Table of Contents
Definition / general | Essential features | Terminology | ICD coding | Epidemiology | Sites | Pathophysiology | Etiology | Diagrams / tables | Clinical features | Diagnosis | Radiology description | Radiology images | Prognostic factors | Case reports | Treatment | Gross description | Gross images | Frozen section description | Frozen section images | Microscopic (histologic) description | Microscopic (histologic) images | Cytology description | Positive stains | Negative stains | Sample pathology report | Differential diagnosis | Additional references | Practice question #1 | Practice answer #1 | Practice question #2 | Practice answer #2Cite this page: Ualiyeva S, Basu A. Adenoma. PathologyOutlines.com website. https://www.pathologyoutlines.com/topic/lungtumoradenomagen.html. Accessed August 29th, 2025.
Definition / general
- Lung adenomas are benign epithelial pulmonary neoplasms
- Lung adenomas include bronchial adenoma (BA) / ciliated muconodular papillary tumor (CMPT), alveolar adenoma, papillary adenoma, mucinous cystadenoma of the lung, mucous gland adenoma of the lung and sclerosing pneumocytoma
Essential features
- Well circumscribed nodules and usually found incidentally
- Benign looking cells with no cytological atypia or proliferation
- Full excision is curative
Terminology
- Bronchiolar adenoma / ciliated muconodular papillary tumor: although not recommended, terminology used in the literature is peripheral papilloma; solitary peripheral ciliated glandular papilloma
- Alveolar adenoma: not recommended
- Papillary adenoma of lung: not recommended
- Mucinous cystadenoma of lung: not recommended
- Mucous gland adenoma of lung: not recommended
ICD coding
Epidemiology
- Lung adenomas affect a wide range of ages (2 months to 80 years), with a slight female predominance in alveolar adenoma and mucinous cystadenoma; male predominance in papillary adenoma of the lung (Hum Pathol 1999;30:158, Cancer 1980;45:1486, J Bronchology Interv Pulmonol 2013;20:52)
- In bronchial adenoma, it usually affects mostly middle to elderly age patients with median age in early 70s without any sex predilection
- Mucous gland adenoma is a very rare entity; it has no sex predilection and has a wide age range (25 - 67 years) (Am J Surg Pathol 1995;19:887)
Sites
- All the adenomas are typically solitary tumors of the peripheral lung
- Rarely, can be located in the hilum, visceral pleura or mediastinum, except for mucous gland adenoma, which arises from proximal bronchus, although very few could be peripheral (J Comput Assist Tomogr 2002;26:358, Respiration 2012;84:142, Hum Pathol 1986;17:1066, Cancer 1980;45:1486, Am J Surg Pathol 2015;39:753, Case Rep Pathol 2013;2013:239173)
Pathophysiology
- Lung adenomas are derived from primitive respiratory epithelium
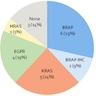
- BRAF, EGFR, KRAS, HRAS, ALK mutations are reported in bronchiolar adenoma / ciliated muconodular papillary tumor; BRAF is the most common mutation, with other mutually exclusive driver alterations (Pathol Int 2017;67:99, Diagn Pathol 2017;12:62, J Thorac Oncol 2016;11:261, Am J Surg Pathol 2018;42:1010)
- Microsatellite instabilities, diploid DNA pattern and nonbalanced translocation t(10;16) have been described in alveolar adenomas (Int J Surg Pathol 2004;12:155, APMIS 2007;115:1443, Cancer Genet Cytogenet 1996;89:34)
- See Diagrams / tables
Etiology
- No predisposing factors are known
Clinical features
- Lung adenomas are typically incidental findings
- Mucous gland adenomas can present with dyspnea, cough, hemoptysis and recurrent pneumonia (Am J Surg Pathol 1995;19:887)
Diagnosis
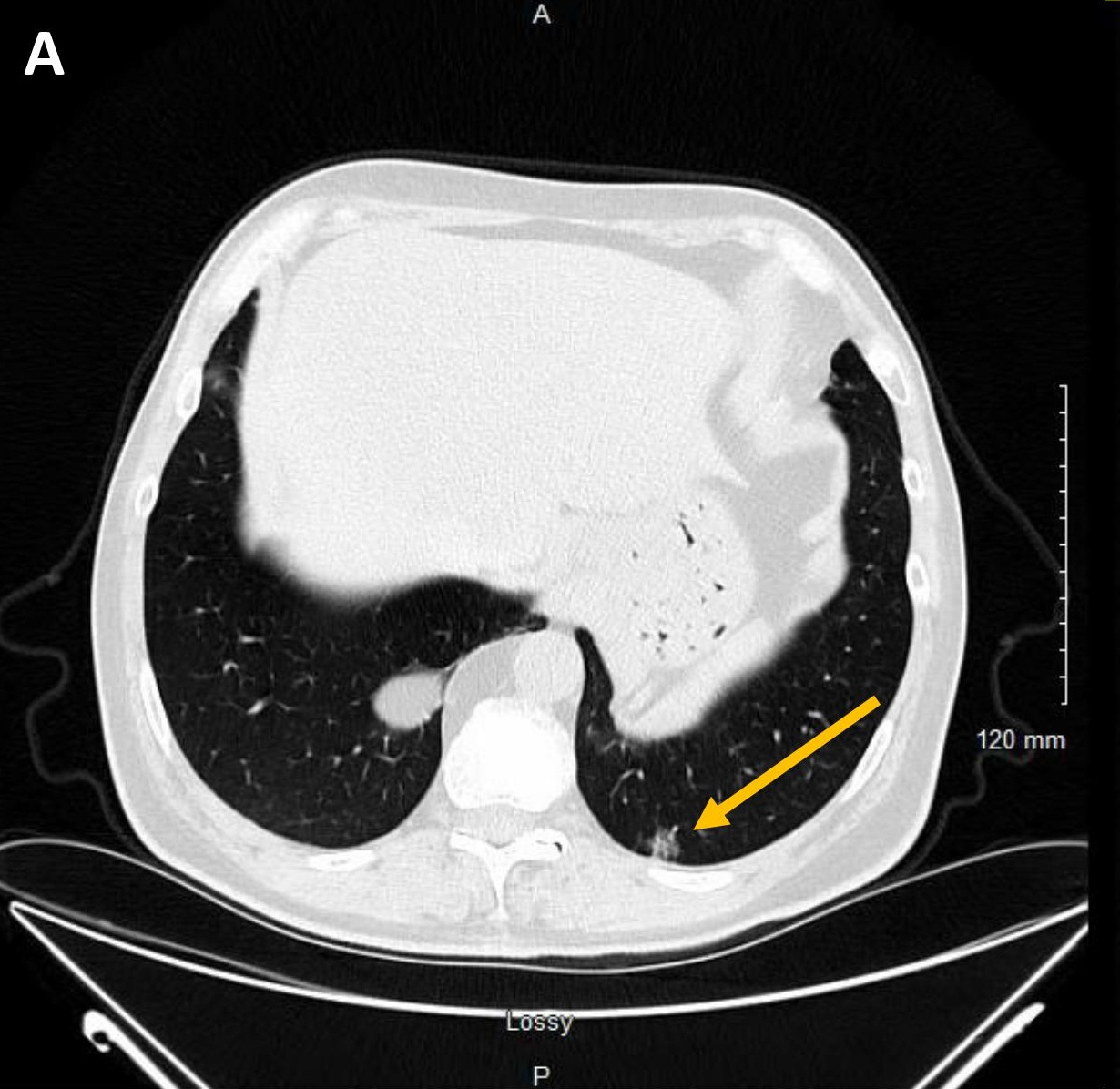
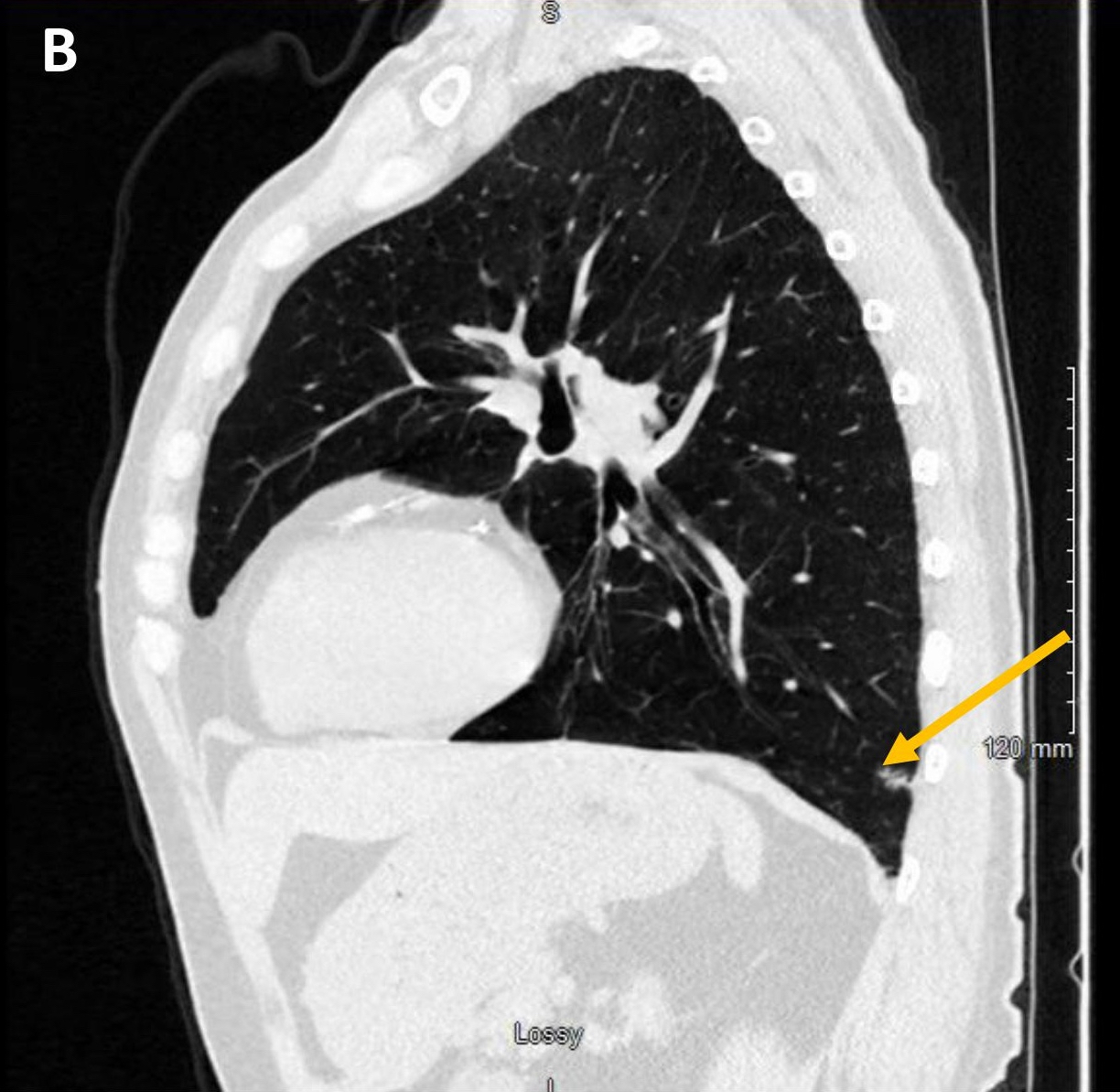
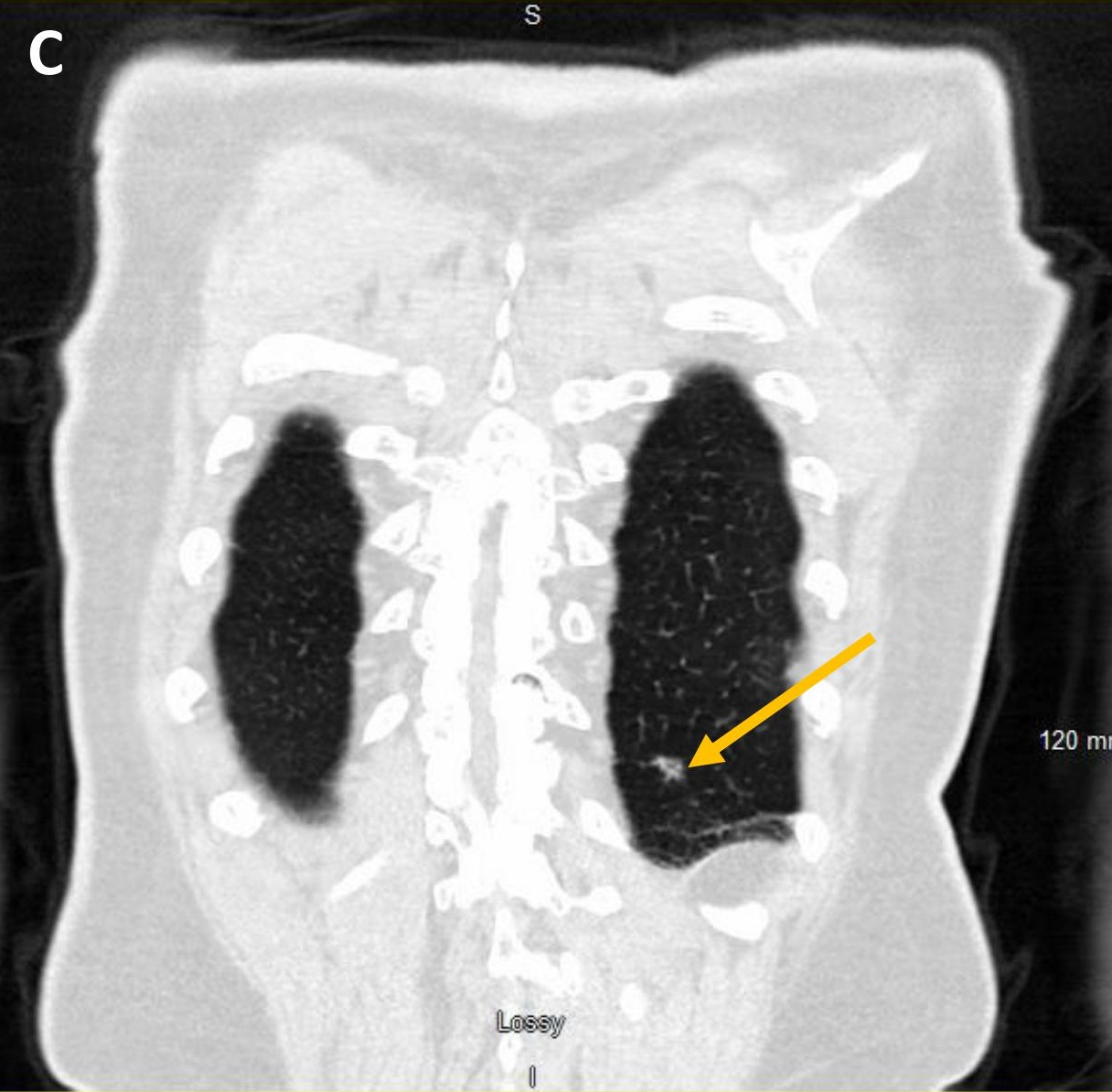
- They may appear as solid or ground glass nodules on computed tomography (CT), with some showing cavitation or cystic spaces (Am J Surg Pathol 2015;39:753, J Thorac Imaging 2002;17:163, Am J Surg Pathol 2018;42:1010)
- Definitive diagnosis requires excision and histopathologic evaluation
- Bronchial adenoma / ciliated muconodular papillary tumor
- Well circumscribed peripherally located nodules with papillary architecture
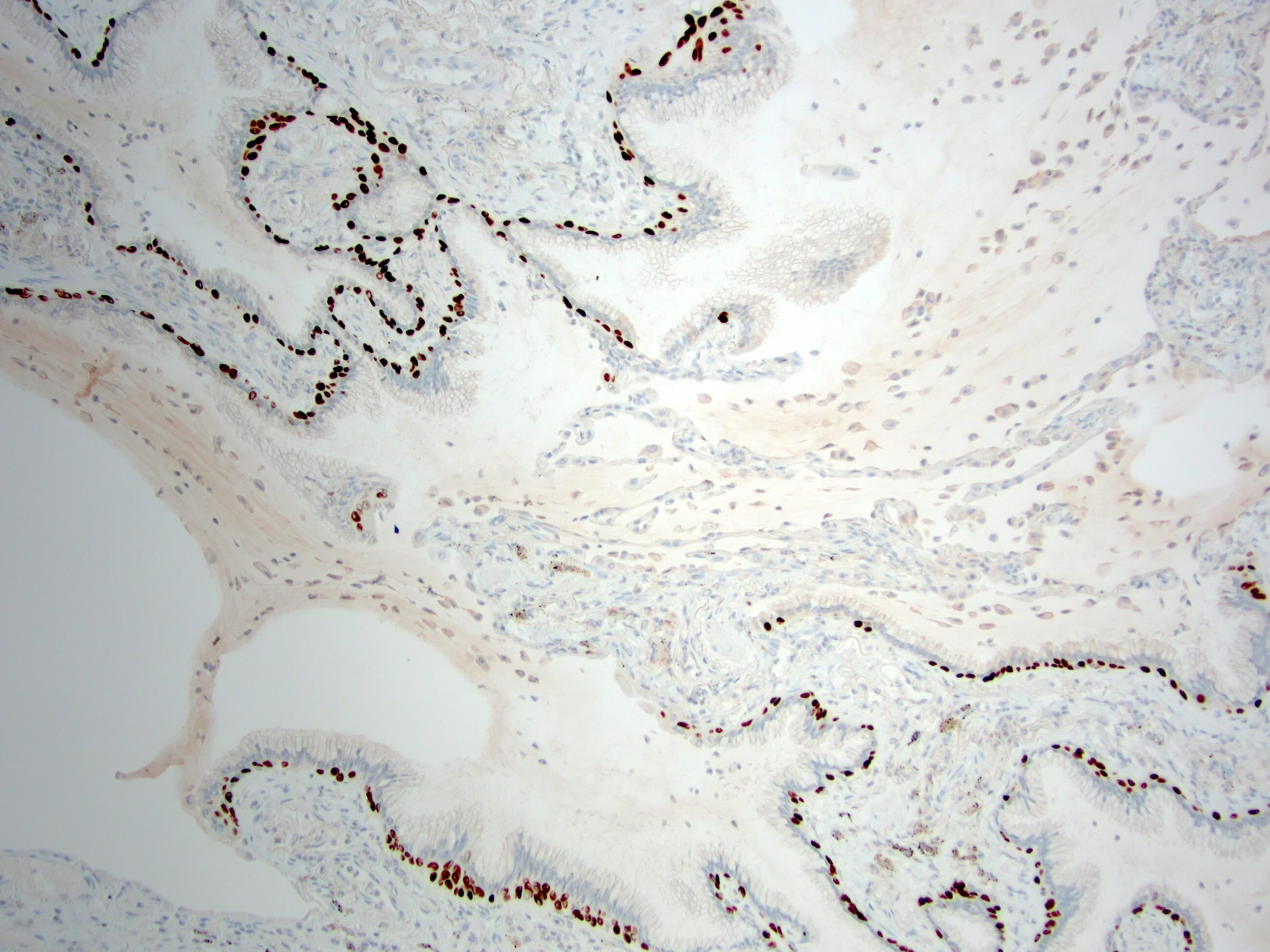
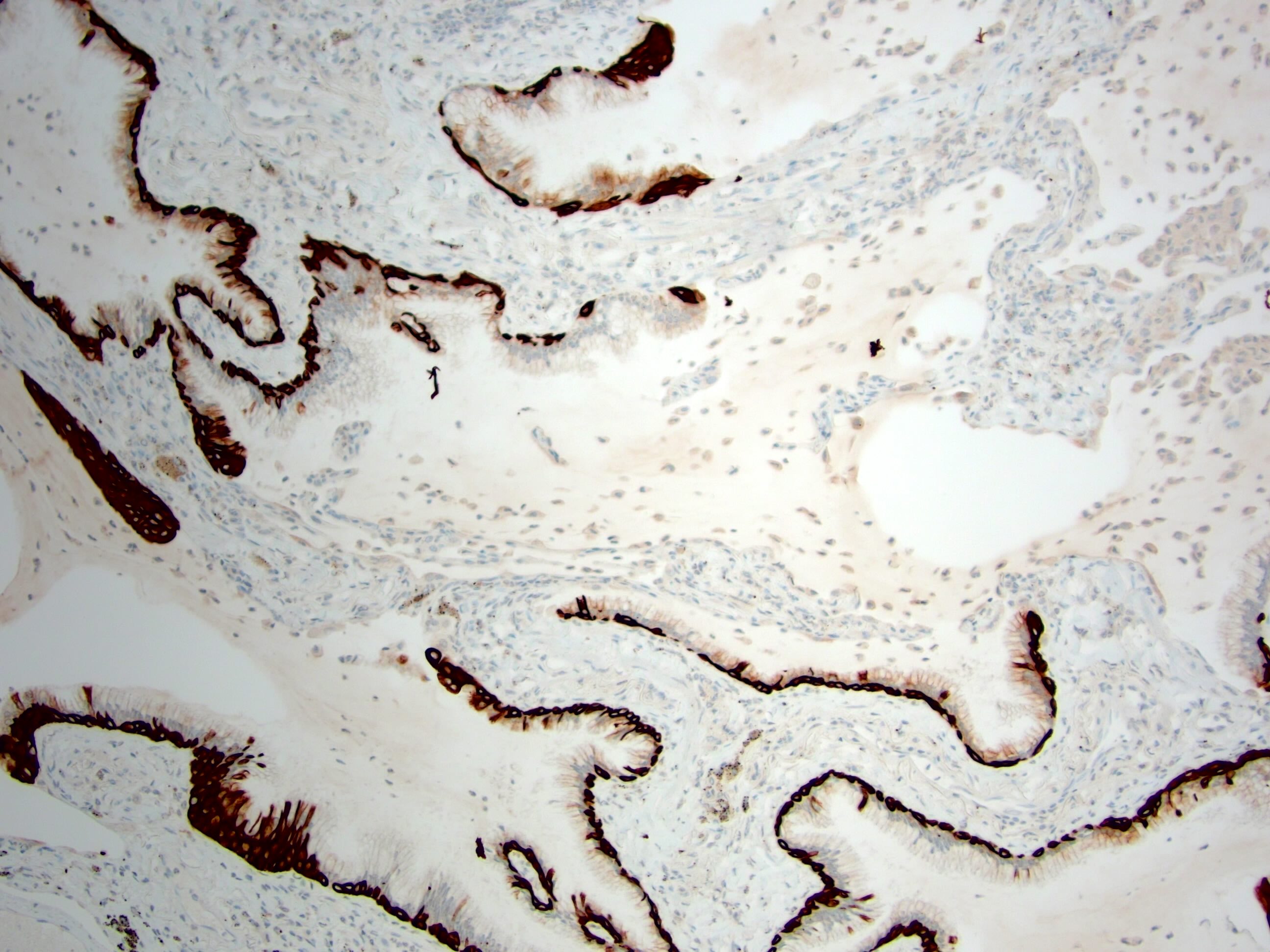
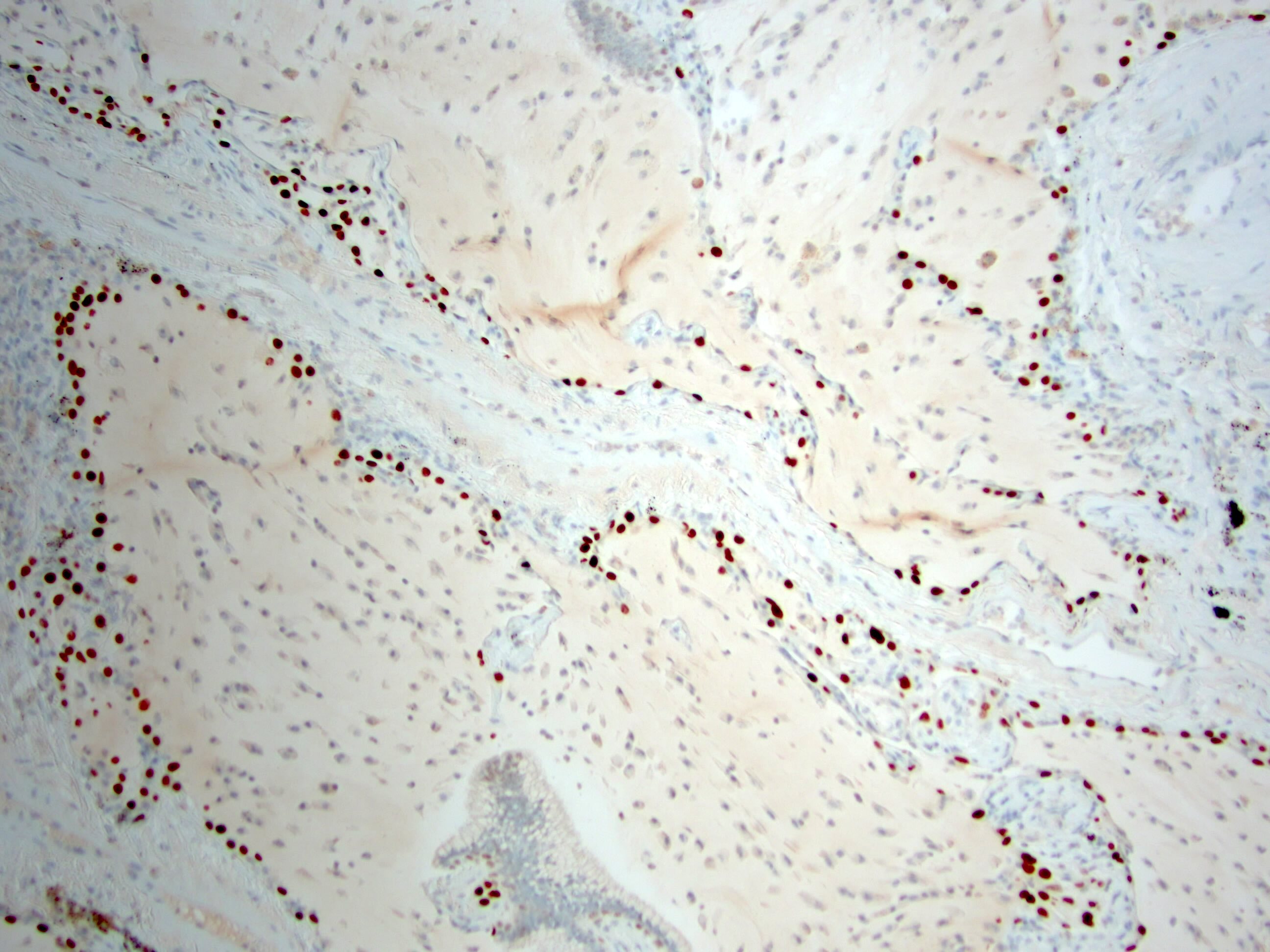
- Double layered cells, basal cells (p40 and CK5/6 positive) and luminal cells (TTF1: positive in distal type and negative or focal positive in proximal type)
- Lack of nuclear atypia and low proliferative index
- Associated with BRAF mutation
- Alveolar adenoma
- Multicystic mass with alveolus-like spaces
- Cysts are lined by a single layer of type II pneumocytes with bland cytology
- Mesenchymal stroma
- Papillary adenoma
- Circumscribed and not capsulated
- Papillary tumor with a single layer
- No cytological atypia / mitosis / necrosis / complex branching architecture
- TTF1 positive
- Mucinous cystadenoma of the lung
- Cystic mass with mucus contents
- Benign proliferation of mucous producing epithelial cells
- Mucous gland adenoma of the lung
- Well circumscribed endobronchial mass
- Acinar, tubular or papillary proliferation of cytologically bland mucous secreting cells
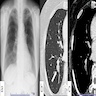
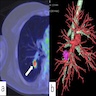
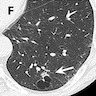
Radiology description
- Usually a solid, solitary, well circumscribed mass, which may rarely be calcified, cystic or cavitary (J Comput Assist Tomogr 2002;26:358, Respiration 2012;84:142, Radiat Med 2004;22:123, Clin Radiol 2011;66:708, Medicine (Baltimore) 2015;94:e498)
- Depending on the type of adenoma, the location would be central or peripheral
Radiology images
Prognostic factors
- Lung adenomas are mostly benign and surgical excision is curative (Arch Pathol Lab Med 2003;127:321, Am J Surg Pathol 2015;39:753, Hum Pathol 1999;30:158)
- Good prognosis, with no reported recurrence and metastasis (Am J Surg Pathol 2015;39:753, Am J Surg Pathol 2018;42:1010, Hum Pathol 2018;82:193)
Case reports
- 51 year old woman with 1.1 cm bronchial adenoma in the right upper lobe (Asian J Surg 2023;46:4090)
- 52 year old woman with incidental finding of a 1.2 cm subpleural alveolar adenoma in the right upper lobe, consisting of multiple cystic spaces filled with eosinophilic granular material and lined by flattened to cuboid epithelial cells without significant atypia (Pathologica 2022;114:326)
- 66 year old nonsmoking woman with a 3.7 cm lobulated irregular papillary adenoma in the posterior basal segment of the right lower lobe of the lung (Diagn Pathol 2022;17:81)
Treatment
- Surgical resection
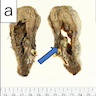
Gross description
- Bronchial adenoma is usually a well circumscribed white-gray nodule measuring 7 - 70 mm; cut surfaces can be solid, cystic or mucoid (Hum Pathol 1986;17:1066, Hum Pathol 1999;30:158, APMIS 2007;115:1443)
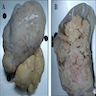
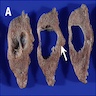
- Alveolar adenoma is a well circumscribed mass, which can have lobulated, multicystic pale yellow to tan cut surfaces
- Papillary adenoma may lack gross papillae or necrosis (J Bronchology Interv Pulmonol 2013;20:52, Am J Clin Pathol 1992;97:393)
- Although size range varies from 2 to 45 mm, these are most commonly 5 - 15 mm
- Mucinous cystadenoma usually consists of a mucin filled cyst, not associated with an airway; generally, cyst walls do not have a mural nodule
- Mucous gland adenomas are well circumscribed and majority of them arise within main, lobar or segmental bronchi; the cut surface is usually tan to gray with mucoid material (Am J Surg Pathol 1995;19:887)
Gross images
Frozen section description
- Bronchiolar adenoma on frozen sections is a mucinous neoplasm with 2 layers of basal and luminal cells
- There is minimal nuclear atypia present with no mitosis, necrosis or pleomorphism
- Presence of cilia in the luminal cells could be an important diagnostic clue for adenoma
- Multilayering can occasionally happen in proximal type bronchiolar adenoma along with basal cell hyperplasia (see Frozen section images), which can be confused for malignancy (Am J Surg Pathol 2023;47:431, Am J Surg Pathol 2015;39:753)
Frozen section images
Microscopic (histologic) description
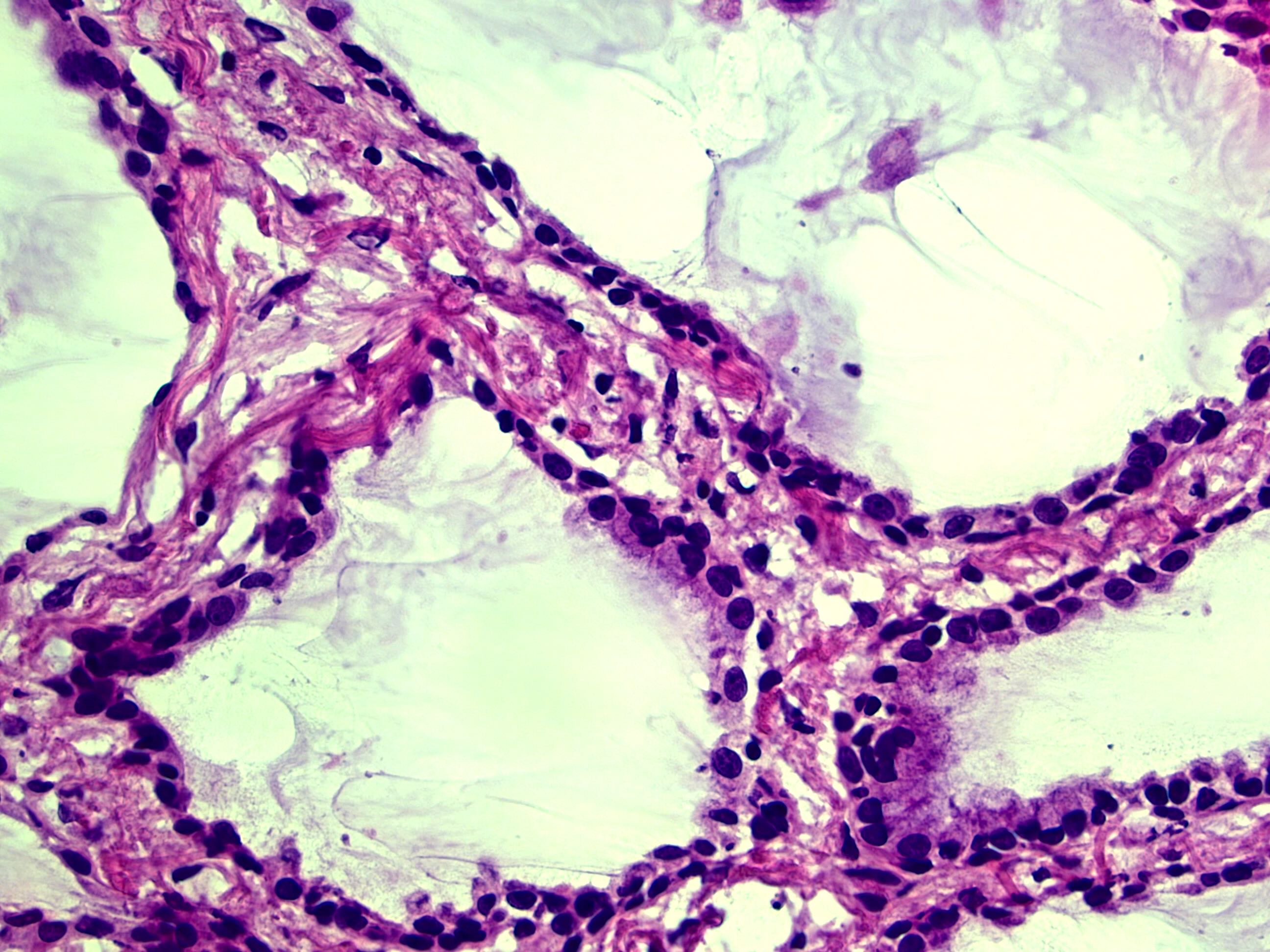
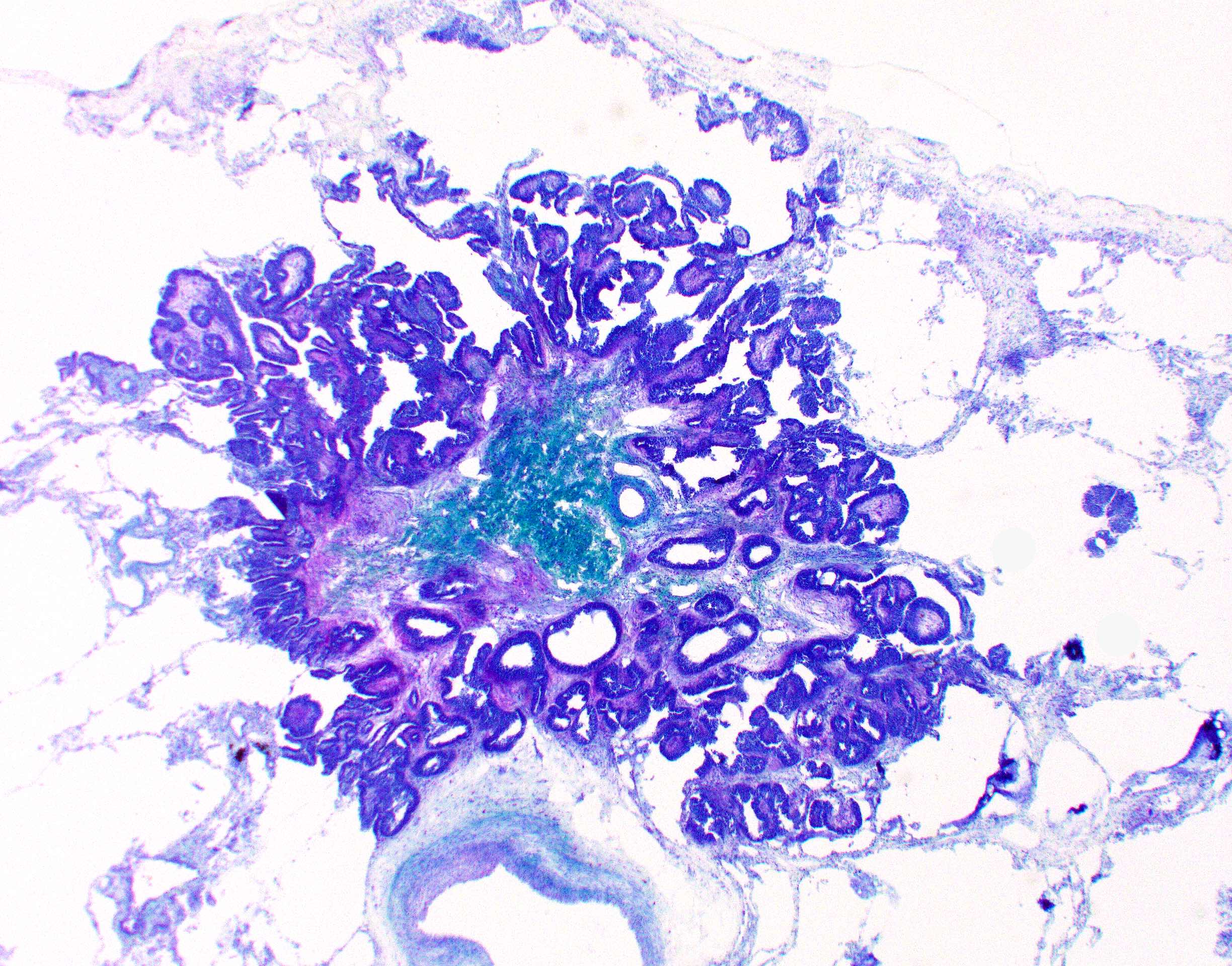
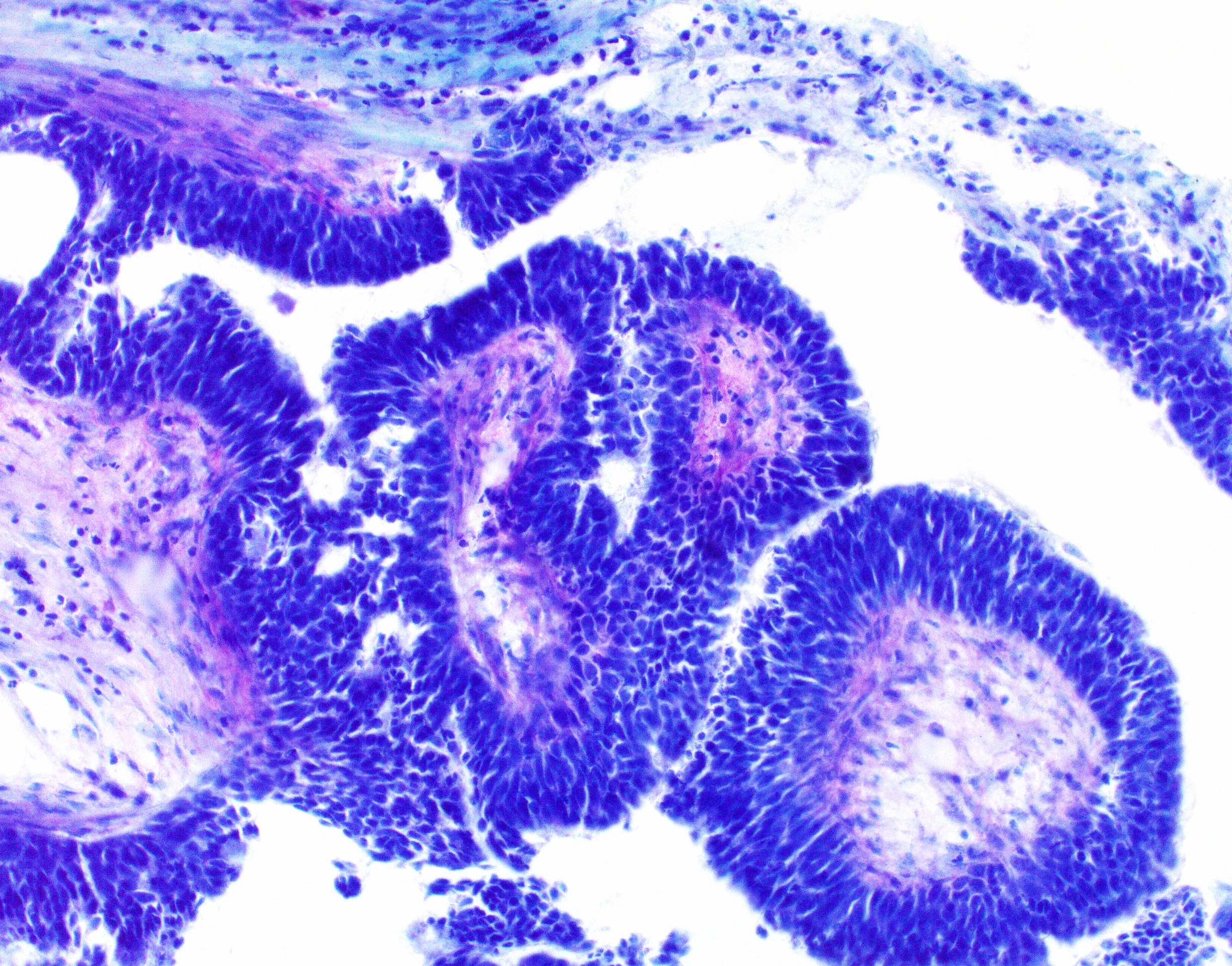
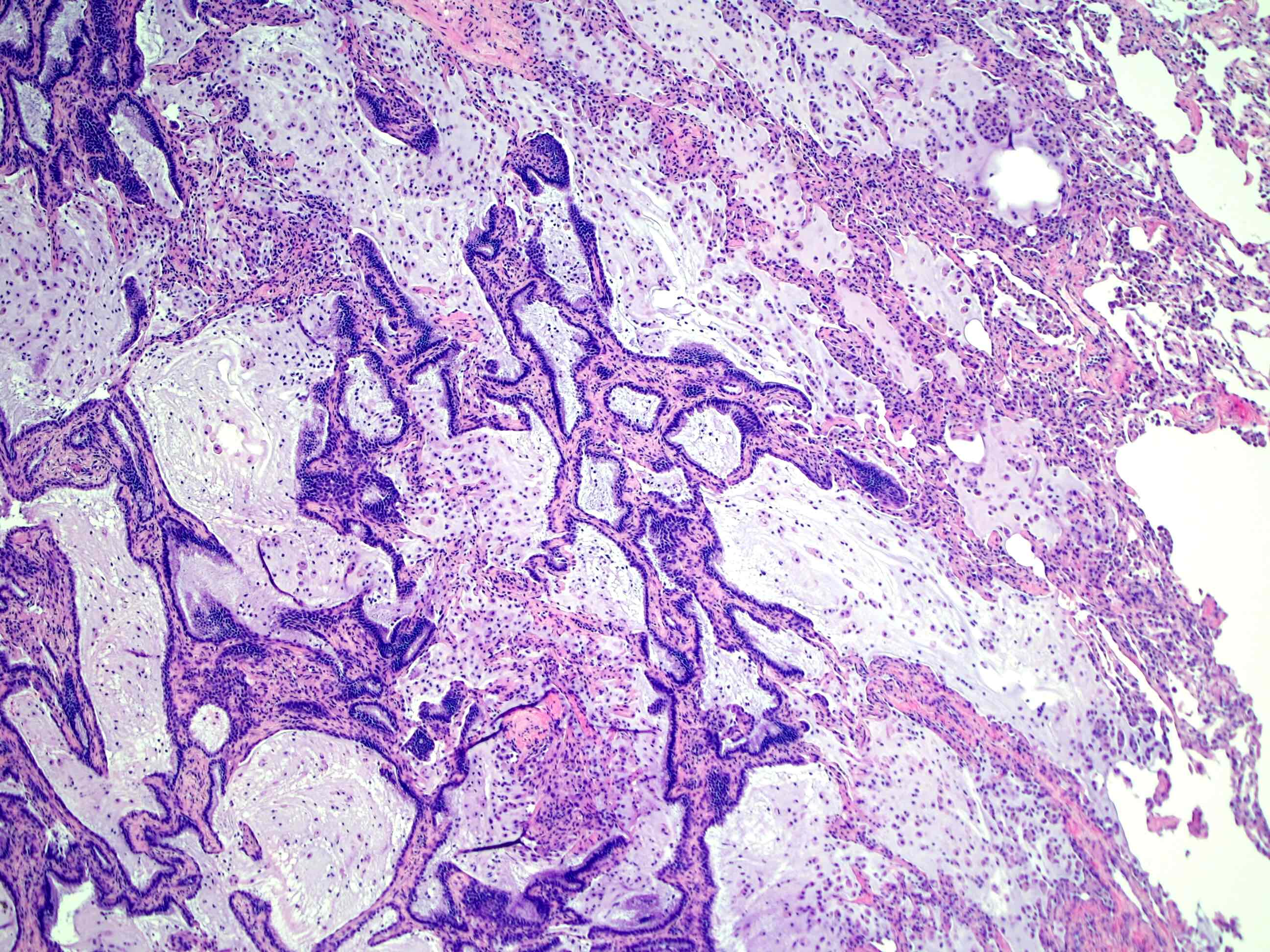
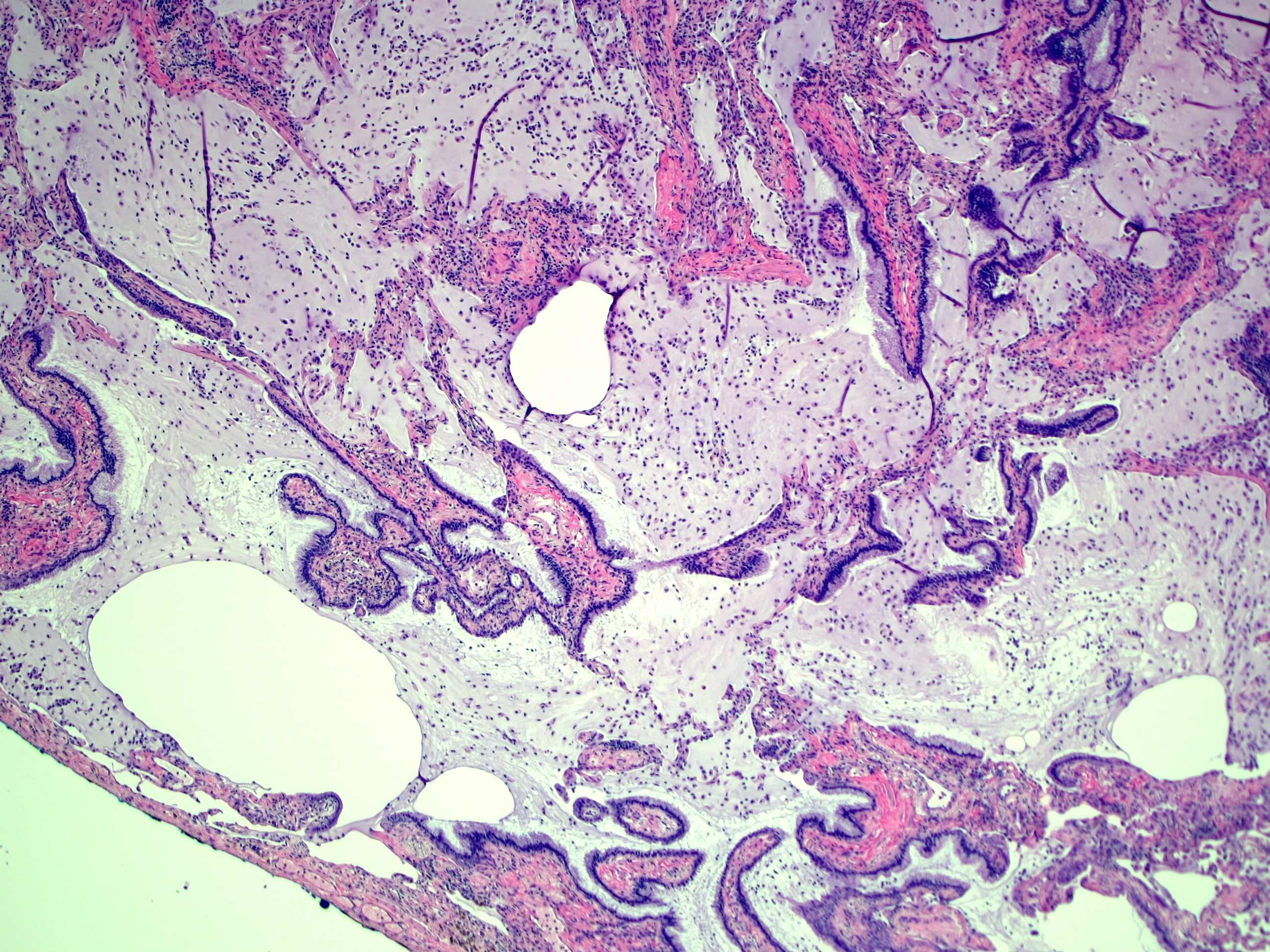
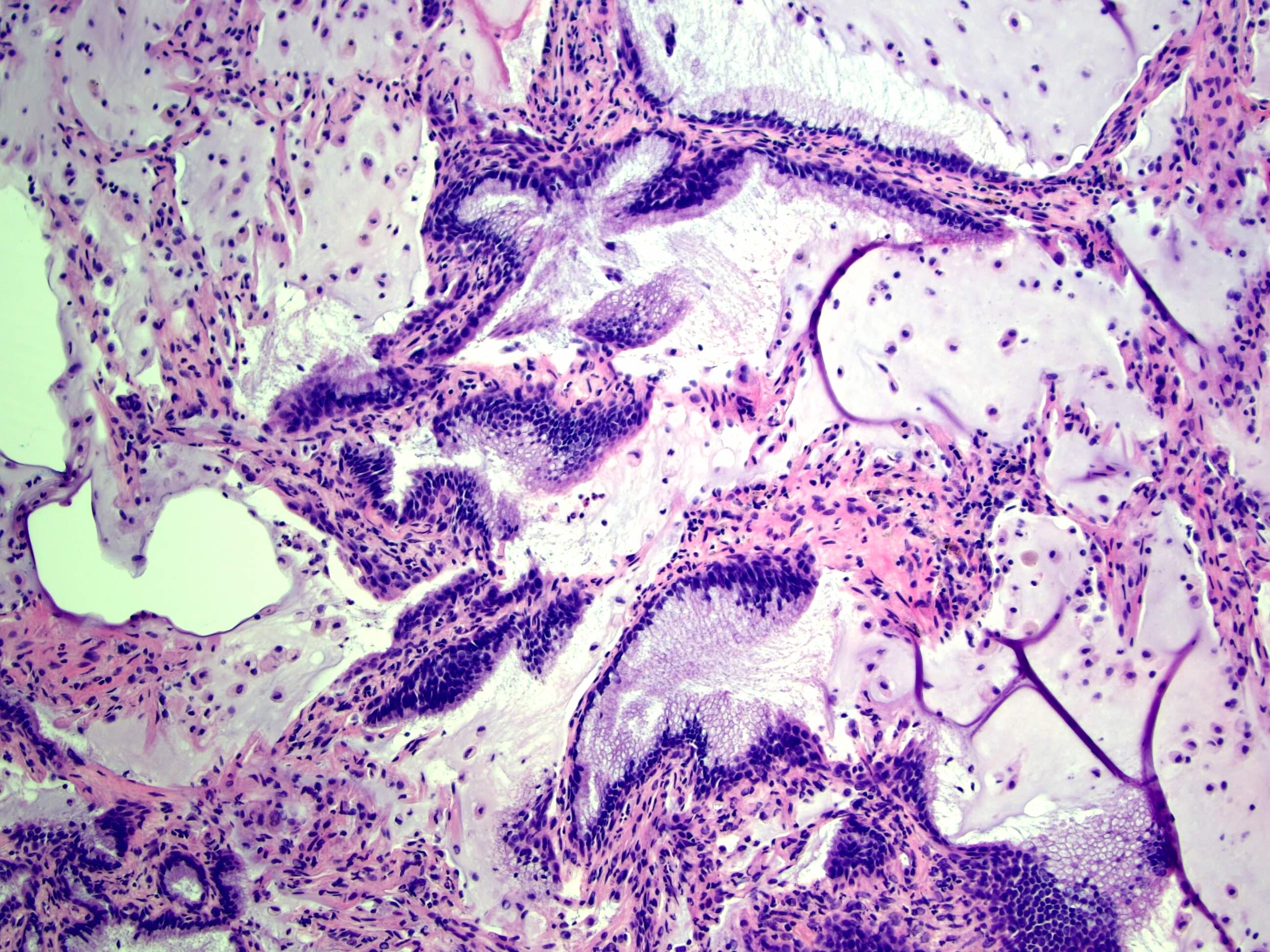
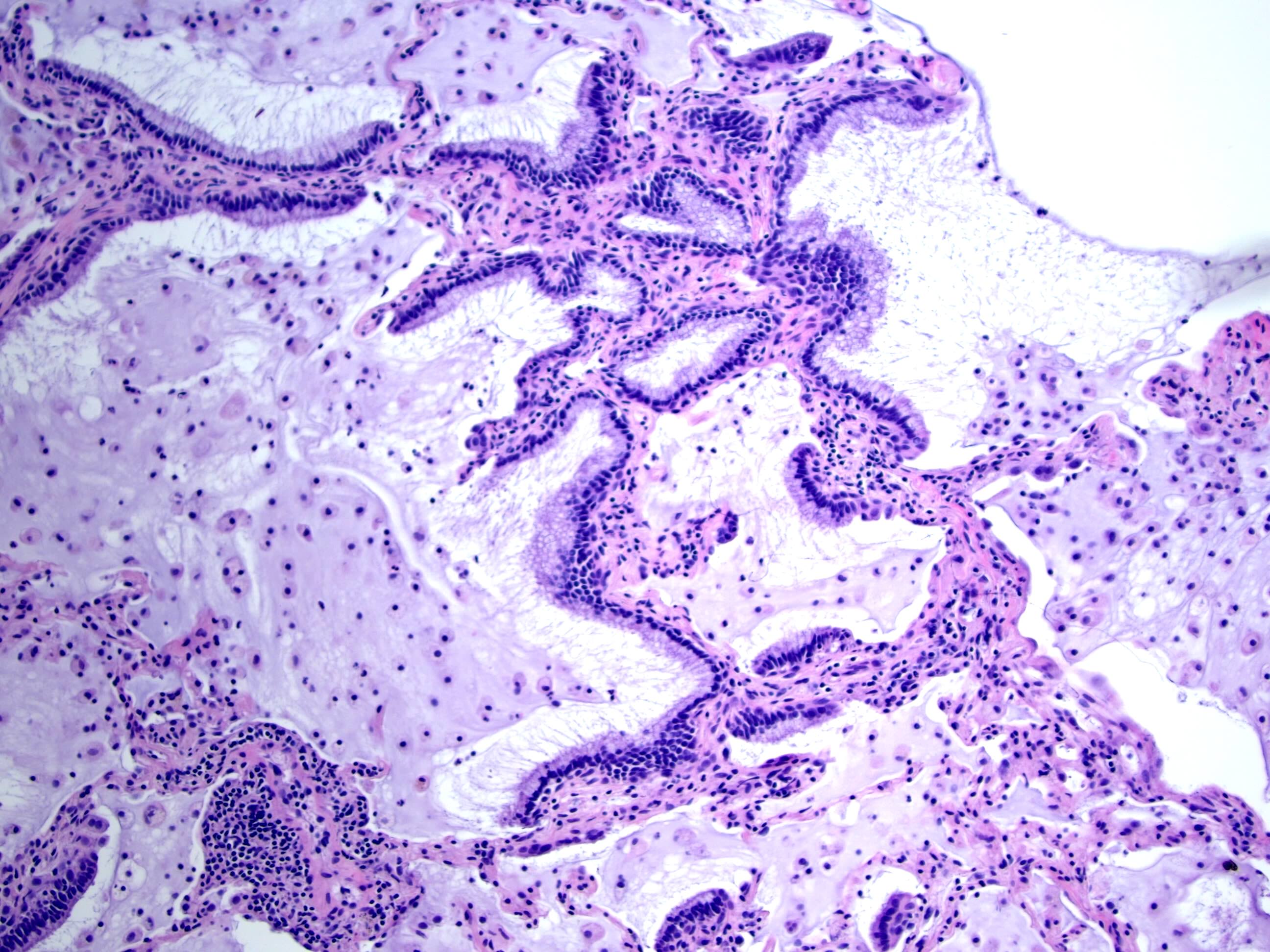
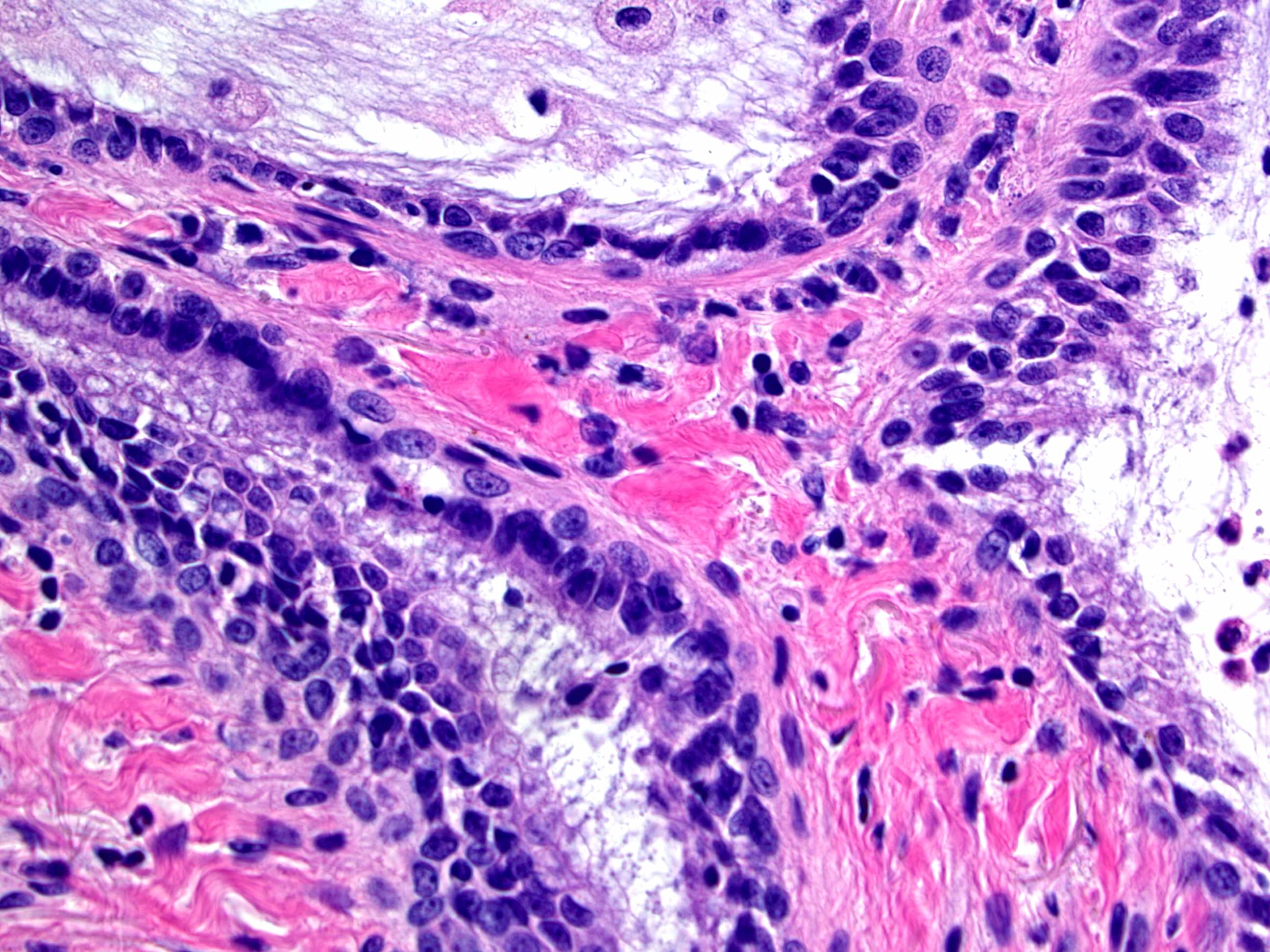
- Bronchiolar adenomas / ciliated muconodular papillary tumors are papillary or flat nodules, involving peribronchiolar lung tissue and composed of bilayer of continuous basal cells and luminal cells (comprising varying proportions of mucinous cells, ciliated cells, Clara cells or type II alveolar epithelial cells) (J Cardiothorac Surg 2019;14:143)
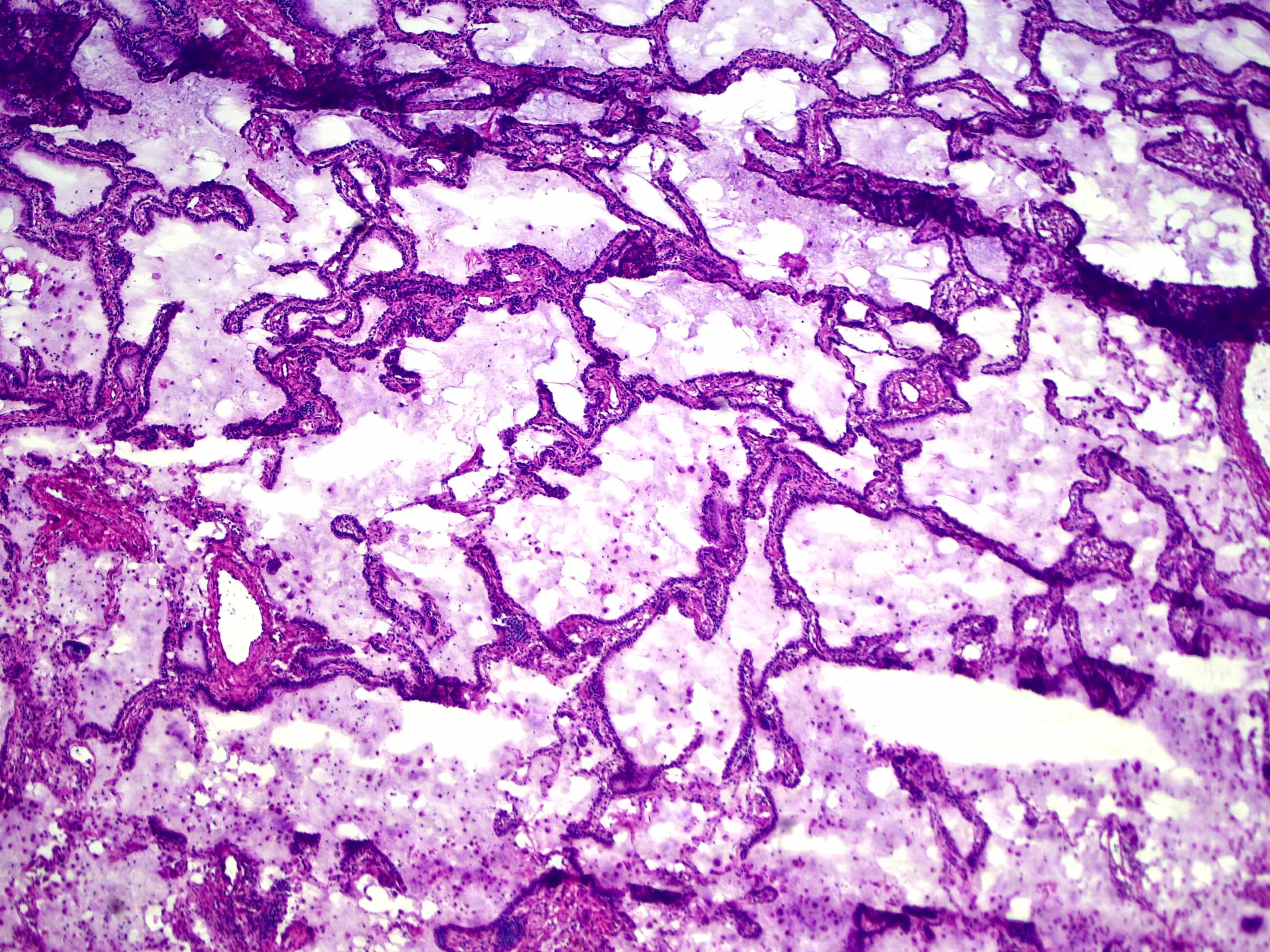
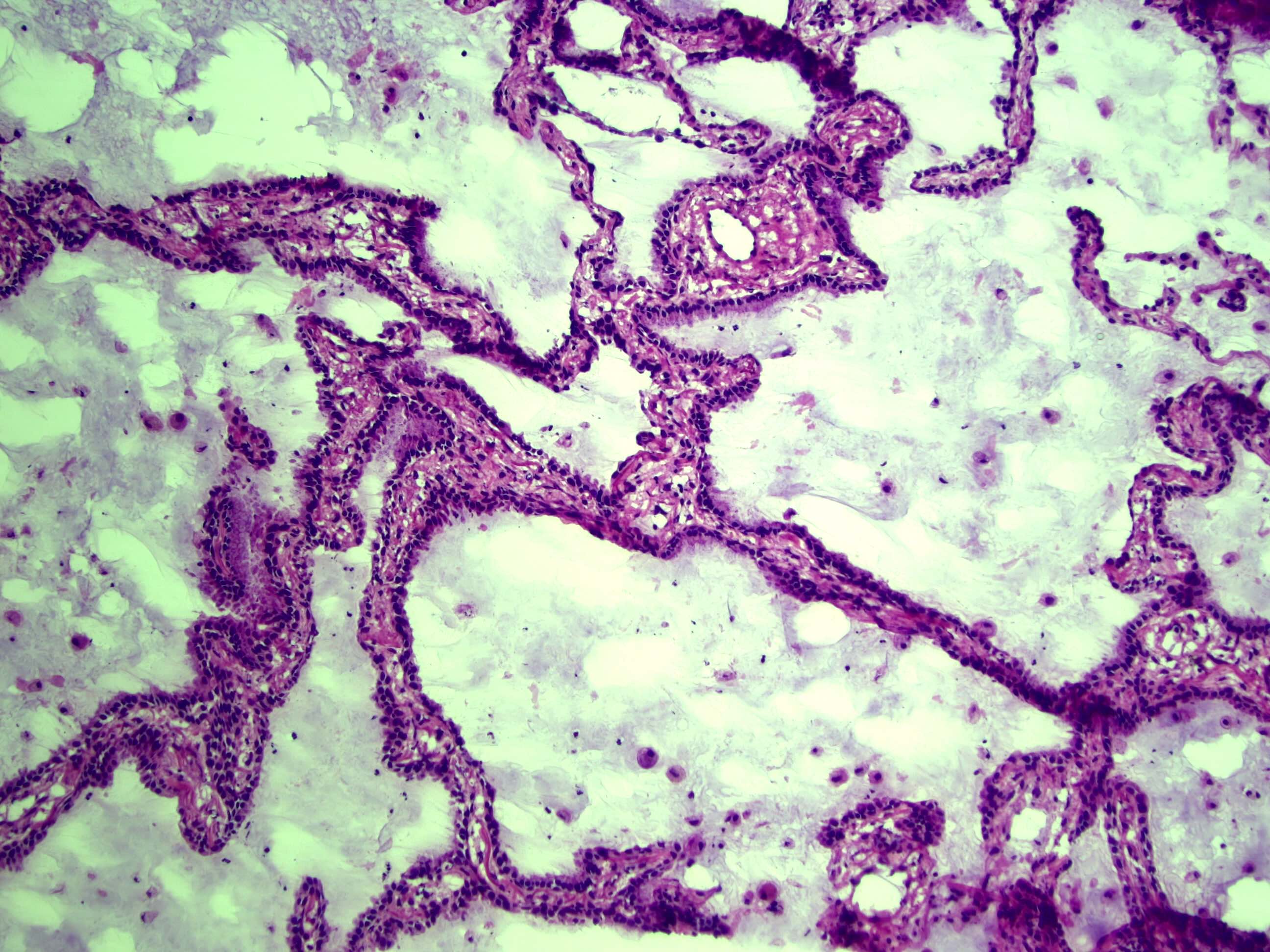
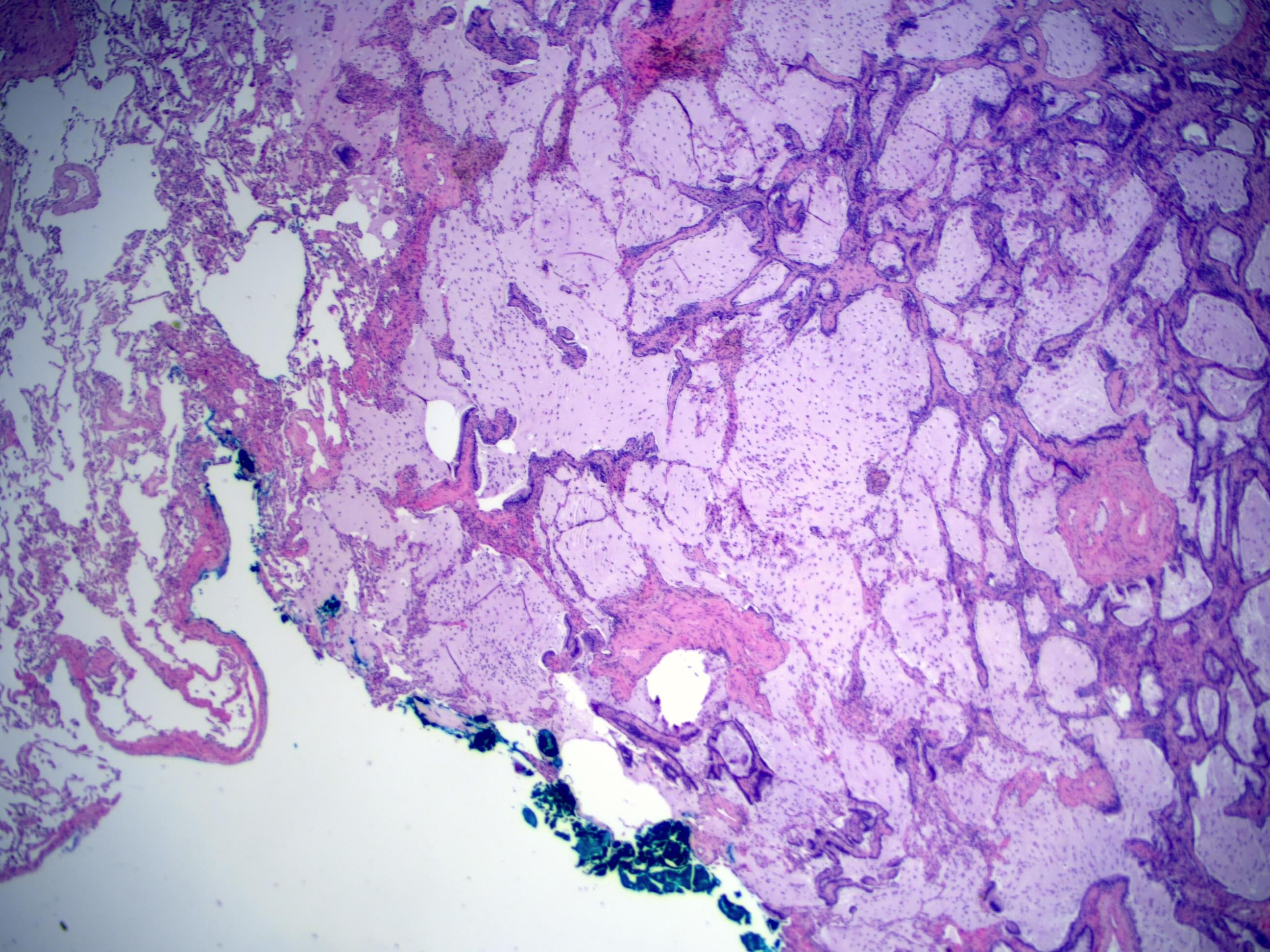
- Alveolar adenoma is comprised of multicystic spaces, filled with pulmonary eosinophilic surfactant; the cysts are lined by flattened to cuboidal epithelial cells, which correspond to type II pneumocytes
- Papillary adenomas are well defined papillary nodules with a fibrovascular core, lined by a single layer of cuboidal or ciliated epithelium (Acta Pathol Jpn 1992;42:56)
- Mucinous cystadenoma is a cyst lined by a discontinuous single layer of low cuboidal to tall columnar mucin secreting epithelial cells and mucinous contents
- Mucous gland adenoma is comprised of mucin filled cystic spaces, lined with bland columnar, cuboidal or flattened mucous secreting cells
Microscopic (histologic) images
Cytology description
- Bronchiolar adenoma / ciliated muconodular papillary tumor
- Columnar cells with cilia and mucous and extracellular mucin (Diagn Cytopathol 2019;47:716)
- Lacks nuclear atypia
- Papillary adenoma: papilla with bland epithelial cells with no nuclear atypia or pleomorphism (Diagn Cytopathol 2016;44:543)
Positive stains
- Bronchiolar adenoma / ciliated muconodular papillary tumor
- Alveolar adenoma
- Cyst lining epithelial cells are positive for cytokeratin, TTF1, Napsin A and surfactant protein
- Papillary adenoma: surface epithelial cells, positive for TTF1, CK7, pancytokeratin, surfactant protein and EMA
- Mucinous cystadenoma
- Epithelial cells positive for pancytokeratin
- Mucous gland adenoma: the epithelial cells are positive for EMA, keratin and CEA
Negative stains
- Neuroendocrine markers (chromogranin, synaptophysin) are negative
- Alveolar adenoma: stromal cells show focal staining for SMA and MSA and rare staining for S100 and CD34
- Alveolar adenoma and papillary adenoma: stromal cells are negative for keratin, TTF1
- Mucinous cystadenoma
- Rarely positive for CEA (Arch Pathol Lab Med 1990;114:1053)
- Epithelial cells negative for TTF1 and surfactant protein (Gen Thorac Cardiovasc Surg 2010;58:287, Arch Pathol Lab Med 1990;114:1053)
- Mucous gland adenoma: the epithelial cells are negative for TTF1
Sample pathology report
- Lung, left lower lobe, lobectomy:
- Benign bronchiolar adenoma / ciliated muconodular papillary tumor (BA / CMPT) (see comment)
- Size: 1.5 x 1.1 x 0.7 cm
- Resection margins: negative for tumor
- Comment: On histology, sections show papillary architecture and are composed of bilayered cells, luminal epithelial cells and continuous basal cells. The luminal cells consist of mucous cells and focal ciliated cells. Luminal cells are predominantly negative for TTF1 and CDX2. Immunostain for CK5/6 and p63 shows a continuous basal cell layer in the lesion. These features support the diagnosis.
- Lung, right upper lobe, biopsy:
- Papillary neoplasm of lung, favor papillary adenoma (see comment)
- Comment: Sections show fragments of papillae with fibrovascular cores, lined with a single layer of cuboidal epithelium without nuclear atypia, pleomorphism or prominent nucleoli. The lesional cells express TTF1 and have a low Ki67 proliferative index (< 1%). The definitive diagnosis is deferred to the complete excisional specimen.
Differential diagnosis
- Bronchiolar adenoma / ciliated muconodular papillary tumor:
- Mucinous adenocarcinoma:
- Peribronchiolar metaplasia:
- Ill defined borders and is usually a multifocal process, often in the setting of interstitial lung disease or small airway injury
- Alveolar adenoma:
- Adenocarcinoma in situ:
- No continuous basal cell layer or ciliated cells
- Presence of nuclear atypia
- Very difficult to differentiate on frozen sections or small biopsies (Am J Clin Pathol 2021;155:832)
- Lymphangioma:
- Cytokeratin and TTF1 staining of the pneumocytes differentiates alveolar adenoma from lymphangioma, where the endothelial cells are keratin negative and D2-40 positive
- Adenocarcinoma in situ:
- Mucinous cystadenoma:
- Colloid carcinoma of the lung:
- Invasive adenocarcinoma with large pools of mucin destroying alveolar walls, which must be present in at least 50% of the tumor
- Metastatic carcinoma from the gastrointestinal tract or ovary:
- Generally multiple, well circumscribed and tend to grow rapidly
- A history of and a panel of immunohistochemical stains can help support the diagnosis
- Bronchogenic cysts:
- Unilocular cyst lined by respiratory type epithelium
- Cyst wall recapitulates bronchial wall with variable amounts of seromucinous glands, cartilage and smooth muscle
- Colloid carcinoma of the lung:
- Mucous gland adenoma:
- Endobronchial metastasis:
- Lesional cells with atypia
- Invasive mucinous adenocarcinoma:
- Involves the alveolar parenchyma
- No exclusive endobronchial growth
- Low grade mucoepidermoid carcinoma:
- Mixture of mucous cells, squamous cells and intermediate cells
- MAML mutation
- Endobronchial metastasis:
Additional references
Practice question #1
Practice answer #1
D. Proliferation of basal cell layer and luminal cells layer. Bronchial adenomas are usually clinically silent well circumscribed peripherally located nodules with papillary architecture, consisting of basal cells and proliferating luminal cells. These lesions lack nuclear atypia and have a low proliferative index. Answer A is incorrect because bronchial adenomas are commonly seen in middle aged to elderly patients. Answer C is incorrect because bronchial adenomas are well circumscribed. Answer B is incorrect because bronchial adenomas are usually cytologically bland.
Comment Here
Reference: Adenoma
Comment Here
Reference: Adenoma
Practice question #2
What is the most common mutation in bronchiolar adenoma / ciliated muconodular papillary tumor?
- ALK
- BRAF
- ERG
- RB1
Practice answer #2
B. BRAF. The most common mutation in bronchial adenoma is BRAF V600E, followed by EGFR exon 19 deletions, exon 20 insertions and KRAS mutations. Answers A, C and D are incorrect because those mutations are not common in bronchial adenomas.
Comment Here
Reference: Adenoma
Comment Here
Reference: Adenoma