Table of Contents
Definition / general | Essential features | ICD coding | Epidemiology | Sites | Etiology | Diagrams / tables | Clinical features | Diagnosis | Laboratory | Radiology description | Radiology images | Prognostic factors | Case reports | Treatment | Gross description | Gross images | Microscopic (histologic) description | Microscopic (histologic) images | Cytology description | Cytology images | Positive stains | Negative stains | Electron microscopy description | Electron microscopy images | Molecular / cytogenetics description | Molecular / cytogenetics images | Videos | Sample pathology report | Differential diagnosis | Additional references | Practice question #1 | Practice answer #1 | Practice question #2 | Practice answer #2Cite this page: Agarwal S. Follicular adenoma. PathologyOutlines.com website. https://www.pathologyoutlines.com/topic/thyroidfollicularadenoma.html. Accessed September 14th, 2025.
Definition / general
- Benign, encapsulated tumor that exhibits thyroid follicular cell differentiation
- Lacks capsular and vascular invasion
- Absent nuclear features of papillary thyroid carcinoma
Essential features
- Benign thyroid tumor, lacking infiltrative properties and usually exhibiting follicular architecture
- Needs to be differentiated from adenomatoid thyroid nodule and other follicular patterned thyroid neoplasms
ICD coding
- ICD-O: 8330/0 - follicular adenoma
Epidemiology
- Incidence: 3 - 5%
- Adults, wide age range; usually in fifth to sixth decades (Clin Endocrinol (Oxf) 2018;88:936)
- Female preponderance
Sites
- Either thyroid lobe, isthmus, ectopic thyroid tissue
Etiology
- Usually sporadic
- Radiation exposure (Cancer 2003;97:2397)
- Iodine deficiency (Cancer 1987;60:3096)
- Familial tumor syndromes
- PTEN (phosphatase and tensin homolog deleted on chromosome ten): younger age of presentation; multiple and bilateral (Ann Diagn Pathol 1999;3:331)
- Carney complex (Diagn Histopathol 2017;23:366)
- MEN1 syndrome (Wermer syndrome)
- McCune-Albright syndrome
- Familial multinodular goiter (FMNG) syndrome
Diagrams / tables
Clinical features
- Painless solitary thyroid nodule
- May be detected incidentally (during palpation or neck ultrasound)
- Rarely compression symptoms, if large
- Hyperthyroidism in case of hyperfunctioning adenomas (Plummer adenoma)
- Reference: Surg Clin North Am 2014;94:499
Diagnosis
- Diagnostic workup is similar to any thyroid nodule
- Ultrasound with fine needle aspiration cytology (FNAC)
Laboratory
- Thyroid function test; usually euthyroid
- Can be hyperthyroid in case of hyperfunctioning adenoma
Radiology description
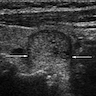
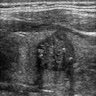
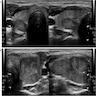
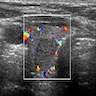
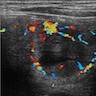
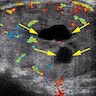
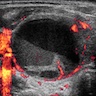
- Sonography: solid / solid cystic nodule, smooth and well defined margins, homogeneous or heterogeneous echotexture, isoechoic or hypoechoic, occasionally peripheral hypoechoic halo (Asian J Surg 2020;43:339, J Ultrasound Med 2014;33:221, AJR Am J Roentgenol 2010;194:44)
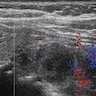
- Doppler ultrasound: absent or low blood flow
- Radionuclide scan: cold nodule; hot nodule if hyperfunctioning
Radiology images
Prognostic factors
- Benign tumor
Case reports
- 3 year old girl with adenochondroma of the thyroid gland (Ear Nose Throat J 2021;100:412S)
- 12 year old boy with follicular adenoma harboring BRAF K601E mutation (Int J Surg Pathol 2017;25:348)
- 29 year old woman with clear cell follicular adenoma of ectopic thyroid (Endocr Pathol 1998;9:339)
- 39 year old woman with follicular adenoma having intracytoplasmic lumina (Cytopathology 2016;27:495)
- 45 year old woman with follicular adenoma with papillary architecture (Cytopathology 2015;26:256)
- 48 year old woman with renal cell carcinoma metastatic to follicular adenoma of thyroid gland (Acta Cytol 2004;48:64)
- 58 year old woman with Plummer adenoma following percutaneous thyroid ethanol injection in thyroid gland (Case Rep Endocrinol 2017;2017:1026139)
- 59 year old woman with metastasis of colonic adenocarcinoma to thyroid follicular adenoma (Pathol Int 2005;55:574)
- 61 year old man with clear cell follicular adenoma of thyroid (Exp Clin Endocrinol Diabetes 2010;118:19)
- 61 year old man with follicular adenoma showing spindle cell metaplasia (Am J Surg Pathol 2019;24:84)
- 63 year old woman with follicular adenoma showing osseous metaplasia (Int J Surg Case Rep 2017;37:83)
- 72 year old man with follicular adenoma showing chondroid metaplasia (Histopathology 1991;18:278)
- 75 year old woman with follicular adenoma showing cellular atypia and mimicking anaplastic thyroid carcinoma on cytology (Diagn Cytopathol 2017;45:928)
Treatment
- Lobectomy
- Hyperfunctioning follicular adenomas: lobectomy preferred over radioiodine (Oncologist 2011;16:585)
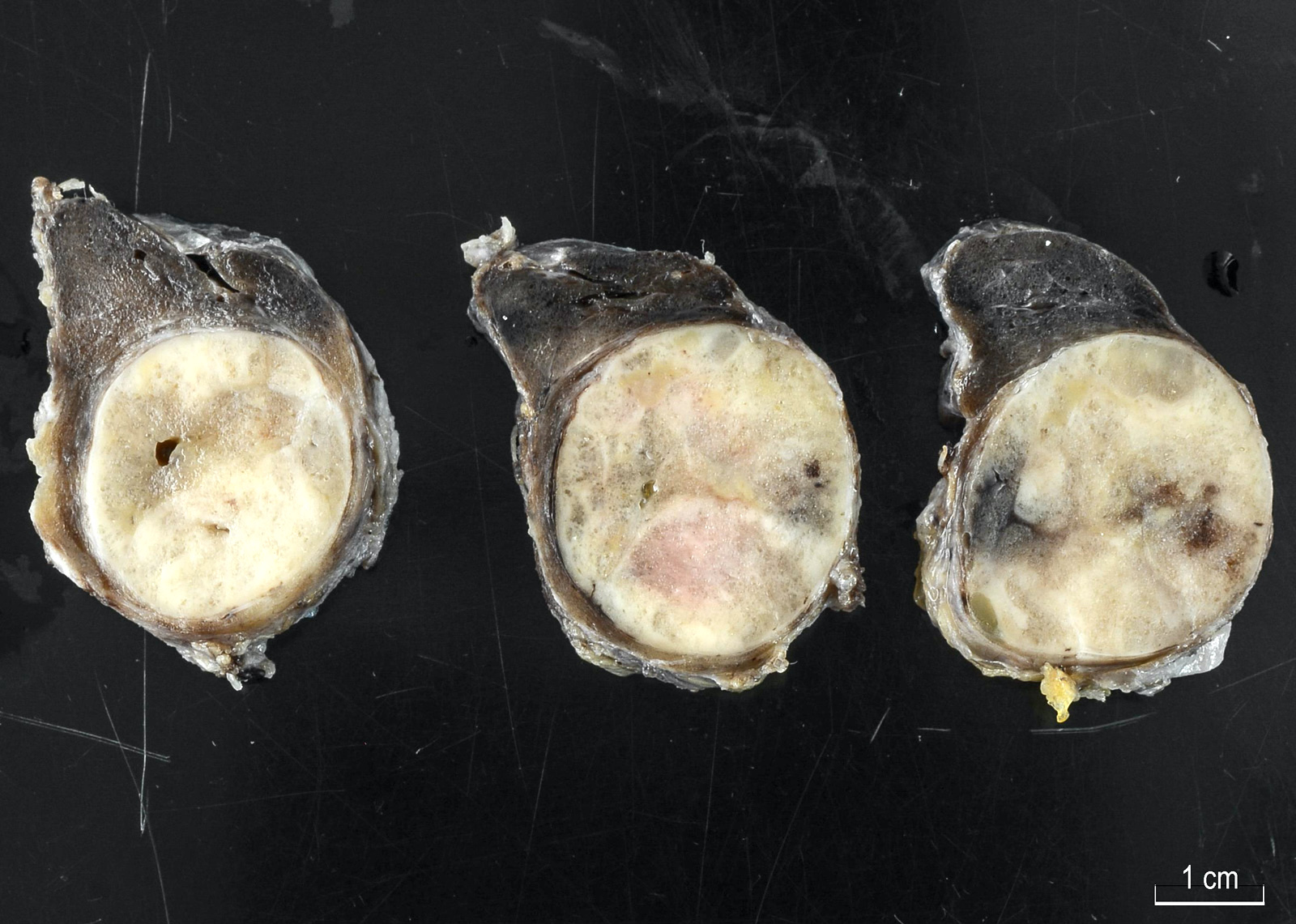
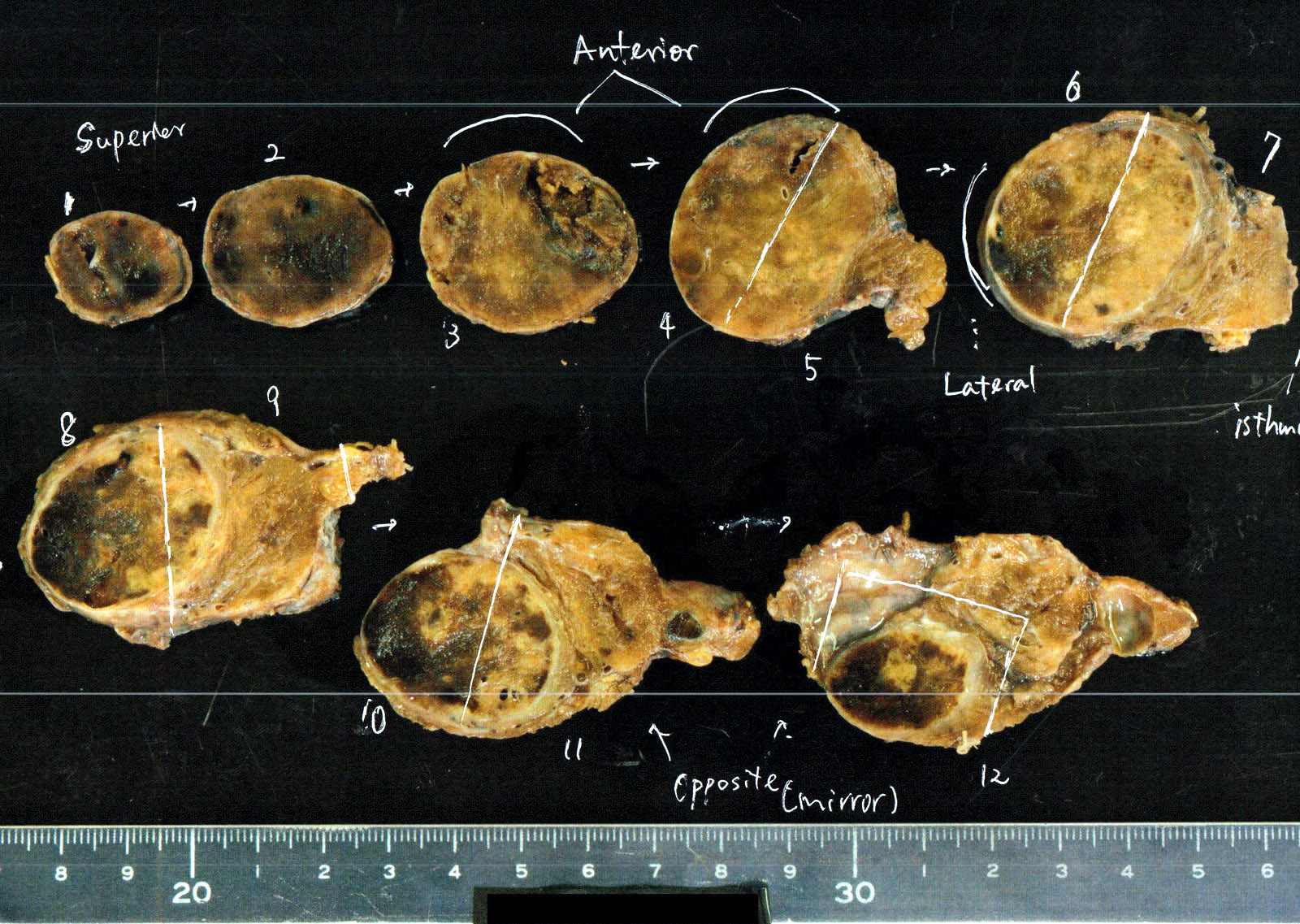
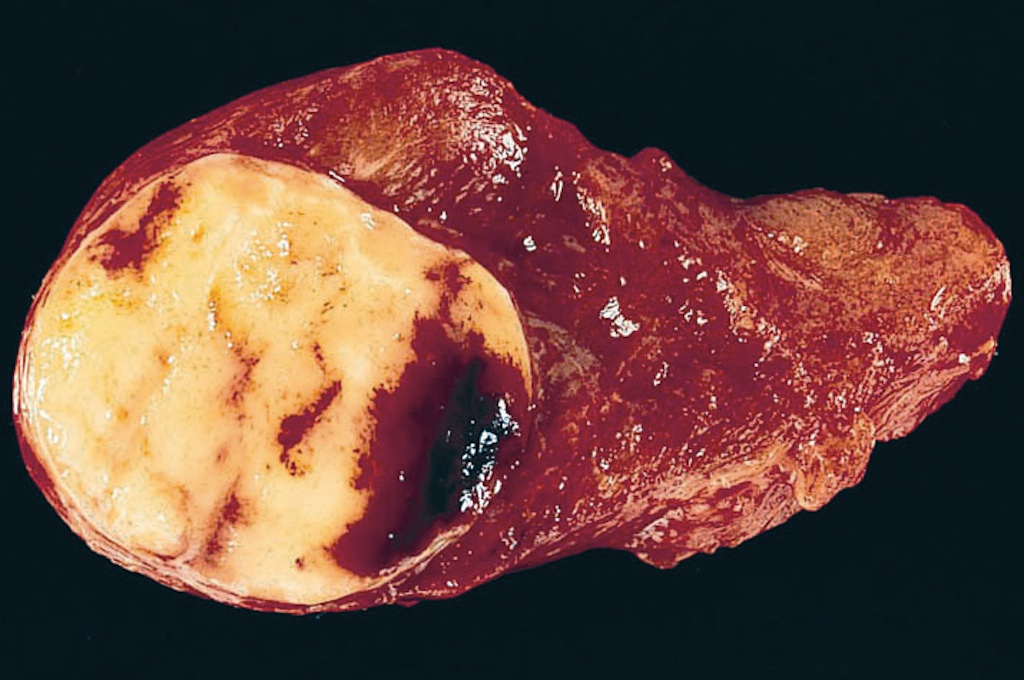
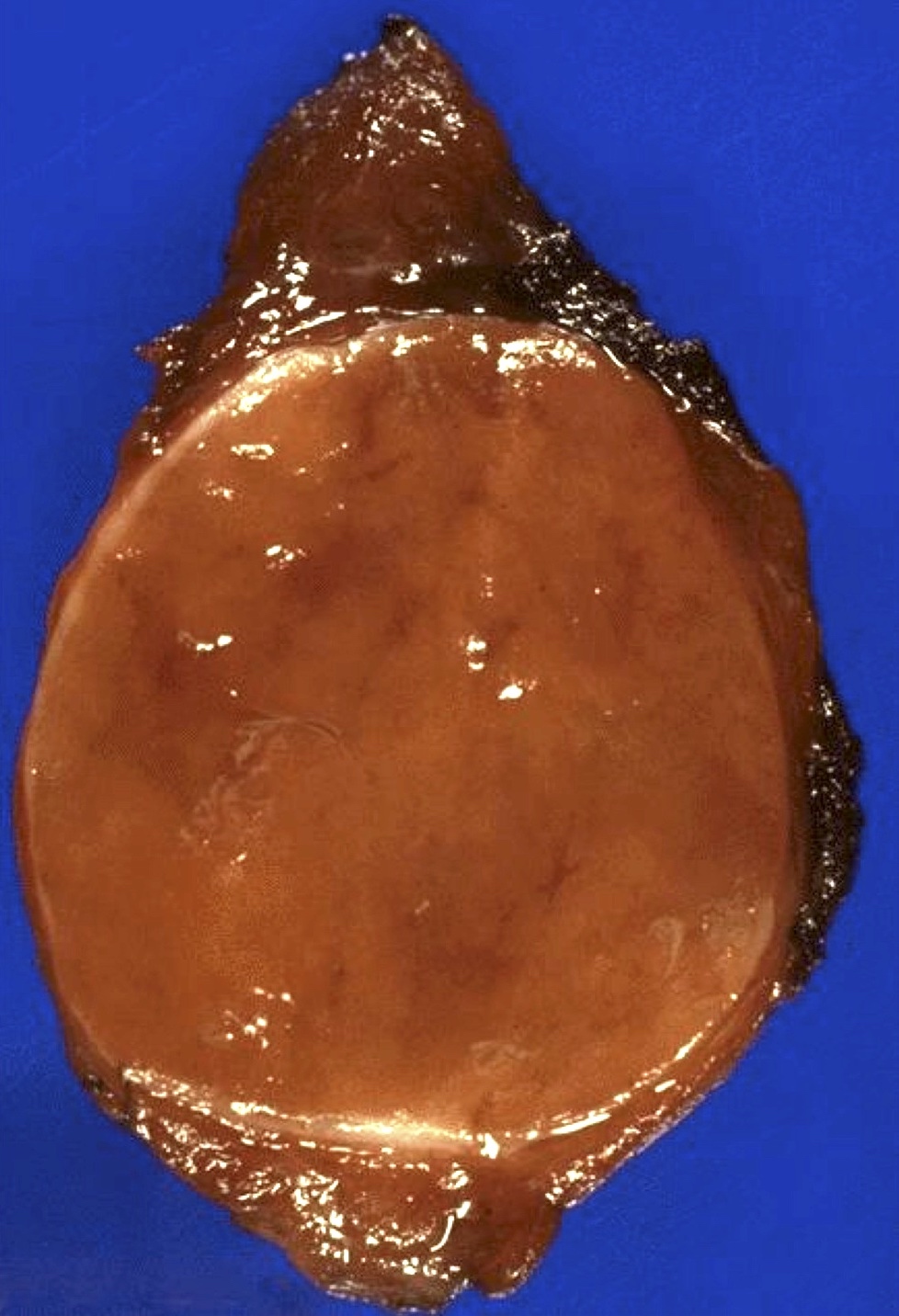
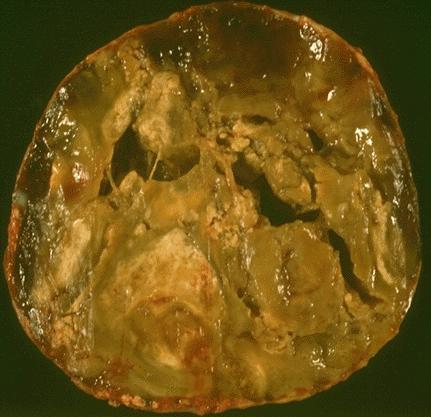
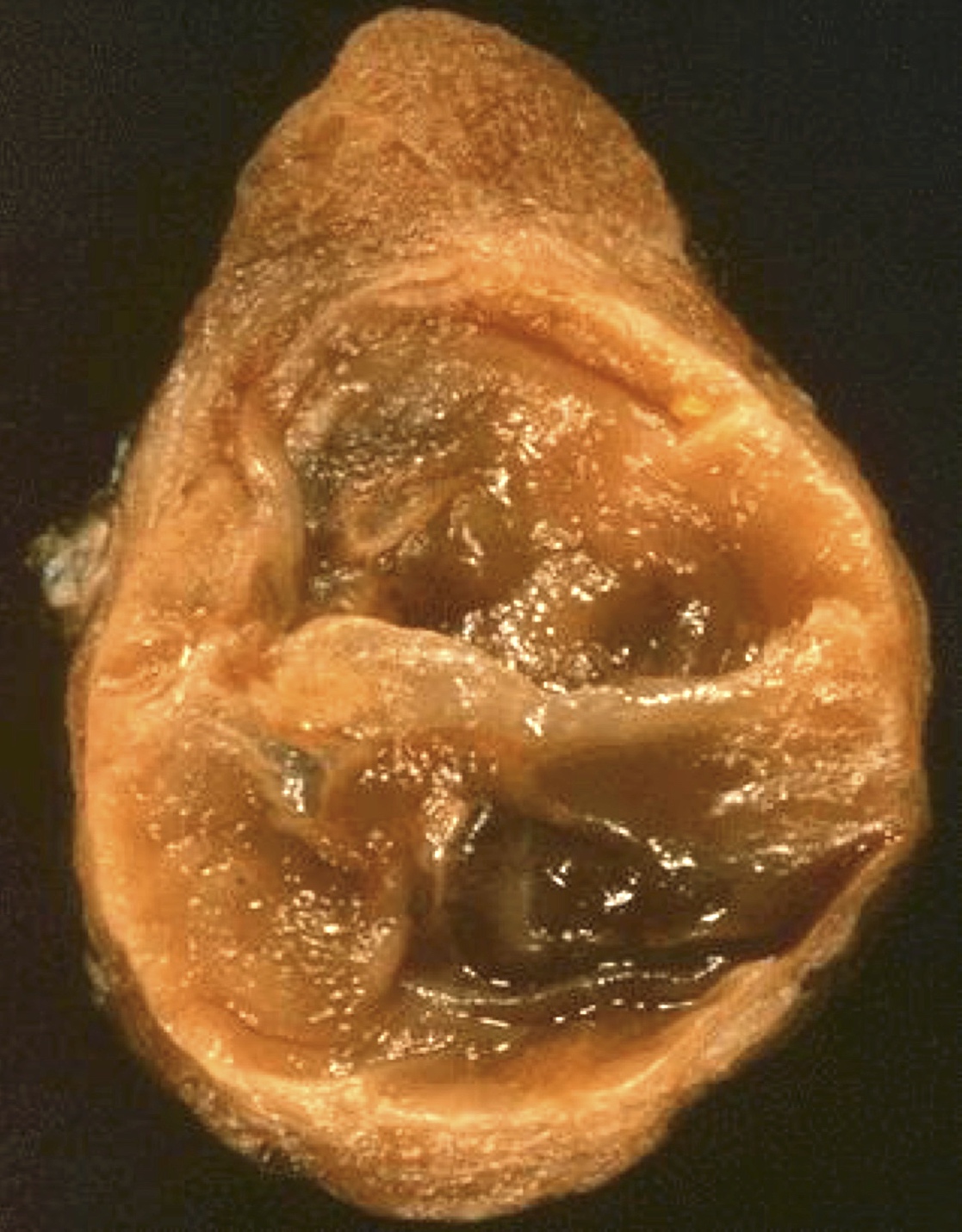
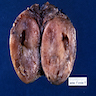
Gross description
- Solitary, encapsulated nodule; multiple if familial
- Variable size (1 - 10 cm)
- Solid, gray-white, tan to light brown
- Secondary changes: hemorrhage, cystic change, fibrosis, calcification, infarction; may develop post-fine needle aspiration cytology
- Rarely black; especially seen with minocycline therapy
Gross images
Contributed by Andrey Bychkov, M.D., Ph.D., Mark R. Wick, M.D. and AFIP
Images hosted on other servers:
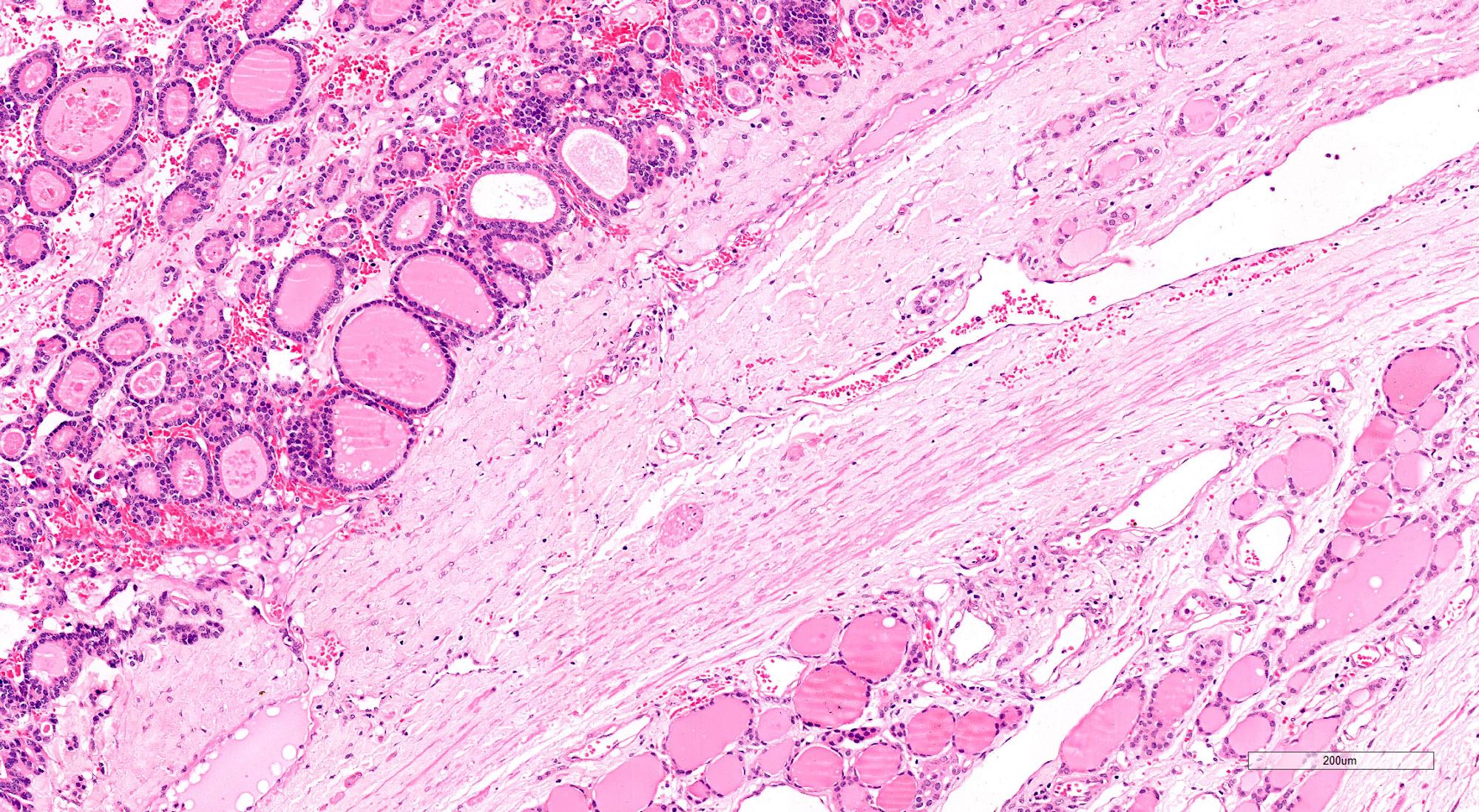
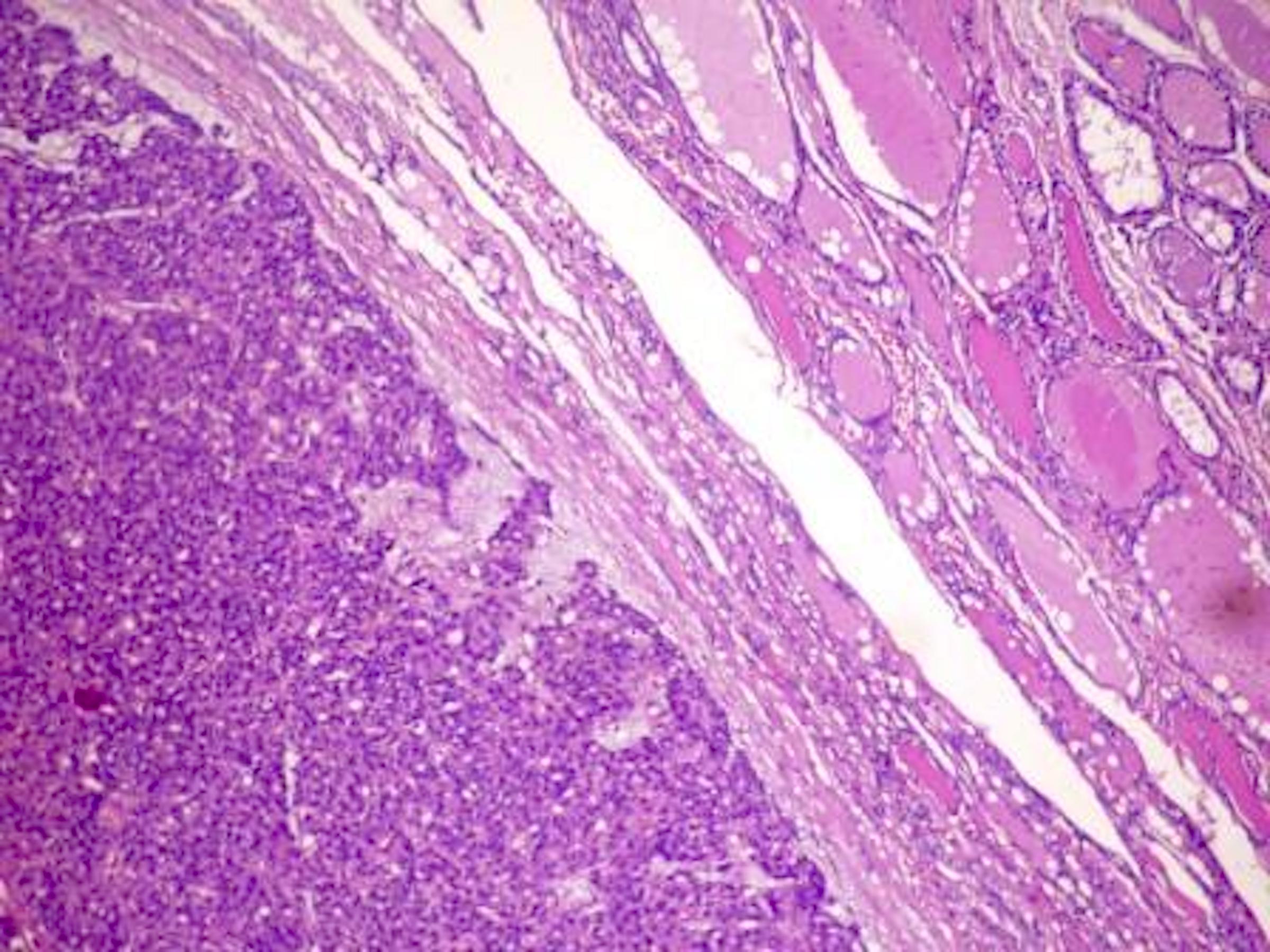
Microscopic (histologic) description
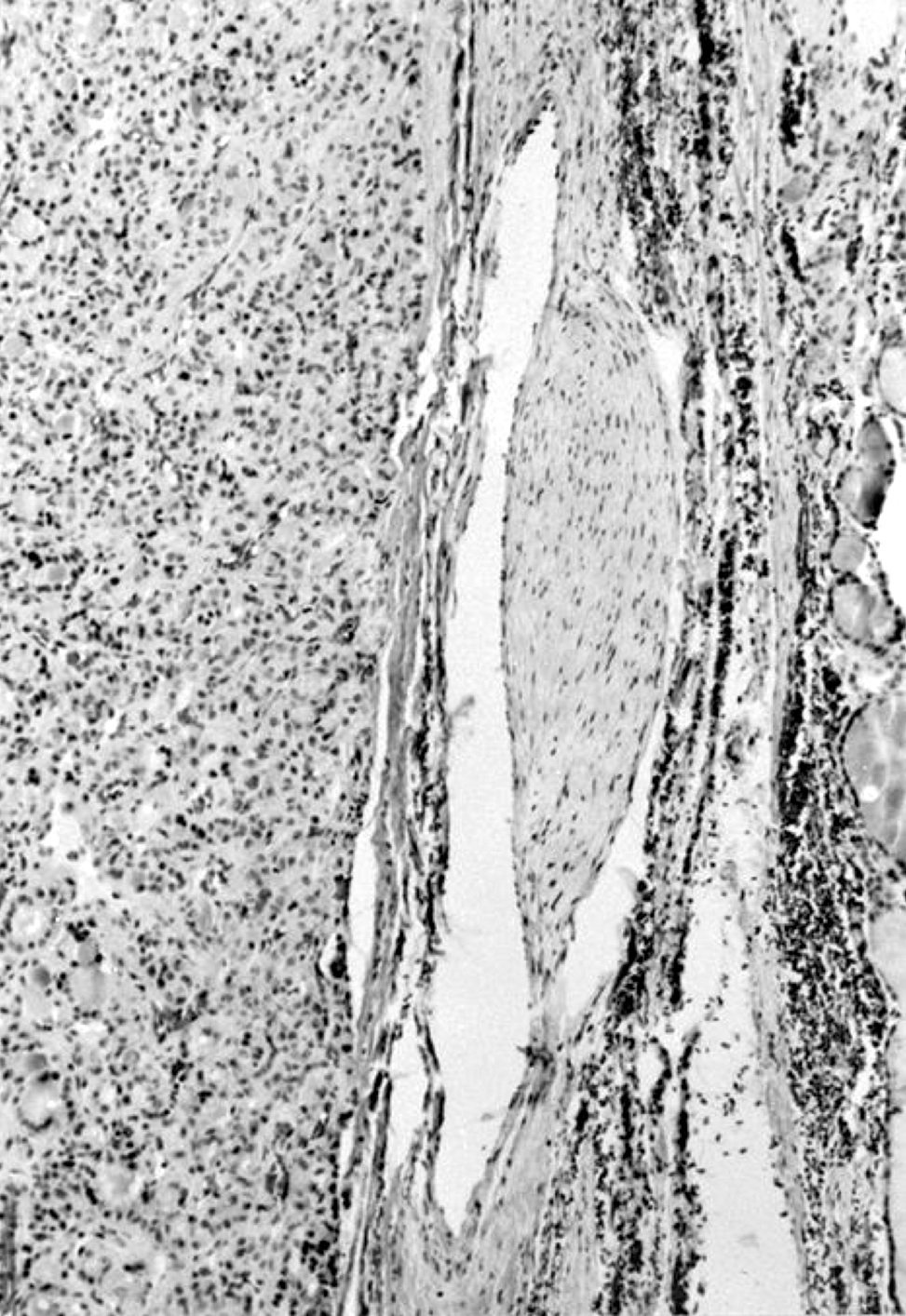
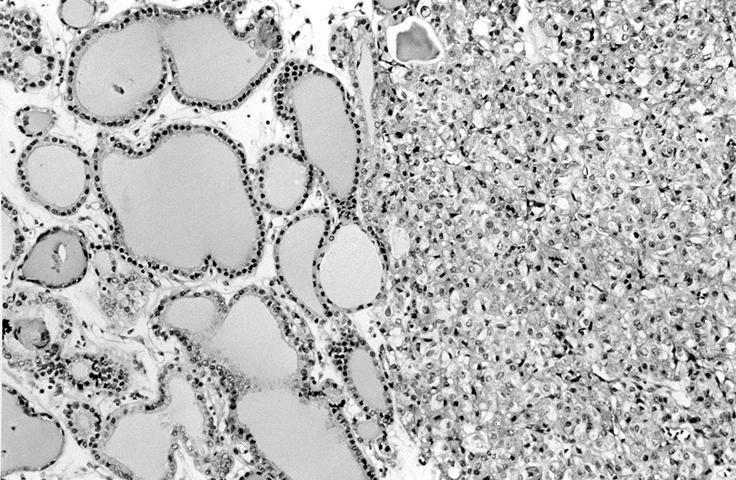
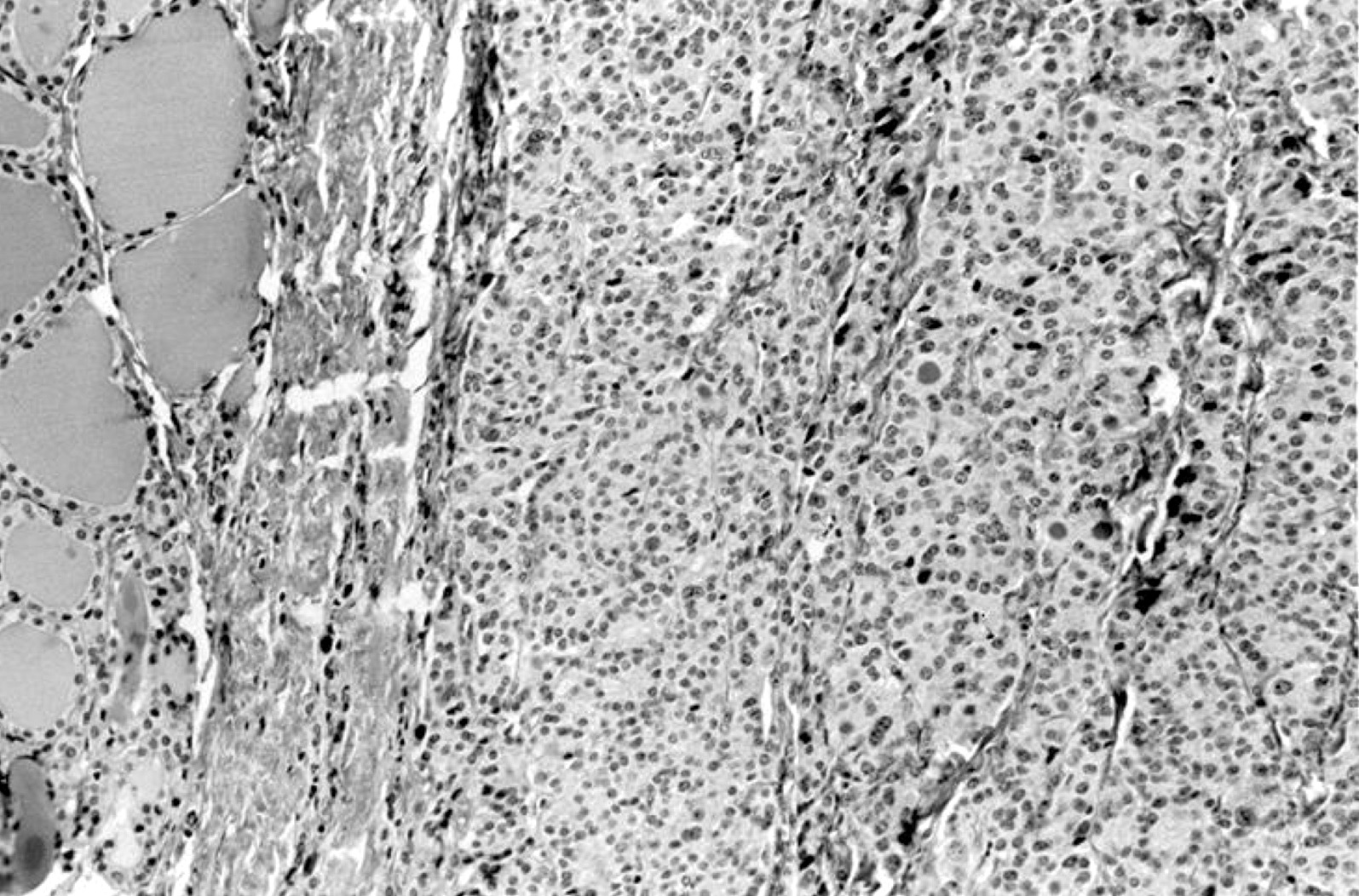
- Architecturally and cytologically different from surrounding gland
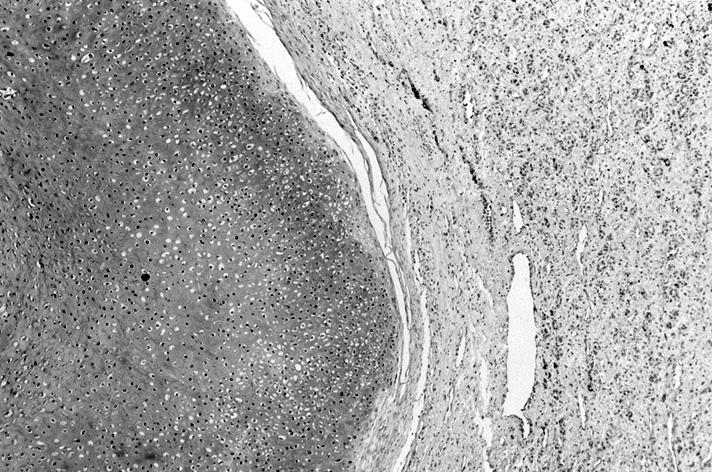
- Compression signs in surrounding thyroid tissue
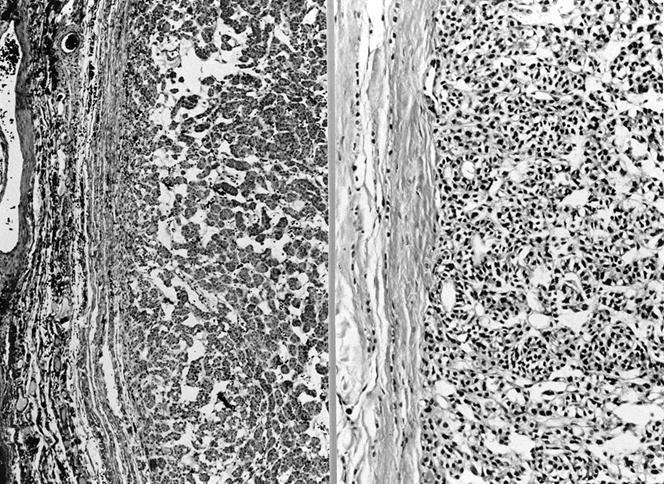
- Encapsulated; thin or moderately thick capsule
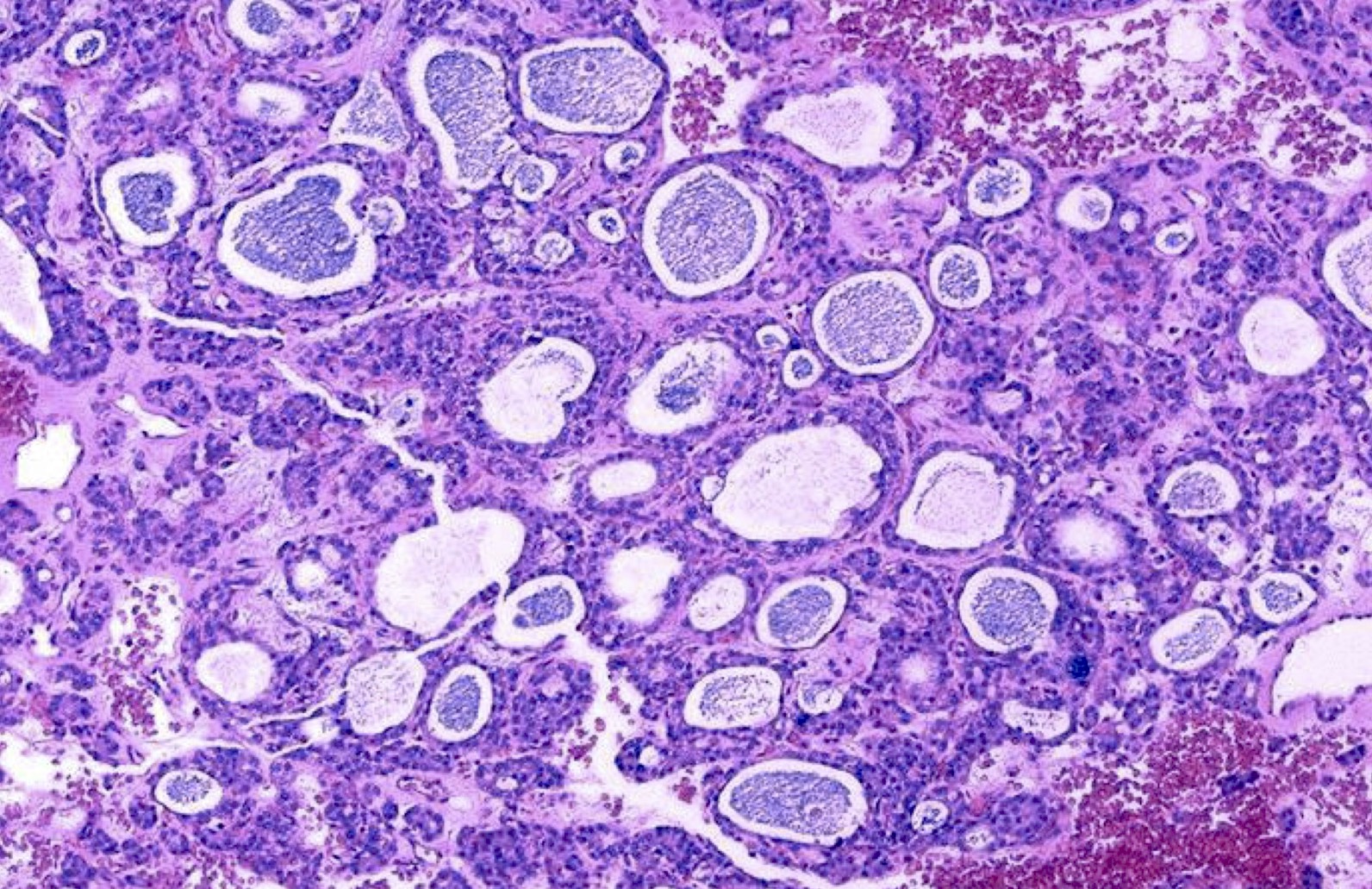
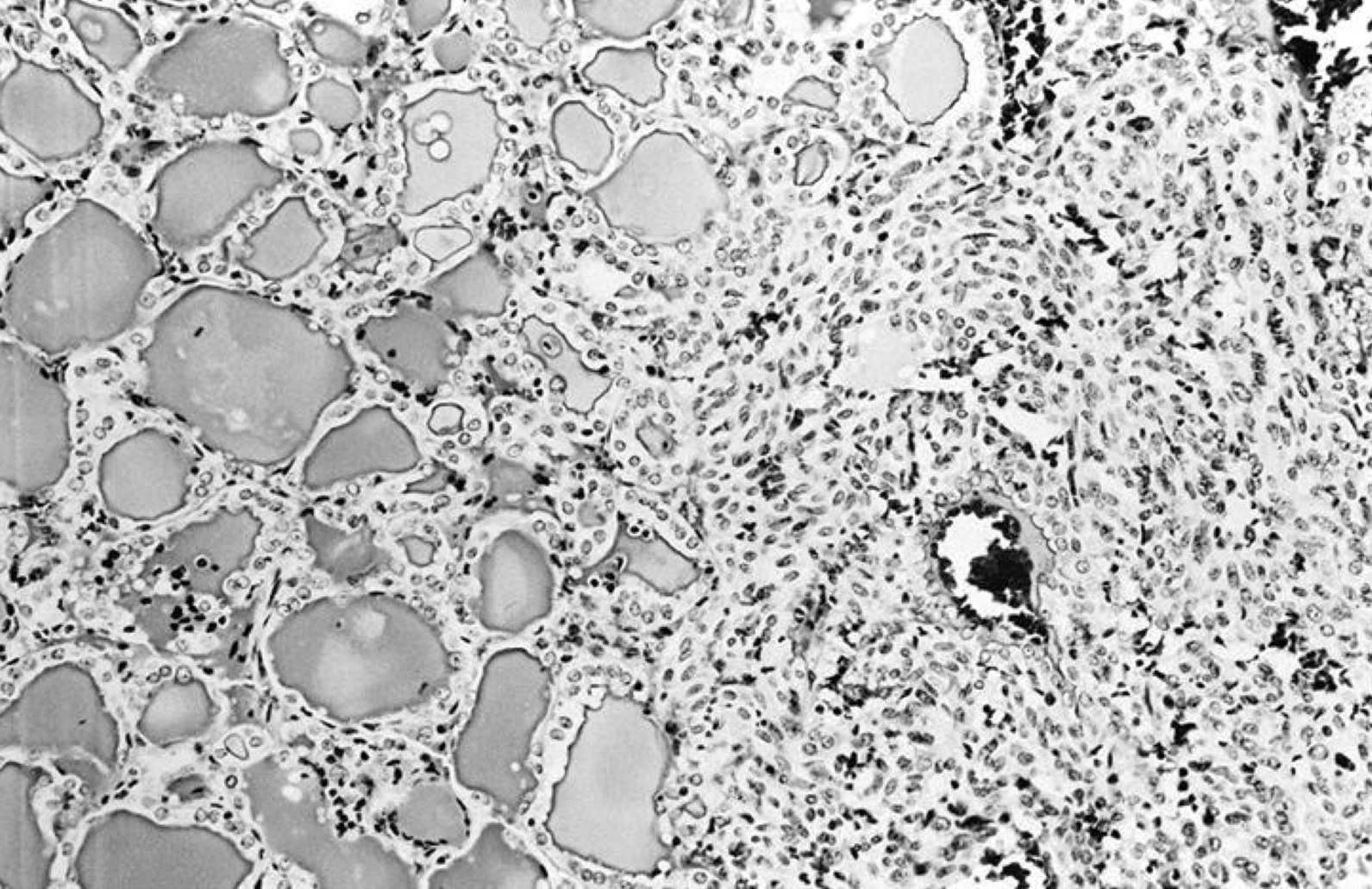
- Architectural patterns (can be seen in any combination)
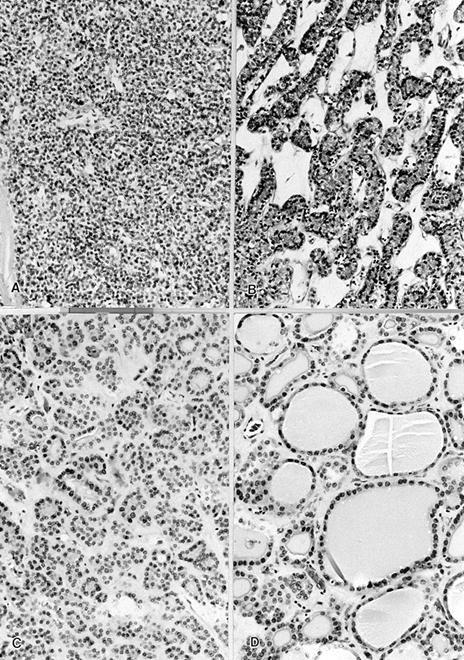
- Normofollicular (simple): size similar to normal thyroid follicles
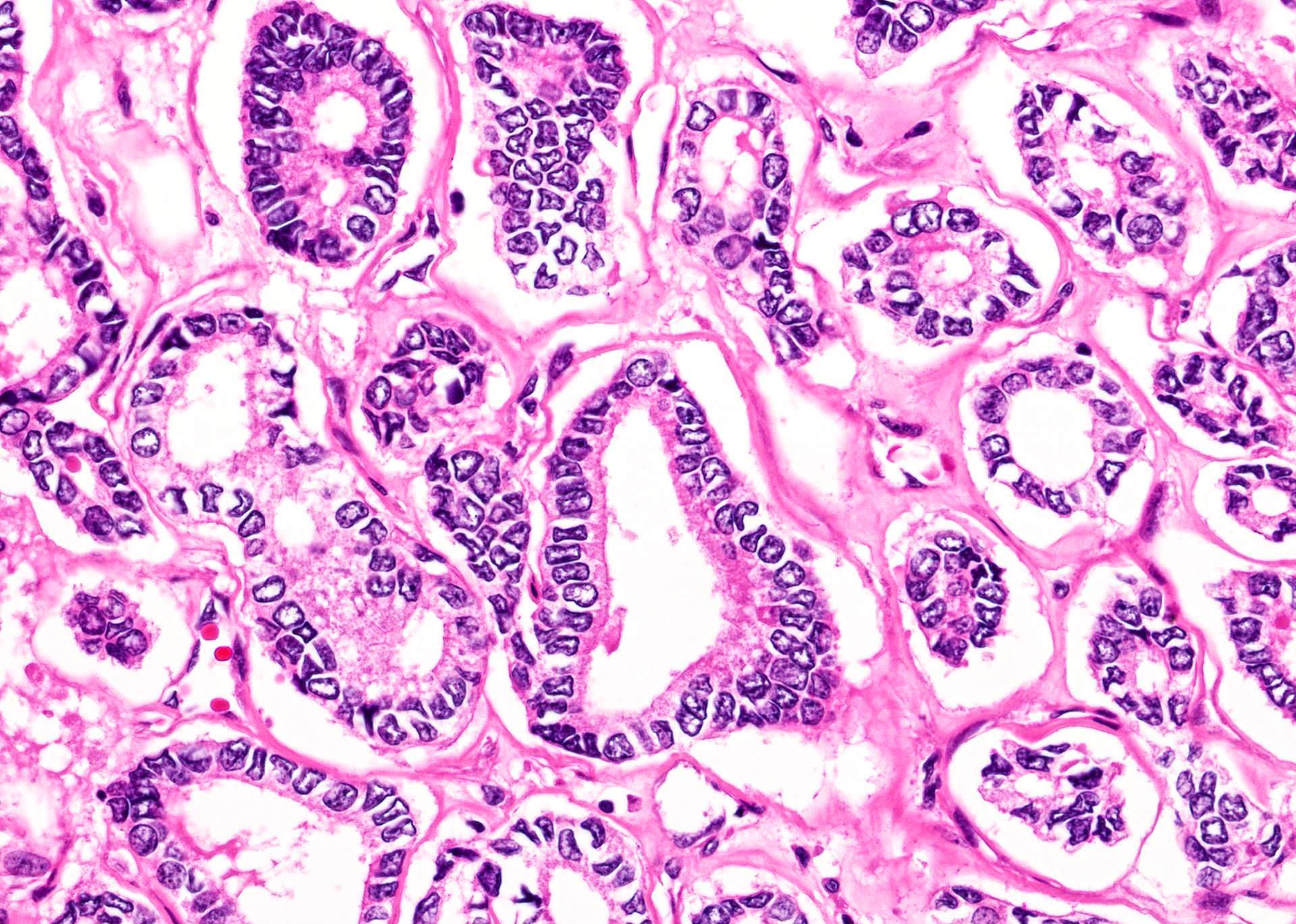
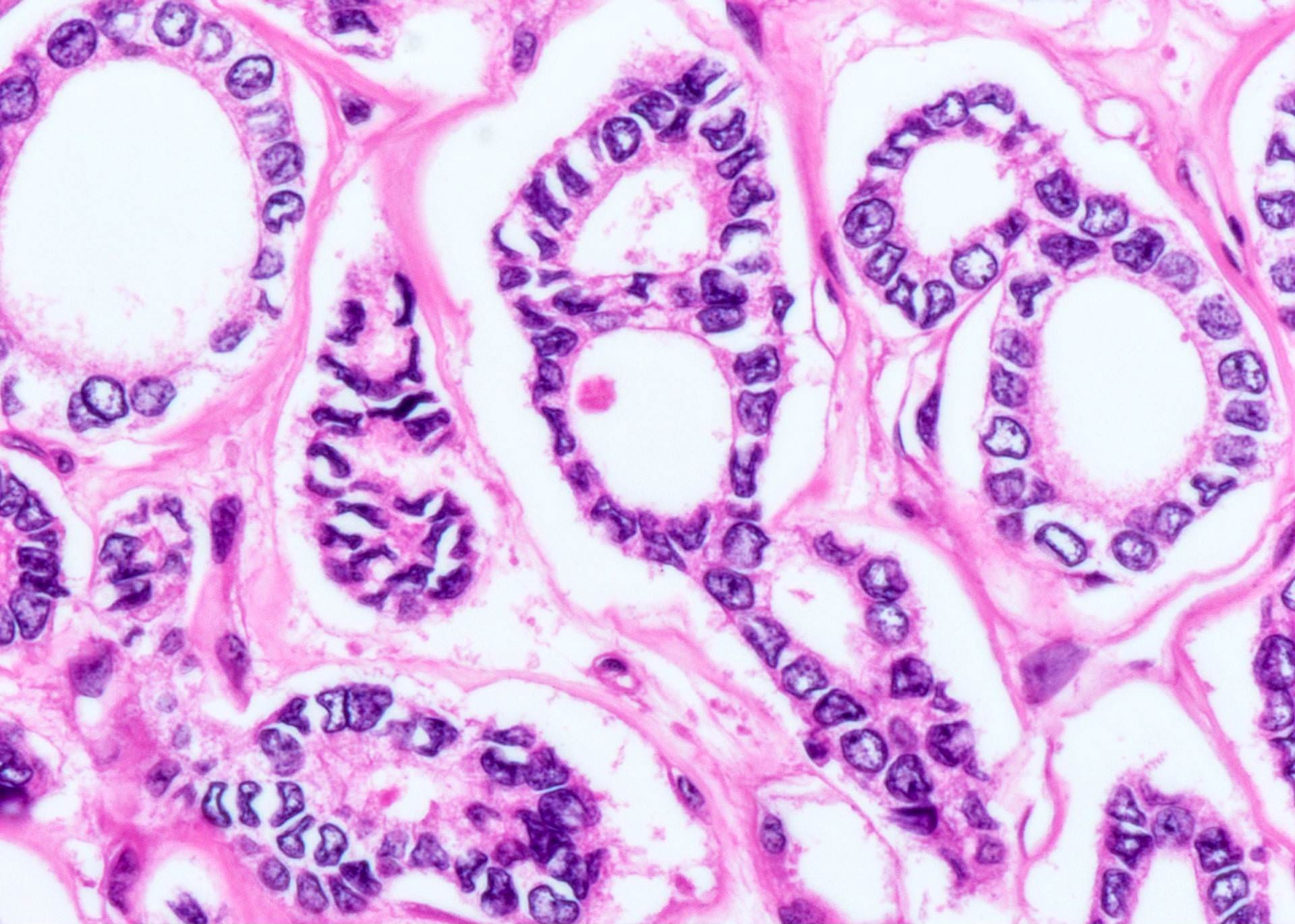
- Microfollicular (fetal): smaller follicles, small amount of intraluminal colloid
- Macrofollicular (colloid): large follicles, flattened epithelium, abundant colloid
- Solid / trabecular (embryonal): minimal or no colloid
- Focal papillary pattern, occasionally; especially in hyperfunctioning adenoma and follicular adenoma with papillary hyperplasia
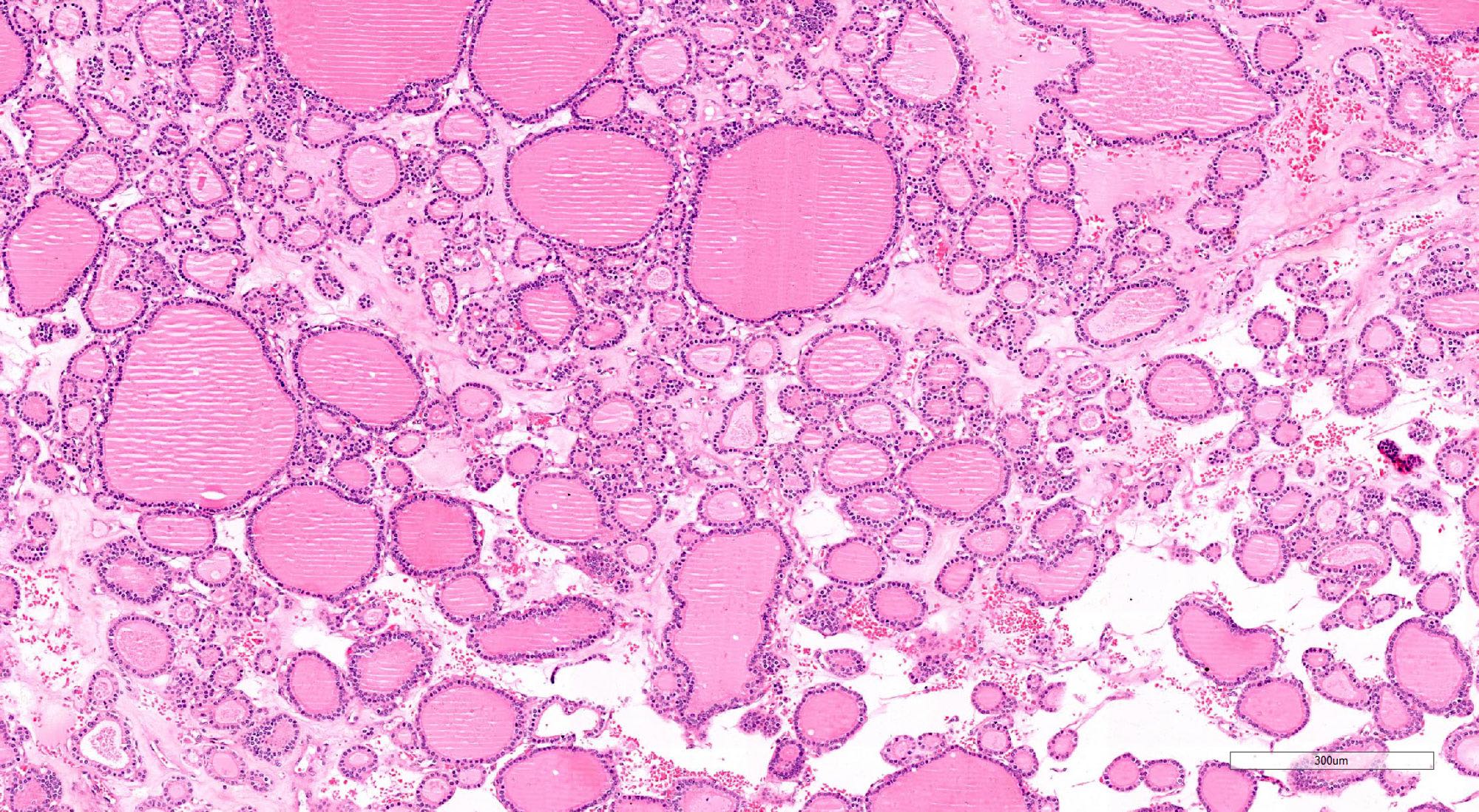
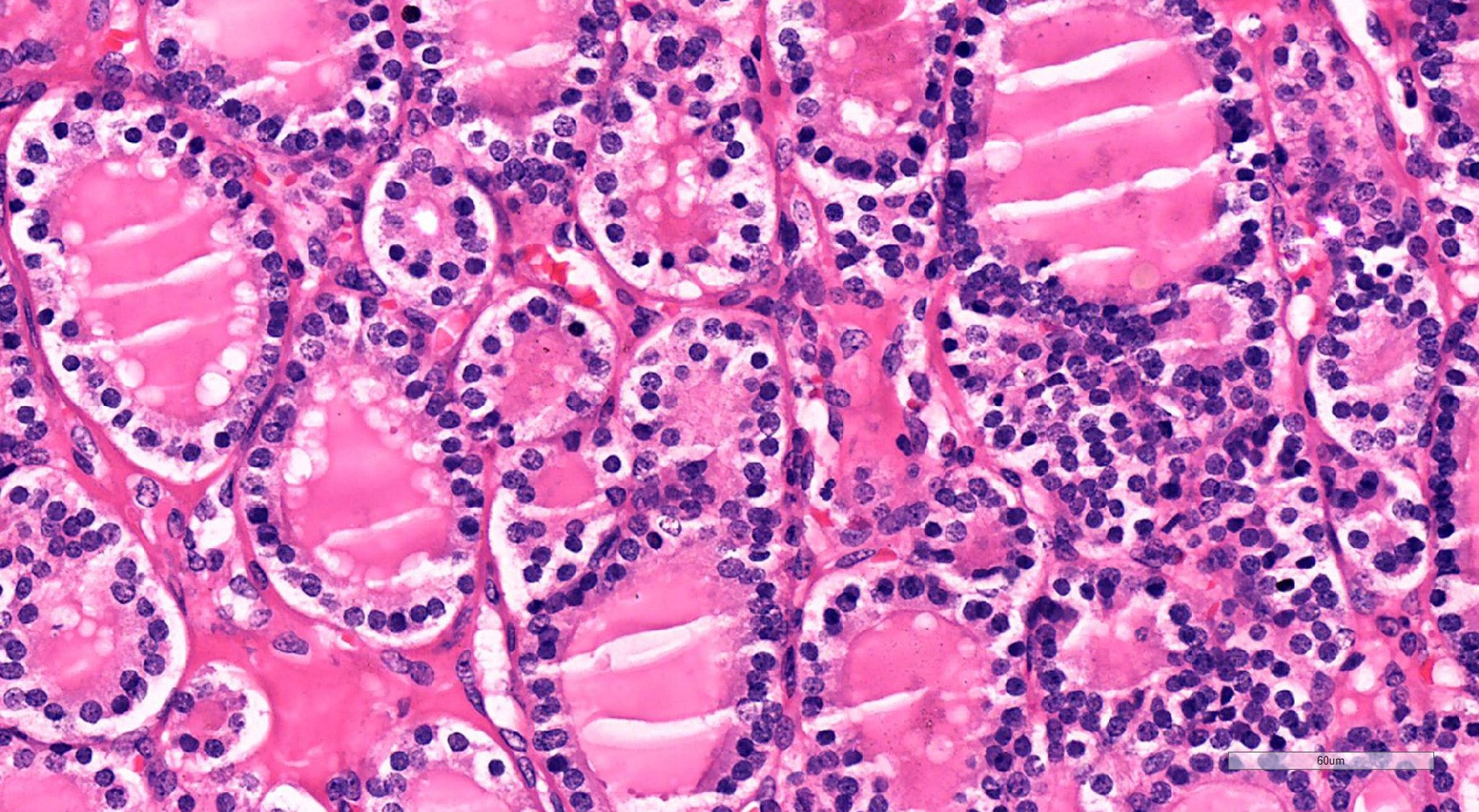
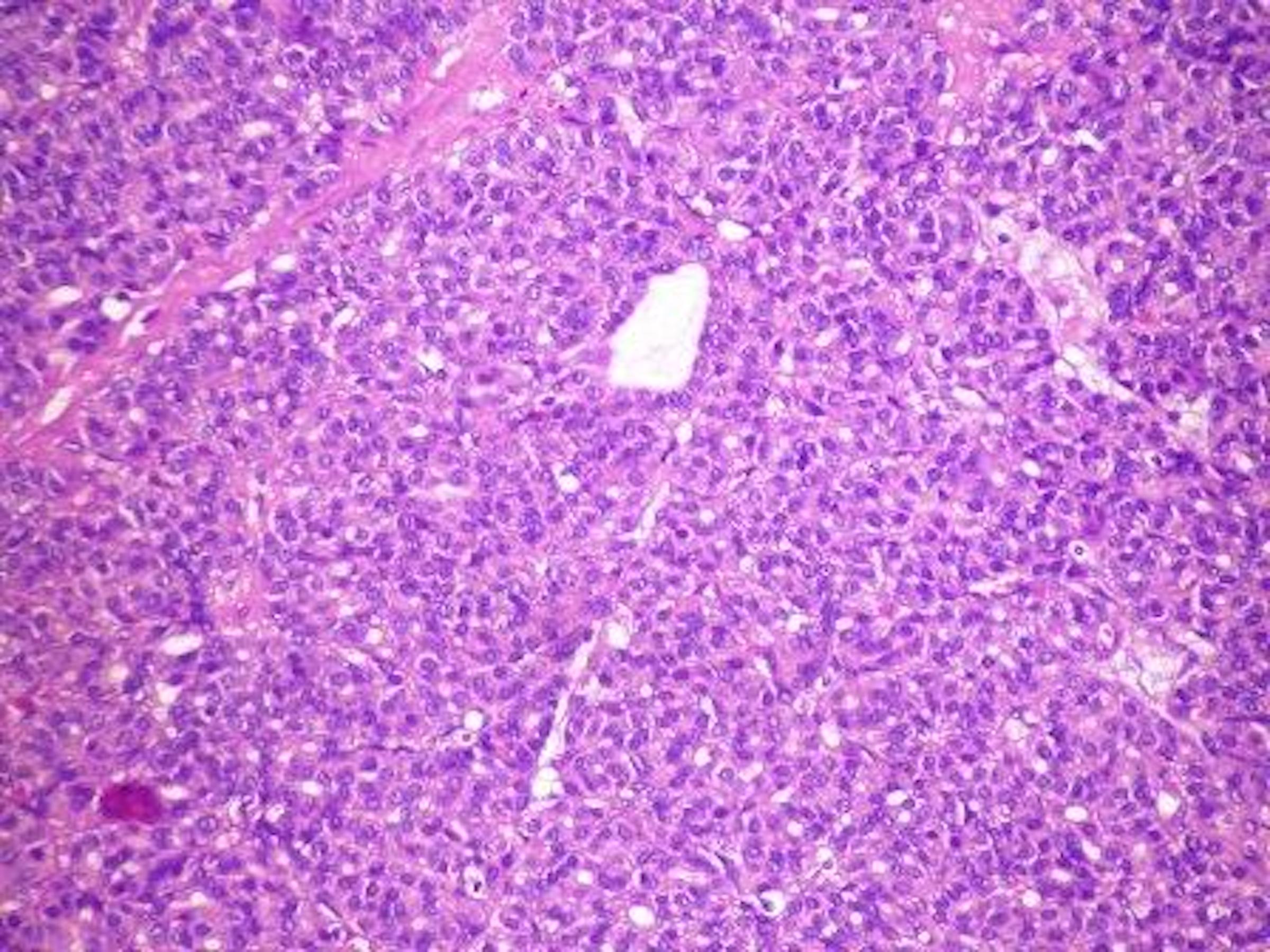
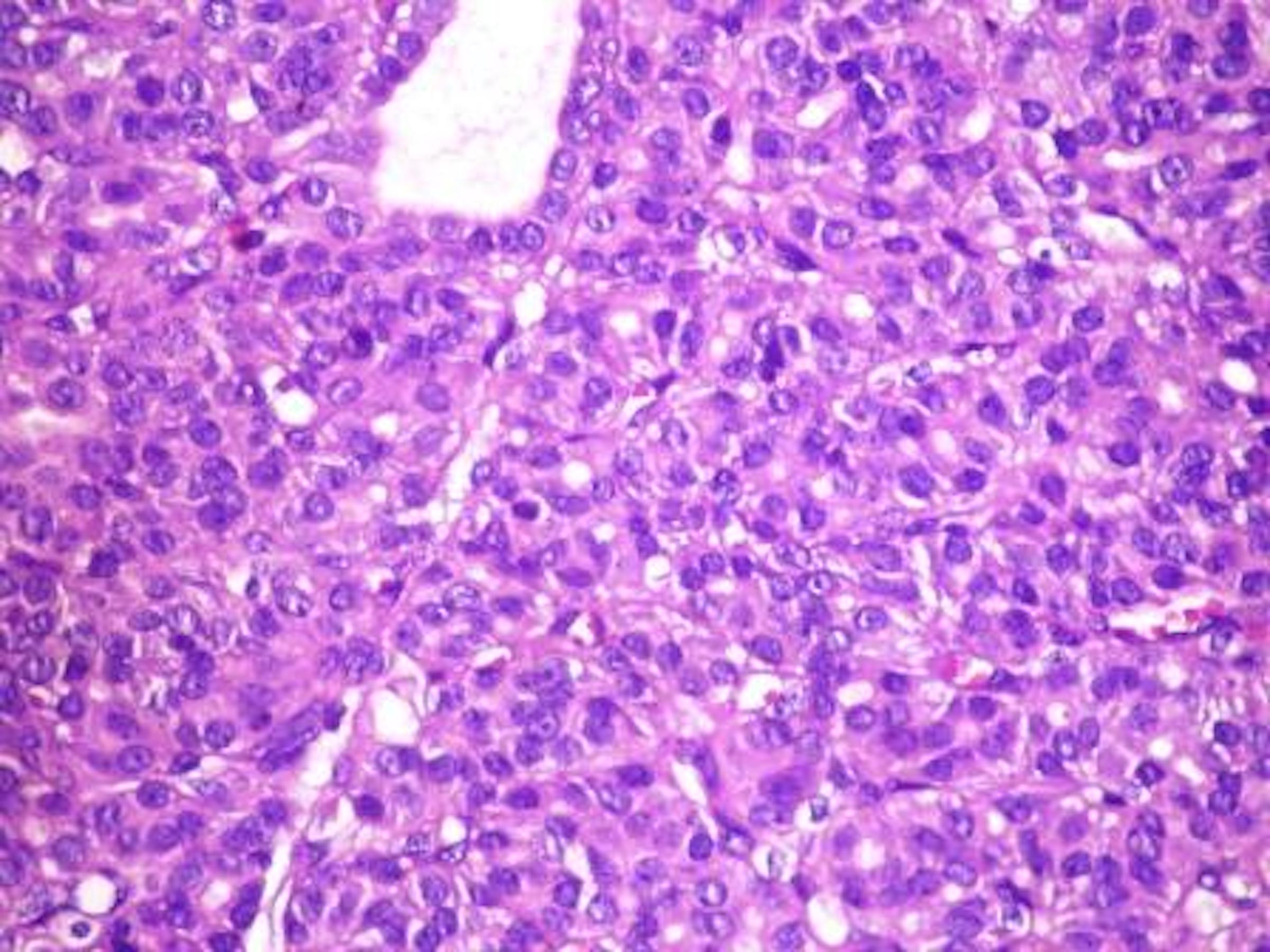
- Cuboidal to low columnar cells
- Small round nuclei, smooth nuclear boundary, uniformly hyperchromatic or euchromatic, dense chromatin, absent nuclear features of papillary thyroid carcinoma, nuclear score 0 or 1 (JAMA Oncol 2016;2:1023)
- Inconspicuous nucleoli
- Rarely, lipid filled vacuoles in cytoplasm
- Mitoses are uncommon
- Scant stroma
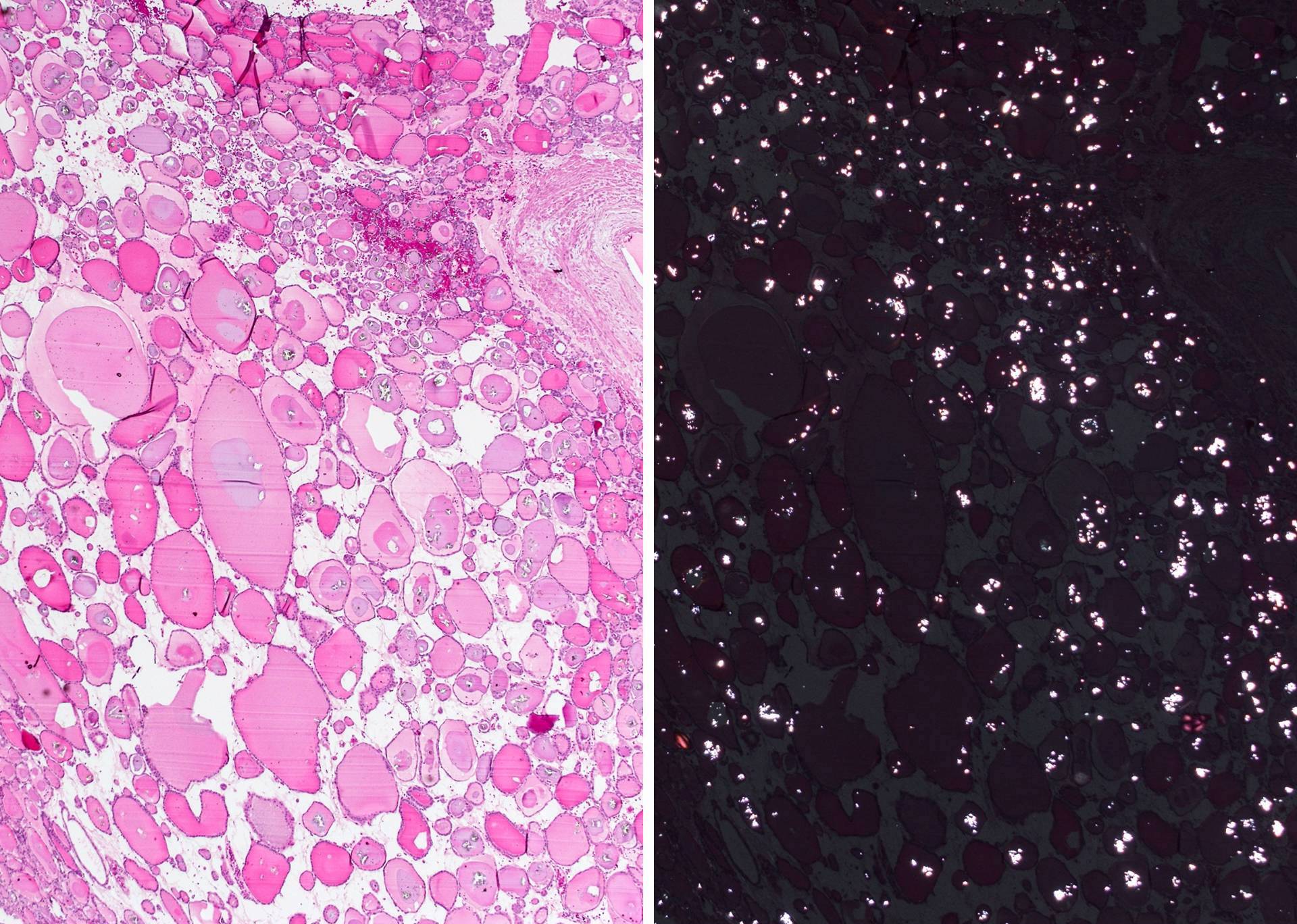
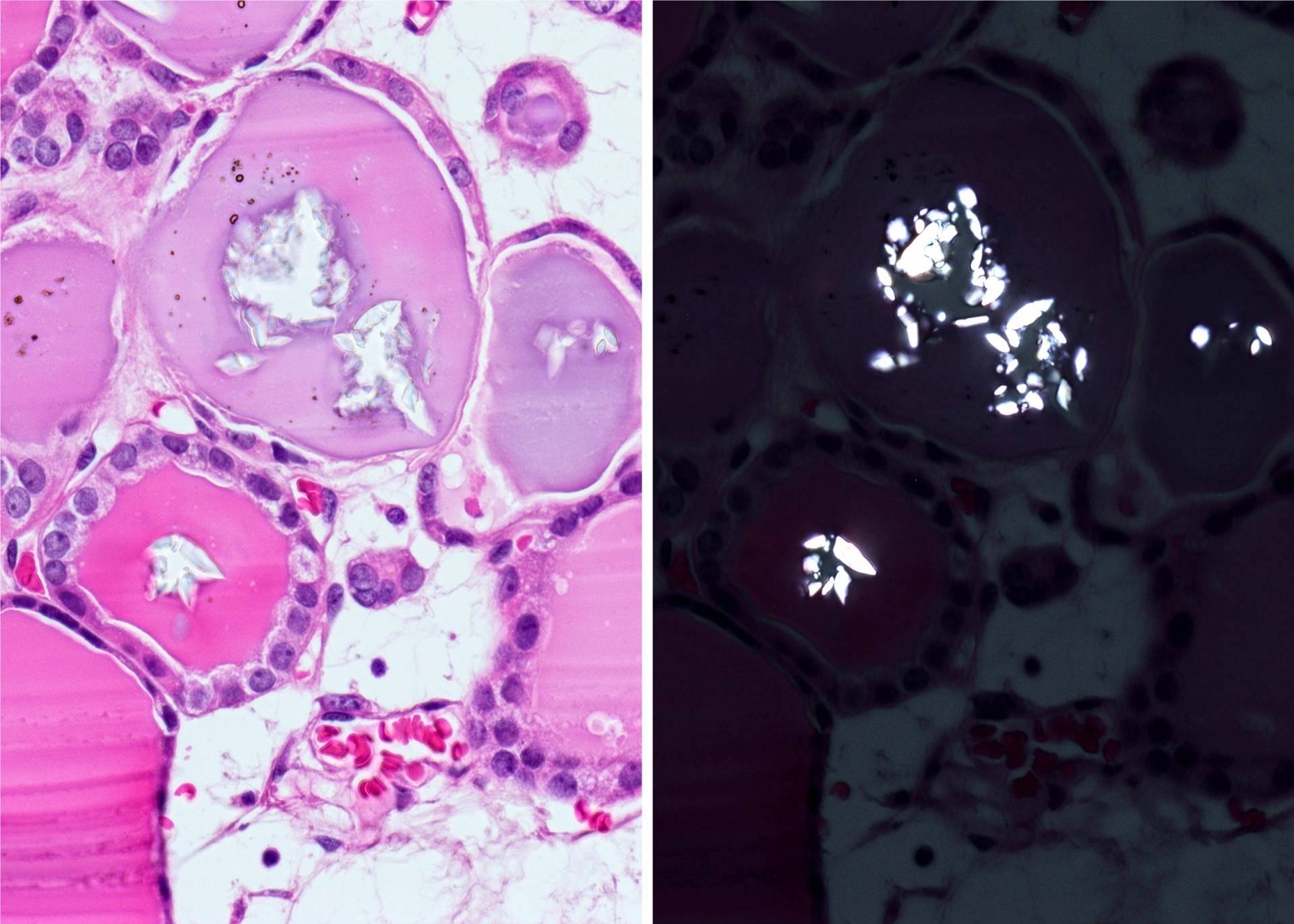
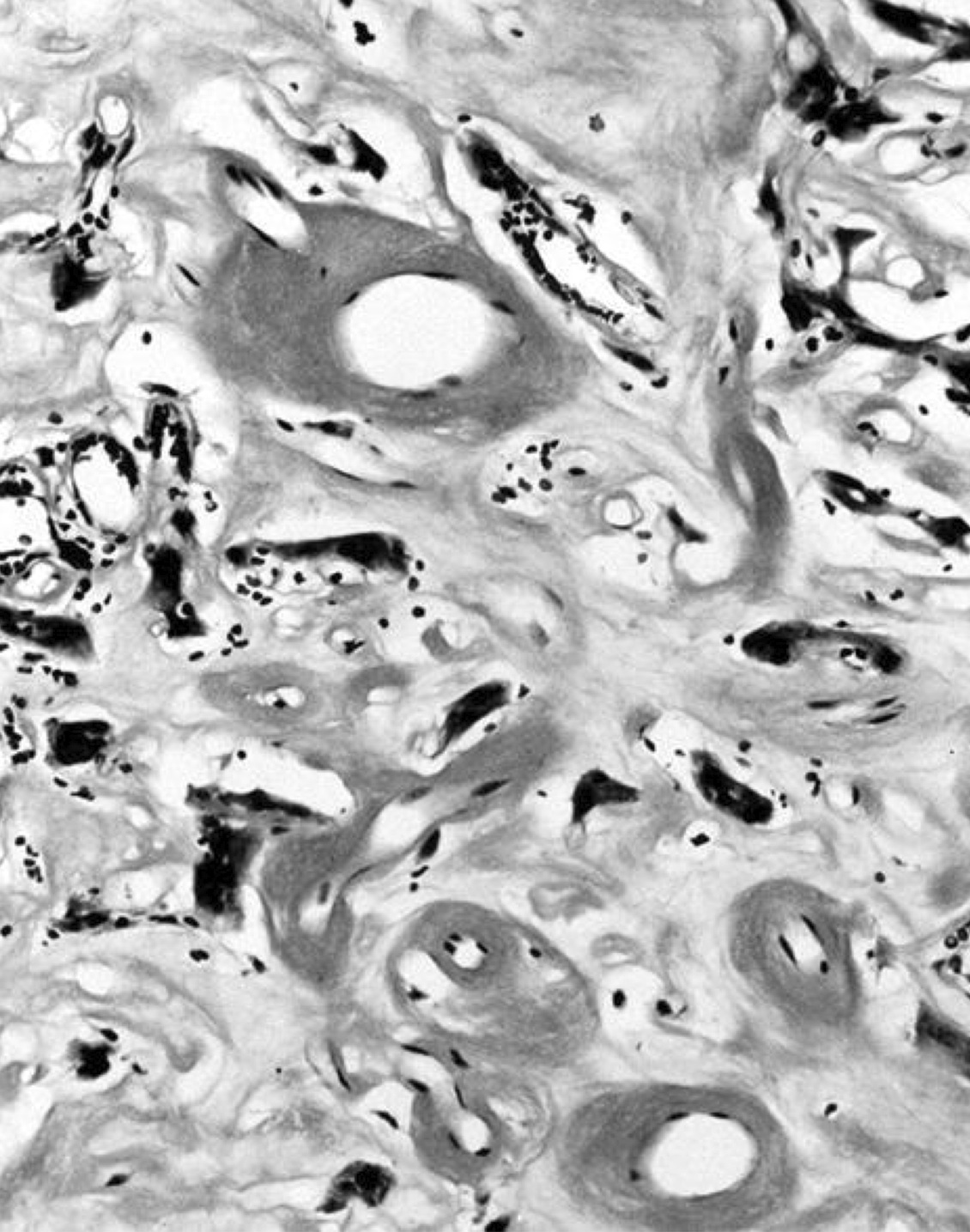
- Secondary changes: fibrosis, hyalinization, hemorrhage, hemosiderin deposition, edema, cystic degeneration, calcification, osseous or cartilaginous metaplasia
- Variants
- Hyperfunctioning adenoma (Plummer adenoma): tall columnar epithelium, papillary infoldings, vacuolated cytoplasm, watery colloid showing scalloping
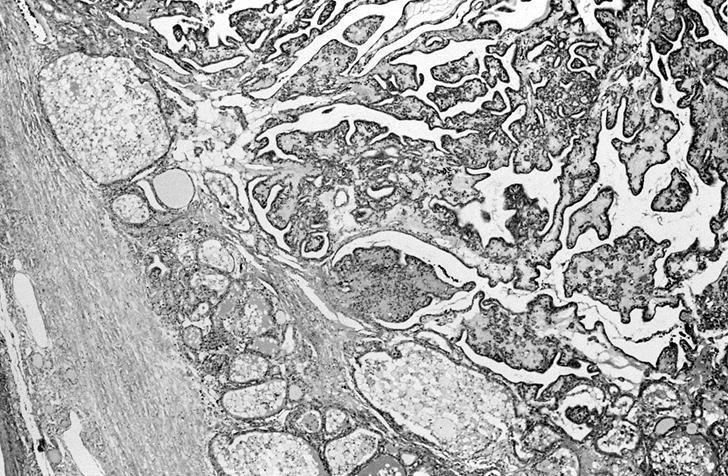
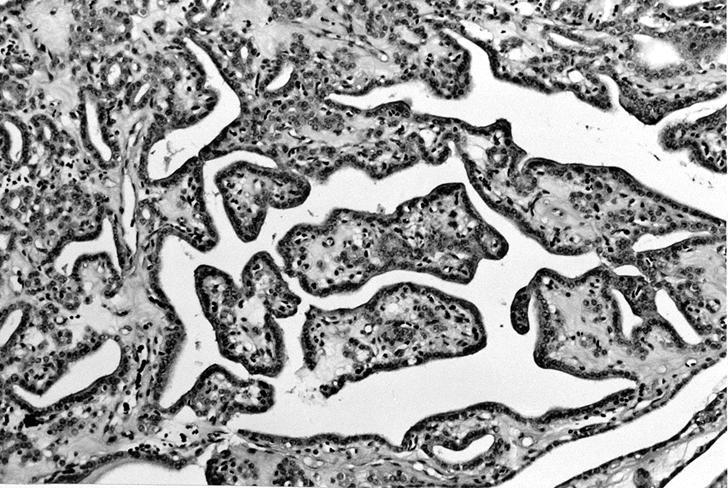
- Follicular adenoma with papillary hyperplasia: cystically dilated follicles, intraluminal papillae
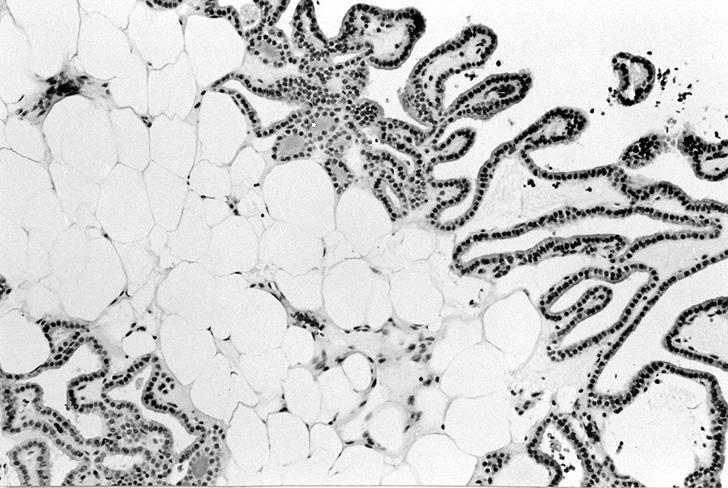
- Lipoadenoma: adipocytic metaplasia of the follicular adenoma
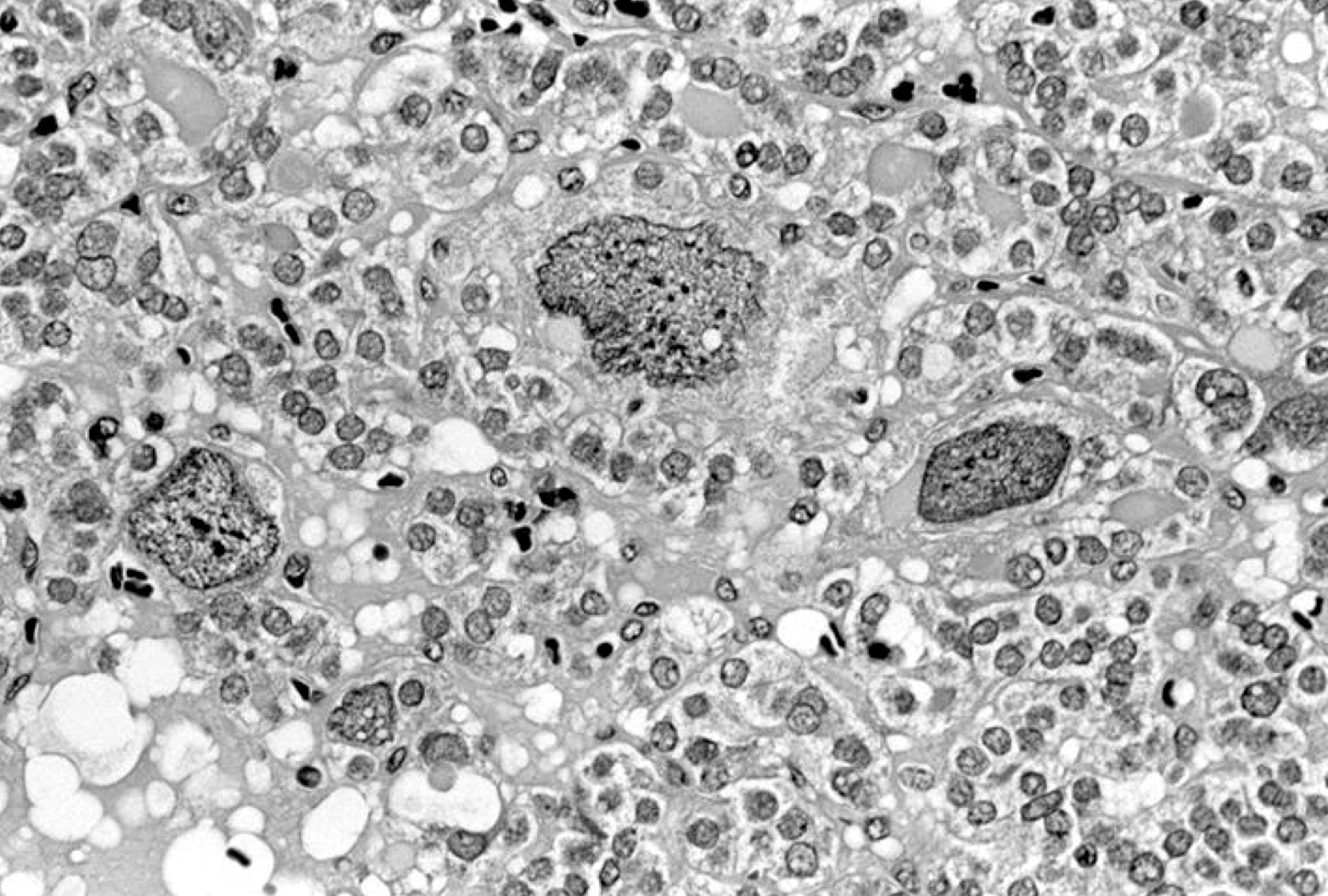
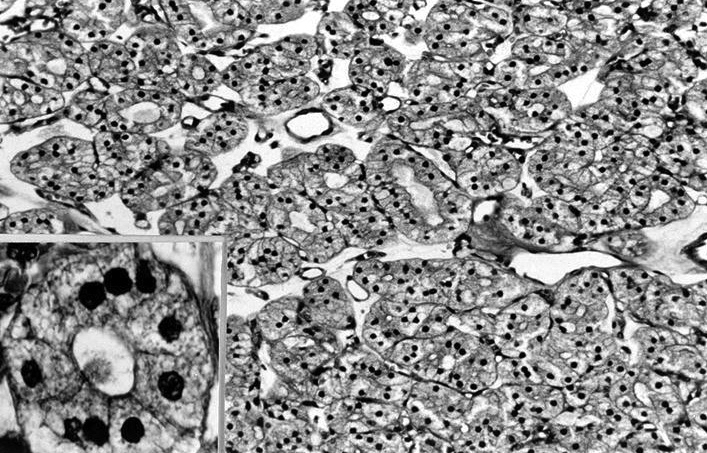
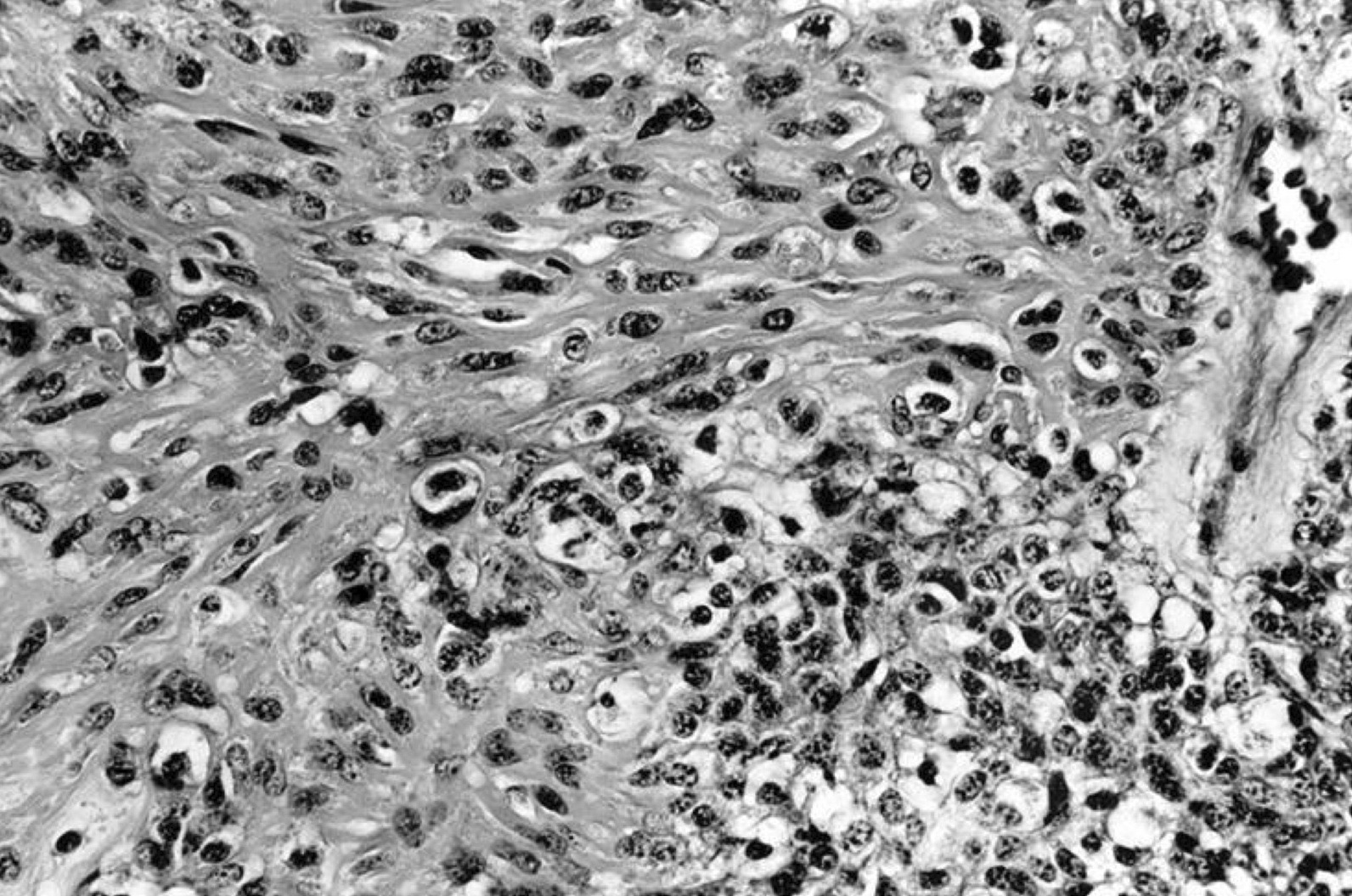
- Follicular adenoma with bizarre nuclei: may be seen after radiation exposure and in hyperfunctioning adenoma
- Signet ring cell follicular adenoma: signet ring cell change
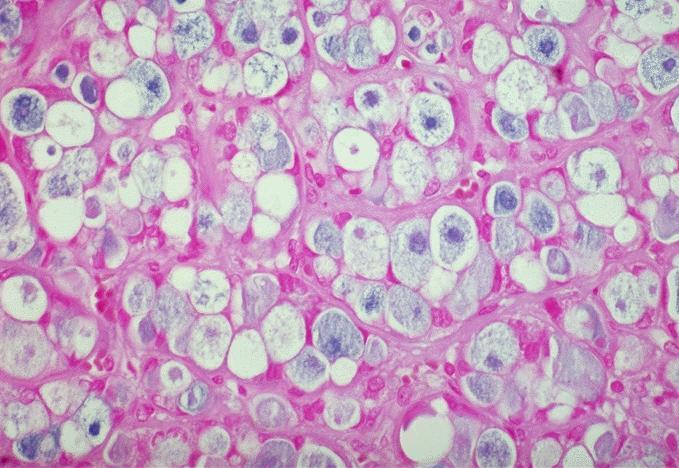
- Clear cell follicular adenoma: follicular adenoma with clear cell change
- Spindle cell follicular adenoma: spindle cell metaplasia
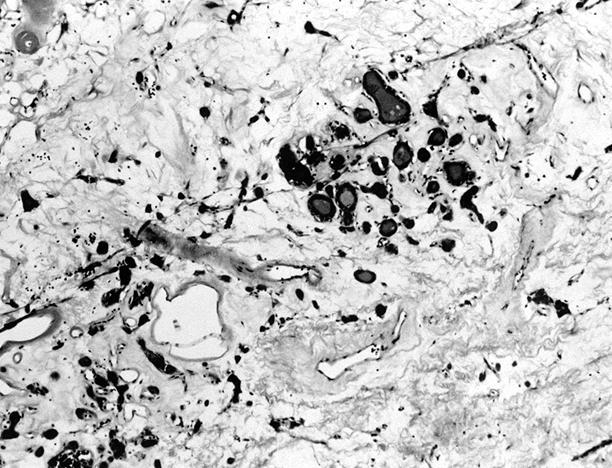
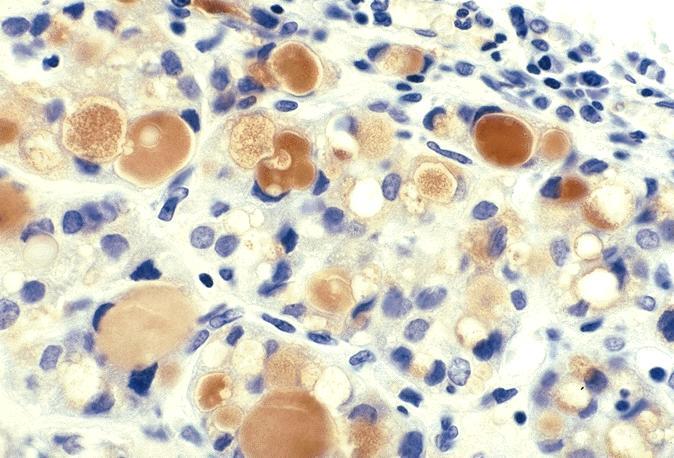
- Black follicular adenoma (black pigment in tumor cell cytoplasm; in patients on minocycline therapy)
- No capsular or vascular invasion after thorough sampling (at least 10 blocks)
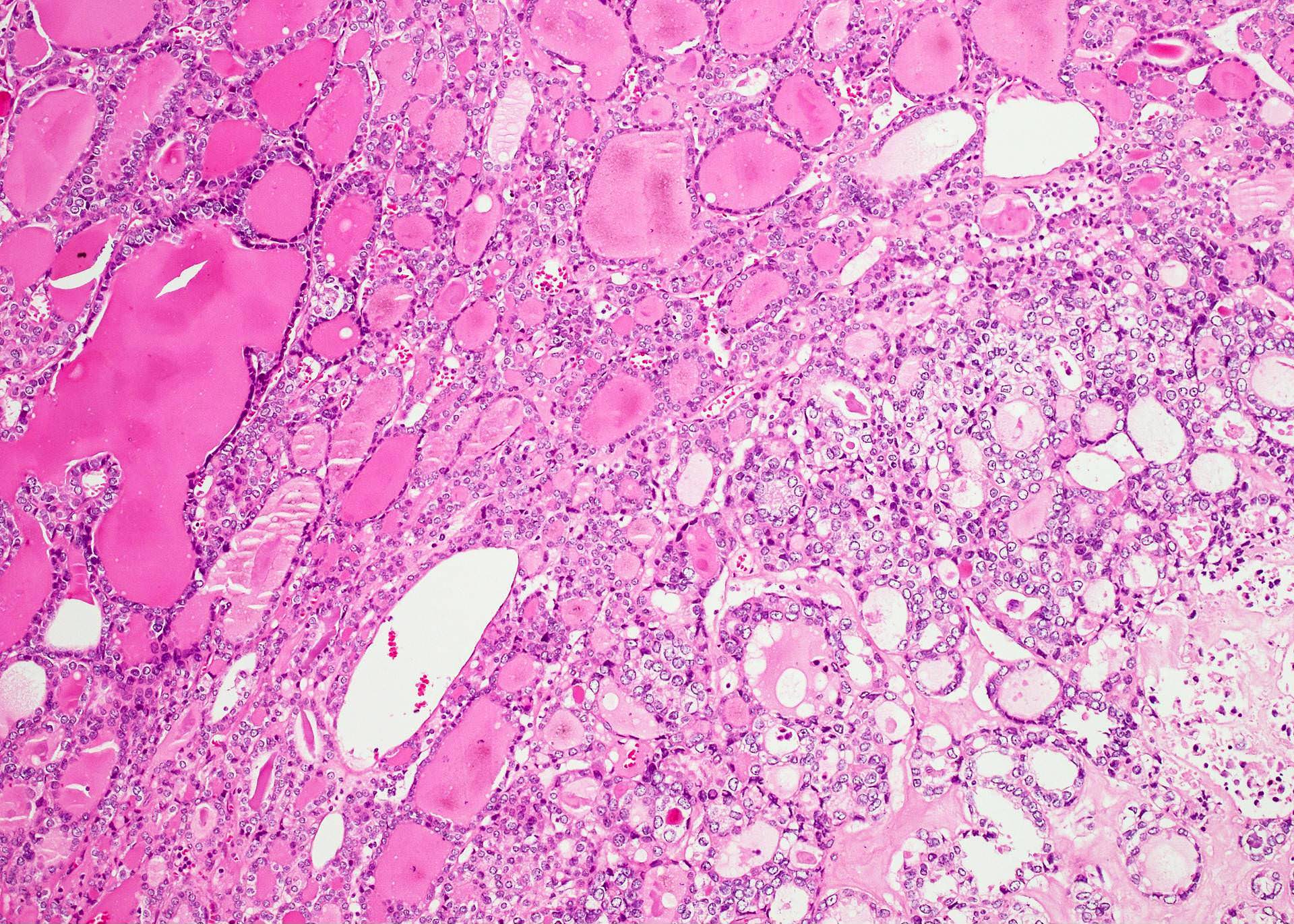
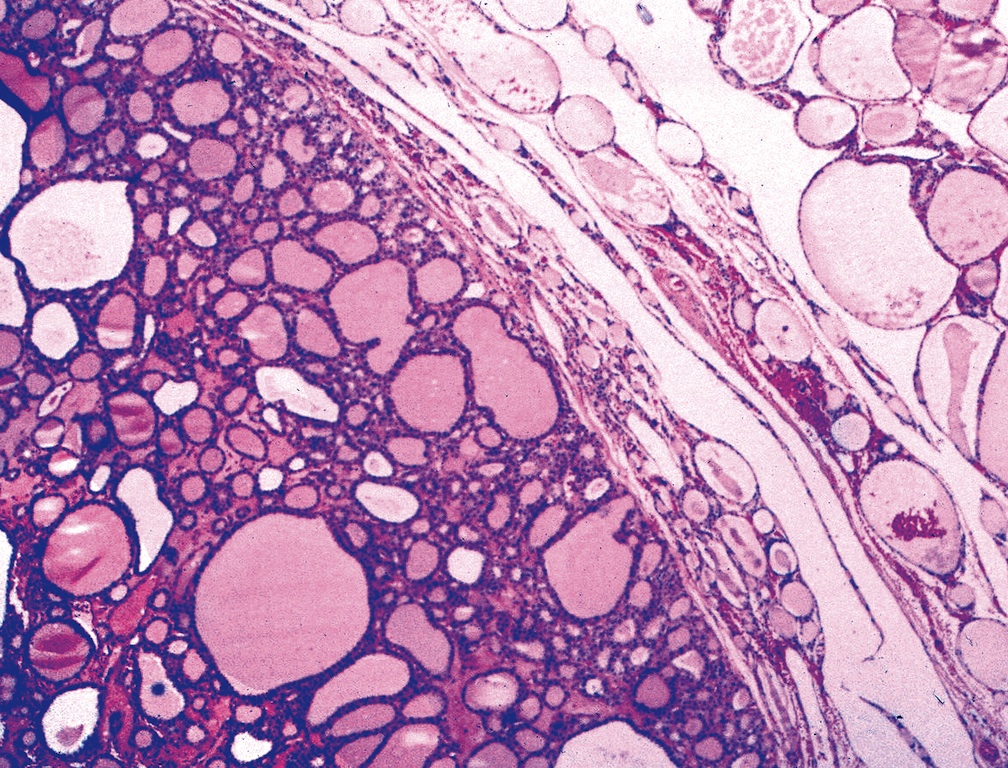
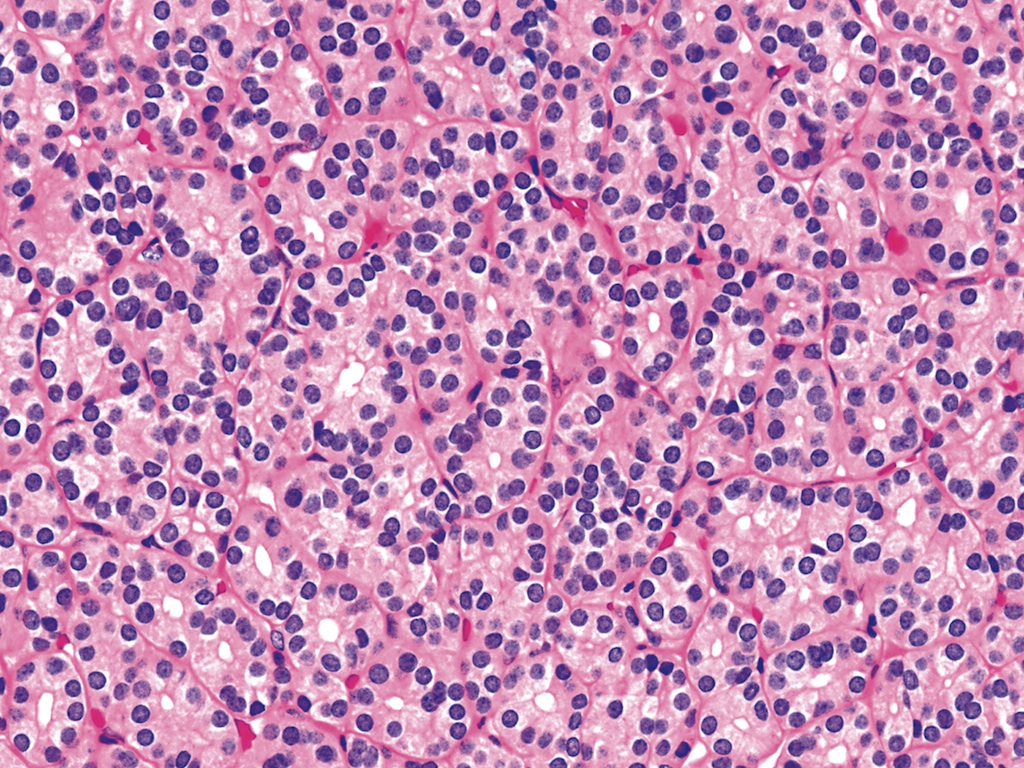
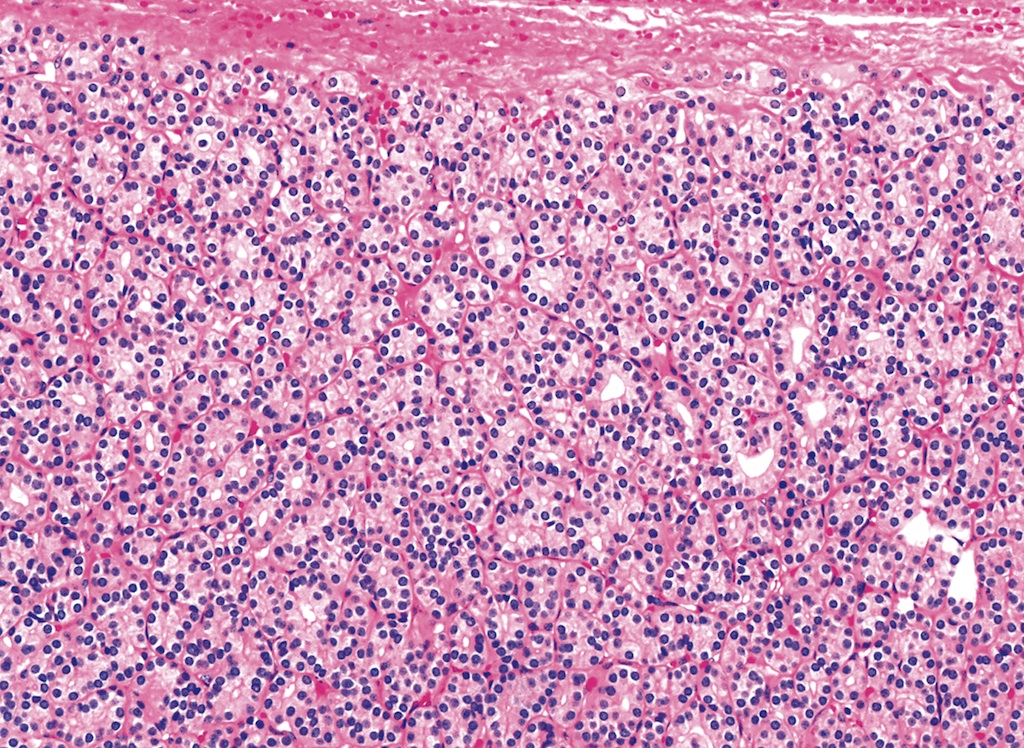
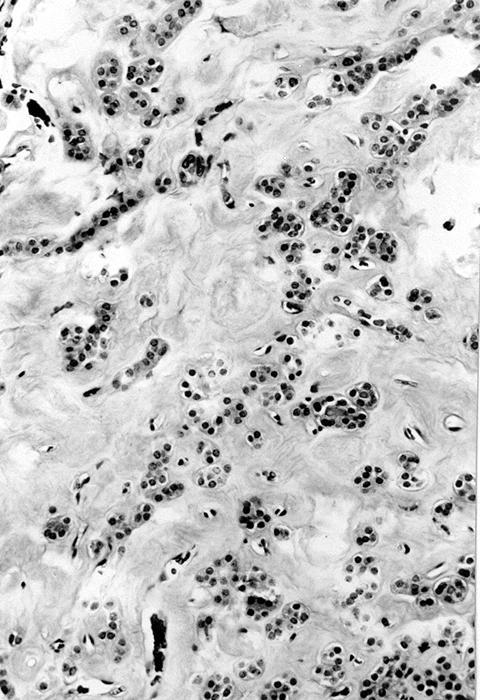
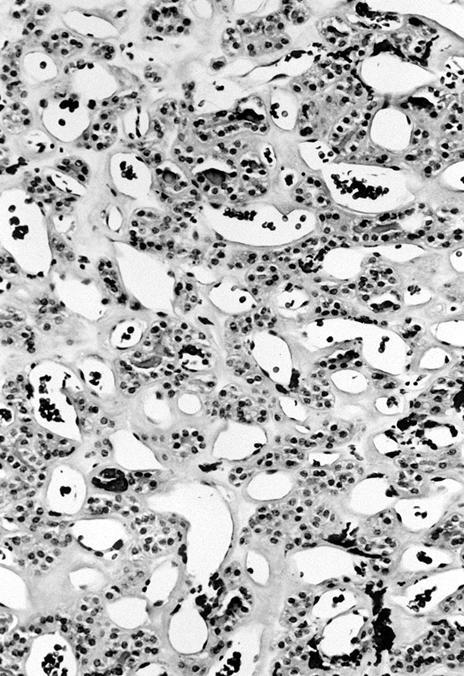
Microscopic (histologic) images
Contributed by Shipra Agarwal, M.D., Andrey Bychkov, M.D., Ph.D., Mark R. Wick, M.D., Asmaa Gaber Abdou, M.D. and AFIP
Patterns:
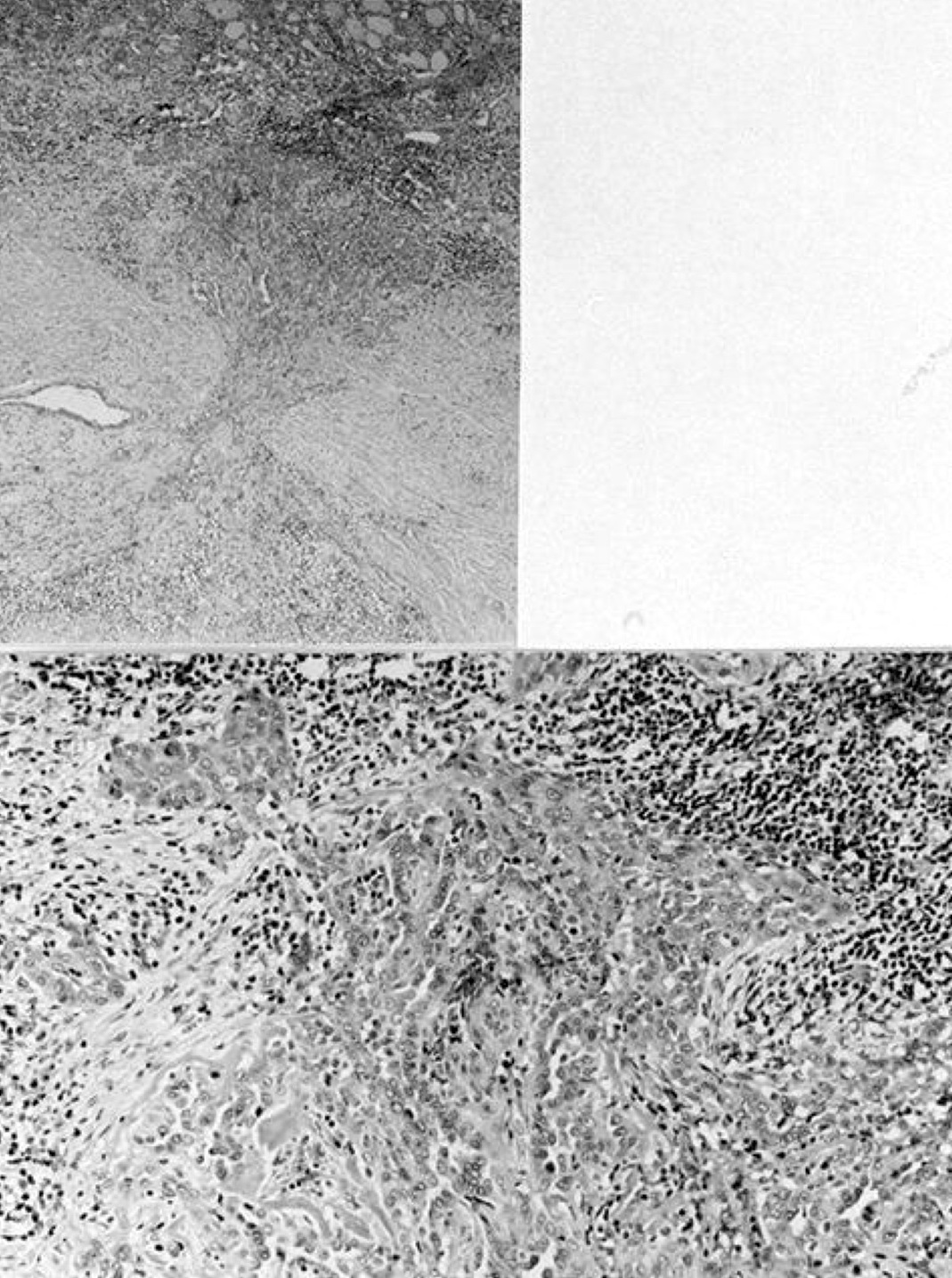
Atypical adenomas:
Not invasion:
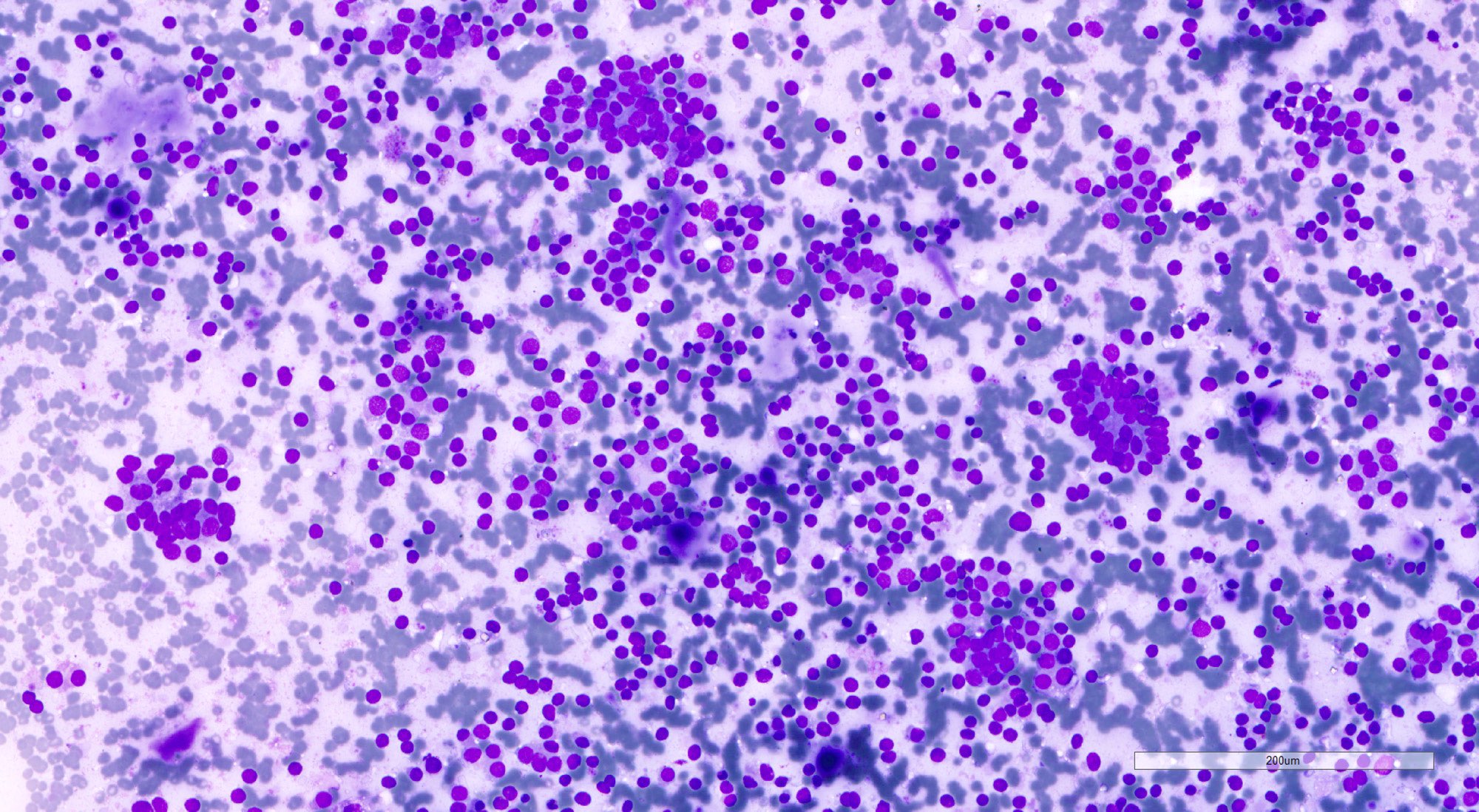
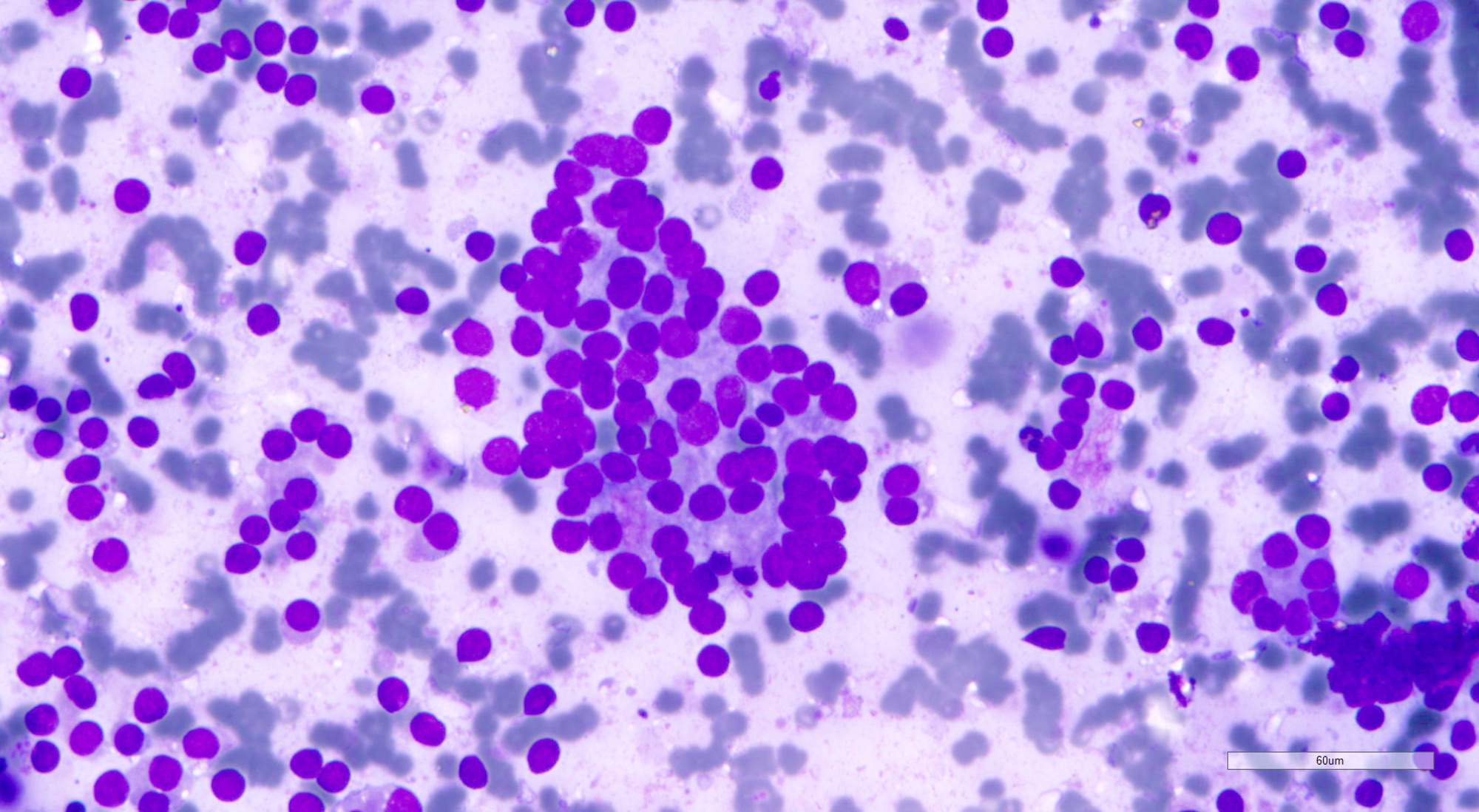
Cytology description
- Cellular aspirate (Korean J Pathol 2013;47:61, J Pathol Transl Med 2018;52:110)
- Cellular crowding
- Variable number of singly dispersed cells
- Microfollicular and solid / trabecular variants: numerous microfollicles, may have scant luminal colloid; absent or minimal background colloid
- Normofollicular and macrofollicular variants: monolayer sheets of follicular cells, abundant colloid; may mimic benign follicular nodule
- Hyperfunctioning follicular adenoma and follicular adenoma with papillary hyperplasia: monolayer sheets of polygonal cells with abundant cytoplasm, flame cells and occasionally, papillary fragments
- Uniform small round to ovoid nuclei, smooth nuclear margin, fine nuclear chromatin
- Absent nuclear features of papillary thyroid carcinoma
- The Bethesda System for Reporting Thyroid Cytopathology (TBSRTC) IV (follicular neoplasm / suspicious for a follicular neoplasm [FN / SFN]), III (atypia of undetermined significance [AUS A]) or II (benign) (Thyroid 2017;27:1341, Clin Endocrinol (Oxf) 2018;88:936)
- Cannot rule out follicular thyroid carcinoma based on cytologic findings
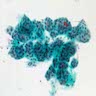
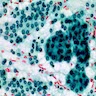
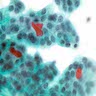
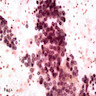
Cytology images
Positive stains
- Thyroid lineage specific markers
- PAX8
- Low molecular weight cytokeratin
- CD56
- Low proliferative index (Ki67 proliferative index < 5%)
- PPARG: rare; correlates with PAX8::PPARG translocation (Am J Surg Pathol 2002;26:1016)
Negative stains
- CK19: usually negative, may be weak and focal (Acta Endocrinol (Buchar) 2016;12:387)
- Chromogranin
- Synaptophysin
- Calcitonin
- CK20
- Rarely galectin3, HBME-1 and CITED1; up to 1 of these can be positive when used as a panel
- Can rarely be positive
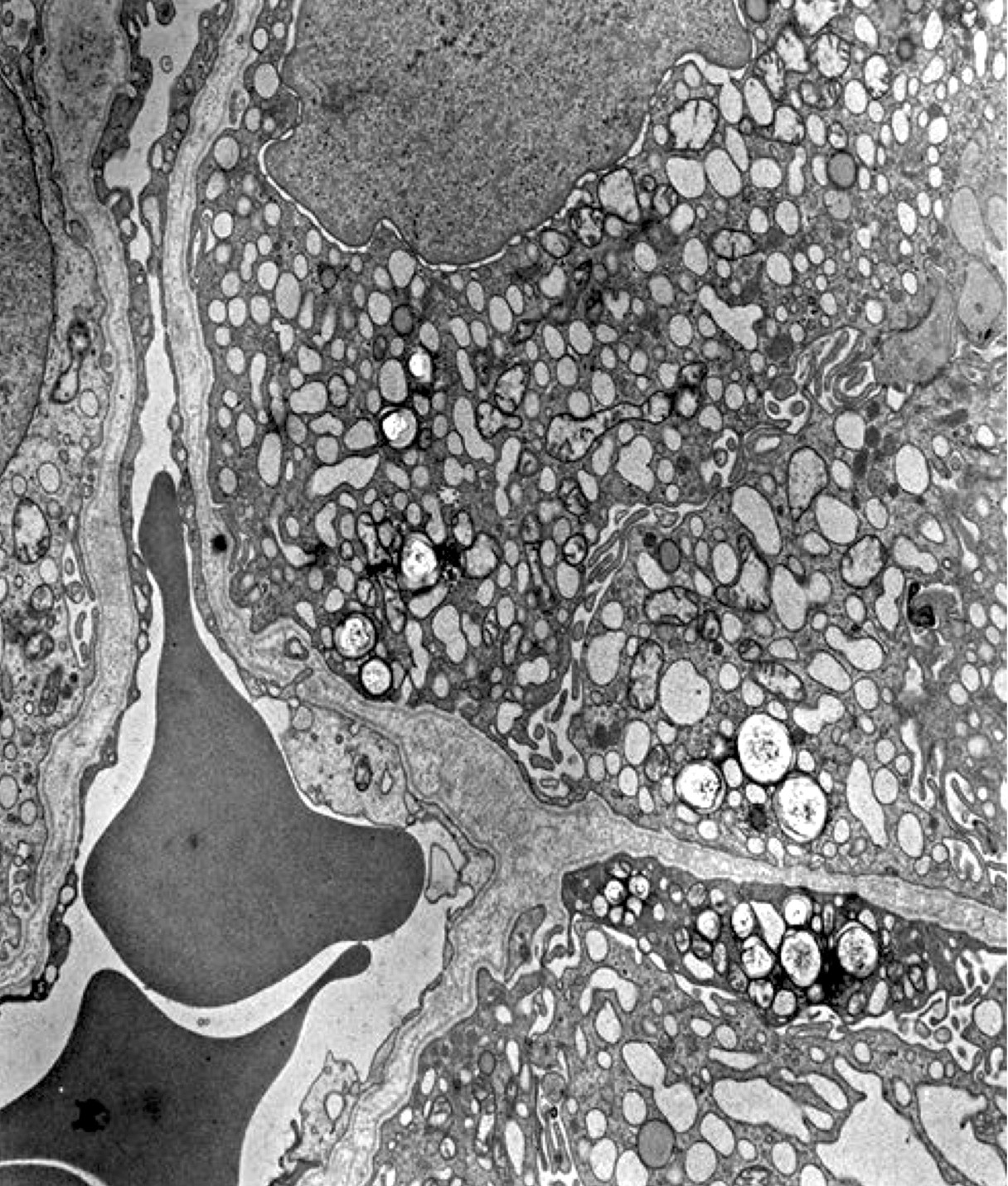
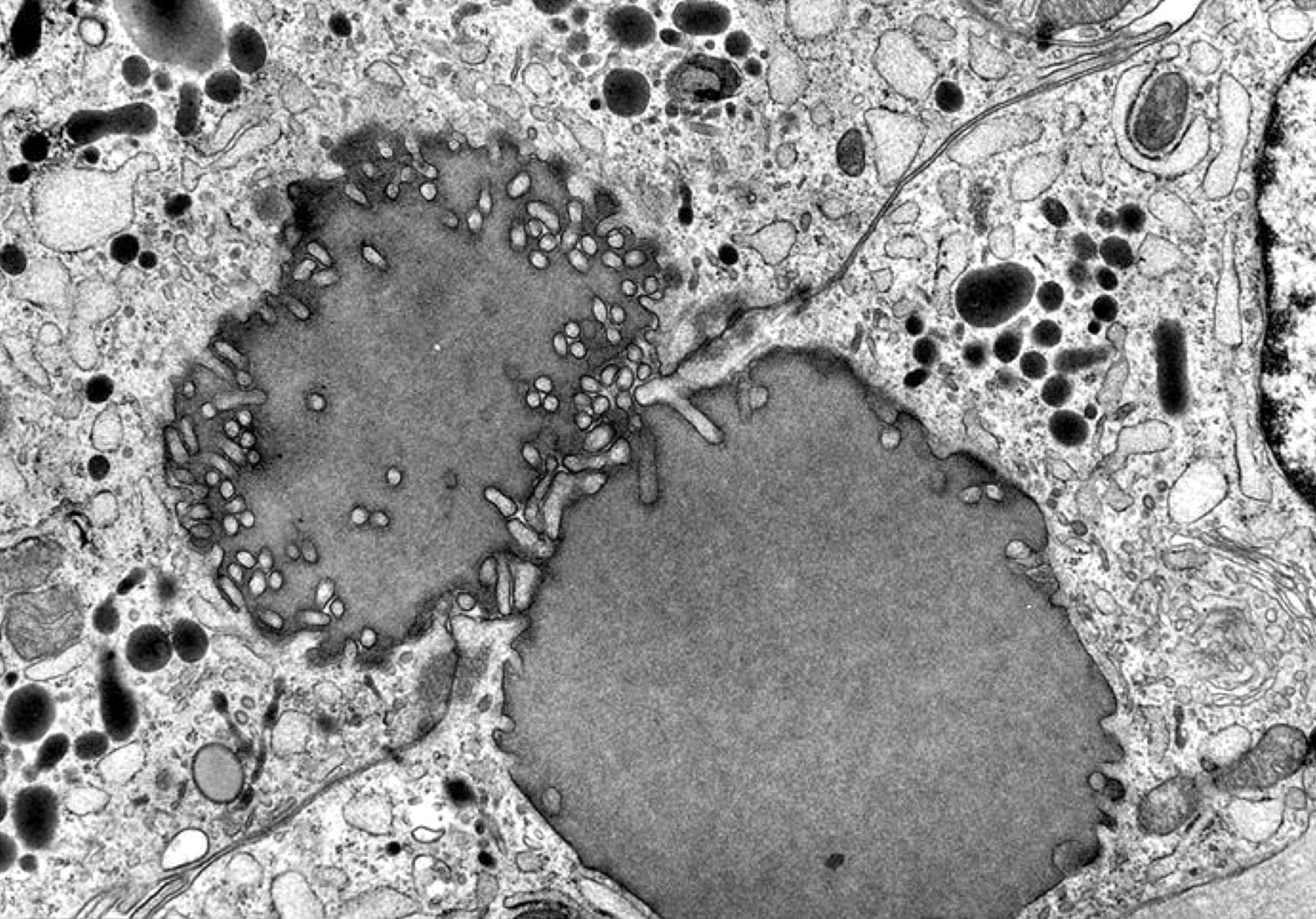
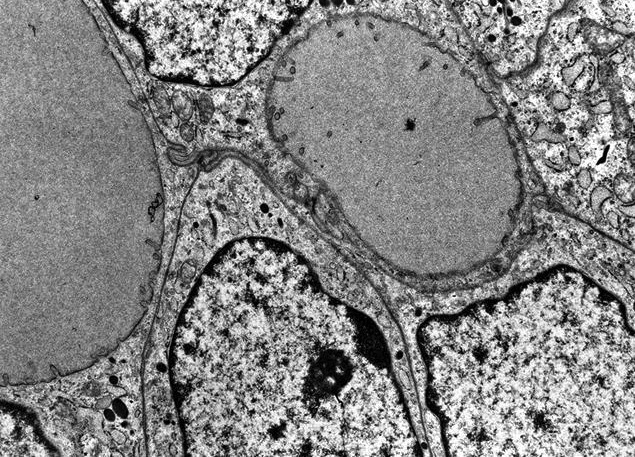
Electron microscopy description
- Similar to normal thyroid gland and hyperplastic nodules
- Hyperfunctioning follicular adenomas: organelle rich cytoplasm, especially rough endoplasmic reticulum; numerous, long microvilli on surface (Am J Clin Pathol 1982;78:299)
- Clear cell follicular adenomas: cytoplasmic vesicles of variable size; these may be dilated cisternae of the rough endoplasmic reticulum or mitochondria, lysosomes or endocytic vesicles (Virchows Arch A Pathol Anat Histol 1978;380:205)
Electron microscopy images
Molecular / cytogenetics description
- Clonal tumor
- RAS gene mutations (20 - 30%), most commonly codon 61 of NRAS, followed by codon 61 of HRAS and least frequently KRAS mutations (Oncotarget 2016;7:69638, PLoS Genet 2016;12:e1006239)
- EIF1AX alterations (10 - 15%) (Endocr Relat Cancer 2016;23:295, PLoS Genet 2016;12:e1006239)
- 13% (Diagn Pathol 2019;14:39)
- Microsatellite instability (MSI) (Mol Diagn Ther 2019;23:369)
- PTEN (5 - 20%) (Cancer Res 1997;57:4710)
- DICER1 (10%)
- BRAF K601E (< 1%)
- PIK3CA
- SPOP (Oncotarget 2016;7:69638)
- KMT2C
- KDM5C
- NF1
- TSHR mutations in 50 - 80% hyperfunctioning adenomas (J Clin Invest 2016;126:3383, J Mol Med (Berl) 2001;78:684)
- GNAS mutations in ~5% of hyperfunctioning adenomas
- EZH1 mutations in 20 - 30% of hyperfunctioning adenomas, usually in combination with TSHR or GNAS mutations
- THADA fusion (Thyroid 2021;31:1212)
- PAX8::PPARG fusion (~10%) (Cancer Genet Cytogenet 2010;196:7)
- Clonal cytogenetic abnormalities and copy number variations (~50%) (Cancer Genet Cytogenet 1998;101:42, PLoS Genet 2016;12:e1006239)
- Gene expression profile partially overlaps with minimally invasive follicular thyroid carcinoma and encapsulated follicular variant of papillary thyroid carcinoma; limited evidence (PLoS Genet 2016;12:e1006239, Oncotarget 2017;9:10343)
- Differential gene expression can help in differential diagnosis between follicular adenoma and follicular thyroid carcinoma (Int J Mol Sci 2017;18:1184, Endocr Connect 2018;7:124)
- Differential expression of miRNAs (miR-146-5p, miR-221-5p, miR-222-3p, miR-30e-3p, miR-152-3p, miR-185-5p, miR-1915-3p, miR-199b-5p, 199a-5p, miR-574-3p, miR-4516 and miR-148b-3p) in follicular adenoma in comparison to noninvasive follicular thyroid neoplasm with papillary-like nuclear features and infiltrative follicular variant of papillary thyroid carcinoma (Mod Pathol 2017;30:39)
Molecular / cytogenetics images
Images hosted on other servers:
Videos
Solitary thyroid nodule
Thyroid: compare and contrast
Histopathology thyroid: follicular adenoma (microfollicular)
Sample pathology report
- Thyroid, right lobectomy:
- Follicular adenoma, right lobe, 3.2 cm
Differential diagnosis
- Nodular hyperplasia with dominant nodule:
- Hyperplastic changes elsewhere in gland
- Often not encapsulated or incomplete capsule of variable thickness
- Variable architectural patterns
- May be multiple; lack of compression signs in adjacent thyroid gland
- Minimally invasive follicular thyroid carcinoma:
- Thick capsule
- Vascular or capsular invasion
- May show increased mitotic activity; may have foci of necrosis
- Immunoreactivity for > 1 of the following markers: galectin3, HBME-1, CITED1 and PPARG
- Presence of PAX8::PPARG or THADA fusions (Diagn Pathol 2010;5:9, Clin Chem 2010;56:391)
- Follicular variant of papillary carcinoma:
- Nuclear features of papillary thyroid carcinoma
- Invasive features, vascular or capsular invasion
- Immunopositive for multiple markers, namely CK19, galectin3, HBME-1, CITED1 and RET; immunonegative for CD56 (Acta Endocrinol (Buchar) 2016;12:387, Diagn Pathol 2010;5:9, Pathol Res Pract 2009;205:303)
- Noninvasive follicular thyroid neoplasm with papillary-like nuclear features (NIFTP):
- Nuclear features of papillary thyroid carcinoma with a nuclear score of 2 or 3 (JAMA Oncol 2016;2:1023)
- Well differentiated tumor of uncertain malignant potential (WDT-UMP):
- Encapsulated tumor
- Equivocal nuclear features of papillary thyroid carcinoma
- Questionable blood vessel or capsular invasion
- Follicular tumor of uncertain malignant potential (FT-UMP):
- Encapsulated tumor
- Questionable vascular or capsular invasion
- Lacks nuclear features of papillary thyroid carcinoma
- Papillary thyroid carcinoma, encapsulated variant:
- Among differential diagnosis of follicular adenoma with papillary hyperplasia
- Nuclear features of papillary thyroid carcinoma
- Papillary thyroid carcinoma, tall cell variant:
- Intrathyroidal parathyroid adenoma / hyperplasia:
- Can mimic follicular adenoma of microfollicular, clear cell type
- Positive for PTH, GATA3, chromogranin, synaptophysin
- Negative for thyroglobulin, TTF1
- Encapsulated medullary thyroid carcinoma of solid or trabecular pattern or with spindle or clear cells:
- Invasive features
- Amyloid deposition
- Salt and pepper chromatin
- Calcitonin positive, thyroglobulin negative
Additional references
Practice question #1
Which of the following best describes this thyroid tumor?
- Benign, completely encapsulated, lacks nuclear features of papillary thyroid carcinoma, absent capsular and vascular invasion
- Benign, partially encapsulated, lacks nuclear features of papillary thyroid carcinoma, absent capsular and vascular invasion
- Malignant, encapsulated, lacks nuclear features of papillary thyroid carcinoma, capsular invasion present
- Uncertain malignant potential, completely encapsulated, lacks nuclear features of papillary thyroid carcinoma, questionable capsular invasion
- Uncertain malignant potential, completely encapsulated, nuclear score 2, lacks capsular and vascular invasion
Practice answer #1
A. Benign, completely encapsulated, lacks nuclear features of papillary thyroid carcinoma, absent capsular and vascular invasion. Follicular adenoma is a benign encapsulated tumor, which lacks capsular and vascular invasion as well as nuclear features of papillary thyroid carcinoma. Answer B is incorrect because follicular adenoma is completely encapsulated, unlike a case of nodular hyperplasia with a dominant nodule that can be unencapsulated or partially encapsulated. Answer C is incorrect because follicular adenoma lacks capsular invasion and is benign, unlike a case of follicular thyroid carcinoma. Answer D is incorrect because follicular adenoma is completely encapsulated, lacks even doubtful foci of invasion and is benign. This will be a case of a follicular tumor of uncertain malignant potential. Answer E is incorrect because follicular adenoma has a nuclear score of 0 or 1 and is benign. A tumor with a nuclear score of 2 and lacking capsular and vascular invasion will be noninvasive follicular thyroid neoplasm with papillary-like nuclear features (NIFTP).
Comment Here
Reference: Follicular adenoma
Comment Here
Reference: Follicular adenoma
Practice question #2
Which of the following immunohistochemical / molecular profiles best fits with the diagnosis of follicular adenoma?
- Galectin3+, HBME-1+, CITED1+
- PAX8-, calcitonin+, chromogranin+
- TTF1+, CD56+, PAX8+
- TTF1+, CK19+, HBME-1+
- TTF1-, synaptophysin+, GATA3+
Practice answer #2
C. TTF1+, CD56+, PAX8+. Follicular adenoma is immunopositive for TTF1, thyroglobulin, PAX8, CK7 and CD56. Answer A is incorrect because follicular adenoma shows immunoreactivity for no more than 1 of the following markers: galectin3, HBME-1 and CITED1. Answer D is incorrect because CK19 is commonly positive in papillary thyroid carcinoma. Answers B and E are incorrect because calcitonin and GATA3 label medullary thyroid carcinoma and parathyroid tissue, respectively.
Comment Here
Reference: Follicular adenoma
Comment Here
Reference: Follicular adenoma