Table of Contents
Definition / general | Essential features | Terminology | Concept of complete autopsy in SIDS / SUDC / SUDEP | Cause and manner of death in SIDS, SUDC and SUDEP | ICD coding | Epidemiology | Pathophysiology | Diagrams / tables | Gross description | Microscopic (histologic) description | Microscopic (histologic) images | Practice question #1 | Practice answer #1 | Practice question #2 | Practice answer #2 | Practice question #3 | Practice answer #3Cite this page: Cohen MC. Sudden unexpected deaths in infants and children. PathologyOutlines.com website. https://www.pathologyoutlines.com/topic/forensicspediatricdeaths.html. Accessed August 29th, 2025.
Definition / general
- Sudden unexpected death in infancy (SUDI) refers to a death that was not anticipated as a significant possibility 24 hours before the death; it would include deaths occurring as a result of an acute illness not anticipated 24 hours before the death, deaths arising from a previously known condition not expected to lead to death or deaths arising from a pre-existing condition not previously recognized (Cohen: The Pediatric and Perinatal Autopsy Manual, 1st Edition, 2014)
- Sudden infant death syndrome (SIDS) or sudden unexplained infant death (SUID) is the sudden death of an infant under 1 year of age with the cause of death unclear after a thorough case investigation, including performance of a complete autopsy, examination of the death scene and a review of the clinical history (Pediatr Pathol 1991;11:677, Boston Children's Hospital: Sudden Infant Death Syndrome (SIDS) [Accessed 9 June 2025], The Lullaby Trust: When a Baby Dies [Accessed 9 June 2025])
- Sudden unexpected death in childhood (SUDC) is the sudden death of a child over the age of 12 months (and up to 18 years old) which remains unexplained after a thorough case investigation, including review of the child's medical history, circumstances of death, a complete autopsy and ancillary testing (Pediatr Dev Pathol 2005;8:307)
- Sudden unexpected death in epilepsy (SUDEP) is the sudden, unwitnessed, nontraumatic and nondrowning death of otherwise healthy patients with known epilepsy and excluding documented status epilepticus, in which the postmortem examination does not reveal a cause of death (Lancet Neurol 2016;15:1075, Epilepsia 2012;53:227)
Essential features
- SIDS / SUID is the sudden death of an infant under 1 year of age with the cause of death unclear after a thorough case investigation, including the performance of a complete autopsy, examination of the death scene and a review of the clinical history (Cohen: The Pediatric and Perinatal Autopsy Manual, 1st Edition, 2014, Pediatr Pathol 1991;11:677, Boston Children's Hospital: Sudden Infant Death Syndrome (SIDS) [Accessed 9 June 2025], The Lullaby Trust: When a Baby Dies [Accessed 9 June 2025])
- SUDC is the same as above but in a child over the age of 12 months (and up to 18 years old) (Pediatr Dev Pathol 2005;8:307)
- SUDEP is the sudden, unwitnessed, nontraumatic and nondrowning death of otherwise healthy patients with known epilepsy and excluding documented status epilepticus, in which the postmortem examination does not reveal a cause of death (Lancet Neurol 2016;15:1075, Epilepsia 2012;53:227)
- Postmortem examination is always negative
- Risk factors have been identified in SIDS and SUDEP
Terminology
- SIDS: SUDI, SUID, undetermined and unascertained
- If a SUID type death occurs in the context of an unsafe sleep environment (e.g., the baby sleeping with adults who have consumed alcohol or drugs, on an adult bed or sofa, with multiple articles of bedding or trapped between 2 surfaces), an accidental manner of death cannot be completely excluded and such cases are best certified as undetermined
Concept of complete autopsy in SIDS / SUDC / SUDEP
- Recommended protocol to conduct the autopsy in an unexpected death in infants and children includes (The Royal College of Pathologists: New Guidelines for the Investigation of Sudden Unexpected Death in Infancy Launched [Accessed 10 June 2025], The Royal College of Pathologists: Guidelines on Autopsy Practice - Sudden Unexpected Deaths in Infancy and Childhood [Accessed 10 June 2025])
- Images: Xray / CT scan
- Full external and internal examination with photographic documentation of positive and negative findings
- Nasopharyngeal swabs for virology and microbiology
- Skin sample for karyotype
- Skin sample for fibroblast culture to investigate fatty acid oxidation
- Tracheal samples for virology and microbiology
- Blood culture
- Blood sample for toxicology
- Lung tissue sample for virology
- Lung swab for microbiology
- Urine (if available): toxicology and organic acid analysis
- Vitreous: toxicology
- Bowel content: virology and microbiology
- Cerebrospinal fluid (CSF): virology and microbiology
- Histology of all organs
- Store a small frozen tissue sample (at -80° C) from kidney, heart, muscle and liver
- After the postmortem investigation, current advice is to conduct whole genome sequencing (WGS) (Am J Med Genet A 2024;194:e63596)
- This is a consented analysis, which is requested by the clinical geneticist and involves a trio analysis (both parents and decedent infant / child frozen tissue sample)
- Numerous gene variants have been identified in SIDS (64.5%), with many of the identified variants known for their involvement in cardiac diseases, neurological disorders, the immune response, the regulation of neuronal excitability and the response to hypoxia and oxidative stress
- WGS analysis and research is still in early stages but it is hypothesized that many gene variants may contribute to the genetic susceptibility to SIDS
Cause and manner of death in SIDS, SUDC and SUDEP
- Cause of death in SIDS, SUDC and SUDEP is unknown after a thorough postmortem with review of family history and death scene investigation
- Manner of death in SIDS, SUDC and SUDEP is natural
- In SIDS, cessation of cardiac and respiratory activity results from a combination of genetic vulnerability, a developmental period and risk factors
- No risk factors have been identified in SUDC
- Manner of death in SUDEP appears to be related to seizure related disfunction of cardiac or respiratory activities (Sleep Med Rev 2011;15:237)
- When it is unknown whether external factors (such as an unsafe sleep environment) may have caused or contributed to the death, the manner of death is best certified as undetermined
ICD coding
Epidemiology
- Risk factors for SIDS / SUID: most SIDS / SUID occur during sleep, prone or side sleeping, inappropriate sleep surface, maternal smoking during pregnancy, sharing the sleep surface with an adult (especially when this person smokes, has taken drugs or alcohol or is excessively tired, particularly when the sleeping surface is a sofa or settee but also includes a bed), head covering, overheating, male sex, family history of SIDS, winter months, having a cold (upper respiratory tract infection), prematurity and low birth weight (Cohen: The Pediatric and Perinatal Autopsy Manual, 1st Edition, 2014, Cohen: Investigation of Sudden Infant Death Syndrome (Diagnostic Pediatric Pathology), 1st Edition, 2019)
- In the U.K., mixed Black African / White, mixed Black Caribbean / White and Black Caribbean babies showed the highest risk of SUDI, compared with the lowest risk of SUDI in Indian, Bangladeshi, Pakistani, White non-British and Black African babies; while White British babies had an intermediate risk (NPEU, University of Oxford: Sudden Infant Death Syndrome (SIDS) and Other Unexplained Infant Death: Nearly 5-Fold Variation in Risk Between Different Ethnic Groups in England and Wales [Accessed 17 February 2025])
- In the U.S., non-Hispanic Black infants have an 83% higher mortality rate from SIDS than non-Hispanic White infants; American Indian / Alaskan Native infants have a 95% higher mortality rate (Duncan: SIDS Sudden Infant and Early Childhood Death - The Past, the Present and the Future, 1st Edition, 2018)
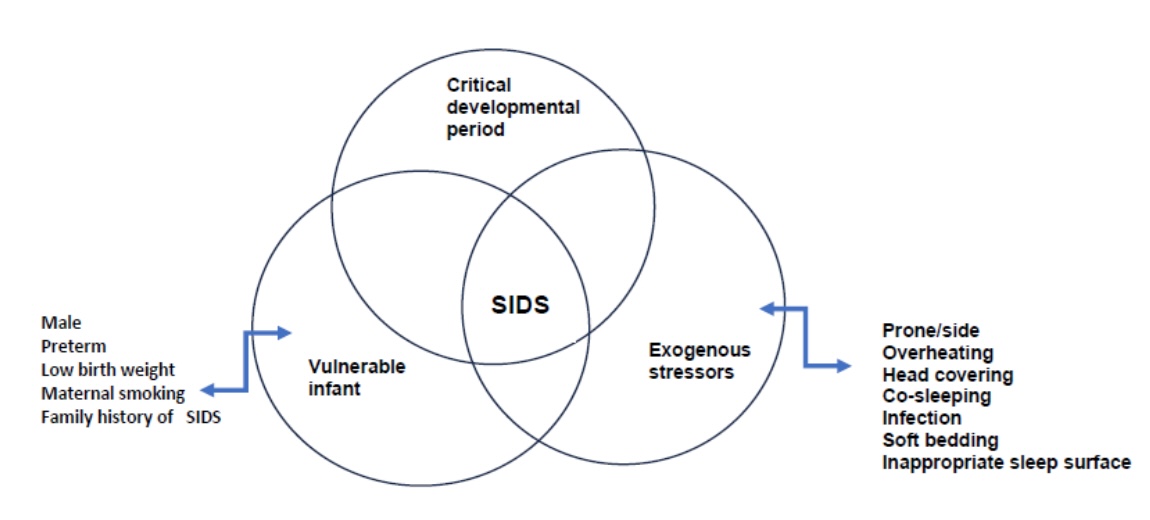
- Triple risk hypothesis (Biol Neonate 1994;65:194)
- According to the triple risk model, SIDS results from the intersection of 3 overlapping factors: a vulnerable infant, a critical developmental period in homeostatic control and an exogenous stressor(s) (see Diagrams / tables)
- Infant will die of SIDS only if he / she possesses all 3 factors; the infant's vulnerability lies latent until he / she enters the critical period and is subject to an exogenous stressor
- Risk factors for SUDC (SUDC UK: Facts About SUDC [Accessed 7 February 2025], JAMA Netw Open 2019;2:e192739)
- No known risk factors for SUDC have been identified; however, most often are between 1 and 4 years of age (62.5%), most often are males (55.3%), unwitnessed death during apparent sleep (95.8%), usually found prone (sleeping on their front) (63.5%), may have an association with febrile seizures (28.8%) or fever or illness symptoms within 48 hours of death (75%)
- Risk factors for SUDEP (Lancet Neurol 2016;15:1075, CDC: Sudden Unexpected Death in Epilepsy [Accessed 7 February 2025])
- Main risk factors: > 3 generalized tonic clonic seizures per year and uncontrolled or frequent seizures
- Possible risk factors: having seizures from a young age, male sex, missing doses of seizure medicine or resistance to antiseizure medication, having seizures during sleep / nocturnal seizures or intellectual impairment or developmental delay
- Incidence of SIDS / SUID: 38.7 deaths per 100,000 live births (Duncan: SIDS Sudden Infant and Early Childhood Death - The Past, the Present and the Future, 1st Edition, 2018)
- Incidence of SUDC: 0.93 per 100,000 between 1 and 4 years of age, where it is the fourth leading cause of death; overall (1 - 18 years) incidence is 1.0 - 1.4 deaths per 100,000 of the population (Pediatr Dev Pathol 2005;8:307, SUDC UK: Facts About SUDC [Accessed 7 February 2025], Duncan: SIDS Sudden Infant and Early Childhood Death - The Past, the Present and the Future, 1st Edition, 2018)
- Incidence of SUDEP in children: 0.22 - 1.11 per 1,000 person years (Epilepsia 2012;53:227)
Pathophysiology
- No definitive pathophysiology has been proved
- SIDS / SUID
- Abnormalities in autonomic control mechanisms and failure in the arousal response to an asphyxiating environment, leading to hypoxic coma, bradycardia and gasping and ultimately, to a failure of autoresuscitation (Cohen: Investigation of Sudden Infant Death Syndrome (Diagnostic Pediatric Pathology), 1st Edition, 2019)
- Genetic heart disease (GHD) also appears to play a role in some cases: a study showed that 12.6% of SIDS cases had ≥ 1 potentially informative, GHD associated variant, although only 4.3% of cases possessed immediately clinically actionable variants (J Am Coll Cardiol 2018;71:1217)
- SUDC
- Pathogenic cardiac variants (in up to 25%), history of febrile seizures (33% cases) and hippocampal abnormalities (44%) (Cohen: The Pediatric and Perinatal Autopsy Manual, 1st Edition, 2014, Front Neurol 2020;11:582051)
- SUDEP
- Unwitnessed terminal seizure episode, usually generalized convulsive type, involving dysregulation of the cardiac, respiratory and autonomic nervous system and linked to underlying physiologic and genetic mechanisms (Epilepsia 2012;53:227, Dev Med Child Neurol 2023;65:1150)
Gross description
- No significant findings; may include anterior lividity with paleness of midface seen when prone, blood stained fluid or frank blood around the nose, petechiae on thymus, heart or pleural surfaces in some cases (Cohen: The Pediatric and Perinatal Autopsy Manual, 1st Edition, 2014, Forensic Sci Med Pathol 2020;16:423)
Microscopic (histologic) description
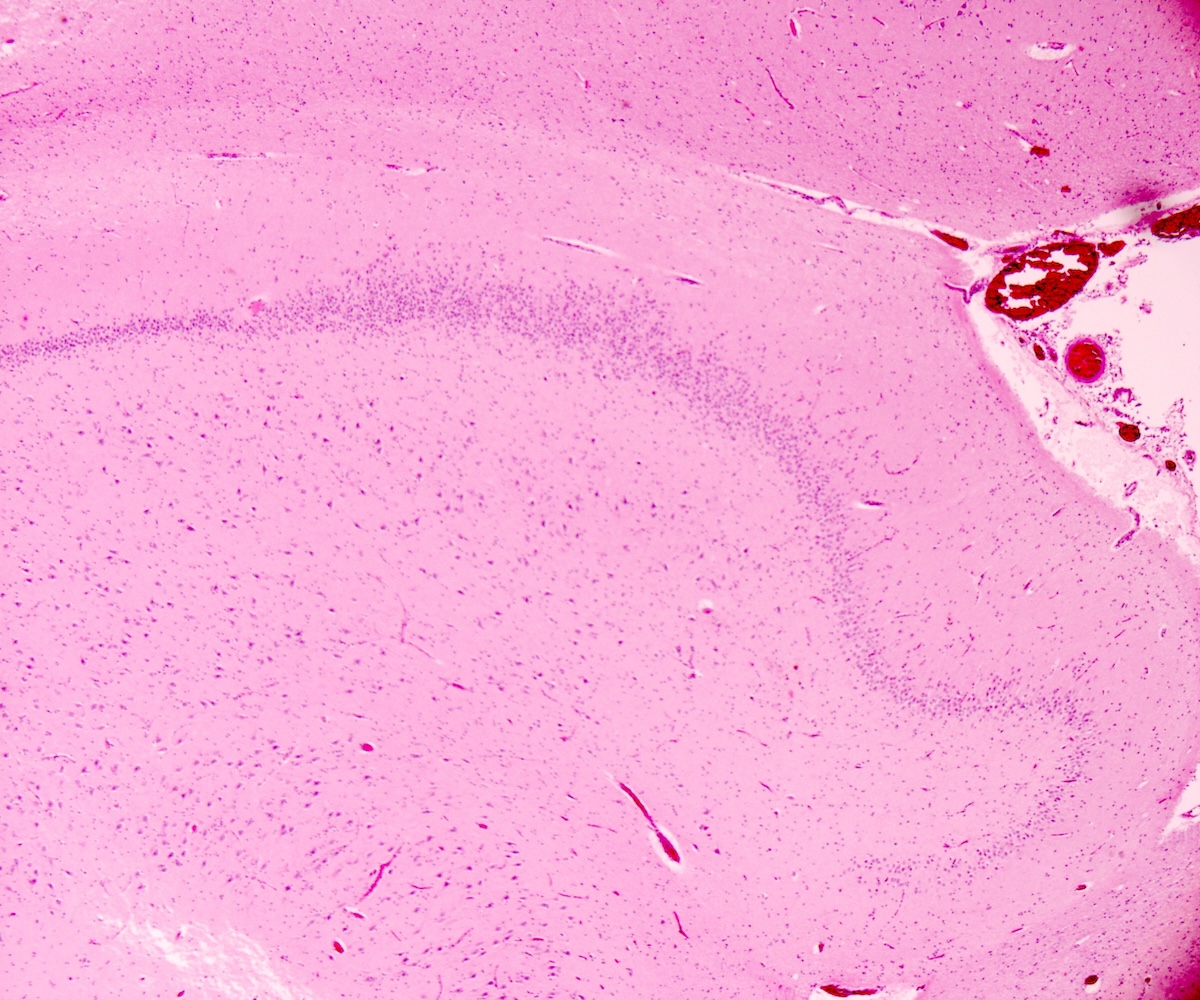
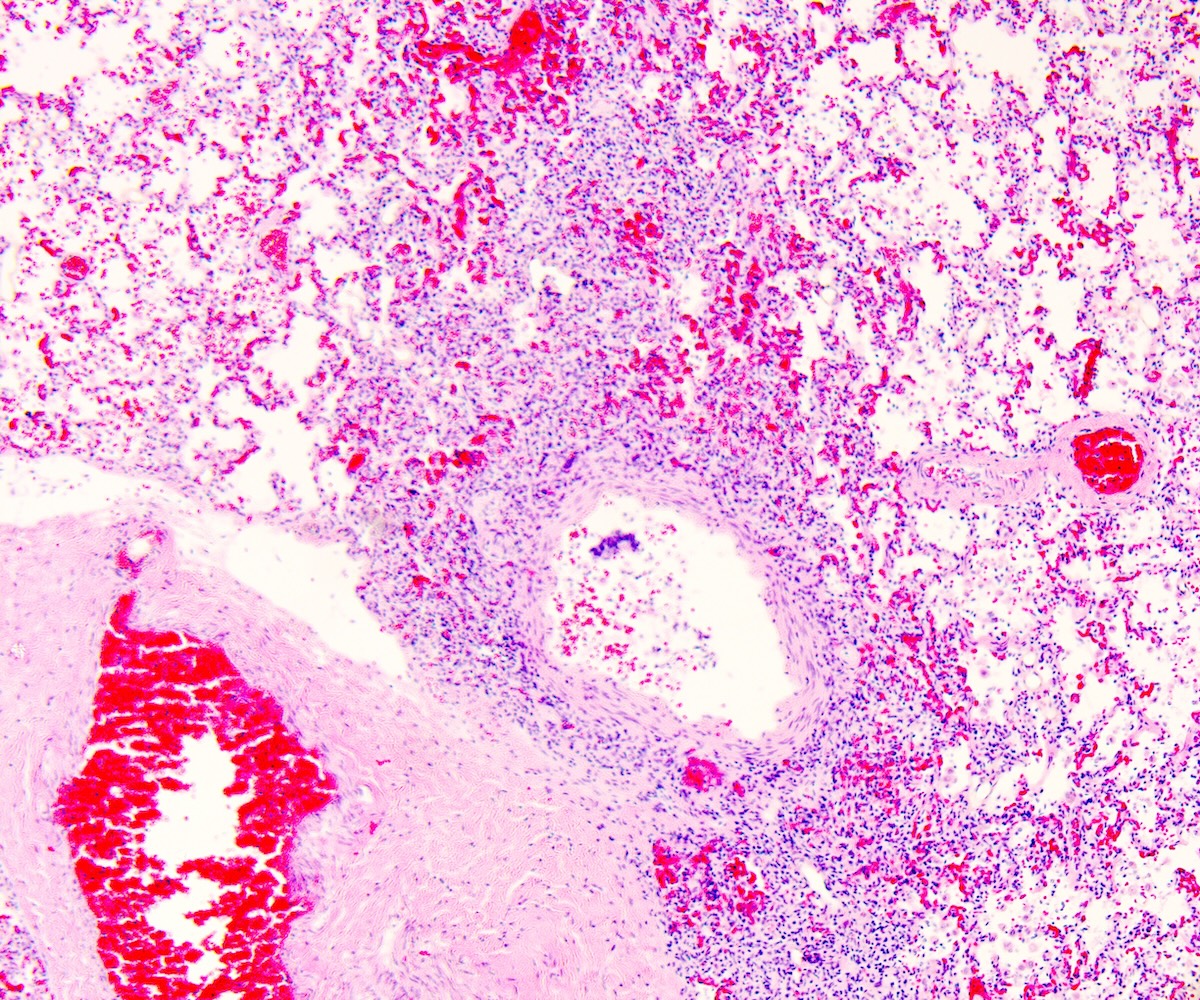
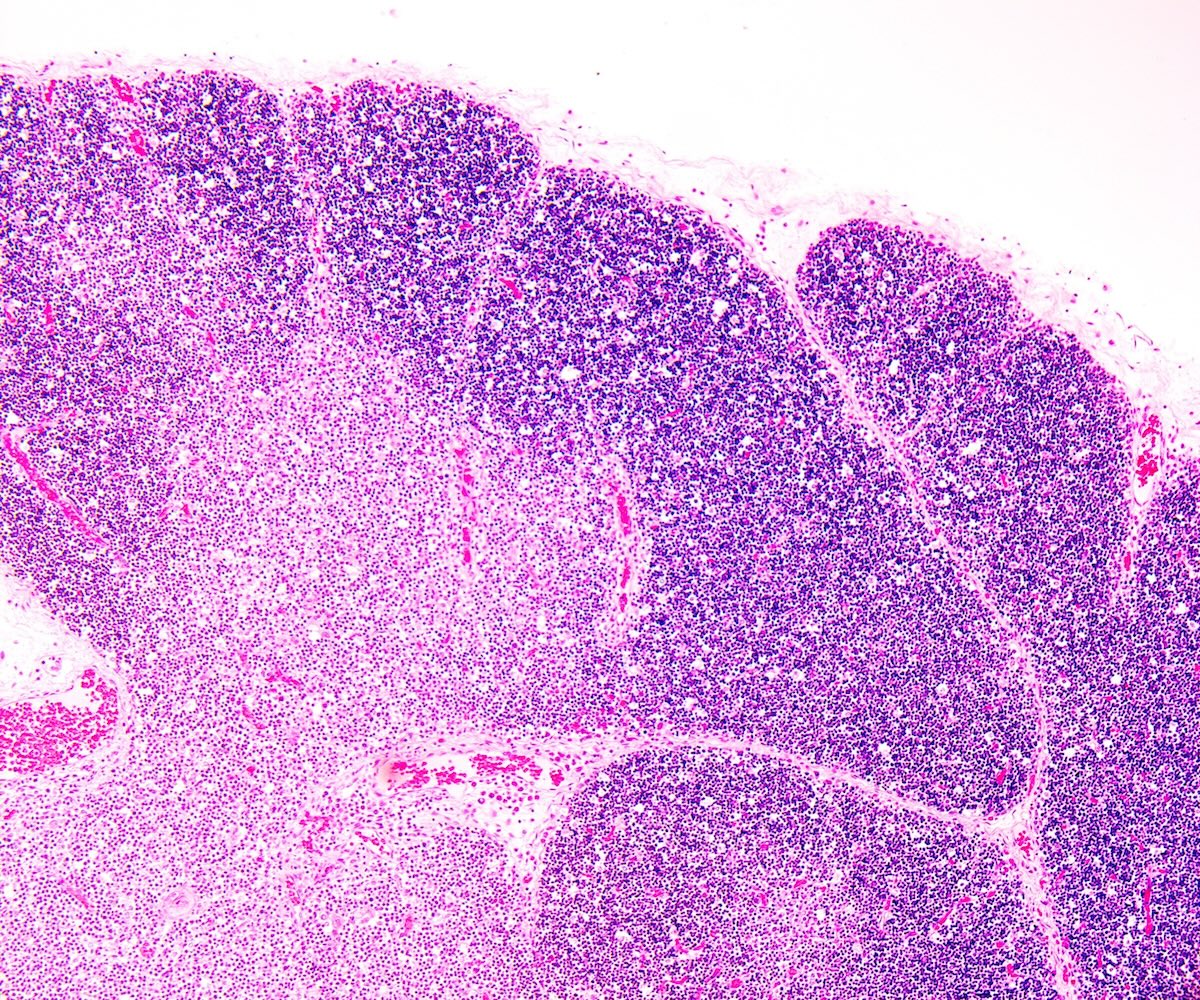
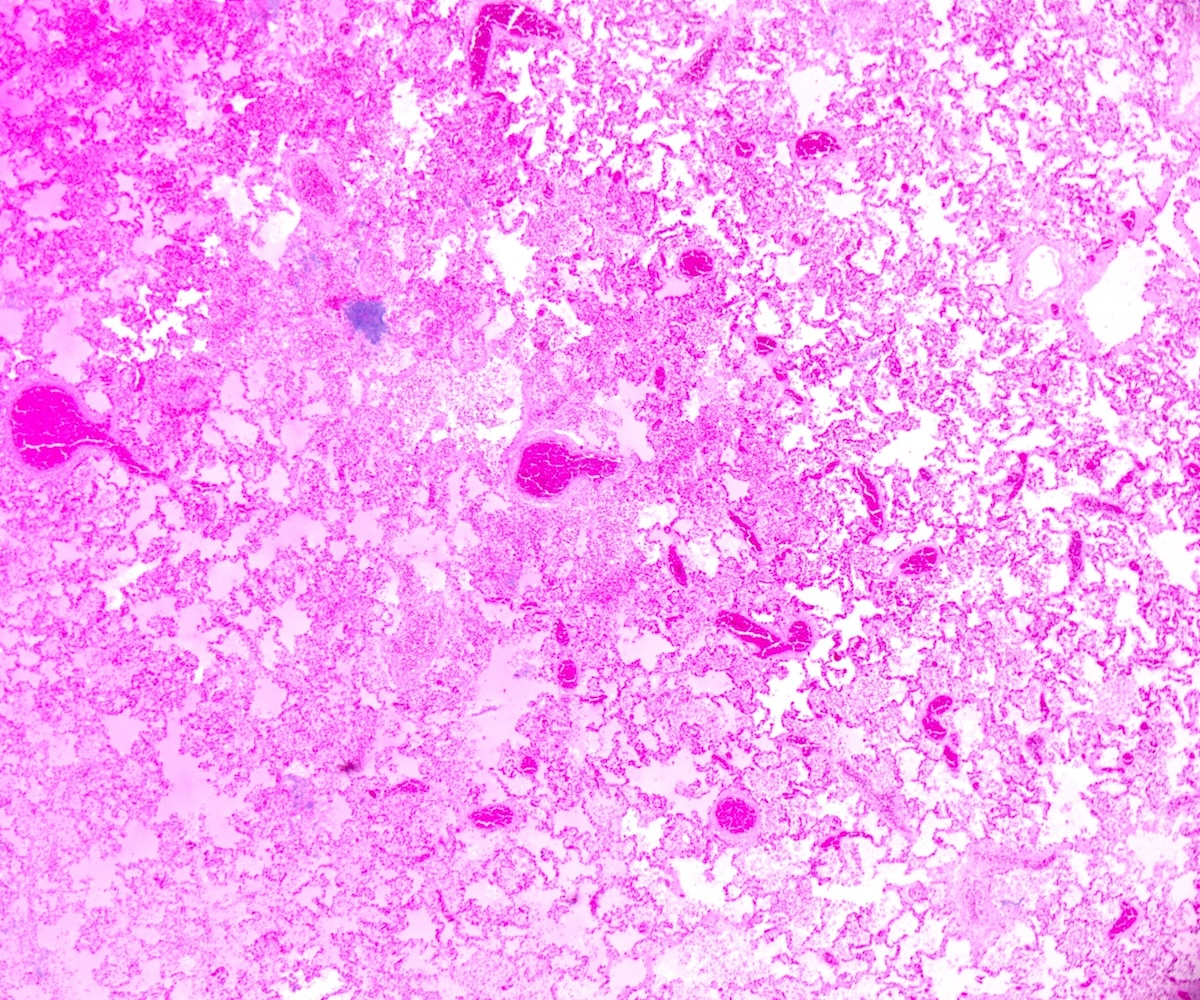
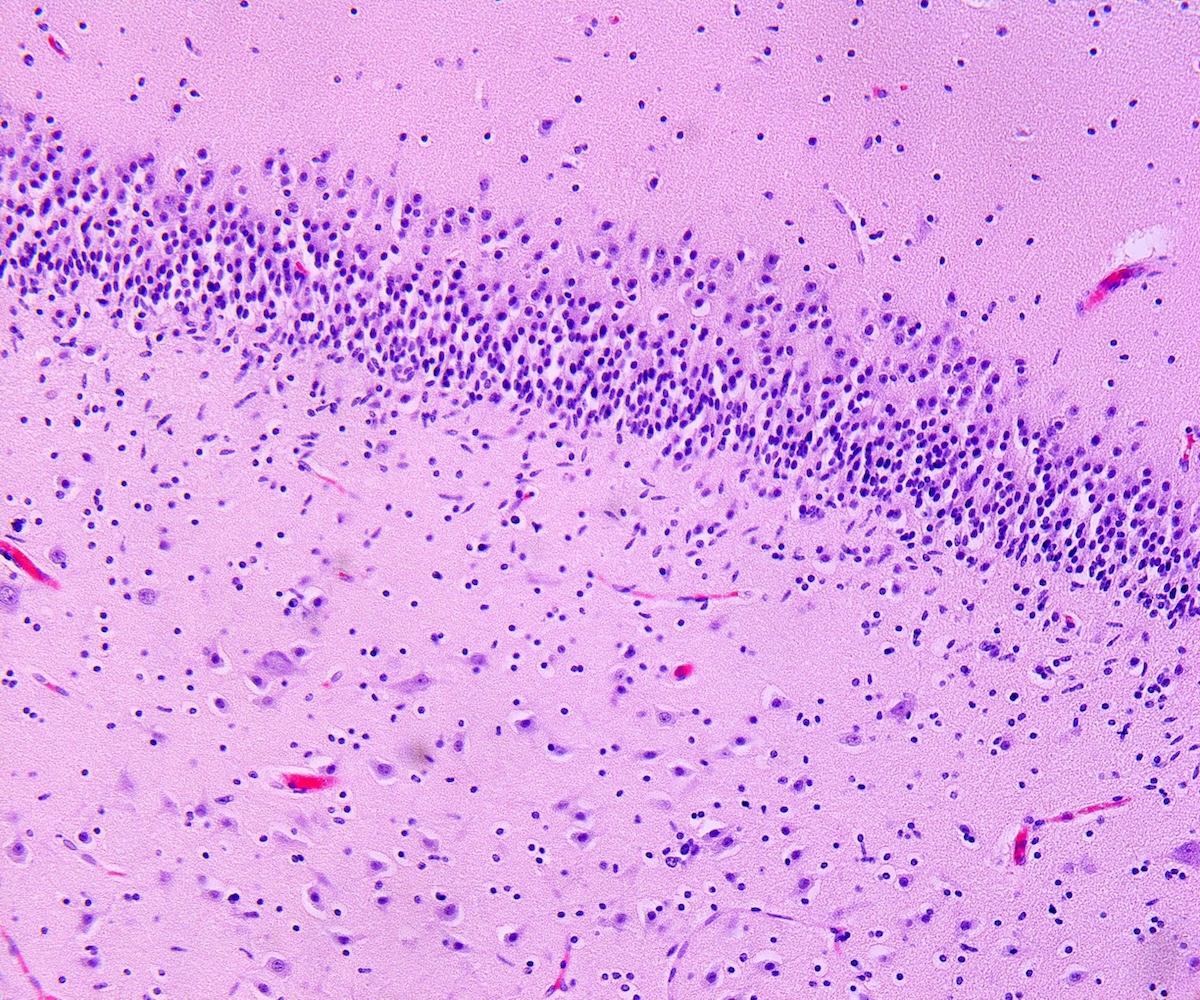
- Nonsignificant microscopic findings: intra-alveolar edema or hemorrhage, acute stress reaction on thymus, expansion of the mucosa associated lymphoid tissue (MALT) in lungs or abnormalities of the hippocampus (more frequent in SUDC and SUDEP than in SIDS) - focal granular cell dispersion, dentate bilamination and gliosis (Cohen: The Pediatric and Perinatal Autopsy Manual, 1st Edition, 2014, Forensic Sci Med Pathol 2020;16:423)
Microscopic (histologic) images
Practice question #1
Which of the following elements is common to sudden infant death syndrome (SIDS), sudden unexpected death in childhood (SUDC) and sudden unexpected death in epilepsy (SUDEP)?
- No cause of death is found
- Occurrence is higher in females
- These conditions share the same incidence
- They have a common etiology
Practice answer #1
A. No cause of death is found. Common to sudden infant death syndrome (SIDS), sudden unexpected death in childhood (SUDC) and sudden unexpected death in epilepsy (SUDEP) is that no cause of death is found after performing a thorough case investigation, including performance of a complete autopsy, examination of the death scene and a review of the clinical history. A complete autopsy includes ancillary investigations such as imaging (CT and Xrays), microbiology and virology from upper and lower airways, bowel content, cerebrospinal fluid (CSF) and any lesion, toxicology, biochemistry (urine) and genetic analysis.
Answer C is incorrect because the incidence is higher for SIDS (0.26 deaths per 1,000 live births in the United Kingdom) than SUDC (1 death per 100,000 children In the United Kingdom). SUDEP incidence is between 0.22 and 1.11 per 1,000 person years. Answer B is incorrect because 60 - 63% of SIDS victims are males. In 2021 in England and Wales, 0.33 deaths per 1,000 live births were males compared with 0.20 for female infants. Answer D is incorrect because although the cause of death in SIDS, SUDC or SUDEP is not known in a specific case, numerous etiologies have been implicated to present as a sudden death with no gross or histological abnormalities. Many of these have a genetic substrate (metabolic, arrhythmias, seizures, arousal failures) that interplay with environmental stressors (tobacco smoke, getting tangled in bedding, a minor illness or a breathing obstruction, sleeping position, hyperthermia, etc.).
Comment Here
Reference: Sudden unexpected deaths in infants and children
Answer C is incorrect because the incidence is higher for SIDS (0.26 deaths per 1,000 live births in the United Kingdom) than SUDC (1 death per 100,000 children In the United Kingdom). SUDEP incidence is between 0.22 and 1.11 per 1,000 person years. Answer B is incorrect because 60 - 63% of SIDS victims are males. In 2021 in England and Wales, 0.33 deaths per 1,000 live births were males compared with 0.20 for female infants. Answer D is incorrect because although the cause of death in SIDS, SUDC or SUDEP is not known in a specific case, numerous etiologies have been implicated to present as a sudden death with no gross or histological abnormalities. Many of these have a genetic substrate (metabolic, arrhythmias, seizures, arousal failures) that interplay with environmental stressors (tobacco smoke, getting tangled in bedding, a minor illness or a breathing obstruction, sleeping position, hyperthermia, etc.).
Comment Here
Reference: Sudden unexpected deaths in infants and children
Practice question #2
Which of the following is a known risk factor for sudden infant death syndrome (SIDS)?
- Cosleeping after alcohol consumption
- Non-Hispanic White racial group
- Recent immunization
- Term pregnancy
Practice answer #2
A. Cosleeping after alcohol consumption. Sharing the sleep surface with an adult is a known risk factor for sudden infant death syndrome (SIDS), especially when the adult smokes, has taken drugs or alcohol or is excessively tired and particularly when the sleeping surface is a sofa or settee (but also includes a bed). Answer D is incorrect because infants born preterm are at 4 times the risk of SIDS compared to infants born at term. Answer B is incorrect because the risk of SIDS varies by race and ethnicity, with Black / African American and American Indian / Alaska Native babies having a higher risk than White, Hispanic and Asian / Pacific Islander babies. Answer C is incorrect because there is no evidence that a recent immunization increases the risk of SIDS. In fact, some research suggests that being up to date on vaccinations may actually reduce the risk of SIDS.
Comment Here
Reference: Sudden unexpected deaths in infants and children
Comment Here
Reference: Sudden unexpected deaths in infants and children
Practice question #3
Practice answer #3
B. Expansion of the mucosa associated lymphoid tissue (MALT). The MALT is the accumulation of B and T lymphocytes in those structures lined by mucosa. Respiratory viral infections (commonly seen in SIDS cases) induce the expansion of the MALT associated with the bronchioles. Upper respiratory viral infections are regarded as a risk factor for SIDS. Answer A is incorrect because acute bronchopneumonia is a pattern of pulmonary infection with acute inflammation, characterized by the presence of patchy fibrinopurulent exudate with neutrophils and bacterial colonies. Answer C is incorrect because hyaline membranes are characterized by the presence of fibrinous membranes lining the alveoli inner walls. In BPD associated with prematurity, hyaline membranes are related to surfactant deficiency. BPD presents an arrest in alveolar development with reduced number of alveoli, alveolar simplification and variable fibrous thickening of alveolar septa and hyperplasia of type II pneumonocytes. Answer D is incorrect because expansion of MALT is a minor feature but not normal. It is usually associated with a respiratory viral infection.
Comment Here
Reference: Sudden unexpected deaths in infants and children
Comment Here
Reference: Sudden unexpected deaths in infants and children