Table of Contents
Definition / general | Epidemiology | Pathophysiology | Clinical features | Case reports | Treatment | Gross description | Gross images | Microscopic (histologic) description | Microscopic (histologic) images | Molecular / cytogenetics description | Electron microscopy description | Electron microscopy imagesCite this page: Ziadie MS. Nephronophthisis. PathologyOutlines.com website. https://www.pathologyoutlines.com/topic/kidneytumornephronophthisis.html. Accessed April 26th, 2024.
Definition / general
- Group of autosomal recessive disorders characterized by corticomedullary cysts, atrophy and interstitial fibrosis
- "Phthisis" (Greek): dwindling or wasting away
- Also referred to as juvenile nephronophthisis medullary cystic kidney disease complex
Epidemiology
- 1:50,000
- Most common genetic cause of pediatric end stage renal disease (ESRD)
Pathophysiology
- Mutations in NPHP genes (produce nephrocystins in cilia / basal body structures, (Eur J Hum Genet 2009;17:406, J Am Soc Nephrol 2007;18:1855), which cause defects in signaling mechanisms that result in defects of planar cell polarity and tissue maintenance (J Am Soc Nephrol 2009;20:23)
Clinical features
- Juvenile form: most common; presents in childhood with polyuria / polydipsia due to cortical and tubulointerstitial damage that progresses to chronic renal failure in 5 - 10 years; no gender preference; also anemia and growth retardation; 12% associated with retinitis pigmentosa
- Adolescent form: similar to juvenile with later (mean, 19 years) presentation
- Infantile: bilateral disease due to cortical cysts with renal failure by 3 years of age; may have extrarenal presentation including retinitis pigmentosa, hepatic fibrosis, skeletal / CNS malformations, situs inversus, etc.
Case reports
- 4 year old girl with basal ganglia calcification and pancreatic lipomatosis (Arch Pathol Lab Med 1988;112:630)
Treatment
- Renal transplant for ESRD (Pediatr Transplant 2008;12:878)
Gross description
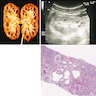
- Normal or small kidneys with firm, granular cortices and corticomedullary cysts
- Infantile forms have enlarged kidneys with cortical cysts
Gross images
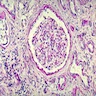
Microscopic (histologic) description
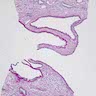
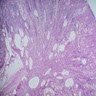
- Severe tubular atrophy with thick basement membranes, interstitial fibrosis and chronic inflammation
- Minimal to advanced glomerulosclerosis
- Cysts at corticomedullary border lined by flattened or cuboidal epithelium
- Liver biopsy may show congenital hepatic fibrosis
Microscopic (histologic) images
Molecular / cytogenetics description
- Mutations in NPHP2 and NPHP3 genes (Kidney Int 2009;75:839), also associated with retinitis pigmentosa, intellectual disability, cerebellar ataxia, bone anomalies and liver fibrosis
- Juvenile subtype associated with mutations in NPHP1 (OMIM 256100) (chromosome 2q), 4 (chromosome 1p)
- Infantile subtype associated with NPHP2 (chromosome 9q)
- Adolescent subtype associated with NPHP3 (chromosome 3q)
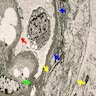
Electron microscopy description
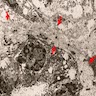
- Homogenously thickened tubular (NOT glomerular) basement membrane, split into thin lamellae, reticulated or disintegrated
Electron microscopy images
Images hosted on other servers:
Tubules:
Glomeruli: