Table of Contents
Definition / general | Essential features | Terminology | ICD coding | Epidemiology | Sites | Pathophysiology | Etiology | Clinical features | Diagnosis | Laboratory | Radiology description | Radiology images | Case reports | Treatment | Clinical images | Microscopic (histologic) description | Microscopic (histologic) images | Molecular / cytogenetics description | Sample pathology report | Differential diagnosis | Additional references | Practice question #1 | Practice answer #1 | Practice question #2 | Practice answer #2Cite this page: Franklin M, Somach S. Hidradenitis suppurativa. PathologyOutlines.com website. https://www.pathologyoutlines.com/topic/skinnontumorhidradenitis.html. Accessed October 5th, 2025.
Definition / general
- Chronic inflammatory disorder of pilosebaceous apocrine unit characterized by nodules, abscesses, fistulae and sinus tracts, with scarring
- Most commonly affects the axillae and groin, among other areas of young adults
Essential features
- Inflammatory disorder of terminal hair bearing skin, most commonly in the axillae and groin, manifesting with nodules, open comedones and draining sinuses with prominent scarring
- Risk factors include female sex, obesity, smoking and family history
- Associated with metabolic syndrome, adverse cardiovascular events and other inflammatory disorders, e.g. psoriasis
- Follicular occlusion is the first step in pathogenesis, followed by epithelial rupture with ensuing inflammation, foreign body reaction, occasionally apocrine involvement and bacterial colonization
- Effective treatment (may involve antibiotics, biologic or surgical measures) is often challenging
Terminology
- Acne inversa
- Verneuil disease
- Note that hidradenitis suppurativa has been described as a misnomer (Int J Dermatol 2005;44:535)
Epidemiology
- Estimated prevalence between 0.00033% and 4.10% (Exp Dermatol 2019;28:769)
- Prevalence in U.S. population recently estimated to be 0.10% (JAMA Dermatol 2017;153:760)
- More than twice as common in women
- Highest among patients aged 30 - 39 years
- Prevalence is more than 3 times greater in African American patients than Caucasian patients
- Onset before 11 years of age estimated to account for 2% of cases (Pediatr Dermatol 1999;16:292)
Sites
- Axillae, inguinal area, inframammary folds, perineum, buttocks, mons pubis, scalp, postauricular area, back (J Cutan Med Surg 2016;20:52, Dermatology 2015;231:184)
- Predilection for apocrine gland bearing areas (Exp Dermatol 2010;19:533)
Pathophysiology
- Historically, the inflammation was thought to originate in the apocrine gland (Br J Dermatol 1990;122:763)
- More recent evidence suggests that follicular occlusion is the primary inciting event (J Am Acad Dermatol 2015;73:S8)
- Occlusion of the follicle is caused by infundibular hyperkeratosis and hyperplasia of the follicular epithelium (Exp Dermatol 2010;19:533)
- Subsequent accumulation of cellular debris, leading to cyst formation (Exp Dermatol 2010;19:533)
- Eventual follicular rupture is met with local immune response and subsequent sinus tract formation (Exp Dermatol 2010;19:533)
- Not a result of inflammation in the apocrine sweat glands or infection (Br J Dermatol 1990;122:763)
- Sebaceous gland volume is reduced but unclear if this has a primary or secondary role in pathogenesis (Br J Dermatol 2011;164:1017)
- Elevated levels of TNF alpha, IL1β, IL10 and IL36 cytokines, as well as Th17 cytokines (e.g. IL17, GM-CSF, IL22, TNF alpha and IFN gamma) (Br J Dermatol 2011;164:1292, Arch Dermatol Res 2017;309:673, J Invest Dermatol 2017;137:2389)
- High Th17 to regulator T cell ratio in lesional HS skin (J Invest Dermatol 2017;137:2389)
- Decreased levels of anti-inflammatory adiponectin (Br J Dermatol 2018;178:792)
- Upregulation of Toll-like receptors, NOD-like receptor protein 3 (NLRP3) inflammasome activity and matrix metalloproteinases (Inflamm Res 2017;66:931)
- Androgens may have deleterious role (J Clin Aesthet Dermatol 2016;9:44)
- Disturbances in cutaneous microbiome and biofilm production may play a role (Br J Dermatol 2017;176:993, JAMA Dermatol 2017;153:897, J Am Acad Dermatol 2015;73:S12)
- Microbiome profiles of lesional skin may have greater proportions of Corynebacterium, Porphyromonas and Peptoniphilus species, as compared with healthy controls (JAMA Dermatol 2017;153:897)
- Propionibacterium more abundant in healthy controls' skin than lesional HS skin (JAMA Dermatol 2017;153:897)
Etiology
- Cause unknown (see Pathophysiology and Clinical features)
Clinical features
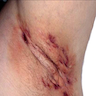
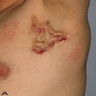
- Characteristic lesions are deep seated painful nodules that expand to form abscesses, which may subsequently rupture and drain (Semin Cutan Med Surg 2017;36:42)
- Draining sinuses, sinus tracts and open comedones with eventual scarring (G Ital Dermatol Venereol 2017;152:46)
- Heat, sweating, physical activity, shaving and friction may exacerbate symptoms (F1000Res 2017;6:1272)
- Alternating between exacerbations and quiescence is typical (G Ital Dermatol Venereol 2017;152:46)
- Axillae, inguinal area, perineum, buttocks and mons pubis most commonly affected but other sites, e.g. scalp, may be affected as well (Semin Cutan Med Surg 2017;36:42, Dermatology 2015;231:184)
- Numerous associations, including obesity, hypertension, thyroid disease, dyslipidemia, psychiatric disease and type VI pityriasis rubra pilaris associated follicular occlusion disease (J Am Acad Dermatol 2014;71:1144, Clin Exp Dermatol 2004;29:480)
- Significant adverse impact on quality of life (J Eur Acad Dermatol Venereol 2018;32:467)
- Increased risk of major adverse cardiovascular events, including myocardial infarction and stroke, as well as all-cause mortality (JAMA Dermatol 2016;152:429)
- Strong association with smoking, i.e. 70 - 90% of HS patients smoke (Br J Dermatol 2018;178:587)
- Odds of developing HS among smokers compared with nonsmokers was 1.9 in one study (Br J Dermatol 2018;178:709)
- Associated with inflammatory disorders, e.g. psoriasis, Crohn's disease, inflammatory arthritis (J Am Acad Dermatol 2018 Nov 28 [Epub ahead of print], Int J Dermatol 2018;57:547, J Rheumatol 2014;41:490)
- A component of several autoinflammatory syndromes, including PASH (pyoderma gangrenosum, acne and hidradenitis suppurativa) and PAPASH (pyoderma gangrenosum, acne, pyogenic arthritis and hidradenitis suppurativa) (Int J Dermatol 2017;56:811)
- Overlap, both in clinical appearance and in pathogenesis, with other follicular occlusion tetrad diseases: acne conglobata, dissecting cellulitis and pilonidal cyst (Indian Dermatol Online J 2014;5:491)
Diagnosis
- 3 criteria for diagnosis: characteristic lesions, predilection for flexural sites and lesion recurrence (Australas J Dermatol 2018;59:267)
- Hurley 3 tiered staging system used to describe disease severity and help select treatment (J Eur Acad Dermatol Venereol 2015;29:619)
- Newer systems (e.g. Sartorius, HSSI, HiSCR) designed to quantify disease intensity and response to treatment (Br J Dermatol 2003;149:211, Int J Dermatol 2010;49:950, Br J Dermatol 2014;171:1434)
- Frequent delay in diagnosis (Br J Dermatol 2015;173:1546)
- Ultrasound may aid in assessment of disease severity (Dermatol Surg 2013;39:1835, Ital J Dermatol Venerol 2021;156:235)
Laboratory
- Decreased ferritin, transferrin saturation and hepcidin (Dermatology 2020;236:52)
- Consider screening for glucose intolerance, hypertension and dyslipidemia (J Eur Acad Dermatol Venereol 2017;31:e411)
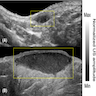
Radiology description
- Ultrasound (Skin Res Technol 2020;26:11)
- Thickened dermis
- Widened hair follicles
- Tracts
- Hypoechoic fluid pockets
- Decreased surrounding tissue echogenicity
- Abscess
Case reports
- 14 year old boy with hidradenitis treated with silver coated textiles (SAGE Open Med Case Rep 2019;7:2050313X19845212)
- 22 year old man with Smith-Magenis syndrome develops hidradenitis (Cureus 2019;11:e4970)
- 33 year old man on sorafenib for papillary thyroid cancer develops hidradenitis (Dermatol Online J 2019;25:13030/qt1s2016td)
- 40 year old woman with severe hidradenitis as a result of ascending infection has a miscarriage (Int J Womens Health 2020;12:939)
- 64 year old man develops squamous cell carcinoma within lesion of hidradenitis (SAGE Open Med Case Rep 2019;7:2050313X19847359)
Treatment
- Lifestyle modification
- Weight loss (Acta Derm Venereol 2014;94:553)
- Smoking cessation (Br J Dermatol 2018;178:709)
- Topical and systemic antibiotics (Dermatol Clin 2016;34:81)
- Topical clindamycin (J Am Acad Dermatol 1998;39:971)
- Oral rifampin and clindamycin combination (Ann Chir Plast Esthet 2017;62:274)
- Tetracyclines (J Am Acad Dermatol 1998;39:971)
- Rifampin, moxifloxacin and metronidazole combination (Ann Chir Plast Esthet 2017;62:274)
- Broad spectrum combination treatment may be best option to limit antibacterial resistance (Ann Chir Plast Esthet 2017;62:274)
- Biologics
- TNF alpha inhibitors (J Dermatolog Treat 2018;29:441, Ann Intern Med 2012;157:846)
- IL17 inhibitors (Immunotherapy 2019;11:45)
- IL12 / 23 inhibitors (Immunotherapy 2019;11:45)
- IL1 inhibitors (J Dermatolog Treat 2018;29:441)
- Hormonal agents
- Estrogen / progesterone combination pills (Br J Dermatol 1986;115:263)
- Finasteride (J Clin Aesthet Dermatol 2016;9:44)
- Spironolactone (Australas J Dermatol 2015;56:192)
- Systemic retinoids (Dermatology 2017;233:120)
- Metformin (J Eur Acad Dermatol Venereol 2013;27:1101)
- Liraglutide (Br J Dermatol 2017;177:858)
- Zinc gluconate (Br J Dermatol 2020;183:e178)
- Low dose systemic corticosteroids (J Am Acad Dermatol 2016;75:1059)
- Intralesional corticosteroids (Int J Rheumatol 2017;2017:8018192)
- May not be more effective than placebo (saline) (Dermatol Surg 2020;46:685)
- Surgical interventions
- Deroofing (F1000Res 2017;6:1272)
- Incision and drainage (Dermatol Clin 2016;34:97)
- Excision (J Eur Acad Dermatol Venereol 2018;32:459)
- Laser (J Plast Reconstr Aesthet Surg 2016;69:1374)
Microscopic (histologic) description
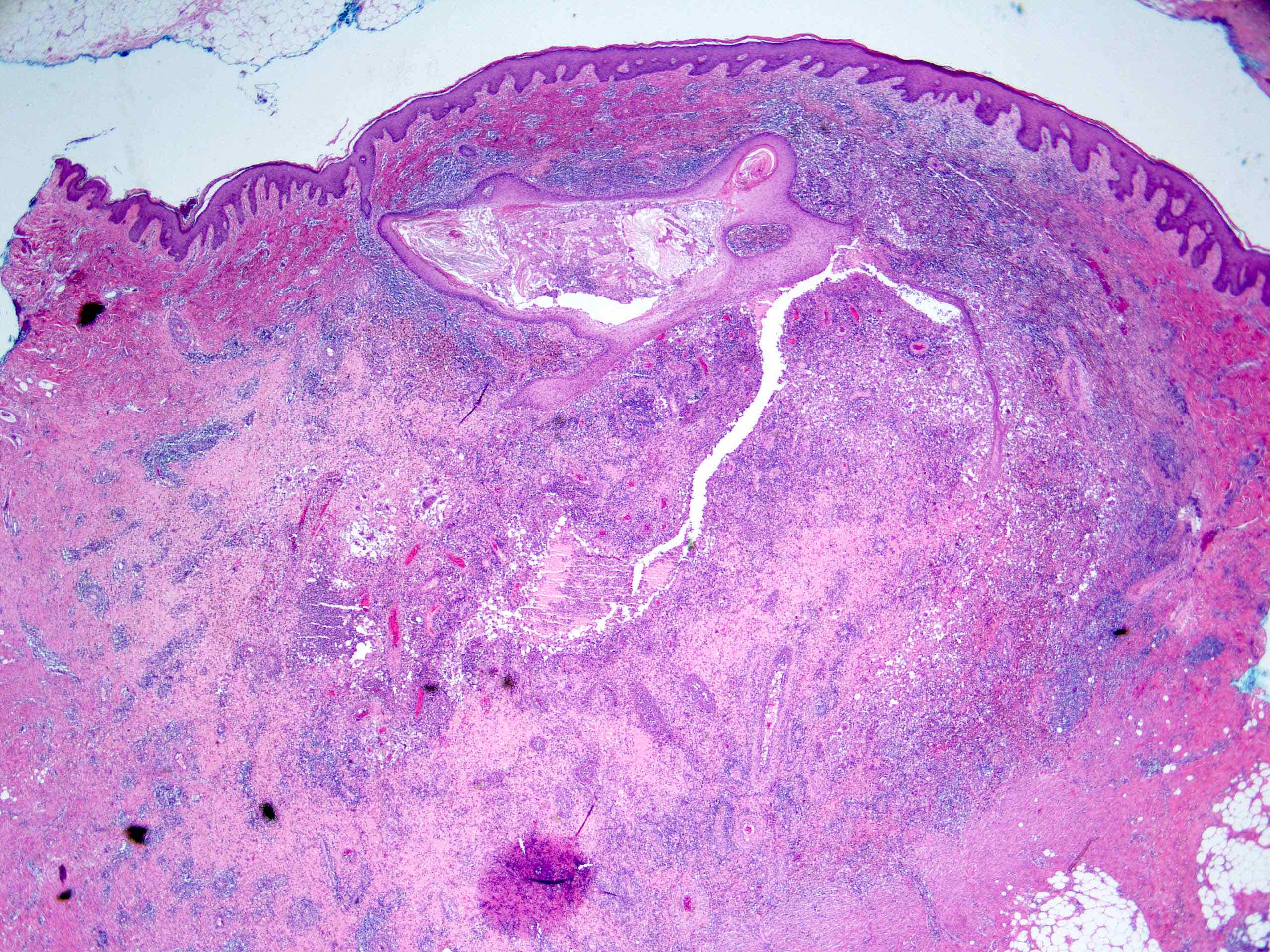
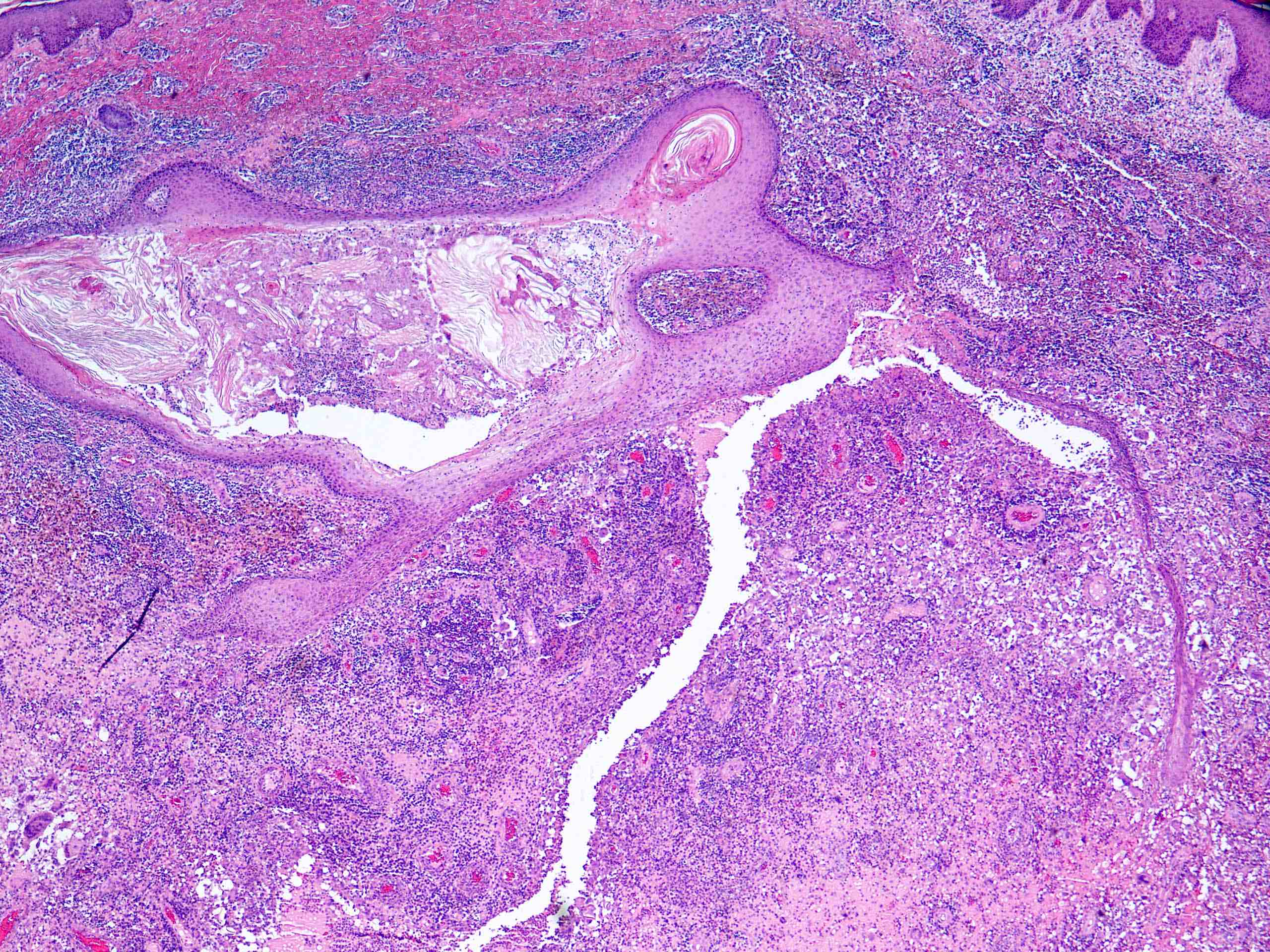
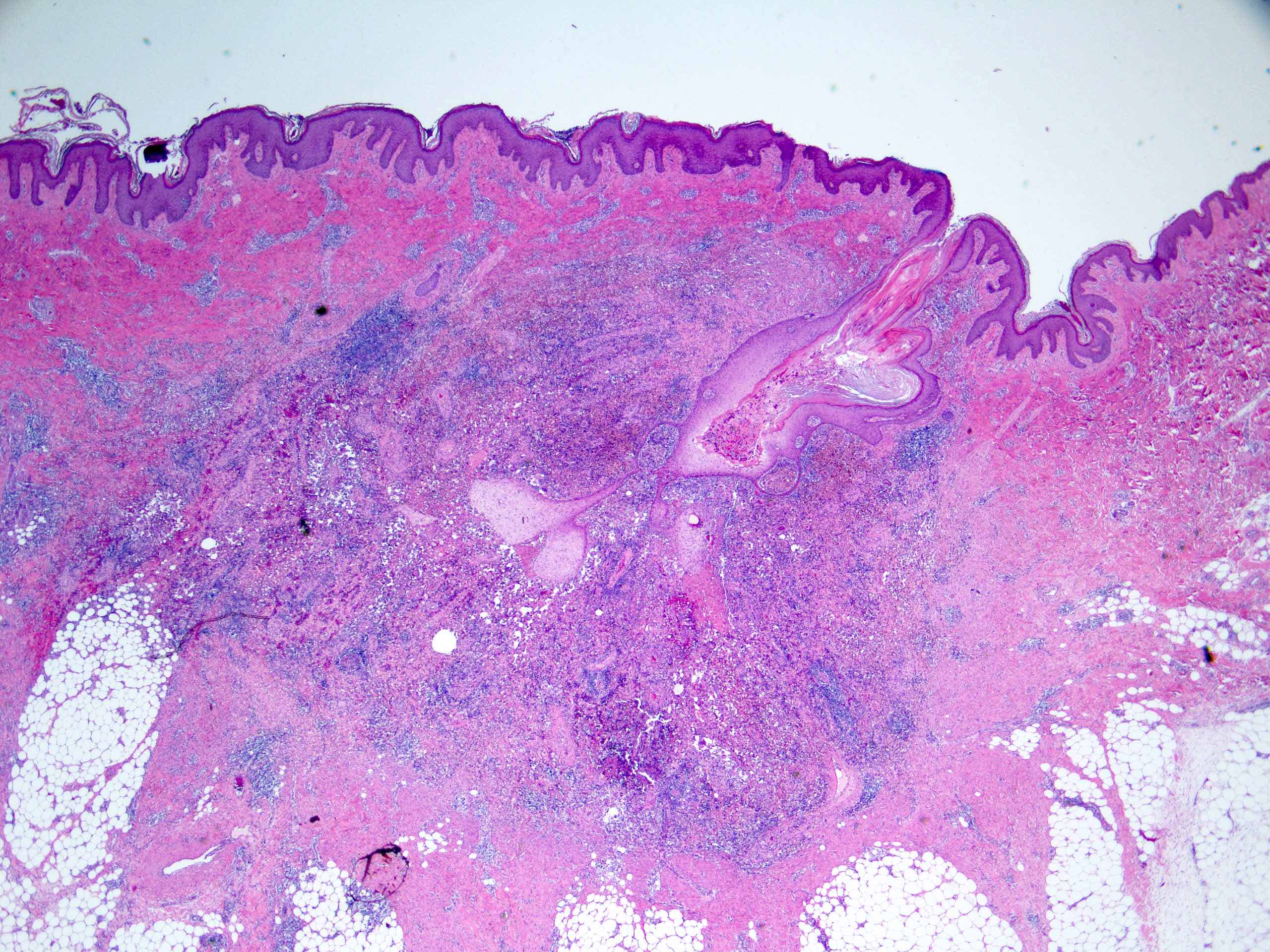
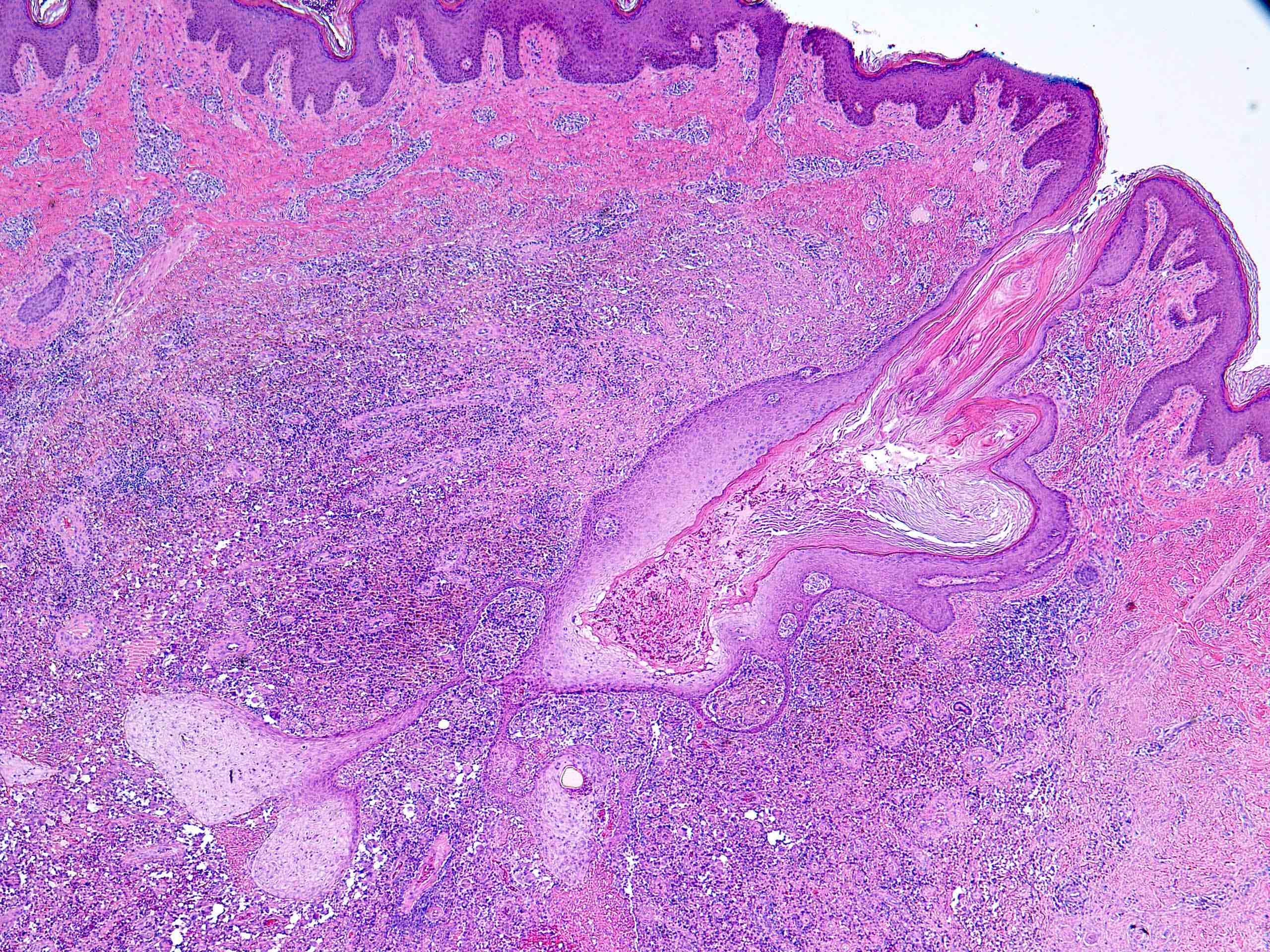
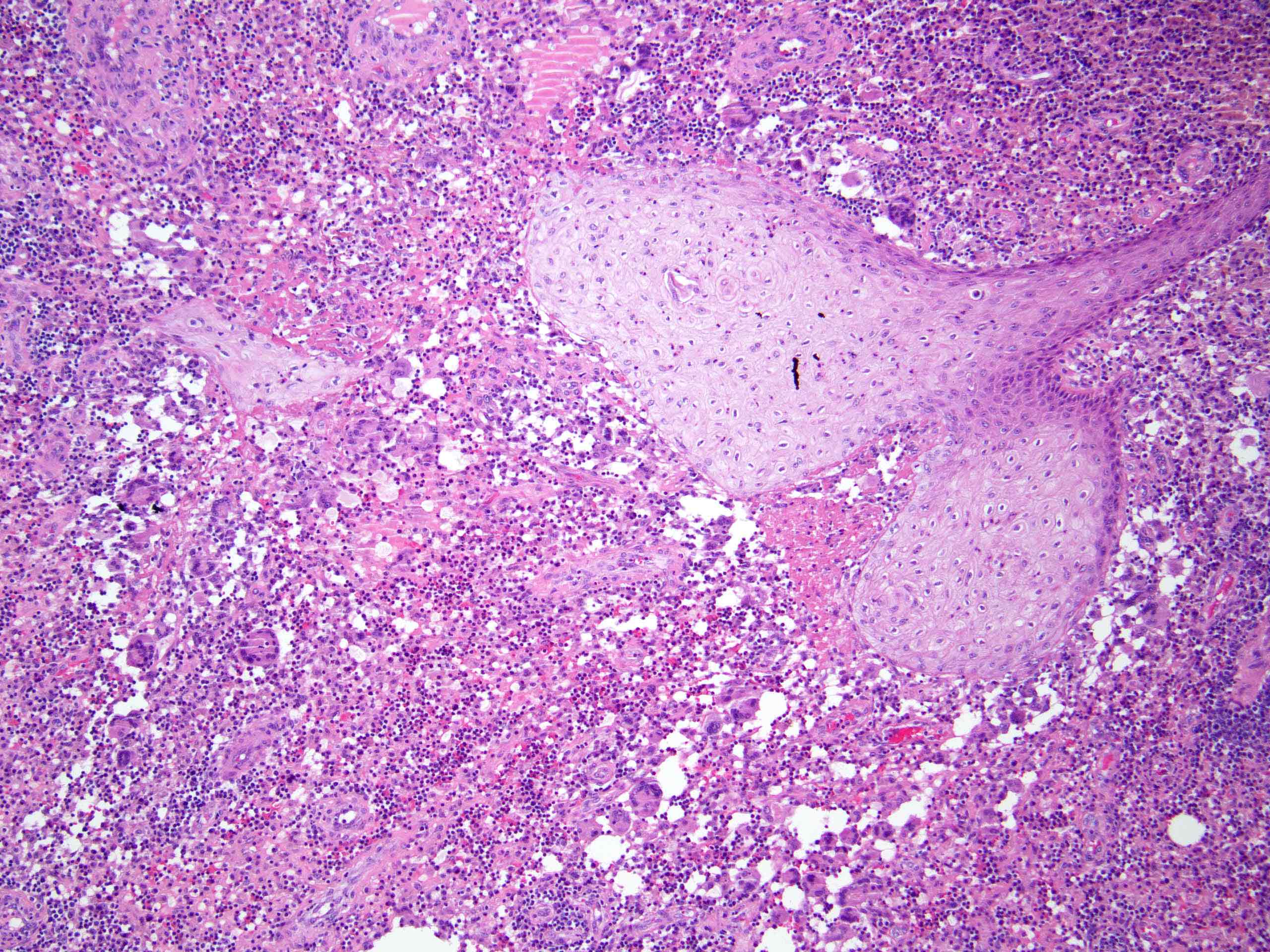
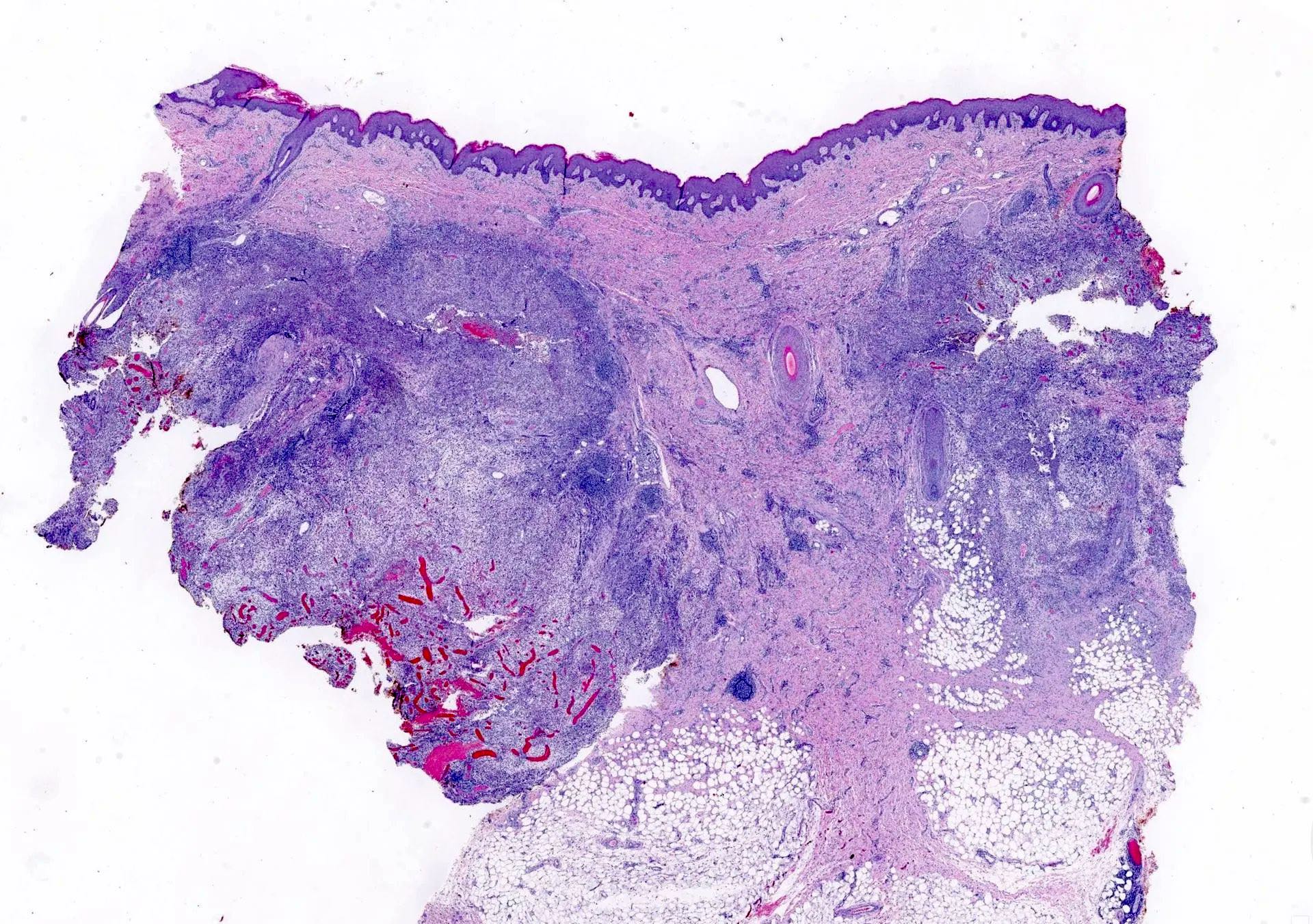
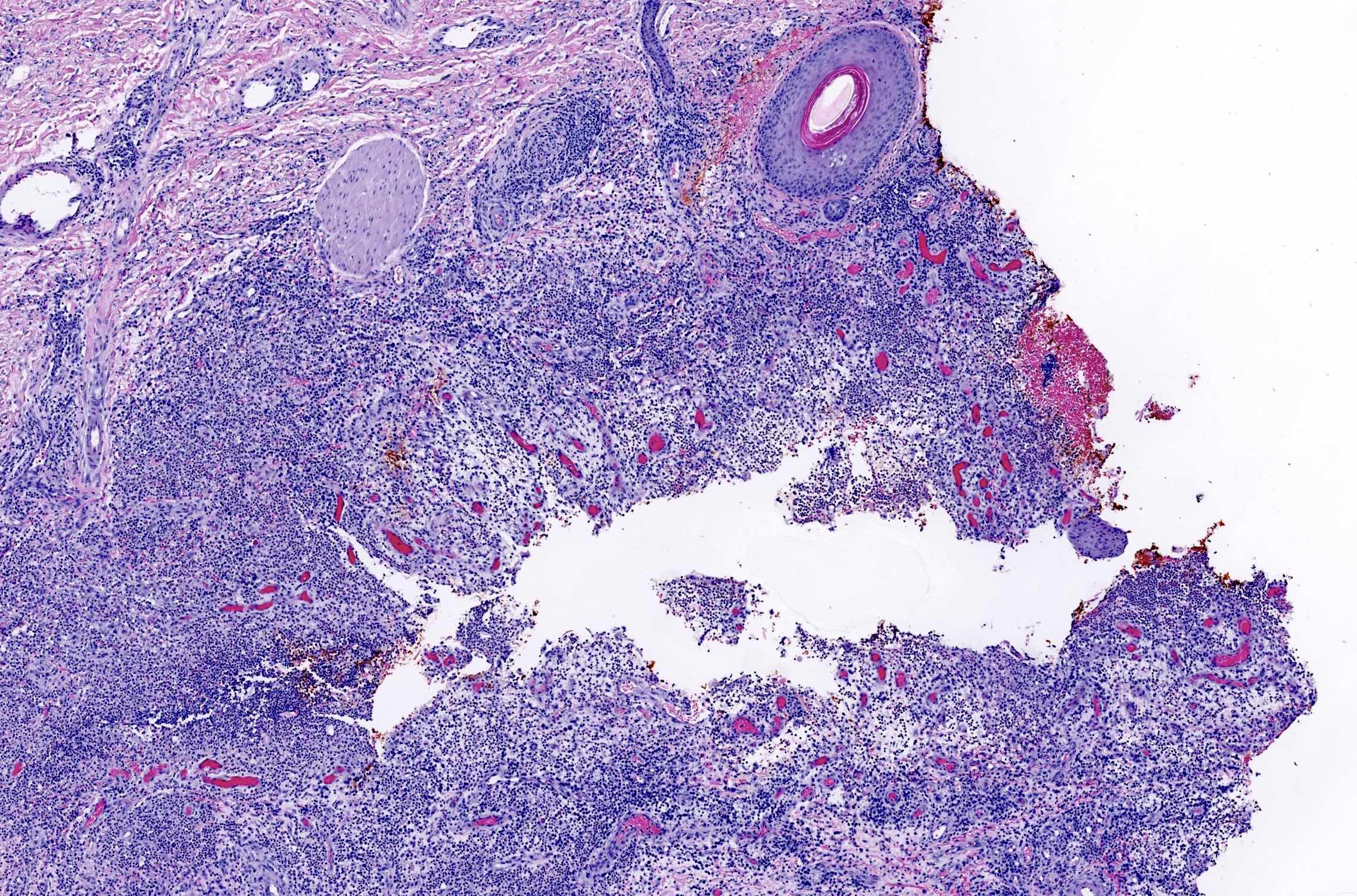
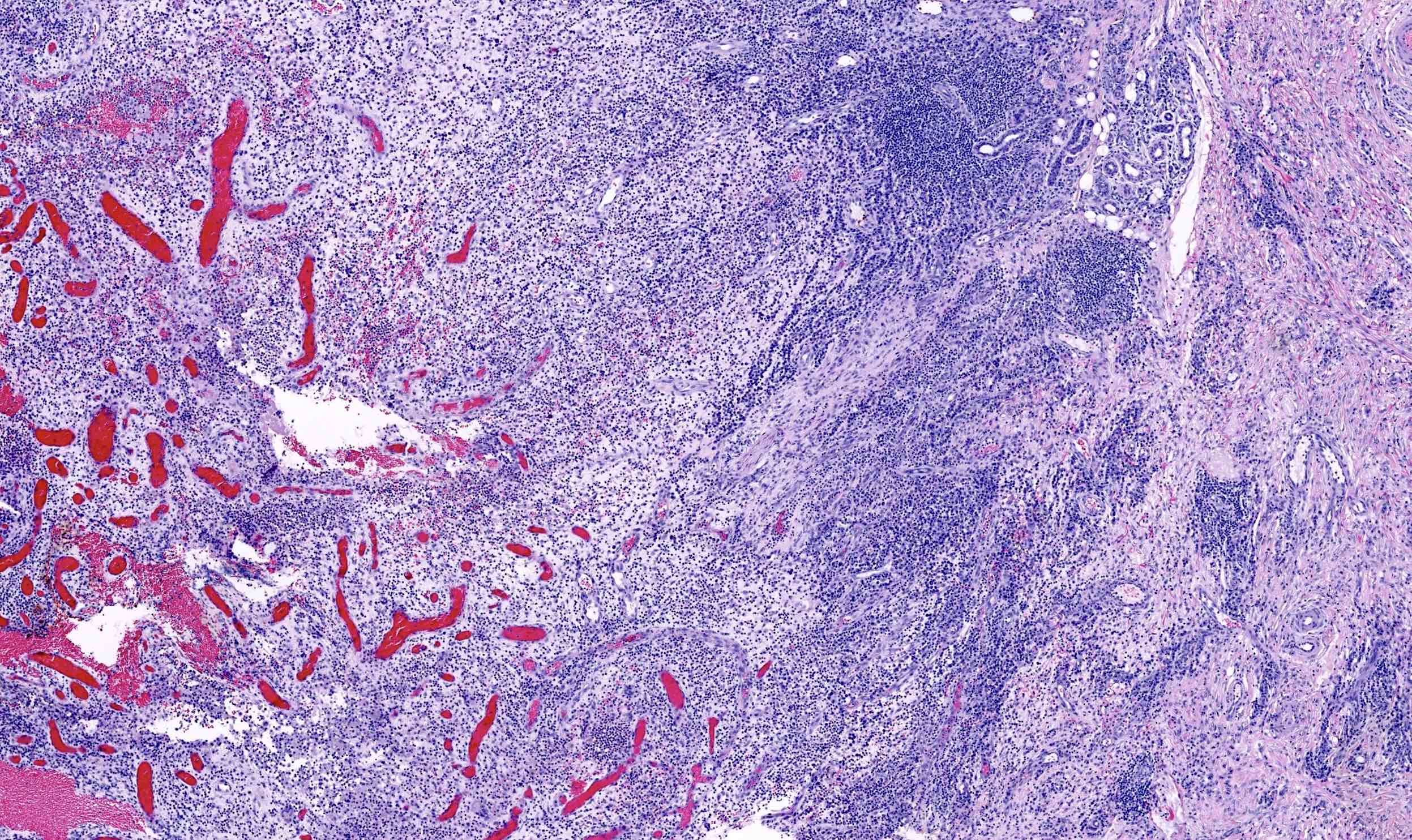
- In early lesions: follicular hyperkeratosis, hyperplasia of follicular epithelium and perifolliculitis (Br J Dermatol 2011;164:367)
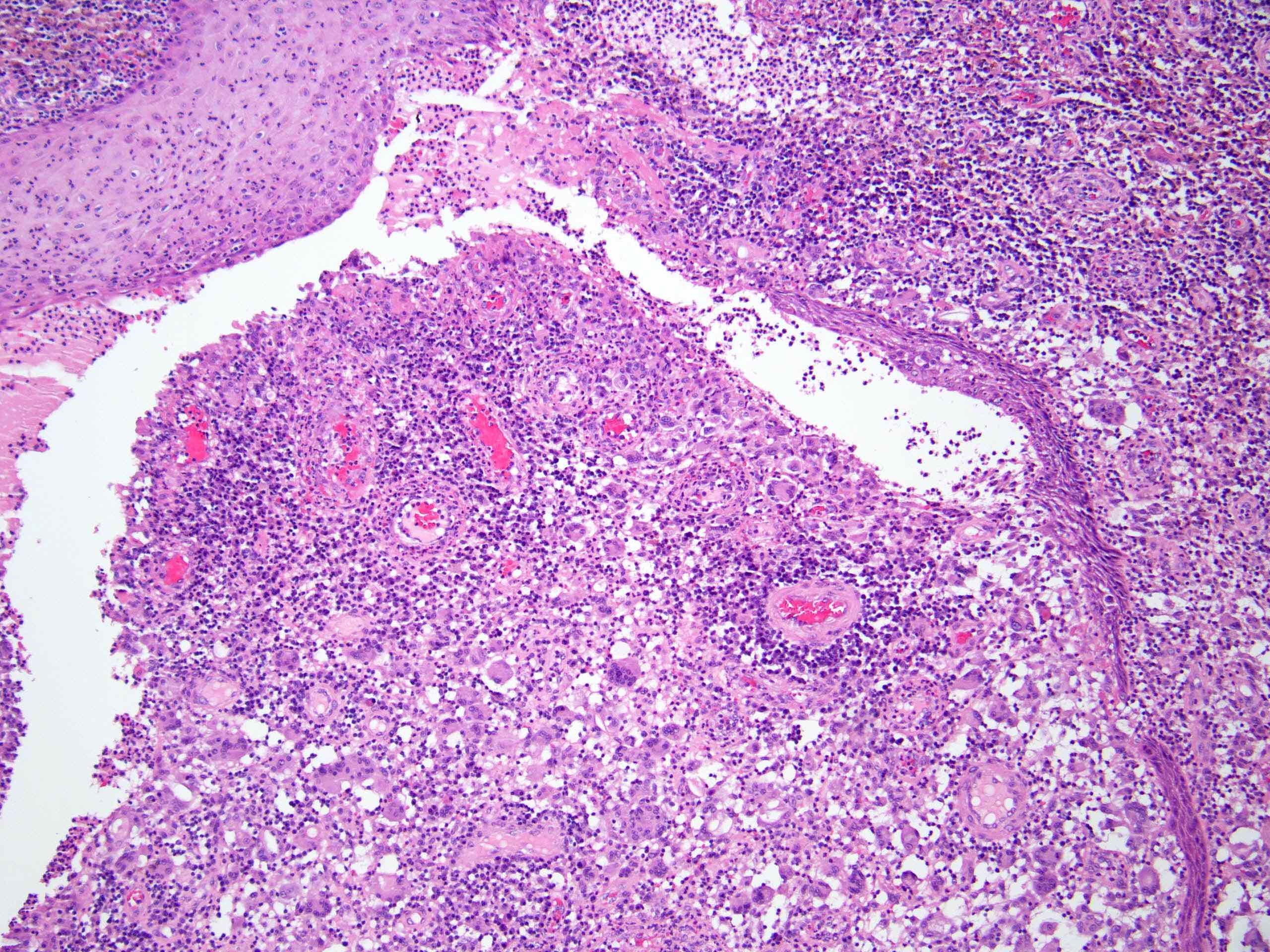
- Dermal mixed inflammatory cell infiltrate, sometimes extending into the subcutis (Br J Dermatol 1990;122:763)
- Neutrophilic abscesses, which may connect with squamous epithelium lined cysts and sinus tracts that extend to the skin surface (Br J Dermatol 1990;122:763)
- Cysts and sinus tracts contain laminated keratin and occasional hair follicles (Br J Dermatol 1990;122:763)
- Granulation tissue with occasional foreign body giant cells present in ~25% of cases (Histopathology 1993;23:111)
- Inflammation involves apocrine glands in a minority of cases (J Am Acad Dermatol 1996;34:994)
- Dense fibrosis surrounding areas of follicular rupture
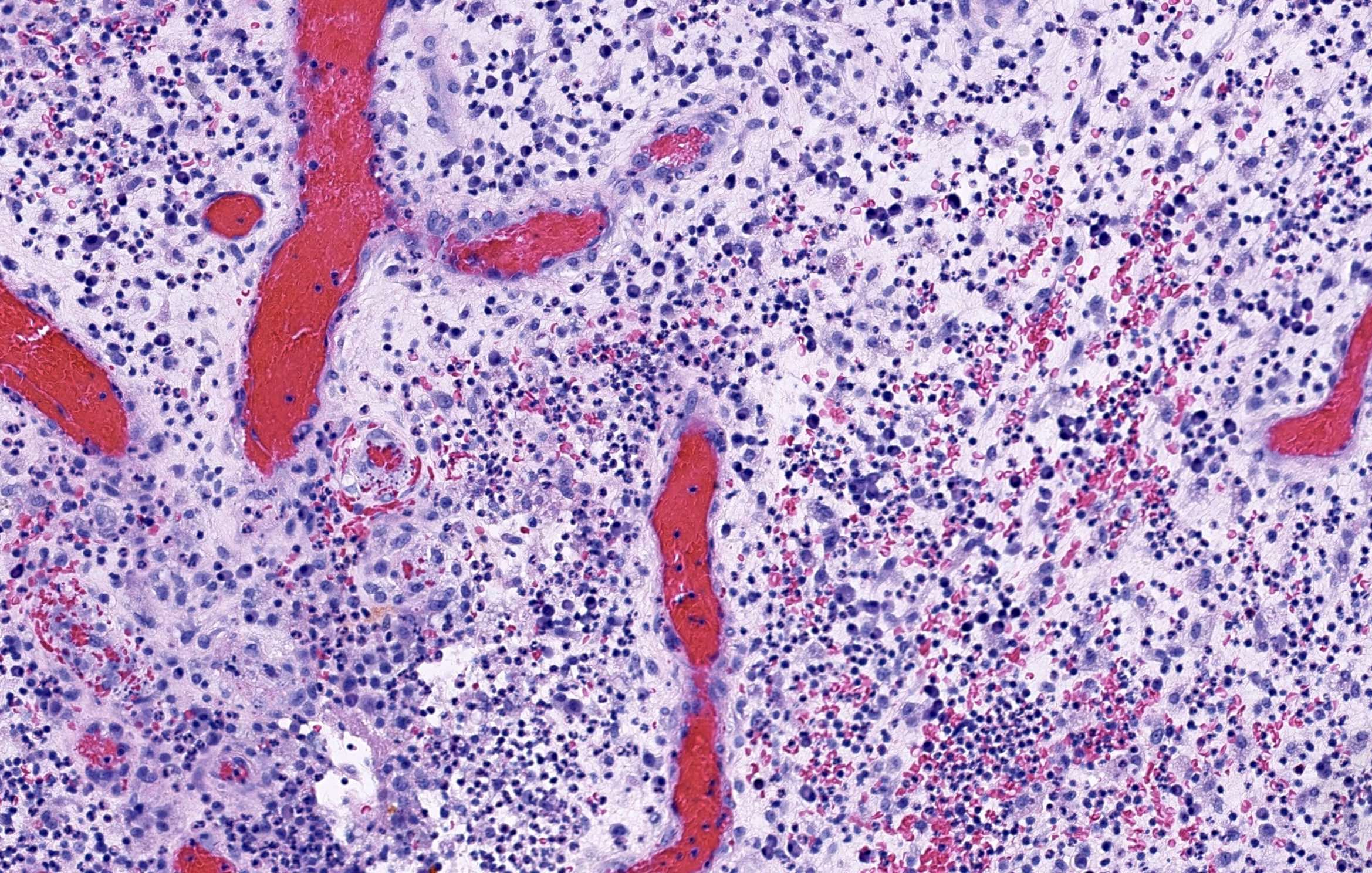
Microscopic (histologic) images
Molecular / cytogenetics description
- Loss of function mutations of 3 genes, NCSTN, PSENEN and PSEN1, which are components of the gamma secretase multiprotein complex (Science 2010;330:1065)
- Upregulation of several cytokines, including tumor necrosis factor alpha, IL17 and IL23 (Front Immunol 2018;9:2965)
- Decreased levels of Drosha and DGRC8 miRNA (J Dermatol Sci 2016;82:166)
- Single nucleotide polymorphisms in tumor necrosis factor gene promoter (Br J Dermatol 2013;168:311)
Sample pathology report
- Right proximal thigh, excision:
- Dermal epithelial lined sinus tract with cyst rupture and surrounding acute and chronic inflammation, consistent with hidradenitis suppurativa
Differential diagnosis
- Other entities within the follicular occlusion tetrad (acne conglobata, pilonidal cyst and dissecting cellulitis) have similar histopathology
- Clinicopathologic correlation, especially with anatomic site, is necessary
- Ruptured follicular cyst / folliculitis:
- Similar histopathology, except dissecting tracts would not be expected
- Soft tissue infection:
- Special stains for microorganisms, as well as tissue cultures, help to exclude this possibility
Additional references
Practice question #1
A 25 year old woman with diabetes presents for draining boils in her axillae and groin. Abnormalities in which of the following cutaneous structures is thought to initiate the pathogenic cascade leading to the inflammatory sequelae of this disease?
- Apocrine glands
- Arrector pili muscle
- Eccrine glands
- Infundibular follicular epithelium
- Sebaceous glands
Practice answer #1
Practice question #2
Which of these is a risk factor for the development of hidradenitis suppurativa?
- Alcohol consumption
- Low BMI
- Male sex
- Smoking
Practice answer #2