Table of Contents
Definition / general | Essential features | ICD coding | Epidemiology | Sites | Pathophysiology | Etiology | Clinical features | Diagnosis | Laboratory | Radiology description | Prognostic factors | Case reports | Treatment | Gross description | Frozen section description | Microscopic (histologic) description | Microscopic (histologic) images | Positive stains | Negative stains | Electron microscopy description | Molecular / cytogenetics description | Sample pathology report | Differential diagnosis | Additional references | Practice question #1 | Practice answer #1 | Practice question #2 | Practice answer #2Cite this page: Reyes F, Skala SL. Microcystic stromal tumor. PathologyOutlines.com website. https://www.pathologyoutlines.com/topic/ovarytumormicrocysticstromal.html. Accessed September 25th, 2025.
Definition / general
- Ovarian stromal tumor with variable microcystic morphology
Essential features
- Ovarian stromal tumor with variably prominent microcystic pattern and regions with lobulated cellular masses separated by hyalinized fibrous stroma
- Aberrant nuclear or cytoplasmic localization of beta catenin
- Rare extracolonic manifestation of familial adenomatous polyposis
ICD coding
- ICD-O: 8590/0 - microcystic stromal tumor
- ICD-11: 2F76 & XH35B3 - neoplasms of uncertain behavior of female genital organs & microcystic stromal tumor
Epidemiology
- Mean age of 45 years (range of 26 - 63 years) (Am J Surg Pathol 2009;33:367)
- May rarely occur as a manifestation of familial adenomatous polyposis (Genes Chromosomes Cancer 2015;54:353, Am J Surg Pathol 2018;42:137, Int J Gynecol Pathol 2016;35:561)
Sites
- Ovary
Pathophysiology
- Presumed to arise from ovarian stromal cells
- Mutually exclusive mutations in CTNNB1 and APC result in aberrant nuclear immunoreactivity for beta catenin and cyclin D1 through activation of the Wnt / beta catenin signaling pathway (Histopathology 2020;76:11)
Etiology
- May rarely occur as a manifestation of familial adenomatous polyposis (Genes Chromosomes Cancer 2015;54:353, Am J Surg Pathol 2018;42:137, Int J Gynecol Pathol 2016;35:561)
Clinical features
- Pelvic mass
- Hormonal manifestations are usually absent (Am J Surg Pathol 2009;33:367)
Diagnosis
- WHO diagnostic criteria
- Essential: stromal neoplasm with variable microcystic morphology
- Desirable
- Diffuse nuclear beta catenin and cyclin D1 immunoreactivity
- Lack of expression of inhibin and calretinin
- Reference: Am J Surg Pathol 2009;33:367
Laboratory
- No specific laboratory findings
Radiology description
- Solid cystic mass with low resistance internal vascularity on ultrasound (Int J Gynaecol Obstet 2024;167:455)
Prognostic factors
- Outcome has been uneventful in most reported cases
- Pelvic recurrence has been reported (4 - 9 years after initial diagnosis) (Hum Pathol 2018;78:171, Int J Gynecol Pathol 2023;42:491)
- Omental and peritoneal involvement / metastasis has been described (Int J Gynecol Pathol 2023;42:491, J Ovarian Res 2021;14:73)
Case reports
- 27 year old pregnant woman with ovarian microcystic stromal tumor with predominant bizarre nuclei coexisting with mucinous cystadenoma (Case Rep Pathol 2022;2022:8457901)
- 33 year old woman with bilateral ovarian recurrence of previously treated microcystic stromal tumor (Hum Pathol 2018;78:171)
- 40 year old woman with ovarian microcystic stromal tumor and familial adenomatous polyposis (Genes Chromosomes Cancer 2015;54:353)
- 45, 56, 61 and 71 year old women with variant morphology of microcystic stromal tumor (Histopathology 2019;74:443)
- 47 year old woman with omental metastasis of ovarian microcystic stromal tumor (J Ovarian Res 2021;14:73)
Treatment
- Complete resection is typically curative, though rare recurrences and metastasis have been reported
Gross description
- Usually unilateral
- Typically < 10 cm; range of 2 - 27 cm (Am J Surg Pathol 2009;33:367, Am J Surg Pathol 2015;39:1420)
- Well demarcated solid to cystic tumor; solid component with tan-white cut surfaces, cysts with tan-pink lining (Int J Gynaecol Obstet 2024;167:455)
- Foci of hemorrhage or necrosis may be present
Frozen section description
Microscopic (histologic) description
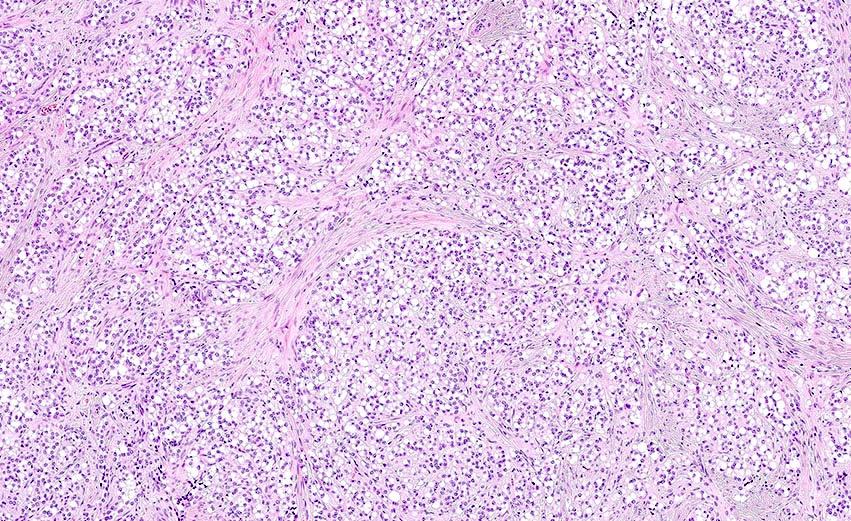
- Distinctive triad of histologic features (Histopathology 2022;80:898)
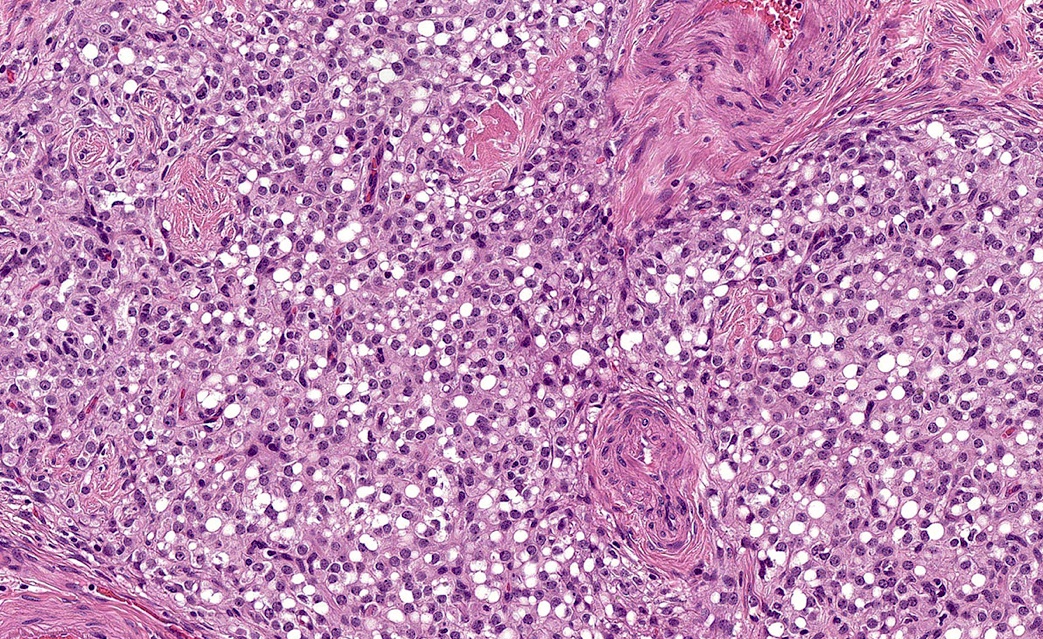
- Microcysts: small, round / oval, cystic spaces that may coalesce into larger irregular channels, sometimes with eosinophilic or basophilic contents (Virchows Arch 2017;470:225)
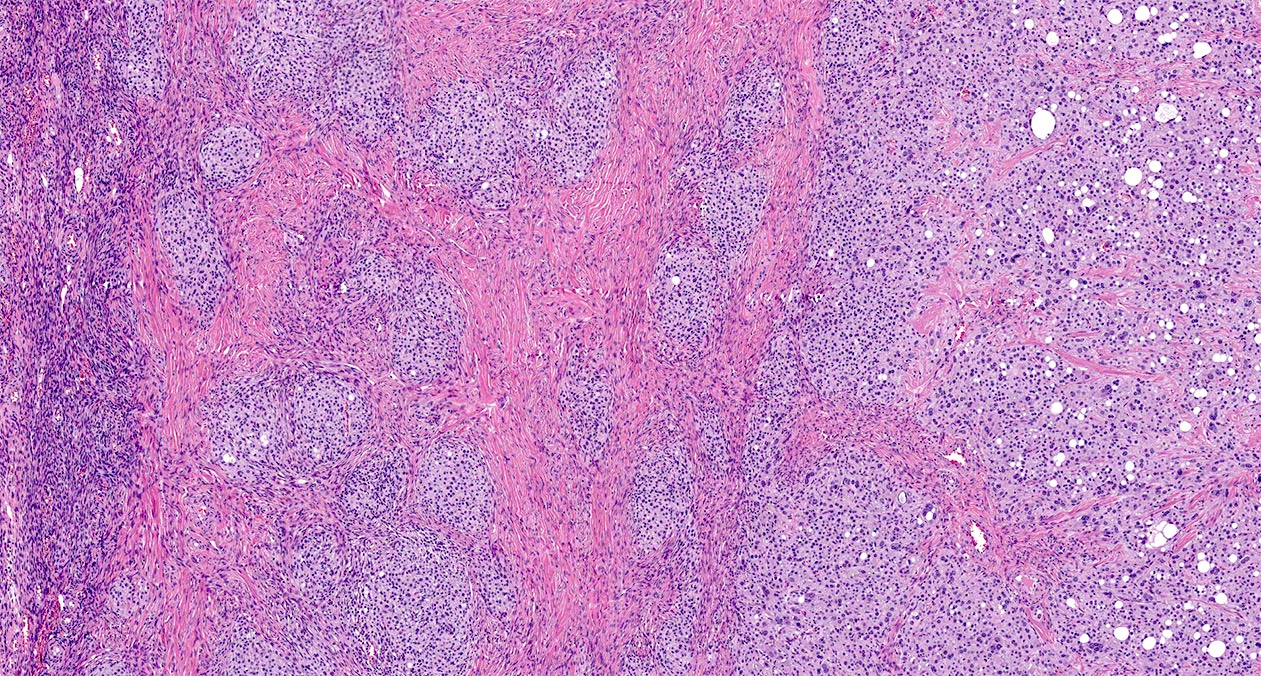
- Solid cellular regions
- Hyalinized hypocellular fibrous stroma
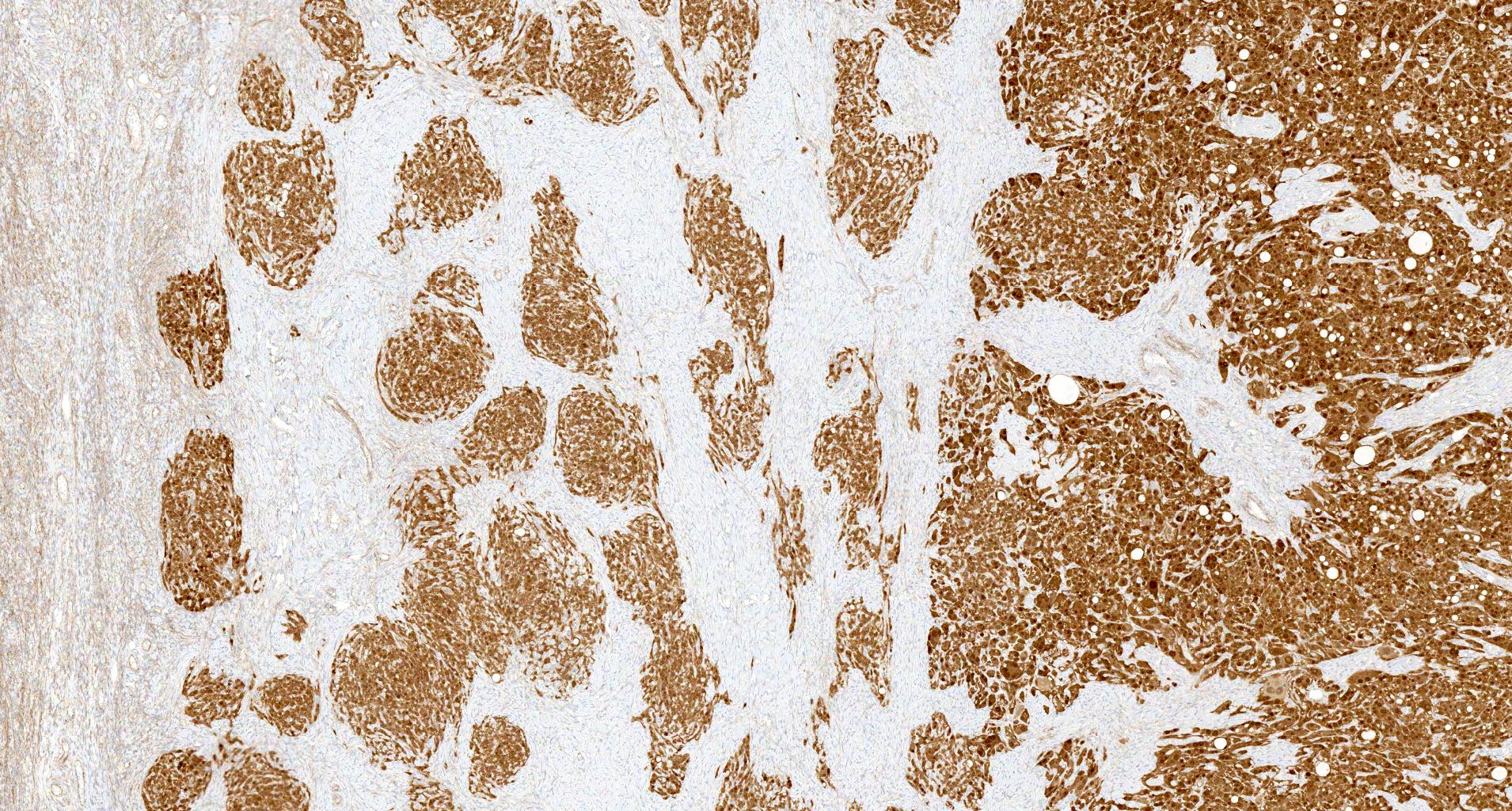
- Multinodular growth with fibrous, hyalinized or myxoid stroma separating nodules (Virchows Arch 2017;470:225)
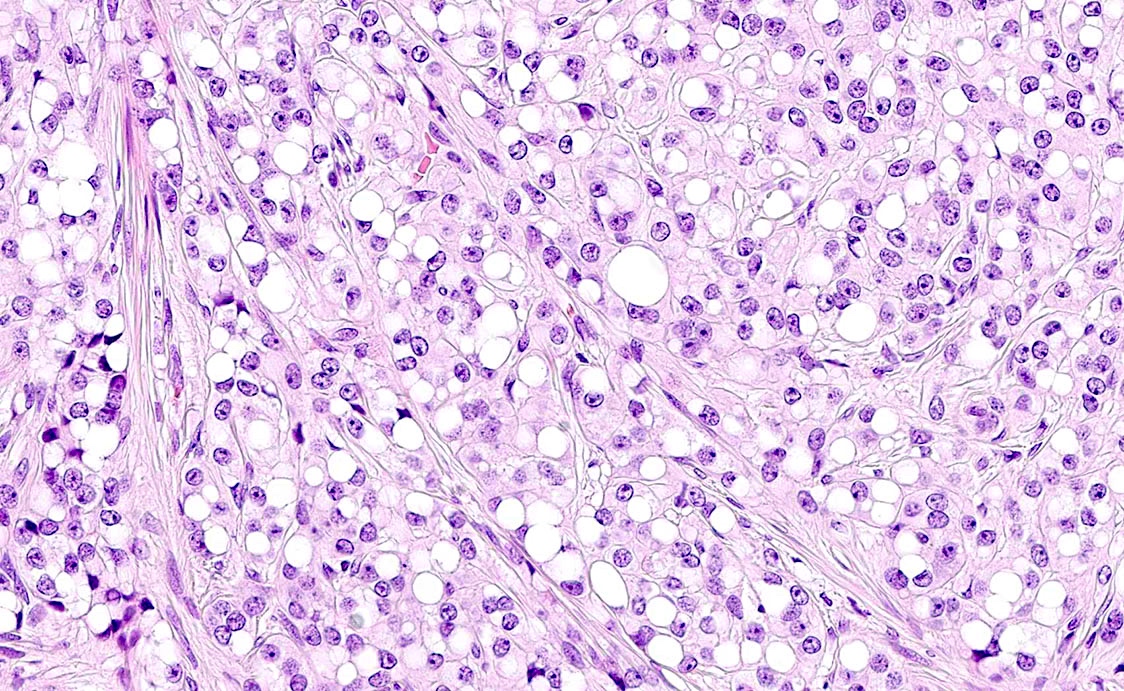
- Cells have a moderate amount of finely granular eosinophilic cytoplasm, bland round / oval nuclei with fine chromatin and indistinct nucleoli (Histopathology 2019;74:443, Front Med (Lausanne) 2020;7:58)
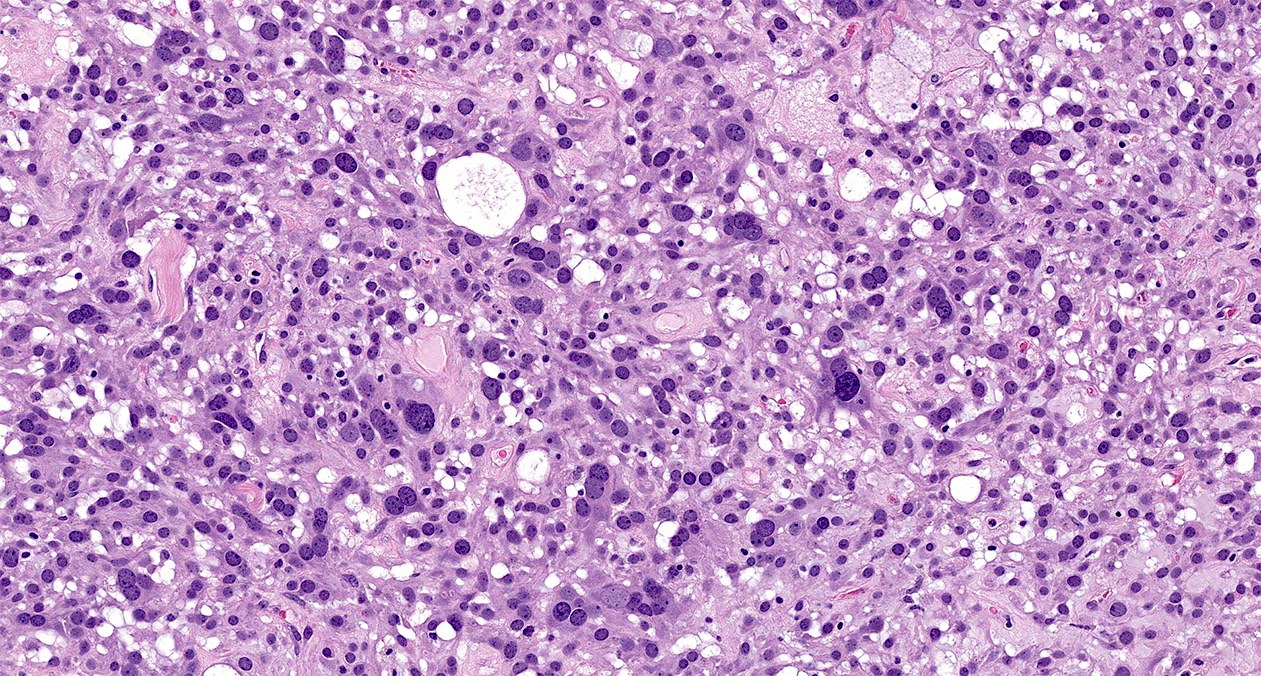
- Multinucleation or enlarged hyperchromatic bizarre nuclei may be seen (Case Rep Pathol 2022;2022:8457901)
- Intracytoplasmic vacuoles are frequently present, sometimes with signet ring morphology (Histopathology 2022;80:898)
- Low mitotic rate (Histopathology 2022;80:898)
- Less common features
- Psammomatous calcifications or osseous metaplasia may be seen in rare cases (Histopathology 2022;80:898)
- Diffuse, nested, tubular, corded or spindle cell growth, sometimes lacking areas with classical morphology (Histopathology 2022;80:898, Histopathology 2019;74:443)
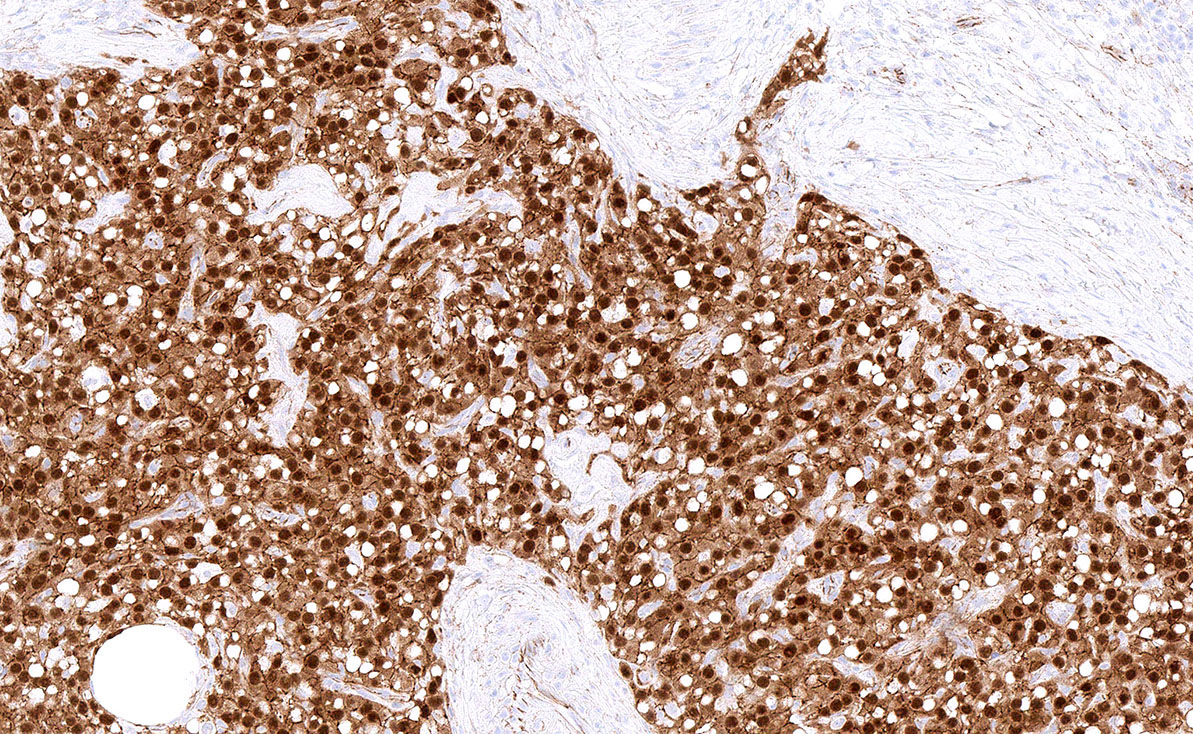
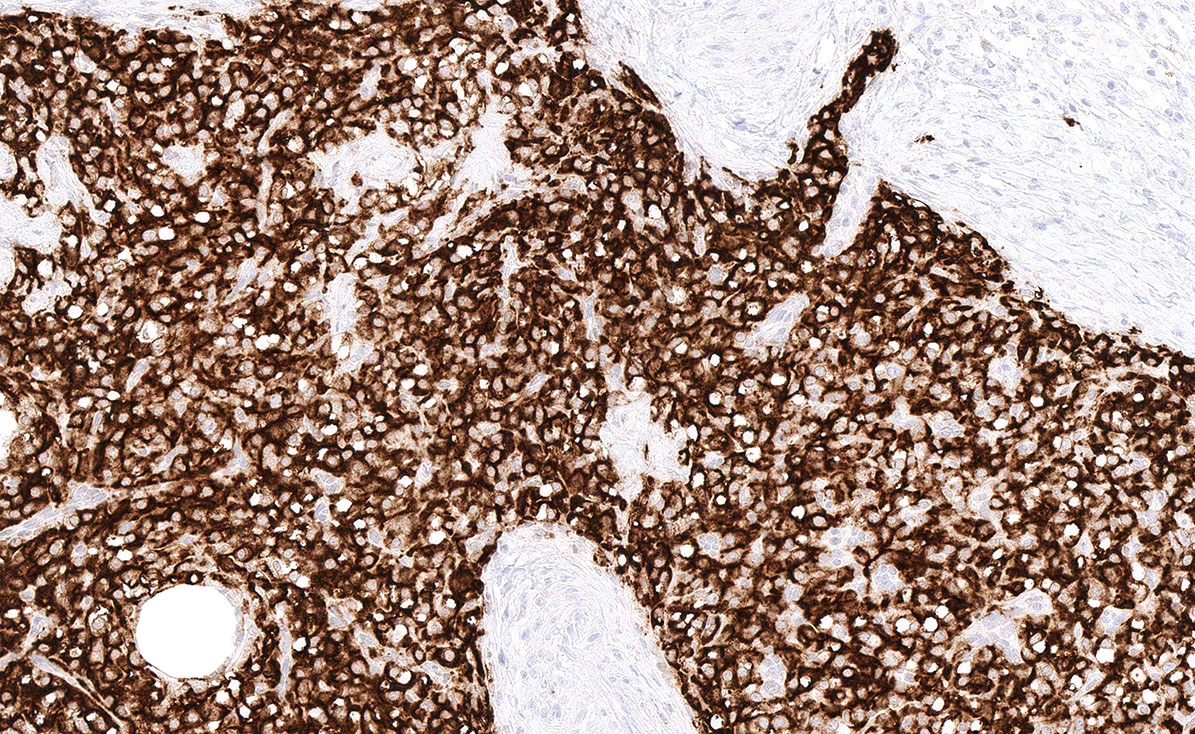
Microscopic (histologic) images
Positive stains
- Beta catenin: aberrant nuclear or cytoplasmic localization (Histopathology 2020;76:11)
- Cyclin D1: diffuse nuclear reactivity (Histopathology 2022;80:898)
- CD10 (Histopathology 2019;74:443)
- WT1 (Histopathology 2019;74:443)
- SF1 (Histopathology 2022;80:898)
- Androgen receptor (Histopathology 2022;80:898, Histopathology 2019;74:443)
- FOXL2 (Histopathology 2020;76:11)
Negative stains
- Estrogen receptor and progesterone receptor are typically negative (Histopathology 2022;80:898)
- Inhibin (Histopathology 2022;80:898)
- Calretinin (Histopathology 2022;80:898)
- Reticulin may show a nested pattern with absence of pericellular staining within nests (Histopathology 2022;80:898)
Electron microscopy description
- Tumor cells with predominantly spindled and stellate morphology with fewer epithelioid cells, arranged in a loose microcystic pattern
- Cytoplasm shows intermediate filaments and variable amounts of other organelles (Ultrastruct Pathol 2014;38:261)
- Centrally placed nuclei are round with thin nuclear membranes and dispersed euchromatin
- Some nuclei have prominent nucleoli
Molecular / cytogenetics description
- Most microcystic stromal tumors harbor somatic mutations (missense or in frame deletion) in CTNNB1 exon 3 (Histopathology 2020;76:11)
- Frameshift, missense and deletion mutations of APC gene described (20%); CTBNN1 and APC mutations thought to be mutually exclusive (Histopathology 2020;76:11, Hum Pathol 2018;78:171)
- Mutations in FOXL2 and DICER1 have been absent in the tumors tested (Virchows Arch 2017;470:225)
Sample pathology report
- Ovary, right, oophorectomy:
- Right ovary with microcystic stromal tumor (6.5 cm) (see comment)
- Comment: Immunohistochemical stains demonstrate that the neoplastic cells are positive for CD10, WT1 and nuclear beta catenin, supporting the morphologic impression of microcystic stromal tumor. While microcystic stromal tumors are usually benign, rare examples of recurrence and metastasis have been reported. Of note, microcystic stromal tumors are sometimes associated with familial adenomatous polyposis syndrome. Clinical correlation is recommended.
Differential diagnosis
- Adult granulosa cell tumor:
- Nuclear grooves
- Call-Exner bodies
- Positive inhibin, calretinin
- Not expected to show nuclear staining for beta catenin
- Negative (or weak / faint) CD10
- Frequent FOXL2 mutation
- Juvenile granulosa cell tumor:
- Granulosa and theca cells line cysts with variable size
- Negative (or at most faint to moderate) CD10
- Mitoses common
- Thecoma:
- Usually occurs in postmenopausal women
- Associated with estrogenic manifestations
- Solid with yellow cut sections
- Cystic degeneration is rare (Int J Clin Exp Pathol 2019;12:2241)
- Should not show even minor classic microcystic morphology (Arch Pathol Lab Med 2018;142:1459)
- Positive inhibin, calretinin
- Not expected to show nuclear staining for beta catenin
- Negative CD10
- Yolk sac tumor:
- Reticular / cystic pattern with primitive appearance and more mitotic activity (Arch Pathol Lab Med 2018;142:1459)
- Schiller-Duval bodies
- Elevated serum AFP
- Positive SALL4, glypican 3, AFP
- Negative FOXL2, CD10
- Not expected to show nuclear staining for beta catenin
- Steroid cell tumor:
- Often associated with increased levels of androgen
- Should not show even minor classic microcystic morphology (Arch Pathol Lab Med 2018;142:1459)
- Most have at least a minor component of lipid rich cells
- Positive inhibin, MelanA, calretinin
- Struma ovarii:
- Positive TTF1, PAX8
- Negative FOXL2, CD10
- Not expected to show nuclear staining for beta catenin
- Endometrioid carcinoma:
- Positive epithelial membrane antigen
- Pitfall: may show nuclear beta catenin expression
- Negative FOXL2
- Solid pseudopapillary neoplasm:
- Many features shared with microcystic stromal tumor; may exist on a spectrum (Int J Clin Exp Pathol 2015;8:11792, Histopathology 2022;80:898)
- Pseudopapillary structures present
- Positive for CD99, progesterone receptor
- Negative for WT1, FOXL2 by immunohistochemistry
- Sclerosing stromal tumor:
- Staghorn-like blood vessels
- Cells within cellular nodules are rounded to polygonal clear vacuolated cells interspersed with fibroblasts and lutein cells
- Positive for inhibin, calretinin
- Negative for WT1, CD10
- Not expected to show nuclear staining for beta catenin
- Signet ring stromal tumor:
- Predominance of small stromal signet ring cells (usually with a single large vacuole)
- CD10 negative or focally positive
- Variable reactivity for inhibin and calretinin
- Negative for cyclin D1
- No nuclear staining for beta catenin
Additional references
Practice question #1
Practice answer #1
B. Microcystic stromal tumor. This tumor shows prominent microcystic features and is not associated with hormonal symptoms. Answer A is incorrect because this tumor does not show the characteristic nuclear grooves or Call-Exner bodies. Answer C is incorrect because this tumor shows prominent microcystic features and is not associated with estrogenic symptoms. Answer D is incorrect because this growth pattern is more consistent with microcystic stromal tumor than yolk sac tumor; Schiller-Duval bodies are not seen in the provided image.
Comment Here
Reference: Microcystic stromal tumor
Comment Here
Reference: Microcystic stromal tumor
Practice question #2
Which staining pattern below is most consistent with a diagnosis of ovarian microcystic stromal tumor?
- Membranous beta catenin, positive WT1, negative inhibin
- Membranous beta catenin, positive WT1, positive inhibin
- Nuclear beta catenin, negative WT1, negative inhibin
- Nuclear beta catenin, positive WT1, negative inhibin
Practice answer #2
D. Nuclear beta catenin, positive WT1, negative inhibin. Microcystic stromal tumors typically show nuclear beta catenin staining, positive WT1 and negative inhibin; therefore, answers A - C are incorrect.
Comment Here
Reference: Microcystic stromal tumor
Comment Here
Reference: Microcystic stromal tumor