All cases are archived on our website. To view them sorted by case number, diagnosis or category, visit our main Case of the Month page. To subscribe or unsubscribe to Case of the Month or our other email lists, click here.
Thanks to Dr. Zlatko Marusic, Sestre Milosrdnice Clinical Hospital (Croatia), for contributing this case.
Orchard Pathology is an all-inclusive CP/AP diagnostic information system designed to accommodate the complex workflow and reporting of clinical, cytology, anatomic and molecular testing.
Orchard Pathology is used for AP only or as a single system that includes clinical and molecularno more need for 2 separate systems. The shared database provides access to the patients history and enables the consolidation of clinical results to the pathology report. Unlike legacy text-based AP systems, Orchard Pathology stores report information in structured data fields that enhance EMR integration and simplify data mining for evaluations; correlation studies; quality assurance; and other management reports.
Visit us at
http://www.OrchardSoft.com.
(1) We have updated the Molecular Pathology chapter with a section on DNA sequencing written by Rodney E. Shackelford, D.O., Ph.D., Tulane University, Louisiana.
(2) We have extensively updated the CD Markers CD1-CD49 chapter, which now has 68 topics, 479 images and 1092 references.
(3) For a "printer friendly page" of any part of our website, we recommend visiting http://www.printfriendly.com, which has options to print with or without images. As this works better than our "printer friendly" versions of chapters, we will remove the printer friendly versions as we update chapters.
Visit and follow our Blog to see recent updates to the website.
Case #198
Clinical history:
A 55 year old woman presented with hematuria. A bladder biopsy was obtained.
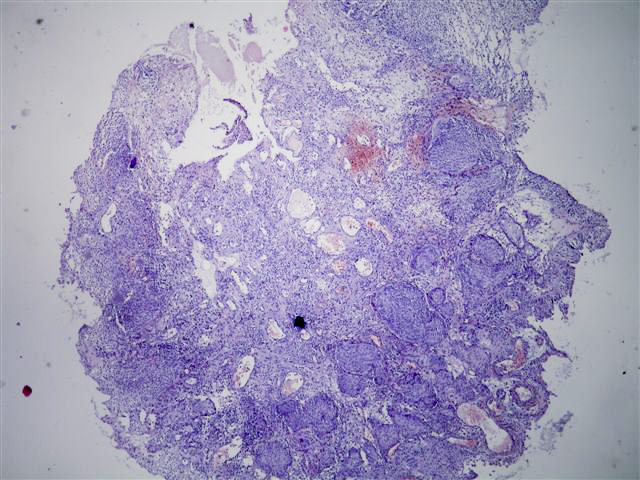
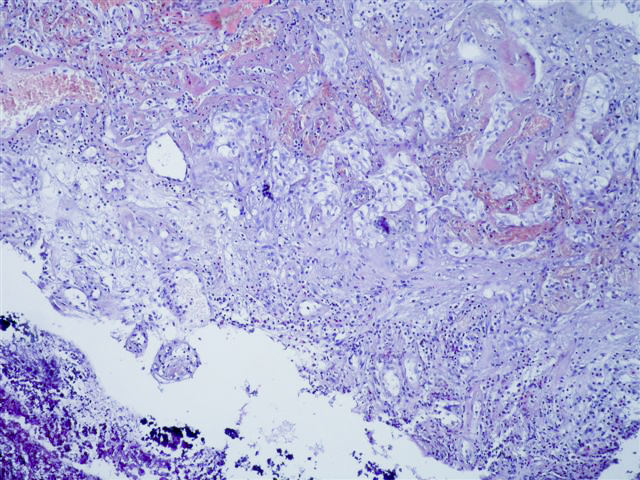
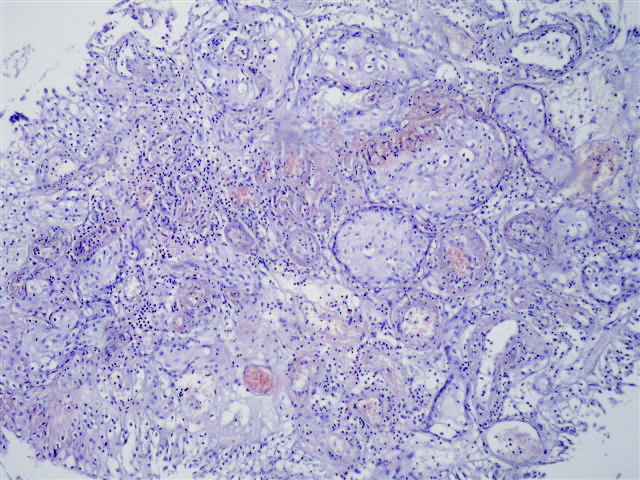
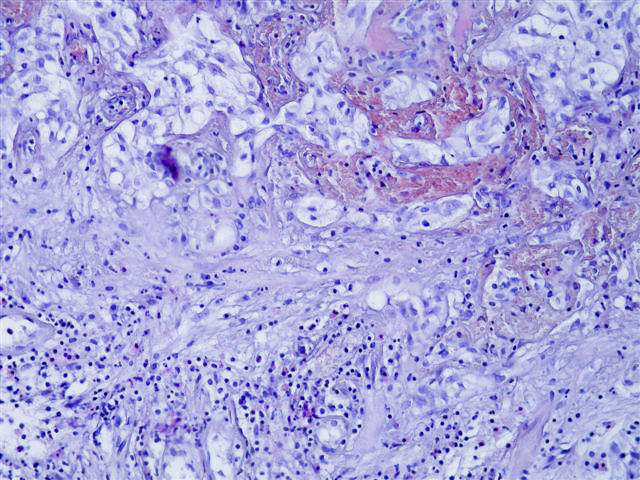
Microscopic images:
What is your diagnosis?
Diagnosis: Pseudocarcinomatous epithelial hyperplasia of the urinary bladder
Discussion:
There is a characteristic downward proliferation of urothelial nests with focal squamous metaplasia but without atypia. The nests wrap around vessels with fibrin deposition and congestion. One of the photomicrographs shows calcifications next to the biopsy fragment.
In 2000, Baker and Young reported 4 cases of radiation cystitis with pseudocarcinomatous proliferations, which were often confused with invasive carcinoma (Hum Pathol 2000;31:678). 2 subsequent case series describe this entity. The first series, by Chan and Epstein (Am J Surg Pathol 2004;28:909), reported on 20 patients with similar biopsy features and a history of pelvic irradiation or systemic chemotherapy. The second case series, by Lane and Epstein, described 8 patients with ischemia or chronic irritation but no history of irradiation (Am J Surg Pathol 2008;32:92). Pseudocarcinomatous epithelial hyperplasia of the urinary bladder has also been described in reviews of pseudoneoplastic or therapy induced lesions of the urinary bladder (Mod Pathol 2009;22:S37).
In the present case, a pathologist search for prior biopsies revealed a history of radation therapy for uterine cancer 3 years previous.
Despite the pseudoinvasive nests, these lesions have characteristic findings that differentiate these cases from invasive carcinoma. Most cases show no mitotic figures but there is frequently hemorrhage, thickened vessels and other radiation associated vascular changes. Other features include fibrin deposition, fibrin thrombi, fibrosis, inflammation, hemosiderin, ulceration, edema and vascular congestion.
No treatment is required for this reactive condition.