Table of Contents
Definition / general | Essential features | Terminology | ICD coding | Epidemiology | Sites | Pathophysiology | Etiology | Clinical features | Diagnosis | Prognostic factors | Case reports | Treatment | Clinical images | Gross description | Microscopic (histologic) description | Microscopic (histologic) images | Virtual slides | Positive stains | Negative stains | Molecular / cytogenetics description | Videos | Sample pathology report | Differential diagnosis | Practice question #1 | Practice answer #1 | Practice question #2 | Practice answer #2Cite this page: Wondimu B, Chang OH. Hidradenoma papilliferum. PathologyOutlines.com website. https://www.pathologyoutlines.com/topic/skintumornonmelanocytichidradenomapap.html. Accessed October 6th, 2025.
Definition / general
- Hidradenoma papilliferum is a benign dermal papulonodular tumor almost always found in the vulva / perianal region of women
Essential features
- Benign neoplasm of modified anogenital mammary-like glands, predominantly found in the vulva / perianal region of women
- Histopathology features include characteristic dermal maze-like growth with papillary / glandular / cyst-like architecture, often with apocrine differentiation
Terminology
- Also referred to as papillary hidradenoma
ICD coding
Epidemiology
- Predominantly women; ages 30 - 80 (Arch Gynecol Obstet 2011;284:1015, Clin Exp Dermatol 2020;45:1035)
- Ectopic hidradenoma papilliferum is only slightly more common in women (Am J Dermatopathol 2003;25:176)
Sites
- Vulva or perianal region
- Rarely involves ectopic sites (head, neck, chest, abdomen) (Indian J Pathol Microbiol 2018;61:287)
- 60% of ectopic HP is present in head and neck region, including eyelid, forehead, face, external auditory canal, post auricular region
- Thought to arise from modified apocrine glands in eyelids / external auditory canal or heterotopic apocrine glands
- Rare case reports of sebaceous differentiation in ectopic HP (Pathology 2019;51:362)
Pathophysiology
- Favored to arise from anogenital mammary-like glands (Am J Dermatopathol 2012;34:104)
Etiology
- Unknown
Clinical features
- Solitary dermal or subcutaneous nodule, < 1 - 2 cm
- Usually asymptomatic but can present with pain, pruritis, discharge or ulceration / bleeding (Calonje: McKee's Pathology of the Skin, 4th Edition, 2011)
Diagnosis
- Clinical diagnosis confirmed with biopsy
- May cause Bartholin cyst or abscess; can be misdiagnosed as such (Arch Gynecol Obstet 2011;284:1015)
Prognostic factors
- Generally excellent prognosis and curative with complete excision
- Can very rarely transform into malignant hidradenocarcinoma papilliferum or aggressive adenosquamous carcinoma (Gynecol Oncol 1989;35:395)
Case reports
- 16 year old boy with upper and lower eyelid lesions (Indian J Pathol Microbiol 2018;61:287)
- 35 and 39 year old women with perianal mass and hemorrhoids (Ann Coloproctol 2019;35:361)
- 36 year old man with left areolar papule (An Bras Dermatol 2018;93:474)
- 38 year old woman with painful vaginal mass (J Med Case Rep 2021;15:162)
- 56 year old man with unilateral hearing loss and an external auditory canal mass (Ann Med Surg (Lond) 2019;49:41)
Treatment
- Conservative surgical excision or excision with wide margins (Arch Gynecol Obstet 2011;284:1015)
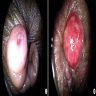
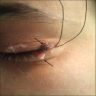
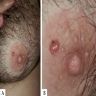
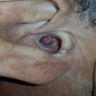
Clinical images
Gross description
- Solid, skin colored papule, usually < 1 - 2 cm
Microscopic (histologic) description
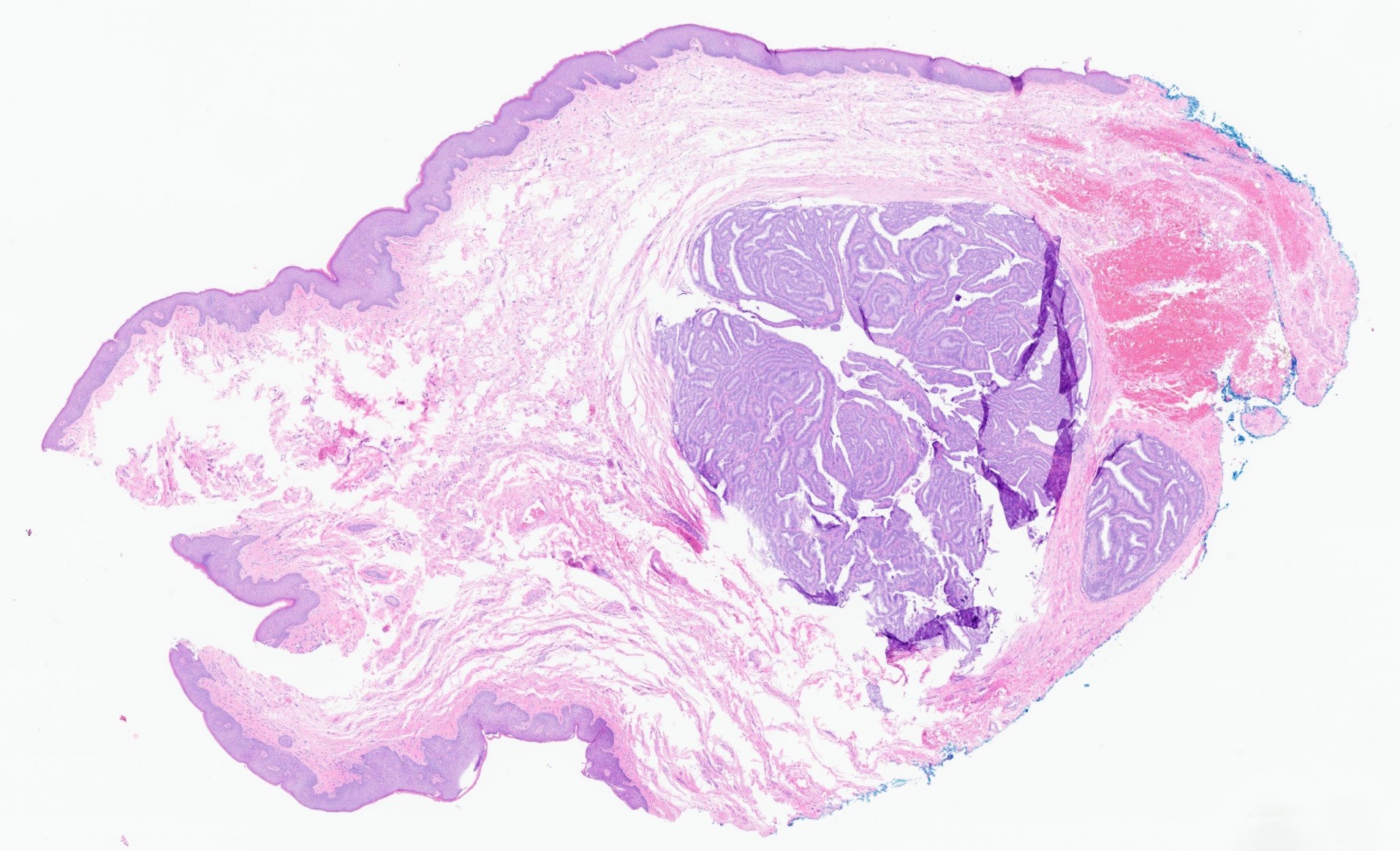
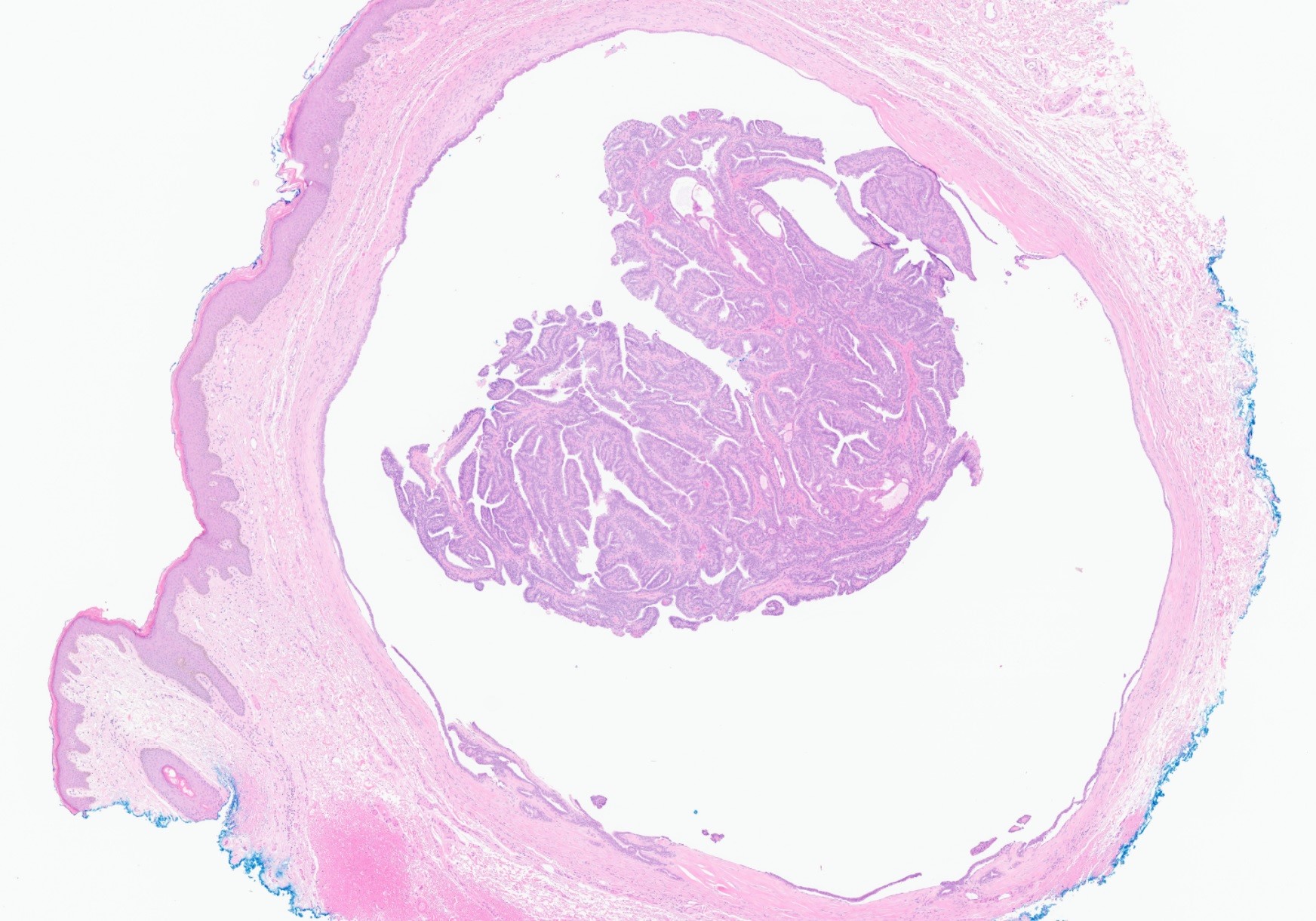
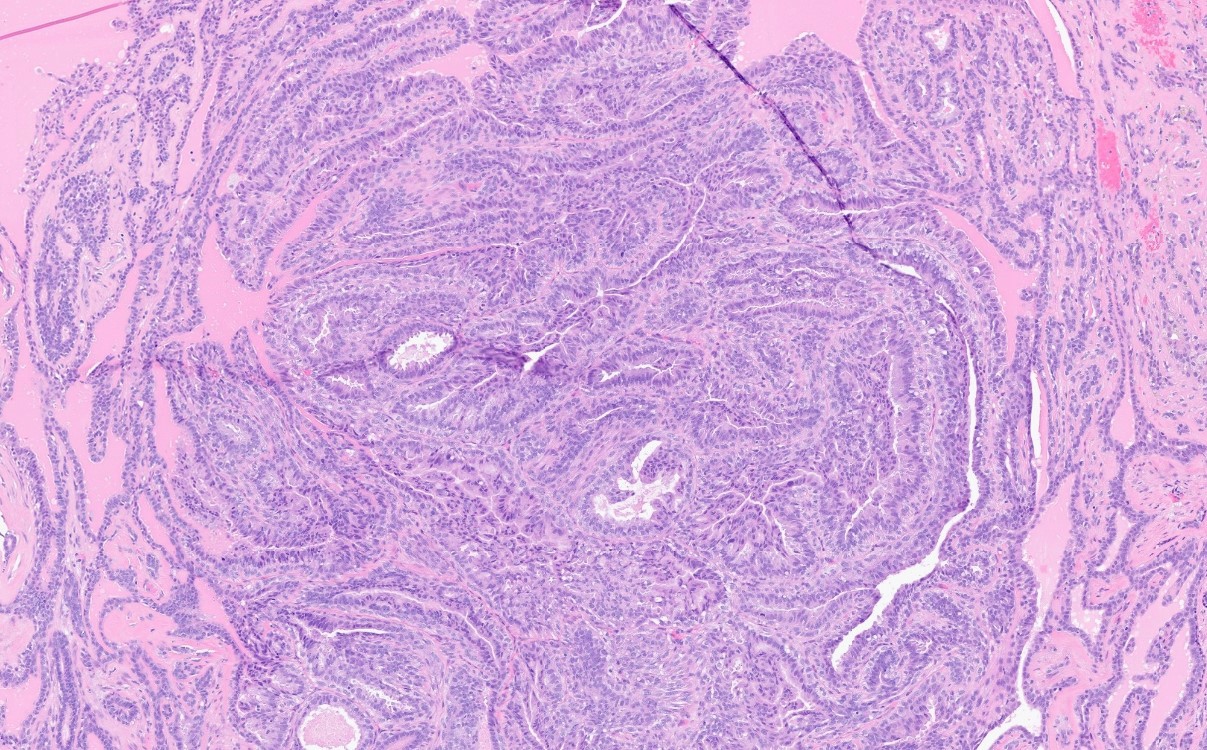
- Well circumscribed dermal maze-like or arborizing proliferation (rarely connected to epidermis), with a combination of papillary, cystic or glandular architecture
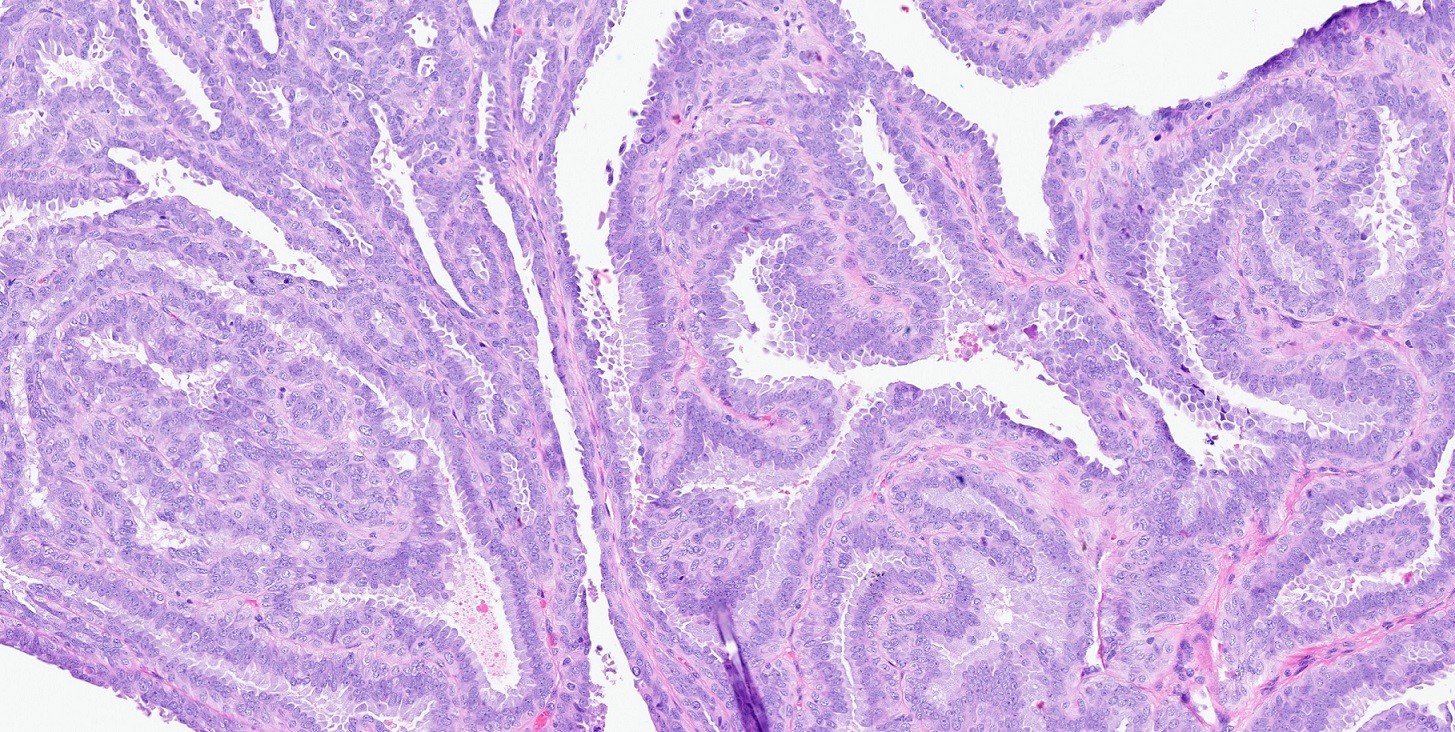
- 2 types of epithelia:
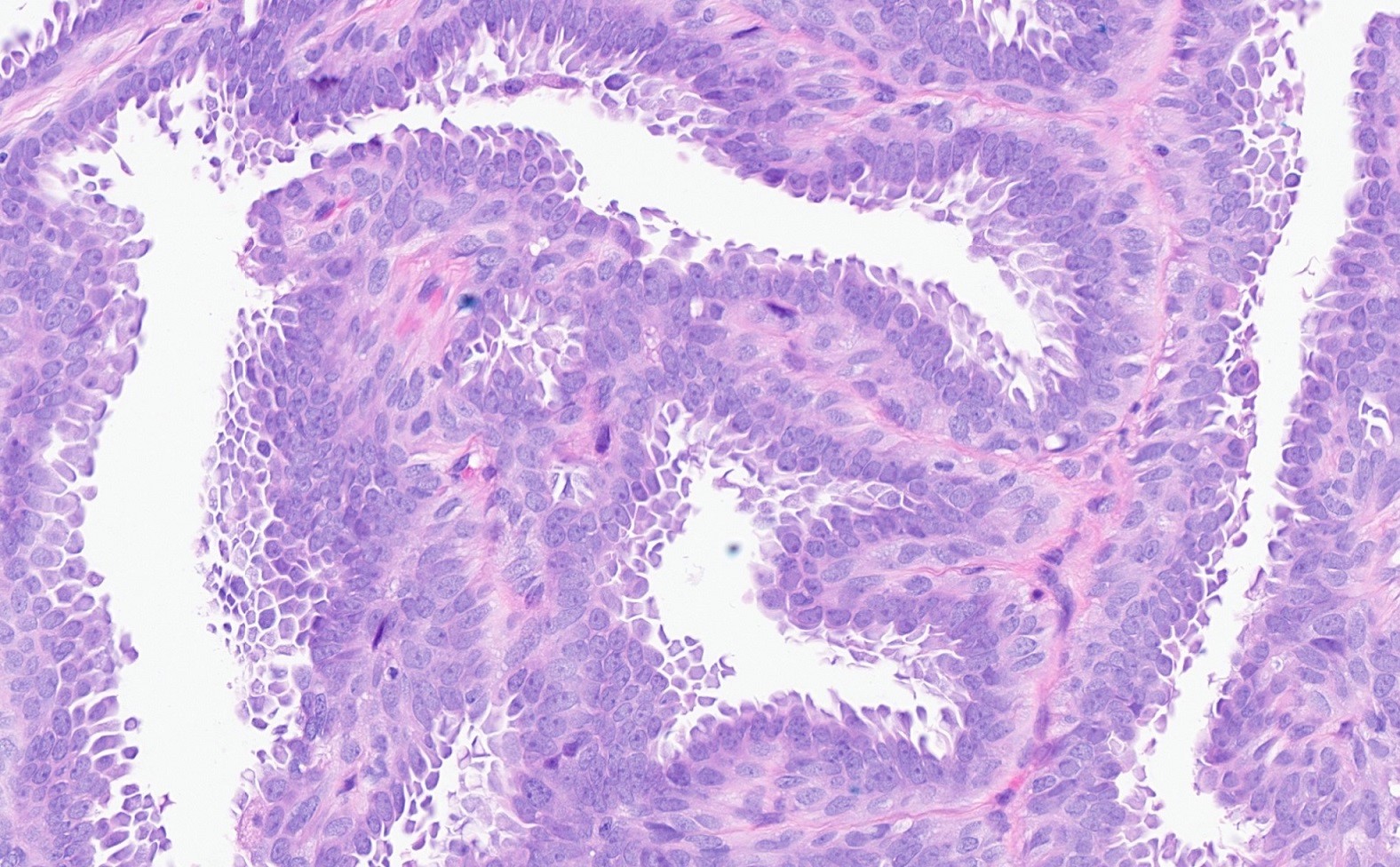
- Luminal layer of tall, columnar cells; cuboidal cells with eosinophilic cytoplasm, decapitation secretion and small, round nuclei (apocrine differentiation)
- Can occasionally exhibit clear cell change (lamprocyte-like changes) (Pathology 2019;51:362)
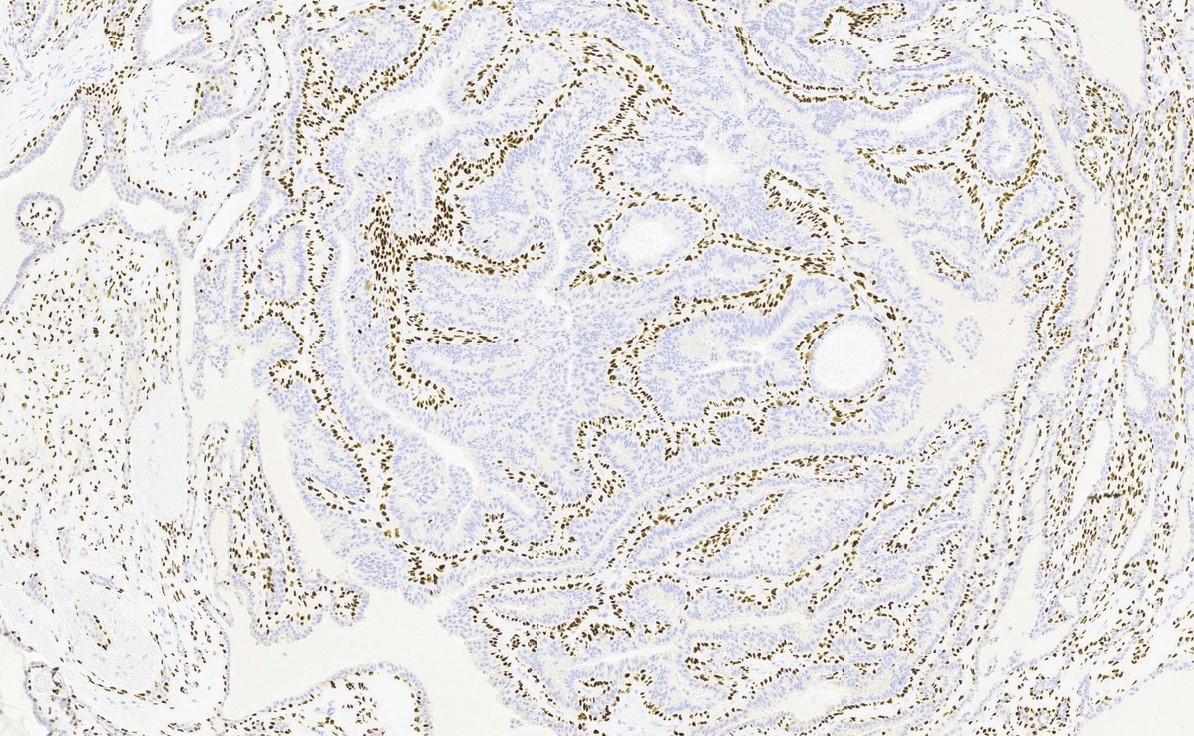
- Underlying layer of thin or cuboidal myoepithelial cells (Am J Dermatopathol 2006;28:322, Ann Coloproctol 2019;35:361)
- Luminal layer of tall, columnar cells; cuboidal cells with eosinophilic cytoplasm, decapitation secretion and small, round nuclei (apocrine differentiation)
- Entrapment of epithelial cells in connective tissue may mimic infiltrative pattern (Arch Gynecol Obstet 2011;284:1015)
- May have connection to the epidermis with associated dermal plasma cell infiltrate (mimics syringocystadenoma papilliferum) (Am J Dermatopathol 2016;38:598)
- Stromal changes: dense stromal plasma cell infiltrate, sclerosis, hyperplasia of myofibroblast-like cells, foamy macrophages
- Metaplasia occasionally present
- Most commonly oxyphilic (eosinophilic, granular cytoplasm, conspicuous nucleoli, occasional pleomorphism), oftentimes leading to misdiagnosis of malignancy (Am J Dermatopathol 2005;27:102)
- Rarely squamous or mucinous metaplasia
- Remnants of anogenital mammary-like glands (AGMLG) often present
- Epithelium of these glands can be normal or exhibit columnar cell change or columnar cell hyperplasia (Am J Dermatopathol 2016;38:598)
- Mitotic rate can be variable and sometimes high but high mitotic rate does not correlate with an aggressive outcome (Am J Dermatopathol 2006;28:322)
- Rare case reports with sebaceous differentiation (in association with ectopic HP) and extramammary Paget disease (J Dermatol 2006;33:256, Am J Dermatopathol 2016;38:598)
Microscopic (histologic) images
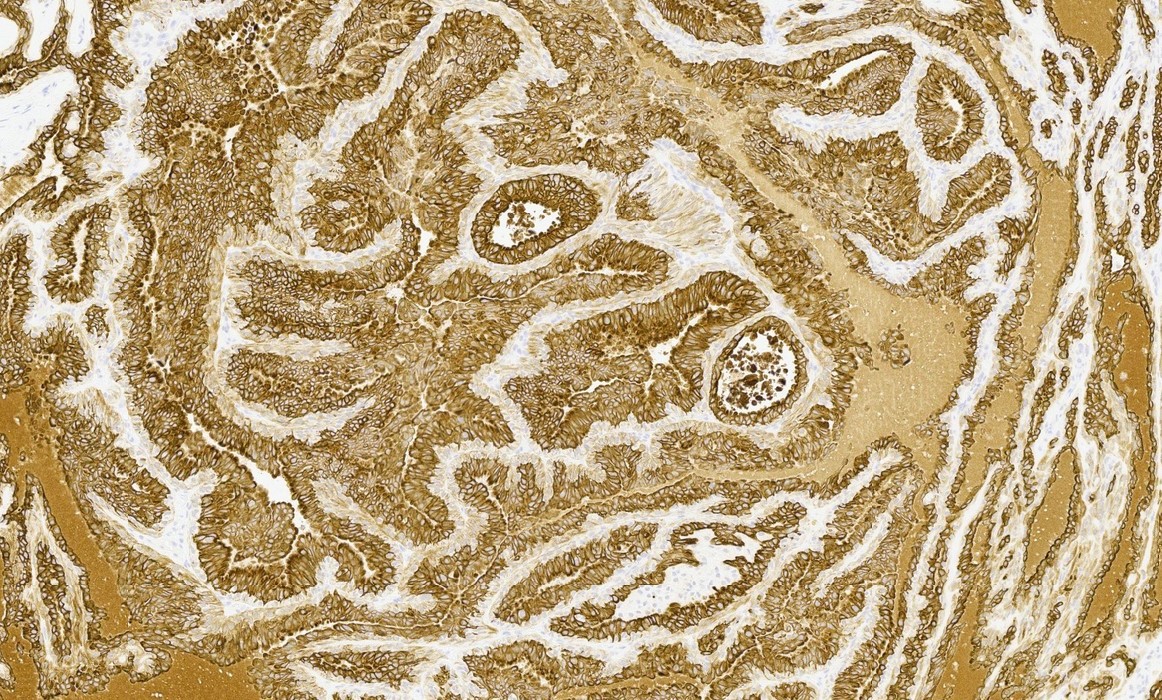
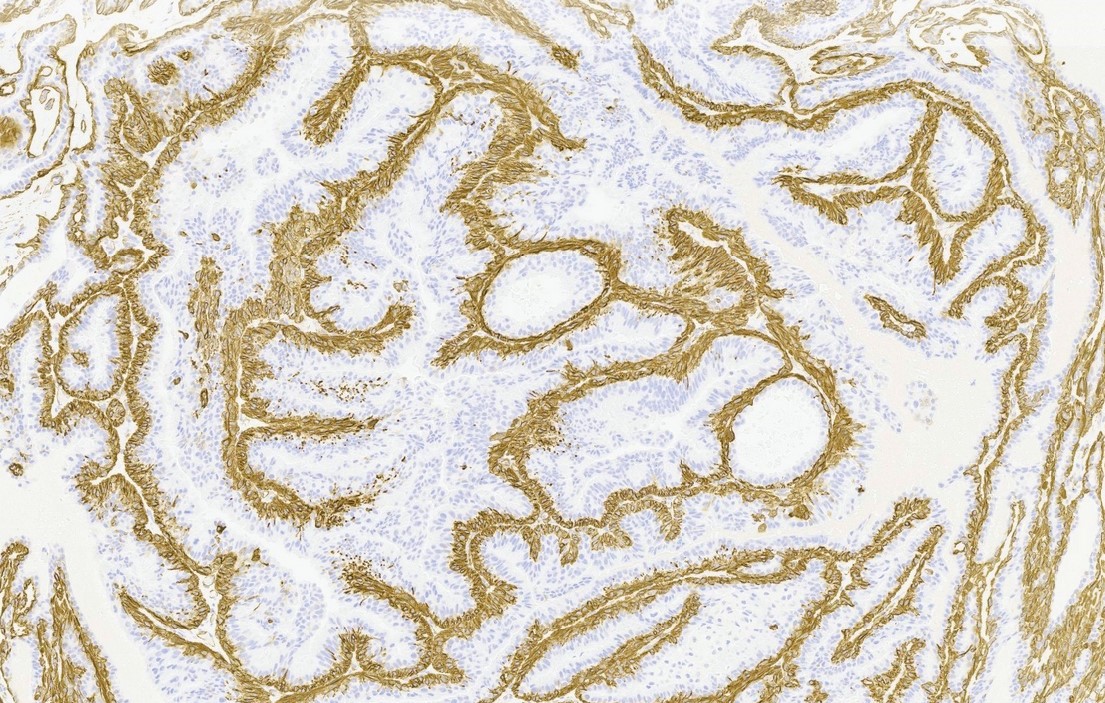
Positive stains
Molecular / cytogenetics description
- Described to harbor mutations in genes involved in PI3K/ATK/MAPK signaling pathways (Pathology 2019;51:362)
- Non-PI3K/AKT mutated cases display mutations in various other genes (PIK3CA PIK3R1, SYNE1, AR, IL6ST, PDGFRB, KMT2C, AR, BTK, DST, KAT6A, BRD3, RNF213, USP9X, ADGRB3, MAGI1, and IL7R) involved in PI3K/AKT signaling
- Rare cases described mutations in BRAF, APC, ERBB4 (Genes Chromosomes Cancer 2016;55:113)
Videos
Diagnostic pearls of hidradenoma papilliferum
Sample pathology report
- Skin, vulva, biopsy:
- Diagnosis: hidradenoma papilliferum (see comment)
- Comment: The biopsy contains a sharply circumscribed, maze-like glandular and papillary architecture without connection to overlying epithelium. The glands are lined by an inner layer of cuboidal cells and an outer layer of myoepithelial cells. Mitotic figures are rare. The morphologic features are most consistent with hidradenoma papilliferum.
Differential diagnosis
- Syringocystadenoma papilliferum:
- Frequently connects to epidermis
- Associated with characteristic plasma cell infiltrate
- More common on head and neck
- Hidradenocarcinoma papilliferum:
- Asymmetric, infiltrative growth pattern, cytologic atypia, cribriform structures (Am J Dermatopathol 2006;28:322)
- Tubular apocrine adenoma:
- Predominantly tubular structures
- Less complex architecture
- Papillary eccrine adenoma:
- Eccrine differentiation
Practice question #1
Practice answer #1
Practice question #2
A 57 year old woman develops a lesion on her vulva. Excision of the lesion shows a glandular and papillary proliferation (shown above). Which of the following is true concerning this lesion?
- Higher mitotic activity indicates worse prognosis
- It is often associated with a plasma cell infiltrate
- It is positive for EMA and GCDFP-15
- Malignant transformation occurs frequently
Practice answer #2