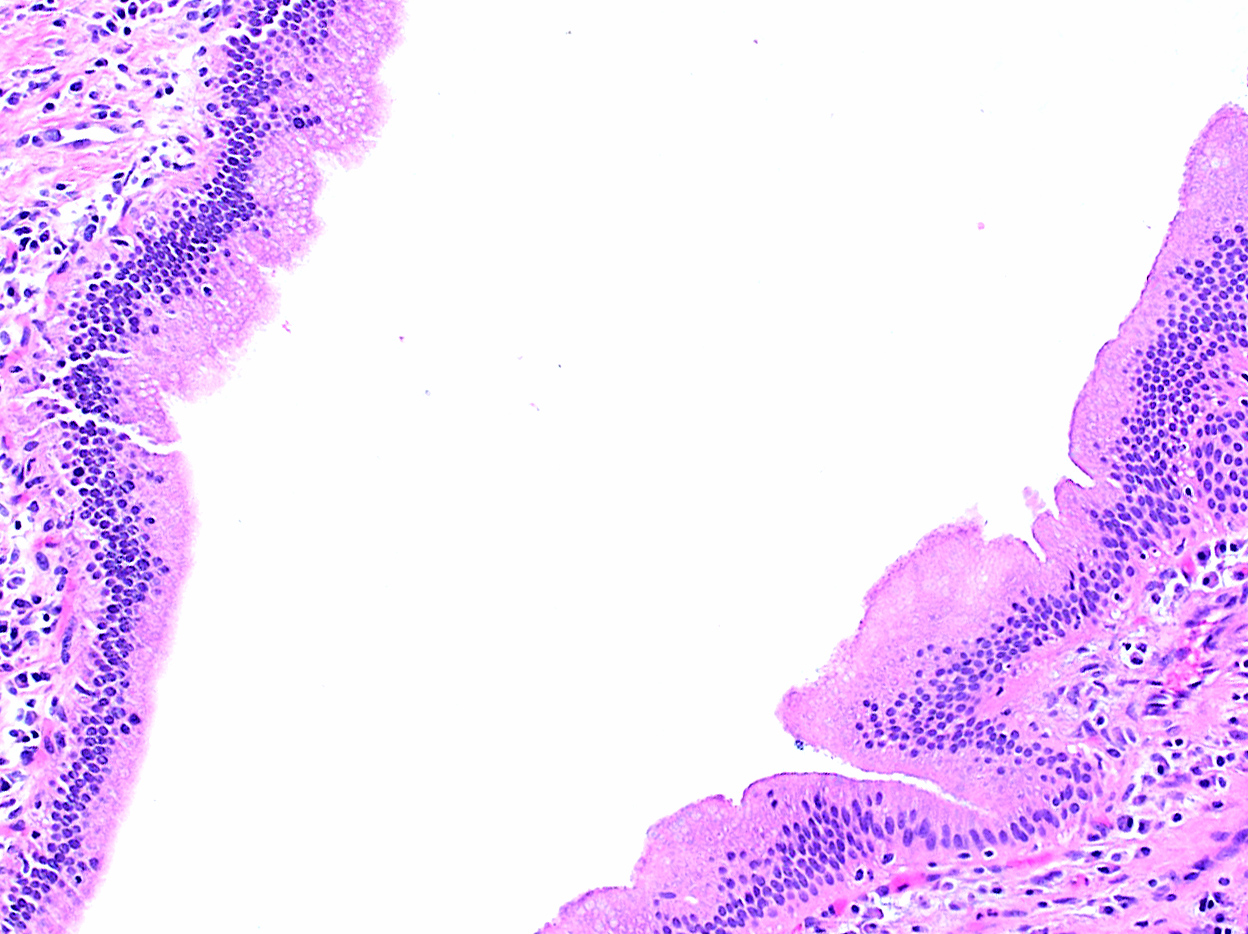
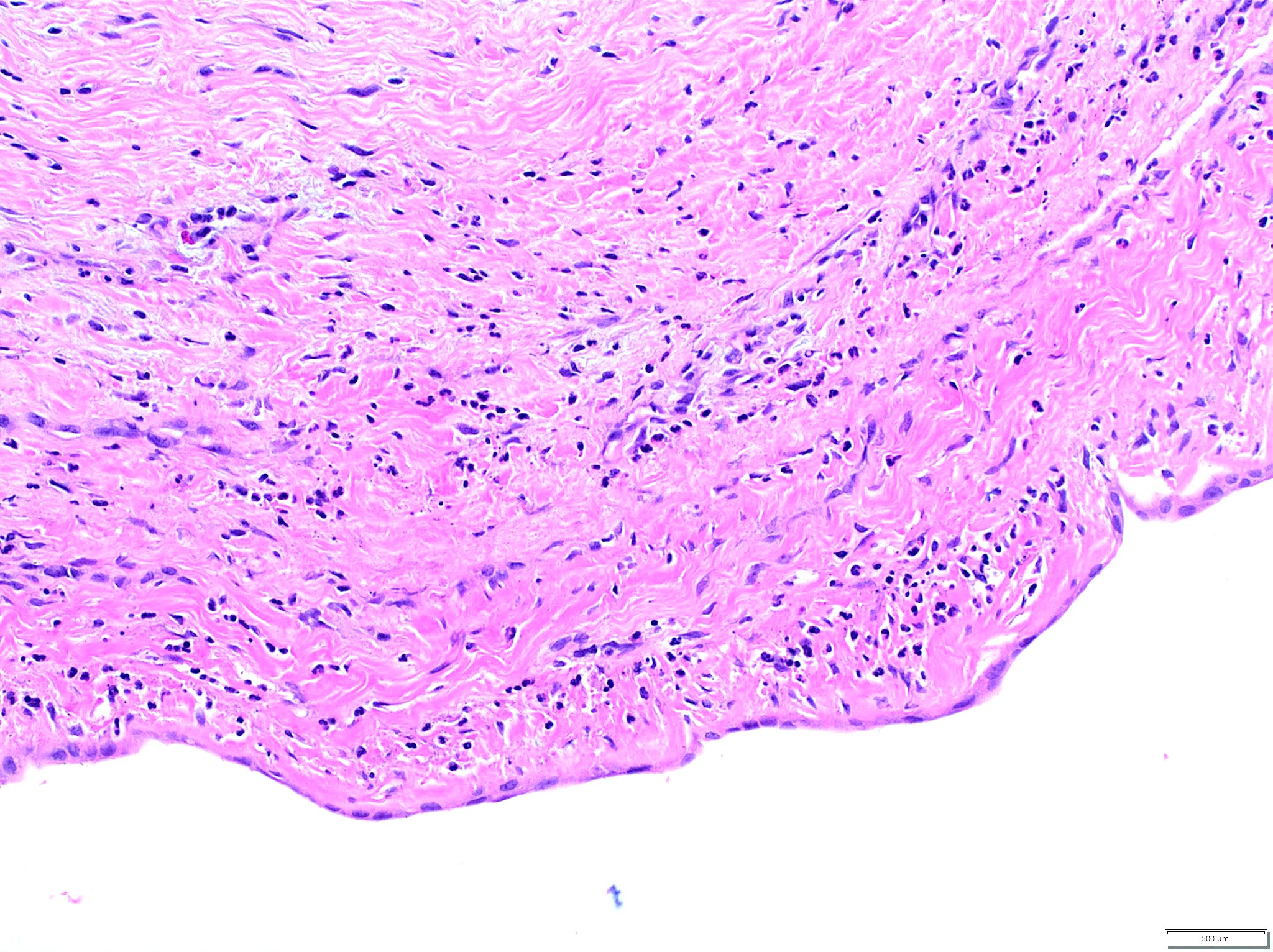
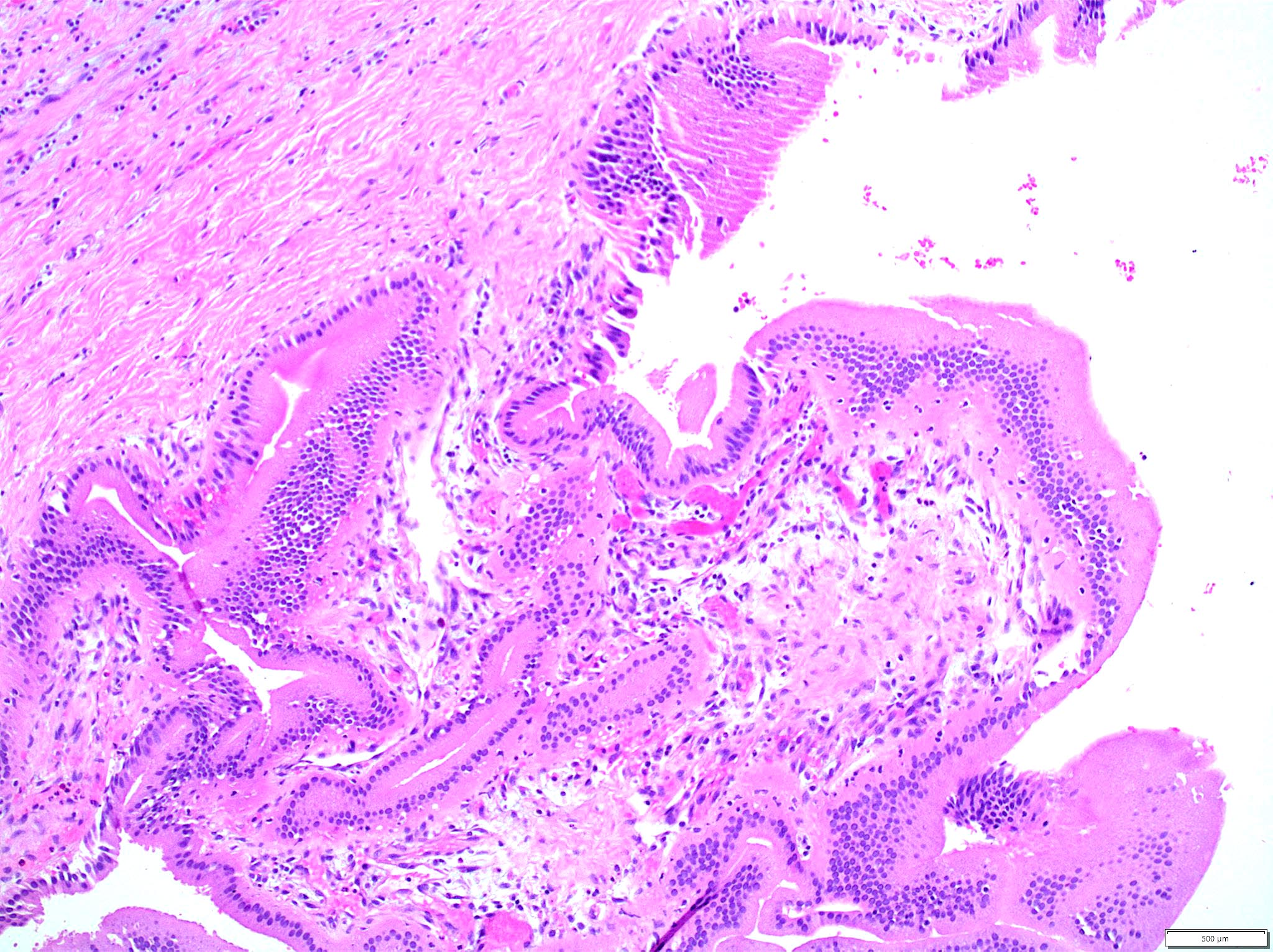
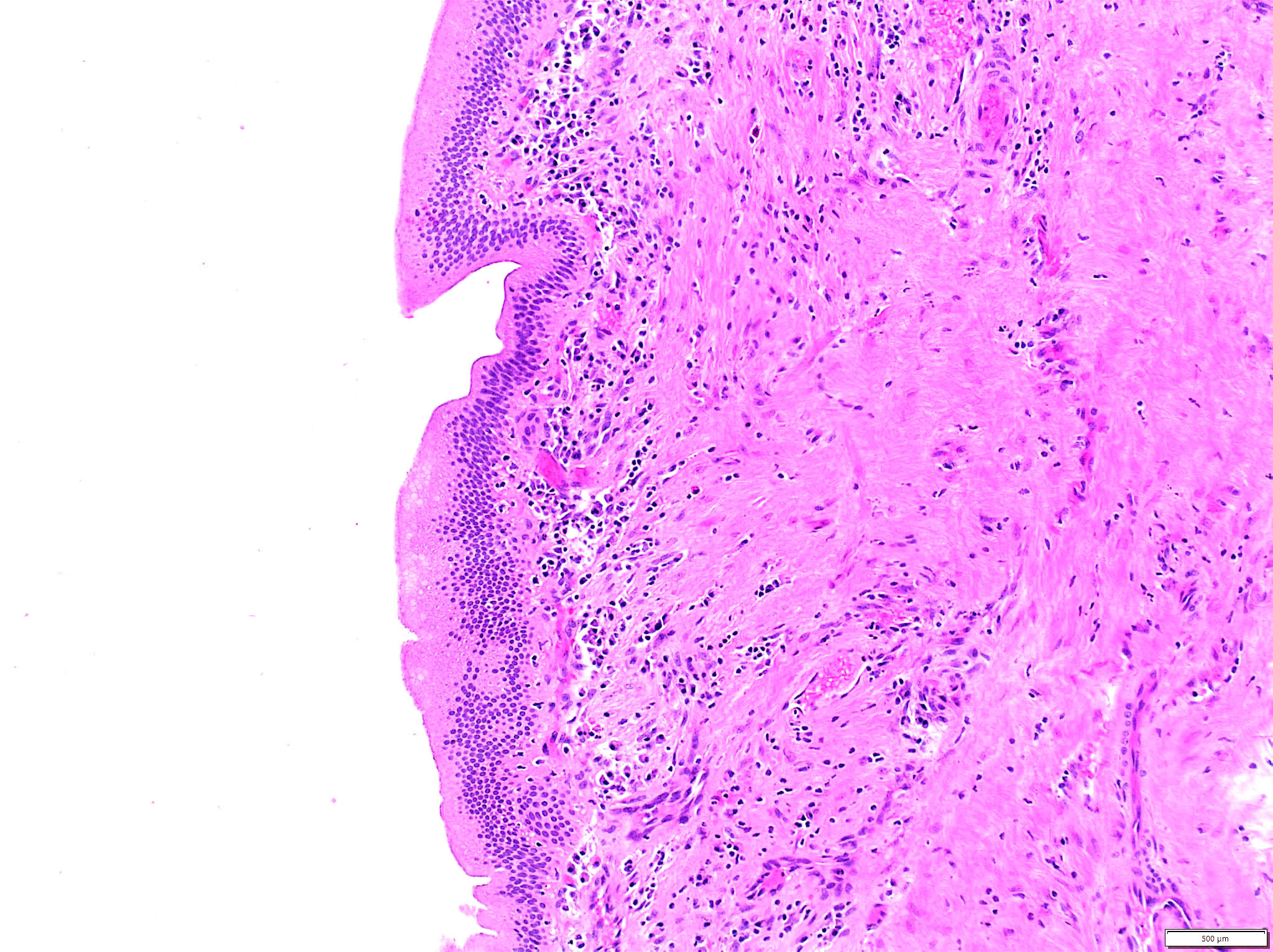
- Choledochal cysts are typically lined by biliary type epithelium with an underlying fibromuscular wall with varying degrees of inflammation, depending on age
- In infants, cysts show mostly intact, flat epithelium with sparse inflammation mainly composed of lymphocytes (J Pediatr Surg 1986;21:430, Am J Surg Pathol 2017;41:354)
- In older children, the epithelium is usually partially denuded or ulcerated, can show reactive alterations and is associated with more prominent mixed acute and chronic inflammation
- Smooth muscle bundles are present to a varying extent in the wall (Am J Surg Pathol 2017;41:354)
- In adults, there are 3 distinct pathology based categories (Am J Surg Pathol 2021;45:627)
- Cystic dilatation of native ducts: most common
- Double bile duct: most of the patients are women
- Gastrointestinal (GI) duplication type: rare and associated with gastrointestinal type mucosa and complete circumferential muscularis propria; may include Todani type III cysts
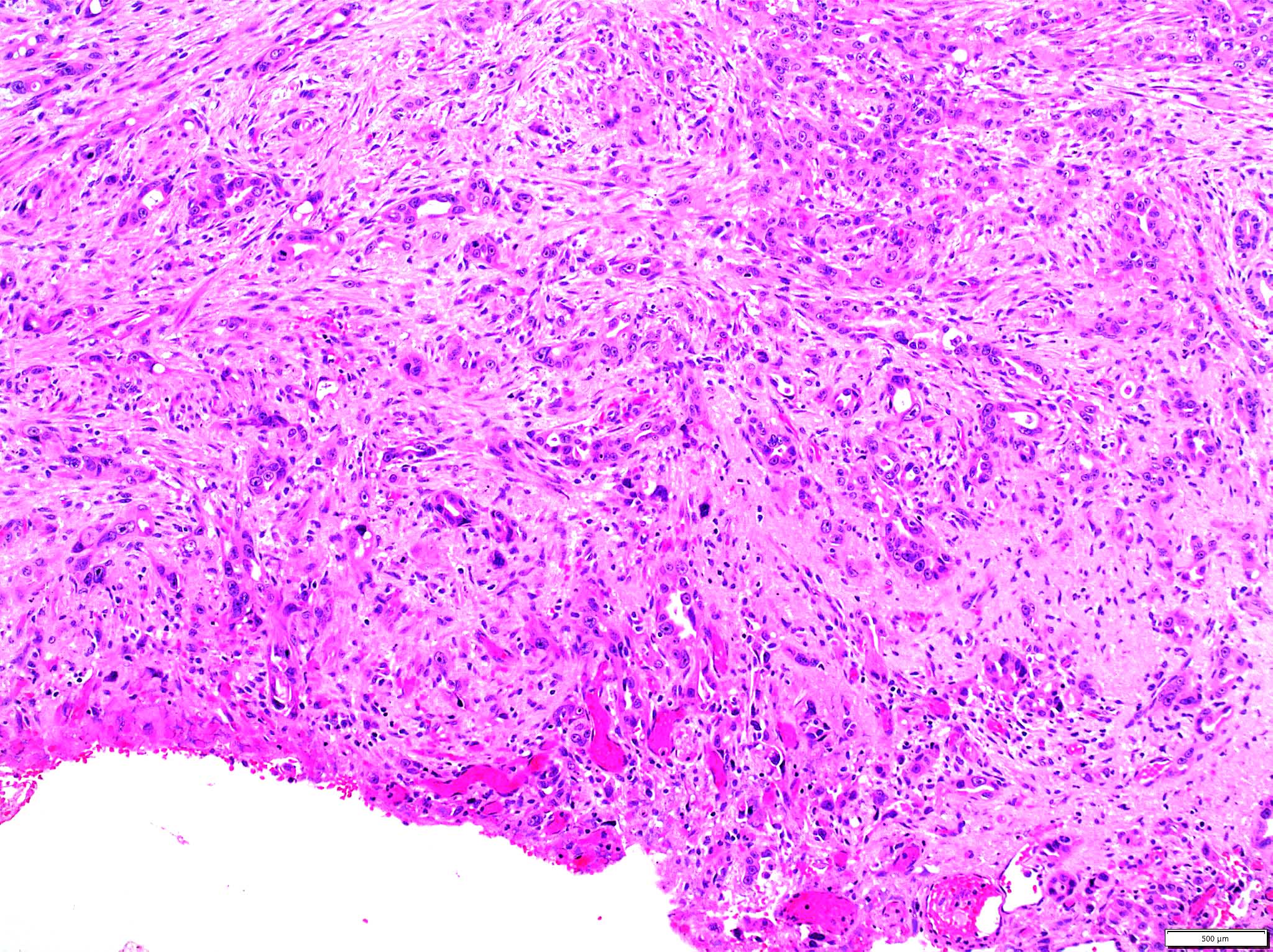
- Histologically, the most common feature is mucosa predominant lymphoplasmacytic infiltrate
- Other features include mucosal erosion / ulceration, acute inflammation and follicular cholangitis pattern with well formed lymphoid aggregates
- Mucosa can show variable hyperplastic changes with or without atypia and intestinal metaplasia
- Peribiliary mucous gland hyperplasia can be present in some cases
- Biliary intraepithelial neoplasia 3 (BilIN3) (high grade dysplasia / carcinoma in situ) can be present
- Cholangiocarcinoma is the most common type of malignancy associated with choledochal cysts
- Rare tumors, such as neuroendocrine tumors and rhabdomyosarcomas, have been described
Microscopic (histologic) images
Videos
Choledochal cyst by
Sonographic Tendencies
Sample pathology report
- Common bile duct, cyst, excision:
- Choledochal cyst with acute and chronic inflammation and reactive epithelial alterations (see comment)
- Negative for dysplasia or malignancy
- Comment: The sections of the dilated common bile duct show a cyst wall lined by reactive biliary epithelium and associated prominent acute and chronic inflammation, mucosal ulceration and foci of mucosal hyperplasia. Features of high grade dysplasia or malignancy are not identified. The findings are consistent with the clinical impression of a choledochal cyst.
Differential diagnosis
- Cystic biliary atresia (Am J Surg Pathol 2017;41:354):
- Cyst surface does not show epithelium or inflammation with a dense sclerotic inner layer and compact collagenous outer layer
- Cyst wall is devoid of smooth muscle, which is always seen to some extent with choledochal cyst
- Extrahepatic biliary atresia is usually seen distal and proximal to the cyst
- Gallbladder duplication (BMJ Case Rep 2021;14:e238971):
- Rarely, type II choledochal cyst can mimic gallbladder duplication on imaging
- Gallbladder duplication shows duplication of all layers of the gallbladder wall
- Pancreatic pseudocysts:
- Large choledochal cysts can mimic pancreatic pseudocysts clinically (Cureus 2022;14:e29806)
- ERCP / MRCP should be helpful to demonstrate no association with the biliary tree
Practice question #1
A 39 year old man presented with severe abdominal pain and jaundice. Ultrasound demonstrated cystic dilatation of the common bile duct, confirmed on magnetic resonance cholangiopancreatography. The patient underwent a surgical resection and microscopic findings of the cyst wall are shown above. What is the diagnosis?
- Biliary atresia
- Choledochal cyst
- Mesenteric cyst
- Pancreatic pseudocyst
Practice answer #1
B. Choledochal cyst. The clinical and histologic findings of an inflamed cyst wall lined by biliary type epithelium are consistent with a choledochal cyst. Answer A is incorrect because the age of presentation and dilated patent common bile duct are not features of biliary atresia. Answer D is incorrect because pancreatic pseudocysts do not show a true epithelial lining. Answer C is incorrect because mesenteric cysts are lined by mesothelium.
Comment Here
Reference: Choledochal cyst
Comment Here
Reference: Choledochal cyst