22 March 2006 - Case #41
All cases are archived on our website. To view them sorted by case number, diagnosis or category, visit our main Case of the Month page. To subscribe or unsubscribe to Case of the Month or our other email lists, click here.
This case was contributed by Dr. Anthony Martyniak, Beth Israel Deaconess Medical Center, Boston, Massachusetts, USA.
Case #41
Clinical history:
A 72 year old woman with a past medical history of hypertension and hypercholesterolemia presented with a several month history of multiple strokes. All causes of her strokes were ruled out, including infection and a hypercoagulable state. Numerous head CTs and MRIs revealed diffuse periventricular white matter change, thought to be chronic microvascular infarction. The patient's mental status did not improve and a brain biopsy was ultimately performed.
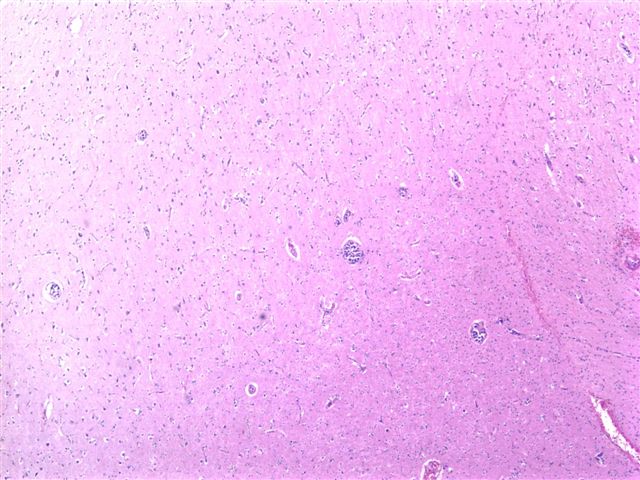
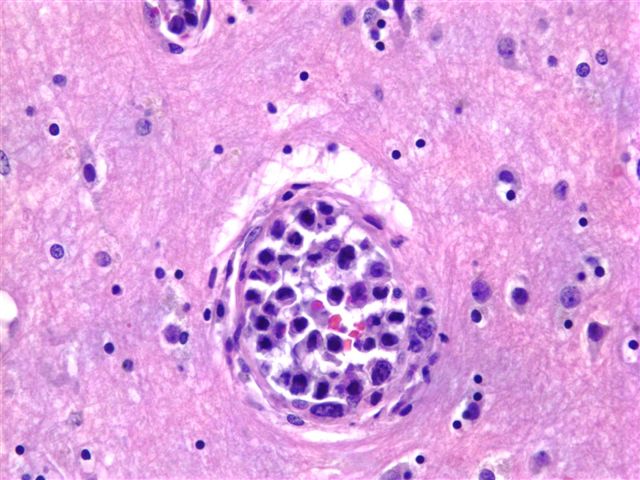
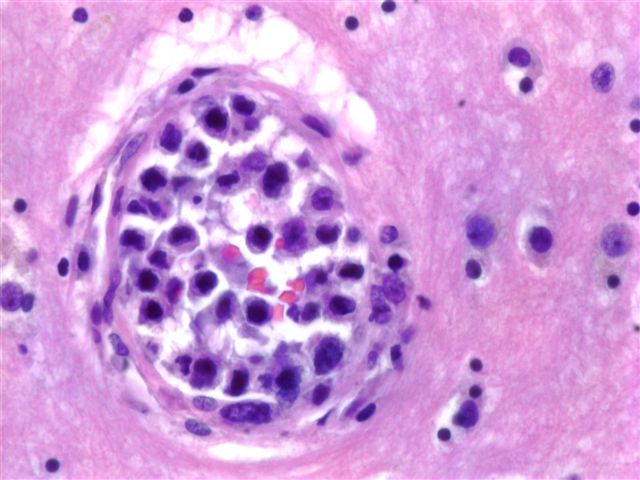
The brain biopsy consisted of cortical gray and white matter with penetrating capillaries and arterioles containing large atypical cells (image 1, image 2). The cells were dyscohesive with irregular nuclear contours and one to several prominent nucleoli (image 3). The cells were immunoreactive for leukocyte common antigen / CD45, CD20 (image 4) and CD79a and were negative for cytokeratins and HMB45.
Microscopic images:
What is your diagnosis?
Diagnosis: Intravascular large B cell lymphoma
Stain image:
Discussion:
Intravascular lymphoma is a rare subtype of diffuse large B cell lymphoma, with intravascular growth in the skin, CNS and other sites. The presenting signs and symptoms are often complex and include mental status changes, as in this case, and rapidly progressive dementia. Patients may present with a mass lesion, a skin rash or fever of unknown origin (Pathol Int 2004;54:231).
Patients are typically elderly, with a median age of 71 years. Although chemotherapy may be effective, these tumors are often not diagnosed until autopsy, which typically shows involvement of most organs (Ann Oncol 2004;15:1215). In this case, the patient was 72 years old and expired 2 weeks after the brain biopsy. A postmortem examination revealed widespread disease, with involvement of the heart, lung, kidneys, adrenals, stomach, pancreas and spleen. No skin lesions were found.
Histologically, the tumor is composed of large centroblast-like lymphoid cells with prominent nucleoli within small vessel lumina, often capillaries. Mitotic figures are frequent and there are often fibrin thrombi. Immunohistochemistry results are similar to diffuse large B cell lymphoma, with immunoreactivity for CD19, CD20, CD22 and CD79a. Tumors are usually BCL2 positive. Rarely, these tumors are T cell lymphomas with corresponding immunoreactivity.
All cases are archived on our website. To view them sorted by case number, diagnosis or category, visit our main Case of the Month page. To subscribe or unsubscribe to Case of the Month or our other email lists, click here.
This case was contributed by Dr. Anthony Martyniak, Beth Israel Deaconess Medical Center, Boston, Massachusetts, USA.
Case #41
Clinical history:
A 72 year old woman with a past medical history of hypertension and hypercholesterolemia presented with a several month history of multiple strokes. All causes of her strokes were ruled out, including infection and a hypercoagulable state. Numerous head CTs and MRIs revealed diffuse periventricular white matter change, thought to be chronic microvascular infarction. The patient's mental status did not improve and a brain biopsy was ultimately performed.
The brain biopsy consisted of cortical gray and white matter with penetrating capillaries and arterioles containing large atypical cells (image 1, image 2). The cells were dyscohesive with irregular nuclear contours and one to several prominent nucleoli (image 3). The cells were immunoreactive for leukocyte common antigen / CD45, CD20 (image 4) and CD79a and were negative for cytokeratins and HMB45.
Microscopic images:
What is your diagnosis?
Click here for diagnosis and discussion:
Diagnosis: Intravascular large B cell lymphoma
Stain image:
Discussion:
Intravascular lymphoma is a rare subtype of diffuse large B cell lymphoma, with intravascular growth in the skin, CNS and other sites. The presenting signs and symptoms are often complex and include mental status changes, as in this case, and rapidly progressive dementia. Patients may present with a mass lesion, a skin rash or fever of unknown origin (Pathol Int 2004;54:231).
Patients are typically elderly, with a median age of 71 years. Although chemotherapy may be effective, these tumors are often not diagnosed until autopsy, which typically shows involvement of most organs (Ann Oncol 2004;15:1215). In this case, the patient was 72 years old and expired 2 weeks after the brain biopsy. A postmortem examination revealed widespread disease, with involvement of the heart, lung, kidneys, adrenals, stomach, pancreas and spleen. No skin lesions were found.
Histologically, the tumor is composed of large centroblast-like lymphoid cells with prominent nucleoli within small vessel lumina, often capillaries. Mitotic figures are frequent and there are often fibrin thrombi. Immunohistochemistry results are similar to diffuse large B cell lymphoma, with immunoreactivity for CD19, CD20, CD22 and CD79a. Tumors are usually BCL2 positive. Rarely, these tumors are T cell lymphomas with corresponding immunoreactivity.