Table of Contents
Definition / general | Essential features | Terminology | ICD coding | Epidemiology | Sites | Pathophysiology | Etiology | Clinical features | Diagnosis | Radiology description | Radiology images | Prognostic factors | Case reports | Treatment | Gross description | Frozen section description | Intraoperative frozen / smear cytology images | Microscopic (histologic) description | Microscopic (histologic) images | Cytology description | Positive stains | Negative stains | Molecular / cytogenetics description | Sample pathology report | Differential diagnosis | Practice question #1 | Practice answer #1 | Practice question #2 | Practice answer #2Cite this page: Lagerstrom I, Pearce T. Spinal ependymoma. PathologyOutlines.com website. https://www.pathologyoutlines.com/topic/cnstumorspinalependymoma.html. Accessed August 29th, 2025.
Definition / general
- Spinal ependymoma is a well circumscribed spinal glioma that consists of cells with round to ovoid nuclei embedded in a fibrillary matrix, often forming perivascular pseudorosettes or true ependymal rosettes that typically exhibit a low mitotic count
- MYCN amplification should be tested in cases that display concerning features, such as microvascular proliferation, necrosis or a high mitotic count
Essential features
- Lacks features of myxopapillary ependymoma and subependymoma
- Ependymomas not molecularly defined can be assigned either CNS WHO grade 2 or grade 3 based on histologic features (Brain Pathol 2020;30:863)
- Spinal ependymoma with MYCN amplification are classified as a distinct entity with a worse prognosis and have not yet been assigned a CNS WHO grade (Acta Neuropathol Commun 2020;8:101, Brain Pathol 2020;30:863)
Terminology
- Histologic subtypes (papillary, clear cell, tanycytic) have no clinical significance and are no longer included in the classification of the disease (Brain Pathol 2020;30:863)
ICD coding
- ICD-O: 9391/3 - spinal ependymoma, NOS
- ICD-11: 2A00.0Z & XH1511 - gliomas of brain, unspecified & ependymoma, NOS
Epidemiology
- Ependymomas account for up to 60% of intramedullary spinal tumors in adults (Radiographics 2000;20:1721)
- Median age at diagnosis ranges from 25 to 45 years across different studies (Childs Nerv Syst 2012;28:2017, Neuro Oncol 2021;23:iii1)
- Neurofibromatosis type 2 is associated with spinal ependymomas, with certain types of NF2 mutations correlated with a higher incidence (Cancer Cell 2015;27:728)
- MYCN amplified spinal ependymomas have a higher incidence in women (1.7:1) and the median age at diagnosis is 31 years (Acta Neuropathol 2019;138:1075)
Sites
- Intramedullary tumors arising in the spinal cord parenchyma, most commonly involving the cervical cord (Radiographics 2000;20:1721)
Pathophysiology
- Spinal ependymoma
- Ependymomas are associated with mutations in the NF2 tumor suppressor gene and loss of chromosome 22q (Cancer Cell 2015;27:728, Lancet 2009;373:1974)
- NF2 deficient spinal cord neural progenitor cells show increased ErbB2 activation, which has been shown to contribute to the development of spinal ependymomas in mouse models (PLoS One 2014;9:e97320)
- Spinal ependymoma, MYCN amplified
- Overexpression of the MYCN protein disrupts the normal cell cycle and promotes unchecked cell proliferation; MYCN amplification is linked to increased tumor aggressiveness, resistance to therapy and worse overall survival rates in various tumors (Mol Cancer Res 2014;12:815)
- There is no clear understanding of how MYCN amplification contributes specifically to ependymoma development
Etiology
- 18 - 53% of patients with neurofibromatosis type 2 develop spinal ependymoma; however, only 20% of cases are symptomatic (Lancet 2009;373:1974)
- Etiology of spinal ependymoma, MYCN amplified, is unknown at this time
Clinical features
- Clinical presentation is nonspecific and depends on the location of the tumor
Diagnosis
- Spinal ependymomas not molecularly defined can be assigned either CNS WHO grade 2 or grade 3 based on histologic features (Brain Pathol 2020;30:863)
- Anaplastic ependymoma has been removed from the classification
- Spinal ependymoma, MYCN amplified, has not yet been assigned a CNS WHO grade
- Spinal ependymomas can be distinguished from myxopapillary ependymomas, subependymomas and MYCN amplified spinal ependymomas using DNA methylation profiling (Cancer Cell 2015;27:728)
Radiology description
- Magnetic resonance imaging (MRI) with contrast enhancement is the preferred imaging modality for ependymomas (Curr Oncol Rep 2022;24:985)
- Imaging features that suggest an ependymoma include a central spinal cord location, the presence of a cleavage plane (a radiolucent line that appears between a tumor and surrounding tissue) and uniform enhancement (Radiographics 2000;20:1721)
Radiology images
Prognostic factors
- Adult spinal ependymomas have a good prognosis following gross total resection (Curr Oncol Rep 2022;24:985)
- Progression free survival (PFS) is improved with radiotherapy after subtotal resection (median PFS was 48 months in patients with subtotal resection alone compared to 96 months in patients with subtotal resection and radiotherapy) (Neuro Oncol 2013;15:208)
- MYCN amplification denotes a poor prognosis with early metastasis and high recurrence rates, even with aggressive treatment (J Neuropathol Exp Neurol 2019;78:791, Acta Neuropathol 2019;138:1075)
Case reports
- 12 year old boy with a 3 month history of back pain and acute onset of weakness (Acta Neuropathol Commun 2021;9:192)
- 12 year old girl, 36 year old man and 56 year old man with spinal ependymomas, MYCN amplified (J Neurosurg Case Lessons 2025;9:CASE24696)
- 16 year old girl with neurofibromatosis type 2 with multiple schwannomas, meningioma and spinal ependymoma (J Med Case Rep 2024;18:95)
- 21 year old man with spinal ependymoma that was discovered following a renal transplant (Exp Clin Transplant 2022;20:871)
Treatment
- Gross total resection is the preferred treatment, with or without adjuvant radiotherapy
- Subtotal resection can be accompanied by radiotherapy to improve progression free survival (Neuro Oncol 2013;15:208)
- Chemotherapy does not currently have a significant role in the primary treatment of ependymal tumors
- ErbB2 might be a potential therapeutic target for treating NF2 deficient spinal ependymomas (PLoS One 2014;9:e97320)
Gross description
- Well circumscribed tumors that may display calcifications, hemorrhage, necrosis and cystic change
Frozen section description
- Moderately cellular and well circumscribed tumor composed of uniform appearing cells, typically with a low mitotic count
- Perivascular pseudorosettes are common, while true ependymal rosettes are infrequently seen
- If high grade features are present, it may not be possible to distinguish spinal ependymoma from other entities, such as MYCN amplified spinal ependymoma and H3 K27 altered diffuse midline glioma
- Reference: Acta Neuropathol 2019;138:1075
Intraoperative frozen / smear cytology images
Microscopic (histologic) description
- Spinal ependymoma
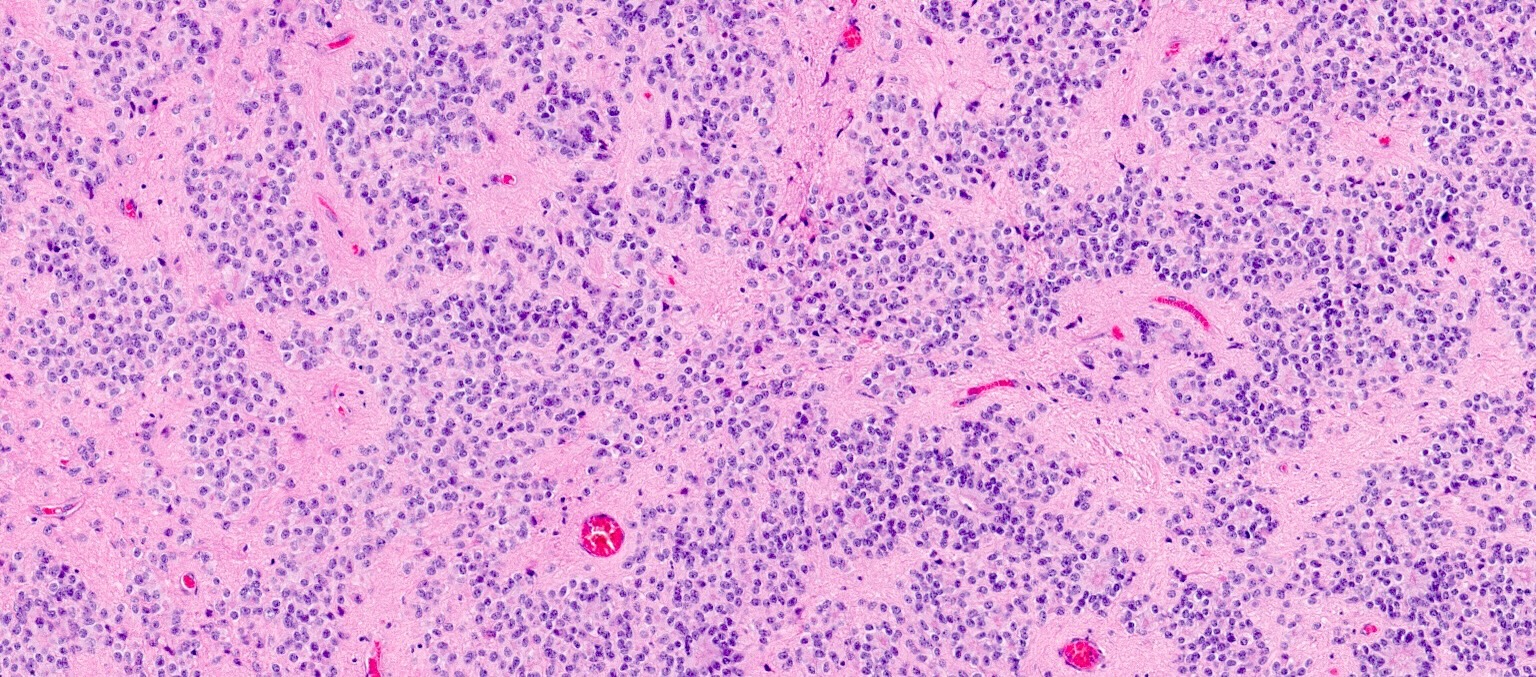
- Composed of isomorphic glial cells with round to oval nuclei and indistinct cell membranes embedded in a fibrillary glial matrix
- Well circumscribed
- Generally low mitotic activity
- Perivascular pseudorosettes are a common histologic feature (tumor cells arranged radially around a central vessel)
- True ependymal rosettes are found in only a minority of cases (Cureus 2023;15:e49086)
- Tanycytic pattern: rare, featuring spindle shaped cells and bipolar processes; can be confused with pilocytic astrocytoma and schwannoma
- Grading of spinal ependymoma
- Like in other locations, criteria to distinguish WHO grade 2 from WHO grade 3 are not firmly defined and are based on morphologic findings that can be somewhat subjective
- In general, WHO grade 2 spinal ependymoma is well circumscribed and has a low to moderate cellular density, rare mitoses and no microvascular proliferation or significant necrosis
- In general, WHO grade 3 spinal ependymoma exhibits higher cellularity, increased mitotic activity, microvascular proliferation or pseudopalisading necrosis (Brain Pathol 2020;30:863, Neuro Oncol 2018;20:445)
- Spinal ependymoma, MYCN amplified, has high grade features (similar to WHO grade 3 spinal ependymoma) including hyperchromatic nuclei with high nuclear to cytoplasmic ratios, higher mitotic count, microvascular proliferation and necrosis (Acta Neuropathol Commun 2020;8:101)
- Histologic subtypes (papillary, clear cell, tanycytic) have no clinical significance and are no longer included in the classification of the disease (Brain Pathol 2020;30:863)
Microscopic (histologic) images
Cytology description
- Isomorphic cells with round to oval nuclei and delicate fibrillary cytoplasm
- Arrangement of tumor cells around blood vessels can occasionally be seen
Positive stains
- GFAP
- S100
- Vimentin
- Dot-like or ring-like perinuclear pattern of EMA
- References: Crit Rev Oncol Hematol 2007;63:81, Neuro Oncol 2018;20:445
Negative stains
Molecular / cytogenetics description
- Mutations in the NF2 tumor suppressor gene and loss of chromosome 22q are characteristic of spinal ependymomas (Cancer Cell 2015;27:728, Lancet 2009;373:1974)
- In one study, 19 of 21 (90%) of spinal ependymomas showed loss of 22q (Cancer Cell 2015;27:728)
- High level MYCN amplification is diagnostic of spinal ependymoma
Sample pathology report
- Cervical spine, intramedullary mass, resection:
- Spinal ependymoma, CNS WHO grade 2 (see comment)
- Comment: Histologic sections show an ependymal neoplasm composed of uniform cells with oval to round nuclei. Numerous perivascular pseudorosettes are identified. No necrosis, microvascular proliferation or mitotic figures are identified. GFAP and S100 immunohistochemical stains are positive while Olig2 is negative. EMA shows dot-like perinuclear staining. The combined morphologic and immunophenotypic findings are most consistent with CNS WHO grade 2 spinal ependymoma.
- Thoracic spine, intramedullary mass, resection:
- Spinal ependymoma, MYCN amplified, CNS WHO grade deferred (see comment)
- Comment: Histologic sections show an ependymal neoplasm composed of cells with high nuclear to cytoplasmic ratio, hyperchromatic nuclei and plentiful mitotic activity. Necrosis and microvascular proliferation are present. Numerous perivascular pseudorosettes are identified. GFAP and S100 immunohistochemical stains are positive while Olig2 and H3F3A K27M are negative. EMA shows dot-like perinuclear staining. MYCN amplification was detected by next generation sequencing and DNA methylation profiling is aligned with spinal ependymoma, MYCN amplified. This molecularly defined ependymal tumor is not currently assigned a CNS WHO grade.
Differential diagnosis
- Myxopapillary ependymoma:
- Distinct histologic appearance with tumor cells radially arranged around hyalinized fibrovascular cores
- Immunoreactive for GFAP and S100 but the dot-like perinuclear staining pattern of EMA is typically absent
- Almost exclusively located in the lumbar region (Radiographics 2000;20:1721)
- Astrocytoma, IDH mutant:
- Variable histology but generally lacks a well defined border with adjacent tissue
- Perivascular pseudorosettes and true ependymal rosettes are absent
- Absent or uncommon mitotic activity in CNS WHO grade 2 tumors
- IDH1 or IDH2 mutation present
- Typically express Olig2
- H3 K27 altered diffuse midline glioma:
- Should be considered when high grade features are present (microvascular proliferation, necrosis, increased mitotic count)
- Can display perivascular arrangement of tumor cells resembling ependymoma-like pseudorosettes
- Typically express Olig2 and are positive for H3F3A K27M
- Schwannoma:
- Subependymoma:
- Most commonly arise in the fourth ventricle and lateral ventricles but may rarely be located in the spinal cord (J Neurooncol 2007;85:297, J Korean Neurosurg Soc 2018;61:233)
- Spinal cord subependymoma should be considered when the tumor is located eccentrically and does not have a clear dissection plane (J Korean Neurosurg Soc 2018;61:233)
- Nuclear clustering and microcysts are common features, which are not seen in spinal ependymoma
- True ependymal rosettes are not present
Practice question #1
The tumor shown above was resected from the cervical spine. The tumor cells express S100 and GFAP and are negative for Olig2. The tumor has a central spinal cord location on MRI and the presence of a cleavage plane is noted. What is the diagnosis?
- Astrocytoma, IDH mutant
- Myxopapillary ependymoma
- Schwannoma
- Spinal ependymoma
Practice answer #1
D. Spinal ependymoma. Spinal ependymoma typically displays low grade histologic features and perivascular pseudorosettes are a hallmark feature. The tumor cells express S100 and GFAP and are negative for Olig2. EMA dot-like perinuclear staining can also be seen. A cervical spine location is typical. Spinal ependymomas are intramedullary neoplasms and have a distinct border between lesional and adjacent uninvolved tissue (indicated by the presence of a cleavage plane on radiology). Answer A is incorrect because IDH mutant astrocytomas typically express Olig2 and have an infiltrative border. Additionally, perivascular psuedorosettes are absent. Answer B is incorrect because myxopapillary ependymomas have a distinct histologic appearance with tumor cells radially arranged around hyalinized fibrovascular cores. Additionally, myxopapillary ependymomas almost exclusively occur in the lumbar spine. Answer C is incorrect because schwannomas are extra-axial lesions characterized by a zonal pattern with cellular areas (Antoni A) and hypocellular areas (Antoni B). Perivascular psuedorosettes are not a feature of schwannomas.
Comment Here
Reference: Spinal ependymoma
Comment Here
Reference: Spinal ependymoma
Practice question #2
A spinal tumor with morphological and immunohistochemical features of ependymoma that displays high grade histologic features should be tested for what molecularly defining alteration?
- IDH mutation
- Loss of chromosome 22q
- MYCN amplification
- ZFTA fusion
Practice answer #2
C. MYCN amplification. High grade histologic features in a spinal ependymoma include hyperchromatic nuclei with high nuclear to cytoplasmic ratios, abundant mitotic activity, microvascular proliferation and necrosis. All spinal ependymomas that display any of these concerning features should be tested for MYCN amplification. Spinal ependymoma, MYCN amplified is a molecularly defined tumor distinct from CNS WHO grade 2 or 3 spinal ependymoma and has a worse prognosis. Answer A is incorrect because an IDH mutation is present in IDH mutant astrocytoma, which would not display features of ependymoma. Answer D is incorrect because the presence of a ZFTA fusion gene is a defining mutation of supratentorial ependymoma, ZFTA fusion positive. Answer B is incorrect because loss of chromosome 22q is not a molecularly defining mutation; however, loss of chromosome 22q is seen in the majority of spinal ependymomas and can be a useful diagnostic feature.
Comment Here
Reference: Spinal ependymoma
Comment Here
Reference: Spinal ependymoma