Table of Contents
Definition / general | Essential features | Terminology | ICD coding | Epidemiology | Sites | Pathophysiology | Etiology | Clinical features | Diagnosis | Radiology description | Prognostic factors | Case reports | Treatment | Gross description | Gross images | Microscopic (histologic) description | Microscopic (histologic) images | Virtual slides | Cytology description | Positive stains | Negative stains | Molecular / cytogenetics description | Sample pathology report | Differential diagnosis | Additional references | Practice question #1 | Practice answer #1 | Practice question #2 | Practice answer #2Cite this page: Shen DL, MacLennan G. Clear cell papillary renal cell tumor. PathologyOutlines.com website. https://www.pathologyoutlines.com/topic/kidneytumorclearcellpapillary.html. Accessed October 5th, 2025.
Definition / general
- Indolent tumor with clear glycogen rich cytoplasm, luminal nuclear polarization, inconspicuous nucleoli and with papillary architecture with fibrovascular stroma
- Distinctive immunohistochemical profile: positive CK7 and CAIX, with negative or patchy CD10 and AMACR
Essential features
- Renamed in WHO 5th edition to reflect indolent behavior (previously was designated as a renal cell carcinoma)
- Clear cytoplasm, luminal nuclear polarization, low nuclear grade (histologic grade 1 - 2)
- Papillary architecture with fibrovascular stroma
- CK7 / CAIX positive; CD10 / AMACR patchy or negative
- Lacks features of high grade malignancies, including necrosis and vascular invasion
- No reported metastasis or recurrence following adequate resection
Terminology
- Not recommended / no longer used: clear cell papillary tumor, clear cell papillary renal cell carcinoma, clear cell tubulopapillary renal cell carcinoma, renal angiomyoadenomatous tumor (Am J Surg Pathol 2010;34:1608, Ann Diagn Pathol 2000;4:311)
ICD coding
- ICD-O: 8323/1 - clear cell papillary renal cell carcinoma
Epidemiology
- 3 - 4% of all renal tumors, mean age of 58.2 years (Mod Pathol 2013;26:697, Hum Pathol 2014;45:59)
- Age: 8 - 88 years
- No gender predilection
- Arises sporadically and with end stage renal disease (ESRD) (Int J Clin Exp Pathol 2014;7:7312)
Sites
- Renal cortex; predominately unifocal, with multifocality in 25% of cases (multifocality is predominantly seen in ESRD patients)
Pathophysiology
- Unknown at this time
Etiology
- Etiology is unclear; lacks genetic modifications and driver mutations frequently associated with other renal cell carcinomas (RCC)
- First described in association with ESRD, particularly acquired cystic disease of the kidney (ACDK) (Am J Surg Pathol 2006;30:141)
- It is now known that most cases arise sporadically, with no evidence of somatic VHL gene inactivation or chromosome 3p loss, unlike clear cell renal cell carcinoma (CCRCC) (Arch Pathol Lab Med 2019;143:1154)
- Believed to be associated with upregulation of the hypoxia inducible factor 1 pathway, similar to other RCCs but through a non-VHL dependent mechanism
- Evidence suggests a shift away from respiratory metabolism, toward sorbitol pathway of tumorigenesis (Elife 2019;8:e38986)
Clinical features
- Usually discovered incidentally during imaging for unrelated disorders (80%) and occasionally with local symptoms (18%) (Eur Urol 2021;79:468)
- Some cases arise in patients with ESRD
- Indolent behavior with presentation at low tumor stage (usually pT1) (Am J Surg Pathol 2013;37:1469)
- No reported metastasis or recurrence in cases with typical pathologic features (Am J Surg Pathol 2013;37:1469)
- May present with multifocal or bilateral tumor distribution (Int J Mol Sci 2021;23:151)
Diagnosis
- Usually initially identified by radiographic imaging (CT or ultrasound)
- Diagnosis confirmed after surgical resection and microscopic examination
Radiology description
- Generally 2 categories of findings: solid and cystic, with Bosniak III or IV features (Urology 2017;103:136, AJR Am J Roentgenol 2020;214:579)
- Solid: mass with relatively low level enhancement, with well defined margins
- Cystic: heterogeneous regions of hyper enhancement and predominantly unilocular
- These findings are shared with both clear cell and papillary renal cell carcinoma enhancement patterns
Prognostic factors
- Unknown at this time
Case reports
- 50 year old man with glomerulonephritis on hemodialysis and 22 mm unifocal renal tumor (IJU Case Rep 2021;4:127)
- 55 year old man with bilateral tumors and concurrent unifocal neuroendocrine tumor in the setting of chronic kidney disease (Case Rep Pathol 2017;2017:9672368)
- 57 year old man with multiple renal tumors (Pathol Res Pract 2016;212:229)
- 58 year old man with concurrent ipsilateral tumor and mucinous tubular and spindle cell carcinoma (Nihon Hinyokika Gakkai Zasshi 2020;111:134)
- 63 year old woman post kidney transplant with multifocal tumor in renal allograft (Can J Urol 2019;26:9794)
- 70 year old man with incidentally found 2 cm renal mass and a history of treated fibrous histiocytoma and liposarcoma (World J Nephrol 2018;7:155)
Treatment
- Radical nephrectomy or nephron sparing surgery, including partial nephrectomy or cryoablation therapy
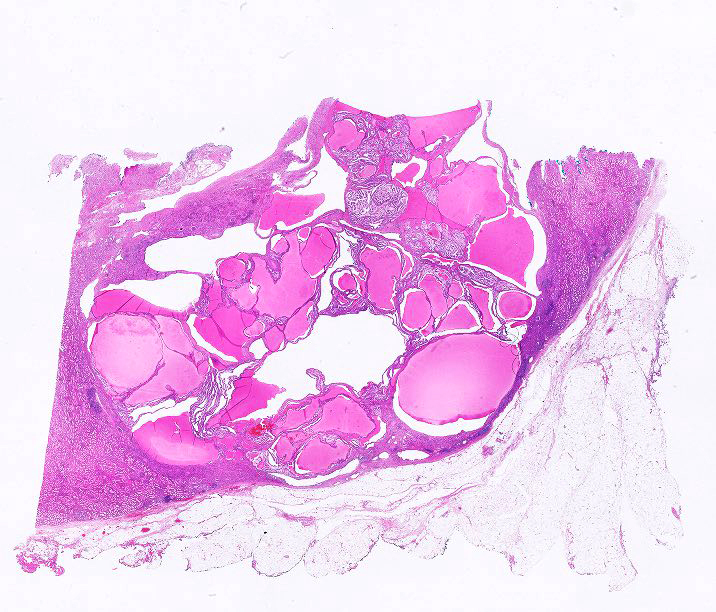
Gross description
- Mean size: 2.0 cm (0.2 - 7.5 cm)
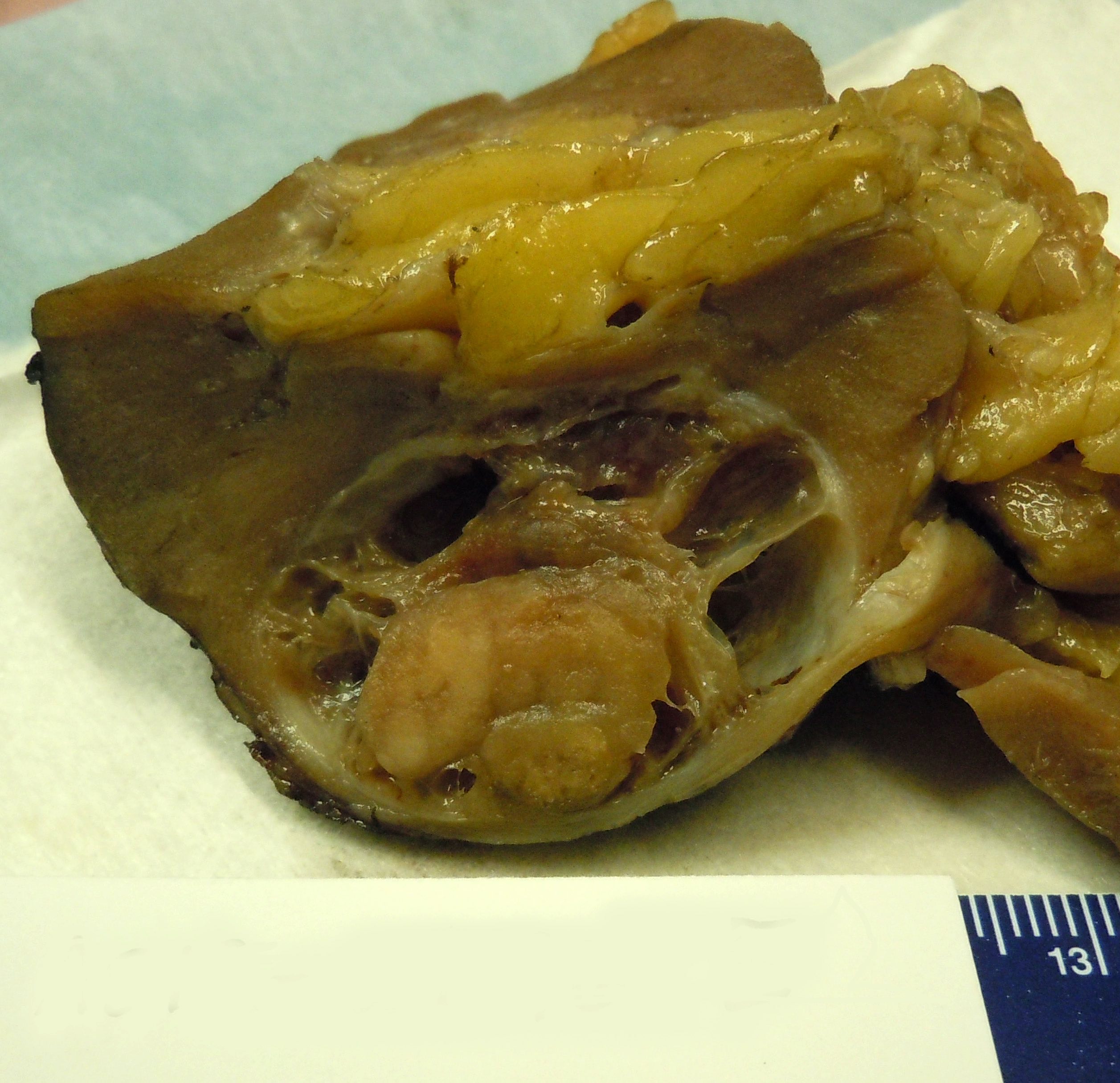
- Solid or cystic, occasionally with flattened peripheral cysts (Int J Mol Sci 2021;23:151)
- Relatively small and well encapsulated within a fibrous capsule
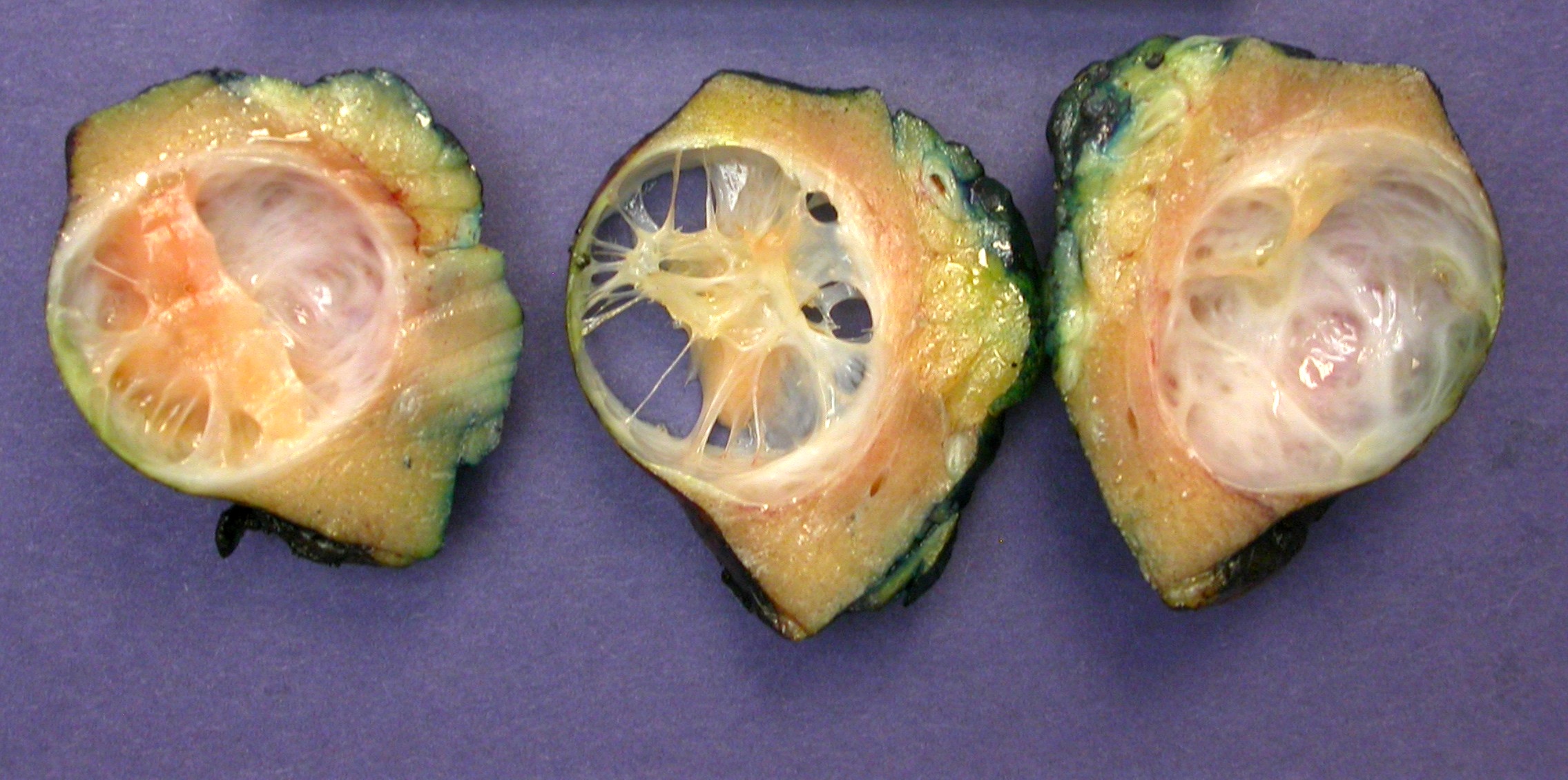
- Solid tumor component cut surface appears tan-white, pink-tan, yellow or red-brown in color
- Necrosis is not observed; focal areas of hemorrhage may occasionally be present
Gross images
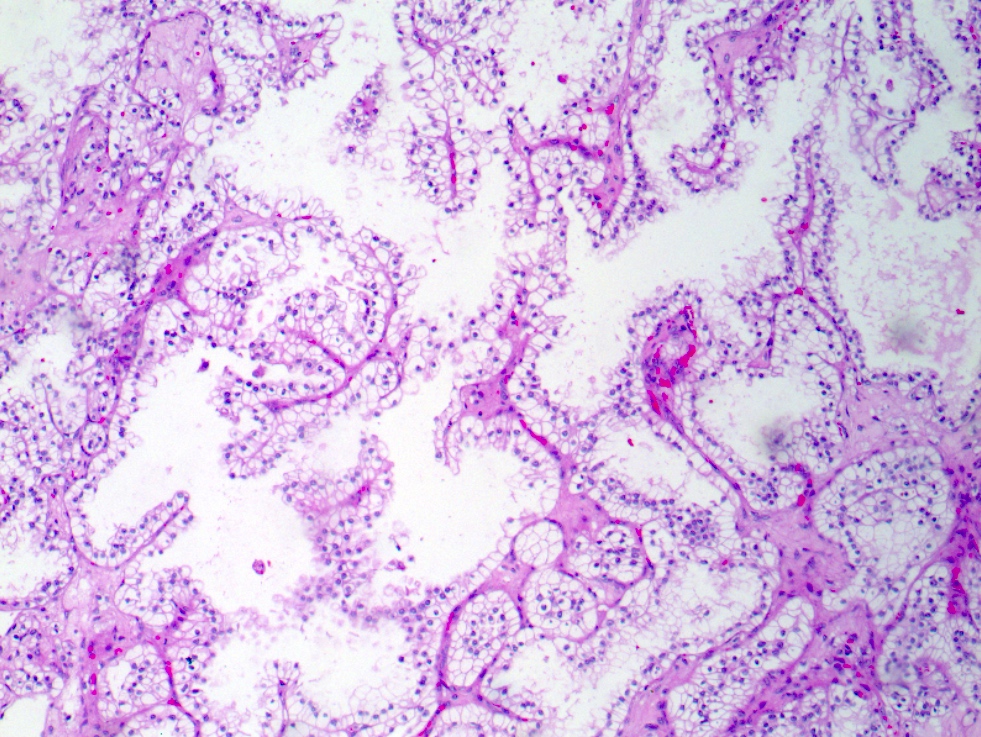
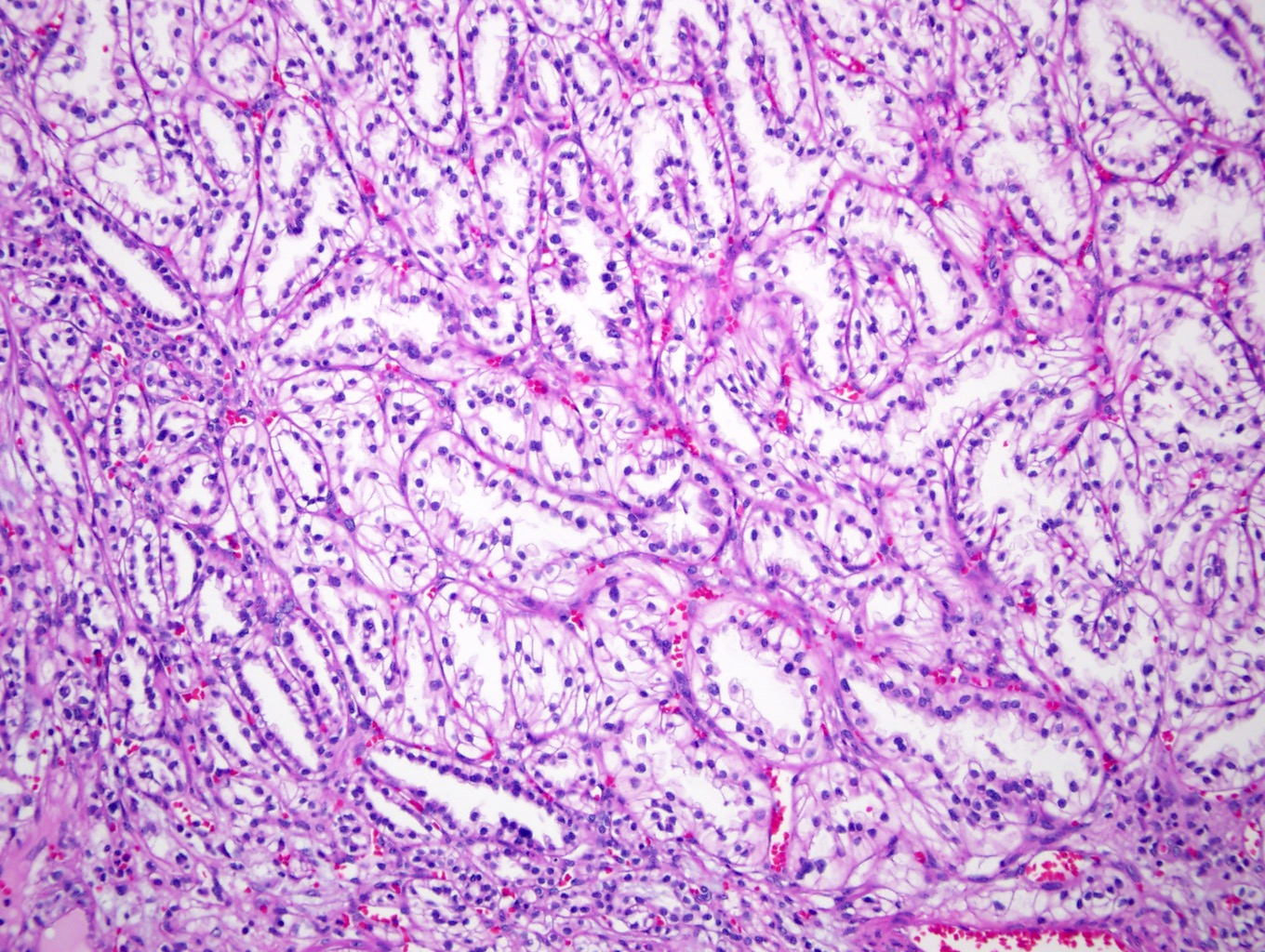
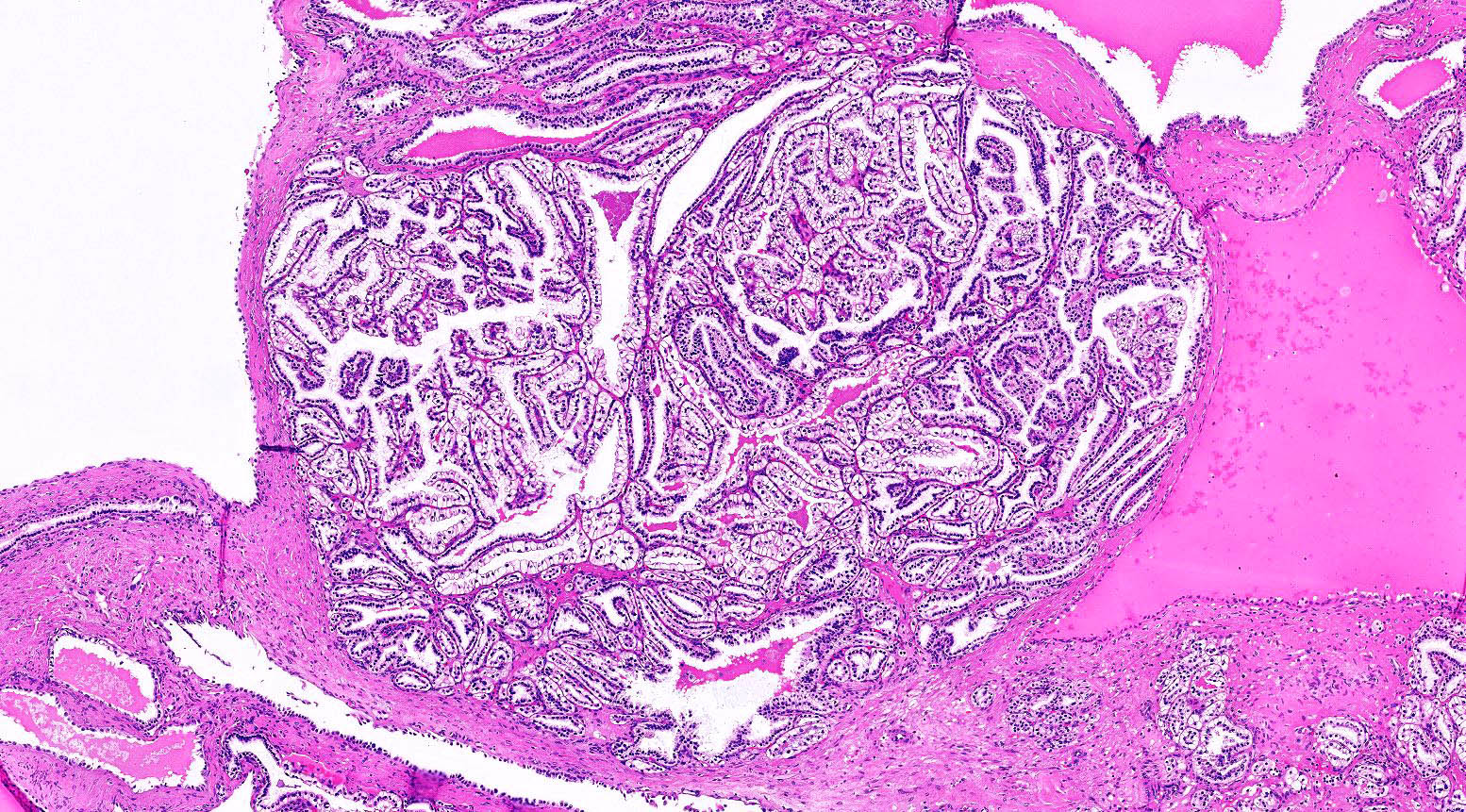
Microscopic (histologic) description
- Various proportions of 2 broad patterns:
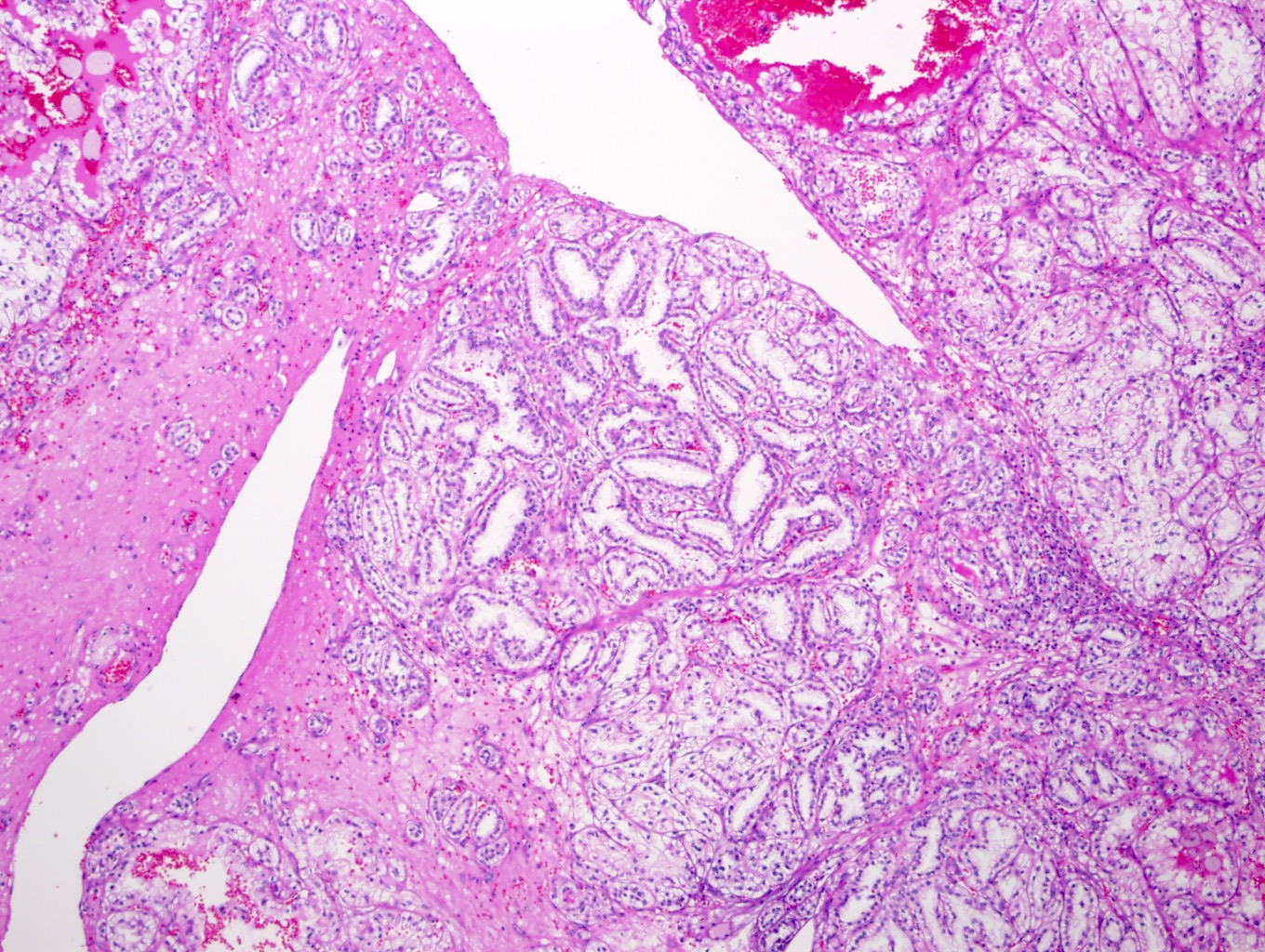
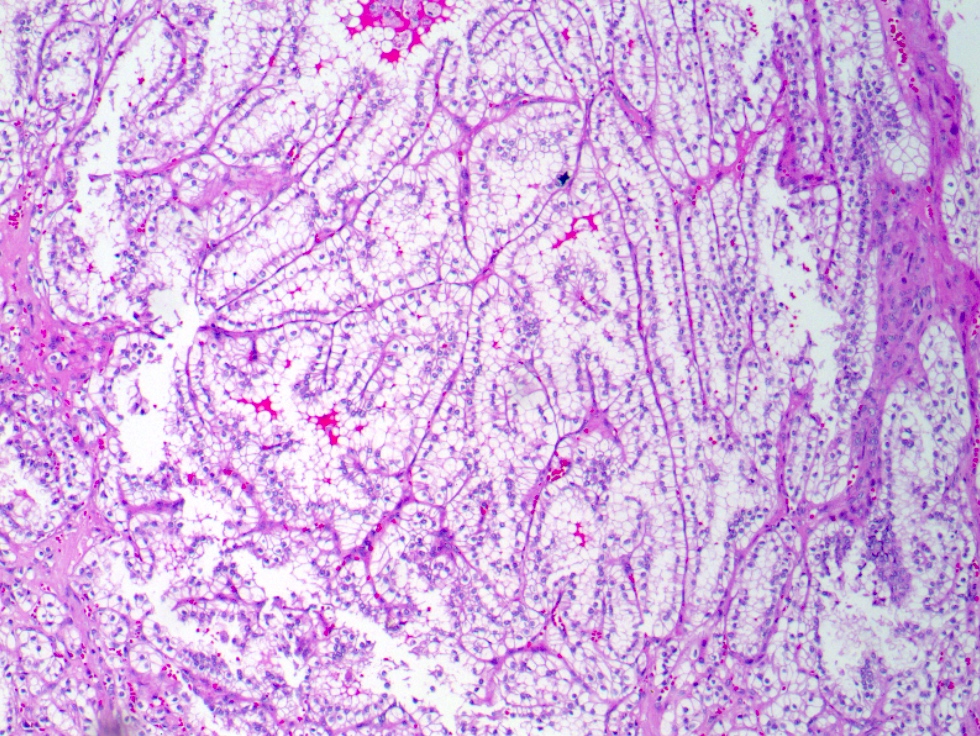
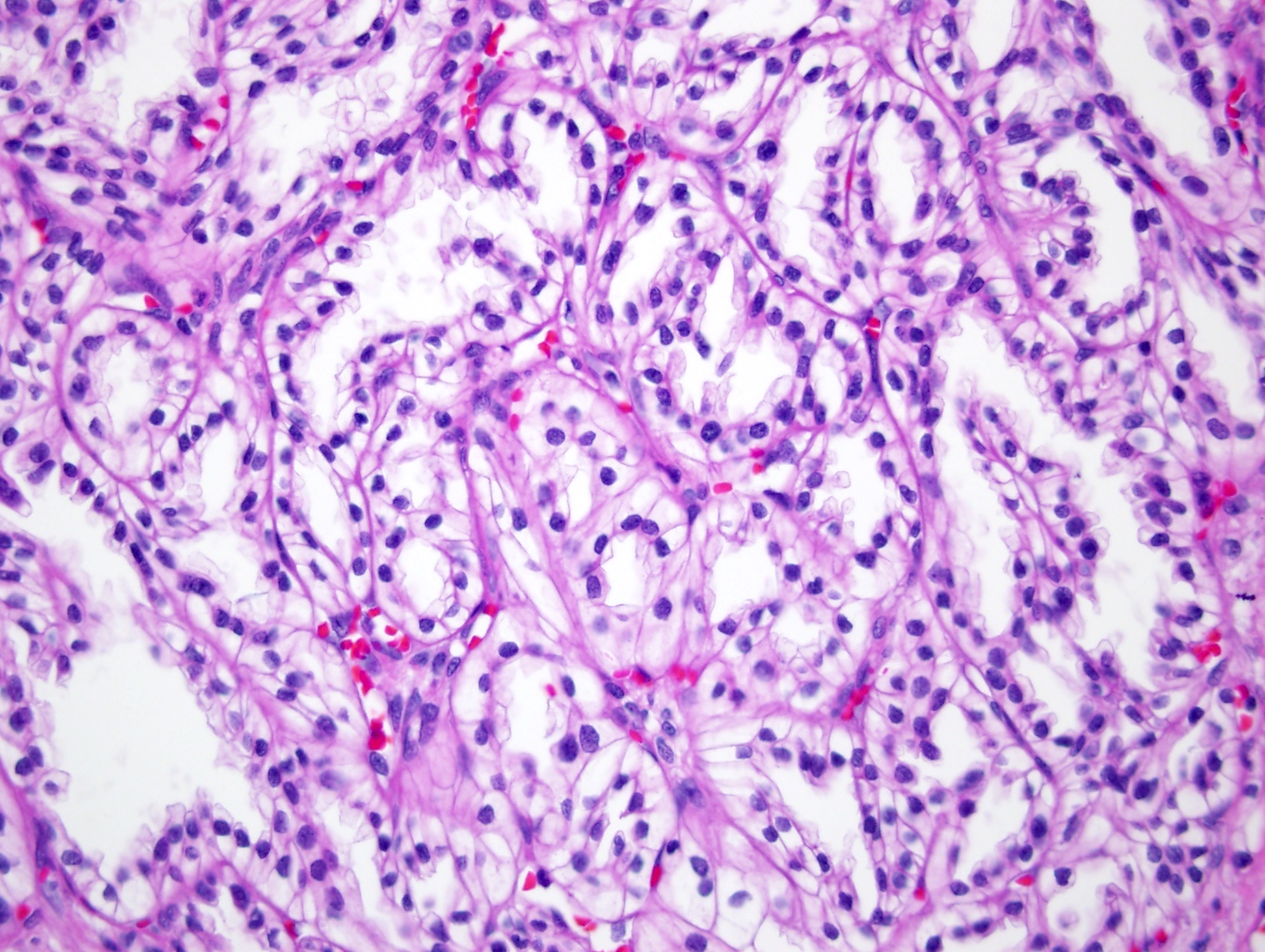
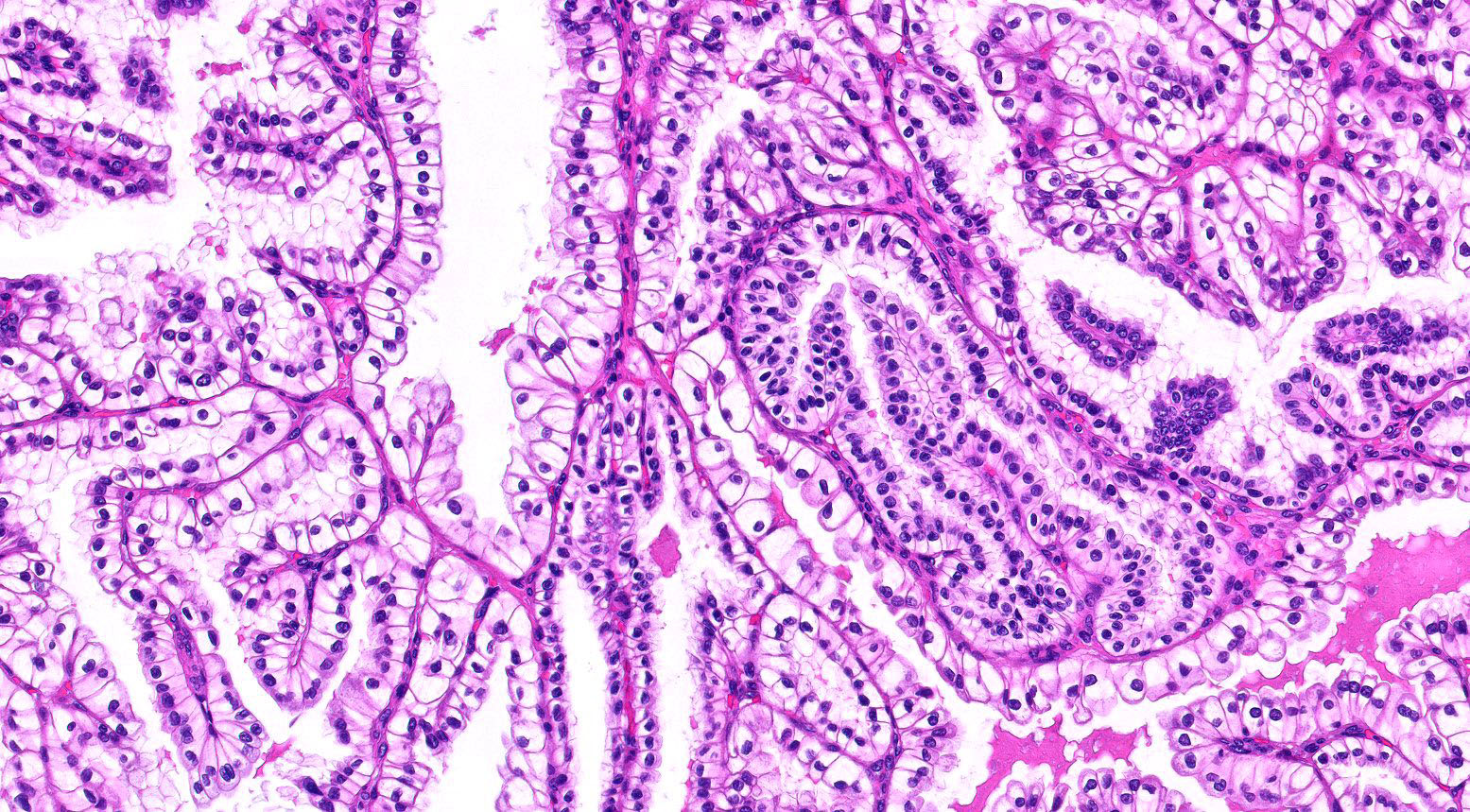
- Focally branched papillary architecture with hypocellular fibrovascular cores lined by cuboidal to flat cells with clear cytoplasm projecting into cystic spaces; extensively branched papillae are uncommon
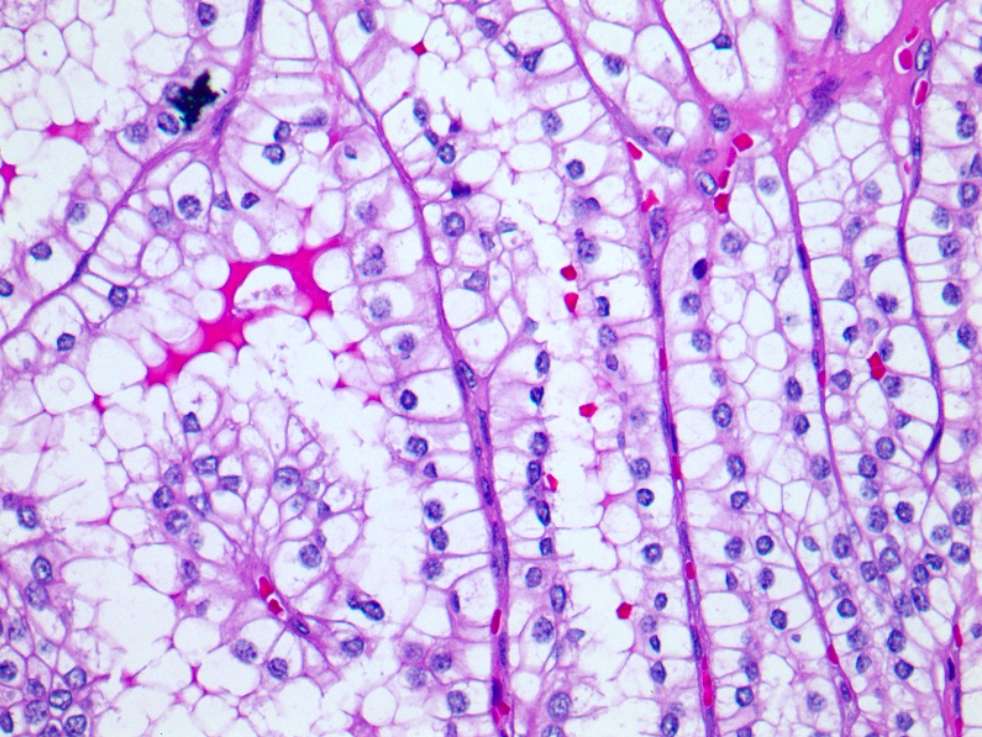
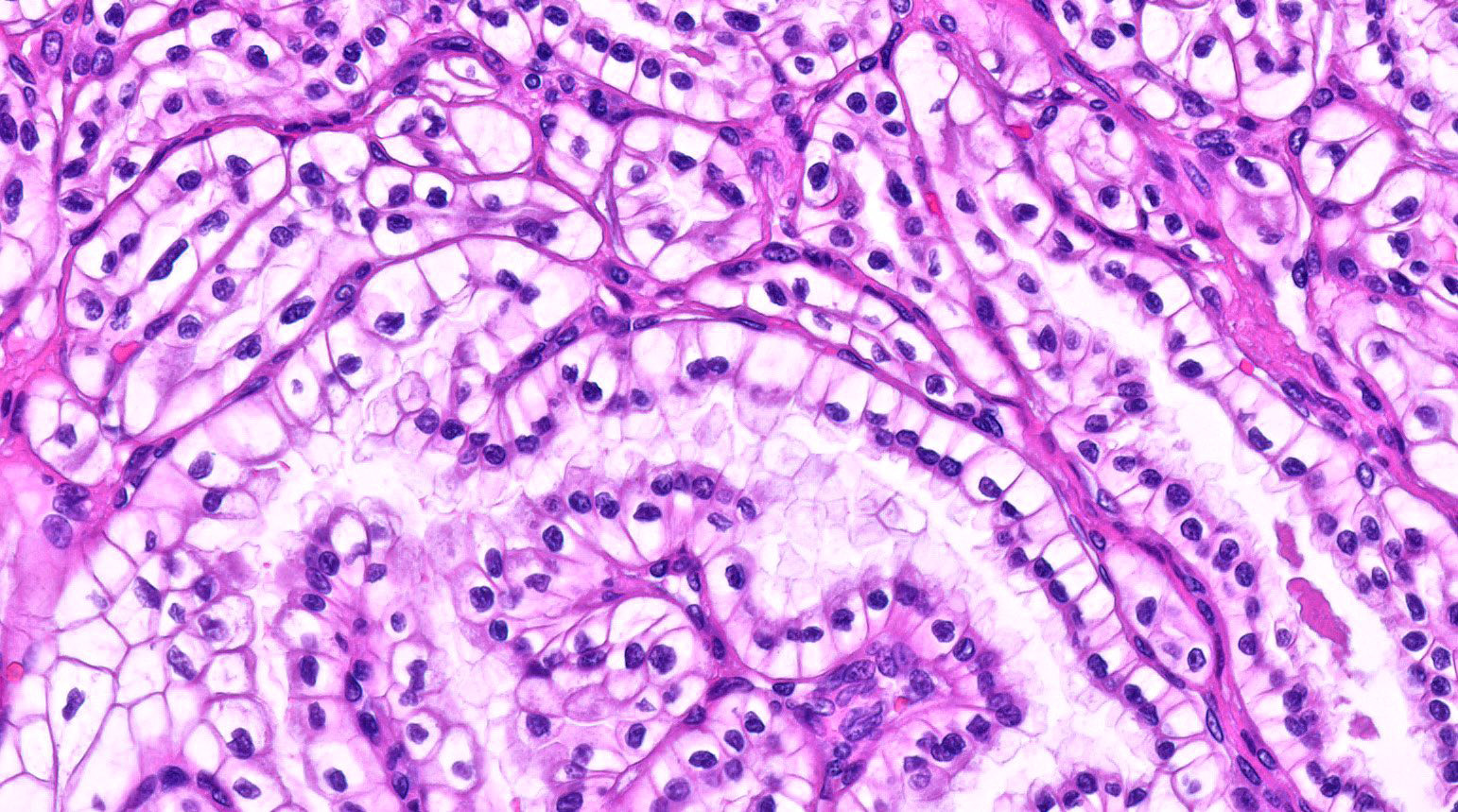
- Areas of dense, compact arrangement of tubular structures lined by clear cells with characteristic luminal polarization of nuclei
- Nuclear and nucleolar size, almost always histologic grade 1 or 2
- Extrarenal extension including vascular invasion is not seen
- Stroma may be fibromyomatous but unusual or conspicuous amounts of fibromyomatous stroma should raise concern for a different entity, a distinct renal epithelial neoplasm harboring mutations in TSC1, TSC2, MTOR and ELOC / TCEB1 (see Differential diagnosis)
- Eosinophilic secretions may be seen
- Reference: Epstein: Differential Diagnoses in Surgical Pathology - Genitourinary System, 2nd Edition, 2022
Microscopic (histologic) images
Cytology description
- Tumor cells arranged in small nests, clusters, arrays or as single cells (Cancer Cytopathol 2017;125:48)
- Columnar tumor cells with eccentric, small, round to oval nuclei with evenly distributed, finely granular chromatin and regular nuclear membrane contour
- Clear cytoplasm containing small vacuoles, with ill defined cytoplasmic borders
- Chief value may be to provide a differential diagnosis that includes clear cell papillary renal cell tumor (Cancer Cytopathol 2021;129:190)
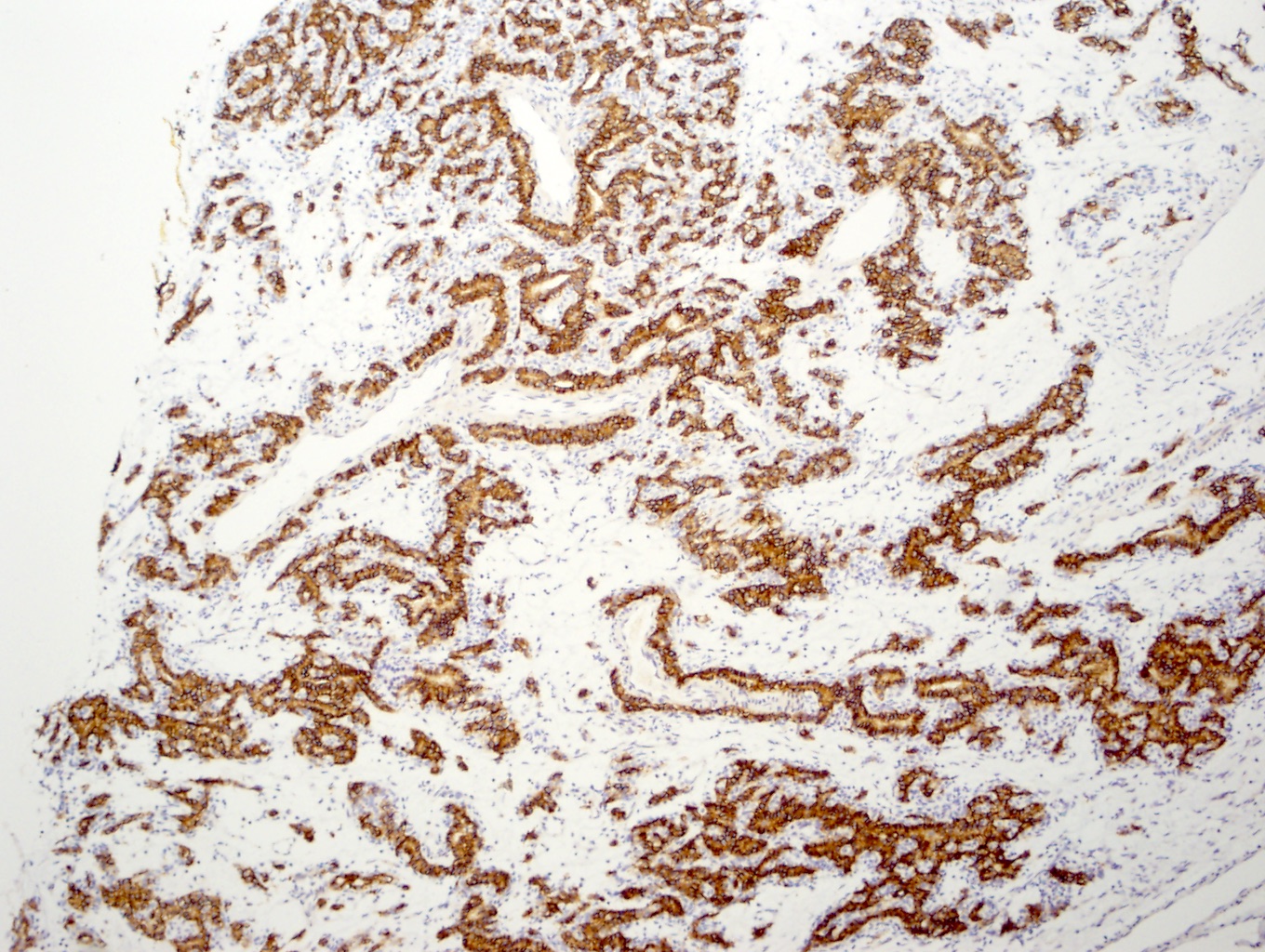
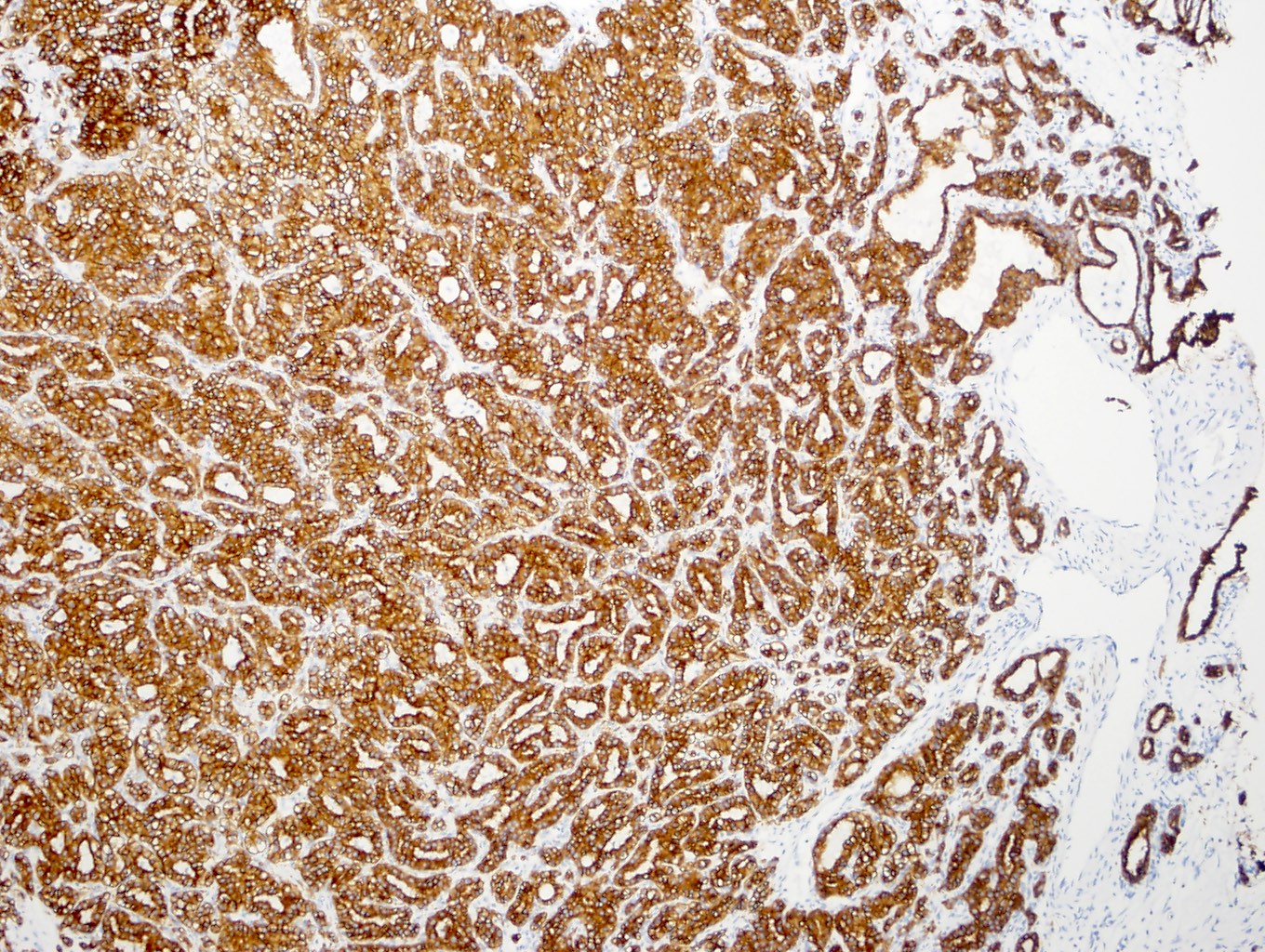
Positive stains
- CAIX: cytoplasmic, cup shaped distribution, with absent staining of luminal aspect
- CK7: diffuse membranous / cytoplasmic staining
- GLUT1: diffuse membranous staining
- GATA3: reported 42 - 76% sensitive, also may be positive in chromophobe (Hum Pathol 2017;66:152, Appl Immunohistochem Mol Morphol 2018;26:316)
- PAX2 / PAX8: nuclear staining
- Epithelial markers, including AE1 / AE3, CAM5.2, EMA, E-cadherin, CK14, CK19, cytokeratin 34 beta E12 (~92% of cases, diffuse and strong cytoplasmic staining) (Pathol Oncol Res 2018;24:447, Pathology 2017;49:10)
- Mesenchymal markers, including vimentin, actin (stromal component, focally positive ~94%), desmin (sporadic) (Mod Pathol 2013;26:697)
- Beta catenin: cytoplasmic
- Parafibromin (Appl Immunohistochem Mol Morphol 2013;21:322)
- CD70 (Histopathology 2014;64:1032)
- CD133 (Histopathology 2014;64:1032)
- p27 (Pathol Oncol Res 2018;24:447)
- Cyclin D1 (Histopathology 2014;64:1032)
- p53, HIF1, c-MET (Pathol Oncol Res 2018;24:447)
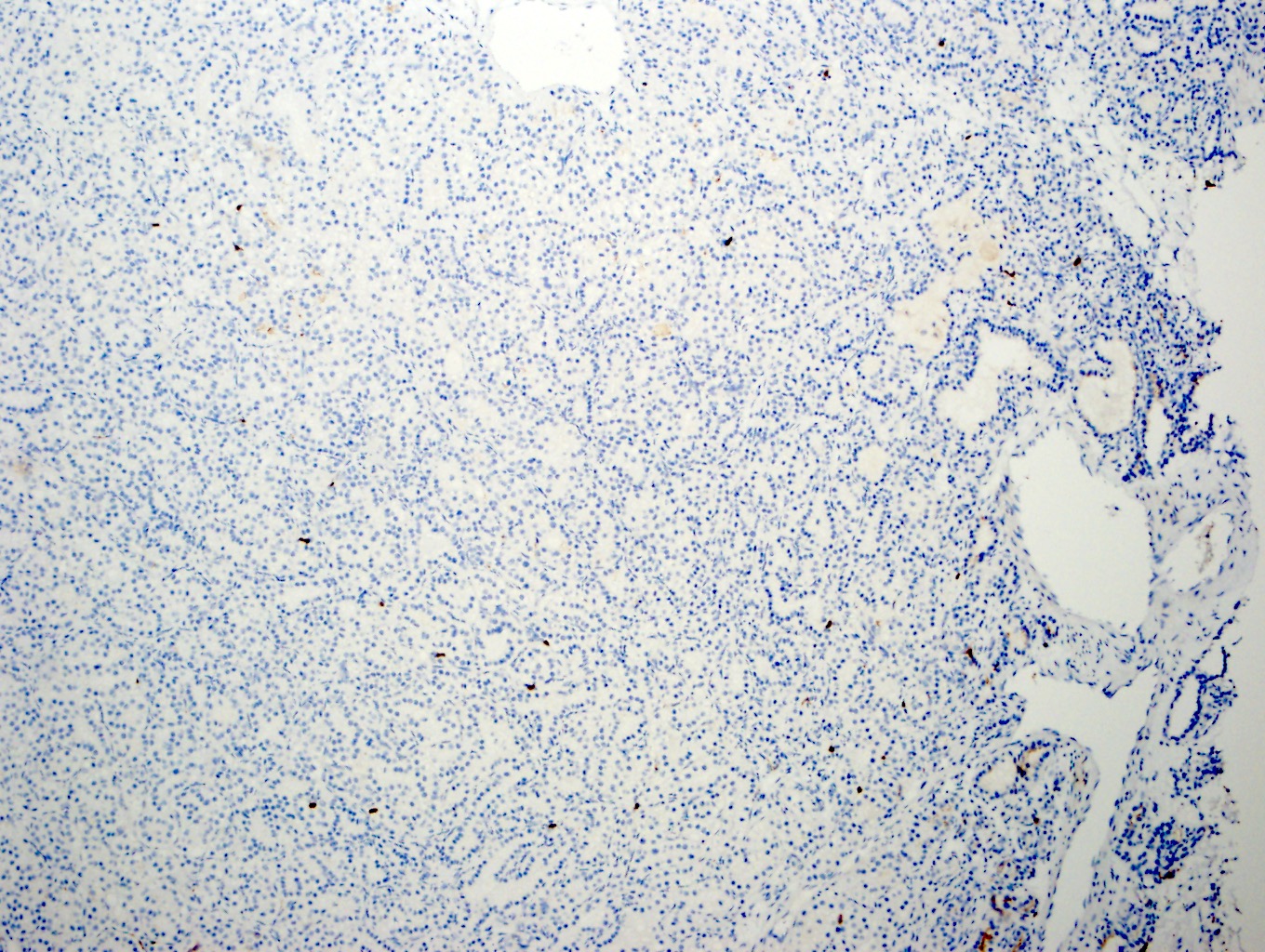
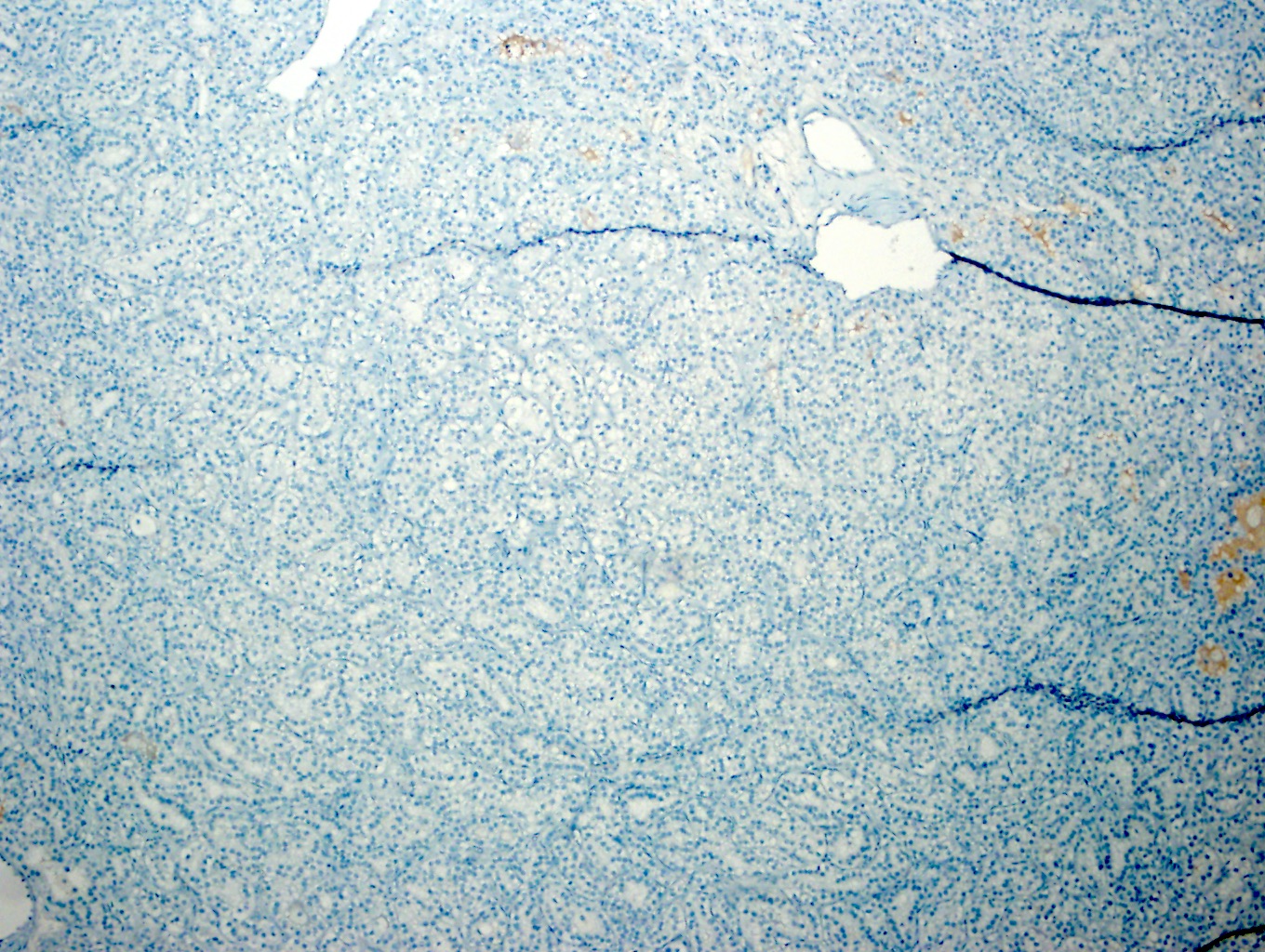
Negative stains
- AMACR / racemase
- CD10: typically negative in solid tumor, may be focally positive in cyst lining areas
- Cathepsin K, RCC Ma (Arch Pathol Lab Med 2012;136:391, Arch Pathol Lab Med 2019;143:1154)
- TFE3, TFEB (Arch Pathol Lab Med 2019;143:1154)
Molecular / cytogenetics description
- Not well understood
- Various chromosomal aberrations identified: monosomy of chromosomes 16, 17, 20; trisomy of chromosomes 10, 12 (Int J Mol Sci 2021;23:151)
- Lower frequency of chromosome 7 and 17 trisomy than PRCC (Int J Mol Sci 2021;23:151)
- Small proportion of patients with von Hippel-Lindau (VHL) disease develop tumor with morphology and immunohistochemical expression consistent with CCPRCT; however, such tumors appear to be genomically related to CCRCC and distinct from CCPRCT (Hum Pathol 2014;45:1966, Am J Surg Pathol 2013;37:1131)
- Absence of VHL gene modifications are observed in cases with immunohistochemical coexpression of CAIX, HIF1 and GLUT1, suggesting VHL mutation independent mechanism of HIF pathway activation
- Hypothesized sorbitol accumulation as a method of HIF1 pathway activation (Int J Clin Exp Pathol 2014;7:7312)
- Mitochondrial DNA:
- Significantly lower mtDNA content compared to other RCC subtypes (Eur Urol 2021;79:468)
- Noncoding RNA:
- Overexpression of miR-200a, miR-200b, miR-200c, miR-141 and miR-429, suggesting enhanced E-cadherin mediated suppression of tumor progression (J Pathol 2014;232:32)
- Upregulation of miR-210 is associated with VHL independent manner of HIF1 pathway activation (J Vet Sci 2013;14:69)
Sample pathology report
- Right kidney, partial nephrectomy:
- Clear cell papillary renal cell tumor, 2.5 cm
- Surgical margins, negative for tumor
- Comment: Immunostaining demonstrate diffuse positivity for CAIX and CK7 and negative staining for CD10 and AMACR.
Differential diagnosis
- Clear cell renal cell carcinoma:
- Papillary renal cell carcinoma:
- Xp11 translocation carcinoma:
- Younger patient demographic
- Abundant psammoma bodies
- TFE3 translocations demonstrable by FISH
- Weakly or focally positive expression of cytokeratins and epithelial membrane antigen
- Majority are cathepsin K positive
- Renal angiomyoadenomatous tumor (RAT):
- Shares similarities in the absence of VHL gene mutations / modifications and chromosome 3p loss
- Biphasic tumor with collapsed acinar architecture and angioleiomyoma-like fibrous / smooth muscle stroma
- Tumors with the appearance of clear cell papillary renal cell tumor but with conspicuous fibromyomatous stroma, may represent a distinct renal epithelial neoplasm harboring mutations in TSC1, TSC2, MTOR and ELOC / TCEB1 (Am J Surg Pathol 2015;39:889, Am J Surg Pathol 2019;43:1135, Am J Surg Pathol 2020;44:571)
Additional references
Practice question #1
Practice answer #1
Practice question #2
Clear cell papillary renal cell tumors are indolent tumors with distinct histologic findings. Which of the following immunohistochemical profiles would best support this diagnosis?
- CD10+, CAIX+, CK7+, AMACR-
- CD10-, CAIX-, CK7+, AMACR-
- CD10-, CAIX+, CK7+, AMACR-
- CD10+, CAIX+, CK7-, AMACR+
- CD10+, CAIX+, CK7- AMACR-
Practice answer #2