Table of Contents
Definition / general | Essential features | ICD coding | Epidemiology | Pathophysiology | Clinical features | Laboratory | Prognostic factors | Case reports | Treatment | Microscopic (histologic) description | Microscopic (histologic) images | Sample pathology report | Differential diagnosis | Board review style question #1 | Board review style answer #1 | Board review style question #2 | Board review style answer #2Cite this page: Gonzalez RS, Chan A. Malnutrition (total parenteral nutrition). PathologyOutlines.com website. https://www.pathologyoutlines.com/topic/liverhyperal.html. Accessed May 12th, 2024.
Definition / general
- Parenteral nutrition provides nutritional support for those patients with prematurity, malabsorption, severe inflammatory bowel disease, necrotizing enterocolitis, congenital gastrointestinal disorders and extensive gastrointestinal surgery, by intravenous infusion of macronutrients (glucose, lipid and amino acids), micronutrients (vitamins and minerals), electrolytes and water
- Hyperalimentation (typically from long-term total parenteral nutrition [TPN]) can cause liver dysfunction that may require combined liver and small bowel transplantation (Dig Dis 1994;12:191, Hepatology 2006;43:9, Gastroenterology 2006;130:S70)
Essential features
- Total parenteral nutrition leads to clinical and pathologic liver injury in 40 - 60% of infants and 15 - 40% of adults (Gastroenterology 2006;130:S70)
- Histology usually shows cholestasis and macrovesicular steatosis
ICD coding
- ICD-10: K71.0 - toxic liver disease with cholestasis
Epidemiology
- More likely to occur in long term, rather than short term, total parenteral nutrition
Pathophysiology
- Poorly understood but likely multifactorial (underlying disease, components and duration of TPN, lack of enteral feeding, recurrent sepsis) (Hepatology 2006;43:9, Aliment Pharmacol Ther 2000;2:54)
Clinical features
- Typically asymptomatic initially
- Usually manifests as mild, reversible liver or biliary injury (Gastroenterol Clin North Am 1989;18:645)
- Infants on total parenteral nutrition may have liver disease progress more rapidly than older patients with jaundice and splenomegaly (Hum Pathol 2012;43:826)
- Clinical severity may not correlate with histologic severity (Hum Pathol 2012;43:826)
- May be fatal (J Pediatr Surg 1982;17:463)
Laboratory
- Elevated conjugated bilirubin is common in children, particularly during sepsis and is usually accompanied by elevation of ALT, ALP and GGT
- Hypoalbuminemia and prolonged PT / INR are late signs
- Thrombocytopenia occurs with splenomegaly secondary to significant liver fibrosis and cirrhosis (Early Hum Dev 2010;86:683)
Prognostic factors
- Total parenteral nutrition may cause more injury in infants small for gestational age or with bronchopulmonary dysplasia (Pediatr Dev Pathol 2004;7:425)
- Fibrosis progresses with increased length of TPN use
Case reports
- 32 week old male on total parenteral nutrition with concern for biliary atresia (BMC Pediatr 2019;19:72)
- 3 year old boy with hepatic encephalopathy (J Neuroimaging 2013;23:248)
- 38 year old man with total parenteral nutrition related cirrhosis (J Gastrointest Surg 2009;13:1717)
- 49 year old man with abnormal liver function (Nutrition 2000;16:1090)
Treatment
- Severe cases may require intestine / liver transplant (Hepatology 2006;43:9)
Microscopic (histologic) description
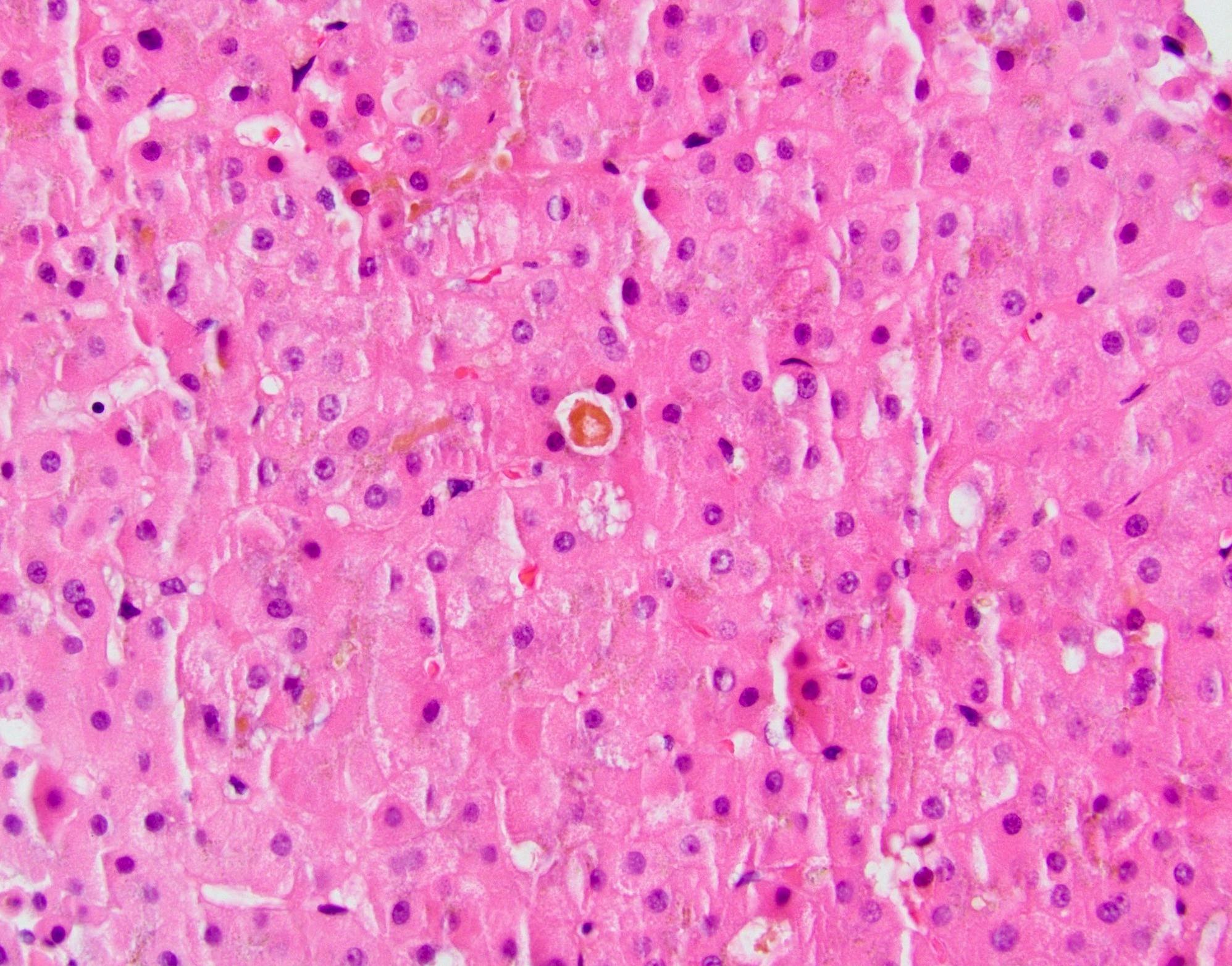
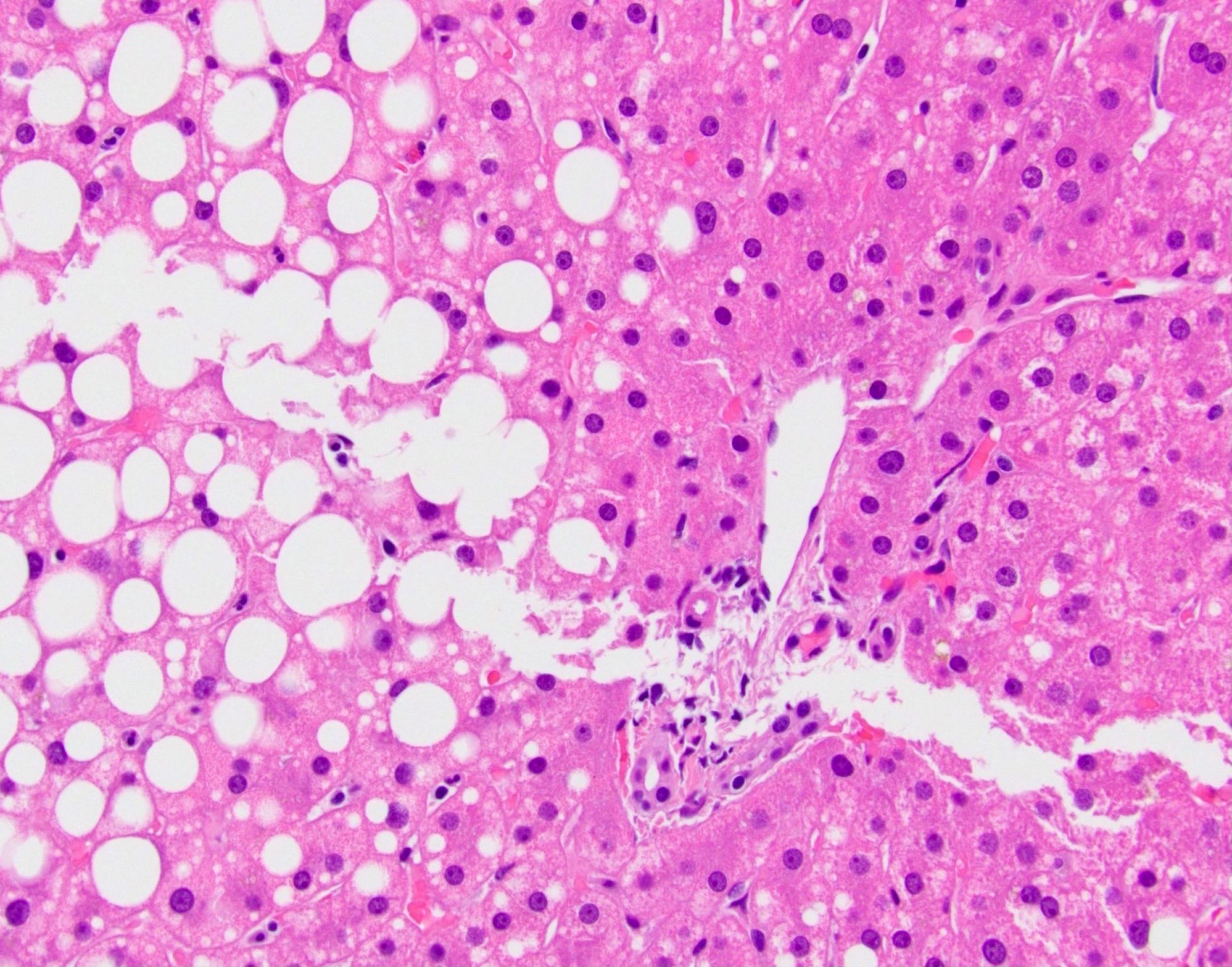
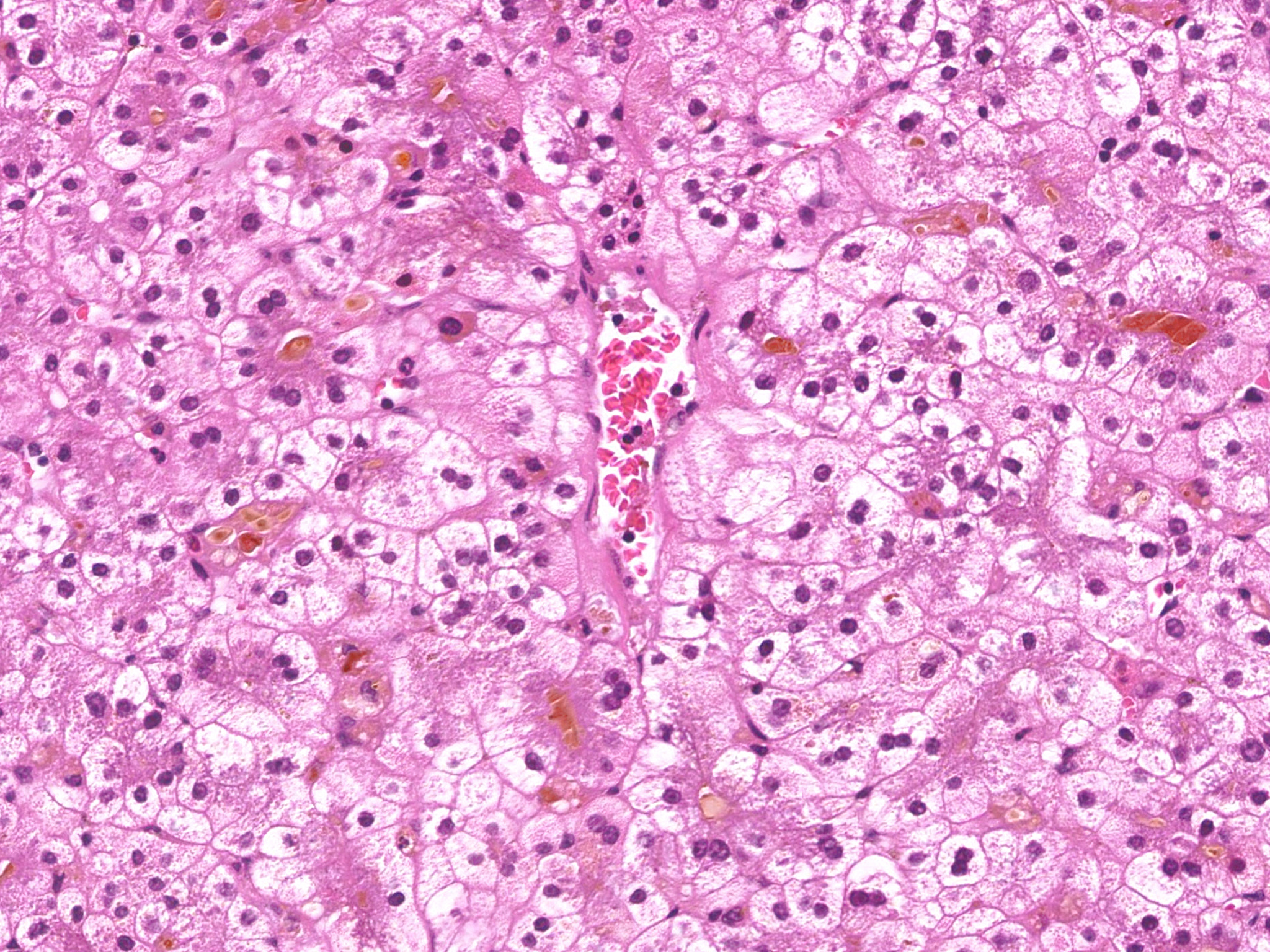
- Variable histology, most often including canalicular cholestasis and periportal macrovesicular steatosis; also ductular reaction, ductopenia, perivenular fibrosis, microvesicular steatosis (Hum Pathol 2012;43:826)
- Cholestasis is more common in neonates than older children / adults
- Steatosis is more common in older children / adults than neonates
- Significant fibrosis may be seen if total parenteral nutrition administered for more than 6 weeks (Pediatr Dev Pathol 2004;7:425)
- Lipofuscin-like pigment and hemosiderin can be seen
- Prominent eosinophilia in portal tract extramedullary hematopoiesis can be seen in pediatric patients (Arch Pathol Lab Med 1981;105:152)
- Phospholipidosis may occur (Gastroenterology 1988;95:183)
Microscopic (histologic) images
Sample pathology report
- Liver, biopsy:
- Mild macrovesicular steatosis and focal canalicular cholestasis (see comment)
- Comment: The findings may be secondary to the patient’s reported long term use of total parenteral nutrition. Other possibilities include fatty liver disease (potentially alcoholic).
Differential diagnosis
- Must rule out other potential causes of liver injury, including sepsis and pre-existing liver disease (Arch Surg 1988;123:1084, Orthop Clin North Am 1983;14:413, Gastroenterology 1993;104:286)
- Alcoholic liver disease:
- May show steatohepatitis and cholestasis
- Should be considered in adult patients not on total parenteral nutrition
- Steatosis more likely perivenular, not periportal
- Bile duct obstruction:
- Portal edema rarely caused by total parenteral nutrition
- May require clinical correlation (Histopathology 1982;6:787)
- Extrahepatic biliary atresia:
- Clinical correlation often necessary for distinction
- Neonatal hepatitis:
- Giant cell transformation and inflammatory infiltrate more common
Board review style question #1
- What are the 2 most classic histologic findings in the liver from patients on long term total parenteral nutrition?
- Ballooning and necrosis
- Cholestasis and iron deposition
- Cholestasis and steatosis
- Necrosis and steatosis
Board review style answer #1
Board review style question #2
Board review style answer #2