Table of Contents
Definition / general | Essential features | Terminology | ICD coding | Epidemiology | Sites | Pathophysiology | Etiology | Clinical features | Diagnosis | Laboratory | Case reports | Treatment | Microscopic (histologic) description | Microscopic (histologic) images | Sample pathology report | Differential diagnosis | Board review style question #1 | Board review style answer #1 | Board review style question #2 | Board review style answer #2Cite this page: Gonzalez RS. Autoimmune cholangitis. PathologyOutlines.com website. https://www.pathologyoutlines.com/topic/liverautoimmunecholangitis.html. Accessed April 26th, 2024.
Definition / general
- Essentially regarded as primary biliary cholangitis in patients with no detectable antimitochondrial antibody (Dig Dis Sci 1995;40:1232, Clin Liver Dis 2004;8:177)
- May in reality serve as a "wastebasket" heading for various related biliary diseases, though this remains unclear (Hepatology 2000;31:1231, Adv Anat Pathol 2002;9:244)
Essential features
- Mimics primary biliary cholangitis clinically and histologically, except antimitochondrial antibody is not detected
- Advanced techniques often do uncover antimitochondrial antibody in these patients
Terminology
- Also called antimitochondrial antibody negative primary biliary cholangitis (AMA negative PBC), autoimmune cholangiopathy
ICD coding
- ICD-10: K74.3 - primary biliary cirrhosis
Epidemiology
- Represents 5 - 10% of patients who otherwise fit diagnostic criteria for primary biliary cholangitis
Sites
- Not applicable
Pathophysiology
- Unclear; presumably autoimmune
Etiology
- Autoimmune disease
- Rare cases have been linked to IgG4 systemic disease, though these more likely represent IgG4 related sclerosing cholangitis (Acta Gastroenterol Latinoam 2011;41:55, J Med Case Rep 2011;5:485)
Clinical features
- More common in women; causes pruritus, fatigue
- Patients may be slightly younger on average than those with primary biliary cholangitis (Dig Dis Sci 1995;40:1232)
- May have worse outcome than antimitochondrial antibody positive primary biliary cholangitis patients (Scand J Gastroenterol 2016;51:745)
- Some patients may seroconvert to antimitochondrial antibody positivity (J Hepatol 1996;25:574)
Diagnosis
- Effectively the same as primary biliary cholangitis, except antimitochondrial antibody negative; true stringent criteria have not been defined (Clin Liver Dis 2018;22:589)
Laboratory
- Positive antinuclear antibody and smooth muscle antibody (at higher rates than primary biliary cholangitis patients); negative antimitochondrial antibody
- May have higher aspartate transaminase and bilirubin levels than primary biliary cholangitis patients (Hepatology 2000;31:1231)
- More sophisticated techniques (including primary biliary cholangitis specific antinuclear antibodies, such as Gp210 and sp100) have shown that many antimitochondrial antibody negative primary biliary cholangitis patients are in fact antimitochondrial antibody positive (Clin Res Hepatol Gastroenterol 2016;40:553, Hepatology 2007;45:659)
- Emerging biomarkers for diagnosis have been identified, though they show poor sensitivity (Clin Chem Lab Med 2017;56:25, Gastroenterol Res Pract 2019;2019:8959103)
Case reports
- 31 year old woman with pruritus, fatigue and weight loss (Euroasian J Hepatogastroenterol 2015;5:122)
- 47 year old woman with painless thyroiditis (Intern Med 1999;38:244)
- 59 year old woman with antimitochondrial antibody positive primary biliary cholangitis converted to antimitochondrial antibody negative (J Korean Med Sci 1999;14:102)
Treatment
- Ursodeoxycholic acid, which may be less successful than for antimitochondrial antibody positive patients
Microscopic (histologic) description
- Essentially the same as primary biliary cholangitis, except perhaps with less chronic portal inflammation
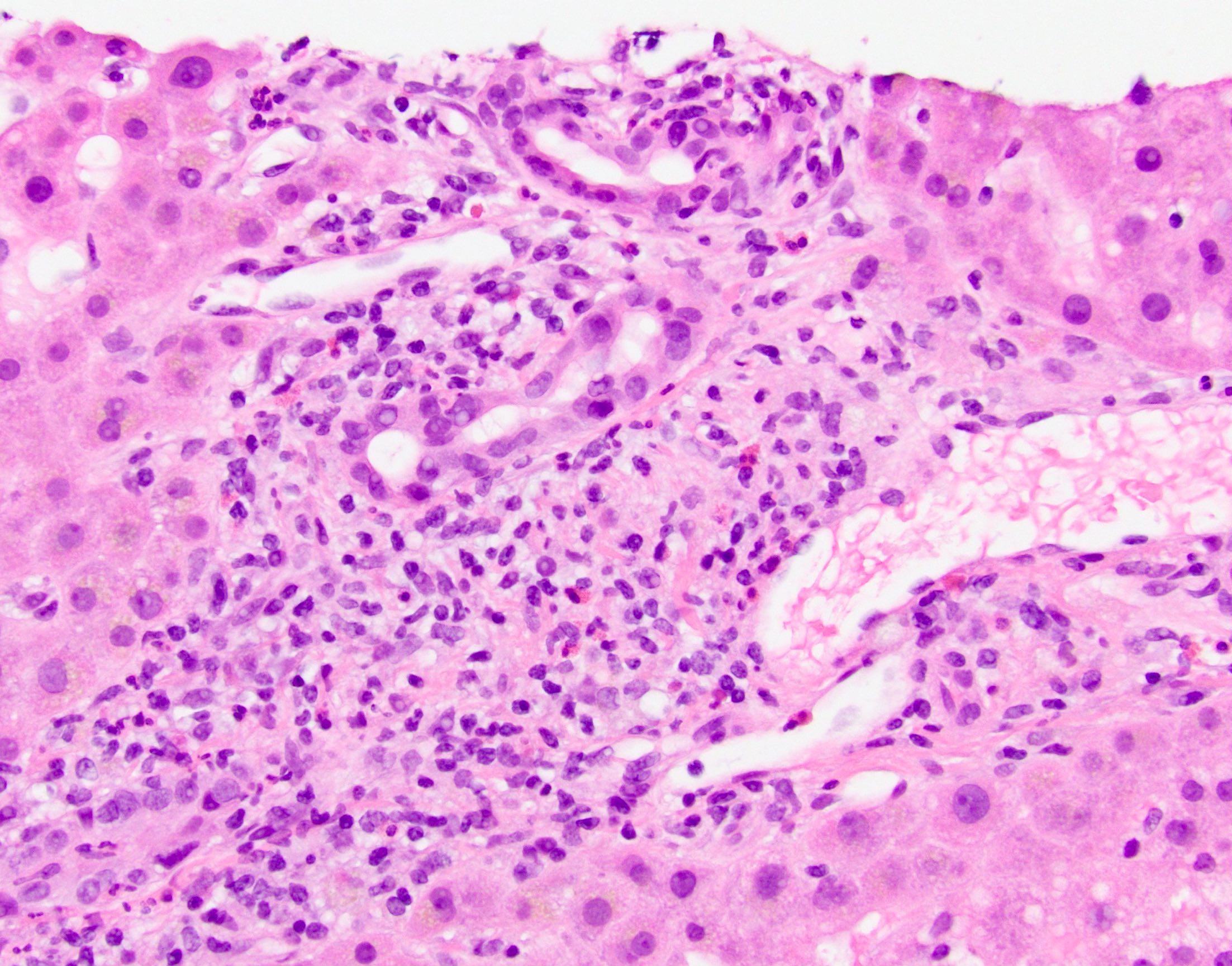
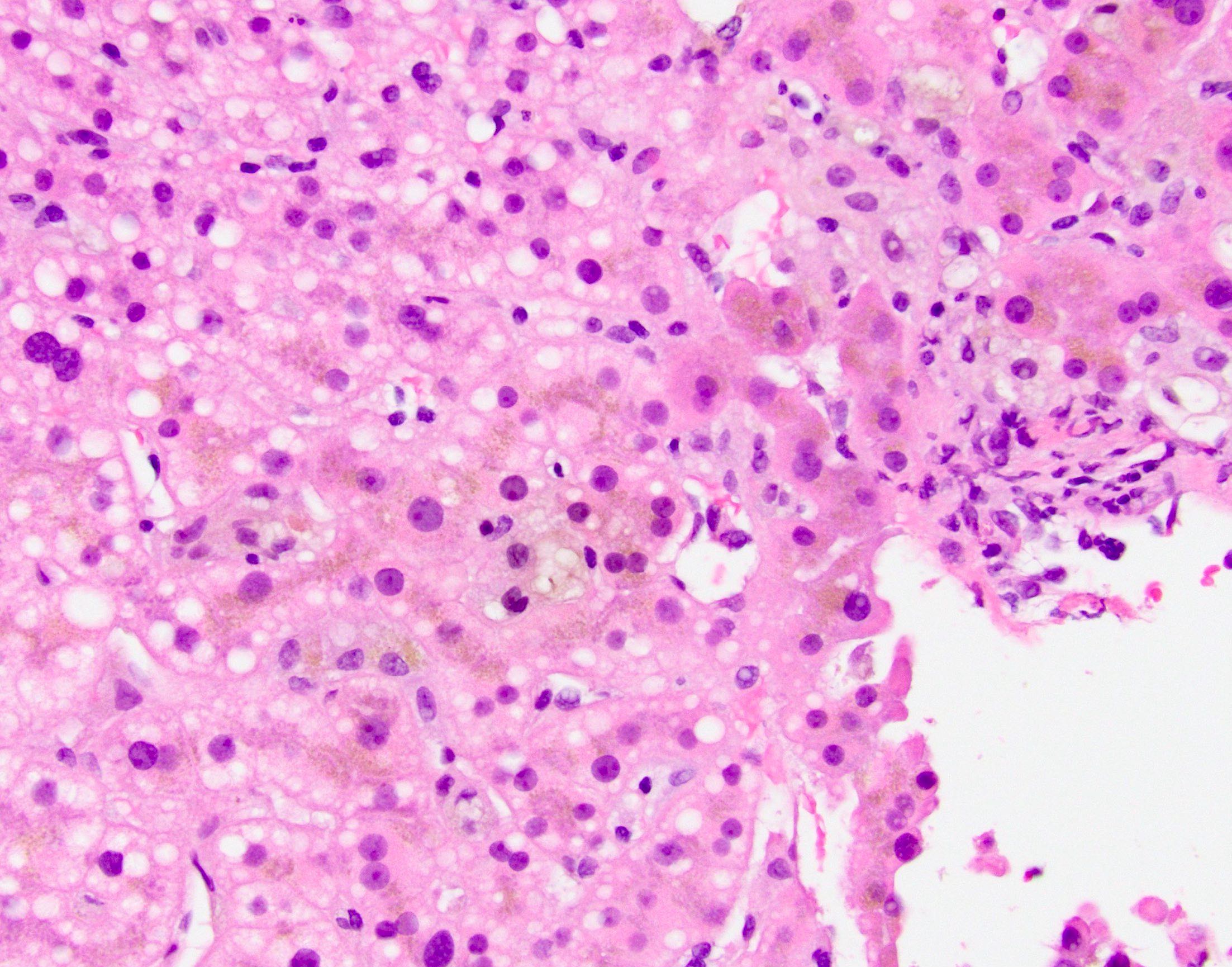
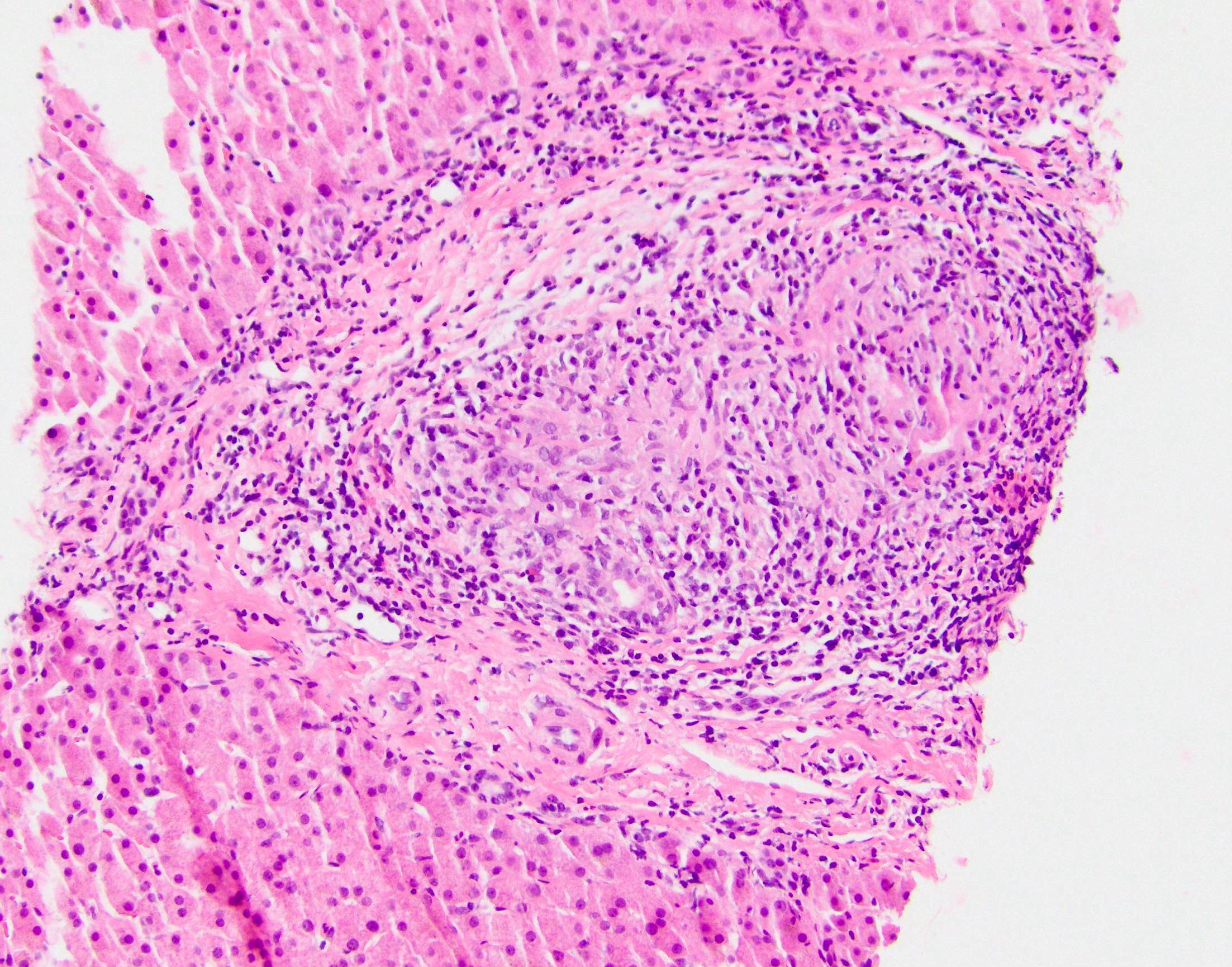
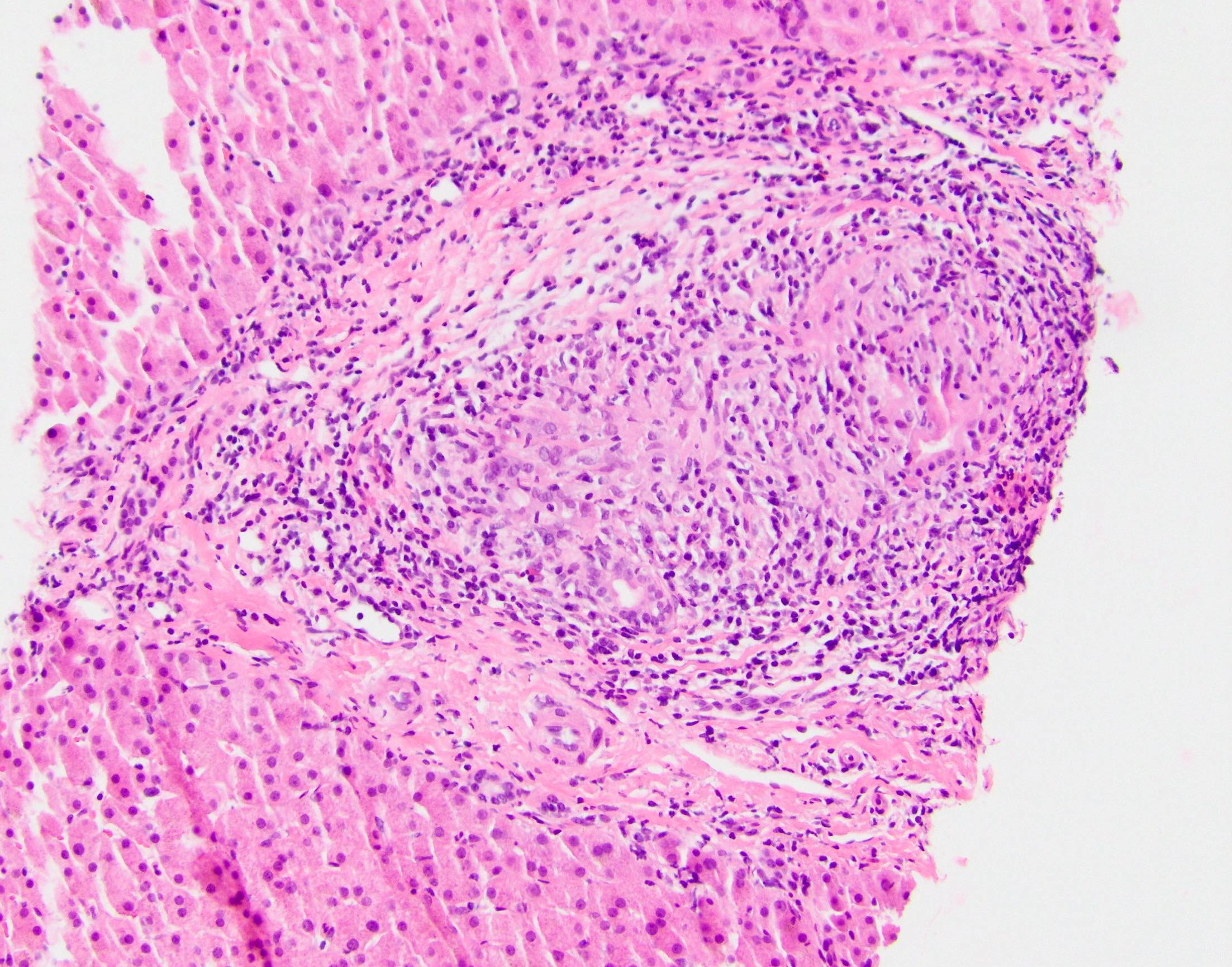
- Florid duct lesions (granulomas destroying bile ducts), lobular granulomas, duct injury and disarray, duct inflammation, ductular reaction, lobular cholestasis, ductopenia late
Microscopic (histologic) images
Sample pathology report
- Liver, biopsy:
- Biliary pattern injury with duct injury, ductular reaction and focal florid duct lesions (see comment)
- Comment: The changes are compatible with primary biliary cholangitis. Given the patient's reported negative antimitochondrial antibody, the overall findings may be most consistent with autoimmune cholangitis (antimitochondrial antibody negative primary biliary cholangitis).
Differential diagnosis
- Primary biliary cholangitis:
- Key distinction is antimitochondrial antibody status (positive in primary biliary cholangitis, negative in autoimmune cholangitis)
- Drug induced liver injury:
- Requires clinical correlation to rule out drug cause (Gastroenterology Res 2019;12:211)
- IgG4 related sclerosing cholangitis:
- Findings typically centered around large ducts, with sclerosis and prominent plasmacytic inflammation (Korean J Hepatol 2011;17:76)
Board review style question #1
What is the key distinction between primary biliary cholangitis and autoimmune cholangitis?
- Alkaline phosphatase level
- Antimitochondrial antibody status
- Antineutrophil cytoplasmic antibody status
- Antinuclear antibody status
- Anti-smooth muscle antibody status
Board review style answer #1
Board review style question #2
A 45 year old woman complaining of jaundice is found to have elevated liver enzymes. The figure above shows a liver biopsy. The patient's physician orders serology for antimitochondrial antibodies, which returns as negative. Which of the following is the most likely explanation?
- The liver sample must have actually come from a different patient
- The patient has autoimmune cholangitis
- The patient has sarcoidosis
- The patient has tuberculosis
- The serology testing returned a false negative result
Board review style answer #2