Table of Contents
Definition / general | Essential features | Terminology | Epidemiology | Pathophysiology | Clinical features | Laboratory | Radiology description | Prognostic factors | Case reports | Treatment | Gross description | Gross images | Microscopic (histologic) description | Positive stains | Negative stains | Molecular / cytogenetics description | Differential diagnosis | Additional references | Board review style question #1 | Board review style answer #1 | Board review style question #2 | Board review style answer #2Cite this page: Srivastava S. Neuroendocrine tumor (carcinoid and atypical carcinoid). PathologyOutlines.com website. https://www.pathologyoutlines.com/topic/cervixcarcinoidtumor.html. Accessed May 13th, 2024.
Definition / general
- Typical carcinoid tumor:
- Grade 1 neuroendocrine tumor
- Recommended terminology for neuroendocrine tumors arising in the cervix is similar to that used for gastroenteropancreatic neuroendocrine tumors
- Same architectural and cytological features as neuroendocrine tumors at other sites
- Atypical carcinoid tumor:
- Neuroendocrine tumor with cytologic atypia and increased mitotic activity compared to typical carcinoid
- Classified as low grade neuroendocrine tumor (previously grade 2 and grade 3 neuroendocrine tumor) (Modern Pathology 2018;31:1770)
Essential features
- Typical carcinoid tumor:
- Low grade (grade 1) neuroendocrine tumor
- Characteristic neuroendocrine and organoid differentiation without nuclear atypia, mitotic figures or necrosis
- No specific recommendation for Ki67 labelling index or mitotic count
- Generally follow an indolent course; however, they retain the potential for metastatic spread
- Atypical carcinoid tumor:
- Aggressive tumor that frequently shows subclinical hematogenous and lymphatic metastases, even in early disease
- Metastasize to liver and may present with carcinoid syndrome
- Urine 5-HIAA levels may be elevated
- Frequently coexist with other more common types of cervical carcinoma such as adenocarcinoma or squamous cell carcinoma
- Development of immunohistochemistry panels and plasma assays for peptides and amines, as well as the widespread use of Octreoscan and PET / CT, has significantly enhanced the identification and diagnosis
Terminology
- For typical carcinoid tumor: low grade neuroendocrine tumor, grade 1
- For atypical carcinoid tumor: low grade neuroendocrine tumor, grade 2 or grade 3 (Modern Pathology 2018;31:1770)
- Updated 2014 World Health Organization (WHO) classification of neuroendocrine tumors of female reproductive organs provides following terminology for uterine cervix which is more in line with the terminology used for GI tract and aligns with the recently proposed unified nomenclature by the International Agency for Research on Cancer (IARC) and World Health Organization (WHO) (Curr Oncol Rep 2017;19:59, Modern Pathology 2018;31:1770)
- Low grade neuroendocrine tumor (typical carcinoid, atypical carcinoid tumor), corresponding to the term neuroendocrine tumor in the 2018 terminology
- High grade neuroendocrine carcinoma (small cell neuroendocrine carcinoma, large cell neuroendocrine carcinoma) corresponding to the term neuroendocrine carcinoma in the 2018 terminology
- Adenocarcinoma admixed with neuroendocrine carcinoma
Epidemiology
- Overall, cervical neuroendocrine tumors represent ~2% of all cervical malignancies (Case Rep Oncol 2017;10:737)
- Cervical low grade neuroendocrine tumors are extremely rare, accounting for less than 0.5% of cervical cancers
- Atypical carcinoid tumors are very rare with only ~15 reported cases in the literature (Am J Surg Pathol 1997;21:905, J Clin Endocrinol Metab 1999;84:4209, Gynecol Oncol 1999;72:3, Gynecol Oncol 2001;81:82, Gynecol Oncol 2003;88:333, J Chemother 2006;18:209)
- Most patients are in fourth to fifth decade
- Patients tend to be younger, more often white / Caucasian compared to more common cervical carcinomas (squamous and adenocarcinoma)
Pathophysiology
- High risk HPV sequences (types 16 and 18) were not present in typical carcinoid tested in some of the studies however their numbers are very small for any reliable generalization (Gynecol Oncol 1999;72:3)
- High risk HPV sequences were present in large cell NEC and small cell neuroendocrine carcinomas tested in these studies (Am J Surg Pathol 2004;28:901)
Clinical features
- May present with vaginal bleeding or discharge, detection of a cervical mass, postcoital spotting, abnormal Pap smear (Gynecol Oncol Case Rep 2013;7:4)
- Symptoms related to ectopic hormone production or carcinoid syndrome are extremely rare for carcinoid tumor (Gynecol Oncol Case Rep 2013;7:4)
Laboratory
- Plasma assays for peptides such as calcitonin, gastrin, serotonin, substance P, vasoactive intestinal peptide, pancreatic polypeptide, somatostatin, adrenocorticotrophic hormone, β-melanocyte-stimulating hormone and histamine may be elevated, although it is not related to clinical symptoms
- Urinary levels of 5-HIAA may be elevated and 24 hour urinary 5-HIAA may be useful
- Chromogranin A is present in the neurosecretory vesicles of neuroendocrine tumor cells and may be detectable in the plasma of such patients
- Serum chromogranin A is a more sensitive and broadly applicable tumor marker for neuroendocrine tumors than is urinary 5-HIAA but it is less specific
- Chromogranin A levels are higher in patients with diffuse metastases than localized disease or isolated hepatic involvement; higher levels may be associated with a poorer prognosis
- Data on the correlation of plasma chromogranin A levels with treatment response and on their prognostic value are not available for cervical carcinoids (Case Rep Oncol 2017;10:737)
Radiology description
- Cross sectional imaging including either a triphasic CT or an MRI should be performed to evaluate the extent of the disease
- Somatostatin receptor scintigraphy (SRS) can localize the tumor, with an overall sensitivity as high as 90%
- Uptake of radiolabeled octreotide is predictive of a clinical response to therapy with somatostatin analogues
- FDG positron emission tomography (PET) may be useful for initial staging
- Octreoscan appears more sensitive than FDG PET
- PET / CT does not provide any meaningful diagnostic information except with aggressive tumors (J Obstet Gynaecol Res 2011;37:636)
Prognostic factors
- Grade 1 neuroendocrine tumors generally follow an indolent course; however, they retain the potential for metastatic spread and their prognosis is difficult to evaluate due to their rarity
- Considered aggressive with metastases to liver and extension outside the uterus
- Paucity of cases with reported follow up yields uncertain prognosis; however, considered to have potential for aggressive behavior since metastases to liver and extension outside the uterus have been reported
- Outcome is considered to be intermediate between carcinoid tumor and high grade neuroendocrine carcinoma
- Most commonly present as stage 1 disease in contrast to squamous cell carcinoma, which usually presents as stage 2 disease
- Prognosis is mainly dependent on tumor stage
- Relationship between size and metastatic propensity has not been established
- Uncertain impact of mitotic rate or Ki67 labeling index
- Most patients with recurrent disease develop metastases (Gynecol Oncol 2017;144:637, Case Rep Oncol 2017;10:737, Gynecol Oncol Case Rep 2013;7:4)
Case reports
- 39 year old woman with numerous metastases to the liver (J Obstet Gynaecol Res 2011;37:636)
- 40 year old woman presented with abnormal cervical cytology (Acta Cytol 1990;34:119)
- 43 year old woman with a nonmetastatic cervical carcinoid (Case Rep Oncol 2017;10:737)
- 44 year old Japanese woman with stage IB1 (Gynecol Oncol Case Rep 2013;7:4)
- 45 year old woman presented with painless vaginal bleeding for 2 months (J Clin Pathol 2018;71:1030)
- 46 year old woman with carcinoid syndrome (J Clin Endocrinol Metab 1999;84:4209)
- 49 year old woman with a polypoid lesion and atypical cervical cytology (Diagn Cytopathol 2012;40:724)
Treatment
- There are currently no recommendations regarding treatment due to rarity of the cases (J Clin Endocrinol Metab 1999;84:4209, Gynecol Oncol Case Rep 2013;7:4)
- Most reported cases were initially treated with radical hysterectomy (Cancer 1979;43:535, Gynecol Oncol 1999;72:3, Acta Obstet Gynecol Scand 1983;62:539, World J Surg 2005;29:92, Gynecol Oncol 2011;122:190)
- Liver lesions should be resected and unresectable lesions should be considered for embolization, radiofrequency ablation or cryotherapy (J Clin Endocrinol Metab 1999;84:4209)
- Efficacy of somatostatin analogues or chemotherapy is uncertain (Gynecol Oncol Case Rep 2013;7:4)
- Octreotide scan (somatostatin analog scintigraphy) can be used to predict response to somatostatin analogs and also inversely correlates to chemotherapy response (Gynecol Oncol 2011;122:190)
- Utility of somatostatin analogues has only been described in the case of systemic manifestations of the carcinoid syndrome (Gynecol Oncol Case Rep 2013;7:4)
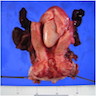
Gross description
- Macroscopic appearance is not distinctive
- Average reported size range is 0.5 - 11 cm in diameter
- Lesions are commonly large, sometimes with a barrel shaped appearance
Microscopic (histologic) description
- Well to moderately differentiated and contain neurosecretory granules
- Growth patterns can be organoid, trabecular, nodular, nests / islands or cord-like
- Rosette-like structures are common
- Cells are round to oval with abundant cytoplasm, elongated nuclei, characteristic finely granular chromatin and visible to prominent nucleoli
- Cells are commonly epithelioid but can be spindled
- Typical carcinoid tumors show a lack of nuclear atypia, mitotic figures and necrosis while atypical carcinoid tumors show insular and trabecular growth, mild to moderate nuclear pleomorphism and focal necrosis
- Mitotic activity has been traditionally assessed in number of mitoses per high power field; however, the 2018 consensus terminology recommends that mitotic count should be expressed as mitoses per mm2 area, ideally counted in up to 10 mm2 to assure accuracy (Modern Pathology 2018;31:1770)
- In typical carcinoid tumors, mitotic activity is absent
- In atypical carcinoid tumors, there is increased mitotic activity (5 - 10 mitotic figures / 10 high powered fields) (Semin Diagn Pathol 2013;30:224)
- The impact of the mitotic rate per 10 HPF and Ki67 labeling index on the prognosis of neuroendocrine tumors has been evaluated in multiple studies, which included NET of gastroenteropancreatic or bronchopulmonary origin mostly
- The same might be true for cervical carcinoids but the overall small sample size prohibits any reliable generalization of patient outcome (Semin Diagn Pathol 2013;30:224)
- No specific evidence for the formulaic use of Ki67 labelling index or mitotic count for grading; immunohistochemical evidence of neuroendocrine differentiation is required for diagnosis (Case Rep Oncol 2017;10:737, Gynecol Oncol 2017;144:637, Semin Diagn Pathol 2013;30:224)
Positive stains
- Synaptophysin, chromogranin, CD56 and neuron specific enolase (NSE), cytokeratin, Ki67 (> 50%) (Case Rep Oncol 2017;10:737, Gynecol Oncol 2017;144:637, Case Rep Oncol 2017;10:737, Semin Diagn Pathol 2013;30:224)
- Cytokeratin, CEA and high risk HPV may be positive
Negative stains
Molecular / cytogenetics description
- High risk HPV sequences (types 16 and 18) were not present in typical carcinoid tested in some of the studies however, their numbers are very small for any reliable generalization (Gynecol Oncol 1999;72:3)
- Oncogenic HPV sequences and allelic losses have been identified; most commonly detected aberrancies are allelic losses, one or more 3p regions and 9p21 (Gynecol Oncol 1999;72:3)
- They usually do not harbor the mutations seen in large cell NEC and small cell carcinoma such as allelic losses and p53 gene abnormalities
- Allelic losses at 5q21-q22 (APC::MCC region), 11q13 (MEN1 gene locus) and RB gene (13q) are relatively infrequent
Differential diagnosis
- Adenocarcinoma and squamous cell carcinoma of cervix (SCC):
- SCC and adenocarcinomas are more common but may coexist with neuroendocrine tumors
- SCC and adenocarcinomas are confined to pelvis in early stages of the disease
- Neuroendocrine markers (synaptophysin and chromogranin) are negative
- p63 is positive in SCC
- CK7, p16 and HPV are positive in adenocarcinoma of cervix
- Other mass forming lesions of the cervix
- Metastatic carcinoid from other locations especially GI tract
Additional references
Board review style question #1
Which of the following is true?
- Typical carcinoids are commonly positive for high risk HPV
- Typical carcinoids commonly present with carcinoid syndrome
- Typical carcinoids frequently metastasize
- Typical carcinoids lack nuclear atypia, mitotic figures and necrosis
Board review style answer #1
D. Typical carcinoids lack nuclear atypia, mitotic figures and necrosis
Comment Here
Reference: Neuroendocrine tumor
Comment Here
Reference: Neuroendocrine tumor
Board review style question #2
Atypical cervical carcinoid is positive for which of the following?
- CD56
- p63
- S100
- Desmin
Board review style answer #2